Abstract
Background
Injuries from sharp materials were a major cause of occupational hazards worldwide.
Objective
To assess the magnitude of sharp material injury and associated factors among health workers in public Hospitals of Hadiya Zone, Central Ethiopia, 2023.
Methods
A hospital-based cross-sectional study was conducted from June 10 to July 10, 2023, on 369 healthcare workers. A simple random sampling technique was used. Data were entered using Epi data 3.1 and analyzed using SPSS Version 25. Binary logistic regression analysis was done, and variables with a p-value of < .05 in the bivariate analysis were taken into the multivariable analysis. Statistical significance was declared at a p-value of < .05 with an adjusted odds ratio (AOR) and 95% confidence interval (95% CI).
Results
The magnitude of sharp material injury among health workers was 30.7% with 95% CI (25.9–35.3). Supervision [AOR 0.13, 95% CI: 0.06–0.27], training [AOR 0.29, 95% CI: 0.14–0.59], protocol about sharp material injury report [AOR 0.32, 95% CI: 0.17–0.63], recap needle [AOR 4.89, 95% CI: 2.47–9.72], dispose sharp materials [AOR 0.38, 95% CI: 0.16–0.88], segregate sharp waste [AOR 0.33, 95% CI: 0.15–0.75], and report any sharp material injury immediately [AOR 0.38, 95% CI: 0.18–0.83] were significantly associated with sharp material injury.
Conclusion
Three in 10 healthcare workers face sharp material injury. Supervision, training, protocol, recapping needles, disposing of sharp materials, segregating sharp waste, and reporting any sharp material injury immediately were found to be significant variables. Therefore, conducting regular supervision from hospital authorized bodies, training healthcare workers, developing and implementing protocols about sharp material injury reports, avoiding recapping needles after injection, proper disposition of sharp materials in safety box after the procedure, adequate segregation of sharp waste from other wastes, and coherent reporting of any sharp material injury immediately might reduce the occurrence of sharp material injury among healthcare workers.
Introduction
Sharp material injuries are cutaneous lesions caused by infected scalpels, needles, glass, or other sharp which expose medical staff to contaminated bodily fluids (Legesse et al., 2015). Sharp material injuries are serious occupational hazards in the healthcare setting, where healthcare professionals bear a disproportionately large share of the total burden, particularly with items that have previously been used on patients (Legesse et al., 2015; Sharew et al., 2017). Each year, ∼3 million healthcare workers are exposed to blood-borne viruses at work, with 90% of infections occurring in low-income countries (Sharew et al., 2017). Globally, unsafe injecting practices were responsible for 2.5% of human immune deficiency virus infections, 40% of hepatitis B virus infections, and 5% of bacterial infections, resulting in 28 million avoidable disability-adjusted life years (Mengistu et al., 2021).
In Africa, the prevalence of sharp material injury ranged from 19.9% to 54.0% with an overall prevalence of 35.7% (Mengistu et al., 2021). Also, the prevalence of sharp material injury in Ethiopia varied across the study settings, ranging from 18.7% to 44.1% (Abebe et al., 2018; Belachew et al., 2017; Desalegn, 2015; Dilie et al., 2017; Gebretsadik Kelebore, 2016; Kaweti & Abegaz, 2014; Mekonnen et al., 2018; Tesafa Bamlie, 2015). However, these studies were profession-specific and focused either on nurses or nurses and midwives. The current study included nurses, midwives, general practitioners, health officers, laboratory technicians, specialists, anesthesia, pharmacy, and integrated surgical officers.
Review of Literature
Works of literature show that lack of infection prevention patient safety training, knowledge about standard precautions, lack of adherence to standard precaution guidelines, work experience, marital status, working load, working department, and working hour shift were significant risk factors of sharp material injury among healthcare workers (Abebe et al., 2018; Bacha Gemechu, 2020; Bekele et al., 2015; Belachew et al., 2017; Borde, 2010; Desalegn, 2015; Dilie et al., 2017; Gebretsadik Kelebore, 2016; Legesse et al., 2015; Tesafa Bamlie, 2015). However, many studies were conducted either in specific professions like nurses and midwifery or focusing specifically on needle injury. As a result, health policymakers were facing difficulties in taking effective preventive measures regarding sharp material injuries. Therefore, this study assessed the magnitude of sharp material injury and associated factors among health workers working in public Hospitals of Hadiya Zone, Central Ethiopia.
Method and Materials
Study Area and Period
A multicenter facility-based cross-sectional study was conducted in the public hospitals of Hadiya Zone. Hadiya zone is located in the Central Ethiopia regional state. There are four public hospitals in the zone, namely; Wachemo University Nigist Eleni Mohammed Memorial Comprehensive Specialized Hospital (WCUNEMMCSH), Homacho, Ginbichu, and Shone hospitals. WUNEMMCSH has 777 healthcare workers and 425 beds, Homacho Hospital has 101 healthcare workers and 28 beds, Gimbichu Hospital has 96 healthcare workers and 29 beds and Shone Hospital has 99 healthcare workers and 38 beds. The study was conducted from June 10 to July 10, 2023.
Eligibility Criteria
All health workers working in the public hospitals of Hadiya Zone during the study period were included. However, healthcare workers who worked for < 6 months, were critically ill, and were on maternal and annual leave at the time of data collection were excluded from the study.
Sample Size Determination
The sample size was calculated using a single population proportion formula, taking the proportion of sharp instrument injury 32.2% from a previous study (Mengistu et al., 2021), a 95% level of confidence, and a 5% margin of error as follows.
By considering the 10% nonresponse rate, the sample size was 369.
Sampling Procedure
The four public hospitals in the zone were included in the study. The number of healthcare workers in each hospital was identified as 777 healthcare workers in WUNEMMCSH, 101 healthcare workers in Homecho Hospital, 96 healthcare workers in Ginbichu Hospital, and 99 healthcare workers in Shone Hospital. Then, the identified number in each hospital was proportionally allocated as 267 healthcare workers from WUNEMMCSH, 35 healthcare workers from Homecho Hospital, 33 healthcare workers from Ginbichu Hospital, and 34 healthcare workers from Shone Hospital. Finally, a simple random sampling technique was used to include healthcare workers from each hospital by considering the human resource registration as a sampling frame in each hospital (Figure 1).
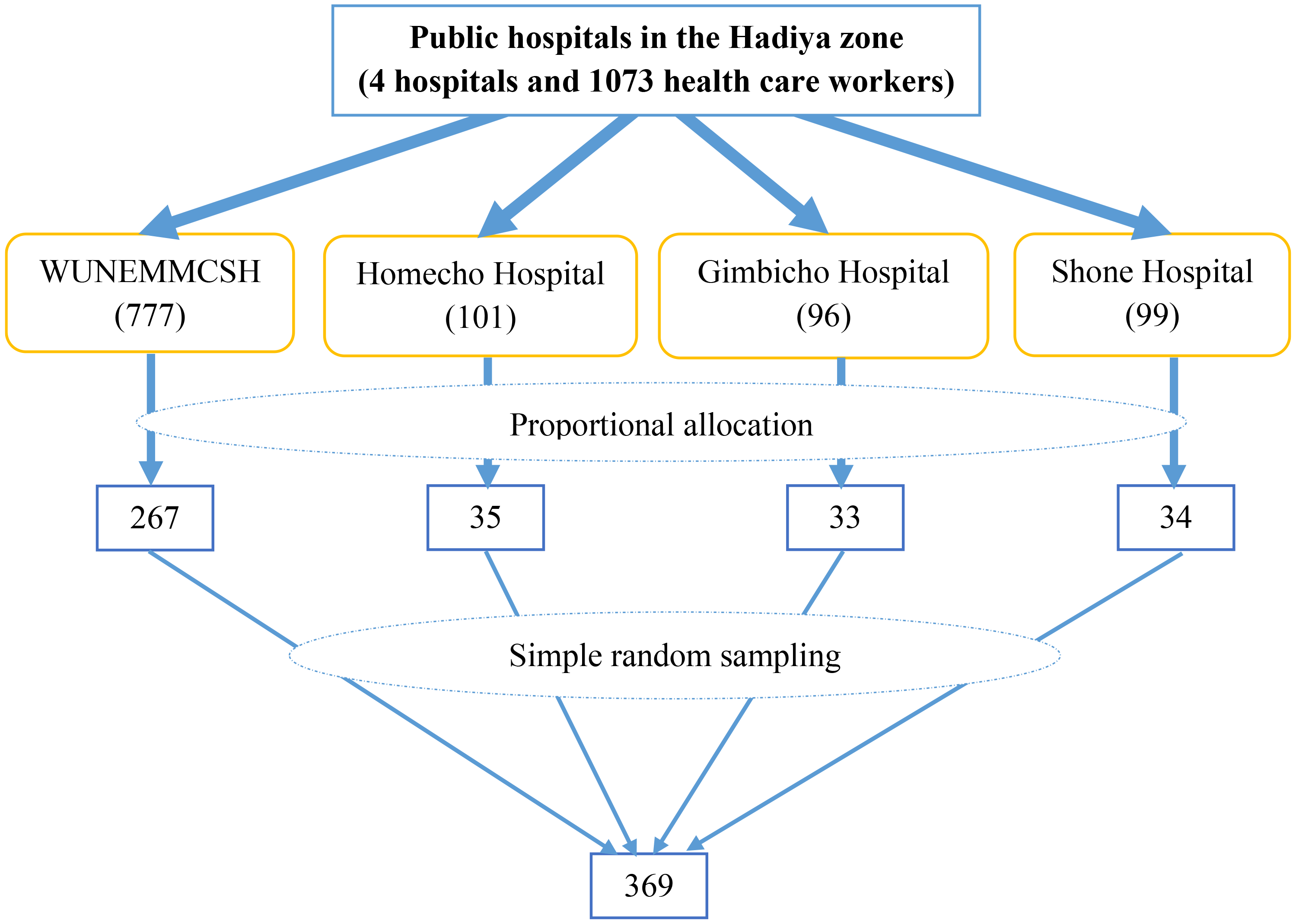
Schematic diagram of the sampling procedure for a study assessing sharp instrument injury and associated factors among health workers working in public Hospitals of Hadiya Zone, Central Ethiopia in 2023.
Study Variables
Independent Variables
Operational Definition
Data Collection Tool and Procedure
Data were collected through a self-administered questionnaire. The tool was structured that was prepared on reviewing different literature (Abebe et al., 2018; Bacha Gemechu, 2020; Borde, 2010; Legesse et al., 2015; Mekonnen et al., 2018; Mengistu et al., 2021). Six biology teachers and four epidemiologists were recruited for data collection and supervision, respectively.
Data Quality Assurance
The tool was prepared in English. A one-day training was given for data collectors and supervisors regarding the objective of the study and ways of data collection, and keeping confidentiality. The pretest was conducted on 5% of the total sample size at Durame town, and the necessary modification was made based on the pretest result before using it for the actual data collection. The supervisors conducted daily supervision and necessary feedback was given for the next day. Each collected data point was checked for completeness daily by supervisors. To determine the internal validity, the Cronbach’s alpha test was done, and it is .856.
Data Analysis
The data were entered into Epi-data Version 3.1 and exported to the Statistical Package for Social Science (SPSS) Version 26 for analysis. Descriptive statistics were computed for all variables according to the type of variables. Categorical variables were assessed by computing frequency and proportions. A binary logistic regression model was used to determine the significant association between dependent and independent variables. First, bivariable logistic regression analysis was conducted between each independent variable and dependent variable. A crude odds ratio (COR) along with a 95% confidence interval (CI) was used to present the results of the bivariable analysis. All variables with association in bivariate analysis at p-value ≤ .05 were entered into a multivariable logistic regression model to assess the adjusted association between dependent and independent variables. An enter method was used to fit a multivariable logistic regression model to identify factors remaining in the model. Multi-collinearity between independent variables was checked for all candidate variables by considering the variable inflation factor and tolerance. The Hosmer-Lemeshow goodness of fit test was used to check model fitness and was satisfied (p-value > .05). The adjusted odds ratio (AOR) along with a 95% CI and p-value < .05 was used to determine the strength of the association and to declare statistical significance in the final model. Finally, the finding was presented using texts, tables, and figures.
Result
Socio-Demographic Characteristics
A total of 368 healthcare workers participated in this study, giving an overall response rate of 99.7%. The mean age of the respondents was 30.43 years with a standard deviation of ± 5.228. Of the healthcare workers, 210 (57.1%) were in the age group of 22–29 years, 219 (59.5%) were female, 257 (69.8%) held a Bachelor of Science degree, and 179 (48.6%) were single. Nurses accounted for 126 (34.2%) of the sample, and 196 (53.3%) had 5 or more years of service (Table 1).
Socio-Demographic Characteristics of Health Workers Working in Public Hospitals of Hadiya Zone, Central Ethiopia in 2023.

Working Environment-Related Factors
The majority, 281 (76.4%), were working both day and night, and similarly, 283 (76.9%) worked for > 40 hr per week. The working department of 85 (23.1%) healthcare workers was the labor and gynecological ward, and 208 (56.5%) reported the absence of a poster about safe injection procedures in the service unit. Supervision from a hospital-authorized body was reported by 166 (45.1%) healthcare workers, and only 142 (38.6%) had taken training about infection prevention and patient safety. Less than half, 149 (40.5%) healthcare workers reported the presence of a protocol for sharp material injury reports in the facility (Table 2).
Working Environment-Related Factors of Health Workers in Public Hospitals of Hadiya Zone, Central Ethiopia in 2023.

Behavior-Related Factors
The majority, 294 (79.9%), use personal protective equipment during the procedure, and one-fourth 92 (25.0%) of them recap needle after injection. The majority, 272 (73.9%) dispose of sharp materials in safety boxes after the procedure, and similarly, 284 (77.2%) segregate sharp waste from other wastes. Only 94 (25.5%) destroy used sharp materials with shreds and 113 (30.7%) healthcare workers report any sharp material injury immediately (Table 3).
Behavior-Related Factors of Health Workers Working in Public Hospitals of Hadiya Zone, Central Ethiopia in 2023 (n = 368).

Sharp Material Injury among Healthcare Workers
Out of the 368 healthcare workers, 113 (30.7%) experienced sharp material injuries in the last 12 months.
Factors Associated With Sharp Material Injury Among Healthcare Workers
In bivariable logistic regression analysis, a poster about safe injection procedure, supervision from hospital authorized body, training about infection prevention and patient safety, protocol about sharp material injury report in the facility, use personal protective equipment during the procedure, recap needle after injection, dispose of sharp materials in safety box after the procedure, segregate sharp waste from other wastes, and report any sharp material injury immediately were significantly associated with sharp material injury among healthcare workers. Whereas in bivariable logistic regression analysis, supervision from hospital authorized body [AOR 0.13, 95% CI: 0.06–0.27], training about infection prevention and patient safety [AOR 0.29, 95% CI: 0.14–0.59], protocol about sharp material injury report in the facility [AOR 0.32, 95% CI: 0.17–0.63], recap needle after injection [AOR 4.89, 95% CI: 2.47–9.72], dispose sharp materials in safety box after procedure [AOR 0.38, 95% CI: 0.16–0.88], segregate sharp waste from other wastes [AOR 0.33, 95% CI: 0.15–0.75], and report any sharp material injury immediately [AOR 0.38, 95% CI: 0.18–0.83] were significantly associated with sharp material injury among healthcare workers (Table 4).
Bivariable and Multivariable Logistic Regression Analysis of Healthcare Workers Working in Public Hospitals of Hadiya Zone, Central Ethiopia in 2023.

Abbreviations: AOR = adjusted odds ratio; CI = confidence interval; COR = crude odds ratio.
“*”: Significant at p-value <.05 and “1” = reference group.
Discussion
The magnitude of sharp material injury in the last 12 months among health workers in Hadiya Zone public hospitals was 30.7% with a 95% CI (25.9–35.3). It was in line with studies conducted in northwest Ethiopia at 31% (Berhan et al., 2021) and Gambela town at 32.2% (Mengistu et al., 2021). This similarity might be because all these facilities are mid-level regional or district hospitals with similar levels of staff training, and national guidelines have been implemented in each hospital.
However, it was higher than in studies conducted in the South Gondar Zone (Berhan et al., 2021) and the Awi Zone (Dilie et al., 2017), where the proportions of injuries were determined during 12-month periods. This might be due to the presence of institutional guidelines, the availability of a safety box, and the proper waste segregation of healthcare workers in the South Gondar and Awi Zone studies. On the other hand, it was lower than a study done in government Hospitals in the Bale Zone, 37.1% (Bekele et al., 2015), Jimma Zone hospitals, 39.3% (Feleke, 2013), and Bahir Dar health centers, 42.8% (Legesse et al., 2015). The possible reasons for these differences might be the lack of adequate sharps disposal sites, such as safety boxes, and lower adherence to standard precautions. Other reasons might be inadequate training and fewer safety guidelines for the prevention of injuries during patient care in our study hospitals. Moreover, adherence to standard precautions may be another possible explanation for this variation.
In this study, supervision from hospital-authorized bodies was significantly associated with sharp material injury among healthcare workers. Healthcare workers who had supervision from the hospital-authorized body were 87% less likely to face sharp material injury compared to those healthcare workers who did not have supervision from hospital hospital-authorized body. The possible explanation for this might be that the supervision from hospital-authorized bodies creates smooth communication among the hospital-authorized bodies and the healthcare workers in identifying training gaps, supplementing personal protective equipment, and other safety and precaution readiness of healthcare workers. In addition, frequent and smooth communication might reduce work tension and enhance self-confidence for health workers.
This study revealed that training about infection prevention and patient safety was significantly associated with sharp material injury among healthcare workers. Healthcare workers who had training about infection prevention and patient safety were 71% less likely to face sharp material injury compared to healthcare workers who did not have training about infection prevention and patient safety. The study findings are similar to studies conducted in Bale Zone (Bekele et al., 2015) and Addis Ababa, Ethiopia (Daniel Nadew, 2015). This implies that updating health professionals on technical skills like standard precautions for self and patient, infection prevention mechanisms, and self-protection methods may decrease the potential exposure.
This study showed that the protocol for sharp material injury reports in the facility was significantly associated with sharp material injury among healthcare workers. Healthcare workers who had a protocol about sharp material injury reports in the facility were 68% less likely to face sharp material injury compared to healthcare workers who did not have a protocol about sharp material injury reports in the facility. The possible explanation for this might be the presence of a protocol about sharp material injury reports in the facility alarms the healthcare workers regarding the safe and proper use of sharp instruments during procedures.
This study suggested that recapping needles after injection was significantly associated with sharp material injury among healthcare workers. Healthcare workers who had to recap the needle after injection were 4.89 times more likely to face sharp material injury compared to healthcare workers who did not recap the needle after injection. The finding is in line with studies conducted in Southern Gondar (Berhan et al., 2021), Awi Zone (Dilie et al., 2017), Arbaminch (Gebretsadik Kelebore, 2016), Hawassa (Kaweti & Abegaz, 2016), Addis Ababa (Daniel Nadew, 2015), and Bahir Dar city (Legesse et al., 2015), Jimma Zone (Belachew et al., 2017), and in Bale Zone (Bekele et al., 2015). This shows that the habit of recapping needles after use increases sharp material injury. In addition, it may be due to that those who had taken the training had a better awareness of standard precautions to be taken for the prevention of sharp material injury and its safety measures.
In this study, the disposal of sharp materials in a safety box after the procedure was significantly associated with sharp material injury among healthcare workers. Healthcare workers who dispose of sharp materials in safety boxes after the procedure were 72% less likely to face sharp material injury compared to healthcare workers who do not dispose of sharp materials in safety boxes after the procedure. This is supported by another study (Berhan et al., 2021) that states disposing of sharp materials properly decreases the odds of sharp material injuries. A possible explanation for this might be disposing of sharp materials properly to eliminate the dangerous wastes that could cause injury.
This study showed that segregating sharp waste from other wastes was significantly associated with sharp material injury among healthcare workers. Healthcare workers who segregate sharp waste from other wastes were 67% less likely to face sharp material injury compared to healthcare workers who do not segregate sharp waste from other wastes. The study findings are similar to the study in southern Gondar (Berhan et al., 2021) in that those unable to dispose of needles and sharp materials separately after use were 3.93 times more likely to sustain needle sticks and sharp injuries than their counterpart. This indicates that the inability to dispose of sharp materials separately may be mixed with other medical wastes and cause injury while collecting the waste.
This study identified that reporting any sharp material injury immediately was significantly associated with sharp material injury among healthcare workers. Healthcare workers who reported any sharp material injury immediately were 62% less likely to face sharp material injury compared to healthcare workers who did not report any sharp material injury immediately. The possibility for this is that a report of sharp material injury from one healthcare worker at a time alarms the rest healthcare workers, and they consider the prevention mechanisms. Literature also suggests that reporting and documenting incidents is one of the basic steps to preventing the occurrence of the injury, and failure to report exposure increases the likelihood of the injury and infection (Becirovic et al., 2013).
Limitations of the Study
The study might be prone to recall and social desirability biases as it assessed the past 12 months. The temporal causality between some explanatory variables and outcomes may not be clearly established due to the cross-sectional design. The step-by-step method was not used to select the best model based on the Akaike information criterion. We suggest longitudinal studies for future researchers.
Implications for Practice
The study assessed and identified the important variables that can be clues for making health strategies and health policies. Reducing injury and maintaining the safety of healthcare workers is the expectation and direction of the Ethiopian Ministry of Health and the World Health Organization. The study identified the need for supervision from hospital managers, training, having a protocol for sharp material injury report mechanism, recapping needles, disposing of sharp materials, segregating sharp waste, and reporting any sharp material injury immediately as significant factors. Therefore, making strategies and activities considering these identifying factors can reduce the occurrence of sharp material injury among healthcare workers.
Conclusion
Three in 10 healthcare workers face sharp material injury. Supervision, training, protocol about sharp material injury reports, recapping, disposing of sharp materials, segregating sharp waste, and reporting any sharp material injury immediately were found to be significant variables for the occurrence of sharp material injury among healthcare workers. Therefore, hospitals should mandate quarterly training, developing and implementing protocols about sharp material injury reports, avoiding recapping needles, proper disposition of sharp materials, proper segregation of sharp waste, and coherent reporting of any sharp material injury immediately might reduce the occurrence of sharp material injury among healthcare workers.
Footnotes
Acknowledgments
We would really like to thank the study participants for their openness to participate kindly provision of the vital records, and scarification of their precious time.
Ethical Considerations
Institutional Review Board of a Hawasa University College of Medicine and Health Science (IRB/170/14).
Informed Consent
A written informed consent was obtained from participants after a detailed explanation of the purpose and benefit of the study right before the individual data collection. The confidentiality issue was assured and their response was kept private. The participants were informed that they had full right to stop or jump any question that was uncomfortable to them at any time.
Authors’ Contribution
Hirut Binora, Alemneh Kabeta, Kumilachew Melak, and Elias Ezo: conceptualization, data curation, formal analysis, investigation, methodology, supervision, validation, visualization, writing–original draft, and writing–review and editing. Hirut Binora, Alemneh Kabetaand, and Asnakech Zekiwos: conceptualization, data curation, formal analysis, investigation, methodology, supervision, validation, visualization, writing–original draft, and writing–review, and editing. Hirut Binora, Kumilachew Melak, Elias Ezo, and Asnakech Zekiwos: conceptualization, formal analysis, methodology, software, and writing–review and editing. Kumilachew Melak, Elias Ezo, and Asnakech Zekiwos: conceptualization, formal analysis, methodology, software, and writing–review and editing. Hirut Binora and Alemneh Kabeta: conceptualization, formal analysis, methodology, software, writing–review and editing. Hirut Binora, Asnakech Zekiwos, and Elias Ezo: conceptualization, formal analysis, methodology, supervision, visualization, writing–original draft, and writing–review and editing. Kumilachew Melak, Elias Ezo, and Asnakech Zekiwos: conceptualization, formal analysis, methodology, software, and writing–review and editing.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research of this study was covered by Fund from Hawassa University. However, the author(s) received no financial support for the authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.

