Abstract
Introduction
Patients awaiting heart surgery often experience reduced physical activity, leading to decreased muscle mass, strength, and endurance.
Objectives
This study aimed to evaluate the effects of cardiopulmonary pre-rehabilitation (CPPR) on physical performance, balance, and fear of falling (FOF) in candidates for coronary artery bypass graft (CABG) surgery.
Methods
This randomized clinical trial was conducted in 2022. Ninety-two candidates for CABG surgery were recruited and randomly allocated to two 46-person groups using block randomization with a block size of 4. Participants in the intervention group received a 1-month CPPR program consisting of Otago exercise, incentive spirometry, walking, and modification of lifestyle and cardiovascular risk factors. Physical performance, balance, and FOF were assessed before and after the intervention and 4 weeks after surgery. Data collection instruments were a demographic and clinical characteristics questionnaire, the Short Physical Performance Battery, Berg Balance Scale, and Falls Efficacy Scale-International. The validity and reliability of these instruments have been established in previous literature and were also confirmed in the present study (Cronbach's alpha > 0.85 for all).
Results
No significant differences were observed between the groups at baseline regarding the mean scores of physical performance, balance, and FOF (p > 0.05). Following the intervention, the CPPR group demonstrated significantly greater improvements in physical performance (p < 0.001) and balance (p < 0.001), and a significantly greater reduction in FOF (p < 0.001) compared to the control group. These significant between-group differences were maintained at the 4-week postoperative assessment.
Conclusion
This study concludes that CPPR is effective in significantly improving physical performance and balance and significantly reducing FOF among the candidates for CABG surgery. Therefore, it can be used to prepare the candidates for CABG surgery and improve postoperative outcomes.
Keywords
Introduction
The most common cardiovascular disease (CVD) is coronary artery disease, in which lipids accumulate in the subendothelial space (Del Buono et al., 2021). A report by the World Health Organization in 2018 showed that 43% of all deaths in Iran were related to CVD (Khademi et al., 2019). More than 80% of CVD-related deaths occur among individuals above 65 years and CVD-related deaths are the leading cause of death in older adulthood (O’Neill & Forman, 2021). Coronary artery bypass graft (CABG) surgery is one of the most principal treatments for CVD (Ghorbani & Bahramnezhad, 2020). Each year, more than eight million CABG surgeries are performed around the world. Moreover 40,000 open-heart surgeries are annually performed in Iran, 50%–60% of which are CABG surgery (Askari & Mehdizadeh, 2019). Although global mortality from these complications has decreased in recent years, it is still strongly associated with patient complications and leads to prolonged hospitalization, which affects patients, families and increases medical costs for the family and the health system (Perelló-Díez & Paz-Lourido, 2018). The prevalence of coronary artery disease and its complications in the country has caused death, disability, and incapacity of a large part of the country's productive forces, especially in the best years of job productivity and ultimately reduced production and increased medical costs (Pakdaman et al., 2020).
Despite great clinical advances in cardiovascular surgeries, the prevalence of postoperative complications is still as high as 30% and hence, patients with these surgeries have poor postoperative quality of life, physical performance, and lifestyle (Mao et al., 2020). Postoperative reduced mobility and physical performance and the adverse physiological and metabolic effects of surgical procedures reduce the function of the cardiovascular, respiratory, gastrointestinal, and musculoskeletal systems and increase insulin resistance (Kehler et al., 2017). These problems put patients at risk for thromboembolism, pneumonia, atelectasis, respiratory failure, and poor surgical wound healing, and reduce physiological reserve by 40% (Scheede-Bergdahl et al., 2019). Besides, reduced physical performance, weakness, and fear of falling (FOF) restrict patients’ postoperative mobility, prolong length of hospital stay, and increase the risks of infection and re-hospitalization (Tazreean et al., 2021). However, relatively little emphasis has been placed on patient optimization in the preoperative period. Since there is a waiting period before surgery for most elective procedures, this period provides an opportunity for pre-rehabilitation and targeted intervention to improve postoperative outcomes (Sharon et al., 2023).
Rehabilitation is one of the most important strategies to improve patients’ conditions after CABG surgery. It refers to a set of interventions to improve performance, reduce disability, and promote coping to environmental changes (Negrini et al., 2022). Postoperative rehabilitation reduces postoperative complications by 30%, shortens the length of hospital stay, and reduces re-hospitalization rate (Barberan-Garcia et al., 2018). Rehabilitation strategies are mostly used after surgeries, while postoperative complications such as loss of appetite, fatigue, pain, depression, and pulmonary problems interfere with postoperative rehabilitation and lifestyle modification (Waite et al., 2017).
Population growth, aging, and better access to healthcare services have increased the request for surgical services and thereby, have increased the waiting time for surgeries (Yau et al., 2021). Patients in the waiting list for elective clinical procedures tend to have limited physical activity during their waiting period, and therefore, it is very likely to have poor postoperative muscle mass, muscular strength, stamina, and physical activity (Ko et al., 2018; Smith et al., 2019). Patients’ poor postoperative conditions and long preoperative waiting time for surgery have turned the preoperative period into an appropriate time for pre-rehabilitation interventions. Cardiopulmonary pre-rehabilitation (CPPR) may be associated with positive postoperative outcomes such as lower complication and death rates, faster recovery, and faster return to preoperative functional status (Sawatzky et al., 2014). Preoperative period is a good time for education about the modification of lifestyle and CVD risk factors because patients are not affected by the symptoms and concerns that occur after surgeries (Wagnild et al., 2021). CPPR includes a wide range of preventive measures which are implemented for the CABG surgery candidates to reduce the incidence or the severity of postoperative complications (Steinmetz et al., 2020). This intervention is a pre-rehabilitation program that can be delivered remotely. Providing care at home can reduce the number of patient visits to the treatment system and significantly reduce treatment costs (Furze et al., 2009). It includes physical and breathing exercises to improve balance and walking ability, improve cardiopulmonary capacity, shorten the length of hospital stay, and reduce the risk of fall and pulmonary complications (Myers et al., 2021). In recent years, preoperative physical exercise interventions such as Otago exercise and inspiratory muscle training were introduced to improve surgical outcomes, exercise capacity, and quality of life, and reduce post-CABG complications (Dastmanesh et al., 2019; Zhang et al., 2023).
Review of Literature
Several previous studies showed that pre-rehabilitation programs significantly reduced the length of postoperative hospital stay, the length of postoperative stay in intensive care unit, and the rate of postoperative complications, and improved maximum respiratory capacity and quality of life after surgery (Arthur et al., 2000; Boreskie et al., 2019; Marmelo et al., 2018; Waite et al., 2017). Nonetheless, there are limited pre-rehabilitation studies into physical and mental complications, nutritional interventions, and risk factor modification (Alshvang, 2018; Furze et al., 2009; Levett & Grimmett, 2019; McCann et al., 2019). Moreover, most studies into the effects of pre-rehabilitation were performed on patients with orthopedic surgeries, and there is limited evidence regarding the effects of pre-rehabilitation before CABG surgery on physical performance, balance, and FOF. This study sought to reduce these gaps. The aim of the study was to evaluate the effects of CPPR on physical performance as a primary, balance, and FOF as secondary outcomes among the candidates for CABG surgery.
Methods
Design
This randomized clinical trial was conducted in 2022. The candidates for elective CABG surgery in Tehran Heart Center and Imam hospital, Tehran, Iran, constituted the study population. These two centers were leading centers for cardiac surgeries in Iran. Sampling was consecutively performed and sampling criteria were an age of above 60 years, a waiting time of at least 4 weeks before CABG surgery, candidacy for elective cardiac surgery for the first time, ability to speak Persian, basic literacy skills, ability to use smartphone and social media, hemodynamic stability, no mental or learning disability, no physical limitation, and no participation in any pre-rehabilitation program. Exclusion criteria were hemodynamic instability and the need for emergency CABG surgery.
Sampling and Allocation
The output of the sample size calculation formula (Figure 1) indicated that 36 participants per group were necessary for the study. Sample size was increased to 46 per group in order to compensate probable withdrawals. Accordingly, 92 candidates for CABG surgery were recruited and randomly allocated to a control group and an intervention group via block randomization with a block size of 4. From the formula σ = 1.5, μ1 = 10.33, μ2 = 9.1 (Waite et al., 2017).
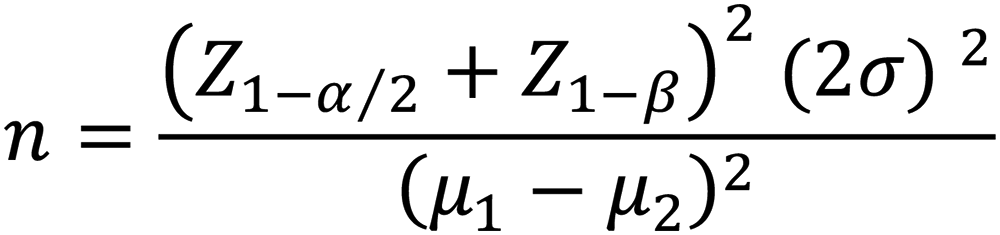
Sample Size Formula.
In this study, the samples were initially selected as available and then randomly assigned to the experimental and control groups. Since the participants in this study gradually entered the study, in order to avoid imbalance in the number of participants in the experimental and control groups, we used block random assignment with square blocks. Using Excel 23 software, blocks of four were defined, in which the houses in each block were randomly divided between the control and experimental groups. Then, based on the arrangement of the houses, cards were prepared, and the arrangement of 92 cards, which represented the group of each participant, was determined. Then, each card was completely covered using a paper cover and the cards were coded in the previously specified order. As each person entered, one card was uncovered in turn, and the group assigned to each person was completely random and with complete blinding of the person responsible for random assignment, and the samples were selected. After obtaining verbal and written informed consent to participate in the study, the relevant questionnaires were completed at the beginning of the study.
Clarification on Settings and Group Allocation
Participants were recruited from both cardiac surgery centers. To minimize selection bias and ensure group comparability, random allocation was performed at the individual level, not the center level. This meant that eligible patients from both centers were pooled together, and each had an equal chance of assignment to either the intervention or control group through block randomization. Consequently, both groups contained participants from both hospitals. All participants received identical standard medical and nursing care per their center's protocols; the only difference was the administration of the CPPR program to the intervention group.
Outcome Measures
The Abbreviated Mental Test Score was used to assess the cognitive performance of all participants. According to the results of this test, none of the participants had cognitive problems and were included in the study (Hodkinson, 1972). Outcome measures were a demographic and clinical characteristics questionnaire, the Short Physical Performance Battery (SPPB), Berg Balance Scale (BBS), and Falls Efficacy Scale-International (FES-I). The demographic and clinical characteristics questionnaire included items on age, gender, marital status, educational level, occupation, income, underlying diseases, smoking, polypharmacy, history of falling, cause of fall, and physical activity.
The SPPB is a test for physical performance assessment. According to this test, each participant was asked to stand in three different positions for 10 seconds, walk a 4-meter distance, and stand and sit on a chair for five times. The duration of the test was measured and scored from zero (“Worst performance”) to 12 (“Best performance”). Better scores indicated better performance (Gómez et al., 2013). Previous studies reported the acceptable validity and reliability of this measure (Kameniar et al., 2024; Pirrasoulzadeh & Dehghanizadeh, 2024). The validity and reliability of the measure were also acceptable in the present study (Cronbach's alpha = 0.85).
The BBS was used to assess balance. This scale has 14 items on 14 tasks, each scored from zero (“Inability to perform the task”) to 4 (“Complete ability to perform the task”). The possible total score of the scale is 0–56, with scores 0–20, 21–40, and 41–56 showing poor balance, moderate balance, and good balance, respectively (Priscila et al., 2017). Previous studies showed that this scale has acceptable validity and reliability (Neuls et al., 2011; Salavati et al., 2012). The analyses for this study also demonstrated excellent validity and reliability for the scale (Cronbach's alpha = 0.915).
The FES-I has 16 items on FOF. Participants were asked to score their concern over falling during 16 activities using the following four-point Likert scale: 1: “Not at all concerned”; 2: “Somewhat concerned”; 3: “Fairly concerned”; and 4: “Very concerned”. The possible total score of the scale is 16–64 and lower scores show lower FOF (Bastani et al., 2021). The validity and reliability of this scale were confirmed in previous studies (Bastani et al., 2021; Delbaere et al., 2010) and also in the present study (Cronbach's alpha = 0.932).
Intervention
The study intervention was a CPPR program consisted of Otago exercise, incentive spirometry, walking, and modification of lifestyle and CVD risk factors. The first author provided CPPR-related education to participants in the intervention group in face-to-face sessions as well as through educational pamphlets and videos. The first author received training in these interventions and obtained a certificate prior to initiating the study. The first session was conducted in person at the clinic for 30 min, then the Otago exercise protocol was performed by the patient at home for 4 weeks, three sessions per week, and the duration of each exercise session was 20 min. Daily walking initially started at 10 min and increased to 30 min of daily walking. The first measurement was taken at the first session at the beginning of the study (before surgery), the second time 4 weeks after rehabilitation exercises (before surgery), and the third measurement 4 weeks after surgery. Participants were asked to perform their exercises in 30-minute thrice-weekly sessions for 4 consecutive weeks before operation. Otago exercises included head and neck, trunk, and ankle exercises as well as balance exercises such as knee bending at standing position, backward walking, toe and heel walking, single-foot standing, position change from sitting to standing position, and stair walking. Pulmonary rehabilitation also consisted of diaphragmatic breathing and chest relaxation (including 10 deep inspirations and expirations), education about appropriate postoperative position and effective coughing, and incentive spirometry. Participants were instructed, using an incentive spirometer, to hold their breath for 5 s with each inhalation, gradually increasing it to 10 s. At least 10 deep breaths per hour while awake and coughing afterwards were recommended to stimulate further clearance of secretions from the lungs. Moreover, participants were also provided with education about self-care, CVD risk factor modification, dietary modification, and anxiety and stress management. Moreover, biweekly telephone interviews were held with them to evaluate their adherence to physical and breathing exercises and dietary and CVD risk factor modifications and also to correct any misconception about cardiac surgery. Participants in the control group received routine care which included no CPPR. At the end of the study, education about Otago and breathing exercises was provided to the control group.
Data Analysis
The data were analyzed through the IBM SPSS Statistics (v. 26.0). Mean, standard deviation, and frequency measures were used for data presentation. The Kolmogorov–Smirnov test was used to test the normality of the data. Between-group comparisons were made through the independent-sample t test, while within-group comparisons were made through the paired-sample t test. The repeated measures analysis of variance was also used to evaluate the effects of CPPR on physical performance, balance, and FOF.
Ethical Considerations
Informed consent was obtained from all participants to participate in the study. All participants were assured that participation in the study was completely voluntary and that they could withdraw from the study at any time. Withdrawal from the study had no impact on the participants’ treatment. Information was kept strictly confidential. Ethical approval for this study was obtained from the Joint Ethics Committee of the Nursing and Midwifery and the Rehabilitation Faculties of Tehran University of Medical Sciences, Tehran, Iran (code: IR.TUMS.FNM.REC.1401.021). Moreover, the study was registered in the Iranian Registry of Clinical Trials (code: IRCT20220523054974N1).
Results
Ninety-two candidates for CABG surgery were recruited to the study and allocated to two 46-person groups. Ten participants from the intervention group were excluded due to opting out of surgery, change in surgery time, affliction by coronavirus disease 2019, or postoperative death. Moreover, eight participants were excluded from the control group due to opting out of surgery or change in surgery time (Figure 2).

The CONSORT Flow Diagram of the Study.
Based on Table 1, most participants in both groups were male and married. Study groups did not differ significantly from each other regarding age, gender, educational level, occupation, social support, financial status, and CVD Underlying diseases including diabetes mellitus, hypertension, hyperlipidemia, and smoking (p > 0.05).
Group Comparisons with Respect to Participants’ Characteristics.

^ = just age presented as Mean and SD; * = significant level.
The results of the repeated measures analysis of variance showed the significant effects of time (F = 139.4; p < 0.001), group (F = 31.74; p < 0.001), and time-group interaction (F = 124.2; p < 0.001) on balance. Therefore, the independent-sample t test with Bonferroni's correction was used for between-group comparisons. Its results showed no significant difference between the groups regarding pretest mean score of balance (t = 1.92; p = 0.058). However, the mean score of balance in the intervention group was significantly more than the control group both after the intervention (t = 6.71; p = 0.001) and after CABG surgery (t = 8.73; p = 0.001) (Table 2).
Within- and Between-Group Comparisons with Respect to the Mean Scores of Physical Performance, Balance, and Fear of Falling.

*Results of repeated measures analysis of variance for within-group changes (time effect).
**Results of repeated measures analysis of variance for between-group changes over time (group effect).
***Results of repeated measures analysis of variance for between-group changes over time (interaction effect).
^independent t-test results with Bonferroni correction.
The results of the repeated measures analysis of variance indicated the significant effects of time (F = 85.13; p < 0.001), group (F = 30.17; p < 0.001), and time-group interaction (F = 54.67; p < 0.001) on physical performance. Post hoc analysis using the independent-sample t test with Bonferroni's correction revealed that while there was no significant difference between the groups regarding the pretest mean score of physical performance (t = 1.84; p = 0.069), the mean score of physical performance in the intervention group was significantly more than the control group both after the intervention (t = 5.75; p = 0.001) and after surgery (t = 7.85; p = 0.001).
Based on the results of the repeated measures analysis of variance, the effects of time (F = 178.8; p < 0.001), group (F = 29.11; p < 0.001), and time-group interaction (F = 62.43; p < 0.001) on FOF were statistically significant. Post hoc analysis via the independent-sample t test with Bonferroni's correction showed that the groups had no significant difference with each other regarding the pretest mean score of FOF (t = 1.78; p = 0.079), while the mean score of FOF in the intervention group was significantly more than the control group both after the intervention (t = 5.15; p = 0.001) and after surgery (t = 8.42; p = 0.001).
The results in Table 2 show that patients who undergo CABG and undergo preoperative rehabilitation intervention show less decline in physical function, balance, and FOF than those who do not receive pre-rehabilitation intervention. According to the analysis, the findings showed that the research hypotheses were all confirmed. The results showed that the pre-rehabilitation program is effective on the physical performance of CABG patients. The pre-rehabilitation program is effective on the balance of CABG patients. The pre-rehabilitation program is effective on the FOF of CABG patients.
Discussion
This study concluded that pre-rehabilitation increases physical performance and reduces postoperative balance loss and FOF in patients undergoing coronary artery bypass surgery. Therefore, the previously stated research hypothesis: “The effect of pre-rehabilitation program on physical performance, balance, and FOF in patients undergoing coronary artery bypass surgery” was accepted for the experimental group and not accepted for the control group. This study evaluated the effects of CPPR on physical performance, balance, and FOF among the candidates for CABG surgery. Findings indicated that CPPR significantly improved physical performance and balance and reduced FOF among the candidates for CABG. Anjali et al. (2020) and Snowdon et al. (2014) studies concluded that in the pre-rehabilitation groups, the number of complications and length of stay were reduced and functional status and maximum respiratory capacity improved. When the 6-min walk test was applied, functional capacity improved, indicating that all patients had a significant improvement in the time–walk relationship. Knight et al. (2022) found that preoperative respiratory rehabilitation was effective in reducing the duration of mechanical ventilation and the total length of hospital stay. Although these studies were not conducted on the elderly as our study, they had similar results.
One of the main findings of the present study was the significant positive effect of CPPR on physical performance. In agreement with this finding, several studies showed that Otago exercise significantly improved physical performance among elderly people (Ghorbanalinejad, 2019; Molino-Lova et al., 2021; Rosko et al., 2018; Suikkanen et al., 2021; Waite et al., 2017). Although these studies differed from the present study regarding intervention duration, sample size, and target population, their findings are in line with the findings of the present study which confirmed the significant positive effect of Otago exercise on physical performance. Otago exercise strengthens the major muscles of the lower extremity, including knee flexors and extensors and hip abductors and thereby, improves physical performance. Contrary to our findings, a randomized trial found that 12-week Otago exercise had no significant positive effect on physical performance among nursing home residents. This may be due to the fact that reduced mobility among patients with cardiovascular surgeries is usually temporary, while reduced mobility among nursing home residents is mainly due to chronic muscular atrophy and reduced muscular strength and hence, long-term interventions are necessary to improve their physical performance.
The findings of the current study also indicated that CPPR significantly improved balance. This is in agreement with the results of several clinical trials which reported that Otago exercise significantly improved balance (Benavent-Caballer et al., 2016; Ferraro et al., 2020; Jahanpeyma et al., 2021; Ries et al., 2015; Yoo et al., 2013). Impaired balance is one of the most prevalent consequences of aging and is mainly due to muscular weakness. Otago exercise improves balance probably through strengthening ankle joint dorsiflexor and plantar flexor muscles which are important to maintain balance.
A significant reduction in FOF was also observed in the CPPR group. Similarly, several clinical studies showed that Otago exercise significantly reduced FOF among patients who received rehabilitation services (Barnett et al., 2017; Dadgari et al., 2016; Dastmanesh et al., 2019; Mat et al., 2018). FOF is quite prevalent among elderly people, increases the risk of falling, reduces engagement in daily activities, and is a major barrier to postoperative mobility. Otago exercise can reduce the risk of falling among elderly people through improving walking ability, aerobic strength and stamina, and concentration. In contrast to the present findings, a systematic review showed that Otago exercise did not significantly reduce FOF among patients above 65 years. This contradiction may be due to the differences among studies with respect to their population.
Strengths and Limitations
This study has several notable strengths. Firstly, it employed a randomized controlled trial design, which is the gold standard for evaluating the efficacy of interventions. Secondly, the outcome measures were assessed using internationally validated and reliable instruments (SPPB, BBS, FES-I), whose psychometric properties were also confirmed in the present study and the target population. Thirdly, the study focused on a comprehensive pre-rehabilitation program and evaluated its impact on under-investigated yet critical outcomes such as balance and FOF in CABG candidates, filling an important gap in the literature. Finally, the study assessed outcomes not only post-intervention but also post-surgery, providing insights into the sustained effects of CPPR.
However, some limitations should be acknowledged. The long-term effects of CPPR beyond 4 weeks post-surgery were not assessed. Due to the nature of the intervention, neither participants nor the individual implementing the intervention could be blinded to the group allocation, which may have introduced performance bias. The attrition of 18 participants, despite the increased initial sample size, might have reduced the statistical power of the study. Finally, the generalizability of the findings may be limited to older adults who are literate and capable of using smartphones, as these were among the inclusion criteria.
Implications
Based on the current study's findings, CPPR significantly improves physical performance and balance and significantly reduces FOF among candidates for CABG surgery. Therefore, a key implication and suggestion for future practice is to integrate comprehensive CPPR programs as a standard component of preoperative care for all eligible patients awaiting CABG surgery. This integration could involve developing standardized, evidence-based CPPR protocols that include components like Otago exercise, incentive spirometry, walking, and modification of lifestyle and cardiovascular risk factors, as evaluated in this study. Implementing accessible delivery models, such as home-based and online education, can increase patients’ engagement in CPPR programs and empower patients and family members to fulfill their needs.
Additionally, encouraging multidisciplinary collaboration among cardiac surgeons, nurses, and specialists in exercise physiology and physical medicine is crucial to facilitate effective referral, education, and management within these programs. Advocating for policy changes and healthcare system support to recognize and fund CPPR as a crucial part of the surgical pathway is also important, given its potential to reduce the physical and mental complications of surgeries, improve quality of life, and reduce healthcare-related costs. The results of this study can be used to develop evidence-based patient-centered guidelines for the rehabilitation of patients with CVD and CABG surgery, and to develop strategies to encourage physicians to refer patients to pre-rehabilitation programs.
Conclusion
Cardiac pre-rehabilitation is a multidisciplinary intervention. This study was conducted in collaboration with a cardiac surgeon, a nurse, and a specialist in exercise physiology and physical medicine. The researcher selected the samples in collaboration with the cardiac surgeon and, under the supervision of the cardiac surgeon, began teaching the samples exercise exercises after receiving training under the supervision of a specialist in physical medicine and rehabilitation.This study concludes that multi-component CPPR has significant positive effects on preoperative and postoperative physical performance, balance, and FOF among the candidates for CABG surgery. Thereby, it may improve disease prognosis, surgical outcomes, and ability to cope with surgical stress, and reduce the costs of postoperative recovery.
Supplemental Material
sj-docx-1-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-docx-1-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Supplemental Material
sj-docx-2-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-docx-2-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Supplemental Material
sj-docx-3-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-docx-3-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Supplemental Material
sj-pdf-4-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-pdf-4-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Supplemental Material
sj-docx-5-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-docx-5-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Supplemental Material
sj-docx-6-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-docx-6-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Supplemental Material
sj-doc-7-son-10.1177_23779608251407768 - Supplemental material for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery
Supplemental material, sj-doc-7-son-10.1177_23779608251407768 for The Effects of Cardiopulmonary Pre-Rehabilitation on Physical Performance, Balance, and Fear of Falling Among the Candidates for Coronary Artery Bypass Graft Surgery by Zoleikha Abbasi, Mahbubeh Shali, Elham Navab, Farshad Sharifi, Amir Hossein Goudarzian and Mehrzad Rahmanian in SAGE Open Nursing
Footnotes
Acknowledgements
This article is the result of a Master's thesis in nursing in Tehran University of Medical Sciences, Tehran, Iran. We would like to thank the reviewers of the thesis, the patients who participated in the study, the medical and nursing staff of the study setting, and the Research Administration of Tehran Faculty of Nursing and Midwifery.
Author Contributions
Conceptualization was done by ZA and MS; data curation was done by ZA and MR; formal analysis was done by FS; funding acquisition was done by EN; investigation was done by ZA and AHG; methodology was done by MS and FS; writing—original draft was done by ZA and MS; writing—review & editing was done by EN, AHG, and MR.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
No potential conflict of interest relevant to this article was reported.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
