Abstract
Introduction
Resistance to antibiotics is a threat confronting health care system worldwide. Nurses play a significant role in combating this threat.
Objectives
The present study examined the knowledge and attitude of nurses towards antibiotic use and prevention of antibiotic resistance.
Methods
The research involved a cross-sectional study conducted in a multi-cultural tertiary healthcare setting. The participants were 341 nurses. A structured self-administered questionnaire with a good validity and reliability (α = 0.7) was used.
Results
The nurses surveyed showed moderate awareness of antibiotic resistance and a fair attitude towards its prevention. There was no significant correlation of demographic features with their overall knowledge and attitude (
Conclusions
Nurses perform a crucial part in infection control, but often lack knowledge of methods to prevent antibiotic resistance. This paucity highlights the importance of tailored interventions to help nurses improve their awareness of antibiotic resistance and create a favorable attitude towards its prevention.
Antibiotics are unequivocally one of the greatest innovations in medicine, but the threat of antibiotic resistance (AR) is now approaching a tipping point. Treatment of infections such as tuberculosis and pneumonia, handling of neonatal disorders, and provision of lifesaving care, such as chemotherapy and surgical procedures, have been seriously compromised as a result of AR (Hiltunen et al., 2017; Martinez, 2012). The reason for this condition was explained as prophylactic antibiotics are commonly administered as part of surgery, organ transplantation, and cancer chemotherapy to prevent infections (Bow, 2013; Bratzler et al., 2013). Rising AR impacts these procedures’ efficiency and could lead to severe medical consequences (i.e., high morbidity, amputation, or demise) (Smith & Coast, 2013). Notably, most common surgical procedures and cancer chemotherapy are almost impossible if AR is not tackled urgently (Nursing Times, 2015). In the USA, it is projected that the organisms leading to surgical site infections (38.7% to 50.9%) and infections following chemotherapy (26.8%) exhibited their resistance towards the standard prophylactic antibiotics (Teillant et al., 2015). Besides, the present situation, which may perhaps be said to mark the beginnings of a post-antibiotic era, urgently calls for newer types of medicine and innovative methods of treatment (Fitchett, 2015).
Studies have shown considerable variability in antibiotic use across countries, with the sale and availability of antibiotics differing widely (Swedres-Svarm, 2012). Heavy antibiotic consumption, it has been reported, aggravates AR (European Centre for Disease Prevention and Control, 2013). Underlying the distribution and use of antibiotics are varying levels of awareness of bacterial resistance among healthcare professionals (Alzoubi et al., 2009). Several misconceptions about the conditions that prompt the use of antibiotics in various illnesses have been reported (Abu-Mostafa et al., 2017; André et al., 2010; Guntu et al., 2016). In a public survey conducted across twelve countries, two-thirds of the respondents claimed that they were aware of AR, though they were not sure of its consequences and prevention. In this context, national and international organizations (such as World Health Organization-WHO and the US Centers for Disease Control-CDC) have proposed strategies to control AR. Education has been identified as a key factor in battling AR (CDC, 2013).
The decreasing effectiveness of antibiotics imposes enormous health and economic burdens on societies globally. Measuring the economic outcomes of antibiotic resistance can help policy-makers and healthcare professionals set priorities (Gandra et al., 2014).
Review of Literature
Researchers have identified gaps in the knowledge and perception of practitioners regarding antibiotic prescription. In research conducted by Asante et al., 2017, in which 379 prescribers participated, with the majority of them being nurses (50%), the researchers noted gaps in the knowledge and perception of antibiotic prescriptions among prescribers. Likewise, awareness of the problems posed by antibiotic prescription was observed to be low among health practitioners in Gambia (Chaw et al., 2017). Along comparable lines but in a very different social context, in a study conducted at an outpatient clinic in the United States, prescriptions were given to 41% patients having clinical diagnoses of conditions that did not require antibiotics (Havers et al., 2018).
Determinants of nurses’ attitudes and actions in their prescription of antimicrobial medication have been researched in the field. Guidelines/protocols, safety, tolerability and effectiveness of the antimicrobial drugs themselves, patient/parent pressure, and training/experience have been examined as regulating factors (Ness et al., 2016). It is a matter of great concern that large numbers of health professionals, including nurses and doctors, lack up-to-date knowledge of AR (Abera et al., 2014). Several investigators highlighted a notable point concerning the insufficient training of healthcare professionals during their bachelor's degree course in the area of antibiotic use and resistance (Wright & Jain, 2004). Accordingly, Ahmad et al. (2015) revealed that pharmacy students possess good knowledge of antibiotic use. Nevertheless, those students’ had a poor attitude over antibiotic use. Compounding the problem is the phenomenon of self-medication, which has come to be identified as global in scope. Antibiotic self-prescription is prevalent among the general public and health professionals (Belkina et al., 2014; Mouhieddine et al., 2015). The key factors contributing to this phenomenon are friendly advice on self-prescription of antibiotics and access to pharmacies (Al Rasheed et al., 2016). Collectively, these phenomena strongly imply the need for a change in attitude toward antibiotic use. Educational strategies and carefully developed guidelines may improve the quality of antibiotic prescribing (Fleming et al., 2013).
Using medicines of quality and strength appropriate to clinical need minimizes the development and spread of resistance (WHO, 2001). This can be achieved through antimicrobial stewardship — a coordinated set of strategies designed to improve the use of antimicrobial agents (Trivedi et al., 2014). Studies have shown that nurses play a major role in initiatives taken to combat AR (Carter et al., 2018; Edwards et al., 2011; Ellen et al., 2017; Gillespie et al., 2013).
Antibiotic stewardship programs include mixed interventions, such as auditing, restriction of specific antibiotics, restriction of treatment duration, and antibiotic cycling or mixing (Cobos-Trigueros et al., 2016). Implementing antimicrobial stewardship programs has been shown to reduce hospital costs and use of antibiotics (Karanika et al., 2016). In 2017, a recent systematic review by Baur et al. (2017) make the case for the co-implementation of improved hand-hygiene interventions with antibiotic stewardship programs for better outcomes. Moreover, nurses can play a significant role in such effort as those are viewed as resource-persons in the implementation and sustenance of infection control practices. Also, nurses can take part in antibiotic stewardship and contribute to the success of care programs. However, nurses should be competent and have the right attitude to provide correct and in-depth information about antibiotic use, which, in turn, would help reduce resistance in patients and the general public. With these concerns and purposes in view, this study was undertaken to examine the knowledge and attitude of nurses regarding antibiotic use and prevention of AR.
Methods
Design and Participants
An institutional cross-sectional study was conducted in an acute healthcare environment in Riyadh, Saudi Arabia, from October 2018 to July 2019. A convenience sampling technique was adopted to choose participants for the study. A sample size of 350 was calculated through the single proportion formula for a finite population. The survey obtained a 97% response rate, with 341 responses to 350 questionnaires that were handed out. Nurses who chose not to take part were excluded from the evaluation.
Data Collection
Data were collected using a structured self-administered questionnaire designed specifically for this study after an extensive review of the literature. The questionnaire comprised three parts. Part 1 included the demographic information of the participants (9 items). Part 2 was related to the nurses’ knowledge of AR. It comprised 20 items categorized into three dimensions: facts about antibiotics, antibiotic resistance, and prevention of AR. All items were in the format of multiple-choice questions containing four different answers, with one right answer. Every correct answer was awarded a score of 1, while a wrong response was given a score of 0. A score of 10 (i.e., 50% correct answers) was used as the cut-off point to determine the level of knowledge; a score >10 was labeled ‘good knowledge’. Part 3 investigated the attitude of nurses towards prevention of AR (15 items). The items were rated on a 5-point Likert scale ranging from 1 (strongly agree) to 5 (strongly disagree). A score of 2.5 (50%) was labeled ‘poor attitude’, 2.6 (51%)–3.0 (59%) as ‘moderate’, and >3 (60%) as ‘good attitude’. A pilot study with a sample size of 120 was conducted to test the validity and reliability of the questionnaire. The tool was validated by 5 experts and the modifications recommended were incorporated into the tool. The reliability of the tool was measured using overall Cronbach's alpha value, which was equal to 0.7. In the current study, nurses were provided with comprehensive information pertaining to the proposed study protocol, and the expected outcomes. The nurses were then invited to participate, consent was obtained, and data collected using the structured questionnaire. Hard-copies of the questionnaire were distributed to the nurses; participating nurses were asked to drop their completed questionnaires in a box outside their department to maintain confidentiality.
Institutional Review Board Approval
Approval was obtained from the Institutional Review Board in the study setting. All the participants were visited in their units by the researchers and informed about the purpose of the study. It was made clear to them that participation was voluntary and their consent was then obtained. Data were collected from the completed questionnaires received. Confidentiality and anonymity were maintained throughout the study.
Data Analysis
The data were entered into a Microsoft Excel spreadsheet, validated for errors, coded, and exported to Statistical Package for Social Science (SPSS) Version 25 for analysis. Descriptive statistics were recorded for the demographic variables. Cronbach's alpha was used to assess the reliability of the survey instrument. Correlation (r) analysis was computed to understand the relation between knowledge of and attitudes toward antibiotics and antibiotic resistance prevention. The Chi-square test was used to find the association between knowledge and demographic variables, as also between attitude and demographic variables. All inferences were drawn at a 95% confidence interval with level of significance of 0.05.
Results
Demographic Characteristics
The majority of the participants [301 (88.3%)] were female. The mean age of the participants was 35.1 years; the mean nursing experience was 12 years. As for the professional qualification of the participants, 67.7% of them had a bachelor's degree, 28.7% a diploma, and 3.5% a master's degree. Most of the participants worked in critical/specialized (44.7%) and Medical (36.5%) nursing practice. 84.8% of the participants were registered nurses (Table 1).
Demographic Characteristics of the Study Population (n = 341).

Nurses’ Knowledge About Facts About Antibiotics, Facts About Antibiotic Resistance, and Prevention of AR
Concerning the facts about antibiotics, effective handwashing is the most important procedure to prevent infection from microorganisms. This item rated the highest, with a score of 97.1%. The lowest score of 29.1% was observed in the item ‘antibiotic resistance’, which is defined as bacterial changes that reduce or eliminate the effectiveness of antibiotics. A total of eleven items were found below 60% and nine items had a score of above 60% as seen in Table 2.
Knowledge Score of Nurses About Facts on Antibiotics, Antibiotic Resistance and Prevention of Antibiotic Resistance: Percentages of Correct Answers.

Attitude Towards Prevention of Antibiotic Resistance
As mentioned above in the ‘Data Collection’ section, participant attitudes were measured on a 5-point Likert scale, with scores ranging from 1 (strongly agree) to 5 (strongly disagree).
As regards the attitude of nurses towards antibiotic self-use, participants reported a mean score of 1.7 for general symptoms of the flu and a mean score 1.6 for antibiotics without a prescription. A good mean score of 4.1 found that participants read and understood the instructions before using antibiotics. A mean score of 2.2, reported for those nurses who kept antibiotics in stock, indicates their attitude towards self-use of antibiotics.
As for the nurses’ attitude towards strategies to prevent AR, their responses resulted in a mean score of 4.0. This indicates their attitude toward taking part in infection-control activities such as sanitation, hand washing, food, and water safety, and vaccination, all of which aim to minimize the spread of antimicrobial resistance. Also, a mean score of 4.0 was seen in escalated issues related to misuse of antibiotics. Half of all participants, with a mean score of 4.3, advised patients to complete the prescribed antibiotic course. A mean score of 4.0 showed how respondents saw themselves playing an active role in educating patients and families about the risk of AR. In the present survey, a mean score of 4.1 was reported that the respondents are advising other healthcare professionals as the appropriate use of antibiotics is important.
Moreover, a mean score of 4.0 showed respondents’ attitude toward their active contribution to institutional policies and guidelines focusing to control antibiotic resistance, which is the responsibility of a nurse. The respondents advocated the use of new generations of antibiotics that can fight diseases more effectively with caution with a mean score of 3.9. Those respondents were also recommending computer-based surveillance facilitating good antibiotic stewardship is important (mean score = 3.9). Further, those agreed that advising incorporating active interventions along with education to prevent antibiotic resistance is necessary one (mean score = 4.0). It is the responsibility of a nurse to follow clinical pathways in the management of infectious diseases is the responsibility of a nurse (mean score = 4.0) (Table 3). These data show the attitude of nurses towards prevention of antibiotic resistance.
Attitude of Nurses Towards Antibiotic use and Prevention of Antibiotic Resistance.

Nurses’ Overall Knowledge and Attitude Regarding Antibiotic use and Prevention of Antibiotic Resistance
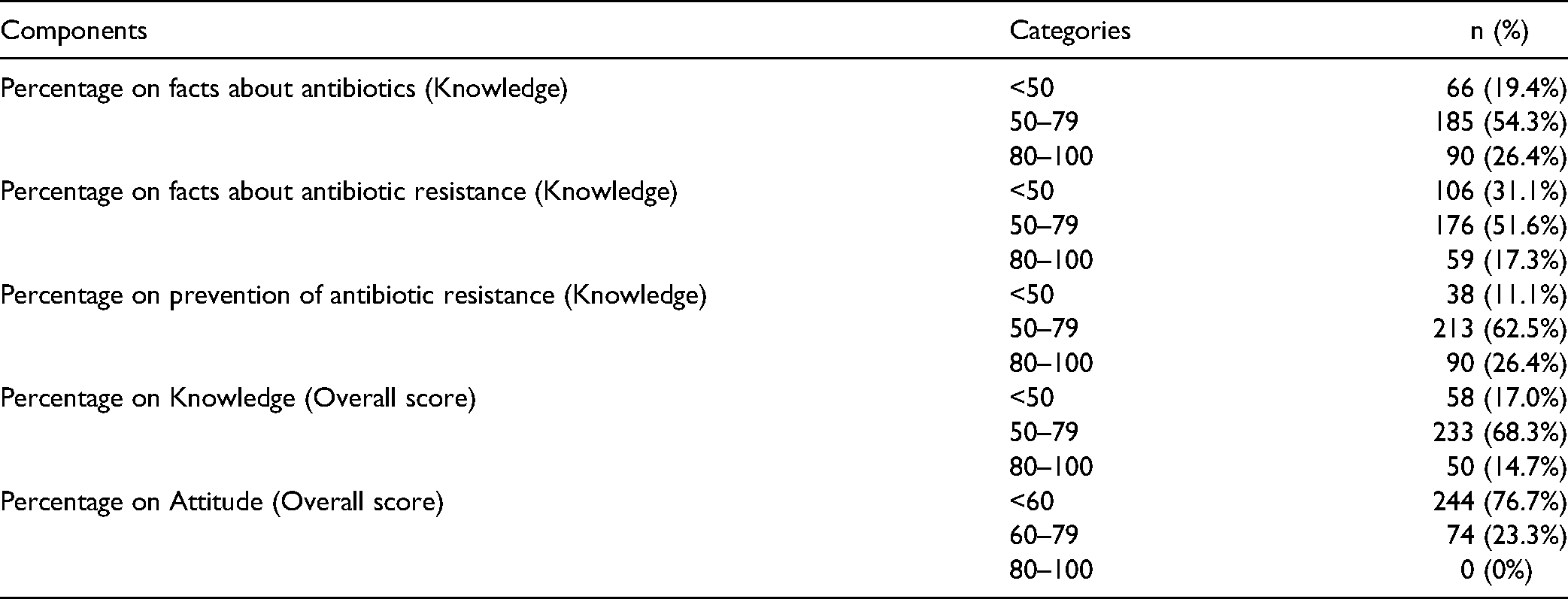
Knowledge of antibiotics among the nurses was observed to be 54.3% with moderate knowledge, 26.4% with good knowledge and 19.4% with poor knowledge. Nurses’ knowledge concerning antibiotic resistance was seen to be 51.6% with moderate knowledge, 31.1% with poor knowledge and 17.3% with good knowledge. Knowledge of prevention of antibiotic resistance was seen to be 62.5% with moderate knowledge, 26.5% with good knowledge and 11.1% with poor knowledge. The overall score on knowledge regarding antibiotics and antibiotic resistance was 68.3% with moderate knowledge, and only 14.7% reported having good knowledge. The overall score on attitude showed 76.7% with good attitude and 23.3% with poor attitude (Table 4).
Overall Assessment of Knowledge and Attitude.
Correlation Between Knowledge and Attitude
As can be seen in Table 5, the results showed a very low correlation between the overall knowledge score and attitude score, where r = 0.024 and
Correlation Between Knowledge and Attitude.

Association of Knowledge with the Demographic Variables
A significant correlation (
Association of Attitude with the Demographic Variables
No statistically significant association was observed between demographic variables such as age, job title, total years of experience, or specific training received on antimicrobial resistance, and the overall attitude towards prevention of AR. No significant statistical association between the overall attitude of participants and gender (
Discussion
Prevention of AR requires a multi-sectoral response, and every individual has a role to play in this context. Healthcare professionals, especially nurses, play an important role in the effort to prevent this global crisis. The experience and mindset of nurses has an impact on caregiving and education. The present research aimed to measure the awareness and attitudes of nurses towards the prevention of AR. There are several noteworthy findings in our study.
Only half of the respondents knew that bacteria can become resistant to antibiotics. The responses showed that nurses were not knowledgeable in this basic concept of antibiotic resistance.
More than half of all respondents had only moderate knowledge of the basics of antibiotics. A similar finding in another study reported that nurses performed poorly on a survey of knowledge, attitudes, and practices related to antibiotic use (Nair et al., 2019). However, our finding contradicts that of three studies in which nurses showed good familiarity with antibiotics (Jayaweerasingham et al., 2019) and knowledge of antibiotics (Sadasivam et al., 2016) (Sanneh et al., 2020). Another study revealed disparity among nurses concerning the awareness and understanding of optimal antibiotic prescribing practices. It revealed that Prescribers with a high awareness score showed positive prescribing actions (Farley et al., 2018). Conflicting opinions of nurses and medical residents concerning the need for antibiotics were reported in yet another study (Ahouah et al., 2019). Collectively, these findings highlight the need for training to address these issues and reinforce the central role of nurses in AR prevention strategies.
In the present study, none of the participants showed a clear, positive attitude, and a majority of the participants (76.7%) had only a fair attitude towards antibiotic use and the prevention of antibiotic resistance. This finding is consistent with a study that reported a negative attitude of nursing staff toward antibiotic use (Sadasivam et al., 2016). Another study reported that trainee nurses reported that intake of antibiotics would help prevent colds from worsening and lead to early recovery, thereby demonstrating a fair attitude (Jayaweerasingham et al., 2019). Yet another study indicated that 37.2% of respondents never discarded leftover antibiotics but rather kept them in stock, and thus revealed their attitude toward antibiotic use (Alex, 2019). In the present study, nurses showed a favorable attitude toward an antimicrobial stewardship program and activities related to such a program. In accord with the findings of this study, a study done in Pakistan reported that most healthcare professionals (HCPs), including nurses showed a positive attitude towards hospital-based antimicrobial stewardship programs (ASPs) regardless of their poor awareness about ASPs (Hayat et al., 2020).
As regards training, only a minority of participants (21%) in the present study had attended specific training on AR; a majority (94.7%) of the participants expressed the need for training on ASPs. This is consistent with the findings of Abera et al. (2014), which stated that most nurses expressed the need for ASPs. According to Alex (2019), it is observed that 87% of students of a medical school expressed the need for more education about AR. These findings illustrate the need for continuing education initiatives to enhance awareness of HCPs (Ahmad et al., 2015). Only a few participants reported that they actively participated in infection-control activities and strategies at the institutional level. The present study noted a positive attitude towards some aspects of prevention; however, the overall attitude of participants towards prevention of AR was negative. This contradicts the finding of Kistler et al. (2017), who reported evidence-based positive attitudes and behaviors of nurses. These findings indicate that a lot of work needs to be done to educate nurses and lay the foundation for an effective ASP.
In our study, we observed no statistically significant association of demographic variables like age, gender, and years of experience with knowledge and attitude towards antibiotics and antibiotic resistance. This finding contradicts to the results of a study by Hayat et al. (2020) who reported a significant association between age and years of experience with the knowledge regarding AR. However, the present study observed a significant association between the nurses’ working unit (
Strengths and Limitations
The present study addresses the major problem of antibiotic resistance and how nurses can play a vital role in devising and implementing strategies to prevent antimicrobial resistance. It also reports the lack of thorough knowledge of antibiotics among the participating nurses and an unfavorable attitude on their part in respect of the prevention of antibiotic resistance. Our study has also identified the need for training and focused intervention for clinical nurses on antimicrobial stewardship and on involving them in the prevention of antibiotic resistance. The present study, however, is limited to nurses in a multicultural health care setting in Riyadh, Saudi Arabia, which limits the generalizability of the findings. The use of antibiotics was basically self-reported, and the response may not be accurate due to difference in the ability of the participants to recall information or due to the tendency to give a socially acceptable answer rather than their actual belief about antibiotic use and prevention of antibiotic resistance. Despite these limitations, this study provides an insight into the frontline nurses’ knowledge and attitude towards prevention of antibiotic resistance.
Implications for Practice
Participation in antimicrobial stewardship programs and prevention of antibiotic resistance requires knowledge and a proactive attitude towards antibiotic resistance. This study identified that nurses need to improve their knowledge and have the right attitude to contribute effectively to strategies of antibiotic resistance prevention and to get involved in antimicrobial stewardship programs. The study provides baseline data in its research setting to develop a program that can enhance the knowledge and attitude of nurses.
Conclusions
Nurses, as frontline health workers, have an important role in the prevention of antibiotic resistance. The present study showed that nurses themselves are not fully aware of the basics of antibiotics antibiotic resistance and the methods to be employed in its prevention. As such, this study highlights the importance of tailored interventions to improve awareness and create a favorable attitude among nurses towards the prevention of antibiotic resistance.
Footnotes
Acknowledgments
We acknowledge the research center at the study setting for the grant and scientific editing services.
Ethical Considerations
Approval for the study was obtained from the Nursing Research Committee and the Institutional Review Board of the hospital under IRB Log Number 18-593. Written informed consent was obtained from all subjects after explaining the purpose of the study. Participation in the study was purely voluntary. Confidentiality and anonymity were maintained throughout the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the King Fahad Medical City (grant number RFA:018-049).
