Abstract
Introduction
Rural nursing programs encounter obstacles in providing nursing education opportunities relevant to the escalating needs of rural healthcare. Rural nursing programs often experience limited clinical placements, a stressed and burned-out rural nursing workforce, and difficulty finding nursing preceptors. Moreover, students studying in rural nursing programs experience increased travel, financial and social burden, and have less access to resources and support from their university. There is limited research giving voice to rural nursing students’ experience and their suggestions for solutions.
Objective
The purpose of this study was to understand the learning challenges of and potential solutions for baccalaureate nursing students attending a rural university.
Methods
This is a descriptive qualitative study using photovoice methodology. Participants captured two pictures of things in their school surroundings or personal life that created learning challenges in rural nursing education, and two pictures of potential solutions to these challenges. Participants titled each picture and, using guided questions provided by the researcher, wrote a short reflection of what the photos represented.
Results
Guided by empowerment education for critical consciousness and using Braun and Clarke's thematic analysis and Oliffe et al.'s layered photograph analysis, two overarching themes emerged: access to resources and clinical learning. Findings highlight financial, academic, and accessibility barriers in rural nursing programs as well as participant-determined solutions that could enhance learning experiences, student well-being, and retention in the rural healthcare workforce.
Conclusions
This study identified targeted resources for nursing students attending a rural nursing baccalaureate program to support their learning, wellbeing, and growth into graduate nurses. This study also identified areas for future research to explore nursing student experiences across rural and urban institutions and develop effective learning support strategies for rural nursing education.
Keywords
Introduction
Historically, rural communities in Nova Scotia have been, and continue to be, underserved by healthcare providers, resources, and programs, which impacts the educational opportunities for students studying in rural nursing baccalaureate programs (Foster et al., 2021). Geographically, rural communities are defined as areas where 10,000 or fewer people live outside the commuting zone of larger urban centers (du Plessis et al., 2001). Often, rural nursing programs have limited clinical placements, a stressed and burned-out rural nursing workforce, and an inability to find nursing preceptors (Ben-Ahmed & Bourgeault, 2022; Nelson & Salami, 2021). Moreover, students studying in rural nursing programs experience increased travel, financial, and social burdens but have less access to resources and support from university administration (Bradley et al., 2020; Hays et al., 2021). Challenges in educating and preparing future rural nursing professionals relate to limited clinical placements and reduced access to specialized training, leading to gaps in hands-on experience, which could negatively impact the health of rural populations (Ben-Ahmed & Bourgeault, 2022; Nelson & Salami, 2021). As a result, new graduates may feel underprepared to manage complex cases, particularly in rural settings where healthcare resources are scarce. This lack of preparedness can contribute to higher turnover rates, workforce shortages, and poorer health outcomes for rural populations (Ben-Ahmed & Bourgeault, 2022; Wilson et al., 2020).
The purpose of this study was to identify and understand the current learning challenges faced by rural nursing students and their suggestions for solutions. This knowledge can inform creative strategies to improve the delivery of nursing education in rural Nova Scotia, Canada. Promoting meaningful and contextual change in undergraduate nursing education may improve the recruitment and retention of graduate nurses to work in these rural communities (Campbell et al., 2022), and who are better prepared for the challenges of working in a rural healthcare environment.
Review of Literature
Studies of facilitators and barriers to rural nursing education are of stand-alone rural and satellite university campuses. Satellite campuses are located remotely from the main university campus; thus, the facilitators and barriers are comparable to those of rural universities (Hays et al., 2021). Students attending rural nursing education programs were more likely to be first-generation students, meaning they were the first in their families to attend university. They were also more likely to be mature-aged (>30 years) and balancing family obligations with school and nursing placements. Rural and satellite campus locations offered opportunities for remote students to go to school closer to work or home, allowing them to live at home, and improved financial accessibility because it was more affordable to live in rural areas (Boehm et al., 2017; Hays et al., 2021). However, this student population faced additional barriers as there was less support from the main university campus administration, resulting in a lack of educational resources and services (Hays et al., 2022).
In addition to the campus experience, rural nursing programs also include clinical placements. Bradley et al. (2020) explored rural clinical placements for nursing and other health professional programs. These students reported positive aspects of their rural clinical placement experience, such as enjoyment of the rural environment and community, positive and friendly work and learning experiences, increased depth and breadth of the clinical environment, and increased practice opportunities. However, they also identified barriers consisting of additional financial costs due to needing a place to stay, increased money spent on gas for travel, and social isolation. Students also described feeling inadequately prepared for and lacking communication about clinical placements, making planning travel and managing schoolwork difficult, and negatively impacting their mental and physical well-being (Bradley et al., 2020).
Rose et al.'s (2023) study of recent nursing graduates indicates that positive experiences in rural nursing programs can improve the retention of nursing graduates to work in rural settings. In their study, rural early career nurses reported that assistance with accommodation and transport, social gatherings to enhance connection, sufficient orientation, and increased frequency of contact with clinical facilitators and multiple mentors would have improved their education experience and capacity in the workplace. They also valued the prioritization of clinical education across diverse topics and greater involvement in choosing rotations and clinical areas. Furthermore, Campbell et al. (2022) also found that satisfaction with nursing school clinical placements in remote locations was associated with consideration of working rurally or remotely after graduation, showing the importance of facilitating positive student experiences in rural clinical environments for hiring nurses in rural healthcare.
Nurses have been identified as the backbone of rural healthcare in Canada (Martin-Misener et al., 2020; Wilson et al., 2020). In rural settings, nurse practitioners and nurses often assume more primary care, health promotion and prevention, rehabilitation, and palliative care responsibilities, with declining physician and other healthcare professional recruitment (Martin-Misener et al., 2020; WHO, 2024). The conditions in rural healthcare not only impact patient outcomes but also create unique challenges for nursing education and training. Understanding that nursing students studying and working in rural areas face unique barriers brings attention to the need to seek rural nursing students’ voices to identify practical solutions. However, little research has captured the voice of nursing students attending rural universities and undertaking rural clinical placements in Nova Scotia and Canada. The research question asked, What learning challenges do rural nursing students face in rural nursing education programs, and what are the potential solutions? Postsecondary nursing programs must prepare future nursing students to work competently within rural settings (Martin-Misener et al., 2020).
Methods
Design
This is a descriptive qualitative study using photovoice methodology to understand students’ experiences attending a rural baccalaureate in nursing program. Photovoice is a qualitative participatory methodology, rooted in Freire's (1973) theory of empowerment education for critical consciousness (Wallerstein & Bernstein, 1988). Using photographs enables participants to identify their unique experiences and perspectives regardless of language, culture, or literacy (Sutton-Brown, 2014). Raising the voices of rural nursing students to identify their educational challenges and share ideas for solutions empowers them to become agents of change in their own learning.
Research Question
What are the learning challenges faced by rural nursing students, and what are their suggestions for solutions?
Sample
After receiving St. Francis Xavier University Research Ethics Board approval, purposive sampling was used to recruit participants from the baccalaureate program in June 2024, from the fourth and seventh semesters of the Accelerated Nursing Program (six semesters taken in two calendar years). In September 2024, recruitment was from those entering the fifth and seventh semesters of the regular 4-year degree program. This participant population was chosen as these students are expected to have gained sufficient experience throughout their three or more semesters of nursing courses to provide valuable insight into this phenomenon. They were also the most accessible group, as students in their final semester are in clinical placements only and are not on campus to participate. The inclusion criteria included the ability to speak, write, and comprehend English, having a personal device to take photographs, being currently enrolled in the nursing program, and having access to the internet and email. Exclusion criteria included nursing students in semesters one through three, as they would not have had enough experience in the nursing-specific aspects of the program to provide meaningful data.
Recruitment was through digital posters and introductory videos shown in nursing classes, posters in the hallway, and emails to the student listserv. Those interested and who also met the inclusion criteria emailed the first author researcher and were provided with an invitation to participate that included a detailed description of the study and a consent form. Table 1 is a summary of the participants, including some demographics.
Participants Demographic Information.
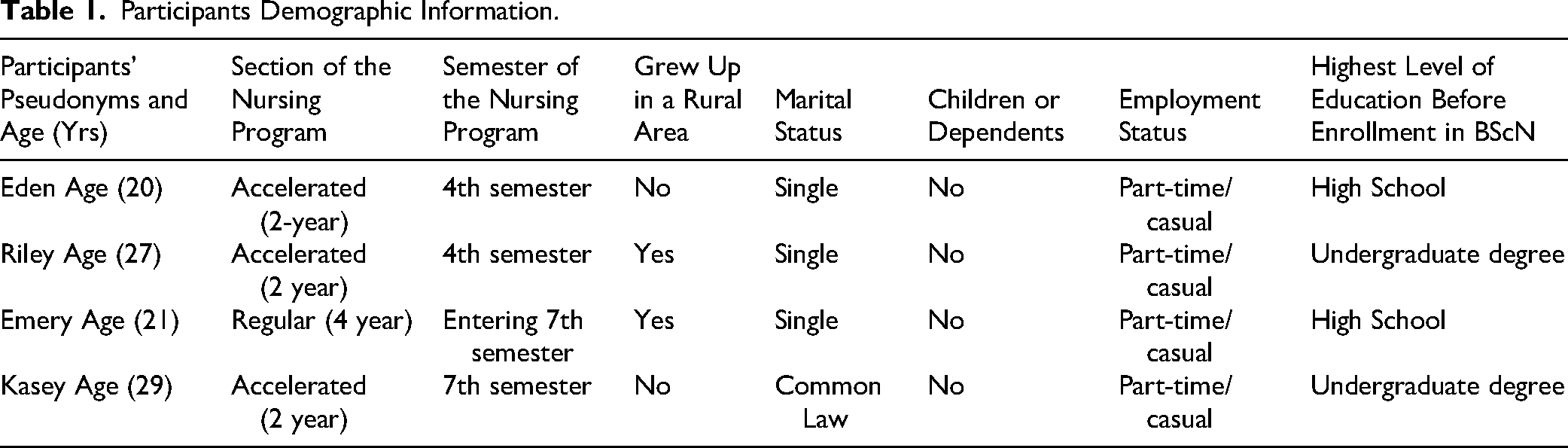
The participants are representative of students in a rural nursing program in Nova Scotia, as rural universities in Nova Scotia predominantly offer undergraduate programs, given the resources required to offer graduate studies, and most students enter an undergraduate program soon after graduating from high school. Although there are students with children enrolled in the undergraduate nursing program, their numbers are significantly smaller compared to those without children; thus, these participants represent the most common demographic of rural undergraduate nursing students.
Although the sample was somewhat homogenous, several strategies were integrated to address unintentional sampling bias. First, the research problem was defined to address a gap in participant voices, putting them at the center of the data collection. Second, to encourage diverse representation, the study utilized a variety of recruitment strategies, making it available to all students enrolled in the nursing program who had completed more than three semesters.
Data Collection
Four participants agreed to participate in the study: three in the accelerated program, recruited in June 2024, and one in the regular stream, recruited in September 2024. The photovoice method is time-consuming, which limited the number of interested participants, and the university timelines for the first author researcher to complete the study meant that recruitment did not extend beyond the fall semester. However, according to Wang and Burris (1997), the goal of photovoice is to encourage in-depth reflection and conversation among participants and in data analysis; therefore, this sample size was ideal and realistic.
After receiving the signed consent form by email, the first author researcher met virtually with each participant to explain the data collection process. Participants were provided with an instruction manual with detailed instructions and guided questions (Appendix 1) to answer by email. The instructions included that participants were to take two photographs of things in their surroundings or personal life that created learning challenges in their rural nursing education, and two photographs of potential solutions. Participants were given 2 weeks to email the photographs, including a title for each photograph, and answers to the guided questions. Participants answered the guided questions about the photographs in an email exchange with the first author researcher, creating a transcript for analysis. The first author researcher manually encrypted email exchanges and used multi-factor authentication on their email account to secure the data exchange. Pseudonyms are used to protect the participants’ identities.
To address any unintentional bias during the data collection process, a standard script and introduction to photovoice data collection processes and safety and ethical considerations were used based on established protocols (Wang & Burris, 1997); additionally, using guiding questions about the photographs that were neutral and open-ended encouraged participant autonomy to take photographs representative of their perspectives and contextual realities.
Data Analysis
The researcher combined Oliffe et al.'s (2008) layered analysis and Braun and Clarke's (2006) thematic analysis to facilitate a simultaneous analysis of photographs and text, thereby guiding a comprehensive exploration of participants’ perspectives and their collaboration on thematic themes within the data (Mooney & Bhui, 2023). Using Braun and Clarke's (2006) 15-point checklist, written text data collected from each participant's email transcript were analyzed using an inductive, reflexive thematic analysis. After reviewing and coding each participant's email transcripts separately, the researcher cross-compared the participants’ email transcripts with their titled photographs, grouping common codes into thematic patterns. The eventual themes were then confirmed with the other two research team members and study participants (Mooney & Bhui, 2023).
Specifically, the photographs were analyzed using Oliffe et al.'s (2008) layered analysis approach, including preview, review, cross-photo comparison, and theorizing for photograph analysis. The preview process involved viewing and linking each study participant's photographs with their answers to the questions from their emails. The review process involved recording similarities and inconsistencies between the visual and written data, outlining directions for theoretical sampling, and thoughts and decisions related to coding and theme development. The researcher viewed photographs in a slideshow in the cross-photo comparison analysis phase. Then, each photograph was sorted into folders of thematic categories based on the titles provided, and reflective memos were written about the photographs, and answers to questions were provided via email. The first author researcher identified themes and subthemes from the relationships among categories connecting written text and visual data, organizing them using a thematic map to visualize relationships and patterns within the data. Theoretical sufficiency was achieved with the data rather than saturation, which is aligns with Braun and Clarke's (2006) and Oliffe et al.'s (2008) theoretical approach to data analysis using photovoice. In other words, the themes are supported by the data rather than reaching a point of no new emerging themes.
To address any unintentional biasing during the data analysis process, the first author researcher employed reflexivity through memoing and member checking, as well as blending Braun and Clarke's (2006) thematic analysis of text and Oliffe et al.'s (2008) layered analysis of the photographs to enrich critical inquiry, capture the contextual nuances of participants’ data, and to minimize implicit potential power imbalances of researcher data interpretation during the analysis process (Wang & Burris, 1997). Specifically, trustworthiness and reliability were addressed through frequent group discussions with the other two researchers to confirm the themes and subthemes. Journaling was used during analysis to ensure that the researcher's decisions on themes and subthemes were recorded and reflected the participants’ experiences. The researcher engaged in member checking via email exchange to confirm the interpretation of each participant's data and that the themes and subthemes accurately represented their experiences.
Ethical Considerations
Signed consent was obtained prior to involving the participants in the study. As part of the information and consent package, participants were informed that participation was voluntary, and they could withdraw at any time without repercussions to their enrollment in the baccalaureate program. Participants were anonymized using pseudonyms, and only the first author researcher knew their identity. All data was exchanged via encrypted email and is stored on a secure server requiring two-factor authentication.
Results
Demographic Characteristics
Four nursing students participated in the study, three enrolled in the accelerated program and one in the 4-year program. Two participants were in the fourth semester, and two were in the seventh semester of the program. The participants had an average age of 24.25 years.
Thematic Findings
Analysis revealed two themes and subthemes that capture the challenges and potential solutions participants identified in their rural nursing education program. The theme resource access includes the related subthemes of inaccessible spaces and services, and creating meaningful campus resources. The second theme, clinical learning, includes the subthemes of far and few placements and opportunities, and developing alternative strategies. Participants submitted 16 photographs; however, only a select few are included in this article, along with excerpts from the email transcripts.
Theme 1: Resource Access
Challenges
The subtheme inaccessible spaces and services captures the challenges participants identified with accessing resources such as suitable study spaces, food services, and academic assistance. They perceived these as negatively impacting their learning, financial security, and mental well-being. Figure 1 is a photograph of a well-known study space on the university campus that students like to use because of the natural lighting and comfortable seating.

A very nice building with very little access.
Two participants in the accelerated program submitted pictures of this space and described limited access in the summer months, which disrupted study routines. Eden explained, “The entire building locks at 5 pm in the summer…the restrictions make it hard to establish a study routine outside class hours.” Riley wrote, “On a Sunday morning in June, the day before our final exam worth 45% of our grade, this building and the library were closed.” Riley also mentioned how other campus spaces were less suitable, “The nursing building… was not air conditioned and under construction, so it was not a comfortable learning environment.”
Additional challenges participants identified were a lack of tutors and the availability of course professors. Emery described “There was none or only one [tutor] available for the course, and the costs were expensive” when explaining difficulties meeting with professors due to office hours and class overlap, and that affordable tutors created obstacles to accessing academic support.
Participants identified an increased financial burden due to a lack of access to campus food services, the gym, and health facilities because they have reduced hours or are closed in the summer months. For example, Riley indicated, “Why are we paying full tuition as if we had access to all of the same amenities as the regular school year?” Riley also described “When we do not have time to meal prep our lunches, which many of us don’t, as many of us have jobs or children/families, we are forced to leave campus during our short breaks and purchase food options” because campus food services had reduced hours during the summer months. Food service for nursing students was also an issue for Emery during the regular fall and winter semesters because no food was available before an early clinical rotation, an issue particular to nursing students.
Figure 2 is Emery's photograph of eating a bagel before clinical to depict food inaccessibility for nursing students despite having paid for a campus meal plan. Emery explained, “This impacts my learning because I am spending my money on food rather than using it on things that would be beneficial to my learning.”

Takeout.
Eden highlighted additional financial burdens associated with clinical placement expenses for rural nursing students, “Added stresses associated with a small town/rural university, including almost zero public transportation services, high cost of foods, increased tuition, especially for out-of-province students [and] worries related to transportation to and from clinical placements.” Eden connected these extra costs to learning outcomes: “It can be difficult to focus on anything in class if you are always hungry or worrying about dinner.”
Solutions
Participants identified solutions for accessing resources, such as increasing access to food resources on campus, learning spaces, and creating opportunities for peer connection and mentoring for academic support.
Figure 3 is Eden's photograph depicting the benefits of extended nursing lab hours for enhancing learning opportunities. Eden described, “This increased flexibility is really helpful for students who have commitments outside of class time and may not be able to utilize open classrooms during their normal hours.” Eden also explained, “Being able to ask for these things [open lab spaces] from my professors has made a big difference in academic performance, and in helping students know that they have support from some administration,” illustrating the positive impact of professor advocacy that led to this extended lab access, reinforcing faculty commitment to student success. Emery proposed other academic support, “a solution could be to have study groups or tutoring available in the campus library for nursing students.” In addition to using the library, Emery explained the benefits of peer tutoring, “It is easier to understand when working one-on-one with a student who has already taken the course…There could be tutors at certain times of the week.”

An open nursing lab.
For access to food and to reduce student costs, Riley proposed, “A solution would be to have an affordable dining option open on campus for students who are in classes all year round.” Eden suggested expanding an existing campus food resource program that provides free food to students and making it more well-known to students to help alleviate food insecurity and offset other expenses, such as travel costs for clinical placements. Eden explained the positive effect on student learning: “Reducing the cost of food security can lead to better concentration levels in school, which would enhance education delivery…knowing that resources like this exist on campus is important for students.”
In addition to accessing food for sustenance, Riley's photograph was of a dining table set with food and drink, to illustrate the importance of social connections in a rural nursing program. Riley explained, “In the summer terms, when there are very few students on campus or in town, we rely on each other for much-needed peer support, socialization, and work collaboration…we would come together and make food and socialize, giving us a sense of togetherness.” These gatherings created an opportunity to connect outside of class, manage stress, and improve mental well-being by giving students space to discuss academic and personal challenges.
Theme II: Clinical Learning
Challenges
The subtheme of far and few placements and opportunities captures all four participants’ experiences of challenges with clinical placements within a rural nursing program. These challenges include the time to travel more than 60 kilometres for clinical placements, and the cost of gas, food, and lodging. Two participants discussed how geographically dispersed clinical placements were, as there is only one local hospital and a few clinics that nursing students can attend. Riley explained, “travel and housing are at the student's expense despite it being one of the most expensive programs offered at the university,” indicating that tuition fees for the nursing program do not cover travel expenses, despite clinical placements being mandatory in the program. As well, Riley discussed inequitable financial burden as those with cars are assigned to more distant clinical placements, where those without vehicles are assigned more locally. Participants also indicated that their clinical placement details often came at the last minute, making a study schedule and planning for expenses and transportation more difficult and stressful.
In addition to challenges related to travel costs and clinical scheduling details, participants also identified large clinical groups and access to clinical instructors as negatively impacting their clinical learning experience. Kasey took Figure 4, a photograph of wild Canadian geese in a field, to humorously illustrate their experience of waiting for an instructor to supervise clinical practice and being in a large clinical group with 7–8 students and only one instructor.

The clinical group waiting for the instructor to be ready.
Kasey explained, “You end up waiting around, being delayed or missing out on skills…I felt like my learning of practical skills was delayed.” Emery shared a similar experience with a lack of access to clinical instructor supervision: “I feel as though my opportunities to practice any skills were limited…this has left me feeling anxious heading into clinical settings.” Participants also identified overcrowding of students in one unit as impacting their learning. Kasey shared, “16 students on one floor that only had approximately 22 beds.” Emery explained, “We have huge groups on the same unit because there is nowhere else to go… because of this, there is less opportunity to learn skills…I feel unprepared for certain things because I have only read about them.”
Solutions
Participants suggested solutions for clinical learning that included smaller clinical groups with more than one clinical instructor and scheduling staggered clinical rotations to ensure fewer nursing students present on a unit, and assistance with costs and transportation from the university. To address the financial burdens of travel expenses to remote clinical placements, Riley suggested that the university provide supportive resources as “Some forms of support could be gas cards, short-term overnight housing options or forms of transportation/carpooling organized by the university.”
Figure 5 is Kasey's photograph of Smarties sorted into colors and smaller piles representing fewer students for each clinical instructor.

Smaller groups.
Kasey explained, “If you had two instructors working together in one group, we wouldn’t require any more meeting space, but I think students would feel more supported in an overwhelming area.” As well, “Stagger having groups on the unit at one time to prevent or lessen the crowding to alleviate students’ feelings of being a burden during clinical placements, helping them feel more accomplished, and improving the unit's overall productivity.” Participants also suggested increasing the use of the nursing school's simulation lab for clinical practice, as indicated by Emery's photograph of the SIM lab and explained that simulation learning offers additional hands-on practice, helping students feel more confident and prepared for clinical placements. “I would feel a lot more prepared heading into fourth year if I had experienced more hands-on prior to this time.” Participants connected these solutions to improved clinical learning for rural nursing students.
Discussion
The study findings revealed two themes: resource access and clinical learning. These themes include challenges and proposed solutions to improve the learning experiences of nursing students enrolled in a rural nursing program, as well as recommendations for future research.
The theme resource access highlights how rural nursing students face significant barriers accessing campus resources, particularly during the summer semester. Limited access to health facilities, gyms, and study spaces, with food services and academic assistance being particularly inaccessible year-round. This inaccessibility is echoed in studies that have identified limited administrative and academic support, as well as resource availability, for students in rural nursing programs (Bydalek et al., 2020; Cockerham et al., 2021; Grant-Smith & de Zwaan, 2019; Lamswood et al., 2024). The availability of learning support, including nursing-specific learning environments and collaborative peer learning opportunities, particularly peer tutoring, has been shown to enhance the critical thinking and decision-making skills required for nursing practice (Eskiyurt & Ozkan, 2024; Saiboon et al., 2021; Wei et al., 2024), as well as supporting school and life balance and learning engagement (Bally et al., 2023). However, these supports are often lacking in rural nursing programs (Bahar et al., 2022; Hays et al., 2022; Nilsson & Lindberg, 2024). To address challenges caused by a lack of academic support, rural nursing programs could consider allocating funding for structured peer tutoring programs, establishing dedicated nursing learning spaces, and increasing opportunities for professor-student interactions. Furthermore, the influence of seasonality on resource accessibility remains underexplored in nursing education research. Given that reduced access to resources during the summer semester was a significant finding of this study, future research should investigate seasonal variations in resource availability across rural and urban nursing programs to develop targeted solutions that promote equity in student support.
Additionally, affordable and convenient on-campus food services are a year-round challenge, with nursing students being impacted more than other student populations due to clinical placement factors. Expenses are increased and are linked to reduced academic performance, concentration, and retention rates (Bydalek et al., 2020; Cockerham et al., 2021; Grant-Smith & de Zwaan, 2019). Proposed solutions to expand affordable, convenient food options on campus, extending service hours of campus meal halls to accommodate clinical schedules, and increasing support for campus food resource centers may mitigate food insecurity and promote equitable learning conditions among rural nursing students (Bydalek et al., 2020). Future research should explore the intersection of food accessibility and financial instability in rural nursing education to guide policy development.
The combination of learning difficulties, financial instability, and uncertainty surrounding clinical placements negatively impacted participants’ mental well-being. Nursing students often experience heightened levels of stress and mental health struggles that can affect academic performance and personal well-being, leading to long-term professional consequences, including burnout and increased nurse turnover rates (Brown et al., 2024; Lavoie-Tremblay et al., 2021). Addressing mental well-being and stress issues among rural nursing students may require a multifaceted approach. This approach could include developing peer support networks, routine mental well-being screenings, and expanded access to on-campus counseling services to foster a resilient student community (Brown et al., 2024; Lavoie-Tremblay et al., 2021). Broader institutional collaboration, such as workshops offered by universities to support students in professional programs and managing heavy study loads, may be helpful in improving nursing students’ well-being and facilitating their transition into future careers (Lavoie-Tremblay et al., 2021).
The theme of clinical learning captures participants’ challenges within the rural clinical settings, particularly how large student groups on small hospital units limit hands-on skill development, which contributes to feelings of being burdensome and unproductive. This challenge aligns with DiMattio and Hudacek's (2020) findings, which suggest that feelings of unproductivity and overcrowding in clinical environments are associated with lower retention rates and dissatisfaction among nurses. Research supports smaller instructor-to-student ratios and staggered scheduling of clinical are strategies that improve clinical supervision and build students’ confidence and competence (George et al., 2020). Smaller clinical groups also enhance critical thinking, clinical decision-making, and self-confidence (Eskiyurt & Ozkan, 2024; Saiboon et al., 2021; Wei et al., 2024). Lower student-to-instructor ratios enable more personalized feedback and guidance, thereby improving clinical competency outcomes (Zhang et al., 2022).
Another solution was to expand simulation-based learning to provide additional opportunities for skill development. High-fidelity simulation training is widely recognized as an effective method for enhancing clinical judgment, critical thinking, and confidence in nursing students (Jefferies, 2020; Radford, 2018). Integrating more simulation experiences into nursing curricula could help alleviate the challenges associated with clinical placements, particularly for students in rural programs with limited access to diverse clinical experiences and resources. However, funding limitations and a lack of resources are common barriers to the effective expansion of simulation learning in rural nursing education; thus, funding initiatives will be important for enhancing simulation learning in such rural programs (Jefferies, 2020; Radford, 2018).
Limited local clinical placements imposed financial and logistical stress, echoing studies that found additional costs for housing, food, and travel expenses for rural nursing students (Grant-Smith & de Zwaan, 2019; Hays et al., 2021; Lamswood et al., 2024). Financial strain from clinical placements has been linked to reduced academic performance, student attrition, and increased stress (Grant-Smith & de Zwaan, 2019).
Potential solutions could include compensation and support for travel expenses through gas cards, organized carpooling, shuttle services, and earlier placement notifications (Grant-Smith & de Zwaan, 2019; Wines, 2016). While participants did not explicitly mention financial aid, research suggests that expanding nursing-specific scholarships and providing financial literacy workshops could support rural nursing students (Grant-Smith & de Zwaan, 2019). Lamswood et al. (2024) suggest paying nursing students for participation in clinical placements to alleviate financial stress. Future research exploring the financial instability of rural nursing students in greater depth, centering student voices in discussions about meaningful financial and resource-based support strategies, would be beneficial.
The findings highlight how limited access to campus resources, academic supports, and financial strain create barriers for rural nursing students, ultimately impacting their learning and well-being. Addressing these challenges through targeted institutional support, such as expanding food and academic services, as well as peer-based initiatives, could help promote equity and success in rural nursing education.
Strengths and Limitations
Methodology
Using email to relay answers to study questions enabled participants to engage in the study at times suitable for them; however, this limited the capture of nonverbal cues and vocal inflections that may have provided additional insight into the participants’ experiences. There is also a gap in time between sending and receiving emails that may have impacted the flow of dialogue. However, this gap allowed participants time to reflect before answering the researcher's questions.
Context
The small-town rural university community may have also impacted privacy concerns, given that the participants and researchers are known to each other, which may have impacted the extent of what participants shared.
Recruitment
The study was conducted over the summer months, which made it more challenging to recruit third- and fourth-year students from the 4-year stream who were off for the summer. The compressed timeline for completing an honors research project in the nursing program, combined with the time required and volume of data associated with the photovoice methodology, meant recruitment could not continue into the regular fall semester. As a result, some student voices may have been underrepresented, and the findings may be more related to accelerated or condensed nursing programs. For example, access to financial support and university resources may differ for year-round study versus the traditional September to April academic year. Future studies to include more participants from the 4-year stream may provide other insights into the rural nursing student experience.
While the participants are representative of most students in a rural nursing baccalaureate program, and recruitment was open to anyone enrolled in the nursing program who wanted to participate, diverse groups were not identified in this study. Future studies could focus recruitment on more diverse groups, such as First Nations or Black Nova Scotian students, to gain specific insights into the rural nursing student experience from diverse perspectives.
Implications for Practice
Moving forward, rural universities should focus on creating targeted, supportive resources for nursing students to support their learning, well-being, and growth into graduate nurses. Universities should consider improving access to health, food, and academic resources to align with nursing students’ clinical schedules and extend services into the summer months.
Rural nursing programs should reduce the ratio of students to nurse educators and stagger clinical placements to improve students’ clinical learning, as well as expand simulation learning as another way to develop clinical competence.
The rural universities should consider travel reimbursement or a shuttle service to help students attend clinical placements located some distance from the university. Communication of clinical placements should be timelier to allow students time to plan time away from campus and organize carpooling. Efforts to address the identified barriers may improve the rural nursing students’ experience and learning, potentially helping with recruitment to rural healthcare after graduation.
Conclusion
This study aimed to identify learning challenges faced by nursing students in a rural nursing program and explore potential solutions to improve nursing education delivery in rural settings. This qualitative investigation used photovoice and was guided by the theoretical perspective of empowerment education for critical consciousness (Wallerstein & Bernstein, 1988) and education empowerment theory to elevate the voices and experiences of rural nursing students using photovoice, empowering them to lead positive change in nursing education delivery (Freire, 1973; Sutton-Brown, 2014). The two themes, resource access and clinical learning, emerged as contextual realities in rural nursing education that created learning challenges and where solutions are possible.
A lack of access to campus food services, study spaces and academic assistance negatively impacted their study routine, learning experience, and increased financial burdens. Solutions include enhancing campus food resources, creating opportunities for peer learning and professor interaction, and enhancing mental well-being resources on campus. The wide geographical range of clinical placement locations and overcrowded and restricted clinical learning environments caused challenges with clinical learning. These conditions increase financial burdens and stress, which impact developing clinical skills and feelings of preparedness for future nursing practice. Creating smaller clinical groups, staggered scheduling, increasing the use of simulation learning, and increased communication from the university with the provision of financially supportive resources emerged as solutions to reduce the burdens and stress on nursing students in rural nursing baccalaureate programs.
Future research is needed to explore further nursing students’ experiences across rural and urban programs to gain more insights into how rurality impacts access to resources, specifically food, financial stability, and mental well-being.
Footnotes
Acknowledgements
The authors would like to thank the students who participated in this study.
Ethical Approval and Consent to Participate
This study was approved by the St Francis Xavier University Research Ethics Committee (Romeo number: 26928) on May 14, 2024.
All participants provided written informed consent prior to participating.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for the research project was provided by the Irving Oil Research Mentorship Award (undergraduate student research award # 26928).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Appendix 1: Guided Questions about the Photographs
Please answer these questions about the pictures you took representing What title would you give this picture? Tell me about this picture you have taken. What about this picture created/is creating learning challenges for you in rural nursing education delivery? How has this impacted your learning in rural nursing education? Is there anything else you want to say about what this photograph represents or means to you? What title would you give this picture? Tell me about the picture you have taken. What about this picture represents/is something that you perceive as a potential solution to learning challenges in rural nursing education delivery? How do you think what you represented in your photograph could be a potential solution to learning challenges in rural nursing education delivery? Is there anything else you want to say about what this photograph represents or means to you?
Please answer these questions about the pictures you took representing
