Abstract
Background:
While the relevance of implementation research in dentistry is increasingly emphasized, practice-based trials are still relatively uncommon in dental research. Despite being critical for successful practice-based research, little is known about the recruitment of dental professionals to participate in practice-based trials. Against this background, the purpose of this study was to extract key learnings about the opportunities and challenges for recruiting dental practices from a large-scale practice-based trial in Germany.
Methods:
Leveraging quantitative and qualitative methods, participation rates of dental practices and experiences of researchers involved in a large-scale trial in German dental practices were examined. Quantitative analyses focused on the rate of practices that initially expressed interest to participate in the trial, the rate of practices that subsequently gave informed consent to participate in the trial, and variations in participation by different modes of invitation for the study. Qualitative data from dental practices and a focus group with the research coordinators were analyzed by means of thematic analysis, focused on drivers and barriers for practices to participate in the trial.
Results:
Of 6,840 invited practices, 287 (4.2%) practices indicated their interest and 159 (2.3%) participated. The mode of invitation was significantly associated with participation (p < 0.05). The practices’ reasons for nonparticipation included shortage of staff and time to adequately integrate the study processes into practice workflows. The research coordinators also identified a lack of established practice-based research networks in dentistry.
Discussion:
While practice-based research is key to driving positive change in oral health systems, the findings of this study suggest considerable barriers for recruiting dental practices to participate in research. Understanding the mechanisms through which participation rates can be increased is crucial for the successful operationalization of practice-based research in dentistry. Implementation-oriented research in dentistry would benefit substantially from enhancements of practice-based research networks.
Trial Registration:
The underlying project was registered prospectively on July 3, 2023, at the German Clinical Trials Register (www.drks.de) under ID DRKS00030587.
Knowledge Transfer Statement:
The results of this study can be used by clinicians and clinical researchers when planning practice recruitment for practice-based trials. This could allow for more precise sample size planning and ultimately contribute to improved patient health through the increased validity of studies.
Keywords
Background
Innovative care approaches are bound to remain on a conceptional level if their actual feasibility is unknown. Here, practice-based research is a vital factor that contributes to the successful implementation of innovations in a day-to-day care setting (Westfall et al. 2007). Especially in the United States and the United Kingdom, it has a history spanning several decades back to the 1960s, with its earliest forms being traceable back to the 1800s (Mold and Peterson 2005; Green and Hickner 2006). The evolution of such implementation-oriented research in medicine is, for example, demonstrated by the call for and emergence of professional practice-based research networks (PBRNs) around the world, as they have been deemed crucial in generating evidence and ultimately initiating change in health systems (Nutting et al. 1999; Lindbloom et al. 2004; Barkham 2014; Klemenc-Ketis et al. 2015; Initiative of German Practice-Based Research Networks 2025). Studies and research networks in the ambulatory sector rely heavily on the participation of physicians’ practices, be it as study participants or as centers that recruit patients. Despite this need, previous evidence suggests low rates of practice participation in translational research around the world (Lionis et al. 2004; VanGeest et al. 2007; Herber et al. 2009; Güthlin et al. 2012; Beerheide 2020; Hennrich et al. 2021; Virnau et al. 2022), such that achieving the desired sample size can be challenging. Low sample sizes pose threats to the validity and generalizability of results (Bower et al. 2009).
However, most existing evidence on practice-based research focuses on primary care in general/family practices. Despite its importance, relatively little is known about practice-based research in dentistry. Dental research is still being performed primarily within university hospitals, not by, with or within dental practices. In addition, compared with primary care practice-based research, structures such as dental PBRNs are a relatively new development, a lot of them having been initiated only during the past 10 to 20 y, with the United Kingdom and the United States being among the forerunners (Mjor 2007). An exceptional example was the Dental Practice-Based Research Network, which included US states as well as European countries (Gilbert et al. 2008), but has since been succeeded by the purely US-centered National Practice-Based Research Network (Gilbert et al. 2013). A review from 2020 suggests that research from PBRNs and independent dental research groups is rather scarce outside of the United States and the United Kingdom, which accounted for about 71% of related publications (Canceill et al. 2021).
Meanwhile, recruiting dental practices to allow for dental practice–based research has received little international attention outside of the United States and the United Kingdom. Evidence from the United Kingdom shows that dental practices already face constant challenges when it comes to recruiting and retaining staff just to run their day-to-day business (Holloway and Chestnutt 2024a, 2024b). Participation in research demands additional time and staff, so successful practice recruitment cannot be taken for granted. It is not clear to which degree recruitment-related evidence from general practice and from the United States and United Kingdom can be simply applied to dental practices around the world. Especially regarding large-scale trials within dental practices, there is little evidence that considers country-specific contexts. Yet, positive change in dental practice depends on domestic evidence. Without identifying and overcoming barriers for practice participation, practice-based research cannot succeed. A lack of data on recruiting dental practices makes it impossible to draw conclusions regarding the planning of a study (e.g., expected dropouts and plausible sample size calculations). Ultimately, this can lead to invalid results and a waste of resources.
To this end, the purpose of the present study was to gain insight into participation of dental practices during a large-scale, practice-based, clustered randomized controlled clinical trial on integrated care for periodontitis and type 2 diabetes mellitus in Germany. Dental PBRNs are largely absent in Germany, except for some smaller local initiatives (Peikert et al. 2020; Canceill et al. 2021), and ambulatory practices are largely absent from implementation-oriented research projects. Factors that affect dental practices’ willingness to participate in research are still largely unknown in Germany. This study adds to the knowledge on study-planning approaches across countries and contexts. The setting in a large-scale cluster randomized controlled trial (RCT) on integrated care allows for an insight into a novel type of intervention at the interface of dental and general medicine.
Methods
Trial and Intervention Description
To gain insights into the opportunities and challenges for recruiting dental practices in a context where practice-based trials have vastly been absent so far, data and lived experiences from the largest dental practice-based trial that has been carried out in Germany to date, the DigIn2Perio project (Hennrich et al. 2024), were leveraged. DigIn2Perio received ethics approval from the ethics committees of the Medical Faculties of Heidelberg (vote No. S-114/2023), Bonn (vote No. 067/23-EP), Düsseldorf (vote No. 2023–2358), the ethics committees of the State Medical Association Baden-Württemberg (vote No. B-F-2023-090-z), and the Medical Association North Rhine (vote No. 2023227). All participants provided written, informed consent. DigIn2Perio includes a clinical study on the implementation of a screening for periodontitis and type 2 diabetes in the German states of Baden-Wuerttemberg and North-Rhine Westphalia (Hennrich et al. 2024). According to the a priori sample size calculation for the trial (applying α = 5% and aiming at a statistical power of 80%), 104 ambulatory dental practices were sought to recruit a total of 15 periodontitis patients each from whom they should collect information at 3 time points (T0, T1, T2) from baseline until 24 mo after. In the intervention arm, the T0 questionnaire included questions on subjective health and validated questions that allowed for the calculation of a type 2 diabetes risk score. Practices had to counsel patients with a heightened risk for type 2 diabetes and refer them to a general practitioner/family physician. The follow-up questionnaires at T1 and T2 gathered data on potential type 2 diabetes mellitus diagnoses and changes in the patients’ health over time. In the control arm, T0 to T2 included identical questionnaires, except the risk score calculation and counseling, so no further measures were taken after the surveys. Patient recruitment was planned to be performed by a dental assistant/nurse within the practice; counseling had to be performed by the dentists themselves.
Mode of Recruitment
Practice recruitment was endorsed by the state-level associations of statutory health insurance dentists. In Baden-Wuerttemberg, eligible practices were identified using the publicly available online database from the state-level association of statutory health insurance dentists. The database provided information on the practices’ medical focus, members, and contact details. Details were retrieved manually by the academic research institution, and duplicates were removed. Most practices approached were single practices owned by the dentist, which resemble the largest group among active dentists in Germany (about 61% in 2023; Bundeszahnärztekammer 2025), followed by group practices and dental ambulatory health care centers (about 34% of active dentists in Germany; Bundeszahnärztekammer 2025). Practices that focused exclusively on orthodontics or oral/maxillofacial surgery, hospitals, private practices, and/or practices that did not provide periodontal therapy were excluded. Practice owners were contacted directly if possible. In North-Rhine Westphalia, the initial process was similar until the state’s association of statutory health insurance dentists offered to identify and contact practices directly.
Practices received a personalized invitation letter with a short description of the study, the requirements for practices, and monetary incentives within the study. In Baden-Wuerttemberg, invitation letters were provided to the practices by the academic research institutions via fax or conventional mail, using their official letterheads. In addition, the state-level association of statutory health insurance dentists published the invitation letter in their electronic newsletter. In North-Rhine Westphalia, the letters were directly prepared and distributed by the state-level association of statutory health insurance dentists via conventional mail, using their official letterhead. In both settings, practices were asked to indicate their interest in participating in the study and to provide the necessary details (name of responsible person and the practices’ contact details). Alternatively, practices could indicate no interest. All practices were asked to reply via fax or (e)mail.
Practices that could not be reached were approached again using an alternative method (e.g., practices with an invalid fax number received the invitation via conventional mail). Practices that explicitly indicated no interest in the study were not approached again. Practices that did not reply to the invitation at all received a reminder via phone. Practices that indicated their interest in participation were randomized to one of the study arms, and the person who replied to the invitation received the documents necessary for participation. The control and intervention groups received similar documents; practices in the intervention group had to sign an additional care contract due to billing and funding regulations. At this stage, practices also had to name 1 dental assistant as the person responsible for conducting the study in the practice.
Practices that did not send back the documents were reminded and, if necessary, supported via phone in intervals of about 2 wk, depending on their availability. As soon as the signed documents arrived, practices were included in the study. The dental assistants received an online tutorial and the materials to carry out the study.
Quantitative Analyses
Data on the number of invitations sent, type of invitation (fax/conventional mail), number of responses to the invitation, indication of interest (yes/no), response after the study documents were received (yes/no), actual participation in the study (yes/no), and specific reasons for not being interested in participating (optional free text) were retrieved from trial documentation sources.
Descriptive (absolute and relative frequencies) and inductive statistical methods (chi-squared tests) to test associations between mode of invitation (fax/conventional mail) and study participation (yes/no) were carried out with R Studio 2024.09.01 (R Core Team 2024).
Qualitative Analyses
A focus group interview with the 5 academic research coordinators of the trial (3 dentists, 1 sociologist, 1 dental nurse; age span: 34–66 y) was carried out toward the end of the practice recruitment phase. This focused on the following aspects (topic guide):
Positive and negative experiences regarding practice recruitment
Own experiences and feedback from the team and practices
Wishes and suggestions for future research
Suggestions for improving dental practice recruitment from researchers and practices
All participants of the focus group gave their informed consent before the interview took place. The focus group was audio-recorded, transcribed verbatim, and analyzed according to the concept of a content-structuring qualitative content analysis as described by Kuckartz (2014).
Results
Quantitative Analyses
Table 1 provides an overview of the response and participation rates of dental practices. Over the course of 12 mo, a total of 6,840 practices were contacted via fax or conventional mail. In Baden-Wuerttemberg, the full number of individually identifiable practices, excluding orthodontists, that were registered with the statutory health insurance association in the state at the time of the study were approached. The overall response rate to the invitation letter was 8.5%, and the overall participation rate was 2.3% (including practices that participated initially and then dropped out of the study at a later point). Chi-square tests showed a significant association between state and participation (p < 0.05) and type of invitation and participation (p < 0.05).
Frequency of Response and Participation of Dental Practices.
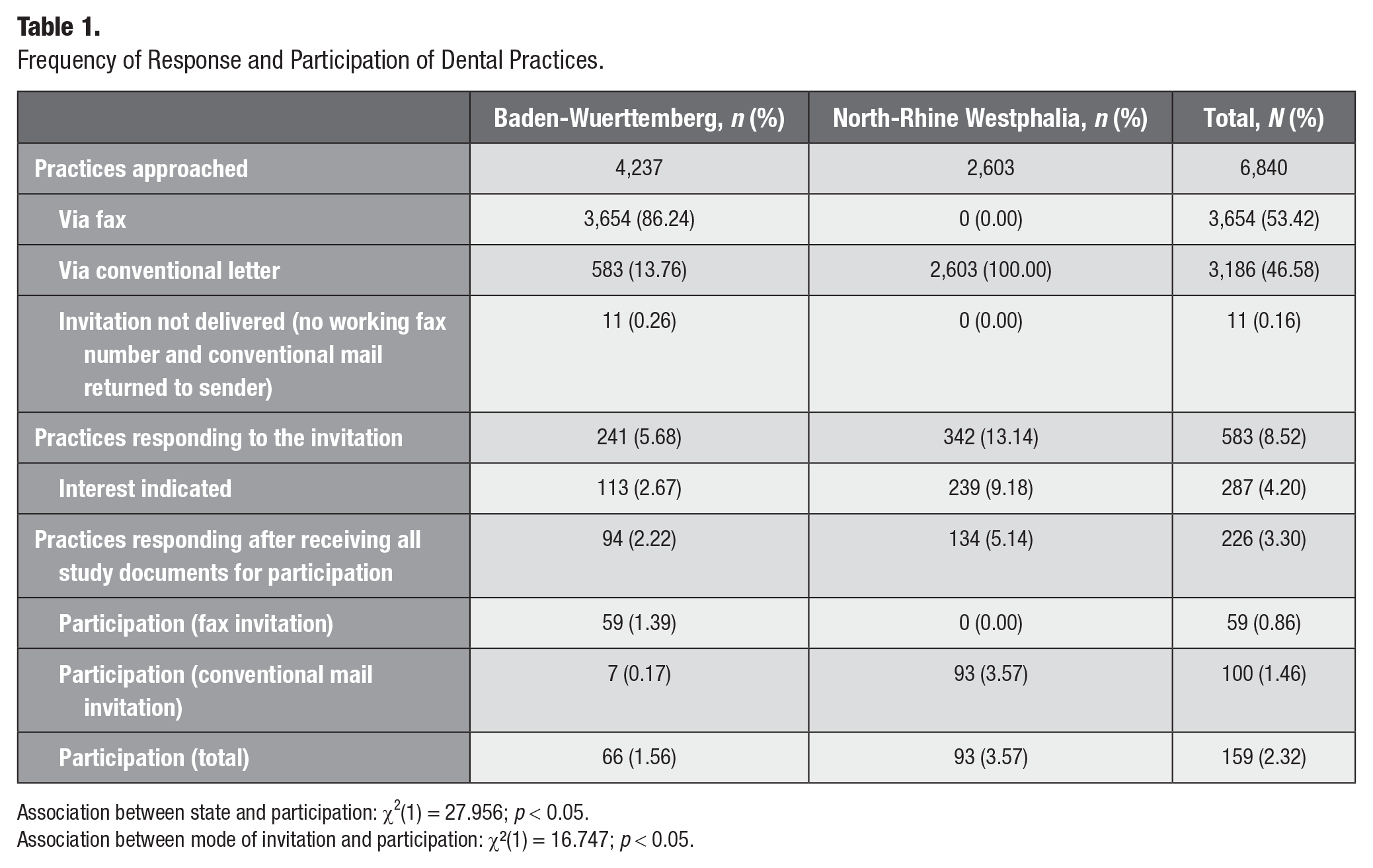
Association between state and participation: χ2(1) = 27.956; p < 0.05.
Association between mode of invitation and participation: χ²(1) = 16.747; p < 0.05.
The main reason reported by practices for not indicating interest or nonparticipation after indicating interest was shortage of staff and time to integrate the study into the practice workflow. Other reasons included health issues of practice personnel, permanent closing of the practice due to retirement, or unexpected death of the owner.
Qualitative Analyses
All 5 research coordinators who were invited took part in the focus group interview. Thematic analysis yielded the following topics regarding recruitment experiences of the research coordinators:
Varying commitment of practices to participate in the study after indicating interest
Staff-related aspects that affected practice participation
Formal requirements that affected practice participation
Lack of previous research experience of practices
Lack of structures enabling research in dental practices
Varying extent of recruitment support from cooperating partners
With regard to suggestions for future research, the main topic was that additional/earlier support from cooperating partners would be desirable.
The participating researchers reported that recruitment was initially expected to be very successful, with a high number of practices indicating interest in the project already at the planning stage after it was publicly announced and even before the invitation letters were sent out:
So, I had the impression that response was very positive there. We received a lot of responses relatively fast. Response to an inquiry that required little commitment seemed to be rather positive back then. (Speaker 5)
When it came to the initial indication of interest as a response to the invitation letter, the overall impression was also perceived as positive, until practices were asked to actually enlist for the study:
In general, when it comes to indicating interest, response was quite alright. Even though we had to contact over 6,500 practices, we received an indication of interest from a solid number of practices that would have sufficed to reach the planned sample sizes. . . . It became critical only after it started to be about commitment to participation. (Speaker 4)
A crucial inhibiting factor reported to the researchers was the shortages of staff in dental practices:
I believe the biggest aspect here really was staff related. So, there were many, many responses like, “We won’t be able to do it anymore, I don’t work there anymore.” Recently, I had a large practice that closed their business. So, here this is, I think, the main aspect. (Speaker 3) Currently, and this has been going on for several years, there is an extreme shortage of dental assistants in all of Germany and practices hunt for each other’s assistants. A lot of them have far too few, and there are a lot of sick leaves, and thus you must understand that some practices don’t want to burden themselves additionally by participating in such a study. (Speaker 1)
An additional inhibiting factor that was reported by the researchers were the legally necessary documents needed for the recruitment of practices, especially the care contract in the intervention group:
So, that’s just a challenge that is caused by the funding mechanism and the inclusion of a health insurer and the respective contracts. You can’t leave it at the background information of 8 to 9 pages, but you need to include a large contract. That was too unsafe for some practices, I’d say—also because of their lack of project experience, so they don’t know that such a contract can be a standard procedure without any critical results. . . . So, there might have been some prejudices we weren’t able to clarify—it was more like, “Yes, I believe you, but I still won’t participate.” (Speaker 4)
However, this differed between states:
We can agree, besides the fact that we didn’t have this issue between control and intervention group. Here, it was more or less equal and there was virtually no practice that, after they received the documents and decided to participate, didn’t sign the contract. That wasn’t a problem. (Speaker 2)
Another aspect noted as an important inhibiting factor was the lack of formalized dental practice networks contrary to, for example, general practices and a lack of study nurses with a focus on dentistry at the research institutions themselves:
Maybe one must also note that there are not only no practice networks in dentistry yet, but also no study nurses who are familiar with this field in a professional way. . . . Basically, this was learning by doing, right? (Speaker 1)
When it comes to suggestions for future research, the researchers primarily stated that more support from the cooperating associations from the get-go could be helpful to enhance efficiency of recruitment:
From my perspective, I wished for kind of a complete overview from the [dental association]. So, what they didn’t hand out due to data protection reasons. A complete list of practices, so that we’re able to contact them. (Speaker 3) I mean, we manually searched for practices . . . in the publicly available databases. . . . That’s a huge effort that bound several people over weeks and months to search for over 4,000 practices in our state and remove duplicates manually. It would have saved lots of time if we had access to lists. . . . Of course, we wished for more support from the [association], I clearly have to say that. . . . Holding back contact information for data protection reasons is probably necessary due to legal reasons—at the same time, this is the same information that is publicly available in their online databases. (Speaker 4)
Discussion
The findings of this study showed that of 6,840 practices that were invited for a large-scale trial in Germany, 8.5% expressed an interest to participate and 2.3% eventually participated in the trial. The state and mode of invitation were significantly associated with the participation rate, with invitations by conventional mail yielding higher success than invitations by fax did. The practices’ reported reasons for nonparticipation included shortage of staff and time to adequately integrate the study processes into practice workflows. In addition, the research coordinators also identified a shortage of established PBRNs in dentistry as a reason for the low response and low participation rates.
While there are extensive data on trial recruitment and participation rates among general practitioners, knowledge on this topic regarding German dental practices is scarce. The present study used recruitment techniques that have been studied previously (Bower et al. 2009; Pit et al. 2014; So et al. 2018; Beerheide 2020; Hennrich et al. 2021), such as monetary incentives, addressing a specific person in the practice, personal contact via phone, and reminders. Still, the overall practice participation rate might be considered very low. However, similar participation rates have also been found in general practices, with rates not exceeding 5% despite extensive recruitment effort (Herber et al. 2009; Güthlin et al. 2012; Hennrich et al. 2021).
The quantitative analyses suggest an association between state as well as mode of invitation and participation, with conventional letters yielding better results than the still widespread fax. The latter might be an explanation for the association between state and participation, since invitations in the state of Baden-Wurttemberg were mainly distributed by fax and those in North-Rhine Westphalia were exclusively distributed by conventional mail. Still, the mode of invitation might not be the only aspect that affected the participation of practices on a state level: contrary to Baden-Wuerttemberg, invitation letters in North-Rhine Westphalia were sent out by the state’s association of statutory health insurance dentists instead of the research institution. Since the letters included the official letterhead of the association and were signed by them, this might have signaled a very strong endorsement by their own profession to receiving dentists, sparking further interest in the study and commitment to participation.
The main inhibiting factor to participation named by practices and perceived by researchers were staff shortages within dental practices and a resulting increase in workload that prevented practices from taking part in the study. These aspects also mirror those known from general practices. In addition, the present study demanded a rather long-term commitment over the course of 3 y. Even though they were allowed to quit the study at any point in time without any repercussions, it can be assumed that practices seriously interested in the study considered the duration and thus might have refrained from participation due to uncertainty about being able to carry out the study until the end. From general practice, it is known that there seems to be a clear difference between recruiting practices as independent centers with own responsibilities (such as was the case regarding patient recruitment and implementation of an intervention in the present study) and recruitment of practices solely as participants (e.g., in surveys). The latter tends to yield higher response rates when proper recruitment strategies are applied (Parkinson et al. 2015; Groenewegen et al. 2016; Virnau et al. 2022). It seems reasonable to assume that the difference in the burden that these varying types of roles impose on clinicians can also be relevant for recruitment success in the dental field, especially when practices suffer from staff shortage.
Besides the factors discussed above, low participation might also have been enhanced by the fact that dental practices in Germany still do not possess extensive research experience, lack institutionalized research networks, and thus require regular support during the research and recruitment process. Dental PBRNs are especially prevalent and active in the United States (Canceill et al. 2021). Still, despite being rather well-established, they also face regular challenges when it comes to recruiting and educating additional practices on research projects and the subsequent implementation of interventions (Gordan et al. 2019). While practices in the present study were approached proactively to answer possible questions and were supported during the onboarding process, the capacities of the respective research institutions might not have been able to fully cover the need for support, making practices refrain from participation. These capacities were further impeded by the need to manually retrieve practice contact data: the retrieval required parts of the institutions’ staff to dedicate significant amounts of time to search within public dentist databases and structure the necessary information, using up resources that otherwise could have been invested to further intensify contact with and support for dental practices.
Finally, it is important to consider the degree to which practitioners deemed this particular study important to themselves and/or their patients. In case they might have seen little added value, it is reasonable to assume that they refrained from participation. However, this was neither hinted at in the statements received from practices nor in the focus group data gathered from the research coordinators. To tackle inhibiting factors such as this, incentives are key. The invitation letters covered monetary incentives and described the overall benefits of the underlying project regarding the integration of dentistry and general practice. In addition, nonmonetary benefits might offer a chance to further increase interest in participation. In particular, occupation-related incentives such as continuing medical education points could be an additional option to explore in future endeavors.
The present study is not without limitations. Due to the specific nature of the underlying practice-based trial (cluster RCT with a focus on screening for diabetes among periodontitis patients), the findings might not be generalizable to other practice-based studies with different designs. It is possible that, for example, recruitment success will be higher in studies that include less effort for practices. However, this study can serve as an example outlining barriers and facilitators regarding recruitment for large-scale trials. While fax and conventional letters were the preferred mode of distributing invitations in the examined trial (drawing from previous experience in primary care in Germany), other modes such as email might yield different response/recruitment rates. In this case, however, there is a chance that the invitation might be overlooked due to the generally large amount of emails that practices receive. Nevertheless, the findings of the present study are highly novel and relevant. Realistic expectations about the rates and motives for dental practices to participate in dental research are pivotal for successful planning and conduct of practice-based research in dentistry. In the absence of such knowledge, the additional time and costs required to achieve the desired sample size can be substantial and jeopardize the return on investment in practice-based research. Hence, the findings reported here have important bearings for the conduct of practice-based studies in dentistry.
Conclusion
Practice-based research is key to drive positive change in oral health systems. The findings of this study suggest considerable barriers for recruiting dental practices to participate in research. Understanding the mechanisms through which participation rates can be increased is key for successful operationalization of practice-based research in dentistry. The relatively low participation rate observed and the experiences of practices and researchers show that recruitment requires significant resources as well as comprehensive support. Limited human resource capacity and lack of research experience in dental practices impedes study participation. Research projects that rely on the participation of dental practices should not only plan to dedicate a significant amount of time and monetary incentives to recruitment but also ensure sustained capacities for dedicated support throughout the recruitment phase. Health services research in dentistry would benefit substantially from enhancements of PBRNs. Practice-based trials offer vast potential for oral health improvement.
Author Contributions
P. Hennrich, contributed to conception, design, data acquisition, analysis, and interpretation, drafted and critically revised the manuscript; V. Fehrer, contributed to design, data acquisition, analysis, and interpretation, critically revised the manuscript; A.L. Müller, J. Daniels-Stumpf, S. Jepsen, contributed to data acquisition and interpretation, critically revised the manuscript; S. Listl, contributed to conception, design, data acquisition, analysis, and interpretation, critically revised the manuscript. All authors gave final approval and agree to be accountable for all aspects of the work.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The DigIn2Perio project is funded by a grant from the Innovation Fund at the German Federal Joint Committee (“Innovationsfonds beim Gemeinsamen Bundesausschuss”). Funding No. 01NVF21115. The funder had no specific role in the conceptualization, design, data collection, analysis, decision to publish, or preparation of the article.
