Abstract
The extensive investment and development of research in molecular biology in the last decades, mainly after the completion of the Human Genome Project, has raised many expectations regarding its impact on Precision-Medicine Era. To meet the new demands for care, it is necessary that the omics sciences be integrated into nursing practice, especially in nursing care. Based on knowledge of structural genomics, it has been improved techniques that enabled the advancement of research related to functional genomics, which together comprising the “omics” sciences including the transcriptomics, proteomics, the epigenomics and metabolomics. The current challenge is to transform this expanded set of information into clinical benefits for patients, through more accurate diagnoses, treatments, and personalized care to the particularities of individuals and communities. For Nursing, the main challenge is the incorporation of the omics sciences in training and professional practice, so that nurses can safely, scientifically, and autonomously empower themselves to provide personalized care to individuals and families based on Precision-Medicine Era. In this paper, a debate on the impacts and challenges for Nursing to incorporate the Precision-Medicine into clinical practice is described.
Introduction
The speed with which new genomic knowledge with potential application to health care is being discovered and has been transforming the health care model is immeasurable(1−2). In fact, the extensive investment and development of research in molecular biology in the last decades, mainly after the completion of the Human Genome Project, has raised many expectations regarding its impact on Precision-Medicine Era (Khoury & Galea, 2016; Lopes-Júnior, 2021a). Additionally, genomic-based health care encompasses diagnosis, prevention and therapy based on the individual's genomic profile. This process considers the health-disease process as the result of combinations between the human genome and the influences of an individual's external and internal environment (Lopes-Júnior, 2021b; Tonkin et al., 2020).
In order to meet the new demands for care, it is necessary that the omics sciences be integrated into nursing practice, especially in nursing care (Lopes-Júnior, 2021a, 2021b; Tonkin et al., 2020). In this context, based on knowledge of structural genomics, it has been improved techniques that enabled the advancement of research related to functional genomics, which together comprising the “omics” sciences including the transcriptomics, proteomics, the epigenomics and metabolomics. Such approaches aim to understand changes in the functioning of the genome at different stages of development and under different environmental conditions, in order to provide a better understanding at the molecular level (Lopes-Júnior, 2021a; Tonkin et al., 2020).
Discussion of Topic
The sequencing of the human genome and the consequent genomic evolution generated high expectations in society and a certain ‘translational anxiety’ (Collins & Varmus, 2015; Iriart, 2019; Khoury & Galea, 2016). The Post-Genomic Era began two decades ago, and since then sequencing equipment and techniques have evolved rapidly to lower the cost of analysis and drastically reduce the time required for sequencing a complete genome (Collins & Varmus, 2015; Iriart, 2019; Khoury & Galea, 2016).
The advancement offered by Next Generation Sequencing – NGS consisted in its ability to produce and process a huge volume of data in an increasingly faster, more cost-effective and accurate way. Thus, with the advent of other technologies, such as bioinformatics, added to the association with the physiological information of patients, for example, through biomarkers, it becomes possible to understand the disease at the molecular level, increasing the effectiveness of diagnosis and treatment of several complex multifactorial diseases (Collins & Varmus, 2015; Iriart, 2019; Khoury & Galea, 2016).
While genomic data are decisive for understanding various diseases and drug effects on physiological systems, the gap between genotype (the individual's genetic load) and phenotype (observable characteristics) can be studied through the characterization of different omic levels, including the levels intermediates: proteome transcriptome, metabolome, in addition to studies of non-coding regions of DNA, rich in microRNAs and long non-coding RNAs, and gene expression sequences (Lopes-Júnior, 2021b; Regan et al., 2019; Tonkin et al., 2020).
Genomics is the science that studies genomes, that is, the complete collection of genes that make up an organism's DNA and their functions, as well as the interactions between them and between them and the internal and external environments (Lopes-Júnior, 2021b; Regan et al., 2019). Transcriptomics studies the set of cellular transcripts (RNA molecules) that genes express at a given time (transcriptome), under certain conditions. Proteomics, on the other hand, is the science that seeks to characterize and understand the set of proteins that constitute the product of the expression of genes in a given organism (proteome) and under what conditions these products are synthesized in certain tissues. While genome analysis allows us to assess the susceptibility of developing a certain condition, proteome analysis can lead to real-time diagnosis of what is happening to the individual. Metabolites are intermediate or end products of metabolism in a biological sample. The set of all low molecular mass metabolites, present or altered in a biological system, is called a metabolome. Metabolomics, in turn, is a field that consists of the systematic study of human metabolism responses to specific cellular processes induced by the use of drugs, environmental changes or the disease itself (Lopes-Júnior, 2021b; Regan et al., 2019).
Regarding functional genomics, reversible and heritable changes in the genome, which do not modify the DNA sequence, but which can make the response of individuals to certain conditions different, should also be considered. This area of knowledge is an object of study in epigenomics. Epigenomics aims to investigate and answer questions about how chemical modifications (for example, methylation, acetylation, phosphorylation, among others) in the nucleotides and histones of the DNA that constitute the genes occur over time as a function of environmental experiences and are transmitted to generations following (Lopes-Júnior, 2021b; Regan et al., 2019). Furthermore, the approach known as systems biology aims to integrate, on a large scale, the information on genotype and phenotype available, in order to enable interventions at a preventive and therapeutic level. This approach uses high-throughput equipment and advanced bioinformatics methods to consolidate, treat and systematize the diverse complex information of structural and functional genetics. The information from the different omics associated with a dataset on the phenotype of patients allow the identification of population subgroups, a necessary condition for diagnosis, prevention and treatments (Collins & Varmus, 2015; Lopes-Júnior, 2021b). (Figure 1).
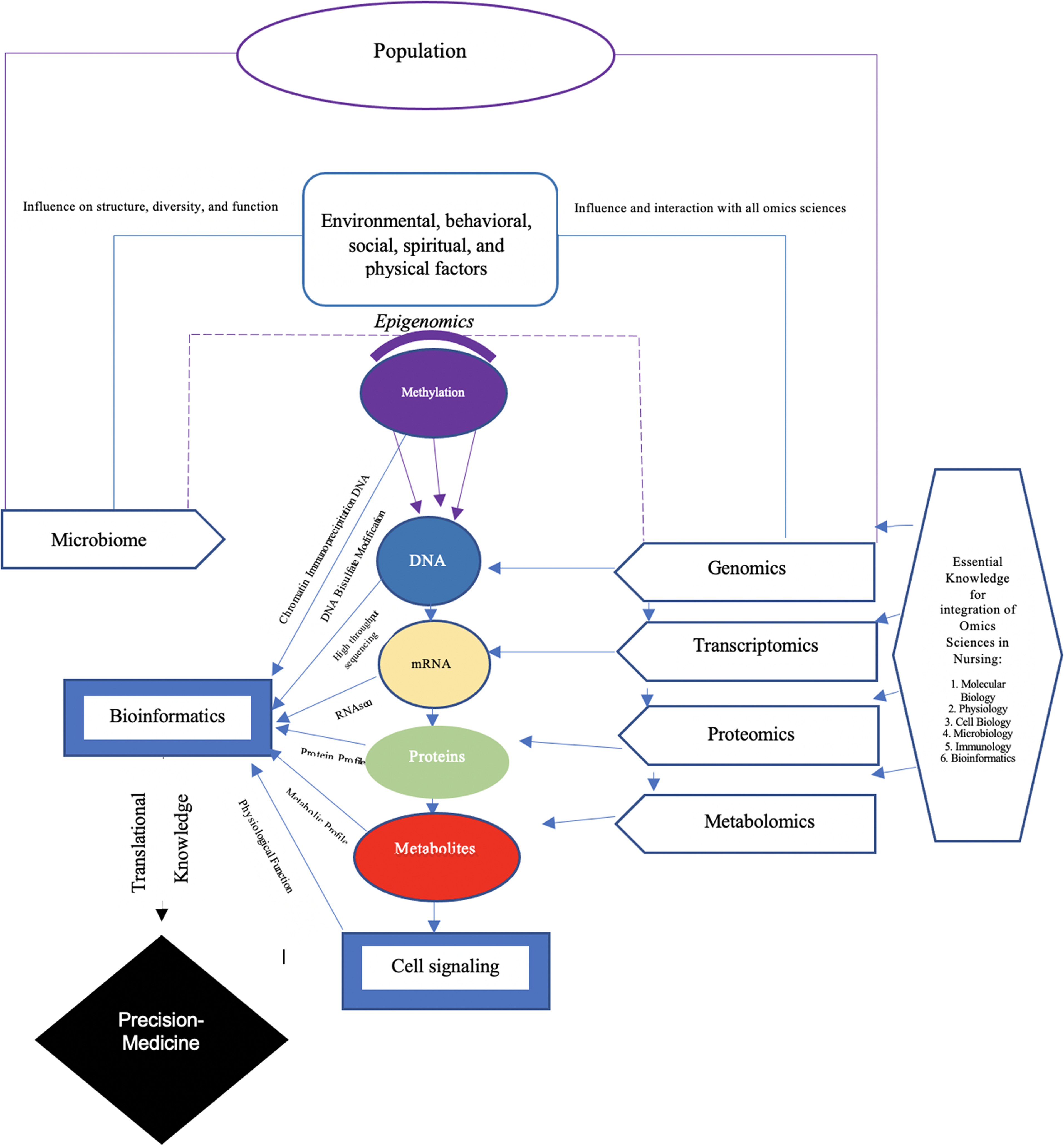
Integration of the omics sciences in nursing. Source: Adapted from Regan et al. (2019).
Current Insights and Interpretations
Precision-Medicine aims to customize treatment according to the biological characteristics of individuals or population subgroups (Collins & Varmus, 2015; Iriart, 2019; Khoury & Galea, 2016; Lopes-Júnior, 2021a). In clinical practice, we commonly observe that patients with similar symptoms may have different diseases, with different causes. Likewise, the same treatment may respond well in certain patients with a disease, but not in others who apparently have the same disease. The foundation of Precision-Medicine lies in the recognition that different groups of individuals have specific genomic characteristics, and those treatments must account for these differences (Collins & Varmus, 2015; Khoury & Galea, 2016).
The Precision-Medicine Era promises to offer, based on the identification of the patient's genetic characteristics, the precise medicine, in the exact dose and at the right time, thus making it more efficient and reducing the costs of medical care. When considering health care, the debate around Precision-Medicine generally includes a broader conception. Called P4 medicine, this concept adds a preventive, predictive, and participatory dimension to personalization (Collins & Varmus, 2015; Khoury & Galea, 2016).
In order for patients and their families to fully benefit from the explosion of omics, health professionals, especially nurses, need to incorporate the underlying principles of genomics that have been shaping all health care practice and that will become increasingly pertinent to their clinical practices (Amorim & Lopes-Júnior, 2021; Fu et al., 2019; Lopes-Júnior, 2013, 2015; Lopes-Júnior et al., 2017; Regan et al., 2019). These principles include, for example, the existence of alternative forms of the same gene (alleles) in the population; the occurrence of similar phenotypes arising from mutations and variations at different loci; the notion that certain diseases in families can arise from genetic variants that cause disease susceptibility through gene-gene and gene-environment interactions; the different types of mutations; the possibility of performing prenatal diagnoses, pre-symptomatic tests and population screenings; that is, unveiling the promise of personalized care to qualify health care (Fu et al., 2019; Lopes-Júnior et al., 2015, 2016, 2021; Regan et al., 2019; Tonkin et al., 2020).
It stands out that successful implementation of personalized nursing care in the Precision-Medicine Era requires interprofessional collaboration, community outreach efforts, and coordination of care. And this point is favorable for Nursing, since nurses are well-positioned to lead the implementation of precision health. Despite the surge of interest and attention to precision health, most nurses are not well-versed in precision health or able to understand its implications for the nursing profession. In this sense, it is imperative for the nursing profession to make strategic plans that promote personalized nursing care in the Precision-Medicine Era comprising nursing research, education, clinical practice, and health policy arenas (Fu et al., 2019).
As mentioned above, the ultimate goal of Precision-Medicine is to enhance precise diagnosis and personalized treatment of both rare and common diseases and to develop a new classification system that would align with greater utilization and application of omic data Khoury and Galea, 2016; Lopes-Júnior, 2021a). In this way, significant advancements have been made to prepare the nursing workforce to drive scientific discoveries and use data to improve population health and prevention efforts in the Precision-Medicine Era. For instance, nurses can investigate the effect of genetic variance in genes (pharmacogenetics) or many genes simultaneously (pharmacogenomics) and how this modifies human responses to pharmacological agents and diet (Dickmann & Ware, 2016; Shiao et al., 2018). By incorporating this knowledge into patient care, nurses can monitor and manage care with pharmacological agents to restore, maintain and promote patients’ health. Thus, nursing in the Precision-Medicine Era requires a focus on each individual's personal risk for disease and the effectiveness of treatments based on individuals’ unique combination of genomics and environmental risk factors. The effort to include nursing in the leadership of Precision-Medicine still faces challenges despite the fact that the nursing perspective is essential for successful implementation (Fu et al., 2019).
In order to deploy personalized nursing care into the Precision-Medicine Era, it is imperative for the nursing profession to make strategic plans that promote precision health in nursing research, education, clinical practice, and health policy. Nurses are well positioned to usher in this new era of Precision-Medicine and lead its integration into health promotion, disease prevention, and treatment using nursing's holistic approach (Fu et al., 2019).
Based on a critical analysis of literature and expert opinions (Fu et al., 2019; Regan et al., 2019; Tonkin et al., 2020), the Chart 1 provides an overview of personalized nursing care in the Precision-Medicine Era presenting the recommendations for nurses in clinical practice, education, research, and health policy.
Recommendations for Nurses in Clinical Practice, Education, Research, and Health Policy to Translate and Integrate the Personalized Nursing Care in the Precision-Medicine Era.

Source: Adapted from Fu et al. (2019).
Conclusions
Technological advances arising from the omics sciences have significantly expanded the set of available data to new possibilities for more effective treatments of diseases. The current challenge is to transform this expanded set of information into clinical benefits for patients, through more accurate diagnosis, treatments, and personalized care to the particularities of individuals and communities.
Nursing roles are paramount in the implementation of Precision-Medicine, including precision delivery of medications based on knowledge of pharmacogenetics, provision of personalized nursing care for patient, provision of family education about the meaning of omic tests, performance of health and family assessments, including the family history, and provision of critical feedback and insight on feasibility of implementing new technologies into workflows at the clinical point of care. With regards to the level of preparation, nurses in every clinical, educational, research and policy setting have an interdisciplinary team role to play in furthering the goals of the Precision-Medicine Era.
For the incorporation of new precision medicine technologies, it is essential to undertake a cost-benefit assessment from an ethical perspective, which considers whether they will be accessible to all who can benefit and whether they will not aggravate health disparities. Finally, for Nursing, the main challenge is the incorporation of the omics sciences in training and professional practice, so that nurses can safely, scientifically, and autonomously empower themselves to provide personalized care to individuals and families based on Precision-Medicine.
Footnotes
Authors' Contributions
LCL Jr conceived the paper, planned, supervised, wrote and interpreted the data, also critically reviewed successive versions of the paper and approved the final version to be published.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Disclaimer
Authors hold sole responsibility for the views expressed in the manuscript, which may not necessarily reflect the opinion or policy of the SAGE Open Nursing.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
