Abstract
Chronic pain (CP) affects over 50 million Americans daily and represents a unique challenge for healthcare professionals due to its complexity. Across all health professions, only a small percentage of the curriculum is devoted to treating patients with CP. Unfortunately, much of the content is delivered passively via lecture without giving students an opportunity to practice the communication skills to effectively treat patients in the clinic. An interprofessional team of health educators identified 5 essential messages that students frequently struggle to convey to patients with CP. Those messages were based on interprofessional and profession-specific competencies to treat patients with CP from the International Association for the Study of Pain. The 5 messages highlighted the importance of (1) therapeutic alliance, (2) consistent interdisciplinary language, (3) patient prognosis, (4) evidence for pain medicine, surgery, and imaging, and (5) early referral to the interprofessional team. For each message, the team summarized relevant research supporting the importance of each individual message that could serve as a foundation for didactic content. The team then developed active learning educational activities that educators could use to have students practice the skills tied to each message. Each learning activity was designed to be delivered in an interprofessional manner.
Keywords
Introduction
Over 50 million Americans suffer from daily chronic pain (CP) that impacts functioning, quality of life, 1 and mental health. 2 CP has also been linked to depression/anxiety symptoms, 3 and suicidal behavior. 4 Pharmacological treatments including opioids have been generally unsuccessful at treating CP,5,6 and have contributed to the opioid crisis. 7 Opioid treatment is associated with an increased risk of opioid use disorder, 8 suicide risk, 9 overdose events, and drug-related death.10,11 With the decline of opioid treatment for CP since 2012 and a rising fentanyl crisis, 12 there is an urgent need to optimize nonpharmacological treatment of CP, 5 and those treatments have been highlighted in the most recent guidelines from the Centers for Disease Control and Prevention (CDC). 13 Unfortunately, patients with CP often prioritize the need for surgery and pain medications in contrast to best-practice recommendations advocating for interprofessional healthcare self-management strategies like exercise.14,15 That disconnect can leave providers feeling uncertain about how to treat patients with CP and frustrated with the lack of an interdisciplinary pain management strategy.16,17 One recent survey of primary care physicians (PCPs) treating patients with CP found that only 31% were satisfied with their ability to provide care to patients with CP, with 43% feeling pressured to prescribe pain medicine. 18 Even when the provider understands what may be useful for a patient, successfully connecting that message to the patient can be a challenge. 19
One potential reason these conversations are difficult is the comparative lack of time spent in healthcare education, across disciplines, in both teaching and, but more importantly practicing, how to evaluate and treat patients with CP.20‐22 The purpose of this article is to share 5 interdisciplinary evidence-based messages and related learning activities that interprofessional health educators could use with their students to improve their skills to evaluate and treat patients in CP. These messages should form the basis for interprofessional learning experiences that allow students to develop and demonstrate competency in evaluating and treating CP.
A recent systematic review of pain content in medical schools found that American medical schools devoted an average of only 11 h of curricular time to pain, with 96% of schools having no required pain medicine content for students.22,23 Physical therapy (PT) schools reported an increase in average pain curricular content from only 4 h 24 to 31 h. 20 Despite CP being an important part of any treatment specialty, medical students report feeling unprepared to treat patients with CP due to insufficient education.25,26 A study of pain education content in schools of pharmacy concluded that coverage of the topic was fragmented and inadequate. 27
Due in part to the opioid crisis,28,29 a shortage of pain physicians, 30 and a plethora of expensive yet ineffective treatments for CP, 15 providers are looking for more effective ways to collaboratively treat patients with CP. For example, including a pharmacist as part of the interprofessional team has demonstrated improved functionality and symptom management, increased use of nonopioid pain medications, and a decrease in both opioid dose and opioid misuse risks.31,32 For patients undergoing arthroscopic hip surgery, simply initiating a PT referral prior to opioid prescribing, compared to opioids before PT, resulted in reductions in total health care costs ($16 995 vs $18 806), total opioid supply (44 days vs 90 days), and percentage of patients that transitioned to chronic long-term opioid use (53%-70%). 33
Other nonopioid and nonsurgical treatment options for patients in CP include exercise,34,35 cognitive behavioral therapy, 36 and sleep hygiene interventions. 37 Another promising treatment is pain neuroscience education (PNE), which involves educating patients about the neurophysiology of CP. 38 Recent systematic reviews have shown PNE to be effective at decreasing kinesiophobia/pain catastrophizing, 39 healthcare utilization, 40 and disability. 41 These beneficial effects are amplified when combined with exercise interventions. 42 These evidence-based approaches may contrast with students’ understanding of the biomedical treatment model, which teaches that all pain is directly due to tissue pathology.43,44 Educators are tasked with giving students evidence for and examples of the effectiveness of biopsychosocial interdisciplinary care for patients with CP.
Fortunately, even brief interventions aimed at changing healthcare provider beliefs away from biomedical and towards biopsychosocial principles of CP appear to be effective.45‐51 Despite encouraging clinical evidence for educating providers about pain, interprofessional health students are likely the most important audience, 52 because clinician beliefs and abilities around pain management are shaped early in their clinical training. 52
Educators in medicine 53 and physical therapy 54 have called for students to be assessed in their ability to evaluate and treat pain in practice-based learning simulations that mirror clinical practice, similar to a competency-based educational model. 55 Unfortunately, the majority of medical schools that assess CP knowledge do so at the cognitive level as opposed to the application level. 53 Students who have only been asked to answer multiple choice questions on CP during school will likely not be well prepared to clinically apply skills like motivational interviewing, 56 active listening, 57 developing a strong therapeutic alliance (TA) with patients, 58 and communicating with other members of the healthcare team. 59 Each of these skills is vital to successfully connecting to patients with CP and supporting behavior change.
While momentum is building to include CP patient management skills into doctor of physical therapy (DPT) program accreditation through the Commission on Accreditation in Physical Therapy Education, 43 this is not currently the case. By using backward design learning theory, 60 educators can design and apply learning experiences that prepare students to meet the ultimate objective, which is to graduate students who are competent in applying the principles of CP management.
Fortunately, medical school, physical therapy, psychology, and pharmacy educators now have access to a growing number of resources to help plan curricular content around CP treatment and practice. Educators in physical therapy,61,62 medicine,63,64 and pharmacy65,66 have outlined courses and activities devoted to pain based on both interprofessional and profession-specific guidelines. The American Association of Colleges of Pharmacy (2023) developed a searchable database of activities conducted at pharmacy institutions as a resource for educators and a method to inform stakeholders about the efforts of schools of pharmacy to address the opioid crisis. There are also a multitude of free resources available to educators to assist in the design of active learning activities, such as Oregon Pain Guidance, 67 the NIH Pain Consortium, 68 and Boston University's SCOPE of Pain podcast series. 69
An interprofessional group representing 10 different health professions 70 outlined core competencies that students should be able to demonstrate to treat patients in pain. 43 Those competencies were expounded further specific to PT students 71 which were then used as a foundation to develop the recent PT profession-wide Pain Education Manual. 72 More broadly, the International Association for the Study of Pain (IASP) has published pain curricula to assist educators from medical schools, 73 physical therapy, 74 occupational therapy, 75 pharmacy, 76 interprofessional education, 77 and undergraduates. 78 Educators also have access to pain curricula at specific medical schools79‐81 to structure their classes. A central tenet of all those curricular models is a strong focus on interprofessional collaboration and knowledge application practice to treat patients with CP.
Multiple brief interprofessional student educational interventions have been detailed in the literature demonstrating that they can be effective at changing student beliefs around pain and understanding of the roles of other professions in CP management. Many focus on improving interprofessional communication between providers which is important for the management of these patients with CP. 82 Others have focused on better understanding opioids/pain physiology, hearing from patients in CP, 83 and developing interprofessional treatment plans.84,85 It is important to continue to highlight the knowledge and competencies that students will need to use during their conversations with patients in CP throughout the curriculum for students to prepare them to be effective clinicians.
Building on the work of Langford et al 86 who asked students to self-report their competency in pain management after an interprofessional learning activity using the Interprofessional Collaborative Competency Scale, 87 educators should attempt to assess students’ postlearning competencies and abilities around treating CP. By assessing competency and not simply recalling knowledge, educators will best prepare interprofessional students for the reality of complex clinical practice.53,54 Unfortunately, both developing and assessing interprofessional active learning application activities that mimic clinical practice is more time-consuming than developing lecture content. Educators who have not taught content related to CP may be unsure which topics and activities are most appropriate for an active learning approach. Our goal is that the 5 interdisciplinary evidence-based messages and related learning activities can be used by interprofessional health educators to improve student skills in the evaluation and treatment of patients in CP. These messages should form the basis for interprofessional learning experiences that allow students to develop and demonstrate competency in evaluating and treating CP.
Process to identify interdisciplinary messages
The nature of this approach was an evidence-based interprofessional CP curricular development narrative review. An interprofessional team of educators representing medicine, pharmacy, physical therapy, and psychology convened over 10 separate meetings in 2022 and 2023 to determine 5 interprofessional CP messages deemed most important for students to learn at the application level. Those messages were based on a contemporary understanding of CP and both interprofessional and profession-specific curricular guidelines such as those created by the IASP. The team then developed active learning educational activities designed to reinforce each message (Supplemental Appendices I-V). Each learning activity included formative/summative assessments, synchronous/asynchronous didactic resources, and a detailed description of the activity designed to reinforce the message. Learning messages were discussed with a medical student graphic artist who created images that reflect the 5 core educational messages; the draft images were shared with the interprofessional team and edited to accurately capture the message of the article.
Five interdisciplinary messages for CP treatment
The 5 interdisciplinary evidence-based messages concerning CP along with a summary of their importance to didactic education are detailed in Table 1.
Five interdisciplinary evidenced-based messages concerning chronic nonmalignant pain.

Message 1: The importance of TA: Trust, empathy, and humility
TA focuses on the connection, warmth, and sense of support created between clinician and patient that empowers the 2 to work collaboratively.57,58 In other words, TA is an indirect measurement of the trust the patient places in a provider to work in a collaborative and connected manner. Unfortunately, patients with CP frequently report a poor TA with their providers. 88 A strong TA enhances the provider's ability to initiate difficult conversations around behavior change and self-management 89 that may run counter to other interventions that a patient might initially prefer. Similarly, patients with CP who felt understood and perceived mutual trust with their providers had higher satisfaction and switched providers less frequently. 90 Figure 1 depicts the importance of the therapeutic alliance.

Therapeutic alliance: scenes from a therapeutic relationship.
A systematic review of the influence of the TA on outcomes for patients with chronic musculoskeletal pain treated by a variety of providers showed a reduction in pain and improvement in physical functioning with higher-rated TA. 91 For physical therapists treating patients with CP, TA is moderately correlated with satisfaction with treatment and the likelihood of recommending that treatment. 92 A study of 3 different treatments for low back pain delivered by physical therapists showed that TA strongly predicted perceived efficacy, pain reduction, and improvement in functioning and disability. 93
Patients in CP unfortunately report that finding providers that both empathize and understand their pain is challenging. 90 There is further evidence that women and individuals from minoritized racial groups with CP may feel particularly misunderstood by their providers, 94 with evidence of racial and gender disparities in pain assessment and treatment.95,96 A lack of focused training for students in all health disciplines in the development of TA and cultural humility may be partially to blame. It is also possible that poor TA is related in part to the challenges that both patients 97 and providers, 98 including students, 99 report in discussing and addressing mental and behavioral health concerns that often accompany CP. With more evidence supporting the importance of TA in improving outcomes for patients with CP, 58 it is important to incorporate TA training, including developing TA when working with diverse patients and comorbid mental health concerns, into health professional education.
Regardless of their specific discipline, health students should be trained to both listen 57 and communicate effectively with patients with CP. 19 Students are highly unlikely to learn how to effectively build TA and utilize patient-centered communication strategies through didactic teaching alone.
Supplemental Appendix I outlines an evidence-based67,100‐107 suggested active learning experience centered on TA. Students work with a simulated patient or lab partner to practice a subjective evaluation, with a special focus on appropriate verbal and nonverbal language that helps the patient feel connected to the clinician. Formative feedback is provided by the simulated patient or classmate to prepare for a summative practical assessment in which the faculty member can ensure students can effectively connect with patients.
Summary of important didactic information: TA
TA is the connection and sense of support that a patient feels between themselves and a clinician.
Patients with CP often report poor TA with their clinicians.
A strong TA appears to be predictive of improved clinical outcomes for those with CP.
Message 2: Interdisciplinary terminology describing pathology: Consistency, language, hope
While best practice recommendations for CP call for a shift from the biomedical model to the biopsychosocial model,108,109 patients still place a high emphasis on biomedical diagnostic information. 110 Unfortunately biomedical diagnostic terminology used to describe pathology can be confusing for patients without a medical background to understand and can vary widely between members of the interdisciplinary team. 111 For example, the diagnostic terminology found in provider notes and imaging results impacts the words patients choose to describe their pain and in turn their perceived prognosis. 112 Figure 2 depicts the importance of consistent terminology to describe pathology.

Consistent terminology for pathology: lost in un-translation.
Words such as “tear,” “bulging,” and “herniated,” while anatomically accurate, can inadvertently increase patient fear, while minimally affecting intervention choices from other members of the team.111,112 Patient confusion over different explanations from different providers about the cause of their pain can increase anxiety about their condition and prognosis. For example, giving patients evidence-based information about back pain rather than imaging their lower back can improve their perceptions of their pain. 113 Likewise, a randomized controlled trial (RCT) that compared medical reassurance to reading magnetic resonance imaging (MRI) results found that reading the specific MRI terminology resulted in patients believing that they were less likely to improve. 97
Confusion is only made worse when there is poor communication between members of the interdisciplinary team. For example, only 16.7% of PCPs reported being satisfied with transition notes from other services where patients received CP care. 18 Ideal communication requires 2 components: (1) providers need to communicate with each other to provide consistent messaging to patients and (2) the interprofessional team must choose accurate patient terminology that minimizes jargon and improves patients’ understanding of their condition and its ability to improve.
Patients with CP benefit from biopsychosocial messaging from providers, and even more so when all providers are communicating the same message. However, switching from the biomedical, pathology-focused language typically used in documentation and interprofessional communication to a biopsychosocial message that does not induce fear can be challenging. Students need the opportunity to practice those patient conversations and hear the perspectives of other disciplines.
Supplemental Appendix II outlines an evidence-based97‐99,111,114‐116 suggested active learning experience centered on using consistent terminology to describe a patient's condition from all members of the interdisciplinary team. Students work as a team to convert biomedical language on an MRI report to biopsychosocial language more appropriate for patient communication. Formative feedback is provided by other student members of the team to prepare for a summative practical assessment where the faculty member can model potential patient responses to communication both with and without biopsychosocial language.
Summary of important didactic information: Consistent terminology
Patients with CP place a high priority on biomedical (anatomical) diagnostic information but may struggle to understand the meaning of that terminology.
A lack of understanding of biomedical diagnostic information (eg, MRI results) can lead patients to worry about their prognosis for recovery.
Research demonstrates measurable changes in clinical outcomes when biopsychosocial as opposed to biomedical terminology is used.
Confusion over their condition and prognosis for recovery is heightened when the interdisciplinary team does not provide patients with consistent biopsychosocial messaging.
Message 3: Assessing and intervening to improve the patient's own prognosis of condition: expectancies, fear, and hope
Most patients with CP do not expect their condition to improve over time either with or without medical care. 110 That is problematic because poor expectations have been linked with lingering pain after surgery, 117 pain during a diagnostic injection, 118 as well as long-term pain intensity and function. 119 Interestingly, patient expectation of recovery was more predictive of shoulder pain recovery for patients referred to PT than physical exam findings or even the physical therapist's expectation of recovery. 120 Advances in understanding of neurobiological underpinnings of CP have highlighted the role of predictive processing in maintaining CP, in that the pain is made worse or sometimes even generated by neurocognitive predictions of pain and bodily harm.121‐123 These predictions contribute to affective states such as fear that can further exacerbate pain via persistent sympathetic activation, contribute to kinesiophobia, and lead to innocuous somatosensory input being perceived and experienced as painful. 124 This predictive pain cycle can become self-reinforcing and may be a primary driver for the chronicity of pain, especially for individuals with centralized pain conditions. Figure 3 depicts the importance of improving a patient’s understanding of a prognosis that includes recovery.

Improving patient's prognosis: the road to recovery.
Indeed, pain catastrophizing, or the cognitive tendency to magnify the threat value of pain and feel helpless in the face of pain, has been consistently linked to higher pain severity, depression, and disability. 125 Providers may inadvertently reinforce these maladaptive processes by emphasizing the role of structural damage, which is often not the driver of CP, or communicating that the patient has an intractable and debilitating condition, which can, unfortunately, become a self-fulfilling prophecy. It is important to ensure that all members of the interprofessional team not only use consistent terminology, but also work collaboratively to provide hope as they describe the patient's prognosis. Inconsistent messaging around prognosis from different team members confuses patients and can negatively impact patient expectations around recovery.
With research showing that educating patients about pain being potentially linked to improving patient expectation of recovery, 126 it is important that patients receive honest yet encouraging messaging from all members of the healthcare team. Consistent, hopeful, and honest feedback from all members of the interdisciplinary team about the recovery process from CP can give patients more adaptive expectations of their functional improvements over time. Practically for a provider referring to another interdisciplinary team member, this might come from how imaging results are discussed, 97 setting realistic expectations for therapy, 127 describing the role of the brain versus structural damage in CP,110,126,128,129 and describing success stories of other patients to improve hope.127,130 For the provider, this may also mean modifying their evaluation away from biomedical, and anatomical diagnoses and instead focusing on measuring function to demonstrate objective progress and continue to optimize expectations of future recovery. 128
To improve patient expectations, providers can use videos that outline the recovery process and what to expect over time. For example, patients with acute whiplash neck pain after a motor vehicle accident who watched a short 10-minute video in the ER reported decreased pain, imaging utilization, pain medicine prescriptions, and incidence of bed rest compared to a group that did not watch the video. 131
Students are highly unlikely to learn how to effectively outline an expected recovery process refraining from nocebo messaging with didactic content alone.
Supplemental Appendix III outlines an evidence-based85,127,132‐135 suggested active learning experience centered on providing a positive prognosis to patients in CP. Students work individually creating discipline-specific messaging to share with a patient in pain regarding their expected recovery. They then meet as an interprofessional team to determine how that messaging can be best shared with a patient and practice that conversation with a simulated patient. Formative feedback is provided by the simulated patient or faculty member to prepare for a summative practical assessment where the faculty member can ensure students can effectively outline an expected recovery process for a patient in pain.
Summary of important didactic information: Importance of positive prognosis
Most patients with CP do not expect their condition to improve.
Patient expectation of recovery has been independently linked to improved clinical outcomes.
Having patients hear what to expect during the recovery process can improve clinical outcomes.
Clinicians should use caution to refrain from nocebo messaging during interactions with patients and provide evidence-based reassurance that injuries will heal.
Message 4: Evidence-based discussion: Pain medications, surgery, and imaging
Pain medications, surgery, and imaging all have important targeted roles to play in our medical system. Unfortunately, in current clinical practice, those 3 interventions are often overused for patients with CP, resulting in poor outcomes when more effective and cheaper treatment options are available but under-utilized.15,136,137 Figure 4 depicts how unnecessary surgery, imaging, and opioids can leave patients trapped without physical therapy and behavioral health.
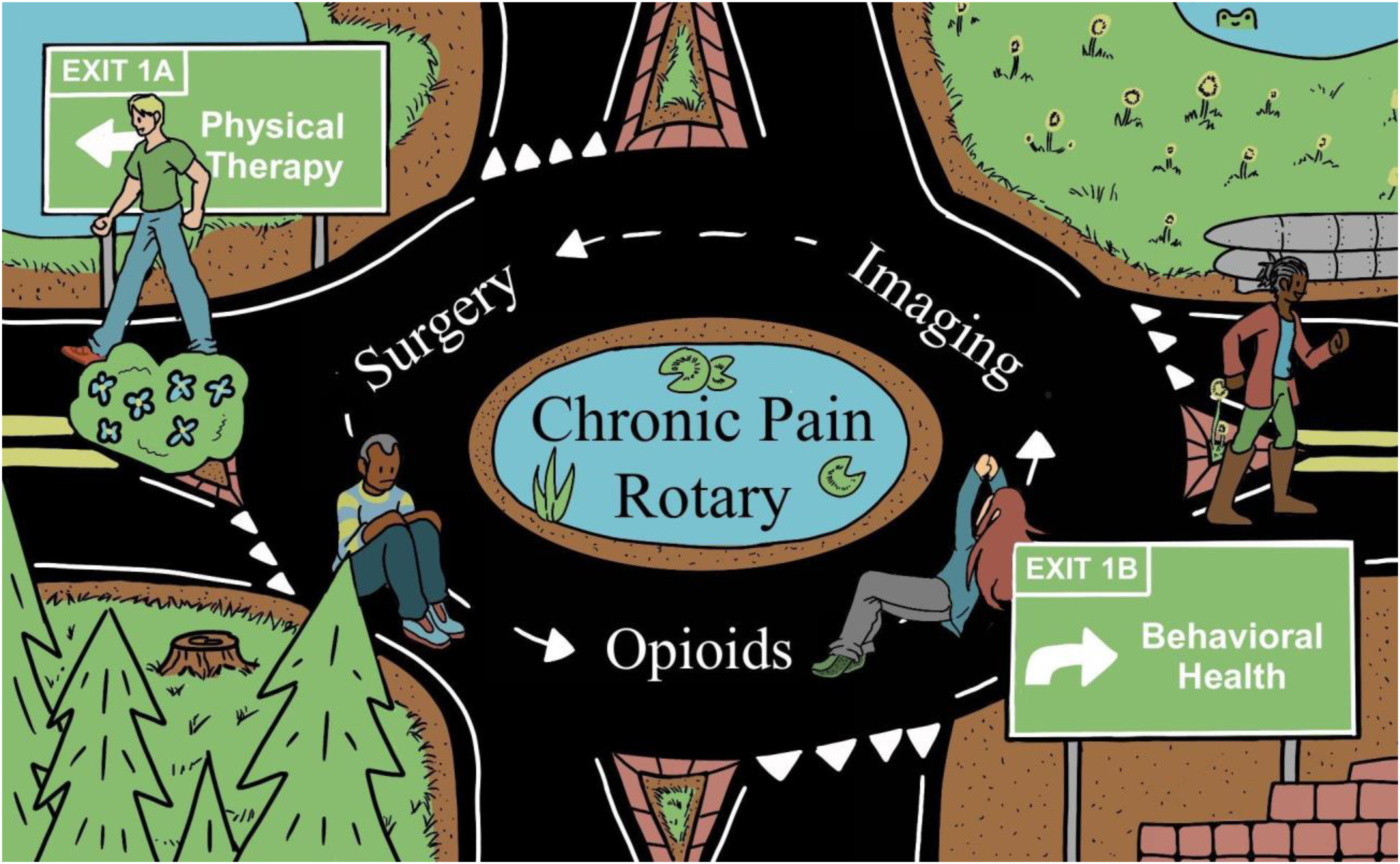
Pain medications, surgery, imaging: the chronic pain rotary.
Pain medications
The 2016 CDC Guideline for Prescribing Opioids for CP recommended nonopioid therapies as a first-line treatment. 138 However, the updated 2022 CDC guidelines note possible misapplication of those recommendations to create biased, inflexible, and harmful policies for patients experiencing and living with CP. 13 The 2022 guidelines stressed individualized person-centered care practices and interprofessional care of CP whenever possible. The guidelines stress again that opioid therapy for CP comes with risks. Opioid use has been associated with an increased risk of cardiovascular events, 5 clinical depression, 139 motor vehicle accidents, 5 suicide, 140 and fractures. 141 Despite those risk factors, many patients perceive opioid medications as necessary to decrease their CP. However, the link between increased opioid medications and CP relief is not supported in the literature. Chen et al 142 demonstrated that for many patients with CP, a reduction in opioid dosage led to a reduction in pain intensity, not an increase in pain intensity. More recently, Fishbain and Pulikal 143 studied the effects of opioid tapering regimens for patients with CP and found that 97% of studies showed that decreasing opioid dosage was associated with either no change in reported pain or an improvement in pain. That study also showed that patients who offered multidisciplinary treatment did better than those who were not.
Surgery
Surgery is an effective and important tool to help manage a variety of conditions; however, surgeries for CP are often used contrary to clinical practice guidelines. For example, despite a multidisciplinary call to action in 2018 to transform how surgery is used to treat low back pain, 144 patients with low back pain continue to be offered low-value spinal fusion surgeries at high rates. 137 Those surgeries are expensive, 145 have high failure rates, 146 and have minimal evidence supporting their use 15 absent neurological findings.
Placebo surgeries have been studied for a variety of health conditions 147 in an attempt to differentiate the biomedical effects of surgeries compared to placebo improvements. While surgical procedures often improve pain and function, their benefits over conservative interventions like placebo surgery, and PT have been minimal to nonexistent for pain arising from labral tears, 148 knee meniscal tears, 149 and tendinopathy. 150 A recent systematic review showed statistically significant but minimal functional improvements in pain and function at 6, 12, and 24 months after a rotator cuff repair compared to conservative care. 151 In fact, a surprisingly high number of patients who are satisfied with their shoulder pain and function after a rotator cuff tear demonstrate a retearing of the surgical site despite being satisfied with their overall function. 152
The purpose of presenting students with evidence that calls into question the efficacy of surgeries is not an attempt to convince students that surgery has no role for patients with CP; rather, it helps reinforce the importance of the evidence-based, biopsychosocial treatment approach. Students can understand how “fixing” the biomedical problem that appears on imaging is not guaranteed to alleviate the problem, highlighting the importance of a more interdisciplinary, patient-centered approach. While more research on placebo surgery needs to be conducted, 147 these studies help reinforce the importance of assessing for and attempting to modify patient treatment expectations, regardless of healthcare discipline. Due to the difficulty of conversations around surgery, both with patients and other members of the interprofessional team, it is imperative that students have an opportunity to practice those discussions prior to entering the clinical setting.
Imaging
Patients consider imaging an important component of the diagnostic and treatment process 153 and may request advanced imaging in the belief that it will change treatment interventions. However, patients with spine pain who receive imaging miss more work, utilize health services more often, and spend more on medical costs than those who do not receive imaging. 154 Furthermore, imaging findings may not depict an accurate representation of the amount of pain someone is experiencing. A prospective study examining lumbar MRIs for patients without low back pain found that when patients did develop low back pain at a later date 84% of the follow-up MRIs were unchanged or improved compared to baseline imaging when the patient was pain-free. 155 Clinicians can use that research to help reassure patients about their prognosis despite findings that may initially appear worrisome. In fact, in a recent RCT, reassuring patients with low back pain that their MRI findings were normal led to improvements in pain intensity, catastrophizing, function, and subjective perception of their condition compared to patients who heard their MRI results without that reassurance. 97
Healthcare providers should not mislead or ignore imaging findings; however, they should carefully consider the language and messaging they use with patients to minimize inadvertent nocebo messaging. 111 One strategy is to review the results of advanced imaging but immediately put results in the context of how often those specific results appear in scans of patients with no pain. Simply including prevalence data on spine imaging findings within a patient's MRI report significantly decreases opioid use one year later. 156 Reviewing imaging findings that do demonstrate pathology for patients with low back pain can give patients a feeling of closure and validate the veracity of their pain complaints. 157 However, that conversation should attempt to leave the patient with a feeling of hope that despite their imaging results, improvement is possible through active interventions.
Conversations around imaging findings can be difficult for students to lead early in their training. Almost like learning a second language, students need to master both biomedical and biopsychosocial vocabulary to describe the same pathology and understand when to use each one. 111 An overly biomedical vocabulary with patients with minimal biopsychosocial understanding can lead to a nocebo effect and cyberchondria 158 where a patient searches online for content and becomes more worried. However, exclusively using biopsychosocial language with patients and providers can lead to decreased confidence that the student understands the pathology. Students of all disciplines should be given opportunities to practice describing imaging findings in different ways to be prepared for the realities of clinical practice.
Supplemental Appendix IV outlines an evidence-based5,15,67‐69,136,143,146,147,156 suggested active learning experience centered on effective evidence-based discussions with patients with CP regarding opioids, surgery, and imaging. Students prepare discipline-specific messaging that they would share with a patient in CP and discuss that messaging as an interdisciplinary team prior to interacting with the simulated patient. Those discussions focused on sharing research about the effectiveness of opioid tapering along with the minimal evidence supporting its use for patients with CP. Students also practice discussing when imaging and surgery are indicated for patients with CP. Formative feedback is provided by the simulated patient and any observers to prepare for a summative practical assessment where the faculty member can roleplay a patient in CP who is convinced that opioids, additional imaging, and surgery are the only ways to “fix” their pain.
Summary of important didactic information: Surgery, opioids, imaging
Despite many patients seeing opioids as beneficial for CP, no level 1 evidence exists that shows opioids are effective at treating CP.
Weaning patients from opioids improves risk factors for multiple injury risks but in many cases results in either unchanged or improved pain scores.
Absent specific patient presentations, clinical practice guidelines do not recommend surgeries for patients with CP as a first-line treatment
Lumbar fusions appear to be expensive and ineffective for patients with CP.
Recent studies that show pathology on imaging in the absence of pain underscore the importance of correlating imaging findings with symptoms and not simply treating imaging findings.
Message 5: Importance of early referral to the interprofessional team: Access, collaboration, and patient communication
Convincing a patient to attend PT or to start exercising when they believe that movement will only make the pain worse is hard to do, especially when patients are requesting other treatment options. Part of the disconnect is that referring providers tend to prioritize improving patient function and minimizing medication side effects, while patients prioritize decreasing pain and receiving a definitive diagnosis of their problem. 159 Unfortunately, contrary to clinical practice guidelines, 13 only a small percentage of patients with CP are referred to PT or psychology despite evidence that shows the importance of early referrals. 160 There are insurance barriers, access barriers, and long-standing historical barriers that limit access and availability of multimodal therapies for patients living with CP. Among individuals with risk factors for CP, engaging in exercise and cognitive behavioral therapy earlier (ie, within 4-8 weeks) appears to reduce the likelihood of chronicity of pain. 161 Figure 5 shows the importance of an early referral.

Early referral: now that's what I call a quick referral.
A scoping review of pharmacists engaged in opioid management activities in primary care settings found an improvement in functionality and symptom management for patients and reduced opioid doses. Changes in prescriber behaviors were also noted including improved adherence to pain management protocols, increased initiation of nonopioid therapies, and increased engagement in risk-mitigating strategies such as prescribing naloxone, accessing prescription monitoring programs, and reduced concomitant prescribing of benzodiazepines. 31 Another scoping review of the pharmacist's role in opioid stewardship highlighted the educational contributions of the pharmacist as a member of the interprofessional healthcare team. Pharmacists’ education of patients and other healthcare professionals was associated with improved pain scores, enhanced knowledge and understanding as well as reducing opioid use. 32
A 2013-2015 survey of PCP referral patterns for patients with knee osteoarthritis (OA) found that out of 1000 visits, only 46 received PT referrals, and 221 received lifestyle counseling, while 498 received NSAIDs and 316 received opioids. 162 Pain medication referrals for knee OA increased from 2007 to 2015 with PT and lifestyle coaching appearing to be under-utilized according to clinical guidelines. 162 Sun et al 163 found a similar under-utilization of PT, with only 29.3% of patients with new-onset musculoskeletal pain receiving physical therapy in < 90 days after their initial medical appointment. Despite low referral rates relative to best practice guidelines, physical therapy remains a low-cost effective treatment for patients in pain, but its effectiveness improves greatly the earlier a patient can begin formal PT.
A systematic review for patients with low back pain found that initiating a PT referral within 30 days of a medical appointment resulted in significant reductions in opioid use, future healthcare utilization, spinal injections, and spine surgery. 164 Even PT within 90 days of a medical appointment is correlated with a 10% reduction in opioid use for shoulder, neck, back, or knee pain and decreased dosage amounts for those who do use opioids. 163
Unfortunately, not all healthcare providers have immediate referral access to other members of the interprofessional team. That is especially true in rural areas where other providers may be located far away. In those situations, clinicians can recommend early referral to telehealth services165‐167 which grew in popularity during the COVID-19 pandemic. 168 Clinicians can also utilize programs like the Project for the Extension for Community Healthcare Outcomes (Project ECHO) 169 to connect with other interprofessional providers to reinforce IASP didactic pain content from an interprofessional approach. 170
All members of the healthcare team whether in the same geographic location or connected electronically can help support the message of exercising and early referral to active patient-centered treatment approaches like PT and psychology. Patients with CP often identify the need for extra support when initiating an exercise program, 171 and that support should be reinforced with consistent messaging from the entire team. Educators should give students an understanding of the research supporting early referrals but more importantly, the opportunity to practice talking with diverse patients about how they can support that behavior change.
Supplemental Appendix V outlines an evidence-based33,101,102,104,105,135,163,164 suggested active learning experience centered on the importance of early referral to the interdisciplinary healthcare team and safe, effective interventions such as exercise. Students prepare discipline-specific reports to the rest of the interprofessional health care team to share and better understand how other disciplines would care for that patient. Those discussions will focus on sharing research about the importance of early referral to all members of the healthcare team and practice discussing both with patients and payers the importance of early referral to both other providers but also encouragement for increasing physical activity. Formative feedback is provided by other student classmates and faculty observing those discussions to prepare for a summative practical assessment where the faculty member can roleplay a patient or payor who is unwilling to try conservative management options like psychology or physical therapy.
Summary of important didactic information: Importance of early referral
Few patients with CP are referred to the interprofessional team early within entering the medical system as recommended by clinical practice guidelines.
Early compared to late referral to physical therapy has been linked with a reduction in opioid dosage, overall cost, and need for additional surgery.
Providers from all disciplines can help reinforce the importance of exercise.
Limitations
This approach had several limitations. First, the authors do not represent all health professions that play a role in interprofessional CP management. Additionally, the messages in this article were developed by a small team of clinician educators without a systematic external review process (other than manuscript peer review) by other providers or patients. All authors were affiliated with the same university so there is potential bias on conclusions that may not be generalizable to all American health professional schools.
Summary
Preparing health science students to evaluate and treat patients with CP requires formative, active learning opportunities that provide an opportunity to receive constructive feedback prior to clinical practice. To prepare students for those assessments, educators should design didactic content built on resources like the IASP curricular guidelines73‐75,77,78 and profession-specific resources. 72 The 5 interprofessional messages presented in this viewpoint aim to highlight learning areas that should be prioritized when teaching healthcare students about CP.
From that didactic foundation, a healthcare educator aiming to redesign their content to utilize active learning within a competency-based educational model 55 should give students opportunities for formative evaluations to enhance preparedness for competency assessment. Competency-based education translates the competencies needed for effective pain treatment into active skills by providing students opportunities to progress from simply observing a faculty member completing a task to eventually doing that task on their own with no supervision. Along the way, supervision needed to perform those “Entrustable Professional Activities” reduces as students demonstrate the ability to perform competencies with less and less supervision. 172 Educators from PT,173‐175 pharmacy, 176 psychology, 177 and medicine 178 have all advocated for an educational shift towards assessing student competency and not simply knowledge recall.
Conclusion
To treat a problem as prevalent and complex as CP, it is imperative that students are given the opportunity early in their education to practice the competencies they will need to demonstrate to effectively manage patients in CP. The 5 messages and active learning activities presented in this viewpoint and Supplemental Appendices serve as a flexible foundation for interprofessional educators to meet their specific educational goals related to teaching students to treat patients with CP. The activities provide a framework on which educators can build, while considering variations needed to accommodate for access to resources such as synchronous access to students of other disciplines and simulated patients.
Supplemental Material
sj-docx-1-mde-10.1177_23821205231221950 - Supplemental material for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application
Supplemental material, sj-docx-1-mde-10.1177_23821205231221950 for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application by Jeb Helms, Laura Frankart, Melissa Bradner, Jonathan Ebersole, Beck Regan and Taylor Crouch in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205231221950 - Supplemental material for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application
Supplemental material, sj-docx-2-mde-10.1177_23821205231221950 for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application by Jeb Helms, Laura Frankart, Melissa Bradner, Jonathan Ebersole, Beck Regan and Taylor Crouch in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-3-mde-10.1177_23821205231221950 - Supplemental material for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application
Supplemental material, sj-docx-3-mde-10.1177_23821205231221950 for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application by Jeb Helms, Laura Frankart, Melissa Bradner, Jonathan Ebersole, Beck Regan and Taylor Crouch in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-4-mde-10.1177_23821205231221950 - Supplemental material for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application
Supplemental material, sj-docx-4-mde-10.1177_23821205231221950 for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application by Jeb Helms, Laura Frankart, Melissa Bradner, Jonathan Ebersole, Beck Regan and Taylor Crouch in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-5-mde-10.1177_23821205231221950 - Supplemental material for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application
Supplemental material, sj-docx-5-mde-10.1177_23821205231221950 for Interprofessional Active Learning for Chronic Pain: Transforming Student Learning From Recall to Application by Jeb Helms, Laura Frankart, Melissa Bradner, Jonathan Ebersole, Beck Regan and Taylor Crouch in Journal of Medical Education and Curricular Development
Footnotes
Authors’ contributions
Jeb Helms—conceptualization, methodology, resources, writing–original draft, writing–review and editing, supervision, and project administration. Laura Frankart—conceptualization, methodology, resources, writing–original draft, writing–review and editing. Melissa Bradner—conceptualization, methodology, resources, writing–original draft, writing–review and editing. Jonathan Ebersole—conceptualization, methodology, resources, writing–original draft, writing–review and editing, and visualization. Beck Regan—visualization and artwork creation. Taylor Crouch—conceptualization, methodology, resources, writing–original draft, writing–review and editing.
FUNDING
The author(s) received no financial support for the research, authorship, and/or publication of this article.
DECLARATION OF CONFLICTING INTERESTS
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
