Abstract
Background
The global nursing shortage continues to strain healthcare systems, with the intention to leave (ITL), which is defined as the likelihood of leaving one's job or profession, emerging as a key contributor to workforce instability.
Objective
The study aims to assess the correlation between sociodemographic characteristics, professional quality of life (ProQoL), critical care nurses’ intention to leave their units, and their intention to leave the nursing profession.
Methods
A cross-sectional descriptive study of 135 critical care nurses in Jordan was conducted between February and May 2024 using an electronic questionnaire that included ITL and ProQoL Version 5. Associations between variables were examined using point-biserial correlation and the Chi-square test. A logistic regression was performed to ascertain the effects of ProQoL and demographics on the likelihood that nurses intended to leave.
Results
Of the 135 nurses surveyed, 56% reported an intention to leave the nursing profession, and 55% expressed intent to leave their current critical care units. Most participants demonstrated moderate levels of compassion satisfaction (85%), compassion fatigue (86%), and burnout (94%). Female nurses reported higher levels of compassion satisfaction, burnout, and compassion fatigue than males. Regression analysis showed that intention to leave the profession was significantly predicted by intention to leave the unit (B = −2.268, p < .05), though burnout was not a significant predictor.
Conclusions
Burnout and compassion fatigue were significantly predictive of ITL, while compassion satisfaction mitigated its likelihood. These findings demonstrate the necessity of proactive and strategic policies designed to address nurses’ physical and mental health conditions and restructure their staffing and scheduling frameworks to retain critical care nurses.
Introduction
Jordan's healthcare system faces a critical nursing shortage, with an estimated gap of over 50,000 nurses, representing approximately 61% of the workforce's needs (Amarneh et al., 2021). The shortage is driven by demographic shifts, a rising burden of non-communicable diseases, and high attrition rates, particularly in demanding environments such as critical care units. The growing pressure on public hospitals, which deliver the majority of inpatient services, makes nurse retention a national priority (Haakenstad et al., 2022)
Nurses represent the largest segment of the healthcare workforce, comprising nearly 44% of healthcare professionals globally (Haakenstad et al., 2022). Nevertheless, retaining skilled nurses remains a pressing challenge due to the emotional and physical demands of the profession, particularly in high-stress settings such as intensive care units (Dobnik et al., 2018). These environments expose nurses to continuous critical care responsibilities, leading to high levels of stress, burnout, and increased turnover intentions (Szekely & Ciobanu, 2024)
This growing challenge threatens the sustainability of healthcare services and underscores the urgent need to address factors influencing nurses’ intention to leave. Understanding predictors of turnover, particularly in intensive care settings, is vital for guiding workforce retention strategies. The Professional Quality of Life (ProQoL), which encompasses compassion satisfaction, burnout, and compassion fatigue, has emerged as a crucial framework for assessing the well-being of healthcare providers and their relationship to turnover intentions (Bahari et al., 2022; Bruyneel et al., 2023).
Review of Literature
Nurses comprise the largest workforce in the healthcare system, accounting for an estimated 19.3 out of 43.5 million healthcare workers worldwide (Haakenstad et al., 2022). Retaining skilled and competent nurses is vital for ensuring continuity of care, especially in critical care units, where high levels of emotional challenges and daily stress, heavy workloads, and coping with issues such as grief and death can aggravate their intention to leave (Dobnik et al., 2018; Ibrahim et al., 2024).
Intention to leave (ITL) is defined as an individual's foreseeable intention to depart from the organization shortly or within a specified timeframe (Goodman et al., 2015; Seki & Özlük, 2024). ITL is considered one of the most reliable predictors of actual turnover behavior (Khan et al., 2019) (Gebregziabher et al., 2020). The annual turnover rate among critical care nurses is about 27% compared to 20% in all other units (Vogt et al., 2023). Moreover, in the United Kingdom, for instance, a considerable proportion of critical care units (CCUs) experience an annual staff turnover exceeding 20%, reaching as high as 42% in some cases (Cutler et al., 2021).
One of the most relevant frameworks for understanding the emotional and psychological experiences of nurses is the ProQoL model, which is defined as the sense of well-being arising from the perceived balance between the burden of a profession and the psychological, organizational, and interpersonal resources used to cope with this burden (Bahari et al., 2022). It consists of three dimensions: compassion satisfaction, burnout, and compassion fatigue (Bahari et al., 2022; Lee et al., 2021). These dimensions are observable among healthcare professionals during individual, community, national, and global crises. Compassion fatigue is also recognized under the term secondary traumatic stress (Lee et al., 2021). The balance between positive compassion satisfaction and negative compassion fatigue within the workplace shows the level of ProQOL (Ruiz-Fernández et al., 2020). Impaired ProQoL has been implicated in the adverse impact on patient care quality, a reduction in patient satisfaction, and, most importantly, an elevated intention among healthcare professionals to leave their respective professions (Hamaideh et al., 2023; Saliya et al., 2024).
Multiple studies have demonstrated that high levels of burnout and compassion fatigue are significantly correlated with nurses’ intention to leave, particularly in high-acuity settings such as intensive care units (ICUs) (Ruiz-Fernández et al., 2020). Compassion satisfaction, conversely, has been shown to buffer against ITL by promoting job engagement and emotional fulfillment (Pang et al., 2020). A systematic review across 23 countries found that up to one-quarter of ICU nurses expressed intent to leave their roles, underscoring the global nature of this issue (Xu et al., 2023)
In the Middle East, particularly Jordan, there is an estimated shortage of approximately 50,164 nurses, representing a 61% gap in the country's healthcare system (Amarneh et al., 2021). This shortage is expected to be further exacerbated by Jordan's projected population doubling by 2030 and the rising prevalence of non-communicable diseases. Moreover, existing challenges in human resources for health, including high turnover rates, limited retention strategies, and insufficient training, further strain the healthcare system (‘Jordan,’ n.d.).
Despite the urgency of this issue, limited empirical research has focused specifically on the predictors of intention to leave among critical care nurses in Jordan. Most national studies have examined general nursing populations or emphasized job satisfaction and burnout without considering the full spectrum of ProQoL dimensions or differentiating between intentions to leave the unit versus the profession.
Objectives
Examine the relation between sociodemographic and occupational factors, characteristics, and critical care nurses’ intention to leave the critical care units and the nursing profession.
Evaluate the influence of the three core components of ProQoL, “satisfaction, burnout, and compassion fatigue,” on nurses’ intention to leave the critical care units and the nursing profession.
Materials and Methods
Study Design
A cross-sectional descriptive quantitative design was employed to assess the determinants of intention to leave among critical care nurses. This design was selected because it facilitates the collection of data from a substantial sample at a single moment, rendering it suitable for discerning correlations among various demographic, organizational, and psychological elements and the intention to depart from the unit or profession. This design aligns with analogous studies in the field, facilitating meaningful comparison with current literature.
Sample and Setting
Jordan has 122 hospitals distributed across the public, private, and military sectors. The public sector accounts for the majority of hospital beds, with approximately 51% of the total, and around 10,000 nurses provide care in these facilities. This study was conducted in three major public hospitals in Jordan: Amman (the capital), Zarqa, and Irbid. Between February and May 2024, data were collected from critical care nurses working in the critical care units in the three selected hospitals.
A prior power analysis was conducted using G*Power 3.1 to estimate the minimum sample size required for binary logistic regression analysis. Assuming a medium effect size (odds ratio = 1.5), α = 0.05, power (1 – β) = 0.80, and 10 predictors, the required minimum sample size was calculated to be 118. The final sample of 135 nurses exceeded this threshold, indicating sufficient power to detect statistically significant associations.
Inclusion/Exclusion Criteria
The total number of registered nurses working in adult critical care units across the three selected public hospitals was 188. Of this population, 135 nurses completed the questionnaire in full, resulting in a response rate of approximately 71.8% (Figure 1). The exclusion criteria aimed to remove nurses who were working at the general units and had less than 6 months of experience working in the critical care units.

A diagram representing study subjects and attrition.
Study Instruments
Data were collected using a questionnaire that contained four sections: a sociodemographic characteristics section, an ITL section developed by the researcher, and the ProQoL Version 5 (Lenz et al., 2024). The original author was permitted to use ProQoL-5 material. Demographic variables contained 13 items, such as gender, marital status, level of education, overall nursing experience, overall critical care experience, overall years of experience in the hospital, unit, monthly income, chronic disease presence, nurse–patient ratio, working hours per week, and shift timing (Souza et al., 2019).
ITL was measured using two researcher-developed questions. The assessment was conducted by asking participants to rate their likelihood of leaving using a Likert-type scale, ranging from 1 to 4, where 1 corresponds to “highly unlikely,” 2 to “unlikely,” 3 to “likely,” and 4 to “highly likely.” The first question evaluated the intention to leave the current clinical position within critical care units, framed as follows: “Considering your career goals, do you intend to transition from a critical care setting to another nursing setting in the upcoming year?” The second question assessed the intention to leave the nursing profession, as articulated in the statement, “Do you intend to exit the nursing profession within the coming year?” Dolbeir employed a single-item measure of job satisfaction, which was validated (Dolbier et al., 2005).
ProQoL, Version 5, was developed and tested by Stamm. It was also used to measure the compassion satisfaction, burnout, and compassion fatigue of critical care nurses. ProQoL is a 30-item self-report measure composed of three subscales (each with 10 items): compassion satisfaction, burnout, and compassion fatigue. Each item is based on a 5-point Likert scale, graded from 1 (never) to 5 (very often). Each subscale is to be interpreted independently. Total scores for each subscale range from 10 to 50 (>22 = low, 23–41 = moderate, <42 = high) (Xie et al., 2021).
Researchers have widely employed the ProQoL instrument, and it has proven to be reliable when applied to the nursing population (Hooper et al., 2010; Young et al., 2011). A recent study reported Cronbach's alpha values of .79 for burnout, .84 for secondary traumatic stress, and .89 for compassion satisfaction (Kelly et al., 2021).
Data Collection
Data collection occurred over 4 months (August to December 2023) through an online survey distributed via institutional email lists and professional networks. The invitation included a description of the study's purpose, assurances of confidentiality, information on voluntary participation, and contact details for the researcher. The questionnaire, hosted on a secure platform, took approximately 5–10 min to complete. To augment participation, reminder messages were sent monthly, and the principal investigator remained available to address any questions during the data collection period.
Statement of Ethics
The University of Jordan Ethical Committee (Approval no. 3456915) and Jordanian Ministry of Health Ethical Research Committee (Approval no. 3125). The nurses voluntarily engaged in the study after being provided comprehensive information about the procedures to safeguard their data confidentiality. The data gathered from participants was completely anonymous, with no identifiable personal information documented. The research's aims and objectives were effectively communicated to the nursing students participating in the study by disseminating informational materials and consent forms.
Statistical Analysis
The Statistical Package for Social Sciences (SPSS), Version 25, was used to analyze data. Descriptive statistics were employed to measure frequencies, percentages, means, and standard deviations. Associations between variables were examined using point-biserial correlation and the Chi-square test. A binary logistic regression was performed to ascertain the effects of ProQoL and demographics on the likelihood that nurses intended to leave the nursing profession and the critical care units. Alongside analyzing direct correlations between predictors and intentions to leave, we evaluated potential confounding variables and effect modifiers that might affect these relationships. Variables such as gender, total years of nursing experience, critical care experience, monthly income, and shift type were incorporated into the regression models to account for any potential confounding factors. The primary emphasis was on burnout, compassion satisfaction, and compassion fatigue; these factors were included to mitigate bias and enhance model validity.
A total of 188 nurses were initially enlisted. Among these, 25 did not give informed consent, and 18 withdrew before finishing the study procedures. This yielded 145 nurses who finalized the data collection. Of these, 10 participants (6.9%) were excluded for providing incomplete responses to essential study variables. The final sample analyzed comprised 135 nurses.
Missing data were handled by listwise deletion (complete-case analysis), which is suitable when the proportion of missing data is reasonably low and the missing data are presumed to be missing at random (MCAR).
Results
A total number of 135 nurses participated in the study, with 50% male, 64% being married, and 11% suffering from chronic illness, including 40% having lumbar pain. Most nurses, 87%, hold a bachelor's degree in nursing, with a mean of 9.2 years of overall nursing experience (SD = 4.8) and 5.7 years of critical care experience (SD = 4.1). Of them, 40% worked in cardiac care units, 33% in general ICU, and 27% (n = 37) in surgical ICU. Nurses work around 43.2 (SD = 7.8) hours weekly, with a mean monthly income of JOD 557 (SD = 122). Most nurses, 52% (n = 70), worked 8-hr shifts, 43% (n = 58) worked 16-hr shifts, and only 29% worked 12-hr shifts. Regarding the nurse–patient ratio, 58.6% were working at a ratio of more than 1:3, 28.1% (n = 38) were working at a 1:3 ratio, and only 13.3% were working at a ratio of less than 1:2 (Table 1).
Demographic Characteristics of Nurses (N = 135).

Table 2 shows subgroup differences in ProQoL components: compassion satisfaction, burnout, and compassion fatigue based on gender and unit type. Female nurses exhibited greater compassion satisfaction (M = 34.2, SD = 6.6) and burnout (M = 29.8, SD = 3.6) than their male counterparts (M = 32.1, SD = 6.3 for compassion satisfaction; M = 28.1, SD = 3.2 for burnout). Furthermore, female nurses demonstrated elevated levels of compassion fatigue (M = 32.1, SD = 6.9) compared to their male counterparts (M = 30.0, SD = 6.5). Nurses in general ICUs exhibited the highest levels of compassion satisfaction (M = 34.0, SD = 6.4), whereas those in CICUs reported the highest levels of burnout (M = 29.5, SD = 3.4) and compassion fatigue (M = 32.5, SD = 6.8). The findings indicate gender- and unit-specific variations in ProQoL that may affect intentions to depart (Table 2).
Subgroup Analysis of ProQoL Scores.
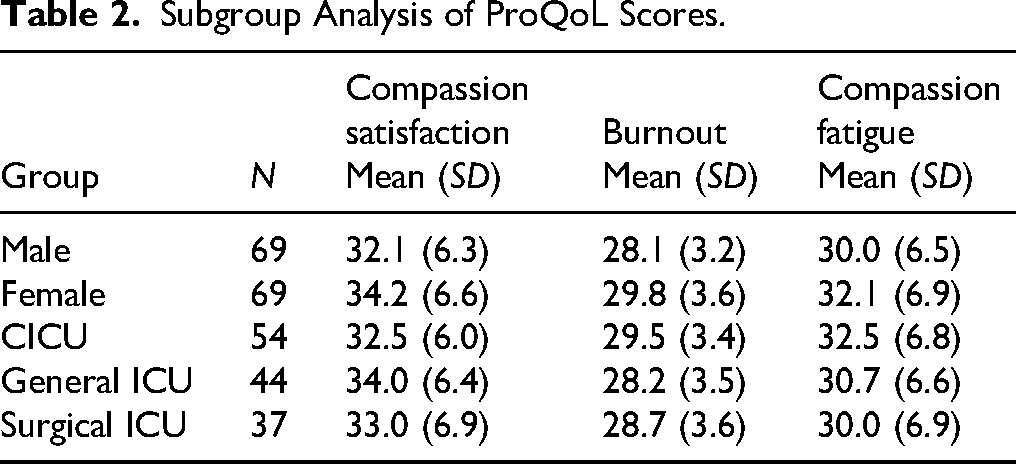
Table 3 summarizes the distribution of responses for intention to leave (both unit and profession), as well as levels of compassion satisfaction, burnout, and compassion fatigue. Fifty-five percent of the nurses had the intention to leave their critical care units and transit to other nursing units in the upcoming year, with the majority of them, 44%, being likely to transit; 32% were unlikely to transit, 13% were highly unlikely to transit, and only 11% were highly likely to transit. Considering the intention to leave the nursing profession, 56% of the nurses intended to leave the nursing profession, with 33% likely to leave, 30% unlikely to leave, 23% highly likely to leave, and 11% highly unlikely to leave the nursing profession.
Description of Study Variables (n = 135).
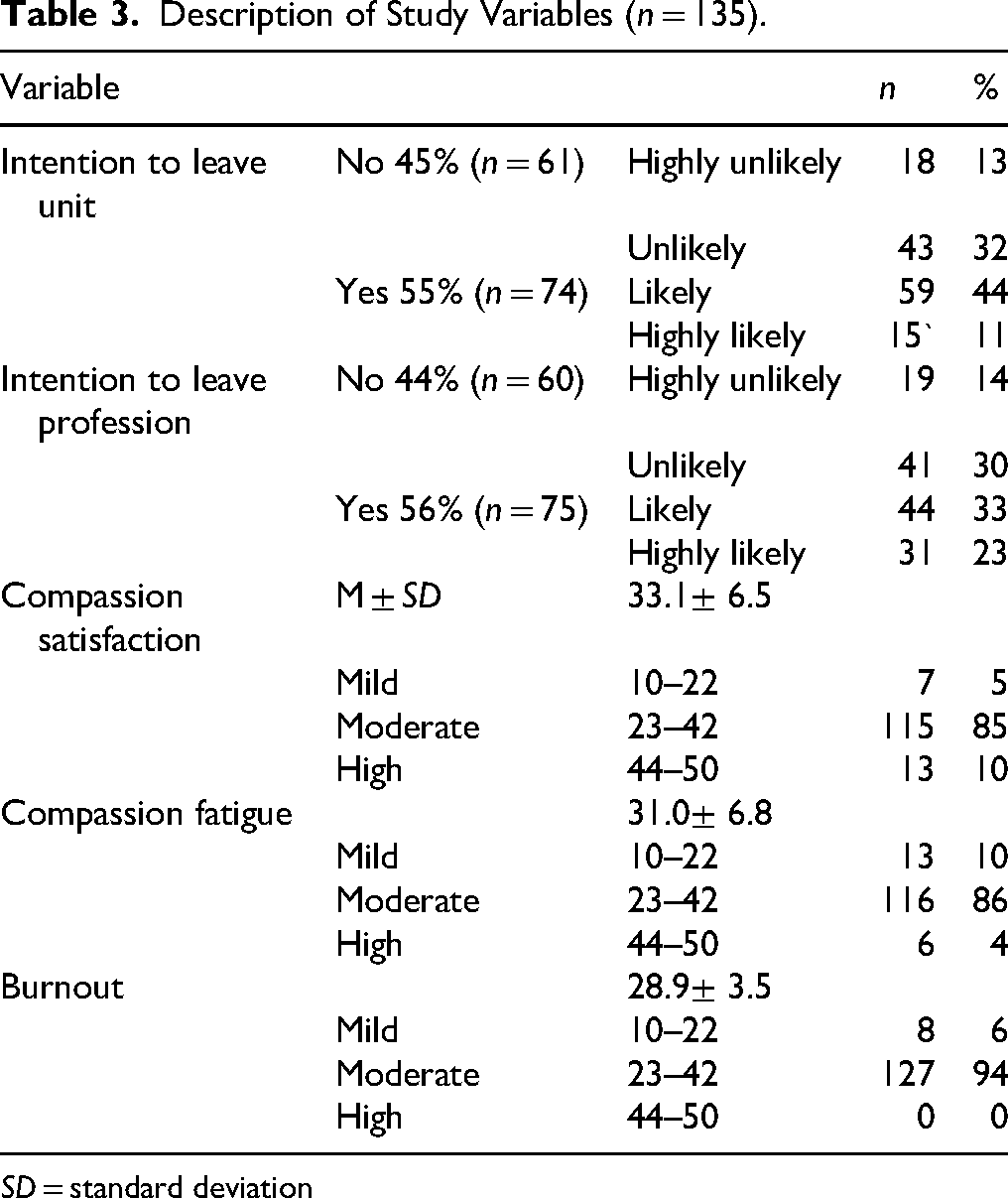
SD = standard deviation
Nurses’ ProQoL showed moderate compassion satisfaction with a mean of 33.1 ± 6.5. Moreover, 85% had a moderate level, 10% had a high level, and 5% had a mild level of compassion satisfaction. Additionally, most nurses exhibited moderate levels of compassion fatigue, with a mean of 31.0 ± 6.8. Most nurses, 86%, had a moderate level of compassion fatigue, 10% had a mild level, and only 4% had a high level. Furthermore, they had a moderate level of burnout with a mean of 28.9 ± 3.5. Most of them, 94%, had a moderate level, and 6% had a mild level, with no nurse scoring high on burnout. Female nurses had higher levels in all dimensions than male nurses (Table 3).
Table 4 presents the correlation matrix for key study variables. A significant positive correlation was observed between intention to leave the unit and intention to leave the profession (r = .455, p < .01), indicating that nurses who consider leaving their units are also more likely to consider leaving the profession. Both turnover intentions were also positively associated with burnout and the total number of years of nursing experience. Burnout was positively correlated with compassion fatigue (r = 0.322, p < 0.01) and negatively correlated with compassion satisfaction (r = –0.296, p < 0.01), supporting the internal consistency of the ProQoL framework. Compassion satisfaction was inversely related to compassion fatigue (r = –.524, p < .01), highlighting the protective role of positive professional experiences.
Matrix of Correlation Between the Variables of the Study (n = 135).

** Correlation is significant at the .01 level (two-tailed). * The correlation is significant at the .05 level (two-tailed).
According to the logistic regression analysis presented in Table 5, several factors significantly influenced healthcare workers’ intention to leave the profession and their current unit. For the intention to leave the profession, the model was statistically significant (Adjusted R² = .50, p < .001), with leaving the unit emerging as a significant negative predictor (B = –2.26). This indicates that those planning to leave their unit are also more likely to consider leaving the profession. Although burnout showed a positive association (B = 0.23), it was not statistically significant (p = .567). Regarding the intention to leave the unit, the model was also significant (Adjusted R² = .41, p < .001), with several positive predictors: monthly income (B = 0.006, p = .038), having a chronic disease (B = 2.31, p = .016), compassion fatigue (B = 0.11, p = .040), working in a coronary intensive care unit (B = 1.30, p = .023), and working 8-hr shifts (B = 1.29, p = .010).
Logistic Regression Analysis of Factors Influencing the Intention to Leave (n = 135).
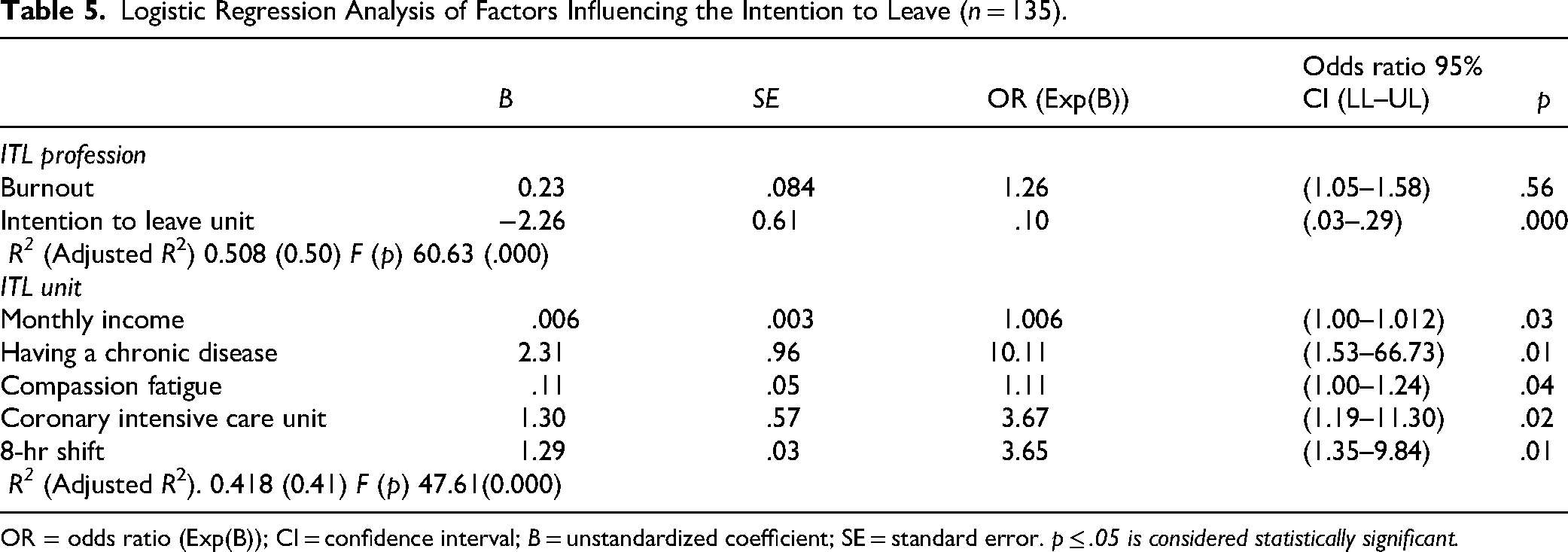
OR = odds ratio (Exp(B)); CI = confidence interval; B = unstandardized coefficient; SE = standard error. p ≤ .05 is considered statistically significant.
Discussion
The primary aim of this study was to investigate the relationship between sociodemographic and occupational parameters and the ProQol of critical care nurses. Additionally, it assesses how nurses’ intention to leave the critical care units and the nursing profession is influenced by the three fundamental elements of professional quality of life: compassion satisfaction, burnout, and compassion fatigue.
This study reported moderate levels of compassion fatigue and burnout among critical care nurses. These findings can be attributed to the inherently high-stress and high-pressure environment of critical care settings, where nurses are frequently exposed to trauma, emotionally intense situations, and complex ethical dilemmas. Such conditions can lead to a gradual depletion of emotional and psychological resilience. Furthermore, a positive correlation was observed between compassion fatigue, burnout, and the ITL, both the unit and the profession. This suggests that unresolved emotional strain may significantly contribute to nurses’ decisions to leave their roles, highlighting the urgent need for targeted mental health support, adequate staffing, and effective workload management strategies within critical care environments.
This study reported moderate levels of compassion satisfaction among critical care nurses, which appears to reflect a balance between the emotional demands and the intrinsic rewards of their roles. Notably, compassion satisfaction was negatively correlated with ITL in both the unit and the profession. This suggests that nurses who find purpose and fulfillment in their work are less likely to consider leaving their profession. Compassion satisfaction may serve as a protective factor, fostering resilience and sustained engagement. Supportive environments that promote meaningful relationships, recognition, and growth opportunities can enhance satisfaction and improve retention.
These findings align with a study conducted in Saudi Arabia (Alharbi et al., 2016), the Philippines (Labrague et al., 2020), Korea (Pang et al., 2020), Canada (Maddigan et al., 2023), and Africa (Shelton, 2023), implying a consistent trend in several healthcare environments. This alignment shows that, despite cultural and institutional differences, elements affecting compassion satisfaction, compassion fatigue, burnout, and intentions to leave among critical care nurses may be universally relevant, hence strengthening the credibility of the present results.
The study found, upon analyzing the data based on gender and unit assignment, that female nurses reported higher scores than male nurses in all three categories. This could reflect their stronger emotional engagement in caring jobs, which would result in both higher compassion satisfaction and more sensitivity to burnout and compassion fatigue. Furthermore, contributing to these gender-based variations are social expectations, role strain, and variations in coping strategies. These results stress the requirement for gender-sensitive support systems in medical environments. This finding echoed a study in Mexico among healthcare workers, which revealed that women reported higher job satisfaction, personal development, and free time management than men (González-Baltazar et al., 2021).
Nurses in general ICUs also showed the highest degrees of compassion satisfaction; those working in CICUs reported the highest degrees of burnout and compassion fatigue. This higher degree could result from a larger patient population with more diverse clinical demands, which would allow nurses to encounter a broad spectrum of treatment situations and effective recoveries. Particularly in cases when patients respond favorably to treatments and are released in better health, this diversity can help foster a stronger sense of professional fulfillment and purpose. In contrast, CICU nurses may face more emotionally and physically taxing surroundings. Typical elements of CICU are high patient acuity, frequent exposure to life-threatening diseases, and prompt, high-stakes procedures. These elements can contribute to increased burnout and compassion fatigue. This finding aligns with the results of studies conducted in the southern West Bank (Ayed et al., 2024) and Greece (Kartsonaki et al., 2023).
According to the study results, more than half of the subjects intended to leave both their current units and the profession. This correlation is also augmented by the results of logistic regression analysis (B = −2.26). The high turnover intention could be a consequence of a combination of structural and personal factors, such as job dissatisfaction, occupational stress, lack of support, inadequate personnel, and limited opportunities for professional growth. More general issues, such as financial pressures and challenges in achieving a work-life balance, could also have an influence. The intention to leave the unit and leave the profession showed a strong positive correlation. This suggests that adverse working conditions, such as inadequate leadership, excessive workloads, and limited opportunities for advancement, may influence retention at the unit level and contribute to decisions to quit the field altogether. These findings corresponded to both national and global patterns. Fifty percent of English critical care nurses stated they planned to leave their units during the next 3 years (Cutler et al., 2021). Twenty-five percent of critical care nurses intended to leave the field, according to a meta-analysis encompassing 23 nations (Xu et al., 2023). These results, taken together, demonstrate the urgent need for organizational projects to improve work conditions. Improving retention at both the unit and professional levels depends on strategies that include encouraging supportive leadership, preserving reasonable workloads, and fostering a healthy workplace culture.
By contrast, continental-based studies conducted in Europe reported that nurses intending to leave the profession were less than 15% (Heinen et al., 2013; Maniscalco et al., 2024). In another study, the intention to leave the profession among critical care nurses was less than a quarter of the sample (Bruyneel et al., 2023). Another study in Jordan revealed that more than half of the nurses did not intend to leave their profession (Salahat & Al-Hamdan, 2022). One more study conducted during the COVID-19 pandemic reported that 11% of the sample indicated they intended to leave their position, and less than 2% indicated their intention to leave the nursing profession (Raso et al., 2021). This variance may be attributable to differences in healthcare infrastructure, nurse–patient ratios, remuneration, working culture, and professional support systems. The timing of data collection may influence outcomes, as degrees of burnout and intentions to leave (ITL) can vary during or following crises.
Ultimately, the presence of a chronic illness, work in a cardiac critical care unit, adherence to 8-hr shifts, and monthly income were substantial predictors of the intention to depart from the unit. The data indicate that personal health issues and job-related factors substantially affect intentions to leave among healthcare workers. This may be elucidated as nurses with chronic health issues may experience increased physical and emotional stress, rendering challenging unit situations less viable. This finding is backed by the results of previous research (Rutledge et al., 2022; Sheekha et al., 2024). Cardiac critical care units typically include elevated acuity and demanding workloads, resulting in increased stress and turnover rates. This corresponds with a study of Survey results from five European countries.
Although 8-hr shifts are typically considered manageable, their monotonous nature, which lacks rest and flexibility, may nonetheless lead to fatigue. This justification is supported by previous results obtained among nurses in Saudi Arabia working in various critical care units (Alhamagi et al., 2024). Moreover, dissatisfaction related to income, especially if perceived as disproportionate to the role's demands, may intensify intentions to leave. A study among Healthcare workers reported that those who are dissatisfied with their income are more likely to consider leaving their positions (Wu et al., 2023). Collectively, these findings underscore the necessity for personalized and systemic interventions that consider both health status and occupational situations.
Strengths
This study offers several strengths that enhance the credibility and relevance of its findings. First, it employed a strong methodological framework, using a cross-sectional design with appropriate statistical analyses, including logistic regression, to examine predictors of turnover intentions. The study also applied the ProQoL Version 5, a well-established and psychometrically validated instrument, to assess compassion satisfaction, burnout, and compassion fatigue. Additionally, the study achieved a relatively high response rate (71.8%), which supports the representativeness and generalizability of the findings within the context of public hospitals in Jordan. The inclusion of both sociodemographic and occupational variables allowed for a more nuanced understanding of the multidimensional factors influencing nurses’ intention to leave their units and the profession.
Limitations
Despite its contributions, this study has several limitations. The cross-sectional design restricts the ability to infer causality between predictor variables and turnover intentions. Self-reported data may introduce biases, such as social desirability and recall bias, which could affect the accuracy of the responses. Furthermore, the study was conducted in only three public hospitals in Jordan, which limits the generalizability of the results to other sectors, such as private or military hospitals, or to different cultural and healthcare settings.
Another limitation involves the use of two researcher-developed single-item measures to assess the intention to leave both the unit and the profession. Although these items were conceptually grounded and aligned with prior research using single-item indicators, they may not fully capture the complexity of turnover intentions. The use of single-item measures limits the ability to assess internal consistency and may reduce overall measurement reliability. Future research would benefit from the development or adoption of psychometrically validated multi-item scales specifically tailored to measure intention to leave within critical care nursing contexts.
Implications
This study provides meaningful insights into the challenges of retaining critical care nurses in Jordan's public hospitals. The findings have particular relevance for national-level health workforce planning, especially in the context of ongoing nurse shortages, workload intensity, and constrained staffing models. Context-specific factors such as low nurse-to-patient ratios, chronic illness among staff, and rigid shift schedules emerge as significant contributors to turnover intentions. They should be prioritized in local policy reforms. These include interventions like targeted mental health support, flexible scheduling, and improved compensation structures tailored to the Jordanian healthcare context.
While the findings are drawn from a Jordanian setting, specific patterns, such as the associations between compassion fatigue, burnout, and intention to leave, reflect well-documented challenges faced by critical care nurses globally. However, we acknowledge that cross-national generalization should be made cautiously. We have, therefore, limited global claims to areas supported by broader literature and have framed our findings as potentially informative rather than representative of international trends. Future research using comparative or multinational data is warranted to examine the universality of these findings across different healthcare systems.
Conclusion
The study highlights a concerning trend of high turnover intentions among critical care nurses, with over half indicating plans to leave their current units or the nursing profession. Factors such as chronic illness alongside ProQoL indicators, especially compassion fatigue and burnout, considerably influence these intentions. Others include organizational elements such as unit type, shifting schedules, salary, and workload, which also affect the decision to leave nursing. This finding highlights the need for proactive and strategic policies that address nurses’ physical and mental health needs and restructure their staffing and scheduling frameworks to retain critical care nurses.
Footnotes
Acknowledgment
The authors would like to thank all participants for their participation in the study.
Ethical Considerations
The University of Jordan Ethical Committee (Approval no. 3456915) and Jordanian Ministry of Health Ethical Research Committee (Approval no. 3125). The nurses voluntarily engaged in the study after being provided comprehensive information about the procedures to safeguard their data confidentiality. The data gathered from participants was completely anonymous, with no identifiable personal information documented. The research's aims and objectives were effectively communicated to the nursing students participating in the study by disseminating informational materials and consent forms.
Informed Consent Statement
Written informed consent was obtained from all participants in the study.
Author Contributions
A.S.: The principal investigator, writing the original draft and methodology; B.G. &O.M.: Results preparation, completing ethical approvals; R.K.I.: Reviewing the manuscript and corresponding author. J.A.: Results writing, original draft preparation, proofreading, and reviewing the manuscript. A.S., B.G., & J.A.: Data collection and reviewing of the manuscript. The authors read and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declare no conflicts of interest; this article does not concern commercial products.
Data Availability Statement
The data supporting this study's findings are available from the corresponding author upon reasonable request.
Artificial Intelligence (AI) Disclosure Statement
AI-unassisted Work.
Statement of Ethics
The study was planned, conducted, and reported in accordance with the World Medical Association (WMA) Declaration of Helsinki.
