Abstract
Introduction
Patient safety is a critical competency for nursing students, highlighting the need to equip them with the knowledge and skills required to foster a culture of safety in healthcare systems.
Aim
This study aimed to examine the mediating effect of patient safety confidence, moderated by campaign participation, on the relationship between nursing students’ patient safety attitude and their willingness to participate in patient safety.
Methods
This study utilized a secondary data analysis approach, analyzing data from a patient safety study conducted in South Korea. The participants included 245 fourth-year undergraduate nursing students recruited using nonprobability convenience sampling. Data were collected in April 2023 through an online survey distributed to members of nursing student-focused online communities. The collected data were analyzed using SPSS PROCESS Macro (models 4 and 14) and bootstrapping method.
Results
The findings underscore the critical role of patient safety confidence as a mediating factor and highlight the positive impact of campaign participation in strengthening nursing students’ engagement in patient safety activities. These insights emphasize the interplay between nursing students’ patient safety attitudes, confidence, and experiential learning opportunities.
Conclusion
To enhance nursing students’ willingness to actively participate in patient safety, fostering positive attitudes and confidence through a well-structured educational strategy is essential. Integrating patient safety topics into the nursing curriculum and providing experiential learning opportunities can prepare students to advocate for safety and contribute to a culture of safety in healthcare.
Introduction
Patient safety is a crucial element in evaluating healthcare quality and a fundamental principle in healthcare delivery. In Korea, from July 2016, when the Patient Safety Reporting and Learning System was introduced, to May 2024, a total of 95,098 patient safety incidents were reported, showing a continuously increasing trend in the number of reports (KOPOS, 2024). Since it is impossible to completely predict the problems threatening patient safety in hospitals, building a safe medical environment through cooperation and interaction among medical professionals is essential (Son et al., 2018). Patient safety involves minimizing the potential for patient harm, which requires establishing and properly managing a safe healthcare system (World Health Organization and WHO Patient Safety, 2009). Additionally, various approaches are necessary to strengthen patient safety, including developing patient safety regulations, building structural systems such as facilities, and encouraging medical staff and patients’ active participation in patient safety activities.
Nurses play a critical role in patient safety activities, making their involvement essential to maintaining safe healthcare environments (Baek & Jeon, 2021; Son et al., 2018). Given the significant number of nurses in healthcare settings, integrating patient safety principles into nursing education is vital to prepare future nurses for their roles (De Rezende et al., 2022). This underscores the need for comprehensive education addressing patient safety perspectives within medical curricula (Klamen et al., 2013; Lee et al., 2020). The World Health Organization (WHO), through its “Global Patient Safety Action Plan 2021–2030,” has emphasized incorporating patient safety principles into healthcare education globally (World Health Organization, 2021). Countries like the United States and the United Kingdom have made strides in this area by adopting simulation-based training and standardized curricula to enhance nursing students’ clinical readiness and application of safety concepts (Alderman & Sherwood, 2024). These global efforts highlight the importance of equipping nursing students with the necessary knowledge and skills to foster a culture of safety in healthcare systems worldwide.
Review of Literature
Nursing students, as premedical professionals, play a critical role in patient safety immediately upon entering clinical practice, necessitating the acquisition of proper knowledge and attitudes about patient safety through their educational curriculum (Mugerwa et al., 2021). While patient safety is recognized as a vital component of clinical nursing (Kim et al., 2018), current nursing curricula lack standardization in the time and content devoted to patient safety education, resulting in fragmented approaches across institutions (Lee et al., 2020). Studies have shown that nursing students’ patient safety knowledge and attitudes positively correlate with their confidence (Park & Park, 2014), which in turn enhances patient safety efficacy (Kim & Jo, 2021). Furthermore, patient safety competency has been identified as the most influential factor in nurses’ safety activities in clinical settings (Baek & Jeon, 2021). To cultivate patient safety competency in nursing students, it is essential to develop and implement standardized and effective educational strategies.
Hospitals are encouraging participation in patient safety activities not only for medical staff but also for patients and their caregivers through various campaigns and events. The WHO celebrates World Patient Safety Day, which is observed annually on September 17, and encourages participation in patient safety campaigns to raise public awareness (World Health Organization, 2021). In addition to the Mint Festival, various patient safety events were conducted for both inpatients and outpatients, including the Speak Up campaign, Patient Safety and Experience Hero campaign, Medication Safety Fence campaign, and Hand Hygiene Champion campaign (Kim, 2022; Oh, 2023). Currently, few studies have demonstrated the effectiveness of patient safety campaigns. Therefore, empirical research is needed to report on the positive effects of patient safety campaigns applied to various participants, including patients, medical staff, and nursing students.
The willingness to participate in patient safety, defined as the proactive intention to engage in safety-related activities, is a critical component of patient safety (Lee, 2018). While studies on this topic have primarily focused on hospitalized patients (Woo et al., 2021) or general adults (Shin, 2020), research specific to nursing students remains limited. Participation in patient safety activities during clinical practice is crucial for nursing students’ professional growth. A lack of willingness to engage can hinder their readiness to act as patient safety advocates (Josef et al., 2023). Therefore, systematic strategies are needed to strengthen nursing students’ willingness to participate in patient safety, ensuring their preparedness for future clinical roles.
The results of previous studies confirmed that nursing students’ patient safety attitude increases patient safety confidence (Kim & Jo, 2021; Park & Park, 2014), and patient safety attitudes have a positive correlation with patient safety management behaviors (Son & Park, 2017). Furthermore, patient safety confidence influences the willingness to participate in patient safety activities (Woo et al., 2021). Patient safety attitudes and confidence are essential determinants of effective safety practices. Positive attitudes among nursing students influence their likelihood of adopting safety-oriented behaviors, while confidence in safety practices directly affects their willingness to actively engage in safety initiatives. Thus, nursing students’ direct participation in patient safety campaigns conducted in hospitals will serve as practical education in internalizing patient safety content.
Previous studies have largely focused on practicing nurses and healthcare professionals, with limited exploration of nursing students’ patient safety attitudes, confidence, and willingness to engage in safety initiatives. This study addresses this gap by examining the mediating role of patient safety confidence and the moderating effect of campaign participation in the relationship between nursing students’ attitudes and willingness to participate in patient safety. As future healthcare providers, nursing students represent a critical group for understanding and improving patient safety education and practices. The conceptual model used in this study is a moderate mediation effects model based on existing theoretical frameworks and empirical research (Hayes, 2022). Building on prior research, the authors developed a mediation model proposing that nursing students’ patient safety attitudes influence their willingness to participate in safety activities through their confidence. Additionally, a moderated mediation model was established to explore whether this relationship differs based on participation in patient safety campaigns (Figure 1).

Research models and path coefficient.
This study aims to analyze the impact of nursing students’ patient safety attitudes on their intention to engage in patient safety practices. Additionally, it seeks to examine the mediating role of patient safety confidence and the moderating effect of participation in patient safety campaigns, thereby identifying differences between campaign participants and nonparticipants. The findings will provide actionable insights for educators and policymakers to design targeted interventions, such as structured patient safety education and campaign initiatives, that enhance nursing students’ preparedness to contribute to safer healthcare environments.
Methods
Research Design
This study was a secondary data analysis to examine the relationship between patient safety attitude, patient safety confidence, and willingness to participate in nursing students and the moderating effect mediated by participation in patient safety campaigns. The primary data was a survey on the current status of patient safety education among undergraduate nursing students in Korea (Shin & Baek, 2023), and this study utilized some of the data to identify factors that affect nursing students’ willingness to participate in patient safety.
Research Participants
This study targeted fourth-year nursing students enrolled in nursing departments nationwide, recruiting 245 participants through convenience sampling. Invitations were extended via online platforms commonly accessed by nursing students, ensuring broad accessibility. To enhance representativeness, participants were drawn from diverse geographic regions, including metropolitan, urban, and rural areas, reflecting South Korea's varied educational and clinical training environments. The sample size was calculated using the G*Power 3.1.9.7 program. For regression analysis with a medium effect size of .15 (Lee, 2018), a type I error of .05, a power of .95, and 12 independent variables, the minimum required sample size was determined to be 184. This study utilized primary data comprising 296 nursing students from 132 nursing departments nationwide, selecting 245 students planning to work in general hospitals after graduation, meeting the required sample size and study objectives.
Research Instruments
Patient Safety Attitude
Patient safety attitude was measured using the patient safety/medical fallibility assessment questionnaire developed by Madigosky et al. (2006) for medical students and the patient safety attitude measurement tool modified by Park and Park (2014) to suit nursing students. Patient safety attitude refers to an individual's beliefs, values, and behavioral patterns to ensure patient safety (Sexton et al., 2006). The patient safety attitude questionnaire consists of 16 items, and the response to each item is on a five-point Likert scale (1 = strongly disagree to 5 = strongly agree). The score ranges from 16 to 80 points, and a higher total score indicates a more desirable attitude toward patient safety. The reliability (Cronbach's α) of the tool used in the study by Park and Park (2014) was .68, and in this study, it was .65.
Patient Safety Confidence
Patient safety confidence was measured using the patient safety confidence measurement tool utilized in the study by Park and Park (2014). Patient safety confidence refers to the confidence to perform patient safety management and activities to ensure patient safety (Park & Park, 2014). The measurement tool consists of 10 items, and the response to each item is on a five-point Likert scale (1 = strongly disagree to 5 = strongly agree). The score ranges from 10 to 50 points, and a higher total score indicates higher patient safety confidence. The reliability (Cronbach's α) of the tool used in the study of Park and Park (2014) was .85, and it was also .85 in this study.
Willingness to Participate in Patient Safety
Willingness to participate in patient safety was measured using a modified version of the Willingness to Participate in Patient Safety Questionnaire, originally developed by Lee (2018) based on a literature review and adapted for nursing students. The measurement tool consists of 13 items across four subfactors (providing information, asking questions, verifying, and reporting suspicions). Responses to each item are on a four-point Likert scale (1 = strongly disagree to 4 = strongly agree). The score range is 18 to 72 points, with higher total scores indicating a greater willingness to participate in patient safety activities. The reliability (Cronbach's α) of the tool used in the study by Lee (2018) was .88, and in the present study, it was .92.
Participation in Patient Safety Campaigns
Participation in patient safety campaigns was assessed by asking respondents to indicate “Yes” or “No” regarding their experience of participating in such campaigns during clinical practice at hospitals. The questionnaire defined patient safety campaigns as event-type activities conducted in hospitals targeting medical staff, patients, and caregivers. Respondents were also asked to write specific campaign names or content. Nursing students’ responses included campaigns such as “Mint Festival,” “Hand Hygiene Monitoring,” “Case Exhibitions,” “Photo Contests,” “Safety Rounding,” and “Leaflet Distribution,” which were themed on patient safety activities such as patient identification, infection prevention, and fall prevention.
Sociodemographic Variables
The sociodemographic variables collected in this study were selected to provide a comprehensive understanding of the participants’ general characteristics and their potential influence on patient safety attitudes, confidence, and willingness to participate. The variables include gender, age, major satisfaction, practice satisfaction, practice period, patient safety education, patient safety training, and patient safety campaign.
Data Collection Methods and Ethical Considerations
The content and method of this study were approved by the Institutional Review Board (IRB) of S University (IRB No: SYU-2023–01–006–002). The data-collection period was from April 19 to 21, 2023. Nursing students were recruited by obtaining permission from the cafe manager and posting a notice in the meeting room for fourth-year students preparing for employment. This study sent a URL address where participants who voluntarily consented could complete the survey, and conducted a web survey until the target number was reached. Before starting the online survey, a research participant explanation was provided to introduce the purpose, content, and procedure of the study. Participants were informed that they could stop or withdraw at any time by expressing their intention to stop responding to the survey or requesting to withdraw consent, without incurring any disadvantages. If the subject read the explanation and checked “agree” on the online consent form, this was replaced with written consent. The collected data (name of the affiliated university, age, gender, etc.) were stored in a locked file to ensure confidentiality, and it was suggested that incomplete data would be automatically deleted. It took about 10 min to complete the questionnaire, and gift certificates were provided to all participants who completed the questionnaire.
Data Analysis
Data were analyzed using the SPSS 25.0 program (IBM Corporation, Armonk, NY, USA). The participants’ general characteristics were analyzed using frequency analysis. Frequency analysis was performed to examine the participants’ general characteristics. Differences in patient safety attitude, patient safety confidence, willingness to participate in patient safety, and campaign participation based on general characteristics were analyzed using the χ2 test, independent t-test, and one-way analysis of variance (ANOVA), with Scheffé's test applied for post hoc analysis. The correlations between patient safety attitude, confidence, and willingness to participate were analyzed using Pearson's correlation coefficient. The mediating effect of patient safety confidence on the relationship between patient safety attitude and willingness to participate in safety activities was analyzed using PROCESS Macro Model 4. The significance of the indirect (mediation) effect was determined using the bootstrapping method, which extracted 10,000 resamples to calculate the 95% confidence interval (CI). To examine the moderated mediation effect of campaign participation (contrast coded as nonparticipants = “0” and participants = “1”) on the relationship between patient safety attitude and willingness to participate, PROCESS Macro Model 14 was applied. Conditional indirect effects were presented by calculating the 95% CI using the bootstrapping method, providing insights into the interaction between patient safety confidence and campaign participation.
Results
General Characteristics
Table 1 shows the participants’ general characteristics. Most of the participants were female students (221, 90.2%), and the majority were in the 21 to 22 age group (55.9%). Satisfaction with the major was “satisfactory” for 199 students (81.2%). Satisfaction with clinical practice was high for 177 students (72.2%). The clinical practice period was “4 months or more” for the largest number of 179 students (73.1%), and 233 students (95.1%) responded that they had experience in patient safety education. The most effective method for patient safety education was practical training at the hospital site for 125 students (51.0%), followed by simulation education for 69 students (28.2%), media-based (video, VR/AR) education for 33 students (13.5%), and lecture and leaflet for 18 students (7.3%). During the clinical practice period, 101 students (41.2%) participated in the patient safety campaign, while 144 students (58.8%) did not participate. Differences in patient safety attitude, patient safety confidence, willingness to participate in patient safety, and participation in campaigns by demographics.
Differences Patient Safety Attitude, Confidence, Willingness to Participate and Campaign Participate According to Demographics (N = 245).
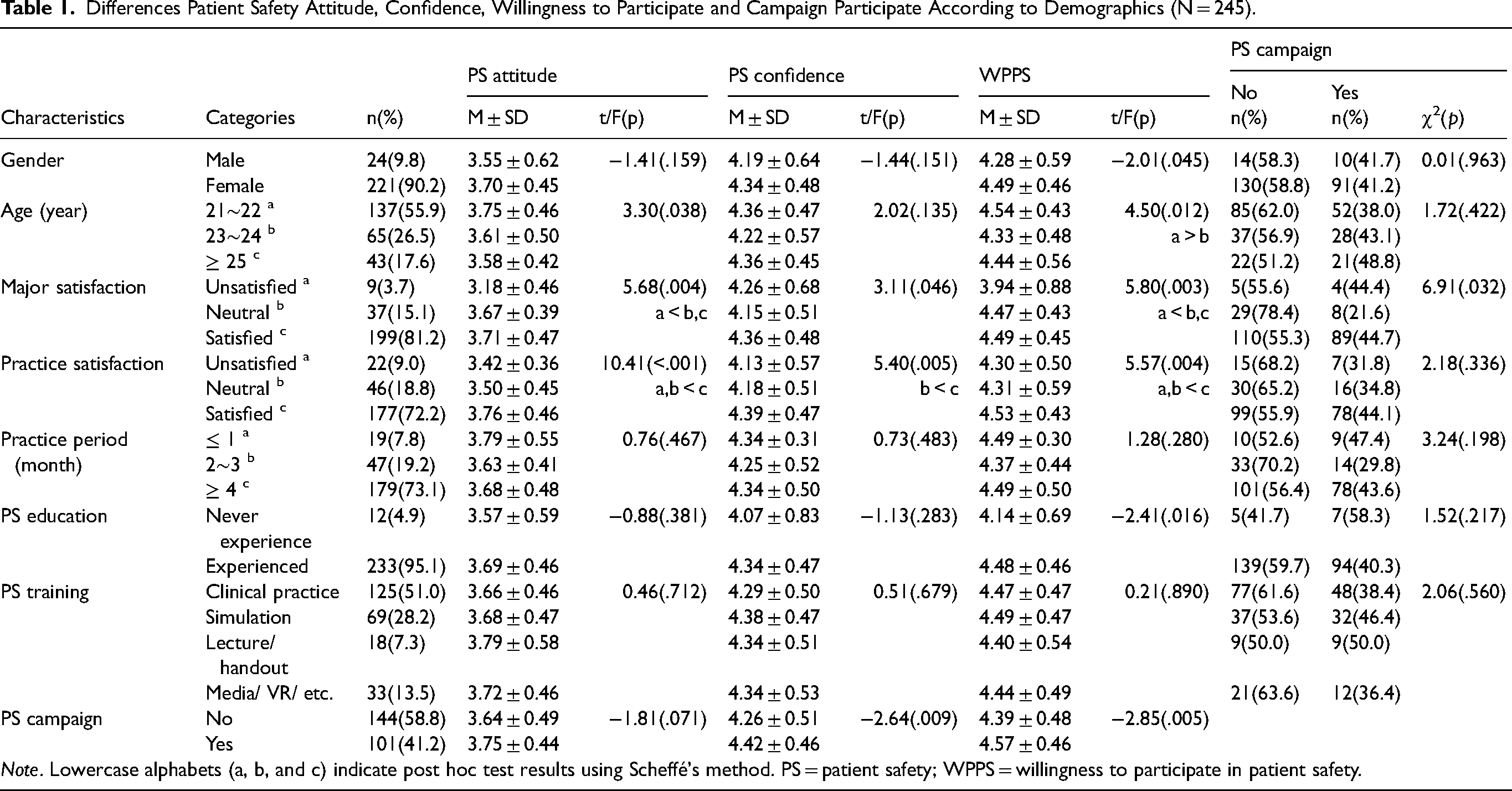
Table 1 shows the differences in research variables by general characteristics. Patient safety attitude showed considerable differences by age (F = 3.30, p = .038), major satisfaction (F = 5.68, p = .004), satisfaction with clinical practice (F = 10.41, p < .001), and the timing of patient safety education (F = 3.06, p = .029). As a result of the post-test, the patient safety attitude scores of the satisfied and average groups were higher than those of the dissatisfied group for specialty satisfaction, and the patient safety attitude scores of the satisfied group were higher than those of the average and dissatisfied groups for clinical-practice satisfaction. The post-test results revealed no significant difference in patient safety attitude scores between groups based on age.
Patient safety confidence showed significant differences depending on clinical practice satisfaction (F = 5.40, p = .005) and participation in patient safety campaigns (t = −2.64, p = .009). As a result of the post-test on clinical-practice satisfaction, the patient safety confidence score was higher in the satisfied group than in the average group, and the patient safety confidence score was higher in the group with experience in participating in patient safety campaigns than in the group without.
Significant differences in willingness to participate in patient safety were observed by gender (t = −2.01, p = .045), age (F = 4.50, p = .012), major satisfaction (F = 5.80, p = .003), satisfaction with clinical practice (F = 5.57, p = .004), experience with patient safety education (t = −2.41, p = .016), and participation in patient safety campaigns (t = −2.85, p = .005). Female students had higher willingness to participate in patient safety scores than male students, and those aged 21 to 22 had higher scores than those aged 23–24. The results of the post-test showed that the satisfaction and average groups had a higher willingness to participate in patient safety than the dissatisfied group in terms of major satisfaction, and the satisfaction group had a higher willingness to participate in patient safety than the average and dissatisfied groups in terms of clinical-practice satisfaction. The group with experience participating in patient safety campaigns had a higher willingness to participate in patient safety than the group without. A statistically significant difference in major satisfaction was found between participants and nonparticipants in patient safety campaigns (χ2 = 6.91, p = .032). Correlations between patient safety attitude, patient safety confidence, and willingness to participate in patient safety.
Table 2 presents the descriptive statistics and correlations of the research variables. Patient safety attitude was 3.68 points (±0.47); patient safety confidence was 4.33 points (±0.50), and patient safety participation willingness was 4.47 points (±0.48). Analysis of the correlation between patient safety attitude, patient safety confidence, and willingness to participate in patient safety revealed that patient safety attitude had a significant positive correlation with patient safety confidence (r = .30, p < .001) and willingness to participate in patient safety (r = .41, p < .001). Patient safety confidence showed a significant positive correlation with patient safety participation willingness (r = .50, p < .001). The mediating effect of patient safety confidence on the relationship between patient safety attitude and willingness to participate in patient safety.
Descriptive Statistics and Correlation of Patient Safety Attitude, Confidence, and Willingness to Participate in Patent Safety (N = 245).
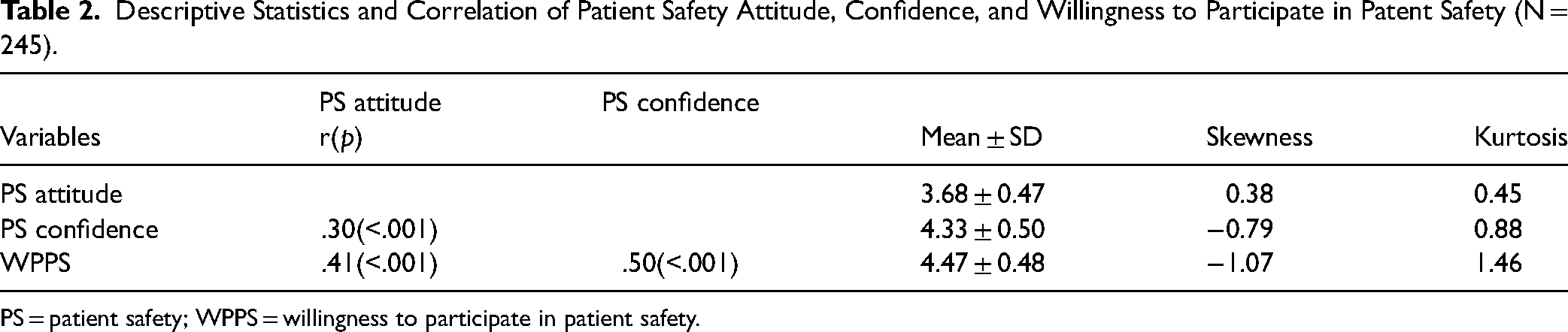
PS = patient safety; WPPS = willingness to participate in patient safety.
Before performing regression analysis, the basic assumptions were confirmed. The skewness of patient safety attitude, patient safety confidence, and willingness to participate were all ±2 or less, and the kurtosis was 7 or less, confirming that they were normally distributed. The Durbin-Watson value was 1.84, and the results of calculating the variance inflation factor (VIF) confirmed that no autocorrelation and multicollinearity problems among independent variables were in the range of 1.03 to 1.52, which satisfied the assumptions.
After controlling for age, major satisfaction, and clinical practice satisfaction, which showed significant differences in nursing students’ willingness to participate in patient safety, the mediating effect of patient safety confidence on the relationship between patient safety attitude and willingness to participate in patient safety was confirmed using PROCESS Macro (model 4; Table 3). In step I, patient safety attitude (independent variable) was found to significantly affect willingness to participate in patient safety (dependent variable) (B = 0.37, p < .001). In step II, patient safety attitude had a significant effect on patient safety confidence (mediator variable) (B = 0.23, p = .001). In step III, patient safety attitude (B = 0.28, p < .001) and patient safety confidence (B = 0.39, p < .001) had a significant effect on willingness to participate in patient safety. As a result of analyzing the mediating effect of patient safety confidence in the relationship between patient safety attitude and willingness to participate in patient safety, the mediating effect was 0.09, and the 95% confidence interval [0.02, 0.18] did not include 0 (zero).
The Mediating Effect of Patient Safety Confidence on the Relationship Between Patient Safety Attitude and Patient Safety Attitude and Willingness to Participate in Patient Safety (N = 245).
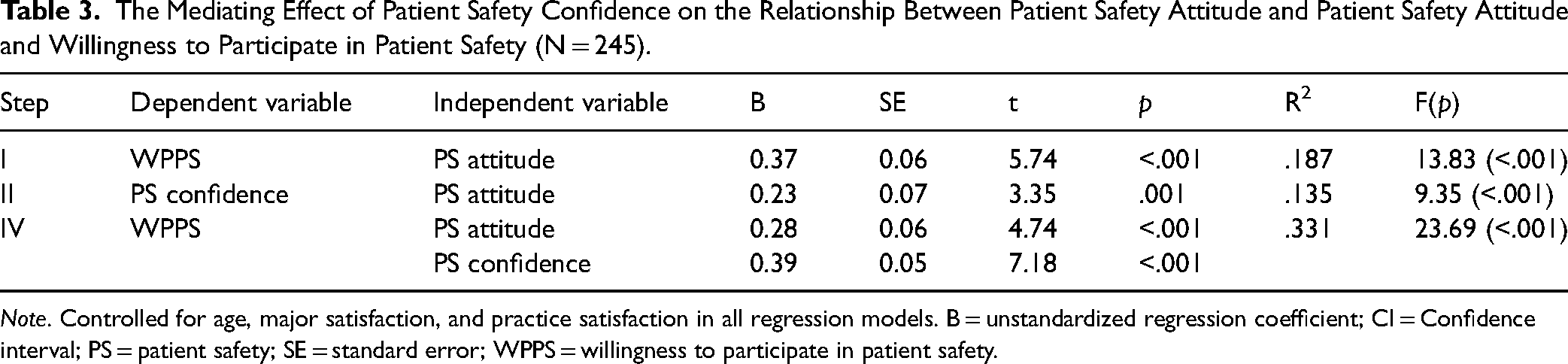
Note. Controlled for age, major satisfaction, and practice satisfaction in all regression models. B = unstandardized regression coefficient; CI = Confidence interval; PS = patient safety; SE = standard error; WPPS = willingness to participate in patient safety.
The Mediating Effect of Patient Safety Confidence Moderated by Campaign Participation
After controlling for age, major satisfaction, and clinical practice satisfaction, which showed significant differences in nursing students’ willingness to participate in patient safety, PROCESS Macro (model 14) was used to analyze whether campaign participation moderated the mediating effect of patient safety confidence (Table 4). In step II, patient safety attitude (independent variable), patient safety confidence (mediator variable), and participation in patient safety campaigns (moderator variable) were input to confirm the effects on the willingness to participate in patient safety (dependent variable). Patient safety attitude had a significant positive effect on the willingness to participate in patient safety (B = 0.28, p < .001), and patient safety confidence had a significant positive effect on the willingness to participate in patient safety (B = 0.72, p < .001). Additionally, the interaction term between patient safety confidence and participation in patient safety campaigns was statistically significant, confirming the moderating effect (B = −0.24, p = .024). The explanatory amount of the final model was 35.2% (R2 = .352, F = 18.35, p < .001). The research model is diagramed with path coefficients, as shown in Figure 1.
The Mediating Effect of Patient Safety Confidence Between Patient Safety Attitude and Willingness to Participate in Patient Safety and Moderated Mediation Effect Analysis of Patient Safety Campaign Participation (N = 245).

Note. Controlled for age, major satisfaction, and practice satisfaction in all regression models. B = unstandardized regression coefficient; CI = Confidence interval; PS = patient safety; SE = standard error; WPPS = willingness to participate in patient safety.
Since the mediating effect of patient safety confidence in the relationship between patient safety attitude and willingness to participate was moderated by campaign participation, the conditional indirect effect was calculated and presented in Table 5. For nonparticipants in patient safety campaigns, it was 0.11 (95% CI [0.02, 0.23]), and for participants, it was 0.05 (95% CI [0.01, 0.12]).
Conditional Indirect Effects (N = 245).

B = unstandardized regression coefficient; CI = Confidence interval; PS = patient safety; SE = standard error; WPPS = willingness to participate in patient safety.
The result that the mediation effect was lower for patient safety campaign participants than for nonparticipants was due to the moderating effect in the relationship between patient safety confidence and willingness to participate in patient safety. Therefore, the moderating effect of patient safety campaign participation was diagramed to help understand the research results. As shown in Figure 2, when patient safety confidence was high, both campaign participants and nonparticipants exhibited high willingness to participate in patient safety. However, when patient safety confidence was low, the willingness to participate decreased more sharply among nonparticipants.

Moderating effect of campaign participation on the relationship between patient safety confidence and willingness to participate in patient safety.
Discussion
This study confirmed the relationship between nursing students’ attitudes toward patient safety, patient safety confidence, and willingness to participate in patient safety and analyzed whether the experience of participating in patient safety campaigns moderated the mediating model. Based on the research results, the following discussions are proposed.
The subgroup analyses revealed key demographic differences influencing nursing students’ engagement in patient safety, offering valuable insights for targeted interventions. While age was not significantly associated with patient safety attitude or confidence, students aged 25 and older demonstrated greater willingness to participate, suggesting that maturity positively influences engagement. Gender differences were also evident, with female students reporting higher confidence and willingness than their male counterparts, highlighting the need for targeted training programs to enhance male students’ participation. Participation in patient safety campaigns significantly boosted confidence and willingness to engage in safety activities, whereas nonparticipants with low confidence showed a sharp decline in engagement. This underscores the importance of expanding opportunities for campaign involvement to improve overall participation. Integrating experiential learning methods and international best practices, such as interprofessional simulations, could address these disparities and strengthen nursing students’ readiness to advocate for patient safety (El Hussein et al., 2022). Tailored educational strategies and experiential interventions based on these subgroup differences could enhance the effectiveness of nursing education and contribute significantly to fostering a culture of safety in healthcare settings.
The findings of this study underscore the importance of fostering a positive patient safety attitude among nursing students to enhance their willingness to engage in safety activities. It is difficult to make a direct comparison as no previous study has examined the willingness of nursing students to participate in patient safety. However, similar to previous research, which found a positive correlation between patient safety attitudes and management behavior (Son & Park, 2017) and a direct effect of safety perception on participation willingness in general adults (Shin, 2020), this study highlights the pivotal role of education. Nursing students encounter patient safety topics throughout their studies, and structured education combining theoretical and practical components is essential for cultivating accurate knowledge, attitudes, and active participation. In a study conducted on hospitalized patients, the willingness to participate in patient safety was found to be a factor that increased patient-participation behavior (Won & Shin, 2024). Moreover, patient safety management education during both academic and clinical training significantly influences students’ safety practices (Choi & Lee, 2015; Jeong et al., 2017). From a clinical perspective, developing nursing students’ willingness to participate in patient safety can have far-reaching implications for healthcare quality. Therefore, structured patient safety education, encompassing both theoretical and practical components, is vital for ensuring their preparedness and effectiveness in clinical settings.
The mediating role of patient safety confidence in the relationship between nursing students’ patient safety attitude and their willingness to participate highlights its critical importance. This finding aligns with previous studies showing that patient safety confidence directly impacts willingness to participate (Woo et al., 2021) and is influenced by patient safety attitude (Jeong et al., 2017). Similar patterns were observed in general hospital inpatients, where safety perception influenced participation behavior via willingness (Won & Shin, 2024). However, conflicting results were reported in emergency medical students, where patient safety attitude did not affect confidence (Ham et al., 2017). Additionally, clinical practice satisfaction significantly influenced nursing students’ attitudes, confidence, and willingness, underscoring the importance of practice-based education. Although theory classes were found to contribute more to confidence development as students advanced in grade (Kim & Song, 2019), other studies reported that group activities and practical training improved knowledge but not attitudes or performance (Kim et al., 2023). To address these gaps, systematic integration of patient safety topics into the nursing curriculum is essential. Experiential learning methods, including simulations, role-playing, and campaign participation, can effectively boost confidence and engagement. By prioritizing these approaches, nursing education can prepare students to become proactive advocates for patient safety, ultimately enhancing healthcare outcomes.
This study revealed that patient safety confidence plays a critical role in the relationship between patient safety attitude and willingness to participate in safety activities, particularly for nonparticipants in patient safety campaigns. While high confidence led to high willingness regardless of campaign participation, low confidence significantly reduced willingness among nonparticipants, emphasizing the need for targeted interventions to boost confidence in this group. Strategies could include simulation-based training, interactive workshops, and peer mentorship programs aimed at fostering confidence and providing practical exposure to patient safety principles. Examples of campaigns like Korea's “Mint Festival,” featuring activities such as patient safety pledges and safety improvement posters (Lee, 2023; Oh, 2023), and global initiatives like the “Speak-up” and “Good-catch” campaigns (Kane et al., 2023; Lozito et al., 2018; Ozieranski et al., 2014; Tetteh et al., 2022), demonstrate how active participation can improve safety perceptions. Universities should embed experiential learning opportunities into nursing curricula, incorporating interprofessional simulations, role-playing scenarios, and case-based discussions to bridge theory and practice. Hospitals can support these efforts by designing campaigns that involve nursing students during clinical rotations and through university collaborations, offering feedback sessions to reinforce learning and confidence. Expanding campaign schedules and diversifying activities to include students with limited clinical access would further enhance engagement and foster a culture of patient safety.
This study analyzed factors influencing the willingness to participate in patient safety among 245 fourth-year nursing students and identified several limitations. First, data collection from an online nursing student café may have introduced selection bias, as online participants might differ in engagement or interest compared to nonusers, limiting generalizability. Future research should employ stratified sampling and diverse recruitment channels to ensure a representative sample. Second, the reliability of the patient safety attitude measurement tool was low (Cronbach's alpha = .65), highlighting the need for refining and validating measurement tools for greater accuracy. Third, systematic and practical patient safety campaign programs should be developed and integrated into theoretical and clinical education to enhance students’ adaptability and engagement. Finally, longitudinal studies are recommended to track changes in attitudes, confidence, and willingness over time, alongside experimental designs to compare the effectiveness of various campaign strategies, providing deeper insights into long-term outcomes.
Conclusions
This study confirmed a significant positive correlation between patient safety attitude, confidence, and willingness to participate in safety activities among fourth-year nursing students. The mediating effect of patient safety confidence, moderated by campaign participation, was stronger in nonparticipants, highlighting the need for targeted interventions to boost confidence in this group. Clinical practice satisfaction also significantly influenced patient safety attitudes, confidence, and willingness, underscoring the importance of practical education. To enhance nursing students’ willingness to participate, fostering a positive attitude toward patient safety and increasing confidence through experiential learning opportunities is essential. Policymakers and hospital administrators should design and expand patient safety campaigns that actively involve nursing students, particularly during clinical rotations, to address gaps for nonparticipants. These strategies can help prepare nursing students to become proactive advocates for patient safety, fostering a safety culture in healthcare and improving patient outcomes.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Statement
Ethical approval was sought and granted by the Institutional Review Board of Sahmyook University (SYU 2023-01-006-002).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Research Foundation of Korea (grant number NRF No. 2022R1F1A106447512).
