Abstract
Introduction
Monkeypox (mpox) is an evolving infectious disease caused by the monkeypox virus (MPXV). On July 23, 2022, the WHO declared the recent mpox outbreaks a public health emergency of international concern (PHEIC), which terminated on May 11, 2023. As of July 11, 2023, 88,288 confirmed cases and 149 deaths have been reported from 112 countries and territories. Currently, mpox is not a PHEIC, as the outbreak and its impacts are nearly over. Nurses played significant roles during the mpox 2022 outbreak as frontline workers.
Purpose
In light of the impending mpox global outbreak in 2022, this brief report provides an update on the enormous difficulties faced by frontline nurses while playing a crucial role in handling the mpox outbreak and some potential solutions to these difficulties. The methodological framework employed in this narrative brief report involves conducting a comprehensive analysis and synthesis of relevant literature and hypothetical scenarios. The aim is to put forth practical strategies that can effectively tackle the difficulties encountered by frontline nurses in the context of the mpox outbreak. Additionally, the report seeks to envision a healthcare system that is more resilient in the face of future challenges.
Conclusion
It is important to understand the challenges the nurses face from their perspective. As frontline health care workers, the various health issues of nurses and their concerns must be taken care of appropriately by adopting optimum health service practices, adequate safety measures, recommended precautionary measures, and boosting them mentally while handling mpox patients. Counseling and the arrangement of workshops are required. Appropriate care should be taken to address the various health issues concerning nurses by adopting health service practices at optimum levels. Side by side, recommended safety and precautionary measures should be followed.
Keywords
Introduction and Purpose
Monkeypox (mpox) is an evolving and re-emerging infectious disease caused by the monkeypox virus (MPXV), and on July 23, 2022, the WHO declared the recent mpox outbreaks a public health emergency of international concern (PHEIC), which terminated on May 11, 2023 (Burki, 2023). As of July 11, 2023, 88,288 confirmed cases from 112 countries and territories, and 149 deaths have been reported (Centers for Disease Control and Prevention [CDC], 2022) As of now, the PHEIC status of mpox has been lifted since mpox outbreak 2022 and its health impacts are nearly over now.
In the face of unprecedented global health crises, frontline nurses emerge as the unsung heroes, confronting immense challenges and demonstrating extraordinary resilience in the fight against infectious diseases. The significance of the nursing profession has been underscored by the occurrence of infectious diseases, such as COVID-19 and mpox (Guelbert, 2022; Saied et al., 2023; Shaffer et al., 2022; Thornhill, Barkati, et al., 2022). The outbreak of mpox, severe viral pathogen, has brought into stark relief the unique set of challenges encountered by nurses in the front lines of healthcare delivery (Ibrahim et al., 2022). During the mpox outbreak, frontline nurses faced a wide range of difficult challenges. One of the primary challenges was the substantial surge of patients, as the virus rapidly disseminated, inundating hospitals with individuals in serious condition (Salvato et al., 2022). The sudden increase in patient numbers imposed a significant strain on nurses, who faced challenges due to limited bed availability and resources. They frequently worked long hours in an effort to uphold the standard of care. Furthermore, they encountered the formidable obstacle of insufficient accessibility to personal protective equipment (PPE), encompassing masks, gowns, and gloves (Dubey et al., 2023; Ibrahim et al., 2022). The limited availability of crucial protective equipment not only increased the likelihood of infection but also induced psychological anguish among nurses, who were concerned about sharing the virus to their families and communities. Furthermore, frontline nurses had a significant emotional and psychological burden (Almarwani et al., 2023). They observed the distress experienced by patients and frequently experienced separation from their loved ones as a result of quarantine protocols. The persistent apprehension regarding the acquisition and dissemination of the virus, along with ethical and moral quandaries linked to the allocation of resources, engendered a climate of stress, anxiety, and moral anguish among nurses, thereby impacting their psychological welfare and general standard of living. The potential long-term consequences of the psychological stress experienced by healthcare workers emerged as a significant concern during the mpox outbreak.
There exists a notable paucity in the scholarly literature with regard to a comprehensive analysis of the precise challenges confronted by nurses in the context of mpox outbreaks, the ramifications of these challenges on the overall healthcare delivery, and the identification of effective strategies aimed at alleviating these obstacles in order to enhance the preparedness of nurses for future mpox outbreaks. The aim of this article is to highlight the risk factors, challenges, and prevention and control measures to safeguard the health of nurses as frontline workers amid the mpox outbreaks. The best way to prevent mpox infection is to avoid being exposed to the virus; thus, spreading knowledge about the risk factors for contracting the disease and the preventative actions that may be taken by individuals, such as nurses, is crucial. This knowledge will aid in raising awareness of high-risk variables and educating individuals, particularly nurses, on mitigation actions they may take to limit exposure to the virus, which is the primary prevention strategy for mpox.
The present narrative brief report utilizes a methodological approach that entails undertaking a thorough examination and synthesis of pertinent literature and hypothetical scenarios. The objective is to propose pragmatic approaches that can efficiently address the challenges faced by frontline nurses within the context of the mpox outbreak. Furthermore, the objective of the report is to conceptualize a healthcare system that exhibits enhanced resilience in response to forthcoming difficulties. Furthermore, our research primarily centered on scholarly articles about healthcare workers, particularly nurses, in the context of the mpox outbreak that occurred between 2022 and 2023. The publications considered in this study were published in the English language and specifically focused on the nursing-related concerns connected with mpox. The design of the investigation was not limited.
Brief Review
Since the smallpox vaccine was discontinued after the disease was declared eradicated in 1980, the unvaccinated population is at a higher risk of contracting MPXV. There is an urgent need to learn more about the origins and dynamics of the spread of mpox so that individuals can be better prepared to protect themselves and others in the face of public health emergencies. To date, the epidemiology of the current mpox virus infection has not been well reported (Strathdee et al., 2023). The clinical presentation of mpox patients throughout this outbreak has been diverse so far. In areas where mpox have been an issue for a long time, more research is needed to understand the ongoing and new sources of infection.
The mpox virus can be spread to humans from infected animals, usually rodents. Human-to-human transmission occurs through direct contact with an infected person's skin lesions, scabs, bed linen, needle-stick injury, and clothing (Ahmed, Dabou, Abdelsamad, Mohamed, Chandran, Chakraborty, et al., 2023; Ahmed, El-Kader, Lorenzo, Chakraborty, Dhama, Mohammed, et al., 2023; Ahmed, Mohamed, Dabou, Abuijlan, Chandran, El-Shall, et al., 2023; Ahmed, Rashad, et al., 2022; Altindis et al., 2022; Harapan et al., 2022; Migaud et al., 2023; Mitjà et al., 2023). Respiratory excretions can also result in the spread of the disease from one person to another, where mpox virus particles can remain infectious in aerosols for 18–90 hours (Verreault et al., 2013), and mpox disease usually lasts 2–4 weeks (Ophinni et al., 2022). The invasion period (lasting 0–5 days) is distinguished by fever, headache, lymphadenopathy, back discomfort, myalgia, and extreme asthenia (Adler et al., 2022). The skin eruption starts 1–3 days after hyperthermia. Faces and extremities are frequently affected (Ahmed, Rashad, et al., 2022; Girometti et al., 2022; Scotti et al., 2023; Tarín-Vicente et al., 2022). The person is infected until the sores have healed and the scabs have come off.
Amid a slew of public health crises, infectious diseases pose a significant risk to the population at large. Healthcare workers' ability to respond to epidemics is essential for the development of executive strategies to handle the difficulties of possible public health emergencies (Ahmed, El-Kader, Lorenzo, Chakraborty, Dhama, Mohammed, et al., 2023; Kumar et al., 2022; Malerba et al., 2020). A substantial role is played by nurses in order to respond to health emergencies like mpox that affect people globally (Organization, 2013; Rony et al., 2023). The role of frontline nurses in disease prevention and surveillance is crucial in case management, as they are the primary team reacting to illness problems during epidemic events in a range of clinical settings. As a result, it is critical that nurses have plans in place to deal with a mpox epidemic (Thornhill, Palich, et al., 2022). Prioritizing the preparation of frontline nurses to deal with infectious diseases is essential when considering the crucial role, they play in the management of current epidemics (Barton & Oladokun, 2022; Kumar et al., 2022). When an epidemic strikes, frontline nurses are counted on to keep their communities safe and alert. There has been a worldwide outbreak of COVID-19, which has wreaked havoc on healthcare providers, testing facilities, public health monitoring systems, safety equipment, and emergency response facilities around the world. The spread of mpox could get out of hand if people do not report cases quickly enough to get them checked out and treated (Rao et al., 2022; Wisner, 2023).
Better clinical management of mpox is needed to reduce symptoms, prevent complications, and shorten the duration of any lasting effects (Ahmed, Mohamed, Dabou, Abuijlan, Chandran, El-Shall, et al., 2023; Kipps, 2022). The best way to stop the spread of mpox is to make people aware of the risks they face and the steps they may take to limit their exposure to the virus (Kumar et al., 2022). Moreover, monitoring the spread of the disease and recording any new instances as soon as they occur are essential for stopping an epidemic in its tracks. During an outbreak of human mpox, the most important risk factor for contracting the virus is intimate contact with an infected patient (Landers et al., 2022). Infection is more common among the families of frontline nurses. Standard infection control precautions, including a single-use N95 respirator, isolation gown, head and shoe covering, googles, hand hygiene, and gloves, should be used by healthcare workers caring for patients with suspected or confirmed mpox virus infection or handling samples from these patients (Ibrahim et al., 2022; Meyer et al., 2023; Miller et al., 2022; Todd, 2022). Furthermore, every health care worker, including nurses, who is exposed to the virus should go through a thorough assessment of their risk for ascertaining their exposure to mpox virus. On the basis of the level of risk counseling regarding isolation, monitoring of oneself and reporting in a timely manner should be offered to them (Manirambona et al., 2023).
All nurses, regardless of sexual orientation or gender identity, should be screened for mpox if they get a rash that looks like the classic case. To spread MPXV, all it takes is direct contact with a patient's lesions, respiratory secretions, or infected things like clothing or bedding. There is currently a low level of threat among the general population (Pinto et al., 2023). Despite the fact that the risks of healthcare-associated illnesses have not yet been identified for this outbreak, nurses who come into contact with infected patients should prevent infections by taking appropriate personal safety measures, including wearing adequate PPE (Ren et al., 2022). Since immunocompromised people are more likely to become really ill with mpox and even die from the virus, the spread of mpox among more susceptible populations could have more devastating health consequences. Nurses and other healthcare workers have a crucial role in preventing the spread of mpox from person to person by educating the public and responding quickly to confirmed cases with isolation, contact tracing, clinical management, and infection prevention measures (Aden et al., 2023; Ahmed, Abdulqadir, Omar, Hussein, Qurbani, Mohamed, et al., 2023; Choi et al., 2023).
Isolation of the patient and protection of the skin and mucous membranes are cornerstones of nursing care for mpox patients. When a patient loses their appetite, they risk becoming dehydrated. The nurse's responsibilities include rehydrating and feeding the patient, checking their vital signs, and keeping a close eye out for complications (Ibrahim et al., 2022; Salvato et al., 2022). The patient should also cover skin lesions as much as possible and use a triple-layer mask to prevent the spread of the disease (e.g., long sleeves, long pants) (Ibrahim et al., 2022). To date, there are no clinically proven therapies for mpox illness (Ahmed, El-Kader, Abdulqadir, Abdullah, Nahed, Chandran, et al., 2023). Most viral illnesses require supportive care, such as fever reducers and fluid replacement to avoid dehydration (Webb et al., 2022). Finally, nurses are the unsung heroes of healthcare. The response to mpox outbreaks and other pandemics depends critically on the safety of medical personnel. Nurses around the world express worry about the lack of resources available to them and their own personal safety in the event of a major epidemic of an infectious disease. Bed and garment changes, contact with lesions, and breathing in a patient's respiratory droplets provide the greatest risks to nurses (Kava et al., 2022). The formation of an effective response to a mpox outbreak requires the close coordination of nurses, health organizations, and authorities on a practical level. A readily adaptable policy framework and set of protocols are also crucial to reducing the prevalence of nosocomial infections in healthcare settings (Mendoza et al., 2022; Miller et al., 2022). Table 1 presents various approaches aimed at mitigating the challenges faced by nurses during a monkeypox epidemic.
Approaches to Mitigate Difficulties Encountered by Nurses Amidst a Monkeypox Epidemic and Similar Infectious Disease Outbreaks.

Discussion
Healthcare providers must have access to ongoing training opportunities, whether they be in-person, online, or a hybrid, if they are to advance their knowledge and skills, sustain the delivery of high-quality treatment, and keep patient outcomes positive. In order to battle infectious diseases, healthcare workers should be educated to give screening, clinical management and treatment, necessary care, and support to patients. Evidence-based teaching methods and state-of-the-art digital study aids should be integrated into these courses (Goyal et al., 2022; Le Pluart et al., 2022). To facilitate rapid scaling-up of response efforts in high-risk nations, an mpox readiness and response curriculum was established. This curriculum should be developed with a training-of-trainers approach and presented via a live online platform; it should also include a free e-Learning program that students may access on their own time and from any device (Ng & Azidah, 2023). There needs to be an update based on the most recent information about the virus and the most effective treatments, as per the guidelines of the WHO. The world's millions of volunteers need to be equipped with the knowledge and abilities to effectively aid their local communities, respond to emergencies, and save lives (Al-Raeei, 2023; Mansoor et al., 2022).
Nurses on the frontlines of healthcare have a critical role in responding to this health emergency, particularly by delivering health education on prevention and infection control, and protecting and caring of patients from stigma and discrimination. The International Council of Nurses called for nurses' protection and other healthcare workers, combat stigma, while caring for MPXV-infected patients (International Council of Nurses, 2022). Healthcare personnel who were not wearing PPE have contracted occupational illnesses from mpox (Vaughan et al., 2020). Therefore, frontline nurses must have access to PPE and other personal safety materials to protect themselves against catching MPXV infection and restrict the further spread of the virus (Guelbert, 2022; Zumla et al., 2022). Any nurse should adhere to their employer's guidelines for treating mpox patients when coming into direct contact with them. Gloves, a surgical face mask or FFP3 mask, and eye protection are required for healthcare professionals if a patient exhibits signs of respiratory infection. The highest degree of PPE for MPXV includes powered air-purifying respirators, coveralls impervious to virus penetration that include a head covering and shoe covers, and gloves. While fit-tested, single-use N95 respirators, isolation gowns, goggles, and gloves provide a comparatively lesser level of protection for MPXV (National Nurses United, 2022). Through in-service or continuing education, they must also access up-to-date information on transmission modes, prevention, diagnosis, treatment, infection control techniques, counseling, and care through online courses (Ahmed, 2022; International Council of Nurses, 2022). To evaluate the exposure of healthcare workers to infection, a thorough risk assessment must be performed on each worker. Based on the risk level, they must also get counseling on self-monitoring, isolation, and quick reporting of symptoms. For instance, a nurse giving medications is likely at a lower risk of contracting an aerosolized virus than a nurse shaking the bed linens of a patient who is infected with MPXV (Palmore & Henderson, 2022). Therefore, standard precautions, additional infection control precautions should be implemented if a patient seeking care is suspected of having a mpox virus infection (Ahmed, Rashad, et al., 2022; Decousser et al., 2023; Lo Piccolo et al., 2023; Raccagni et al., 2023; Safir et al., 2023; Zachary et al., 2023). Infection prevention and control personnel should be notified immediately. Activities that could resuspend dried material from lesions should be avoided. Whether suspected or confirmed, a patient with mpox should be housed in a single-person room; special air handling is not required. Doors should always be kept shut (if it is safe to do so). The patient should have a separate bathroom. Transporting and moving the patient outside the room should be restricted to medically necessary causes. Waste management in the setting of health care is another important issue, and knowledge regarding this aspect should be provided to nurses through the arrangement of workshops (Lulli et al., 2022).
Working as a nurse means increasing the liability and risks of infection and stress. Lit letters have shown that the average working hours of nurses per week significantly predict stress and other negative consequences. In addition, caring for mpox patients might also influence the nurses’ stress levels. For this reason, improving employment and working conditions for nurses and work-life balance is significant. Reducing the burden on nurses' lives by restricting their working hours can improve their health and ameliorate safety concerns. Thus, shift work for 4–6 hours is the way of organizing working hours to maintain a service beyond the regular daytime.
Responders on the scene may be the first medical personnel to see a mpox patient. Medical professionals should be aware of the potential signs and symptoms of mpox so they can properly diagnose the condition. In addition, they need to take extra measures to stop the spread of disease and make sure the transfer of patients under care goes well at the destination hospital. mpox in 2022, and the primer and identify-isolate-inform (3I) tool for emergency medical services professionals have more information available on their background, presentation, and management (Koenig et al., 2022).
There is a link between the wide range of concerns related to mental health and the outbreak of emerging infectious diseases like COVID-19 (Ganesan et al., 2021; Kumar & Nayar, 2021). As we witnessed in the COVID-19 crisis, nurses are always on the frontlines of any health emergency, and there is a high probability of them getting physically and emotionally affected (Lorente et al., 2021). Since nurses play an integral part in managing the public health emergency crisis, it is important to understand the challenges they face from their perspective. There is a linkage between the mpox signs and symptoms, methods to check its spread, and several stressors (Curtis et al., 2023; Hayes et al., 2024). Such stressors include panic, fear, anger, anxiousness, social isolation, exhaustion, financial loss, and stigma. The nurses can be mentally stressed due to the uncertainty concerning the disease (Aroyewun et al., 2022).
Nurses’ mental health is an important aspect that interferes with their ability to work. Counseling is considered an effective strategy to enhance mental health and reduce psychological problems, including stress (Ahmed, M-Amin, et al., 2022; Dubey et al., 2023; Hans et al., 2022; Ibrahim et al., 2022; Nimbi et al., 2023). It is regarded as a part of regular follow-up by psychologists during this pandemic of COVID-19. Besides the additional stress that comes from the new communicable disease, mpox, leading to their exhaustion, they should always be acknowledged whenever possible (Palmore & Henderson, 2022). In addition, face-to-face or online counseling should be provided to the nurses to keep them healthy during present mpox outbreaks and global public health emergencies, improving the quality of care for mpox patients. Governments, policymakers, and health officials should introduce policies such as counseling sessions to combat psychological stress and address the other general concerns of the nurses (Ahmed, Abdulqadir, Omar, Abdullah, Rahman, Hussein, et al., 2023; Ahmed, M-Amin, et al., 2022).
The CDC advises vaccination of laboratory and medical staff as well as anyone else who may come into contact with MPXV-infected patients. As nurses are on the front lines of any health organization and are at the greatest risk of being infected, their vaccination should be given top priority (Angelo et al., 2022; O’Malley, 2022; Titanji et al., 2022). The Smallpox vaccine (JYNNEOS™, also known as Imvamune, Imvanex, or MVA-BN; ACAM2000®), may provide up to 85% protection in preventing MPXV infection through cross-protection expected after pre-exposure and post-exposure prophylaxis (Chakraborty et al., 2022; Poland et al., 2022). Health care workers in the UK are advised to get two doses of the smallpox vaccine spaced at least 28 days apart as a pre-exposure immunization, even if they wear complete PPE (UKHSA, 2022). In addition, the smallpox vaccination is being administered as post-exposure prophylaxis to certain contacts, such as healthcare workers who deal with suspected cases without PPE or confirmed cases while wearing PPE (Gallagher, 2022). In order to prevent or lessen MPXV infection, vaccination should be given as soon as feasible within 4 days post-exposure. For people who are at high risk of continuing exposure, the time frame may be extended to 14 days (UKHSA, 2022). An overview of optimal health service practices, challenges faced by frontline nurses during the 2022 mpox outbreak, and futuristic counteracting strategies is presented in Figure 1.
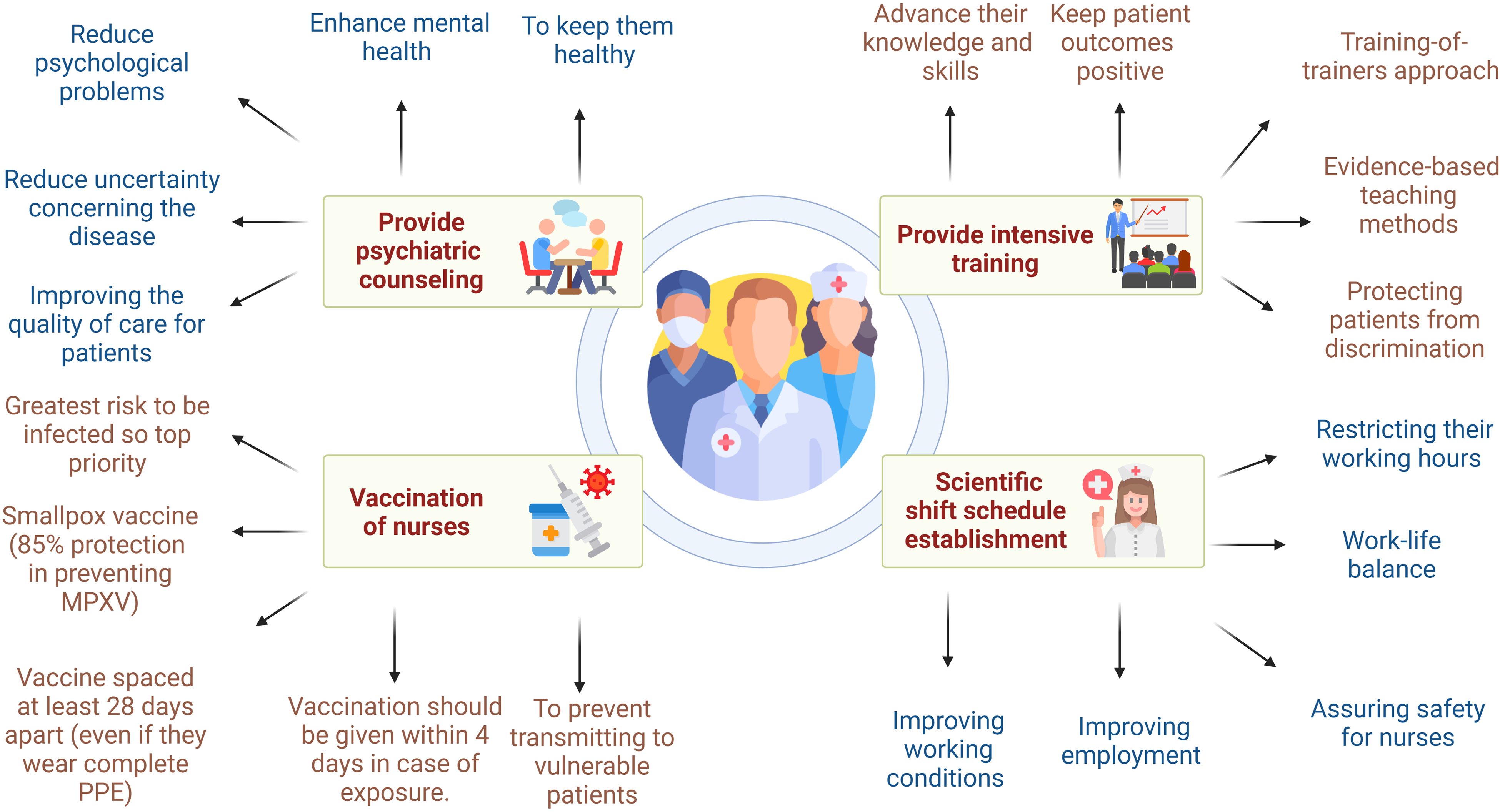
Optimal health service practices, challenges faced by frontline nurses during the 2022 mpox outbreak, and futuristic mitigating strategies.
Importance to Nursing Profession
In the midst of the COVID-19 epidemic, a strong line of communication has been established between public health departments and infection control organizations like the CDC, which can be leveraged to organize the resources needed to mount an effective reaction to the Mpox infestation. A coordinated effort from all relevant authorities offers the best chance of containing the mpox outbreak before it becomes a pandemic. Every day, nurses face new obstacles due to the unpredictability of illness outbreaks that could escalate into worldwide pandemics. For this reason, it is essential to create a novel framework for the early detection, prevention, and treatment of mental health issues among nurses as part of a more comprehensive, holistic strategy. In particular, healthcare employees, including nurses, administrators, and community leaders, should collaborate to develop an ethical code for pandemic situations that can strengthen the moral fiber of healthcare personnel. Promotion of preventive action is necessary in case of any suspected mpox case among nurses. This includes adherence to safety measures to control infection as well as protective measures. This will help in preventing infection among groups that are more vulnerable to infection, viz., pregnant and aged staff or those staff who are immunocompromised. Healthcare professionals and nurses need to be protected by the mpox vaccination, be aware of the risks and challenges, and be ready to deal with any potential infectious outbreaks while maintaining a high index of suspicion and strictly adhering to the recommended precautions for infection control. As frontline health care workers, the various health issues of nurses and their personal concerns must be taken care of appropriately by adopting optimum health service practices, adequate safety measures, and recommended precautionary measures, along with boosting their mental health while handling mpox patients in any future public health emergency situation.
Conclusion
In conclusion, nurses are the backbone of healthcare facilities. In the face of pandemics and public health emergencies of global concern, like COVID-19 and mpox, respectively, it is crucial to ensure the safety of medical personnel. It's a worldwide problem that nurses don’t get enough help or protection from the government during major epidemics of infectious diseases. Practical cooperation between nurses, health organizations, and authorities is crucial for developing a successful response to a mpox epidemic. Furthermore, the availability of flexible policies and protocols is a key component in reducing nosocomial infection rates among nurses.
Footnotes
Acknowledgments
The authors are thankful to their respective institutions/universities for the completion of this work.
Author Contributions
SKA contributed to conceptualization and design. SKA, EAD, FMI, and MGM wrote the first draft. SKA, KD, DC, SC, JB, TBE, and MRI reviewed the literature and updated and edited the manuscript. All authors read and agreed for the final manuscript.
Data Availability Statement
All the data is available on the paper and listed as references.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
