Abstract
Introduction
Cervical cancer is mostly caused by high-risk Human papillomavirus HPV, with an estimation prevalence of HPV of 99.7% worldwide. The US Food and Drug Administration (FDA) approved an HPV test for primary cervical screening in 2014. An HPV-DNA test, which provides higher protection against invasive cervical carcinomas, is replacing the long-standing Pap smear as the primary method of cervical cancer screening.
Objective
To explore nurses’ experience and knowledge of HPV DNA testing and how screening impacts on women's health through increasing awareness and proposing actions for health education strategies.
Method
A qualitative exploratory study was conducted on a purposeful sample of 25 qualified nurses, who were all employed in regional hospitals within a gynecological department in Kirkuk, Iraq. The nurses were interviewed with a semi-structured topic guide between November 2021 and February 2022. Responses were transcribed verbatim, translated into English and analysed using a content thematic analysis approach.
Results
Four themes with associated sub-themes emerged following coding and peer review. Participants had lack of experience and fragmented knowledge of HPV DNA testing/screening. Culturally sensitive resources for patients and training for nurses was identified key requirements.
Conclusions
Currently, there are no facilities for a HPV testing/screening services available in Iraq. The role of nurses undertaking HPV screening is not established and yet nurses represent the largest sector of health professionals. The dissemination of a collaborative HPV screening training programme to include clinical competence and knowledge for nurses and gynaecologists may improve knowledge, and could also be effective in improving patient awareness and engagement with cervical health.
Introduction
Persistent infection with Human papillomavirus (HPV) is currently affirmed as the main cause of cervical cancer with an estimation prevalence of HPV worldwide of 99.7% (Santesso et al., 2016). As a consequence, HPV test/vaccine has been incorporated into both primary and secondary cervical cancer prevention strategies (Santesso et al., 2016). HPV infection is a highly transmissible infection and the majority of sexually active women will likely have an HPV infection in their life time (Castellsagué, 2008). The use of HPV DNA testing to triage low-grade cytological abnormalities has been shown to be more sensitive for earlier detection of cervical intraepithelial neoplasia grade (CIN) II+, compared to standard liquid-based cytology alone (Santesso et al., 2016). The cervical screening procedure remains the same, a single sample of cells are taken from the cervix, if viral HPV DNA or RNA is detected the same sample is used to prepare a cytology slide for examination under a microscope (National Health Service [NHS], 2017). Furthermore, it permits earlier return to routine recall in those with mild cytological abnormalities who are negative for high-risk HPV; and for those testing negative post-treatment, follow-up is considerably shortened (Beachler et al., 2017). On average HPV infection clears within 1–2 years in 90% of cases and only 50%–60% of women develop serum antibodies to HPV after natural infection (Castellsagué, 2008).
Review of Literature
Cohort studies with up to 10 years of follow-up data have indicated after clearance the same HPV type can occasionally reappear (Santesso et al., 2016; Kerkar, Latta, Salvi, & Mania , 2011; Perez et al., 2017). The HPV test, administered alone without the Pap smear test, was recently recognized as a cervical cancer screening option. The US Food and Drug Administration (FDA) approved a HPV test for primary screening in 2014. This method is considered as a possible screening method that could be applicable for low-middle income countries (Beachler et al., 2017; Perez et al., 2017). The cervical cancer prevention program is undeveloped in Iraq. Opportunistic screening is used when women present with gynecological symptoms. In government hospitals, a small clinic known as the, unit of early detection of cervical cancer, offers cervical cancer screening services (Ali, Clark, Ghalib, Skirton, & Donaldson, 2021). Perceived local disease prevalence is important for understanding risk perceptions in relation to health behaviours and health outcomes, however, a literature search did not identify any studies on the HPV prevalence in Iraq (Ali et al., 2021).
Generally gynecologists are responsible for undertaking smear tests in healthcare settings in Iraq, where unwell women have been assigned to them for investigations. (Ali et al., 2021). While the role of nurses performing smears/HPV is not well established (Ali et al., 2021; Ali, Skirton, Clark, & Donaldson, 2017). Previous studies have indicated the necessity for nurses to be adequately informed of HPV testing (Rasul, Moghdam, Karim, & Cheraghi, 2019; Kolutek, & Avci, 2014; Wilson et al., 2016). The Global Advisory Panel on the Future of Nursing (GAP-FON) was introduced in November 2016 with the goal of encouraging global nursing collaboration and enhancing global health (Wilson et al., 2016). Nurses can educate about early diagnosis and screening but need to be aware of the women's cultural values, life styles and health-disease perceptions (Patel, Austin-Smith, Sherman, Tincello & Moss, 2017). The ethnic variety, social customs, and traditional norms of Iraqi women are thought to have an impact on the burdens and patterns of cervical screening uptake (Ali et al., 2021). Embarrassment and personal modesty seem to be major obstacles. Iraqi women have social features including shyness when it comes to physically visualizing private or intimate information about the female anatomy, which may impede discussion about cervical cancer as a private or sensitive health issue (Ali et al., 2017). Iraq currently lacks a nationwide cervical screening program. Although there are no established guidelines for the role and obligations of nurses in this respect, it was assumed that they were aware of the necessity of HPV testing and cervical screening for the early detection of cervical cancer.
The purpose of this qualitative study was to explore nurses’ experience toward HPV testing to determine nurse's role and how this can positively impact women's health. The objectives of the study were:
What are nurses’ responses to HPV testing/screening and their role in preventing cervical cancer. How the nurses’ role can be actioned into nursing education, health promotions and clinical practice.
Methods
Study Design
The method employed in this study aligned with an exploratory qualitative methodology utilizing qualitative thematic content analysis to interpret underlying meaning the nurse participants placed on their role, experiences, and thoughts through individual in-depth interviews. Qualitative methodology is within the interpretative epistemological framework, where understanding of multiple realities or interpretations of the phenomenon of interest are sought (Polit & Beck, 2018).
This study was collaboration between the primary researcher, a consultant gynecologist in Iraq (authors, 1, 3) and an academic and clinical midwife in the UK (author, 2). A purposive sample of 25 nurses working in the unit of early detection of cervical cancer/departments of women's gynecological issues were recruited (n = 25). The primary researcher, embraced the interpretative nature of the narratives through facilitation of the human experience and the social context of the research setting (Moule, Aveyard, & Goodman, 2016).
Research Question
What do nurses know about HPV testing/screening and how their role can impact on women's cervical health promotion through education and training?
Data Collection
The study took place between November 2021 and February 2022. A day before each interview, participants received SMS reminders about the time and place of the interview in the hospital. Informed consent was obtained before conducting the interviews. Data collection and analysis were done simultaneously and continued until saturation was achieved and no new themes emerged.
All interviews with participants were carried out in a quiet room at the hospital that assured confidentiality and privacy. The conversation began with a greeting, an introduction, and an explanation of the study. The participant demographic characteristics were covered first (Table 1). The topic guide with open ended questions as presented in Table 2 was followed by the primary researcher. Participants were encouraged to provide their own thoughts on each of the issues presented. Follow-up questions were utilized to stimulate more discussion until no more conversations about the topics emerged. All interviews were audio-recorded in two local languages (Arabic and Kurdish) afterwards transcribed verbatim, and translated into English. Each interview took between 30 and 60 min. The interviews were conducted according to participants’ preferred languages to foster a relaxed environment where participants may openly discuss HPV and cervical cancer.
Sample Characteristics (n = 25 Qualified Registered Nurses).

Study Guide Topics.

The primary researcher is multilingual fluent in Kurdish, Arabic and English, this level of linguistic ability enabled the facilitation of the chosen participant language and accurate translation into English. The second author, whose first language is English, added an additional check for accuracy and authenticity of the translation through careful reading of the translated scripts to check for language translation accuracies. Different languages/dialects were used to ensure a truthful reflection of the data and increase the validity of the study, the participant confirmability of the intended meaning was sought (Harvey & Land, 2017; Parahoo, 2014).
Participants were assigned pseudonyms and identifying material was removed. All narrative data was anonymised on transcription and these scripts are kept securely on a password protected electronic device. The translations and verbatim transcriptions were peer reviewed by the third author, an Iraqi gynecologist who is also multilingual in Turkish, Kurdish, Arabic and English. Five participants requested to read their transcripts, which did not result in any requested changes. Involvement of the participants in peer review enhanced transparency of the process and verified the core themes emerging.
Sample
Participants who were eligible for this study were qualified nurses who had a range of experiences within a gynecological and women's health context. They were employed at three main hospitals and the healthcare centers in Kirkuk (n = 25). Most had achieved a Bachelor of Nursing Science (BSc) except a few who held a Diploma level degree in nursing. Purposive sampling method was employed to recruit participants through in-person recruitment to eligible nurses who met the inclusion criteria. Thirty two nurses accepted to be interviewed. However, after collecting and analyzing the data from 25 nurses, saturation was achieved and no novel themes emerged. Purposeful sampling of the participants was justified, as there was an intention to best understand the phenomena under research and meet the inclusion criteria (Harvey & Land, 2017).
Inclusion/Exclusion Criteria
In fulfilling the eligibility criterion for the study, the crucial component to the recruitment strategy was the inclusion of nurses. The inclusion criteria required the participants to be registered nurses, currently employed in women's health services and have a role in counselling women who attended for HPV screening. Those excluded were gynecologists or medical doctors and nurses not employed in the women's health services.
Data Analysis
A thematic content analysis approach was utilised to code the meaning extrapolated from narrative data into broader themes and sub-themes (Harvey & Land, 2017). The three researchers, two based in Iraq and the other in the UK, familiarised themselves with the data through a series of reading and re-reading independently. The researchers thus, ensuring inter-coding reliability, discussed data analysis and coding. This added rigour to the themes by facilitating accuracy and trustworthiness in the analysis phase (Paratoo, 2014). The UK based researcher was careful to ensure the meaning extracted correlated with the original translation. Collation of these discussions provided an audit trail. Emergent themes generated were finalised via zoom calls between the researchers and four overarching themes were agreed.
Results
Characteristics of the Sample
Seventeen participants had achieved a BSc in nursing science, and eight participants held a nursing Diploma. All the participants were female (n=25). Ten of the interviewed nurses were working at the unit of early detection of cervical cancer. The experience of the nurses working at this unit ranged from 1 to 15 years, yet just three obtained specialized training on collecting cervical samples. Meanwhile, fifteen of the interviewed nurses were working as a nurse in women's health departments. All participants had post-qualifying years of nursing experience; however, most of them reported lack of experience in terms of HPV testing /screening and the link to cervical cancer.
Research Question Results
Themes/Categories emerging from interview analysis with nurses
Four overarching themes were identified with sub-categories emerging from the analysis (Table 3).
Identification of Themes and Sub-Themes.
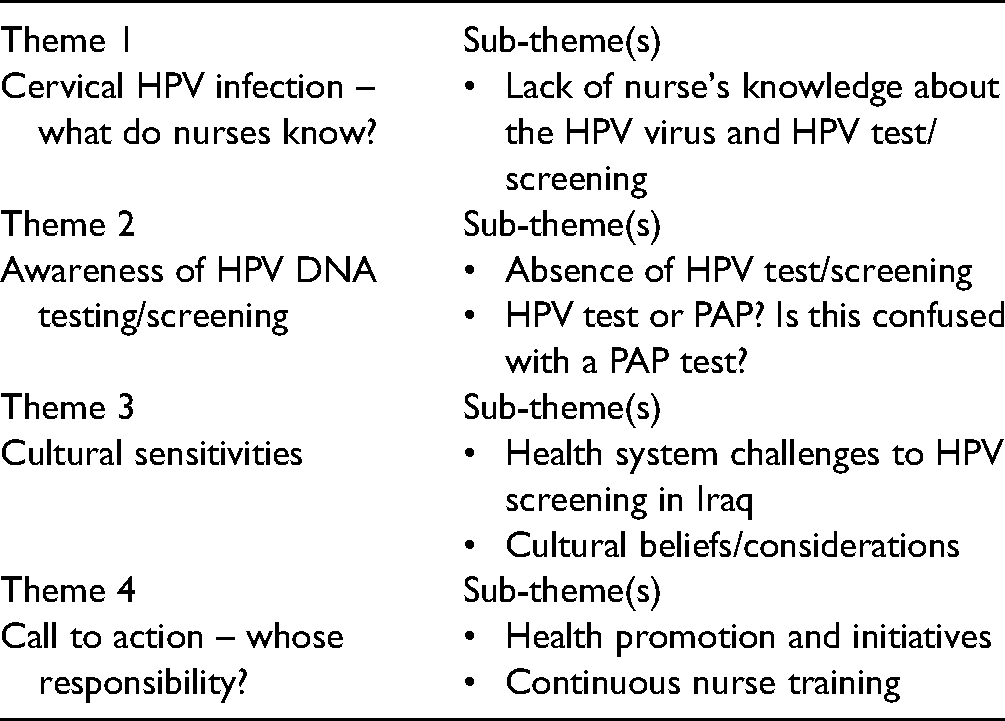
Theme 1*
Cervical HPV infection – what do nurses know?
Nurses’ information regarding cervical HPV infection and how it might be transmitted was mostly inadequate with some concerns and inaccurate accounts of how HPV could be spread in a population.
“This virus may be transmitted from husband to wife, especially if the husband swims in the swimming pools. I heard men can get this virus from swimming pools.”
(Nurse A)
“This virus can be transmitted when there is poor hygiene, mostly from using public restrooms” (Nurse L)
Only two nurses of the 25 interviewed, demonstrated accurate knowledge of HPV and how it is transmitted sexually.
“This virus comes from multiple sexual relationships and eventually this virus will cause cervical cancer”. (Nurse F)
“More often sexual activity increases the chance of having HPV infection.” (Nurse N)
This finding reveals the lack of accurate information and knowledge that most of the nurses had on the cervical HPV infection.
Theme 2*
Awareness of HPV DNA testing/screening
Generally, there was confusion related to the differences between the HPV or the Pap smear test, then how these tests protect women from developing cervical cancer.
Nurses reported that HPV test/screening is not currently available in any local regional hospitals, only Pap smears on an opportunistic basis for symptomatic women.
“To be honest currently, we are not offering this service to women in this unit. Rarely gynaecologists are referring suspected women whom experience offensive vaginal discharge to this unit for HPV testing. So, there is no screening, we just perform a Pap test for suspected cases in this unit”. (Nurse B)
Most of the interviewed nurses declared there is a substantial knowledge gap among nurses in terms of HPV test and its relationship to cervical cancer.
“I believe that the majority of nurses do not understand or even realize the relationship between HPV and cervical cancer … They make absolutely no connection at all between HPV and cervical cancer”. (Nurse F)
“I had no idea that HPV testing was even an option. Regardless of whether
It's either a swab or urine test, simply don’t have the required knowledge” (Nurse J)
This theme suggests a lack of clinical exposure to a screening service, which may have influenced the participants’ lack of knowledge as evidenced by their responses.
Theme 3*
Cultural sensitivities
Participants reported the need for cultural consideration regarding the HPV test, and the nurses’ role in raising awareness in encouraging women to attend for cervical screening. They gave first-hand accounts from women who expressed concerns that they were being judged and the perceived shame associated with being asked such questions regarding cervical screening.
“HPV test is not acceptable among women in our culture” (Nurse D)
“A woman in the hospital who has been told to get this test done! You know what was her reaction?” (Laughter) she said “Do you think I am not a good woman?” (Nurse K)
The nurse participants discussed their role as, fundamental, in ensuring that the awareness of cervical health was raised with women within a culturally sensitive dialogue despite the subject not being socially acceptable.
“The most important issue is, nurses should instruct women about this test because as you know our culture is different and women mostly belief that HPV is a shameful disease” (Nurse F)
One of the nurses claimed that women are avoiding the subject because they are aware that it is connected to sexual misconduct.
“The fact remains, though, that I believe women are avoiding the topic, because they are very certain that it has connected to sexual behaviour. I mean that it's connected to sleeping with inappropriate individual” (Nurse G)
This theme indicates the need for developing culturally appropriate interventions to enhance HPV testing uptake among women.
Theme 4*
Call to Action – whose responsibility?
Nurses recommended solutions to increase awareness among Iraqi nurses. Many reported the need for training courses along with a willingness to further educate themselves on the topic.
“Nurses are in urgent need for continuous training courses guided and run by doctors. I think theoretical and clinical courses should be compulsory for nurses at least every 6 months” (Nurse E)
One of the interviewed nurses reported the shortage of training for the recently graduated nurses
“You know, the problem here is; we have a shortage of training for nurses, for example, I graduated eight years ago, but I haven't attended any training courses yet” (Nurse H)
Also, interviewed nurses mentioned the need for clear explanation in different local language in order to raise nurses’ awareness of the HPV test,
“ I think having additional assistance in very simple explanations in different languages may be helpful. Maybe we should get together and work on it” (Nurse l)
Some other nurse proposed online courses for nurses on obtaining smear and HPV samples.
“online courses are needed to encourage nurses to be engaged in taking smears and HPV testing” (Nurse S)
The main focus of this theme was the widespread view that nurses wanted to remain current in their knowledge. Solutions such as professional nursing development opportunities via symposiums or educational programmes and patient resources in different languages/dialects were suggested
Discussion
The purpose of this study was to develop a better understanding of the nurse's perceptions of HPV testing/screening and how this links to improving public health for women by preventing cervical cancer. The findings revealed the absence of regular organized HPV testing/screening in the local regional hospitals. The study's most unexpected finding was that nurses were not consistently been involved in collecting smears/HPV test, which was thought to be primarily a nurse duty. Furthermore, nurses have had a low level of HPV knowledge with most of them having misconceptions about the HPV test/screening rationale. Similar inadequate levels of knowledge and awareness about HPV and its’ relation to cervical cancer was reported by previous studies conducted in Iraq (Ali et al., 2017; Hwaid, 2013; Alwan, Al-Attar, Al Mallah, & Abdulla, 2017). The qualified nurses interviewed revealed that the HPV test is not available at local hospitals with no intervention strategies being employed in most of primary health care centers or local hospitals in Iraq. This practice is clearly inconsistent with the recommendations of Mayrand et al., (2007) whose analyses revealed that HPV testing has greater sensitivity for detection of cervical cancer, compared with Pap smear testing. A study by the Royal College of Obstetricians and Gynaecologists (RCOG) stated that numerous researchers have indicated the potential benefits of incorporating HPV testing for high-risk genotypes into cervical screening (Royal College of Obstetricians and Gynaecologists [RCOG], 2016). According to the World Health Organization (WHO), Iraq has 10.74 million women aged 15 and above who are at risk of developing cervical cancer (Ali et al., 2017). Therefore, establishment of evidence based cervical cancer prevention strategies, and continuing care for women with cervical cancer is of crucial importance.
Many researchers have argued that one of the main issues of cervical cancer prevention in most Arab Muslim countries is the lack of HPV awareness among health care providers (Saadoon, Amin, & Jadoo, 2014; Ibrahim, Daniel, Hussein, Assafi, & Othman, 2019; Hweissa, Lim, & Su, 2016). The findings of the present study also provide evidence that all participants were confused between the Pap smear and HPV test. Providing essential information through well-organized health promotion activities and communication advocated by nursing professionals can reduce barriers for women and enable the uptake of the HPV test (Hweissa et al., 2016). However, the results of the present study suggest that the cultural acceptability of HPV testing/screening for women in Iraq has yet to be determined. Personal embarrassment and humility may lead to non-disclosure of signs and symptoms (Ali et al., 2017; Rasul et al., 2019). Modesty and reticence are social characteristics expected of women when discussing or visualizing the female body. Shyness about intimacy and sexual relationships could prevent necessary professional discussions about HPV test and it is relation to cervical cancer (Snijders et al., 2013). Our study confirmed that there are significant sociocultural barriers to cervical screening organization in Iraq. This issue must be addressed, and more research is needed to establish what strategies are culturally acceptable to women in Iraq.
HPV self-sampling is a promising alternative for screening in under-resourced areas lacking medical services for women who are reluctant to participate in screening (Hweissa et al., 2016). It is noteworthy that cervical screening programmes are changing nationwide and are increasingly based on screening using HPV testing rather than cytology (Snijders et al., 2013). Thus, Iraqi nurses need to be adequately supported and prepared for these changes and the associated patient communication issues to improve public health awareness, so that screening uptake is not negatively affected.
A recent study by the primary researcher confirmed that a health policy change is urgently required to promote nurses as the lead practitioner for cervical screening in Iraq so enabling more women to be screened and detected in the early disease stage (Ali et al., 2017). The training of more nurses to screen women for HPV would enable the gynaecologists to focus on performing the intervention treatment before the cancer becomes established or inoperable. As political instability and violence persist after decades of war, Iraq has significant health issues, notably in the performance of healthcare services (Ali et al., 2017). The WHO has supported the development of training and courses for nursing leaders, however, more action is required to restore nursing in Iraq (World Health Organization [WHO], 2016).
Strengths and Limitations
It is a limitation of this study that all nurses interviewed were located to health centers in one city. The location of the study, revealed the unavailability of HPV testing/screening facilities. This may have impacted on the integrity of the responses. Meanwhile, our study's strength resides in the fact that we concentrated on a qualitative investigation of nurses’ perspectives on their real-world experiences. Through this process, we were able to obtain a comprehensive overview of the challenging working practices the nurses encountered, which revealed nurses have inadequate training to provide this preventative screening service. Therefore, it is recommended, this study be replicated with further health care professionals in other Iraqi cities and wider across other Muslim countries and communities.
Implications for Practice
The findings from this study identify the requirement for a collaborative cervical screening training package for nurses as the first line professionals in women's cervical health. This can have a positive impact on women's health promotion and screening interventions in Iraq.
Conclusion
Nurses represent the largest sector of health professionals; therefore, the dissemination of a HPV testing/screening knowledge and clinical skills competence, could form a robust training programme for nurses. A collaboration with gynecological colleagues could also be effective in improving women's cervical awareness and compliance with attending for screening enabling earlier intervention. The inclusion of a women's health module as part of the undergraduate nursing programme to educate future nurses of their role in promoting cervical health to women may increase screening utilization and ensure accurate information giving. This study further evidences the need for a systematic, culturally sensitive, population-based HPV testing/screening programme in Iraq for the benefit all women.
Footnotes
Acknowledgements
The authors would like to thank all the participants for expressing their detailed accounts of their experience on the topic.
Author Contributions
Study design: S.A., R.L.
Data collection: S.A., A.G.
Data analysis: S.A., R.L, and A.G
Manuscript writing and revisions for important intellectual content:
S.A., R, L, and A.G
Ethical Approval
This study was granted ethical approval from Kirkuk Health directorate [Ref. no. 34031].
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
