Abstract
Introduction:
Canada’s national health insurance historically excluded dental care until the introduction of the Interim Canada Dental Benefit (CBD) in October 2022. This represented a paradigm shift toward enhancing dental care accessibility for children younger than 12 y from lower-income families. This study investigated parents’ perspectives on access to oral health care and the Interim CDB.
Methods:
The Strategic Counsel for Health Canada collected data from participants across Canada using an online survey administered in March 2023. Data were administered to parents of children younger than 12 y with a household income less than $90,000. The survey included 45 questions covering demographics, barriers to accessing dental care, and awareness of the Interim CBD. Paired/overlap t test for means and paired/overlap z test for percentages were performed, with statistical significance set at P ≤ 0.05.
Results:
A total of 2,203 participants completed the survey, with a response rate of 65%. Most participants expressed concerns about the costs (90.9%) and accessibility (80.9%) of dental care, indicated that regular dental visits for children are important (97.2%), and would take their children more frequently to dental appointments if they had extra money (79.9%). Some of the barriers preventing regular dental visits for children included the costs of service and transportation and lack of insurance. Most parents supported the Interim CDB (87%), with the greatest support coming from the provinces of Manitoba and Saskatchewan (90.4%).
Conclusion:
This research underscores the imperative for ongoing evaluation and policy refinement to ensure the Canadian Dental Care Plan (CDCP) effectively addresses the nuanced needs of Canadian families, fostering a more inclusive and accessible dental care system. Parents’ concerns regarding dental care and their support for the Interim CDB signal a clear mandate for improving program outreach and accessibility through the CDCP.
Knowledge Transfer Statement:
This study showed the significant concerns reported by survey participants about dental care affordability in Canada and the highly positive perception of the Interim Canada Dental Benefit (CDB). This supports the necessity of programs such as the CDB and Canadian Dental Care Plan, which are crucial for the success of a policy intervention. Concern about accessing dental services, despite the availability of insurance, indicates ongoing barriers to dental care, suggesting areas for future policy refinements.
Introduction
Historically, Canada’s national health insurance (Medicare) has not included dental care, reflecting the country’s focus on equitable access to broader health care services. Public spending on dental care in Canada accounts for only about 6% of total dental expenditures, which is significantly lower compared with countries such as the United States (13%) and other nations with similar health care systems, such as the United Kingdom, where the public dental care program is more robust and comprehensive (Quiñonez et al. 2022). The limited public funding in Canada covers the cost of dental care for certain groups of people. The federal government funds dental care services to specific groups, including state-recognized Indigenous populations (registered First Nations and Inuit) and the country’s Armed Forces (Farmer et al. 2022). Meanwhile, provincial governments finance dental care for low-income children, social welfare recipients, individuals with disabilities, and those with craniofacial disorders (Canadian Academy of Health Sciences 2014). Municipalities often co-share costs for low-income children’s care and social welfare recipients with provinces, whereas low-income seniors receive independent care from municipalities. Despite these government investments, access to oral health care remains a significant challenge, with more than 32% of Canadians reporting financial barriers to accessing dental services and nearly 48% of uninsured individuals avoiding necessary care due to cost (Canadian Academy of Health Sciences 2014; Moharrami et al. 2024; Schroth et al. 2024). As Canada progresses in its efforts to enhance oral health policies, international perspectives are helpful. Free dental care at the point of service for children is offered in some countries, such as the United Kingdom and the Nordic countries. Australia’s public dental program provides free or low-cost services to eligible adults and children, with a focus on those with health care cards or pensions. Unfortunately, similar to Canada, access can be limited due to availability and long wait times, highlighting a common challenge faced by public dental health systems worldwide.
Access to care is a complex issue that includes affordability, availability, accessibility, acceptability, awareness, and accommodation (Saurman 2016). The Interim Canada Dental Benefit (CDB) and the Canadian Dental Care Plan (CDCP) are significant steps toward equitable dental care in Canada. These initiatives aim to improve affordability for lower-income families and promote inclusivity in health care. Community feedback, especially from parents and children, is essential for assessing the effectiveness of these programs and identifying areas for improvement.
In October 2022, the Canadian government launched the Interim CDB for children <12 y of age from families with annual incomes <$90,000 without private dental insurance (Canada Revenue Agency 2022; Department of Finance Canada 2022; Government of Canada 2022; Rabson 2023; Rollason 2023). The “cost of living relief for dental care and rental housing bill” provides financial support up to $650 for each child if the family’s adjusted net income is <$70,000, while $390 is provided if the adjusted net income is between $70,000 and $79,999 and $260 if it is between $80,000 and $89,999 (Canada Revenue Agency 2022; Department of Finance Canada 2022; Government of Canada 2022). The Interim CDB is a precursor to the CDCP. The Interim CDB sunset June 30, 2024, while the CDCP commenced by mid-2024, providing coverage for uninsured Canadians with an annual family income <$90,000 (Nadeau 2023).
To receive the Interim CDB, families must have had a child or children <12 y of age at the time of application, no private dental insurance, and an adjusted family net income of <$90,000 per year. In addition, families must have filed a 2022 tax return with the Canada Revenue Agency and incurred out-of-pocket dental care expenses for their child between October 1, 2022, and June 30, 2024 (Nadeau 2023).
Research shows that multiple factors influence children’s use of dental services. These include their parents’ dental care utilization, level of education and socioeconomic status, income, employment status, access to dental care, dental insurance, behavioral beliefs, perceived power, subjective norms, and parental preventative practices (Isonget al. 2010; Badri et al. 2014; Nagdev et al. 2023). Furthermore, studies have shown that racial and ethnic disparities in dental care utilization are significantly reduced when a child has a parent who uses oral health care and has access to childcare and continuous insurance coverage (Guarnizo-Herreno and Wehby 2012).
This study’s aim was to investigate the perspectives of parents of children younger than 12 y on dental care accessibility challenges and the Interim CDB in anticipation of the CDCP.
Methods
This cross-sectional study analyzed data collected from a public opinion research online survey undertaken by The Strategic Counsel on behalf of Health Canada’s Oral Health Branch in 2023 (Health Canada 2023).
Quotas were applied to the base sample (n = 2,000) to ensure broad representation from all regions of Canada and a more significant proportion (70%) of Canadian parents with no access to private dental care insurance, as this is one of the requirements for eligibility for the Interim CDB (Health Canada 2023). Two additional “sample boosts” (n = 100 each) were carried out to ensure good representation from those residing in remote areas (those located more than 350 km from the nearest dental professional and/or without year-round road access) and those who identify as being a member of an ethnic minority community (Table 1). The estimated sample size was calculated to detect differences of ±5% at a 95% confidence interval for key variables, based on the target population. A weighting scheme was applied during analysis to align the sample size with the distribution of the Canadian population by region, based on the Census 2021 from Statistics Canada. Inclusion of parents from rural and remote areas, as well as ethnic minorities, was purposeful to obtain the experiences of often underresearched demographics, contributing to a more inclusive understanding of dental care accessibility.
Characteristics of the Participants.
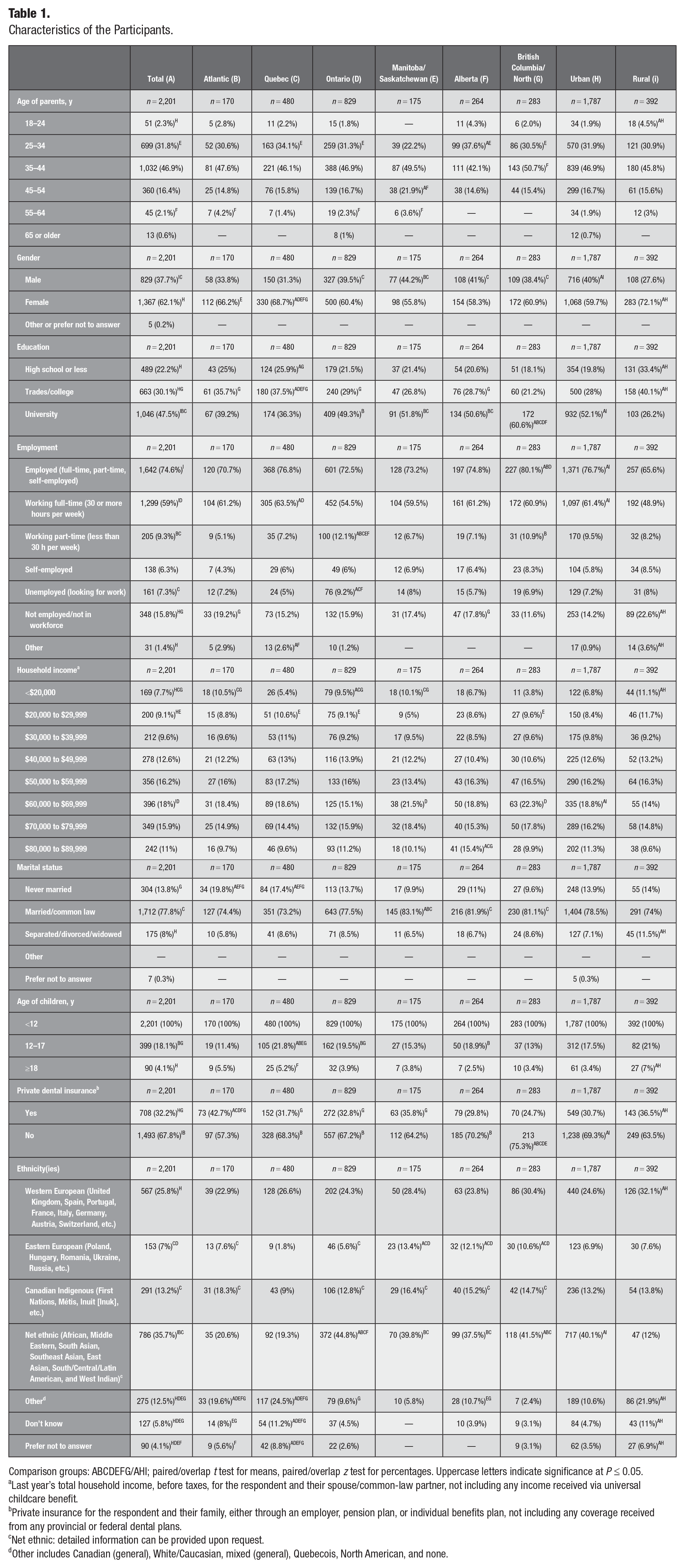
Comparison groups: ABCDEFG/AHI; paired/overlap t test for means, paired/overlap z test for percentages. Uppercase letters indicate significance at P ≤ 0.05.
Last year’s total household income, before taxes, for the respondent and their spouse/common-law partner, not including any income received via universal childcare benefit.
Private insurance for the respondent and their family, either through an employer, pension plan, or individual benefits plan, not including any coverage received from any provincial or federal dental plans.
Net ethnic: detailed information can be provided upon request.
Other includes Canadian (general), White/Caucasian, mixed (general), Quebecois, North American, and none.
A telephone recruit-to-online approach was used to reach those residing in remote communities who met the eligibility criteria. The survey was administered from March 3 until March 30, 2023, and the detailed methodology used for sample design can be found in the Canada Dental Benefit Baseline Survey Final Report (HC POR —22-32; Health Canada 2023). Data from this study were accessed from the Government of Canada’s “Library and Archives Canada collection” website at https://epe.bac-lac.gc.ca/100/200/301/pwgsc-tpsgc/por-ef/health/2023/126-22-e/index.html.
Institutional ethics approval was not required as this study used aggregate and anonymized data that did not contain personal identifiers.
The online survey included 45 questions covering the demographic characteristics of the respondents (e.g., age, gender, education, and employment), attitudes toward dental care, access to and use of dental services, barriers to accessing dental care for children, and awareness and views on the Interim CDB. The survey questions were developed in collaboration with Health Canada, with pretesting conducted among 32 participants (21 English, 11 French) to ensure validity and comprehensibility (Health Canada 2023).
The analyses were stratified by province/region and by place of residence (urban: a city or large town or rural: outside a city or a large town). The place of residence was determined based on the postal code or was self-reported by those who preferred not to provide a postal code. Values less than 5 were suppressed for confidentiality purposes. Statistical analysis was undertaken by the Strategic Council and included paired/overlap t test for means and paired/overlap z test for percentages, with statistical significance set at P ≤ 0.05. This work follows the STROBE guidelines checklist for cross-sectional studies.
Results
Characteristics of the Participants
This was a self-complete 15-min online survey aimed at parents of children <12 y of age with an annual household income <$90,000 Canadian. All participants were older than 18 y. A total of 2,203 parents completed the online survey (65% response rate). Most participants were between 25 and 44 y old (78%), female (62.1%), married or in common-law relationships (77.8%), employed (74.6%), lacked private dental insurance (67.8%), had university (47.5%) or trades/college (30.1%) education level, lived in urban centers (81.2%), and were from Ontario (37.7%) (Table 1). There was a wide distribution of household income levels, with nearly 45% earning $60,000 or more. The distribution of income levels showed some regional variation, with the Atlantic region having a higher proportion of participants earning less than $40,000. The ethnic backgrounds of participants were diverse, with the largest group being Western European (25.8%), whereas another 13.2% identified as Canadian Indigenous.
View and Concern about the Affordability of and Access to Dental Care
Most participants (90.9%) were very or somewhat concerned about the affordability of dental care in Canada, with regional responses ranging from 88% in Atlantic Canada to 93.3% in Manitoba and Saskatchewan. There was no difference in responses between urban and rural dwellers. Further, 80.9% were very or somewhat concerned about accessing the services of a dentist or oral health care professional (Table 2), with regional responses ranging from 73.9% in Atlantic Canada to 83.9% in Manitoba and Saskatchewan. Interestingly, those living in urban areas were more likely to report concerns about accessing services of a dentist or oral health care professional than those from rural areas were (82.3% vs. 74.2%).
Concern about Affordability of Dental Care and Access to Services of an Oral Health Care Professional and Views on Dental Care for Children, by Region.
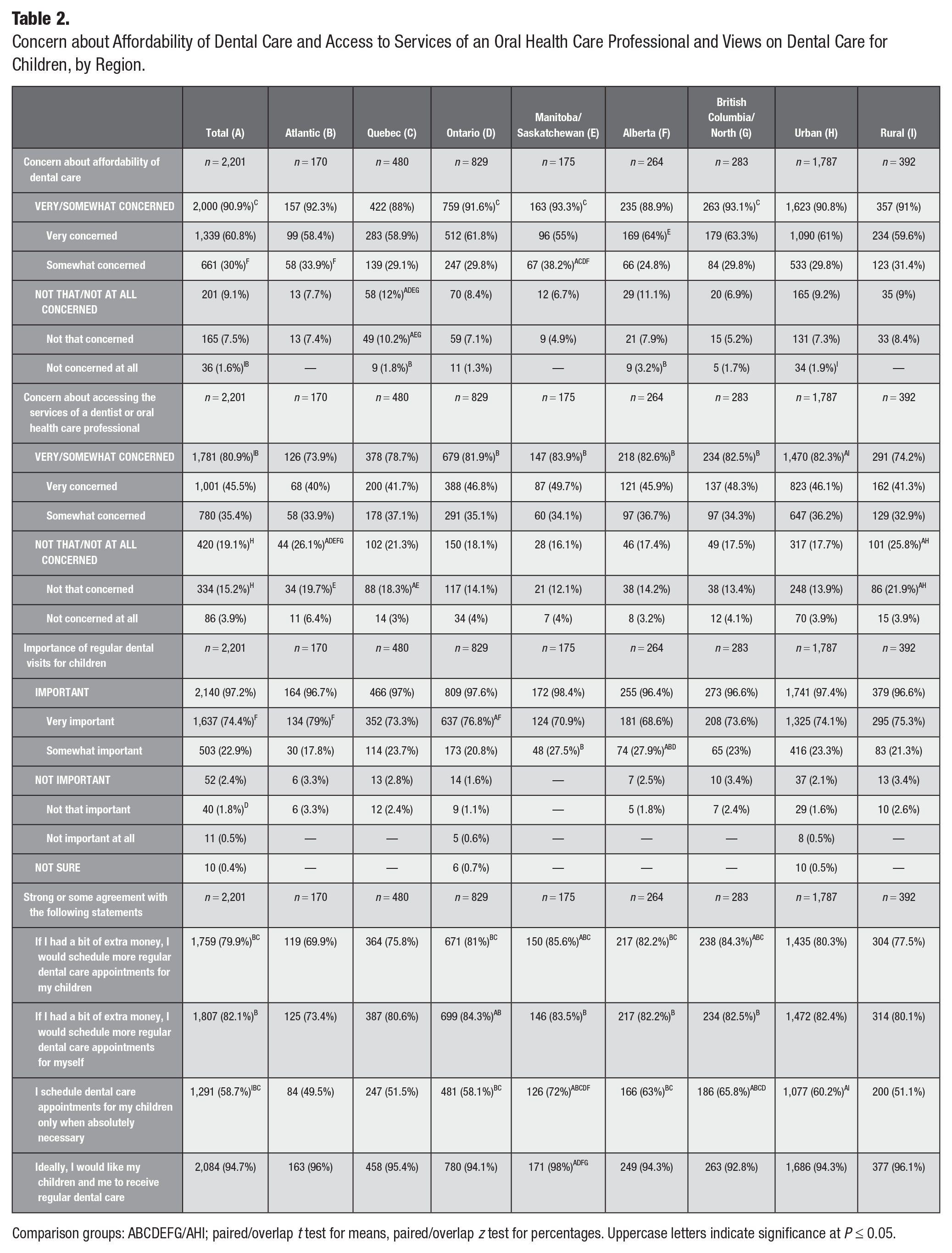
Comparison groups: ABCDEFG/AHI; paired/overlap t test for means, paired/overlap z test for percentages. Uppercase letters indicate significance at P ≤ 0.05.
Almost all participants (97.2%) indicated that regular dental visits for children were important, with similar responses across regions and between urban and rural dwellers (Table 2). When asked, most participants reported they would schedule more regular dental care appointments for their children (79.9%) or themselves (82.1%) if they had a bit of extra money. However, there were some regional variations for scheduling more regular dental care appointments for children (ranging from 69.9% in Atlantic Canada to 85.6% in Manitoba and Saskatchewan) and parents (ranging from 73.4% in Atlantic Canada to 83.5% in Manitoba and Saskatchewan). Overall, 58.7% of respondents indicated that they schedule dental care appointments for their children only when absolutely necessary, with regional variations (ranging from 49.5% in Atlantic Canada to 72.0% in Manitoba and Saskatchewan) and urban and rural differences (60.2% vs. 51.1%). In addition, 94.7% of the participants strongly or somewhat agreed that, ideally, they would like their children and themselves to receive regular dental care (Table 2).
Access to Dental Services for Children
Overall, 51.3% of the participants reported having access to a dentist or oral health professional for their whole family, and 18.5% had access only for their children (Table 3). The Atlantic region had the highest proportion of respondents (59.9%) reporting they had access to dental services for the whole family, while Manitoba and Saskatchewan had the lowest proportion of residents reporting access to dental services for the entire family (47.3%). Surprisingly, more participants in rural regions reported having access to dental services for the whole family than those from urban areas did (58.1% vs. 49.7%).
Access to and Use of Dental Services for Children Oral Health Care, by Region.
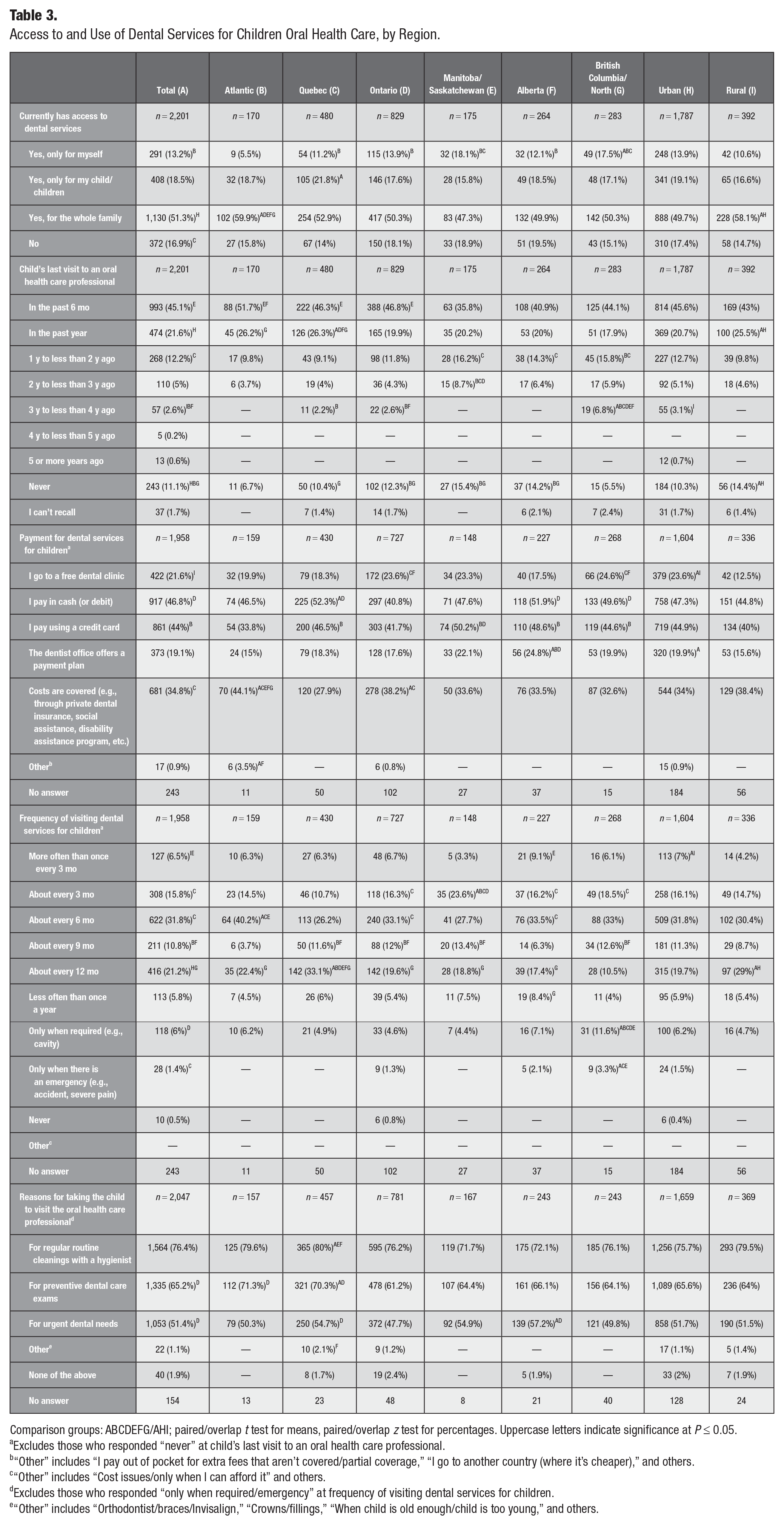
Comparison groups: ABCDEFG/AHI; paired/overlap t test for means, paired/overlap z test for percentages. Uppercase letters indicate significance at P ≤ 0.05.
Excludes those who responded “never” at child’s last visit to an oral health care professional.
“Other” includes “I pay out of pocket for extra fees that aren’t covered/partial coverage,” “I go to another country (where it’s cheaper),” and others.
“Other” includes “Cost issues/only when I can afford it” and others.
Excludes those who responded “only when required/emergency” at frequency of visiting dental services for children.
“Other” includes “Orthodontist/braces/Invisalign,” “Crowns/fillings,” “When child is old enough/child is too young,” and others.
Furthermore, 45.1% of participants reported taking their child to a dental office or oral health professional within the past 6 mo prior to the survey (Table 3), with results ranging from 51.7% in Atlantic Canada to 35.8% in Manitoba and Saskatchewan. There was no significant difference between urban and rural respondents. Overall, 66.7% reported that their child last visited an oral health care professional within the past year or less, with results ranging from 77.9% in Atlantic Canada to 56.0% in Manitoba and Saskatchewan. More parents from rural regions (25.5%) as compared with urban regions (20.7%) reported their child last visited an oral health care provider within the past year. However, 11.1% of the parents reported that they had never taken their child/children to an oral health care professional. This proportion was highest in Manitoba/Saskatchewan (15.4%), followed by Alberta (14.2%), Ontario (12.3%), and in rural regions (14.4%). Only 34.8% of respondents reported having the costs of dental services for children covered by an insurance or government program, with many having to pay for these services out of pocket. More than half of the parents from Quebec (52.3%) and Alberta (51.9%) reported paying in cash or debit for their child’s dental services. British Columbia (24.6%), Manitoba and Saskatchewan (23.6%), and urban dwellers (23.6%) had the highest proportion of parents taking their children to free dental clinics.
Overall, 31.8% of the respondents took their children to see a dentist or other oral health care professional every 6 mo, and the most common reasons for taking their child to visit an oral health care professional were routine cleanings, preventive dental exams, and urgent dental needs (Table 3). When asked about the barriers preventing parents from taking their child to see an oral health care professional regularly, participants selected the cost of the service (41%), lack of insurance (28%), cost of transportation (25%), cannot miss school or work (19%), and anxiety or fear (17%), among others (Fig.).
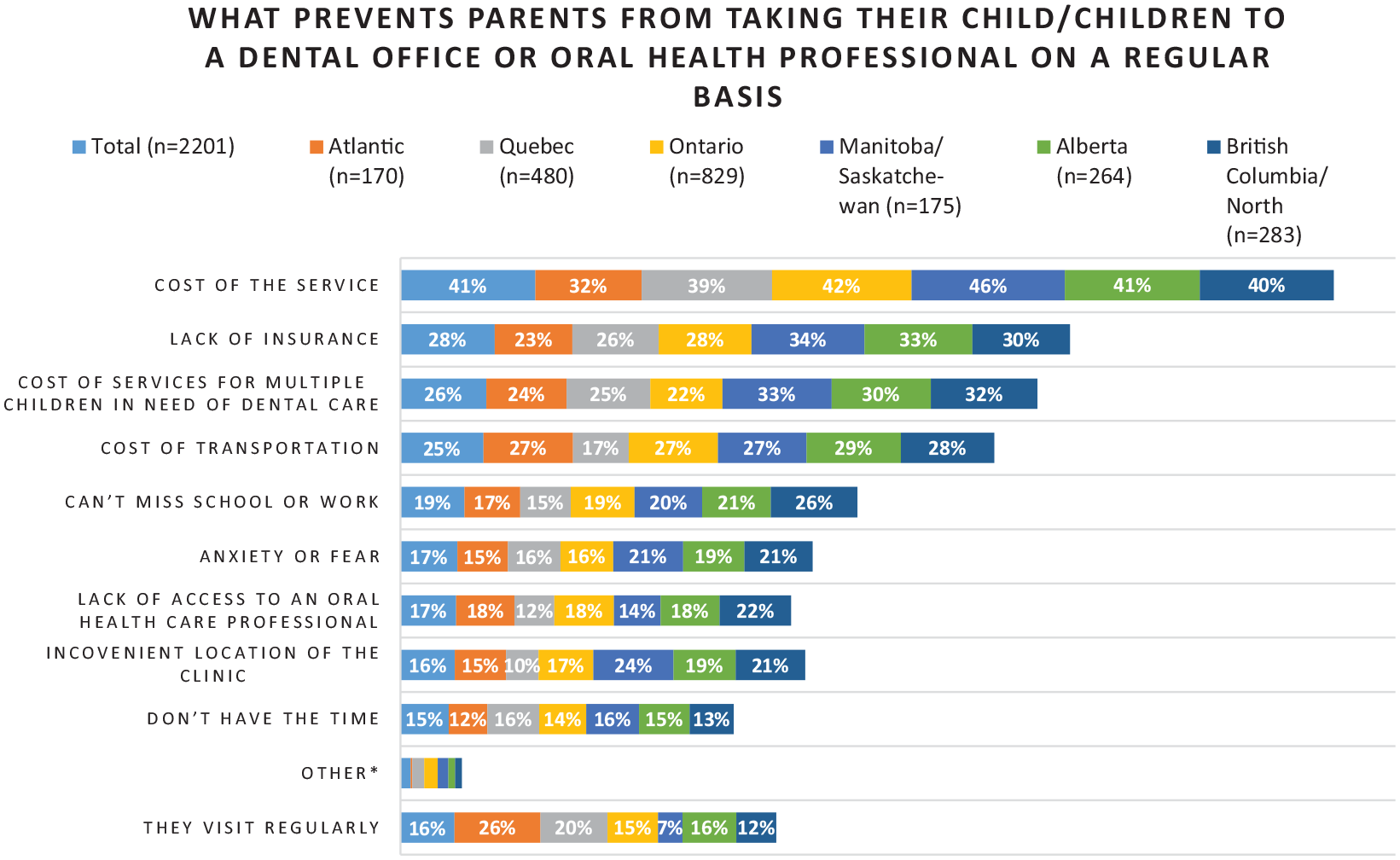
Barriers to accessing dental care for children. The percentage represents the proportion of the total number of respondents from each region who selected that barrier. The participants may have selected more than one barrier.
Awareness of and Support for the Interim CDB
Six in 10 parents reported hearing about the Interim CDB, but only 22.4% were well informed about the program. Manitoba/Saskatchewan (37.8%) and Atlantic Canada (37.5%) had the highest proportion of people unaware of the Interim CDB. Interestingly, a higher proportion of parents were aware of the program in rural areas (67.9%) compared with urban areas (63.3%). At the same time, parents from rural areas were less likely to apply for the CDB than parents from urban areas were. More than 70% of the respondents from British Columbia/North had applied or planned to apply for the program. Atlantic Canada had the lowest proportion of participants (54.5%) who had applied or planned to apply for the program (Table 4). More than 60% of the participants without access to dental insurance had heard about the program, and more than 70% were planning to apply or had applied already (Table 4). Most parents (87%) supported the interim CDB program, with the greatest support for the interim CDB coming from Manitoba and Saskatchewan (90.4%).
Awareness about the Interim Canada Dental Benefit and Number of Applicants.
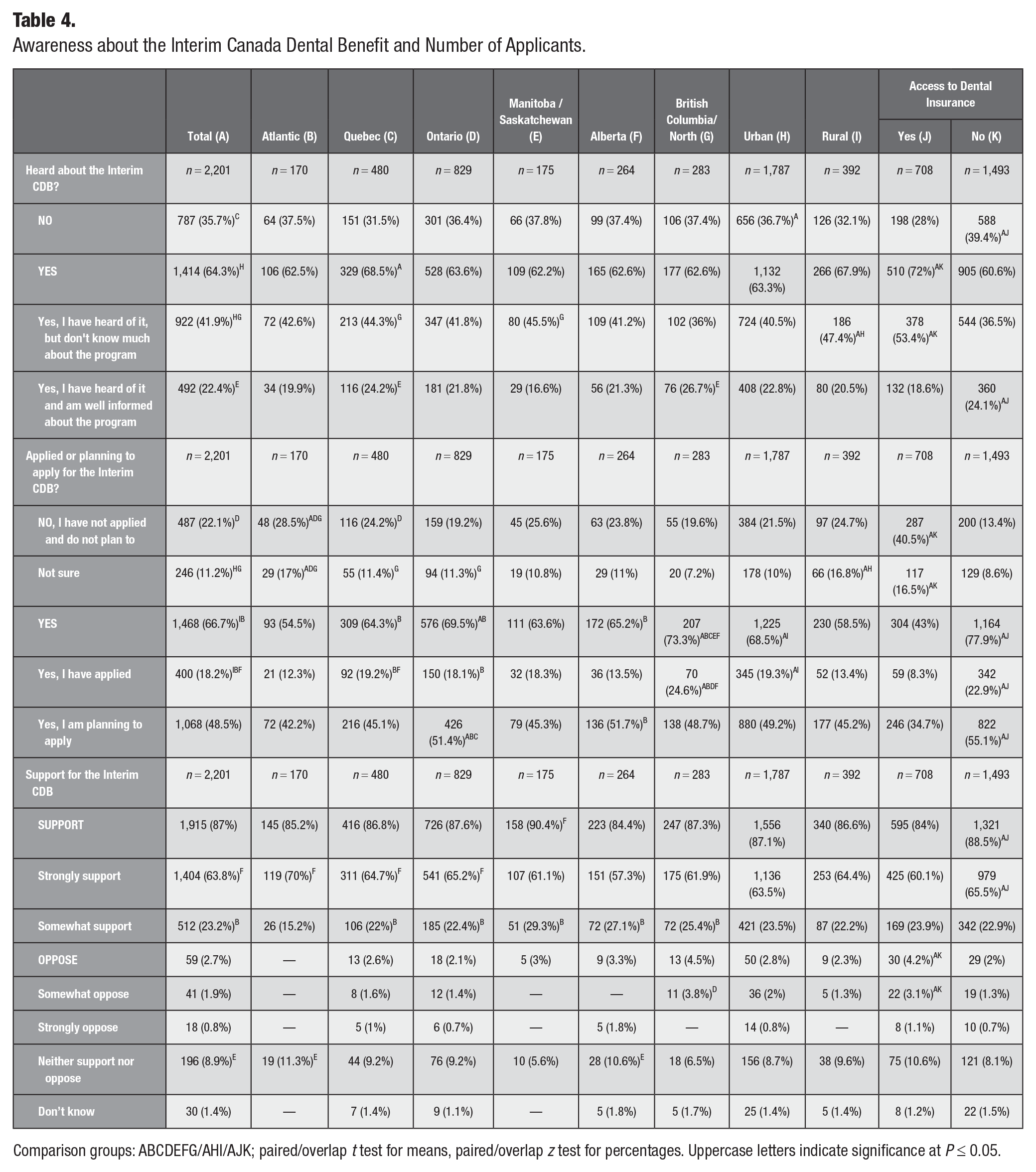
Comparison groups: ABCDEFG/AHI/AJK; paired/overlap t test for means, paired/overlap z test for percentages. Uppercase letters indicate significance at P ≤ 0.05.
Discussion
This study identified that many Canadian parents report challenges in accessing oral health care for their children younger than 12 y. Specifically, we identified that parents reported concerns about the affordability of dental care, have concerns about accessing services of an oral health professional, schedule dental appointments for their children only when necessary, indicate that they do not have access to an oral health professional, and have to pay for their children’s dental treatment out of pocket. In addition, parents identified numerous barriers to care, including the cost of services, transportation issues, lack of insurance, absence from work or school, anxiety or fear, inconvenient location of the dental clinic, or lack of access to an oral health care professional. Awareness, a domain of access to care, may be influenced by language and culture. Studies have identified language barriers as a significant impediment, especially among immigrant families, affecting their ability to access dental care (Reza et al. 2016). The government can address access-to-care issues by providing multilingual resources as part of the CDCP rollout. These challenges are especially pronounced in certain regions. Respondents strongly supported the interim CDB policy, which precedes the CDCP. It is important for the government to collaborate with First Nations, Métis, and Inuit communities to raise awareness of new investments in oral health care in rural and remote areas where dental providers are scarce.
The analysis revealed substantial concerns about the affordability and accessibility of dental care, with more than 90% of participants expressing some level of concern. As 32.2% of the participants had private dental insurance, this demonstrates that some people with dental coverage may still experience cost-related barriers, including being underinsured. In addition, they may be sympathetic to the affordability of oral health care as they may have other family or friends who are uninsured or underinsured and face challenges in accessing it. A recent study analyzing data from the 2017–2018 Canadian Community Health Survey (CCHS) reported that some people living in Ontario, despite having private dental insurance, still face financial barriers to accessing dental care (Abdelrehim and Singhal 2024). Similarly, data from the 2022 CCHS showed that 16% of Canadian adults with private insurance and 47.4% of those uninsured reported avoidance of dental care because of the cost (Moharrami et al. 2024).
Notably, the analysis underscored a strong consensus on the importance of regular dental visits for children, with 97% of respondents acknowledging its significance. This is consistent with the literature, emphasizing the critical role of early dental care in long-term oral health outcomes (American Academy of Pediatric Dentistry Pediatric Oral Health Research and Policy Center 2014). Studies have shown that regular dental checkups in childhood can significantly reduce the incidence of oral diseases (Khan et al. 2024), highlighting the public health implications of some Canadian parents seeking dental care only reactively, such as for cavities or emergencies. This reactive approach to dental health can lead to increased long-term health issues and costs. Programs such as the CDB and CDCP could help in shifting public attitudes toward more preventive care approaches, aiming to reduce the frequency and severity of emergency dental conditions.
Access to oral health care can be influenced by place of residence, with increasing oral health disparities seen in children from rural regions (Schroth et al. 2016). This study could not explain why rural-dwelling participants reported better access to care. The study’s findings are not entirely generalizable to all rural populations, as it did not include participants from very remote areas of Canada, where access to oral health care is limited and reliable internet service for the online survey was unavailable. Contrary to common perceptions, in the study, rural areas sometimes report better access and more frequent dental visits for children than urban areas do. This phenomenon may be attributed to targeted rural health initiatives or the lesser competition for dental services in these areas (Sulo et al. 2022). Such findings suggest that rural dental service provision might benefit from unique models of care tailored to their less dense populations.
The Canadian Federal Budget 2024 announced the government’s intent to include more health care professionals working in rural and remote communities (e.g., dentists and dental hygienists) in the Canada Student Loan Forgiveness Program, which is currently available only for doctors and nurses (Government of Canada 2024). In the United States, loan repayment programs have effectively influenced health care providers’ practice locations and retention in rural communities (Renner et al. 2010). Providing incentives for new graduates to work in underserved communities could help address the current distribution of oral health care providers in Canada and increase access to care in oral health professional shortage areas. Proposals such as mobile dental clinics and enhancements to public transportation could provide more consistent and widespread access to dental care facilities, particularly benefiting those in underserved rural areas (Pourat et al. 2020; Partido et al. 2021; Patel et al. 2023). These measures could alleviate some of the geographical and physical barriers currently hindering consistent dental care access, ensuring that all children and families receive more readily preventative and routine dental services.
Significant disparities in access to dental care were also observed between regions in Canada, with Manitoba and Saskatchewan reporting poorer access and a higher reliance on urgent or emergency dental services compared with other provinces. Many individuals in these 2 provinces had a higher rate of seeking care only when necessary, and a notable number of children did not see a dental professional. This reflects broader challenges in access observed in these regions, particularly in rural and remote areas. Despite these challenges, substantial public support for the CDB in these provinces indicates a strong community recognition of the substantial gaps in the existing dental care system, and this is demonstrated by their higher and above national rates of children receiving the Interim CDB (Schroth et al. 2024).
While there is a clear demand for better dental care, organized dentistry in Manitoba has shown resistance to the CDCP. At the beginning of 2024, 44% of the licensed members of the Manitoba Dental Association participated in a survey, and the results showed that most (89%) of the respondents we unlikely or very unlikely to participate as a provider in the CDCP (Manitoba Dental Association 2024). This highlights a significant gap between public support for funding oral health care for the uninsured and dentists’ opposition to the CDCP. Given the existing access issues, this significant opposition suggests a complex interaction between health care policy and professional practice norms. This scenario underscores the need for innovative solutions to bridge these gaps.
The introduction of the Interim CDB marked a significant milestone in updating the Canadian oral health policy (Gaffar et al. 2024) and addressing the affordability and accessibility challenges that have long plagued the Canadian dental care system. However, while our study sheds light on the high levels of concern among parents regarding dental care costs and access, it is imperative to contextualize these findings within the broader spectrum of dental care challenges faced nationally. The Interim CDB and, more recently, the CDCP are designed to mitigate financial barriers to dental care. However, these programs may not adequately address other crucial barriers, such as lack of awareness, accessibility challenges, and cultural appropriateness of services (Hopcraft 2024). These gaps emphasize the need for strategies that go beyond cost reduction to ensure inclusive access to dental care. The government could implement mobile dental units for remote areas, integrate dental services in community health centers, and extend clinic hours for working families. Expanding public awareness campaigns and culturally sensitive outreach can also help address barriers related to awareness and acceptance, highlighting the transformative potential of these initiatives.
The high rate of awareness (64%) and intended application (67%) for the Interim CDB among the participants reflects a proactive stance toward using available resources for dental care. This is indicative of a broader trend observed in recent research, in which public health initiatives are increasingly recognized and used by the community, suggesting a positive shift toward more informed health behavior and resource utilization (Zheng et al. 2024). However, these results also indicate the need for improved communication and outreach efforts to ensure all eligible families are informed and can access these supports, as more than one-third appeared unaware of the interim CDB.
Globally, the challenges of affordability and accessibility in oral health care resonate with findings from other nations with similar health care systems. For example, our data highlight barriers that parallel those seen in countries such as Australia and the United States, where cost and geographic disparities hinder equitable access to care. These findings provide valuable insights for policy makers worldwide who aim to design inclusive dental care initiatives, such as universal oral health care.
Limitations
This study has limitations due to its reliance on an online survey, which may have excluded noninternet users, those in rural areas with limited internet access, and individuals who were unwilling to participate. This could introduce selection bias, as their attitudes and behaviors may differ from those who responded (Health Canada 2023). The sampling format may have had an impact on the findings in rural and urban areas. Consequently, this cohort may not be representative of the entire target Canadian population. Furthermore, the cross-sectional design limits the ability to ascertain causality between perceived barriers and actual utilization of the CDB. The use of aggregated data did not allow further analyses of associations. Exploring parental perceptions toward the Interim CDB could greatly benefit from a more diversified methodological framework, possibly incorporating qualitative components to capture a more nuanced understanding of these perceptions.
Continuous community feedback and robust data analysis should guide the evolution of these initiatives moving forward. This approach will ensure that the dental care system in Canada becomes more inclusive and responsive to the needs of its population, paving the way toward eliminating oral health disparities across the country.
Conclusion
This study has substantiated the presence of significant barriers to dental care access in Canada among parents of children younger than 12 y. The responses identified concerns with the affordability of dental care and accessing services of an oral health care professional and lack of access to dental services, with many parents scheduling dental appointments for their children only when absolutely necessary and agreeing that if they had extra money, they would schedule more regular dental appointments for their children. Barriers to accessing oral health care include cost of services and transportation to the dental office, lack of insurance, and others. The widespread support across Canada for the Interim CDB reflects a strong public consensus on the need for more affordable dental care options.
Author Contributions
A. Menon, V. Cruz de Jesus, R.J. Schroth, contributed to conception, design, data analysis and interpretation, drafted and critically revised the manuscript; J.I. Virtanen, contributed to data interpretation, critically revised the manuscript. All authors gave final approval and agree to be accountable for all aspects of the work.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this research was made possible from Dr. Schroth’s Canadian Institutes of Health Research Applied Public Health Chair in Public Health Approaches to Improve Access to Oral Health Care and Oral Health Status for Young Children in Canada.
