Abstract
Introduction:
Implicit bias is a form of unconscious bias that can affect judgment, decisions, and behaviors.
Objectives:
This scoping review examined what scientific literature exists about implicit bias demonstrated by dental/dental hygiene students and providers and, when possible, how these implicit biases are associated with patients’ oral health outcomes.
Methods:
This scoping review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR). This review included English-language PubMed peer-reviewed studies meeting inclusion criteria, published through October 2023, measuring the implicit bias of dental/dental hygiene students or professionals and how such bias can affect patient oral health outcomes.
Results:
A total of 363 records were found. After removing duplicates (n = 114) and title screening (n = 60), 54 abstracts were screened, 24 reports were assessed, and 10 were included in the final review. Implicit bias was assessed using the Implicit Association Test (IAT), Brief IAT (BIAT), and Color-Blind Racial Attitudes Scale (CoBRAS). BIAT scores revealed a pro-White unconscious racial bias in clinical decision-making among dental professionals, and additional IAT results suggested implicit racial preferences for European Americans over African Americans; non-White participants showed more positive implicit preferences toward African Americans in comparison with White participants. Studies using CoBRAS suggest moderate levels of color-blind racial attitudes among students and professionals, indicating an unawareness of racism and a need to further understand the implications of bias on patient outcomes.
Conclusion:
Despite small sample sizes and a lack of racial/ethnic diversity that limit their generalizability, the included studies provide evidence for implicit racial bias held by some dental/dental hygiene students and professionals that may affect the oral health outcomes of patients. Training to increase awareness of and reduce implicit bias among those providing oral health care is an important first step to providing a more equitable health care system for all patients.
Knowledge Transfer Statement:
Despite small sample sizes and a lack of racial/ethnic diversity that limit their generalizability, the included studies provide evidence for implicit racial bias held by some dental/dental hygiene students and professionals that may affect the oral health outcomes of patients. Training to increase awareness of and reduce implicit bias among those providing oral health care is an important first step to providing a more equitable health care system for all patients.
Keywords
Introduction
Bias, as defined by the National Institutes of Health, consists of the attitudes, behaviors, and actions that hold favor toward or against an individual or group compared with another (National Institutes of Health 2021). More specifically, implicit bias is a form of unintentional and automatic bias that affects judgment, decisions, and behaviors that is often driven by subconscious thoughts (Shah and Bohlen 2023). This means individuals are unaware of their implicit beliefs and attitudes, complicating their understanding and ownership of these implicit thoughts.
Implicit bias can be harmful when certain social identities (e.g., race, gender, socioeconomic position) are associated with negative characteristics, adversely affecting others’ behavior toward individuals with these social identities. Implicit bias is especially harmful in the health care setting—contributing to disparities in health and health care. This bias can perpetuate a lack of diversity in the workforce and contribute to inequitable distributions of research and funding (Sabin 2022). Bias may manifest in a health professional’s attitudes and behaviors in response to a patient’s race, ethnicity, weight, disability, sexual orientation, gender, or age, among other variables. Explicit bias differs from implicit bias, as the former relates to thoughts openly expressed and formed with consciousness and awareness (Patel et al. 2019). Because a person’s implicit bias often occurs outside their conscious awareness, it is typically not measured using methods that rely on a person’s explicit self-reports, such as surveys.
One of the most common measures of implicit bias is the Implicit Association Test (IAT), which measures response times when an individual is asked to match 2 concepts that they implicitly feel are either highly associated or less associated with one another (Greenwald et al., 1998). As an example, a person may explicitly disavow holding negative impressions of Black individuals but may take longer to respond to matching positive words to “Black” while taking less time to match negative terms to “Black,” suggesting negative implicit biases toward Black individuals that the person may not be aware of (Goedderz and Hahn, 2022). Both the explicit and implicit biases held by health care providers can exacerbate and contribute to health disparities that predominately affect historically marginalized communities.
According to a National Academy of Medicine report, individuals from racially and ethnically minoritized backgrounds receive lower-quality health care in comparison with White individuals, even in the case of comparable insurance status, income, age, and severity of conditions (Bridges 2018). In comparison with White individuals, historically marginalized individuals are less likely to receive adequate cardiac care (Cavender et al. 2013), kidney dialysis (Boulware and Mohottige 2021), or kidney transplants (Wesselman et al. 2021). Individuals from racially and ethnically minoritized backgrounds also have a lower likelihood of receiving equitable treatment for stroke, cancer, or AIDS (Bridges 2018). In addition, non-White patients receive fewer cardiovascular interventions and renal transplants and are less likely to receive pain medication prescriptions, Black women have a greater likelihood of dying after breast cancer diagnosis, and Black men are less likely to receive chemotherapy and radiation therapy for prostate cancer and more likely to have testicles removed (Joint Commission Division of Health Care Improvement 2016).
Implicit bias can be learned from cultural exposure to negative commentary and stereotyping and internalized over time (Sabin 2022). A study by Van Ryn and colleagues (2015) demonstrated that nearly 50% of medical students in the United States have been exposed to negative comments regarding Black patients from attending or resident physicians. In this study, the same cohort of medical students later demonstrated significantly more implicit racial bias in their fourth year in comparison with their first year of medical education (Van Ryn et al. 2015). This highlights the importance of education around implicit bias and the recognition and mitigation of this bias in medical training.
As implicit bias persists toward marginalized communities and significant disparities exist in health outcomes, it is essential to address bias among all health care providers. Implicit bias in the medical setting has been extensively researched; however, a significant gap exists regarding implicit bias in oral health care settings. Because of the lack of literature on dental/dental hygiene students’ and professionals’ implicit biases, a scoping review was undertaken to assess the current state of the literature. A scoping review maps evidence on a specific topic and identifies the main takeaways, theories, sources, and knowledge gaps (Tricco et al. 2018). The goal of this scoping review is to examine what scientific literature exists about implicit bias demonstrated by dental/dental hygiene students and providers and, when possible, how these implicit biases are associated with patients’ oral health outcomes.
Methods
This scoping review adhered to the recommendations of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) (Tricco et al. 2018).
Eligibility Criteria
Peer-reviewed studies following any study design were deemed eligible for inclusion in this review if they:
measured the implicit bias expressed by dental/dental hygiene students and professionals or
measured how such implicit bias can affect patient oral health outcomes.
Studies were excluded from consideration if they
did not focus on implicit bias in the oral health profession but only in the general medical or health care setting or
examined only explicit bias without addressing implicit bias.
While it is important to acknowledge the impact of implicit bias experienced by dental/dental hygiene students and professionals, this review aimed to focus on patient oral health outcomes. In addition, a wide variety of implicit biases exists (Shah and Bohlen 2023). No specific marginalized groups were therefore included in the search strategy. Similarly, we did not include any specific study types or measures of implicit bias in the search strategy to conduct as comprehensive a search as possible (Table 1).
Terms Used to Search PubMed for Articles Meeting Inclusion and Exclusion Criteria.
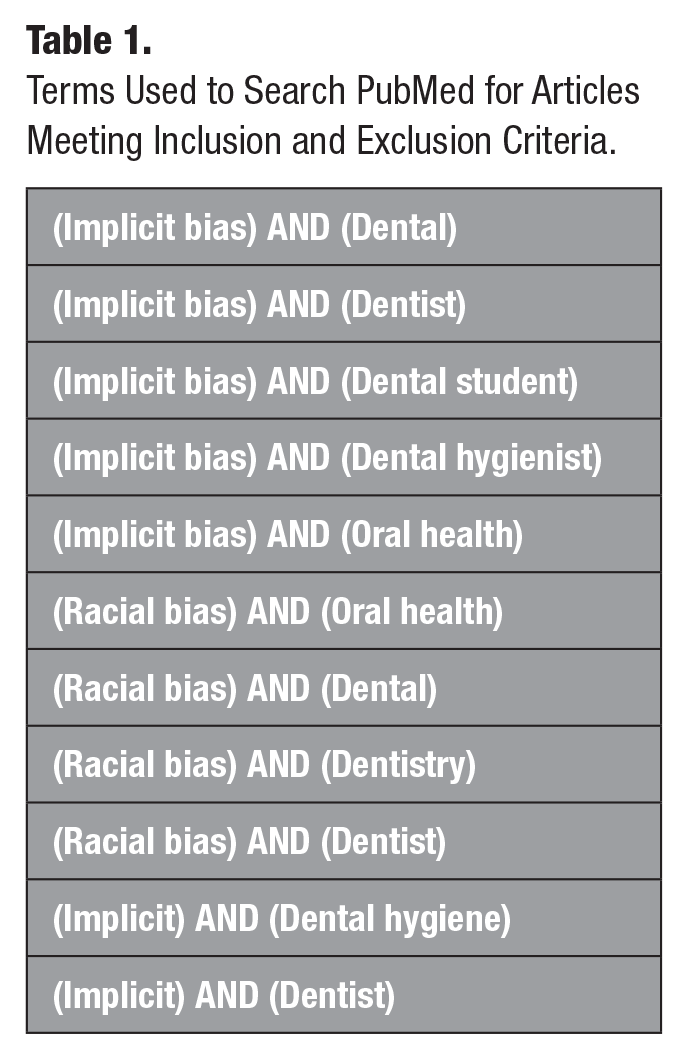

The primary author (P.M.) conducted the initial search and identified the first set of records (N = 363). Please see Table 1 for the keywords used to search for articles meeting the inclusion and exclusion criteria. After removing duplicate records (n = 114), the primary author screened the remaining abstracts for inclusion/exclusion criteria and reviewed the remaining full-text papers for eligibility, extracting data regarding the subject of the study (dental/dental hygiene students and/or providers), the measure(s) of implicit bias used, and, when applicable, the association with patients’ oral health outcomes. The senior author (L.J.H.) concurrently and independently reviewed 20 of the manuscripts for the data listed above. The primary and senior authors then discussed their independent conclusions regarding the relevance of each article. Although not needed, if there had been disagreement between the 2 authors, a third author would have been included to resolve any discrepancies.
English-language studies indexed in PubMed that met inclusion criteria and were published through October 2023 were included in our search. A total of 363 records were identified, and 114 duplicate records were removed before screening (Figure). After title screening, 54 abstracts were screened, and 30 were excluded for not adhering to inclusion criteria. Subsequently, 24 reports were assessed for eligibility. Fourteen of these reports were deemed ineligible according to our exclusion criteria, and 10 studies were included in our final review per the inclusion criteria.

PRISMA flow chart describing the inclusion and exclusion of reviewed studies.
Results
Summary of Included Studies
One of the 10 studies examined implicit biases of dental students (Su and Behar-Horenstein 2017), 3 involved dental hygiene students (Ludwig et al., 2019; Ludwig and Suedbeck 2023a, 2023b), 1 assessed dental hygiene faculty members (Cahoon et al. 2023), and 1 involved dental school faculty members (Su and Behar-Horenstein 2017). Two of the 9 included studies assessed the implicit biases of dentists in practice (Patel et al. 2019; Plessas 2019), and 2 involved practicing dental hygienists (Ludwig et al. 2022; Morzenti et al 2023). Two papers described research done in Italy (Patel et al. 2019; Plessas 2019); the remaining studies were conducted in the United States.
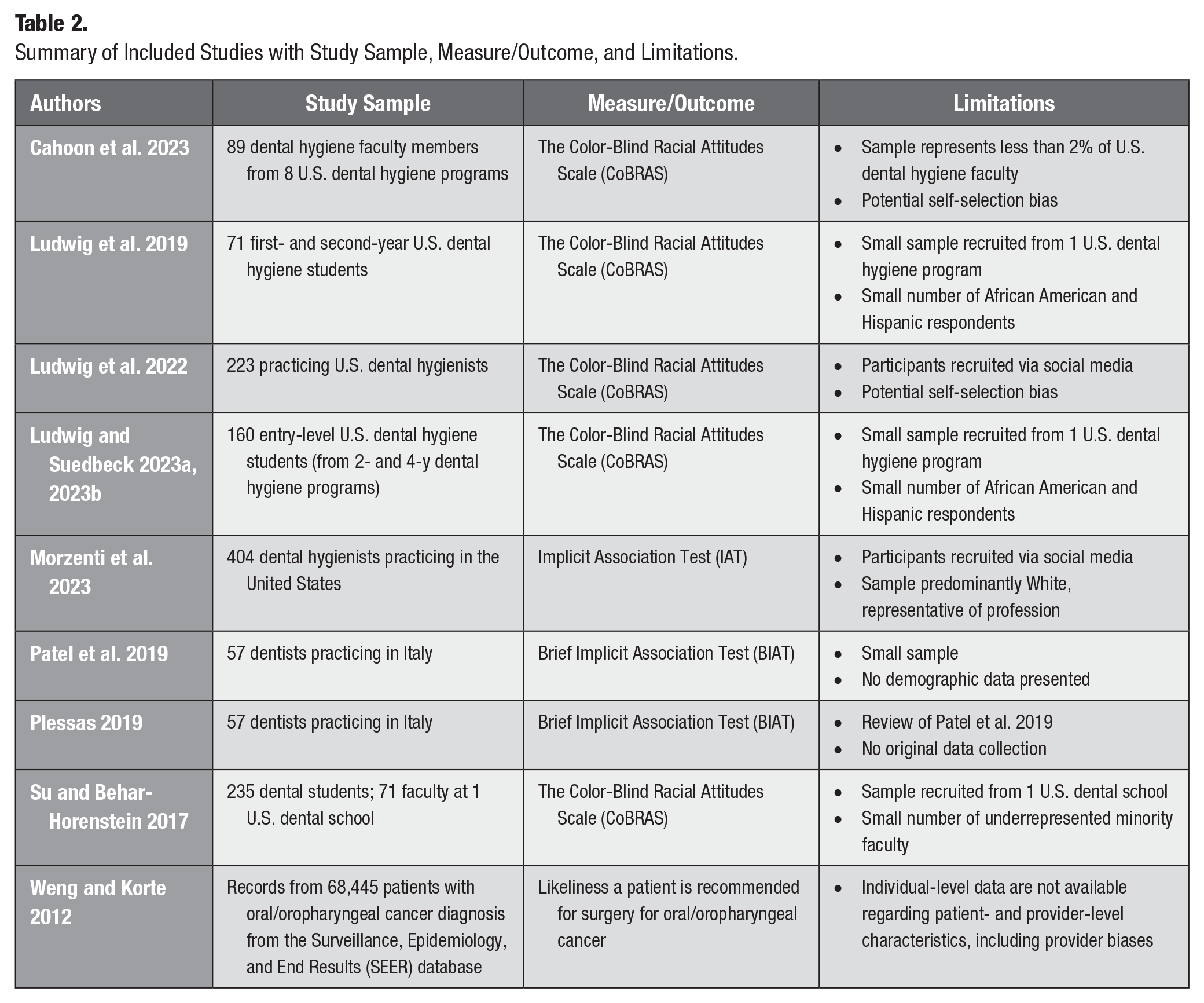
All but 1 study used survey methodology to collect cross-sectional observational data; 1 exception was a secondary data analysis conducted using the Surveillance, Epidemiology, and End Results (SEER) database (Weng and Korte 2011). Three studies included measures of patient oral health outcomes, whether actual (recommendations for surgery for oral/oropharyngeal cancer; Weng and Korte 2011) or hypothetical, such as a clinical vignette (Patel et al. 2019; Plessas 2019). Three studies (Patel et al. 2019; Plessas 2019; Morzenti et al. 2023) used either the IAT (Greenwald et al. 2009) or the Brief IAT (BIAT; Sriram and Greenwald 2009). Six studies used the Color-Blind Racial Attitudes Scale (CoBRAS; Neville et al. 2000a; 2000b; Su and Behar-Horenstein 2017; Ludwig et al. 2019; Ludwig et al. 2022; Cahoon et al. 2023; Ludwig and Suedbeck 2023a, 2023b). Each of the 10 studies is described in detail below and in Table 2, based on the measure used to assess respondents’ implicit biases.
Summary of Included Studies with Study Sample, Measure/Outcome, and Limitations.
IAT/BIAT
The existing literature related to the implicit bias of oral health professionals focused primarily on bias toward racially and ethnically minoritized groups, rather than other marginalized groups. One study used the IAT (Morzenti et al. 2023) and 2 used the BIAT (Patel et al. 2019; Plessas 2019). The IAT has good reliability and incremental predictive validity and is recommended for researchers who wish to study automatic judgment (Greenwald et al. 2009). The BIAT includes the same 4 categories and stimulus-response mappings as used in the IAT, however with only one-third the number of trials as the IAT (Sriram and Greenwald 2009). The BIAT has high test-retest reliability (r = 0.8) and internal consistency (α = 0.8; Slabbinck et al. 2018).
Morzenti and colleagues (2023) used the IAT to examine implicit racial bias among 404 dental hygienists practicing in the United States. More than two-thirds (n = 274; 67.8%) of participants showed a preference for (White) European Americans over (Black) African Americans. Specifically, IAT d-scores increased with age, suggesting greater levels of implicit bias among older hygienists. Individuals with less than 5 y of work experience scored slightly lower on the IAT compared with those with 21 or more years of experience, demonstrating slightly lower levels of implicit racial preferences toward European Americans among those with less working experience. In addition, non-White participants indicated higher positive implicit preferences for African Americans in comparison with White participants, suggesting that more negative implicit biases exist toward racial and ethnic identities different from one’s own. While the survey used for this study was targeted to all practicing dental hygienists in the United States, data for only 404 respondents were included in the data analysis, representing less than 1% of the dental hygiene workforce (Data USA 2023). Respondents were recruited via social media invitations through national dental hygiene groups, meaning that hygienists without regular access to social media may not have been invited to participate. Although the study sample was predominantly White (80%), this is representative of the U.S. dental hygiene profession in general (Data USA 2023). Results from this study call attention to the importance of creating earlier awareness of implicit biases for active prevention.
Patel and colleagues (2019) used the BIAT in a randomized clinical trial based in Italy to assess whether patients’ race affects dentists’ clinical decision-making. Dentists read a clinical vignette representing a diagnosis of irreversible pulpitis in which endodontic treatment (root canal) was a viable treatment option. The same clinical presentation was used for the entire study; however, half of the participants received a case describing a Black patient and the other half a case description of a White patient. To ensure the 2 fictional patients looked as similar as possible, the 2 images of the patient were created from the same individual. However, one image was generated as a White woman and the other as a Black woman.
A total of 57 dentists participated in the study, with 28 assigned to the Black patient case and 29 to the White patient case. Two BIATs were used to measure implicit bias: a race preference BIAT and a race dental cooperativeness BIAT (created for study). The race preference BIAT measured participants’ implicit association of race with likable and unlikeable terms, such as “wonderful” and “awful.” The race dental cooperativeness BIAT measured implicit associations between Black and White individuals using cooperative and uncooperative statements related to dental treatment such as “irregular attender” or “easily anesthetized.” The authors note that a high race cooperation score “indicates a more pro-White bias whereas a lower (negative score) indicates a pro-black bias” (online Appendix; Morzenti et al. 2023). As previously described, the BIAT measures the strength of automatic associations based on average reaction times.
The results from Patel et al. (2019) showed a near-equal diagnosis of irreversible pulpitis, regardless of whether the patient was Black (71%) or White (72.4%). However, the recommendation of a root canal was stronger for the White patient (86%) compared with the Black patient (61%). Responses indicated a bias toward extraction for the Black patient in comparison with the White patient, with 90% of study participants responding they would “definitely” or “probably” not recommend extraction for the White patient, compared with 50% for the Black patient. Overall, participants indicated a pro-White bias, with 91% of clinician participants indicating high race preference scores and 79% indicating high race dental cooperation scores. In turn, participants with high race preference scores and high race cooperation scores were significantly more likely to strongly recommend extraction for the Black patient. The Patel et al. (2019) study was conducted with a very small group of dentists (n = 57), so the generalizability of the findings is limited. There were no data presented on the racial or ethnic background of the dentists who participated. The authors stated they used the BIAT because pilot study participants’ attention flagged during longer IAT sessions. The Plessas (2019) study commented on the original Patel study and did not include original data collection of its own. The authors concluded that dentists’ decision-making was affected by the patient’s race (Patel et al. 2019; Plessas 2019).
CoBRAS
The concept of color-blind racial attitudes refers to the unawareness of racial dynamics, such as the belief that racism does not exist, as well as the unawareness of White privilege and institutional discrimination (Chao 2006). This concept has become popular in scholarly discourse, as cited in several nonconstitutional law books and an American Psychologist Association pamphlet (Neville et al. 2000b). The CoBRAS (Neville et al. 2000a, 2000b) is a 20-item measurement tool used to measure a study participant’s lack of awareness or denial of racism and racial dynamics. The scale includes 3 subscales: unawareness of racial privilege (7 items), unawareness of institutional racism (7 items), and unawareness of blatant racial issues (6 items). Total scale scores range from 20 to 120, and subscale scores range from 7 to 42; higher scores indicate participants’ higher level of unawareness or denial of racism. The CoBRAS has a high level of internal reliability (Cronbach’s alpha = 0.86) and also shows good concurrent validity with 2 measures of racial prejudice, namely, the Quick Discrimination Index and the Modern Racism Scale (Neville et al. 2000a, 2000b).
Ludwig et al. (2019) conducted a pilot study using CoBRAS to determine the color-blind racial attitudes of 71 first- and second-year dental hygiene students. There were no statistically significant differences in overall CoBRAS scores by age, race, gender, or year in the program. White and Asian students showed moderate levels of overall unawareness or denial of racism, whereas African American and Hispanic students showed low levels of overall unawareness or denial of racism. White and Asian students had the highest scores on all 3 subscales compared with African American and Hispanic students; however, the generalizability of these findings is limited, given the small number of participants within these subgroups. In addition, this study included a small sample consisting primarily of women aged 18 to 29 y recruited from only 1 dental hygiene program in 1 state (Virginia, USA), so the generalizability of the findings to all dental hygiene students is also limited.
Ludwig et al. (2019) conducted a subsequent cross-sectional study to measure CoBRAS overall and subscale scores among 160 entry-level dental hygiene students (Ludwig and Suedbeck 2023a, 2023b). The responses of dental hygiene students reflected moderate levels of unawareness of racism, White privilege, institutional discrimination, and more overt acts of racism. Second-year students and those in a 4-y bachelor’s (B.S.) program had lower overall CoBRAS scores than first-year students and those in a 2-year associate’s (A.S.) degree program did. White and A.S. students were more aware of the implications of White racial privilege, whereas B.S. students were more aware of institutional types of racism or racial inequities. This study expanded its recruitment to all dental hygiene students in the state of Virginia and included a sample size that is approximately twice that of the earlier study (Ludwig et al. 2019). That said, this study included the same limitations as the earlier study of a small overall sample size and lack of diversity regarding age, race, and ethnicity; thus, conclusions drawn about implicit biases of dental hygiene students should be made with caution.
Ludwig et al. (2022) surveyed a convenience sample of 223 clinical dental hygienists. Participants’ responses reflected overall moderate levels of unawareness of racism. Younger hygienists and hygienists identifying as African American scored significantly lower on the CoBRAS than did older hygienists and hygienists identifying their race as “other.” Younger participants were more aware of institutional racism compared with older participants. Participants were generally aware of White racial privilege and more overt, pervasive racism. Dental hygienists were recruited to participate in this study through a social media–based snowball approach similar to that of Morzenti et al. (2023), which limits the representation of dental hygienists who do not use social media or do so only sporadically. Also, the researchers invited participants to take part in a study on color-blind attitudes, which may have limited the recruitment to individuals who were already knowledgeable and comfortable with this concept (and potentially less likely to express color-blind attitudes).
Su and Behar-Horenstein (2017) assessed CoBRAS scores among 235 students and 71 faculty at 1 U.S. dental school. Female and underrepresented minority (URM) students demonstrated greater sensitivity to racism in comparison with male and majority students. Non-URM faculty were more aware of racial privilege than non-URM students were, and URM faculty were less aware of institutional discrimination than URM students were. This study benefitted from a greater than 90% response rate from both dental students and faculty members yet represents findings from only 1 U.S. dental school at 1 point in time. Comparisons including URM faculty should be made with caution due to the small number of URM faculty in that 1 school.
Cahoon and colleagues (2023) sent the CoBRAS survey to faculty from 8 U.S. hygiene programs. Responses indicated moderate levels of color-blind racial attitudes and, specifically, moderate levels of unawareness of racial privilege and institutional discrimination. Generally, dental hygiene faculty (n = 89) were aware of and able to identify the existence of blatant racism within society. This study expands the recruitment of dental hygiene faculty to a nationwide approach, yet the sample providing complete data comprises less than 2% of the 4,840 dental hygiene faculty members teaching in the United States at the time the study was conducted (American Dental Association 2022). The researchers also noted that individuals who were more aware of and comfortable discussing and answering questions about racism and racial privilege may have been more likely to participate in this study.
Implicit Racial Bias in Oral/Oropharyngeal Cancer
Weng and Korte (2012) aimed to assess the impact of race on the likeliness a patient was recommended for surgery, the first line of treatment, after an oral and oropharyngeal cancer diagnosis, using SEER data (n = 68,445). The odds of not being recommended surgery were twice as high for Black patients as for White patients, irrespective of patients’ cancer stage and socioeconomic status. Racial disparities in surgery recommendation varied by age, geography, and tumor subsite. This study benefitted from a large sample of nearly 70,000 individuals from a population-based study. As with many cross-sectional, big-data studies of its kind, individual-level data were not available regarding factors such as patient socioeconomic status (e.g., income, insurance status) or provider-level biases, which makes drawing causal conclusions about reasons for surgical recommendations impossible.
Discussion
This is the first scoping review to examine the scientific literature related to implicit bias held by dental students, dental hygiene students, faculty, and dental professionals. This scoping review shows there is a dearth of large-scale studies examining implicit biases expressed by these students and professionals, particularly showing associations with patients’ oral health outcomes. The 3 studies examining patient-related outcomes (Weng and Korte 2012; Patel et al. 2019; Plessas 2019) demonstrated significant differences in treatment recommendations by patient race for oral cancer and irreversible pulpitis. Studies of dentists (Patel et al. 2019; Plessas 2019), dental hygienists (Morzenti et al 2023; Ludwig et al. 2022), dental hygiene and dental educators (Su and Behar-Horenstein 2017; Cahoon et al. 2023), dental students (Su and Behar-Horenstein 2017), and dental hygiene students (Ludwig et al., 2019; Ludwig and Suedbeck 2023a, 2023b) all demonstrated a tendency to assign more positive attitudes toward White individuals than non-White individuals, although there was variability seen by respondent age, race/ethnicity, education levels, and years in practice. It is critical to understand the extent of implicit bias among dental students and professionals, as bias can affect clinical decision-making and patient oral health outcomes, which may perpetuate oral health inequities among marginalized populations (Weng and Korte 2012; Su and Behar-Horenstein 2017; Patel et al. 2019; Ludwig et al. 2019; Ludwig et al. 2022; Morzenti et al. 2023; Cahoon et al. 2023; Ludwig and Suedbeck 2023a, 2023b).
The examined studies suggest negative bias to be more prominent for individuals from racial and ethnic identities different from one’s own (Morzenti et al. 2023). This calls attention to the impact of intergroup bias or “the systematic tendency to evaluate one’s own membership group (the in-group) or its members more favorably than a nonmembership group (the out-group) or its members” (Hewstone et al. 2002). Personal favoritism for the in-group can translate into issues and misunderstandings in interracial clinical interactions and thus contribute to health care disparities (Penner et al. 2017). For example, in a clinician–patient interaction, the clinician and patient may react to one another as more of a representative of a different group, rather than as individuals (Penner et al. 2017). Awareness of intergroup bias encourages dental professionals to individualize patients, acknowledging them as unique individuals rather than grouping them into racial or social stereotypes (Penner et al. 2014).
This scoping review also identified an individual’s racial identity as a significant variable in their perceptions of racial dynamics and racism (Su and Behar-Horenstein 2017; Cahoon et al. 2023). For example, African American individuals presented with greater awareness of the presence of racism in society in comparison with their racial and ethnic counterparts (Ludwig et al. 2019; Ludwig et al. 2022). A study by the Pew Research Center found that nearly half of Americans (46%) claimed there is “a lot” of discrimination against Black individuals, while only 14% claim White individuals face “a lot” of discrimination (Daniller 2021). Greater awareness of racism among African American individuals perhaps stems from their unfortunate exposure to discriminatory actions against them and their community. Small numbers of dental professionals from marginalized backgrounds and the unawareness of racism among racial majority (White) providers reinforce the need for bias self-awareness as well as increasing workforce diversity (Mertz et al. 2016).
There is currently a great disparity between the number of African Americans, Hispanics, and American Indians in the broader U.S. population in comparison with their presence among U.S. dental professionals (Lacy et al. 2012). Limited diversity among dental professionals likely plays a role in clinical decision-making bias when treating patients from racially and ethnically minoritized backgrounds (Borrell and Williams 2022). In addition, oral health needs are often unmet for many individuals from racially and ethnically minoritized backgrounds, emphasizing the important role of the representation of health care professionals from racially and ethnically minoritized backgrounds (Lacy et al. 2012). Thus, diversifying the profession may reduce implicit bias among providers as well as advance oral health equity. Dental graduates from schools with greater numbers of African American students in the first-year class report feeling more prepared to provide oral health care for diverse groups, accept and respect diverse patients, and integrate cultural differences into treatment planning (Andersen et al. 2007). Increasing the diversity of dental student populations can expose students early on to the cultural diversity necessary to improve their cultural responsiveness and awareness of racism.
In addition to racial identity, one’s education level can play a role in implicit bias. With more educational experience, students are more aware of racism (Ludwig and Suedbeck 2023a). University environments may allow for greater opportunity to attend events and join student groups that encourage learning about diversity and culture. In addition, baccalaureate education may allow for additional curriculum and patient experience to increase exposure to these topics (Ludwig and Suedbeck 2023a). This scoping review reiterates the importance of integrating implicit bias training early in dental education. Studies cite the effectiveness of implementing education on the color-blind ideology and recognizing stereotyping and implicit bias (Ludwig and Suedbeck 2023b). For example, a longitudinal study by Devine et al. (2012) demonstrated that a 12-wk prejudice habit-breaking intervention can result in long-term reductions in implicit racial bias. A growing number of states are requiring training in implicit bias and/or cultural competency to obtain or renew a dental license (American Association of Orthodontists 2024). States should consider offering validated trainings such as the one described by Devine et al. (2012) as a requirement for dental and dental hygiene licensure. Perhaps the IAT and CoBRAS tools within these educational programs could be used to identify early implicit bias, increase awareness, and measure bias reduction throughout a program’s duration. Early and continuous awareness of implicit bias and active prevention are critical to reducing the adverse effects of bias among dental/dental hygiene students, dental hygienists, and dentists.
Age itself can be a factor in the unawareness of the denial of racism. For example, younger dental hygienists are more aware of racism (less in denial) in comparison with older participants, and URM faculty are less aware of institutional discrimination in contrast to younger URM students (Cahoon et al. 2023; Ludwig et al. 2022). These findings call into question the reason why older adults may be less aware of the existence of racism. In response, evidence points to the generational context that failed to acknowledge racism in which many older adults were raised and potential age-related deficits in inhibiting automatic and prejudicial thoughts (Von Hippel et al. 2000; Stewart et al. 2009).
This scoping review highlights the critical need for large-scale studies of implicit bias that are representative of dental/dental hygiene students and professionals in terms of gender, age, race and ethnicity, and geographic location. The studies reviewed here are an important first step in examining implicit bias among those who provide oral health care for an increasingly diverse U.S. population. However, their small scale and lack of generalizability to the broader oral health student and professional communities is a significant limitation to the current understanding of how implicit bias affects patient oral health outcomes. Also, this research identified studies examining implicit bias only related to racial/ethnic identity and not related to any other marginalized identity (e.g., gender, age, language spoken, weight, etc.). Although race is a social, rather than biological, construct (Bastos et al. 2018), understanding the implicit biases toward this construct of those who provide oral health care is critical to understand one source of oral health inequities.
There were no studies identified in the literature that examined how the intersection of different identities may interact with implicit bias expressed by students or providers. For example, would dentists surveyed in the study by Patel et al. (2019) have provided different recommendations if the patient presented in the case were a White or Black male, compared with a female patient? Future research should examine the how the intersection of patients’ identities interacts with dental/dental hygiene students’ and providers’ implicit biases.
Limitations
Some limitations may have influenced this scoping review. A total of 10 studies were included in our final review, which is a limited number of studies, particularly in comparison with the research on implicit bias within the medical and health care space at large. Narrowing the research to the dental profession limited the number of studies that matched our inclusion criteria and thus the generalizability of our findings. In addition, the search was limited to the PubMed database and evaluated only reports in the English language—2 additional limitations to the generalizability of our findings. While limitations of each included study are included in the Results section, this article does not include a detailed critical appraisal of each included study.
Future Directions and Recommendations
The studies included in this scoping review centered on the discussion of implicit bias related to race and ethnicity, with differences in oral health professionals’ race, age, and education level. Future research should continue to evaluate the role of implicit bias in clinical decision-making, the relationships built between patients and providers, and oral health disparities. Future studies should also consider diving deeper into additional biases such as religious bias, socioeconomic bias, and weight bias, among others, to adequately evaluate the role of implicit bias among dental/dental hygiene students and professionals. As oral health is inextricably linked to overall health (Heaton et al. 2023), it is critical to understand how implicit bias affects patient outcomes in both oral and overall health. In addition, only 1 study collected original data on patient oral health outcomes (Patel et al., 2019); as this study was conducted in Italy, researchers in the United States and other countries should aim to replicate these findings elsewhere. Future research should evaluate how implicit bias directly affects oral health outcomes. Currently, most literature focuses on strategies to combat implicit bias in the broader health care context; however, future research should continue to narrow its focus on interventions specifically within oral health. Lastly, we would like to recognize the existence of explicit bias within oral health and the importance of further research in this space. However, our scoping review focuses on implicit bias.
Conclusion
The goal of this scoping review was to examine what scientific literature exists about implicit bias demonstrated by dental/dental hygiene students and providers and, when possible, how these implicit biases are associated with patients’ oral health outcomes. This review highlights the small number of oral health–specific studies of implicit bias and the even more limited number of studies that examine how implicit bias can affect patients’ oral health outcomes. Despite the small sample sizes and lack of racial/ethnic diversity that limit the generalizability of the studies examined in this scoping review, the findings of these studies provide evidence for implicit racial bias held by some dental/dental hygiene students and professionals that may affect patient oral health outcomes. Training to increase the awareness of and reduce implicit bias among those providing oral health care is an important first step to providing a more equitable health care system for all patients.
Author Contributions
P. Martin, L.J. Heaton, contributed to conception, design, data acquisition, analysis, and interpretation, drafted and critically revised the manuscript; K. Rafia, M. Minter-Jordan, E.P. Tranby, P.D. Edouard, R. Taylor, contributed to conception, data interpretation, drafted and critically revised the manuscript. All authors gave final approval and agree to be accountable for all aspects of the work.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: CareQuest Institute for Oral Health provided full-time salary support for this work for Ms. Martin and Drs. Rafia, Minter-Jordan, Tranby, and Heaton. Support for Ms. Taylor and Dr. Edouard’s work was supported by the National Association of Chronic Disease Directors.
