Abstract
Introduction
Although African women constitute the majority of the continent's population and play a central role in economic development, their reproductive health needs remain overlooked. Infertility is often regarded as a tragedy, carrying profound psychosocial consequences. The resulting stress and societal pressure undermine women's well-being and drive many to pursue alternative treatment options in their search for motherhood. This systematic review aims to map the existing evidence on complementary approaches to the management of female infertility in Africa.
Methods
A systematic review was conducted through searching English databases, including PubMed, Scopus, CINAHL, Google Scholar, EBSCOhost, Medline, ProQuest, and ScienceDirect. The screening of titles, abstracts, and full texts was conducted using searches such as CAM/therapy, women, and infertility. All studies published in peer-reviewed journals from 2020 to 2025 which examined women's needs in the field of CAM use were included in the review. Out of the 300 records reviewed, 30 studies were included in the final review.
Results
The 30 studies reviewed revealed widespread use of complementary approaches to infertility management among African women. These practices were shaped by sociocultural beliefs, psychosocial pressures, accessibility, and perceived limitations of conventional care. Overall, the findings indicate a strong tendency toward pluralistic health-seeking behaviors in the management of female infertility across African settings.
Conclusion
Women experiencing infertility frequently seek treatments beyond conventional medicine, including herbal remedies, prayers, plant-based products, lifestyle and dietary changes, allopathic therapies, indigenous counselling, and acupuncture in their pursuit of pregnancy.
Introduction
Addressing infertility and its associated challenges is a critical aspect of sexual and reproductive health and rights (SRHR). Despite its significance, infertility remains insufficiently prioritized within the global SRHR agenda. Tackling this issue is essential for the realization of Sustainable Development Goals (SDGs) 3 and 5, which focus on ensuring healthy lives and promoting gender equality, respectively (Cox et al., 2022; WHO, 2023).
Infertility is estimated to impact millions of people worldwide, often with devastating consequences that affect one's physical, psychological, social, and financial well-being (Armah et al., 2022; Kyei et al., 2021; Thoma et al., 2021; WHO, 2023).
Generally, infertility is defined as a disease of the male or female reproductive system, often causing an inability to achieve a pregnancy or live birth despite unprotected sexual intercourse (WHO, 2023).
In most communities, infertility is mostly attributed to women, even though the cause of infertility could be either a male or female factor. Women often bear the societal burden of infertility, particularly in societies where a woman's identity and social value are closely tied to her ability to bear children (Azimi-Nezhad et al., 2022; Thoma et al., 2021).
In Africa, infertility poses serious psychosocial threats, including anxiety, depression, marital instability, divorce, stigma, and family disruption (Kyei et al., 2021; Odoi, 2023).
Country-specific accounts reveal entrenched discrimination: for instance, in Ghana, women face stigma, branded as witches, accused of using their wombs for rituals and even dehumanizing burial practices in the case of death (Adda et al., 2025; Kuug et al., 2023).
Women with infertility in Zimbabwe, Malawi, and Cameroon, experienced derogatory labelling, social scorn, mockery, divorce, and separation with cultural practices such as “Fiisi,” wherein a male member of the community is permitted to impregnate a woman who has been unable to conceive within her marriage (Elwell, 2022; Mashaah et al., 2024; Mpono et al., 2024).
In Guinea and Nigeria, women with infertility encounter rejection in personal, social, and professional spheres, whereas they were also labelled as “less than” or “incomplete” due to their inability to conceive (Joseph-Shehu et al., 2024; Leno et al., 2022).
Children are regarded as vital to family inheritance in Africa and are also an integral part of the transition process (Kyei et al., 2021). This, therefore, implies that in Africa, the true meaning of marriage is only accomplished when there is an announcement of a child being born.
The current researchers perceived that the longer there is a delay in childbearing, the closer women get to menopause, and this may further drive them to pursue answers from any source, be it spiritual, traditional, or holistic approaches.
Given the high societal expectations, social pressures, and the deeply rooted pronatalist beliefs in African communities, women experiencing infertility are likely to explore various management options that align with their financial, cultural, and spiritual circumstances in their quest for children.
The findings of a related study on the quest for conception and exploring treatment patterns associated with infertility in Ghana have revealed that, in addition to conventional medicine, women with infertility sought various traditional methods and religious practices, whereas some women also combine spiritual healing with either herbal or orthodox medicine (Hiadzi & Boafo, 2020).
Women with infertility utilized various forms of complementary and alternative medicine (CAM), including herbal remedies, acupuncture, prayer, and vows. Among Iranian women, the use of other spiritual approaches was particularly prevalent, reflecting their strong belief in the power of God (Azimi-Nezhad et al., 2022).
In the case of the Yoruba, people of Southwestern Nigeria, and some parts of Nigeria, plant products were observed to have diverse potentials. As a result, plant products were used for the treatment of female infertility (Subair & Ade-Ademilua, 2022).
Women with infertility reported frequently switching from one source of care to another due to perceived impediments in the use of orthodox medicine (Naab et al., 2021). Various herbs and plant-based remedies are used to enhance fertility and support reproductive health, as some are believed to offer potential benefits for improving reproductive outcomes.
Desperation stemming from pressures exerted by husbands’ relatives, family members, friends, and the prolonged duration of infertility was a major factor driving women to seek diverse remedies, including traditional methods of infertility treatment (TMIT), in the hope of achieving a positive outcome (Nwosu et al., 2022).
Complementary management of infertility encompasses key domains, including education and information, psychological counselling, supportive care, access to complementary and alternative medicine (CAM), culturally appropriate treatments, and the integration of CAM with conventional care, all of which are essential for comprehensive infertility management (Sharifi & Roudsari, 2022).
Despite advances in assisted reproductive technologies and modern gadgets to manage infertility and its related issues in South Africa, women with infertility consulted with indigenous healthcare practitioners (IHCP) to restore their fertility (Baakeleng et al., 2023).
Spirituality plays a crucial role in the complementary management of female infertility. Evidence suggests that strong spiritual practices enhance coping, improve mental well-being, and support better reproductive health outcomes among women and couples facing infertility (Arhin et al., 2025; Naab et al., 2025).
The desperation to find the exact remedy that would work for them led to “healer shopping” and a combination of treatments, including conventional, herbal, spiritual, psychosocial, and nutritional approaches.
What is missing in the literature is existing evidence on the complementary management of female infertility in Africa. This review, therefore, examined existing evidence on the complementary management of female infertility in Africa. Findings would inform the development of programs or protocols that integrate complementary management in traditional infertility treatment.
Operational Definition of Terms
Materials and Methods
Study Design
A systematic review in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement published in 2020 was adapted to review existing evidence on the complementary management of female infertility in Africa. An account of the PRISMA statement recommendations was described (Table 1).
Summary of Studies on the Characteristics of Complementary Management of Infertility.

Databases and Search Strategy
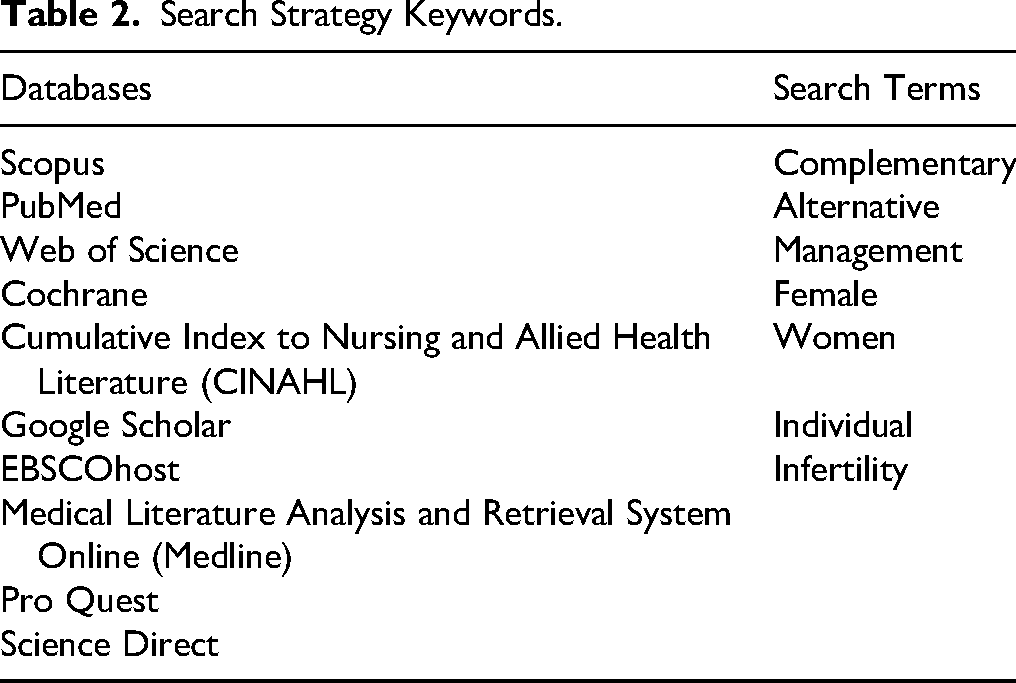
A methodical search of international electronic databases, including Scopus, PubMed, Web of Science, Cochrane, CINAHL, Google Scholar, EBSCOhost, Medline, ProQuest, and Science Direct, was employed, and the precise keywords from the topic were utilized. The search for papers was executed using keywords such as complementary, alternative, management, female, women, and infertility (Table 2).
Search Strategy Keywords.
Eligibility Criteria
Inclusion Criteria
The study's inclusion criteria include (a) studies published in English between 2020 and 2025, (b) studies conducted on the complementary management of women with infertility in Africa.
Exclusion Criteria
The study excludes book chapters, mini reviews, short commentaries, doctoral theses or conference presentations, and studies focusing on other issues related to infertility beyond the researchers’ intended research (Table 3).
Inclusion and Exclusion Criteria for Acceptable Articles.

Data Selection
All authors contributed to data selection and extraction, ensuring the removal of duplicate records at the outset. Relevant studies were identified through title and abstract screening, supplemented by additional searches. Of the 300 articles reviewed, 30 met the inclusion criteria: 10 qualitative, five quantitative, four comprehensive reviews, three systematic reviews, and eight employing other methodologies. Extracted data included authorship, year, country, study design and sample characteristics, purpose, and key findings. The study selection process is detailed in the PRISMA flowchart (Figure 1).

PRISMA flow diagram for literature search.
Data Extraction and Analysis
A self-structured data extraction form was used to collect relevant information, with discrepancies resolved by consensus. Article titles and abstracts were screened for eligibility, followed by full-text reviews of selected studies. Data were summarized in accordance with the PRISMA 2020 guidelines (Page et al., 2021), and eligible studies were compiled using the adapted PRISMA framework. Extracted variables included author (s), year, study location, purpose, design, sample size, duration of infertility, type and duration of complementary modalities, and key findings.
Results
Search Outcome
Figure 1 shows the flowchart of the study selection process. A total of 300 records were identified through various databases. After removing 34 duplicates, 266 records remained for screening. Of these, 122 were excluded based on title and abstract review. The full texts of 144 records were assessed, leading to the exclusion of 80 articles. Subsequently, 64 articles were evaluated for eligibility, with 34 more excluded. Ultimately, 30 studies were included in the final review. The main characteristics of the 30 studies included in the study are presented in Table 1, and the search results are depicted in the PRISMA 2020 flow diagram (Figure 1).
Discussion
Despite advances in modern infertility treatments, it is anticipated that many women may continue to combine multiple modalities to increase their chances of conception and manage societal pressures. In Ghana, a study on women's quest for conception revealed that, alongside biomedical care, women with infertility frequently used herbal remedies sourced from traditional healers, herbal vendors, or “Mallam” (Hiadzi & Boafo, 2020).
Prevailing sociocultural perceptions of infertility are likely to shape treatment-seeking behaviors, leading many individuals to prefer traditional or nonorthodox approaches. In Ghana's Upper East region, infertility is often attributed to spiritual causes, leading individuals to perform sacrifices to appease the gods. Herbal preparations are also widely used, sometimes in combination with “black” medicine, in the hope of accelerating conception (Kuug et al., 2023).
Although women with infertility often receive biomedical treatment, their expectations are not always fully met (Armah et al., 2022; Armah et al., 2024). A study in Ghana revealed that these women sought psychological, social, and spiritual support for holistic care, yet such needs remained unaddressed (Armah et al., 2022; Armah et al., 2024).
In Ghana, alongside biomedical management, various supportive interventions such as counselling, cognitive behavioral therapy, acceptance and commitment therapy, educational programs, spiritual practices, emotionally focused therapy, and integrative body-mind-spirit approaches are incorporated in some fertility settings to provide holistic care for women diagnosed with infertility (Armah et al., 2021).
The findings align with other studies in Africa. Notably, in South Africa, despite having modern health infrastructure and technologies for infertility care, women still sought support from indigenous healthcare practitioners (IHCPs) for herbal remedies, counselling (in-person or telephonic), and spiritual guidance through prayer. These women perceived IHCPs as experts and described their approach as holistic, with many reporting successful conception and viable pregnancies (Baakeleng et al., 2023).
It is noteworthy that in South Africa, homoeopaths provide alternative treatment options for women with infertility, tailored to the underlying cause. Common recommendations include dietary and lifestyle modifications, as well as health supplements, while modern plant-based remedies have also shown potential in improving female fertility (Anderson et al., 2024; Singh et al., 2024).
Naab et al. (2025) highlighted that women with infertility often rely on religiosity and spirituality as coping mechanisms. According to the researchers, spirituality provides hope, enhances quality of life and well-being, alleviates emotional stress, and may even increase the likelihood of successful treatment outcomes. This finding aligns with Hiadzi and Boafo (2020) and Arhin et al. (2025), who observed that individuals experiencing infertility frequently turn to spiritual therapies.
In Ghana and South Africa, studies show that women often begin their fertility journey with spiritual practices such as hope and prayer, and the pursuit of children commonly involves social, spiritual, and religious interventions (Whittaker et al., 2025).
In Nigeria, many women with infertility seek solutions from multiple sources, frequently relying on traditional methods such as medicinal plants to enhance their reproductive health. The high patronage of herbal remedies is largely influenced by factors such as the women's age, length of marriage, distance to healthcare facilities, societal pressures, and the relative affordability of traditional treatments (Maduka & Okubor, 2024; Nwosu et al., 2022; Ogunlakin et al., 2023).
It is worth noting that women with infertility in Mali also utilized plant products for herbal preparations to manage their infertility issues (Togola et al., 2023). A study in Zimbabwe revealed that traditional healthcare practitioners managed female infertility using both medicinal plants and spirit mediums. Spirit mediums were consulted to establish appropriate diagnoses and guide management, while herbalists relied on plant-based remedies for treatment (Mashaah et al., 2024).
Similarly, in Tanzania and Morocco, women with infertility turned to medicinal plants as alternative treatments, as these are widely regarded as vital sources of medicine for addressing reproductive health issues, including infertility (Kacholi et al., 2023; Slighoua et al., 2020).
Women with infertility in Ethiopia, aside from being spiritual, utilized traditional medicine, and also employed child adoption as a choice to silence factors that made their lives bitter (Adane et al., 2024).
A recent study in Sudan found that the high cost and limited availability of modern infertility treatments drove many women to adopt self-management strategies, particularly through herbal medicine. Notably, herbal use was also common among elite women, likely reflecting their greater awareness of both the potential risks and benefits of such remedies (Babikir et al., 2025).
In Sudan, many women received treatments rooted in religious practices, such as reciting Qur’anic verses from Shaikhs or wearing Qur’an inscriptions prepared as amulets, while others were given concoction drinks (Babikir et al., 2021). These practices were faithfully observed by Sudanese women in the hope of enhancing their fertility.
Although this current study examined the complementary management of infertility among African women, where societal pressure to bear children often compels them to seek alternative treatments. Similar patterns are observed beyond Africa; for instance, in India, women experiencing infertility report comparable stress and turn to traditional healers. Practices include cleansing rituals, the use of herbal mixtures with alcohol, dietary restrictions, and, in some cases, harmful interventions such as abdominal burns (dagani) and the removal of “black blood” (phasani) (Jadhav & Govil, 2023).
In India again, a recent study on holistic approaches to managing female infertility revealed that, in addition to conventional medical treatments, women also adopted strategies such as diet therapy, physical activity, lifestyle modifications, and the use of medicinal plants to optimize reproductive health (Nahid et al., 2025).
A recent study on herbal therapeutics for female infertility found that Korean women preferred herbal medicine as an alternative treatment, citing higher pregnancy success rates and better outcomes compared to other methods (Hyun et al., 2024). This aligns with the findings of Noh et al., who reported that Korean women with infertility also used plant-derived natural products with positive results. Such natural therapies are increasingly regarded as potential alternatives to conventional infertility treatments (Noh et al., 2020).
Despite the unsafe and sometimes unhygienic nature of certain treatment practices, women with infertility often overlook these risks due to desperation. A study in Turkey found that such women frequently relied on traditional methods, including the use of specific foodstuffs, prayers, and the consumption of herbal remedies (Emül et al., 2024).
Another interesting finding in Turkey revealed that women with infertility combined different management approaches to attain pregnancy, with the commonest being changes in sexual activity, dietary habits, and the performance of certain religious rituals (Taner & Güneri, 2023).
In China, the difficult experiences faced by women with infertility often drive them to seek alternative treatment modalities. Beyond causing desperation, infertility negatively impacts their overall health and social life. However, many women reported positive outcomes after using nonorthodox approaches to address infertility (Saeed & Liu, 2022).
An interesting finding is that the experiences of infertility among Iranian women are similar to those in other countries. Despite advancements in assisted reproductive technologies, many Iranian women still turn to complementary and alternative medicine (CAM), including herbal preparations, acupuncture, prayers, and vows, in the hope of achieving successful outcomes (Azimi-Nezhad et al., 2022).
In Iran again, women with infertility expressed the desire to complement conventional treatment with educational, informational, psychological, spiritual, counselling, and supportive interventions that align with their cultural values and personal needs (Sharifi et al., 2021; Sharifi & Roudsari, 2022).
Notably, women with infertility encounter similar psychosocial challenges across contexts, and when conventional treatments fail, many resort to alternative options. Frequently, they combine herbal remedies, concoctions, and other traditional practices, often engaging in healer shopping without fully considering potential risks, which may compromise their health.
Again, the pursuit of diverse treatment modalities by women with infertility reflects medical pluralism, as they seek and utilize multiple approaches in their quest for a solution. However, this practice carries important implications for clinical assessment, diagnosis, and treatment, since many women present late to healthcare facilities with complications arising from the excessive use of concoctions and herbal remedies.
Strengths and Limitations
Limited research has examined complementary management of female infertility in the African context, hence the inclusion of similar literature from other geographical areas. This review addresses that gap by providing insights to inform clinical practice and policy while underscoring the need for culturally appropriate interventions. Nonetheless, its findings are not widely generalizable, and variations in complementary approaches across studies hinder direct comparisons.
Implications/Recommendations
Nursing Practice
By integrating evidence-based CAM approaches, fertility healthcare providers can develop holistic care plans that incorporate complementary and alternative therapies while remaining culturally sensitive.
Research and Policy
Future research should focus on clinical trials to evaluate the efficacy, safety, and mechanisms of CAM interventions in African women with infertility. Additionally, there is a need to incorporate validated CAM therapies into national health insurance schemes.
Education
Nursing and midwifery curricula can incorporate evidence-based CAM content, preparing future practitioners for culturally responsive infertility care.
Conclusion
Emerging evidence suggests that women facing infertility adopt diverse health-seeking strategies influenced by psychosocial stressors, advancing age, and prolonged childlessness. These strategies may include biomedical care, traditional medicine, complementary and alternative medicine (CAM), and religious or spiritual practices, the latter being the most common coping mechanism. Despite potential risks which may be linked to certain traditional practices, many women persist in using them in their quest to overcome infertility.
Footnotes
Acknowledgment
The authors would like to acknowledge all authors whose work has been referenced and the open-access resources (databases and journals) that facilitated the review process.
ORCID iDs
Author Contributions
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All data presented in this review are within the manuscript.
