Abstract
Introduction
Pacific Islands have among the highest prevalence of pediatric hearing impairment in the world. Given the limited availability of ear and hearing specialists in the Pacific region, the broader health professional community plays a vital role in the prevention of avoidable pediatric hearing impairment. Nurses emerge as one of the ideal candidates for task-sharing in the administration of ear and hearing care at the public and primary healthcare levels.
Objectives
The aim of this study is to evaluate the awareness and perceptions of university nursing students in Samoa to pediatric hearing impairment and hearing healthcare.
Methods
This study employed a cross-sectional study design. A 10-item questionnaire was administered to university nursing students in Samoa (N = 100). The statements aimed to evaluate perceptions towards childhood hearing impairment, as well as awareness of causal factors of permanent childhood hearing loss and available hearing healthcare. Participants were required to provide a response based on the five-point Likert scale “Strongly Agree,” “Agree,” “Neutral/Don’t know,” “Disagree,” and “Strongly Disagree.”
Results
Overall, 79% of participants responded “Disagree/Strongly Disagree” to the item “Hearing loss is not that important because it does not kill.” Overall, 52% of respondents were aware of hearing impairment as a public health concern in Samoa. Early identification and intervention services for newborns with hearing impairment are nonexistent in Samoa, and awareness was low for the importance of early detection (62%) and amplification suitability for babies (49%). Overall, awareness was also low for causal factors of permanent sensorineural hearing loss.
Conclusions
A borderline neutral/positive perception was found among our future nursing professionals to engage with pediatric hearing impairment in Samoa. Awareness regarding the causes of permanent childhood hearing impairment, as well as early identification and intervention services, could be integrated in the university curriculum.
Introduction/Background
The Pacific Islands have among the highest levels of ear disease and hearing impairment in the world (WHO, 2021), and the adverse effects of childhood hearing disorders on speech, language, cognitive, and motor skill development are well-known (WHO, 2016). Given that ear and hearing specialists are limited throughout the Pacific Islands (Sanders et al., 2015; Thorne et al., 2019), a public health approach to reducing the avoidable burden of hearing impairment among children is recommended (Kaspar et al., 2016; Kaspar et al., 2018). Registered nurses emerge as one of the leading candidates to collaborate in the implementation of strategies to address childhood hearing impairment at the public and primary health care levels in the Pacific Islands.
Review of Literature
A review of the literature indicates that there is relatively little research on the awareness and perceptions of health practitioners to childhood hearing impairment and hearing healthcare in low- and middle-income countries. The studies available usually investigate awareness and perceptions of medical practitioners only (López-Vázquez et al., 2009; Olusanya & Roberts, 2006; Yerraguntla et al., 2016). Furthermore, research from low- and middle-income countries tends to focus on awareness and perceptions towards the implementation of newborn/infant hearing screening programs, with the aim of improving existing early hearing identification and intervention strategies for babies with congenital or early-onset hearing impairment (Khan & Joseph, 2020; Mazlan & Min, 2018; Ravi et al., 2017; Ravi et al., 2018). Only one study was found that investigated awareness and perceptions of nurses (Sanju et al., 2018): a total of 115 nurses from India who worked in primary care, corporate, and government hospitals completed an online survey, and the results found that both awareness and perceptions to childhood hearing impairment were low.
There are only three studies of this kind from the Pacific Islands. The first explored awareness and perceptions towards childhood hearing loss among parents in the Solomon Islands (Kaspar et al., 2017). Parents were overwhelmingly supportive of community-based ear and hearing health services for both infants (96%) and school-age children (99.3%) (Kaspar et al., 2017). The second study similarly investigated awareness and perceptions towards childhood hearing impairment among urban and rural/remote female caregivers in Samoa, and also found high support for hearing health services for infants (98%) and school students (97.3%) (Kaspar et al., 2023). A third study investigated awareness and perceptions towards childhood hearing impairment among doctors and medical students in Samoa (Kaspar et al., 2022), and again the results showed positive support for the implementation of childhood hearing services (95.8%). In order to investigate health professional readiness to meet caregiver support for community-based ear and hearing health healthcare, further assessment of current and future health professionals’ attitudes towards such services in the Pacific Islands is desirable. Given the leading role of nurses in primary healthcare delivery in the Pacific Islands, a study on the awareness and perceptions of current and future nursing professionals specifically is essential.
The Ear, Nose, and Throat (ENT) Department of the Tupua Tamasese Meaole Hospital in Samoa is currently engaged in developing initiatives to manage childhood hearing loss in the national public and primary health care system. The newly updated Samoan Baby Health Book includes advice on ear healthcare, as well as a hearing milestone checklist (Kaspar, Driscoll et al., 2021). The Samoan Baby Health Books are mostly completed by registered nurses during an infant's visit to the Well-Baby Clinics, which includes the Expanded Program on Immunization. As hearing health gains increased exposure among current and future nursing health professionals, the present study was conducted to evaluate the awareness and perceptions of nursing students attending the National University of Samoa. The results of the study should guide curriculum development, and be translational to other university-level nursing courses in the Pacific Islands.
Methods
Design
The present study used a cross-sectional design, and is a modified version of a previously published study protocol (Kaspar, Pifeleti et al., 2021). The decision to report medical and nursing student results separately was made in order to highlight the recommendations unique to each health profession.
Study Instrument
The study questionnaire was disseminated to participants by the researchers during prearranged class times, and took approximately 10–15 min to complete. The questionnaire was an adaptation of the English-language questionnaire used in the original study from Nigeria (Olusanya & Roberts, 2006): although the original study was aimed at medical professionals, the research team concluded that, in the absence of questionnaires aimed at nurses, this would be appropriate for use in the present study. The only modification was the substitution of “Nigerian children” for “Samoan children.”
The participants were asked to complete demographic information by selecting gender (male/female) and indicating their age in years. The questionnaire was composed of 10 questions which were rated on a five-point Likert scale, and each participant was instructed to place an “X” according to their response of “Strongly Agree,” “Agree,” “Not sure,” “Disagree,” or “Strongly Disagree.” Three questions related to awareness of causes of childhood hearing impairment, three questions assessed awareness of interventions for childhood hearing impairment, and four questions investigated perceptions to childhood hearing impairment. Bloom's cutoff criteria were used to assess awareness as high (80%–100%), moderate (60%–79%), or low (<60%), and perceptions as positive (80%–100%), neutral (60%–79%), or negative (<60%). The research team collected the deidentified questionnaires upon completion, and stored them for data entry and analysis at the ENT Department office.
Research Question
What are the awareness and perception levels of university nursing students in Samoa towards pediatric hearing impairment and hearing healthcare?
Sample and Inclusion/Exclusion Criteria
All students enrolled in the Bachelor of Nursing (Years 1–3) at the National University of Samoa in 2021 were eligible for the study (N = 179). English literacy skills are a requirement of university enrolment in Samoa, and the eligible participants for the present study were deemed sufficiently able to read and respond to the English-language study questionnaire. An announcement and invitation to participate in the study were made by the research team during prearranged class times (i.e., class ended 10–15 min early to allow for completion of the data collection). There was no predetermined sample size for this study, nor were there any incentives offered to encourage participation in the study; however, the announcement stated that an aim of the study was to improve the nursing curriculum. All willing participants signed a consent form, and all nonparticipating students were allowed to leave the classroom.
Ethical Considerations
Ethical approval for the study was obtained from (1) the Health Research Committee of the Government of Samoa Ministry of Health, (2) the University Research Ethics Committee of the National University of Samoa, and (3) the University of Queensland Medical Research Ethics Committee. All participants signed a consent form, and completed the study questionnaire anonymously. The chief investigator conducted and supervised all data handling and analysis.
Statistical Analysis
The completed questionnaires were stored at the time of data collection (AK, MSM), and then the results were later entered into a purpose-designed SPSS Statistical Software Package spreadsheet (AK) and analyzed (AK, CD).
The responses were calculated for each statement according to age, gender, and year of study subgroup. Chi-square tests of significance were considered; however, proportion sizes were deemed too small for useful comparisons. Thus, data analysis was again modified from the published study protocol to suit the data set (Kaspar, Pifeleti et al., 2021).
Results
Sample Characteristics
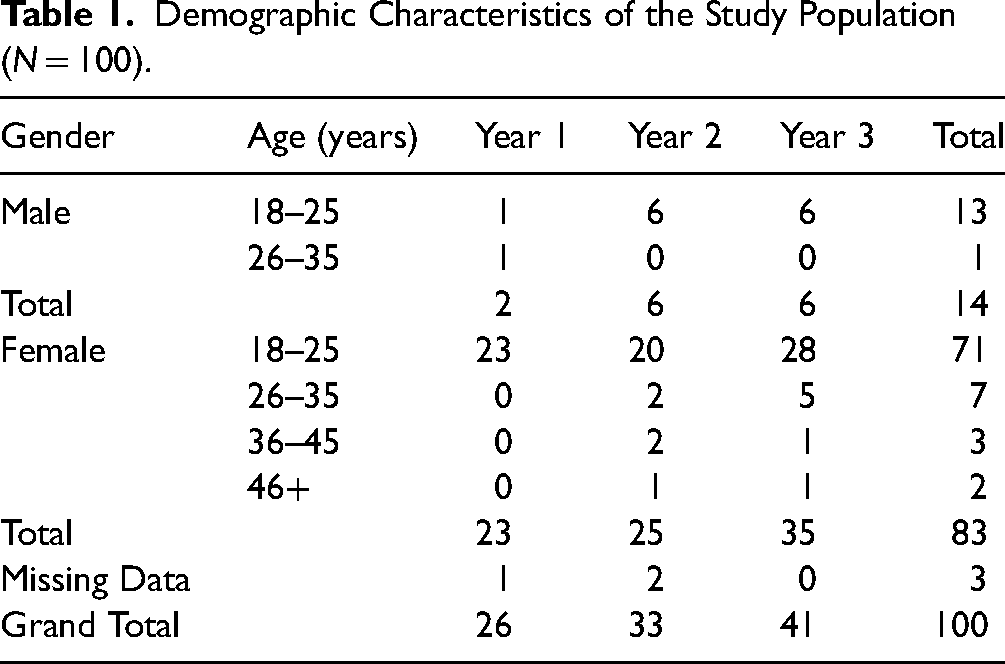
The sample characteristics are summarized in Table 1. A 55.9% participation rate was achieved for the study. The total study population (N = 100) consisted of 14 males and 83 females, and gender data were missing for three participants. The age distribution ranged from 18 to 51 years, with a mean of 22.91 years (SD = 5.5 years). The population distribution according to year of study was Year 1 (N = 26), Year 2 (N = 33), and Year 3 (N = 41). The majority of study participants (71%) were female students in the 18–25 year age group, with participant numbers fairly evenly distributed over the 3 years of study subgroups.
Demographic Characteristics of the Study Population (N = 100).
Awareness and Perceptions of University Nursing Students in Samoa to Pediatric Hearing Impairment and Hearing Healthcare
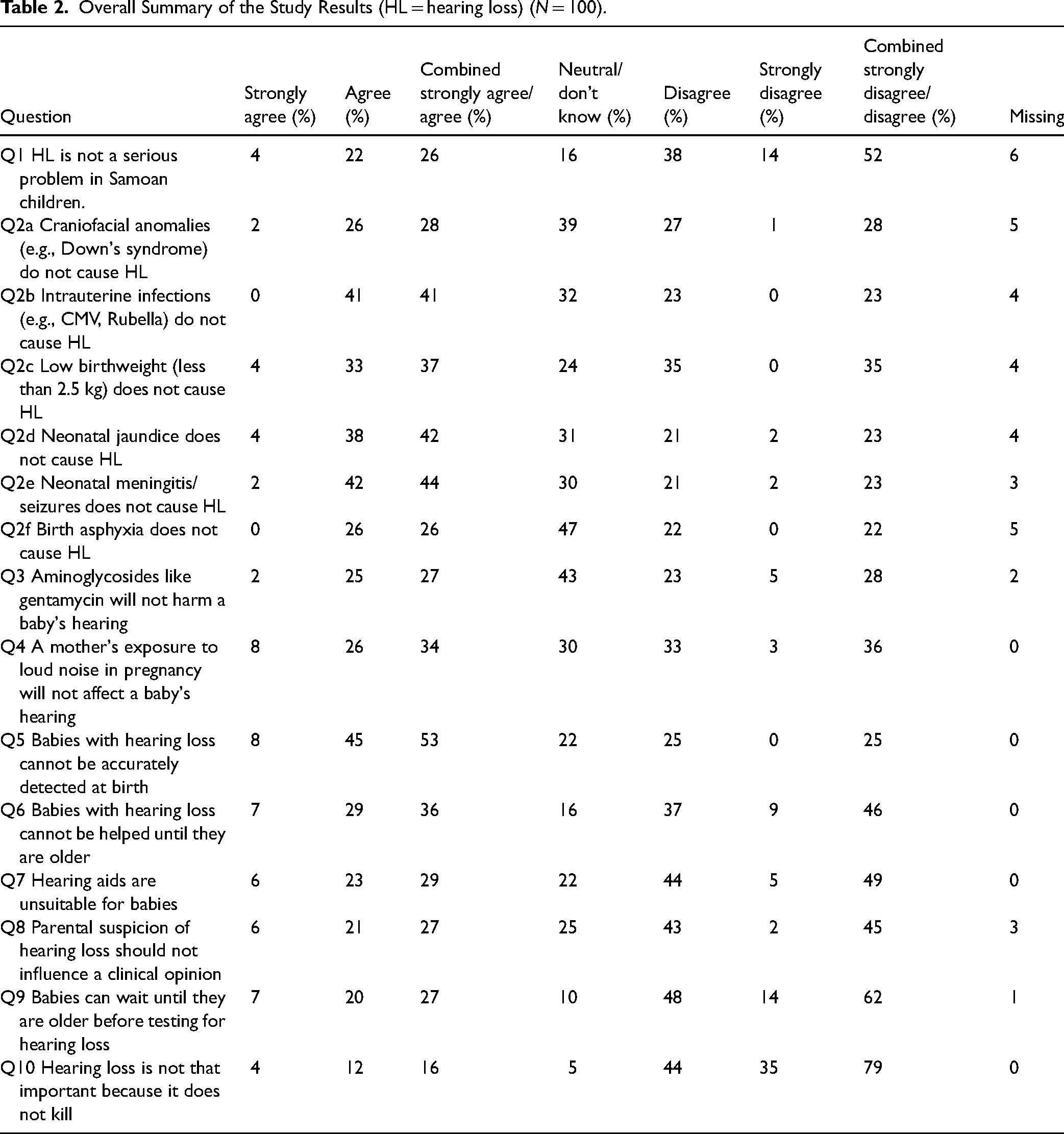
An overall summary of the study results and their interpretation are presented in Tables 2 and 3, respectively. Overall, there were neutral perceptions to engaging with services for children with hearing impairment, with 79% of participants responding “Disagree/Strongly Disagree” to the item “Hearing loss is not that important because it does not kill.” Overall, 52% of respondents selected “disagree” (38%) or “strongly disagree” (14%) to the item that “Hearing loss is not a serious problem in Samoan children.” The highest awareness of causal factors for permanent pediatric hearing impairment was measured for maternal exposure to loud noise (36%), followed by low birthweight (35%), and with awareness of all other causes ranging between 22% and 28%. Overall, there was generally low awareness of early identification and intervention options for babies born with hearing impairment. The participants selected “disagree” or “strongly disagree” to the items “babies can wait until they are older before testing for hearing loss” (62%), “hearing aids unsuitable for babies” (49%), and “babies with hearing loss can’t be helped until they are older” (46%). Awareness was lowest for the item “babies with hearing loss cannot be accurately detected at birth” (25%). There were 45% of participants who disagreed or strongly disagreed with the statement that “parental suspicion should not influence clinical opinion.”
Overall Summary of the Study Results (HL = hearing loss) (N = 100).
Interpretation of the Study Results Based on Bloom's Criteriaa.

Awareness: high (80%–100%), moderate (60%–79%), low (<60%). Perceptions: positive (80%–100%), neutral (60%–79%), negative (<60%).
Discussion
Childhood hearing loss is a major public health concern in the Pacific Islands. Given the scarcity of ear and hearing specialists in the region, nurses may be considered suitable candidates for addressing childhood hearing loss through public and primary healthcare initiatives. The present study found neutral perceptions among nursing students towards addressing childhood hearing impairment in Samoa (79%). Although only half of the students (52%) were aware that hearing impairment is a major public health concern among children in Samoa, the borderline neutral/positive perceptions of these future nursing professionals may suggest some willingness to support the ongoing development of primary level ear and hearing health services.
At this time, the university curriculum for nurses does not include training on the causal factors of pediatric hearing loss that may be present at birth or develop during the early neonatal period. This may account for the relatively low scores measured in the present study. Given that the latest edition of the Samoan Baby Health Book will include a risk-factor questionnaire for childhood hearing impairment (Kaspar, Driscoll et al., 2021), there is a case for the inclusion of this information in the university course curriculum for nurses. The causes of childhood hearing impairment may be integrated with course components on public/primary health provision through the well-baby clinics.
The results of the present study showed low levels of awareness for early identification and intervention for childhood hearing impairment. This was an unsurprising result given that there is no newborn/infant hearing screening in Samoa, and that amplification services are dependent on overseas specialist visits. The fact that almost half of the participants were aware of early identification and intervention services may be explained by the close relationship between Samoa and New Zealand, and the fact that people in Samoa may know of such health services through the experiences of their family living overseas. While Samoa does not have the resources at this time to implement an early hearing identification and intervention program (Kaspar et al., 2020), the updated Samoan Baby Health Book will include a hearing development milestone checklist to enable early identification of infants and toddlers with hearing impairment (Kaspar, Driscoll et al., 2021).
Strengths and Limitations
A limitation of the present study was that the questionnaire was administered in English. Although the research team was advised that English literacy was high among university students, the “double-negative” language format of the questionnaire may have caused confusion. It is recommended that future questionnaires are presented in both English and Samoan. This should be acceptable to any Samoan population group given that most forms/documents in Samoa are structured bilingually.
Another limitation was that tests of significance between age and gender variables were not performed as subgroup sizes were deemed too small for meaningful comparisons (i.e., a significant proportion of nursing students were female and in the 18–25-year age group). A similar study among qualified nurses in Samoa may present an opportunity for a study design where the influence of gender and age variables on awareness and perceptions of childhood hearing loss may be assessed. A further limitation was that home residence data were not collected (i.e., urban/rural/remote), and this may also be important data to collect in future studies among both student and qualified nurses.
Implications for Practice
The ENT Clinic of Samoa will continue to partner with the National University of Samoa School of Nursing for ongoing curriculum development that prepares future nurses for supporting ear and hearing healthcare. Curriculum development on childhood hearing health may be extended beyond the School of Nursing, and considered for other courses such as Inclusive Education (i.e., role of teachers for students with hearing difficulties) and/or the Masters of Public Health (i.e., integration of school-based hearing screening into the national PEN Fa’a Samoa public health initiative) (Kaspar et al., 2023).
The study results suggest that increasing awareness of childhood hearing loss among qualified nurses would also be beneficial. The ENT Clinic nurses have already had opportunities to present on ear and hearing health at the fortnightly continuing medical education sessions for nurses, and further opportunities may be investigated for existing nursing workshops (i.e., child health) and/or the annual nursing conference.
The study results also support the ongoing delivery of the World Health Organization Primary Ear and Hearing Care training workshops by the ENT Clinic, where the inclusion of nurses from rural and remote areas of Samoa is a priority (Kaspar & Pifeleti, 2022).
Conclusions
Borderline neutral/positive perceptions were found among our future nursing professionals to engage with pediatric hearing impairment in Samoa. Awareness regarding causes of permanent childhood hearing impairment, as well as early identification and intervention services, could be improved by their inclusion in the university curriculum.
Footnotes
Acknowledgements
The authors would like to thank and acknowledge Dr Filipina Amosa-Lei Sam (School of Medicine) for her assistance in facilitating this research study.
Author Contribution Statement
AK: study design, data collection, data entry, data analysis, manuscript preparation. MSM: data collection, manuscript review and feedback. CD data analysis, manuscript review and feedback. SP: manuscript review and feedback.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Statement
Ethical approval for the study was obtained from (1) the Health Research Committee of the Government of Samoa Ministry of Health, (2) the University Research Ethics Committee of the National University of Samoa, and (3) the University of Queensland Medical Research Ethics Committee.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
