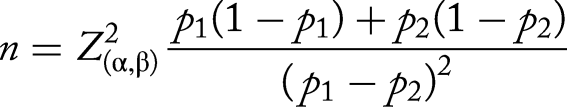Abstract
OBJECTIVES
To improve 4 skills (communication, history-taking, past history-taking, and documentation) in medical students, we designed and pilot-tested a curriculum to teach a sample of Year 4 (Y4) students these skills and compared the clinical performance of these students with students not receiving the intervention.
METHODS
The study focused on the new curriculum's effectiveness in enhancing students’ performance of these skills. To minimize exposure across groups, participants were divided into intervention and control groups at random and placed in various classrooms. We evaluated each group's clinical competency 3 times: prior to the intervention, 9 weeks afterward, and 2 years later.
RESULTS
There was no difference at baseline between the 2 groups. Immediately following the intervention, the mean score of the intervention group's skills was significantly higher than before and higher than the control group in each clinical skill. The performance difference between the 2 groups was maintained for 2 years following the intervention.
CONCLUSIONS
Following a 9-week curriculum, evaluators rated students’ performance higher than their counterparts who learned these skills through standard informal exposure in the clinical setting. The fact that this performance advantage was maintained for 2 years following the intervention is a testament to the durability of the intervention and the value of dedicated training in these critical areas at an early point in students’ clinical careers.
Introduction
Teaching and learning in the clinical setting are cornerstones of medical education. Communication with patients and history taking are critical skills for medical students to master in their training.1–3 These are the building blocks for advanced clinical skills, including diagnostic reasoning, clinical decision-making, patient education, and counseling. Accurate and precise documentation is a critical skill that builds students’ capacity to synthesize subjective and objective information, summarize and prioritize a patient's problems, and apply clinical reasoning in formulating an assessment and plan.4,5 These skills are best learned while working in a clinical environment through observed practice and feedback from experienced supervisors and multiple opportunities to refine their skills. 6 However, students who enter their clerkships without a foundation in clinical skills may be at a disadvantage in acquiring these skills in a busy clinical environment that does not have a formal clinical skills curriculum and where demands of patient care may overshadow the teaching of basic skills.7,8 A vast body of research demonstrates that students entering clinical clerkships have not yet mastered these 4 clinical skills.9–11 Several medical schools in the United States and other countries have already adopted formal training for these skills.12–14 Nevertheless, formal training in these clinical abilities has been notably lacking at medical schools in Vietnam, where students in the first 3 preclinical years have little direct interaction with patients, exposure to clinical settings, or instruction in these clinical skills. Most medical students worked on their own to enhance these abilities, resulting in poor performance when confronted with patients. To address this deficiency in our university and to contribute to improving the overall quality of clinical teaching and learning at Haiphong University of Medicine and Pharmacy (HPUMP), we developed an intervention to provide students with formal training in these clinical skills in year 4, their first clerkship year. If successful, this training would become standard practice for all medical students at our university and might be adapted by other universities in Vietnam.
Subjects and methods
Ethical statement
Research methods were performed in accordance with the relevant guidelines and regulations of the Declaration of Helsinki. Ethics approval was obtained from the Research Ethics Board of Haiphong University of Medicine and Pharmacy. The Research Council of HPUMP reviewed and approved this research protocol.
Written informed consent was obtained from all participants.
Ethics Approval Number: 210/QD-YDHP – 01/03/2019
Subjects
187 fourth-year (Y4) students.
Place and duration of study
The study was carried out at Haiphong University of Medicine and Pharmacy, Haiphong, Vietnam from 01/04/2019 to 01/10/2021.
Sample size
The sample size for the group of students in the intervention group:
We calculated the minimum sample size for the intervention group to be 60 students. In fact, the intervention group was conducted with 93 students.
Criteria
Inclusion criteria
Fourth-year students who are studying general practitioner at Haiphong University of Medicine and Pharmacy.
Exclusion criteria
Any students who decline to participate.
Methods
Research design: Randomized controlled educational trial with blinded assessment. Each class at HPUMP consists of approximately 562 students, randomly divided into 12 classes for administrative purposes. In order to limit exposure and possible contamination of the intervention and control groups, we randomly selected Y4 students from different classes for the intervention and control groups. The research was conducted in the Pediatric and Surgery departments of Haiphong University of Medicine and Pharmacy.
The intervention group was planned to include 93 students randomly selected from Classes A and B; the control group 94 students randomly selected from Classes E and F.
Intervention
The intervention consisted of formal training in 4 key clinical skills through 18 structured modules: communication with patients (8 modules), history taking (current illness and past medical history [5 modules], and documentation in medical records [5 modules] [see Supplemental Appendix 1]). Sessions were 2 to 4 h each. Students in the control group acquired these skills through their clinical exposures during clerkships, as is standard practice for clerkship students, without formal or standardized training.
All modules were designed by the Health Professionals Education and Training for Health System Reforms Project (Vietnamese Ministry of Health) (see Intervention Framework – Supplemental Appendix).
Student performance was assessed in the 4 clinical domains using a 44-item checklist (see Checklist 1 to 4 – Supplemental Appendix). Assessments occurred at baseline, following the 9-week intervention, and 2 years following the intervention. Assessors included lecturers from the UMP, postgraduate students, resident physicians, and medical specialists. All assessors were trained in techniques of clinical observation and trained to use the checklist and were blinded as to student status (control vs intervention).
Performance was evaluated using a 3-point rubric:
point: skill not performed point: skill performed incorrectly or incompletely points: skill performed correctly and completely
Statistical analysis
We calculated the average score of skills for the intervention and control groups at baseline, 9 weeks, and 2 years. We compared the performance of the intervention and control groups at each stage as well as the progress of each group across the stages.
Results
Table 1 demonstrates no baseline difference between intervention and control groups in summary scores for communication skills. Shortly after the intervention (at 9 weeks), there was a significant increase in scores for the intervention group (P < .001) but no significant change in scores for the control group (P > .05). After 2 years, the intervention group demonstrated significant improvement compared to immediate postintervention scores (P < .001), whereas the control group showed improvement (P < .01). All differences are statistically significant.
Comparison of students’ communication skill scores before, and after intervention for 9 weeks, for 2 years, and with the control group.
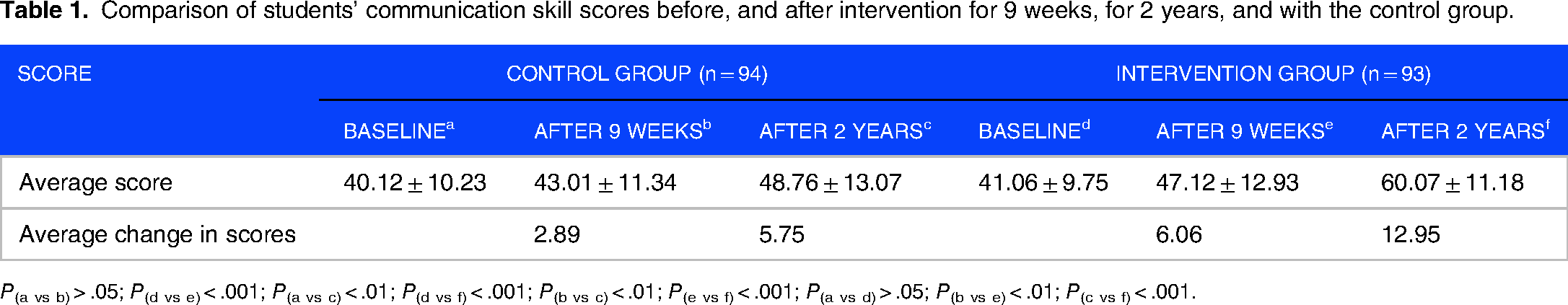
P(a vs b) > .05; P(d vs e) < .001; P(a vs c) < .01; P(d vs f) < .001; P(b vs c) < .01; P(e vs f) < .001; P(a vs d) > .05; P(b vs e) < .01; P(c vs f) < .001.
A similar pattern was found for both history-taking skills (history of present illness and past medical history). Table 2 demonstrates that baseline skill levels for the history of present illness showed no significant difference between intervention and control groups. At 9 weeks, the average score for the intervention group had improved significantly compared to baseline (P < .001) and was significantly higher than the control group (P < .01). At 2 years, the average score of the intervention group increased significantly compared to previous measurements and compared with the control group (P < .001 for the intervention group and P < .001 for the control group).
Comparison of students’ taking history skills and taking past history scores before and after intervention for 9 weeks, for 2 years, and compared with the control group.
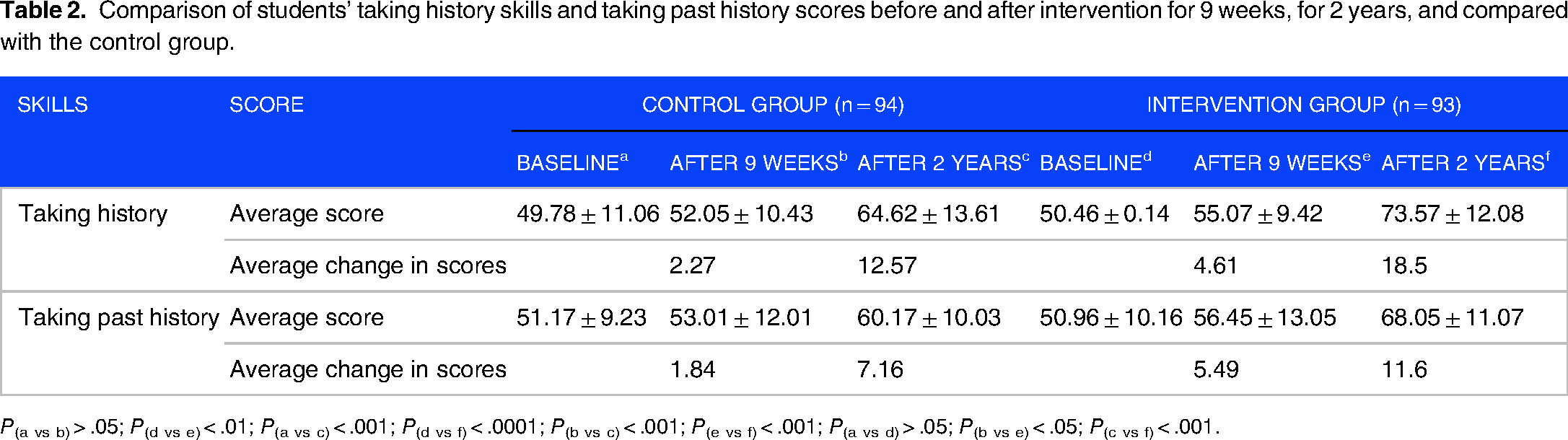
P(a vs b) > .05; P(d vs e) < .01; P(a vs c) < .001; P(d vs f) < .0001; P(b vs c) < .001; P(e vs f) < .001; P(a vs d) > .05; P(b vs e) < .05; P(c vs f) < .001.
Table 2 also demonstrates a similar pattern of results for the skill of taking a past medical history.
Table 3 demonstrates an identical pattern of difference in the skill of documentation in the medical record. There were no baseline differences between the control and intervention groups. The scores of the intervention group increased significantly at 9 weeks compared to baseline and control, and also increased at 2 years follow-up compared to previous scores and the control group.
Comparison of students’ writing medical record skill scores before and after intervention for 9 weeks, for 2 years, and in comparison with the control group.

P(a vs b) > .05; P(d vs e) < .01; P(a vs c) < .001; P(d vs f) < .001; P(b vs c) < .001; P(e vs f) < .001; P(a vs d) > .05; P(b vs e) < .05; P(c vs f) < .001.
In summary, the same pattern of comparative improvement in performance scores was observed across all 4 therapeutic areas: scores for these skills in the intervention group at 9 weeks considerably increased compared to baseline, and this trend continued at the 2-year follow-up point. Scores for these skills in the control group changed minimally at 9 weeks and modestly at the 2-year follow-up point; at both 9 weeks and 2 years, the scores for the intervention group were significantly higher than those for the control group. Nevertheless, the difference in communication and documentation skills between the 2 groups at 9 weeks and 2 years was more notable than the difference in history-taking and past history-taking skills between the 2 groups.
Discussion
Communication is the cornerstone of the relationship between the patient and the physician. Communication includes several essential domains: emotional relationship, including the establishment of trust and expression of compassion; bidirectional transmission of crucial information between patient and physician; and motivation and engagement in decision-making, behavior change, and self-care. History-taking skills are foundational for students to master more advanced and complex areas of communication, including conveying “bad news,” discussing end-of-life decisions, 9 and addressing the concerns of angry and dissatisfied patients and families.11,12,15 Students must also learn to communicate effectively with peers and members of the clinical team. Research has shown that effective communication is critical to improving patients’ health outcomes and ensuring patient satisfaction and patient safety.1,3,12,16
An important question, then, is where and how do students acquire clinical skills? The clinical environment is a rich learning environment in which students can practice clinical skills with guidance and feedback from experienced clinicians, peers, and near-peers. They learn through modeling themselves after those with greater clinical experience, and they learn through the practical application of the knowledge they have acquired through their preclinical curriculum. However, this apprenticeship model, while necessary and valuable, may not be sufficient to guarantee the acquisition of the range of skills or the level of competence expected of a year 4 student who is then prepared to move to the higher levels of clinical responsibility and independence expected in years 5 and 6.
Our study underscores several essential points. The first is that at baseline, as they enter the clinical environment of their clerkships, students at HPUMP, like students at many medical schools without a formal curriculum for clinical skills and limited clinical exposure in preclerkship years, have poorly developed clinical skills in the 4 key clinical areas studied. However, our study demonstrates that these skills can be taught and that a formal curriculum can lead to significant improvement. Thus, our study adds to a substantial body of evidence that formal training in clinical skills is possible and effective, and that there is a multitude of effective teaching strategies. For example, a review of strategies for teaching medical history identifies several effective approaches, including role-plays, interviews with real patients followed by feedback and discussion, and opportunities for videotaped reviews. 17 Niedermier 18 describes the effectiveness of a formal curriculum for medical students in documentation in an electronic medical record.
It is beyond the scope of this study to discuss the relative effectiveness of specific teaching strategies, but evidence suggests that a dedicated course and curriculum are superior to learning through informal exposure. In a study by Ahmed, 10 medical students at the University of Bahr Elghazal, Khartoum, Sudan, where clinical skills were integrated into other educational programs, without a dedicated clinical skills curriculum, clerkship students were found to lack basic communication skills. In contrast, students at Maastricht University learn communication skills through a highly structured skills lab curriculum. 13 The findings indicate strong student support for the value of a dedicated longitudinal curriculum focusing on communication and physical exam skills.
Research by Dorsch et al 19 on third-year medical students focused on an intervention to improve evidence-based medicine (EBM) skills by promoting history-taking skills. This quasi-experimental study using a pre–post-test design measured attitudes and skills in applying EBM among a sample of third-year student volunteers. The average score in 2 key EBM skills, precise clinical questioning and finding the best clinical evidence, increased from 3 to 4 on a 5-point scale, statistically significant at the P < .05 level.
Our study also suggests the potential value of a formal curriculum as a catalyst and promoter of informal learning in the clinical environment. In our study, the difference between the students who received formal and standardized training in clinical skills early in year 4 not only persisted but widened over the 2-year observation period. One can presume that students in the control and intervention groups had similar clinical exposures during their clerkship. The fact that the differences in performance persisted and widened suggests that, as educators, we cannot count on exposure and role modeling alone; students must have formal training as well as clinical exposure in order to master clinical skills. It is possible that the skills learned through the formal curriculum allowed the students in the intervention group to benefit and consolidate the skills that they learned through clinical exposure and from role models. Although both control and intervention students had multiple opportunities to learn through repeated practice, perhaps the curriculum provided students in the intervention group not only with a toolbox of concrete skills to begin with but also with a framework for deliberate, self-directed learning with which to approach their learning in the clinical environment. Communication, history taking, and documentation are discrete skills up to a point. They are also highly interdependent. Indeed, most formal models for teaching clinical skills integrate several domains. For example, both One Minute Preceptor 20 and SNAPPS 21 are effective methods for teaching communication skills. However, both also teach history-taking skills, clinical reasoning, and diagnostic skills. It is possible that through exposure to formal curricula in clinical skills, students gain practice integrating their knowledge and skills that serve as a foundation for their continued learning in the clinical environment.
The primary limitation of this research is that it was only conducted on Y4 students, the assessment was based on Pediatrics and Surgical clerkships, and the sample size was limited. Another restriction is that throughout the 2-year follow-up period, trainees may learn from their peers and supervisors and polish their abilities, which might be a confounding variable in our study. Further studies, including qualitative studies of how students apply to learn from a curriculum such as ours to learning in the clinical environment, might shed light on which specific aspects of the curriculum contribute to the sustained and widening advantage that the curriculum provides.
Recommendation
Formal training in core clinical skills should become standard for all medical students. Further studies should investigate the optimal timing for this training and identify the most effective curricula for training students in these skills. These might include earlier exposure to patients and clinical skills beginning in the preclerkship years. Novel curricular designs, including a longitudinal approach that would allow students to learn and practice clinical skills over several years in various clinical settings before they enter their clerkship years, might further enhance clinical skills and allow students to enter their clerkships well-prepared for more advanced clinical roles.
Conclusion
Our study demonstrates that students entering clerkships at HPUMP need an extra course to enhance 4 core clinical skills. Following a 9-week curriculum, evaluators rated students’ performance higher than their counterparts who learned these skills through standard informal exposure in the clinical setting. The fact that this performance advantage was maintained for 2 years following the intervention is a testament to the durability of the intervention and the value of dedicated training in these critical areas at an early point in students’ clinical careers. Formal training in 4 key clinical skills early in year 4 leads to meaningful and sustainable improvements in the performance of these skills compared to the traditional informal and nonstandardized approach.
Supplemental Material
sj-docx-1-mde-10.1177_23821205231175034 - Supplemental material for Effectiveness of a New Clinical and Communication Curriculum for Medical Students: Result of a Double-Blinded Randomized Controlled Educational Trial
Supplemental material, sj-docx-1-mde-10.1177_23821205231175034 for Effectiveness of a New Clinical and Communication Curriculum for Medical Students: Result of a Double-Blinded Randomized Controlled Educational Trial by Sang Ngoc Nguyen, Hanh Thi Pham, Lam Tung Vu and Truong Xuan Pham, Barbara Gottlieb in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205231175034 - Supplemental material for Effectiveness of a New Clinical and Communication Curriculum for Medical Students: Result of a Double-Blinded Randomized Controlled Educational Trial
Supplemental material, sj-docx-2-mde-10.1177_23821205231175034 for Effectiveness of a New Clinical and Communication Curriculum for Medical Students: Result of a Double-Blinded Randomized Controlled Educational Trial by Sang Ngoc Nguyen, Hanh Thi Pham, Lam Tung Vu and Truong Xuan Pham, Barbara Gottlieb in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-3-mde-10.1177_23821205231175034 - Supplemental material for Effectiveness of a New Clinical and Communication Curriculum for Medical Students: Result of a Double-Blinded Randomized Controlled Educational Trial
Supplemental material, sj-docx-3-mde-10.1177_23821205231175034 for Effectiveness of a New Clinical and Communication Curriculum for Medical Students: Result of a Double-Blinded Randomized Controlled Educational Trial by Sang Ngoc Nguyen, Hanh Thi Pham, Lam Tung Vu and Truong Xuan Pham, Barbara Gottlieb in Journal of Medical Education and Curricular Development
Footnotes
Abbreviations
Acknowledgements
We would like to acknowledge that a preprint of this work has been submitted at ![]() . We thank the reviewers and editors of the preprint for their valuable feedback that helped improve the manuscript. We would like to thank Haiphong University of Medicine and Pharmacy as well as everyone who participated in this study.
. We thank the reviewers and editors of the preprint for their valuable feedback that helped improve the manuscript. We would like to thank Haiphong University of Medicine and Pharmacy as well as everyone who participated in this study.
FUNDING
The authors received no financial support for the research, authorship, and/or publication of this article.
DECLARATION OF CONFLICTING INTERESTS
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contribution
Sang NN and Hanh TP, Lam TV participated in the study design, protocol development, and performance, data analysis, interpretation of data, writing the manuscript, carrying out the clinical data collection and data analysis, and observing the patient during the treatment. Truong XP and Barbara Gottlieb reviewed the manuscript. All authors read and approved the final manuscript.
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Trial Registration
Since our study was not a health-related trial and this type of study is not provided a Trial registration number in Vietnam, there is no Trial registration number for our study.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.