Abstract
OBJECTIVES
Burnout is common among junior faculty. Professional development has been proposed as a method to improve engagement and reduce burnout among academic physicians. The Penn State College of Medicine Junior Faculty Development Program (JFDP) is a well-established, interdisciplinary program. However, an increase in burnout was noted among participants during the program. The authors sought to quantify the change in burnout seen among JFDP participants across 3 cohorts, and to explore sources of well-being and burnout among participants.
METHODS
Through a sequential explanatory mixed methods approach, participants in the 2018/19, 2019/20, and 2020/21 cohorts took a survey assessing burnout (Copenhagen Burnout Inventory), quality of life (QoL), job satisfaction, and work–home conflict at the start and end of the course. Descriptive statistics were generated as well as Pearson χ2 test/Fisher exact test for categorical variables and Wilcoxon rank sum tests for continuous variables for group comparisons. To better understand the outcome, past participants were invited to interviews regarding their experience of burnout during the course. Inductive thematic analysis (kappa = 0.86) was used to derive themes.
RESULTS
Start- and end-of-course surveys were completed by 84 and 75 participants, respectively (response rates: 95.5% and 85.2%). Burnout associated with patient/learner/client/colleague increased (P = .005) and QoL decreased (P = .02) at the end compared with the start. Nonsignificant trends toward worsening in other burnout categories, work–home conflict, and job satisfaction were also observed. Nineteen interviews yielded themes related to risks and protective factors for burnout including competing demands, benefits of networking, professional growth, and challenges related to diverse faculty roles.
CONCLUSION
Junior Faculty Development Program participants demonstrated worsening of burnout and QoL during the program while benefiting from opportunities including skill building and networking. The impact of Junior Faculty Development Programs on the well-being of participants should be considered as an element of their design, evaluation, and refinement over time.
Introduction
Burnout is common among faculty in academic health centers (AHCs)1–3 and is associated with significant personal and professional consequences.3,4 Early career faculty are at higher risk for burnout.5,6 Faculty development has been proposed as a method to address burnout among academic faculty,7–9 with some programs showing benefits in burnout-related factors.10–12 However, the impact of professional development programs on burnout among junior faculty at AHCs is not yet well-defined.
The Penn State College of Medicine (PSCOM) Junior Faculty Development Program (JFDP) is a well-established, interdisciplinary program.13,14 We routinely measured burnout among JFDP participants at the start and near the end of the program to foster self-reflection and group dialogue on the topic. We found an apparent increase in burnout later in the program and sought to understand these findings.
We aimed to quantify the change in burnout seen among JFDP participants in 3 consecutive cohorts, and to explore sources of well-being and burnout among participants through a sequential explanatory mixed-methods approach.
Methods
This study received IRB approval from the Penn State Human Research Protection Program (HRPP) on July 16, 2020 (Study #15576). Verbal informed consent was approved by the Penn State HRPP and was provided by each participant prior to participation.
Study Design
This mixed-methods study utilized a sequential explanatory design. The interview portion of the study was designed and executed after survey completion.
Program
A curriculum was designed in 2003 for junior faculty to encourage inquiry, collaboration, and improvements in participants’ academic careers.
14
Participants are selected through a competitive application process, with approximately 90% of applicants accepted. Applicants must have a letter from their chair indicating support for their intended project and a guarantee of 0.1 full-time equivalent (FTE) dedicated time. Though the specific content has evolved over the years, the essential elements have remained constant. Participants meet for 2 to 3 hours every Friday morning at 7
Junior Faculty Development Program Curricular Elements.

Junior Faculty Development Program Participant Expectations.

Participants
We recruited participants based on the following inclusion criteria: (1) graduate members of the JFDP program at PSCOM from the 2018/19, 2019/20, and 2020/21 cohorts (n = 88), (2) adults aged 18 years or older, and (3) fluent in written and spoken English. JFPD participants from pre-2018 cohorts were excluded
Quantitative Evaluation
Participants from Cohorts 1 (2018/19), 2 (2019/20), and 3
Quantitative Assessment of Burnout, Quality of Life, Job Satisfaction, and Work–Home Conflict.

aCategorizes burnout related to personal, work, and clients. For the purposes of this study, considering the interdisciplinary nature of the participants including clinicians from multiple disciplines and basic scientists, the “clients” category was expanded to include patients, learners, clients, and/or colleagues.
Qualitative Evaluation
The authors followed the Standards for Reporting Qualitative Research framework.
Interview participants from Cohorts 1 and 2 were recruited via email. A convenience sample of interview participants were selected on a first-come, first-serve basis until saturation was reached (Figure 1). As saturation was reached during interviews with Cohorts 1 and 2, it was not necessary to pursue additional interviews with Cohort 3.

Consolidated Criteria for Reporting Qualitative Studies (COREQ) Flow Diagram.
Study author JP conducted 15- to 20-min, one-on-one, audio-recorded telephone interviews using a semistructured interview guide (Figure 2) between Nov sixth and December 23, 2020. All interviews were done with participants who had completed the program approximately 6 to 18 months prior. We felt those who had completed the program would have a perspective on its full scope and its effects on their career trajectory. Recent graduates were recruited to optimize recall of program impact on well-being. Audio files of the interviews were professionally transcribed with all identifiers removed.

Semistructured Interview Guide.
Data Analysis
Quantitative
Anonymity prevented pre-post analysis of each individual's responses. All data was grouped into “fall” (near the start of the program) and “spring” (near the end of the program). Quantitative analysis of outcomes was performed using the R statistical program (version 4.0.2) to generate reproducible statistical analyses and tables. Basic descriptive statistics were generated, as well as Pearson χ2 test/Fisher exact test for categorical variables and Wilcoxon rank sum tests for continuous variables.
Qualitative
Thematic analysis describes the systematic process for coding data that was used to answer the research question. 18 Study team members (TR, HS, JP, and EV) reviewed transcripts line-by-line to develop relevant codes reflecting participant experiences within JFDP. Using NVivo Version 12, 2 coders (JP and EV) coded 20% of the transcripts (n = 4) using the codebook. Reliability and agreement of individual coding was compared between the coders. After adjustments were made to the codebook, coders reached an acceptable kappa (k = 0.86). Using the finalized codebook, coder JP coded the remaining transcripts. Coded transcripts were shared with study team members (TR, HS, JP, and EV) who discussed initial emerging themes. Coded data were reviewed and themes finalized in a second meeting with the larger research group.
Results
Quantitative
Eighty-four and 75 participants completed the fall and spring surveys, respectively (response rates: 95.5% and 85.2%). For both survey periods, participants were mostly female, white non-Hispanic, early in their careers (<5 years working), in their mid to upper 30s, and had total FTE ≥ 0.90 and clinical FTE < 0.90 (Table 4).
Junior Faculty Development Program Participant Demographics Arranged by Assessment Period (Fall, n = 84; Spring, n = 75) Between 2018 and 2021.

Results (Table 5) showed significantly increased patient/learner/client/colleague burnout (P = .005) and significantly decreased QoL (P = .02) in the spring compared with the fall. Nonsignificant trends toward worsening in other burnout categories, WHC, and job satisfaction were also observed.
Summary of Outcome Variables for Fall (n = 84) Versus Spring (75) for Junior Faculty Development Program Participants Between 2018 and 2021.
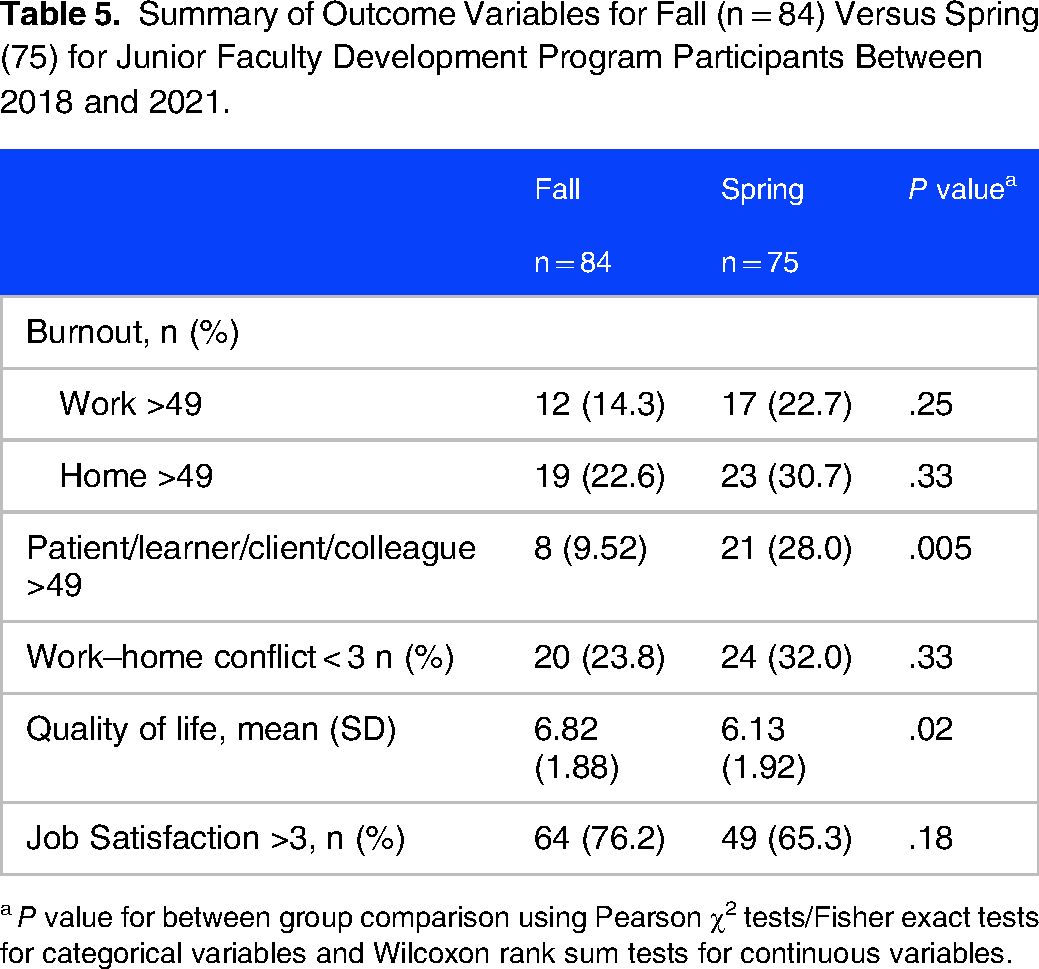
a P value for between group comparison using Pearson χ2 tests/Fisher exact tests for categorical variables and Wilcoxon rank sum tests for continuous variables.
Qualitative
Saturation of data was reached after 20 interviews. Nine participants were interviewed from Cohort 1, and 11 from Cohort 2. One recording was lost due to a technological error, therefore, only 19 interviews were used in the analysis. Overall, participants found JFDP to be helpful in their growth as faculty, and would recommend the program to other faculty. There were 4 themes (Tables 6 and 7), describing positive rewards of the program and suggesting possibilities for improvements and barriers that may have led to a greater sense of burnout.
Codes Used to Support Theme Development for Junior Faculty Development Program Interviewees (n = 19).

a # of participants = the number of participants with quotes that could be coded here.
b # of references = the number of times this code was referenced; that is, one participant could have mentioned more than one topic that was coded here. None of the data were double-coded, meaning a quote was only coded once, to one code only.
Qualitative Themes and Representative Quotes From Junior Faculty Development Program Interviewees (n = 19).

Participation in the program led to personal growth including improvements in knowledge, scholarly skills, and motivation to continue research.
Participants gained skills in research and knowledge of resources available at the institution. Participants also gained confidence in these skills allowing for personal growth and development, and motivation to pursue their interests after completing the program. “I remember leaving those morning JFDP sessions just feeling the sense of enthusiasm and excitement for where I work and my goals for myself. … I have these exciting goals and I feel like a meaningful part of this institution and that's my decision.”
Participants appreciated networking opportunities and support at multiple levels, and felt the program would be beneficial to others.
The participants described their appreciation of support inside and outside the program. Overall participants had a positive experience in the program and would recommend it to their colleagues. “My mentor and I [are] still [in] contact regularly for things that have nothing to do with JFDP, and just learning different faces around the hospital. So that would be my top ‘why’ to participate.”
Competing program requirements, clinical work, and family responsibilities left participants feeling overwhelmed.
Difficulty of managing work–life responsibilities often left participants spending time working outside of dedicated JFDP time to complete responsibilities. This increased feelings of stress and burnout. Some found it difficult to complete program requirements while managing other responsibilities and more intense projects. “I think the balance of work, academics and family responsibilities created a sense of feeling overwhelmed and helpless at times.”
Program characteristics, such as its breadth, timing, and reliance on supportive mentors and departments contributed to burnout and frustration.
Participants expressed frustration and discordance regarding their expectations of the program. While some participants noted their lack of skills in research basics or poor time management, others blamed COVID-19-related factors, institutional barriers, or unsupportive work environments. “And just with the lack of skillset going into that made it even harder. I think for some people who were already PhDs in research, this was a breeze for them to do a grant application.”
Discussion
Participants in this program demonstrated significant worsening of patient/client/learner/colleague burnout and QoL during the program. Trends toward worsening work and personal burnout, job satisfaction, and WHC were also observed. These findings contrast with prior reports suggesting improvement in well-being related factors associated with professional development,10–12 and raise questions about the possibility of using it to address burnout. 7
Qualitative findings suggest the challenges of increased workload and incorporating new skills were the main drivers of increased stress and burnout (Theme 3). Interviewees articulated that the program increased their workload and created difficulty in managing assignments with personal and professional responsibilities. The onset of COVID-19 during the study period likely impacted demands related to teaching, clinical care, and research. Although all chairs were asked to reaffirm their commitment to each JFDP participant's protected time, several participants reported to the program leadership that they were unable to attend JFDP sessions or fully participate due to increased or unanticipated clinical demands. The pandemic also resulted in worsening burnout for clinicians across the United States.19,20 We were unable to control for this national trend in our study. Interviews took place in November to December 2020, and participants’ experiences related to COVID may have influenced their responses in ways that were not accounted for in the qualitative analysis. Given participants’ reports of difficulties balancing program assignments with personal and professional responsibilities, increasing demands related to the pandemic may have exacerbated existing challenges. We elected not to change the nature of the study to focus on the impact of COVID-19 given the inclusion of prepandemic cohorts in the analysis and the commonality of stressors reported among all cohorts. Programs should be judicious regarding workload expectations and ensure a commensurate decrease in other responsibilities to safeguard the sustainability of participation. Flexibility in the face of unexpected shifts in participants’ personal or professional demands may also be advisable.
Some characteristics of the program, including its breadth, intensity, timing, and interdisciplinary nature may have also contributed to increased stress and burnout (Theme 4). Other programs may have differing program characteristics, requirements, structure, or support which may shift outcomes. A review of the published literature suggests that typical JFDPs are discipline-specific and of short duration (several days to a week in length).21–24 While we believe the multidisciplinary and year-long weekly structure of our program has benefits, its breadth and intensity may overwhelm participants while making comparisons to other programs challenging.
Amid evidence of worsening burnout and QoL during the program, some qualitative responses revealed that participants appreciated the program. All interviewees stated they would recommend the program to colleagues. While this may represent selection bias, reported benefits of skill building, networking, collaboration, and institutional knowledge were clearly seen in the data, despite the concomitant challenges. Our findings echo prior research demonstrating the protective effects of engagement 25 and social connectedness 26 against burnout and reinforce the potential for professional development programs to enhance key elements which prevent and mitigate burnout.
The majority of participants were women, a trend which reflects the composition of the cohorts that made up this study (2018-2019; 16 women, 14 men, 2019-2020; 22 women, 8 men, 2020-2021; 20 women, 12 men). Historically, participants in JFDP are split approximately 50% male and 50% female, but this breakdown varies from year to year, with a recent trend toward more female participants (approximately 55%-75% female). Burnout and WHC have both been shown to be more common among women.4,27,28 Because our analysis was descriptive, we cannot comment on whether female predominance in both pre- and post-surveys resulted in a meaningful influence on the finding of worsening burnout during the program.
Mentorship was highlighted as both beneficial (Theme 2) and problematic (Theme 4) by participants. This reinforces the importance of mentorship relationships in faculty development. Effective mentorship facilitated perspective taking and effective project navigation, while failure to connect with a mentor was cited as grounds for project abandonment and dissatisfaction. This suggests there may be value in additional training for both mentors and mentees to optimize this critical relationship in faculty development endeavors.
Several changes in the program have been made since the conclusion of this study in an attempt to reduce the stress of participation, starting with the 2023 to 2024 cohort. First, class start time was moved from 7
Limitations include a single site, small sample size, and lack of demographic data for qualitative interview participants. COVID-related changes influenced participants’ experiences and may limit generalizability of the results.
Conclusions
JFDP participants demonstrated worsening of burnout and QoL during participation in the program, while benefiting from opportunities related to skill building and networking. The impact of such programs on the well-being of participants should be considered as an element of their design, evaluation, and refinement over time.
Footnotes
Authors’ Note
Previous presentations: Results of this study have been presented in a poster format at the 2022 AAFP Physician Health and Well-being Conference; March 30-April 2, 2022; Naples, FL.
Acknowledgements
The authors would like to acknowledge the Qualitative and Mixed Methods Core at Penn State College of Medicine, operating within the Clinical and Translational Science Institute, for assistance with the interview guide, analysis, and interpretation of themes.
Author Contributions
Timothy D. Riley, MD contributed to study design, quantitative and qualitative data analysis, manuscript writing and editing. Jessica A. Parascando, MPH contributed to study design, quantitative and qualitative data analysis, manuscript writing, and editing. Erika VanDyke, MPH contributed to qualitative data analysis, manuscript writing, and editing. Heather L. Stuckey, Ed.D contributed to study design, qualitative data analysis, manuscript writing, and editing. Huamei Dong, PhD contributed to quantitative data analysis, manuscript writing, and editing. Omrana Pasha-Razzak, MBBS, MSPH contributed to qualitative data analysis, manuscript writing, and editing. Lawrence E. Kass, MD, MEd contributed to qualitative data analysis, manuscript writing, and editing. Jennifer McCall-Hosenfeld MD, MSc contributed to qualitative data analysis, manuscript writing, and editing. Sarah K. Bronson, PhD contributed to qualitative data analysis, manuscript writing, and editing.
DECLARATION OF CONFLICTING INTERESTS
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
FUNDING
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding was provided by a general fund in the Department of Cellular and Molecular Physiology at Penn State College of Medicine.
Ethical Approval
Ethical approval was granted by the Penn State University Human Research Protection Program on July 16, 2020 (Study #15576).
