Abstract
The incidence of mental illness continues to increase since the start of the COVID-19 pandemic (Mental Health America, 2022). Demand for mental health services has grown, and providers report being “unable to meet the demand” or having an increase in wait times for access to care (American Psychological Association, 2022, para. 1). Due to this increase in demand, more patients are seeking mental health care from their primary care providers. Over the past decade, integrative models of care have been expanding into mental health care (Lake, 2017). Integrative Nursing is a strategy for improving the quality of care provided to patients seeking care for mental health diagnoses, as well as those with a goal of increasing mental health and wellbeing. This article proposes that Integrative Nursing can serve as a framework for providing whole-person mental health care.
The incidence of all mental illness in adults in the United States in 2020 was estimated to be 21% (U.S. Department of Health and Human Services, 2022); a noted increase has been reported since the beginning of the COVID-19 global pandemic (Mental Health America, 2022). In an article in
The demand for mental health care has increased dramatically since the pandemic began, according to the 2022 COVID-19 Practitioner Impact Survey conducted by the American Psychological Association ([APA], 2022). The APA reported that the demand for treatment of anxiety and depression has remained high in the years 2020-2022, and the need for treatment of substance use disorders, trauma, and stress-related disorders has grown. Practitioners also reported an increase in severity of symptoms they are treating; according to the survey, 60% of practitioners reported having no openings for new patients, 46% reported being “unable to meet the demand for treatment,” and 72% reported longer waiting lists since the start of COVID-19 (APA, 2022).
The increase in demand for mental health services leaves mental health and primary care providers searching for improved models of care to meet the growing demand for treatment, the increase in complexity of patients ‘needs, and providers ‘own need for health and wellbeing. Over the past decade, integrative models of care have been growing and expanding into mental health care (Lake, 2017). Mental health and wellbeing exist on a continuum of illness to wellness. Health-care providers must recognize that the presence of mental illness does not mean the absence of mental wellbeing; similarly, the absence of diagnosable mental illness does not guarantee the presence of mental wellbeing (Madhuleena, 2019). Therefore, it is useful for providers to consider the full range of conventional and integrative approaches to mental health care. While conventional interventions are well aligned with diagnosable mental illness, integrative interventions can serve as an important complement to manage secondary symptoms, enhance wellbeing, and build resilience as individuals fluctuate on the continuum of mental health. Varteresian and Lavretsky (2018) recommend that psychiatrists take an integrative approach to care as a means of promoting wellbeing, filling gaps in conventional care, and meeting patient demand. Nurses can apply a similar approach.
Integrative Nursing is one strategy that can serve as a useful framework for addressing the current needs of the health-care system, including the unique needs of mental health care, as a way of improving patient care while also considering the wellbeing of care providers (Kreitzer & Koithan, 2019). “Integrative Nursing is a way of being, knowing and doing that advances a whole health perspective to optimize wellbeing. Integrative nurses use evidence-informed strategies, including integrative therapies to support whole-person, system, and planetary healing” (Kreitzer et al., 2022, para 1). As a framework for practice, Integrative Nursing includes six principles that shape and inform care across patient populations and clinical settings. The principles are closely aligned with the American Nurses Association's (ANA)

Principles of Integrative Nursing
Psychiatric Mental Health Nurse Practitioners are held accountable for competence in helping patients use both pharmacological and nonpharmacological interventions to enhance their mental wellbeing by the National Organization of Nurse Practitioner Faculties (Population-Focused Competencies Task Force, 2013). Understanding the evidence base of complementary and integrative approaches and their application to practice is a critical component of meeting this competency. The National Organization of Nurse Practitioner Faculties ‘
Ensures patient safety through the appropriate prescription and management of pharmacologic and non-pharmacologic interventions.
Guides the patient in evaluating the appropriate use of complementary and alternative therapies. (Population-Focused Competencies Task Force, 2013).
Regardless of population focus, all nurses, including advanced practice nurses, have a responsibility for basic competence in the integration of non-pharmacological approaches to care. With the increased demand for mental health care and the shortage of access to mental health providers, nurses in a variety of settings, especially primary care, need resources to provide a whole-person approach to mental health care (Health Resources and Services Administration, 2022). Providing this upstream approach to care has the potential to prevent worsening of both mental and physical health symptoms, reduce health-care expenditures, and avoid the need to escalate care to scarce specialty resources.
Application of Integrative Care in Nursing Practice
Interpreting and applying the evidence base for integrative therapies and approaches can be challenging. There is no reliable database for searching
A common misconception is that integrative approaches should be reserved for patients with the least severe mental health diagnoses. While it is crucial that integrative approaches be used in primary care to prevent escalation of symptoms and interventions, it is equally important to use integrative therapies for serious mental illnesses, in conjunction with necessary pharmacologic management. The previously described Cochrane search revealed evidence for integrative approaches in patients with severe mental illness, including 26 systematic reviews related to schizophrenia and psychosis and the use of a variety of “complementary and alternative” approaches as adjunct interventions for the management of symptomatology associated with those diagnoses. Though much of the evidence is not strong enough to draw broad recommendations, it can be a guide for individualized whole-person care and provide an understanding of the safety profile of many integrative approaches. For example, eight studies reviewed the addition of omega-3 supplementation to a complete plan of care that includes medication management. The studies suggested that patients required smaller doses of neuroleptics and experienced improvements in mental state when omega-3 supplementation was added to their plan of care (Irving et al., 2006). Thirty studies reviewed the use of acupuncture for the management of schizophrenia symptomatology in addition to medications. Though the studies ranged in size and quality, outcomes such as reduced risk of relapse and fewer extrapyramidal symptoms were noted (Shen et al., 2014).
Integrative Mental Health Clinical Pathway
Patients often seek strategies in addition to or as an alternative to medication management. In cases of both uncomplicated and recurrent or persistent mental health diagnoses at all levels of severity, it may be reasonable to consider adjunct integrative interventions. Principle Five of the Principles of Integrative Nursing (see Figure 1) recommends the use of the full range of evidence-based interventions, beginning with the least intensive whenever possible (Kreitzer et al, 2022). Patients seeking care for mental health may present at various points on the treatment spectrum, from treatment-naive to treatment-resistant, or somewhere in between. Using person-centered and relationship-based care, as described in Principle Three (Kreitzer et al, 2022), the nurse can design an individualized plan of care using the Integrative Mental Health Clinical Pathway as a guide. A clinical vignette describes the application of the clinical pathway in practice.
This clinical pathway is designed to serve as an evidence-based, point-of-care tool in both psychiatric and primary care settings. The tool is designed to offer suggestions for performing a whole-person assessment and to organize the full spectrum of conventional and integrative interventions. While the focus of this clinical pathway is on all mental illnesses, with emphasis on depression and anxiety, components of it may also be useful for patients with severe mental illness, as well as patients with no diagnosable mental illness whose care goals include enhancing wellbeing and building resilience.
An Integrative Approach to Assessment
Providing person-centered and relationship-based integrative care begins with a comprehensive assessment. The Wellbeing Model (see Figure 2) serves as a complement to the Biopsychosocial Model (Tripathi et al, 2019), and may provide an avenue for probing deeper into the three components of that model: biological, social, and psychological. Consider the elements of the Wellbeing Model as an approach to whole-person care and strengths- based assessment. Using the Wellbeing Model also encourages consideration of social determinants of health and other environmental and community factors that may impact physical, mental, and emotional health and wellbeing.

The Wellbeing Model
Figures 3 and 4 show the Integrative Mental Health Clinical Pathway, beginning with considerations for performing an integrative assessment (Figure 3), and progressing through four levels of interventions, moving from least to most intensive (Figure 4).
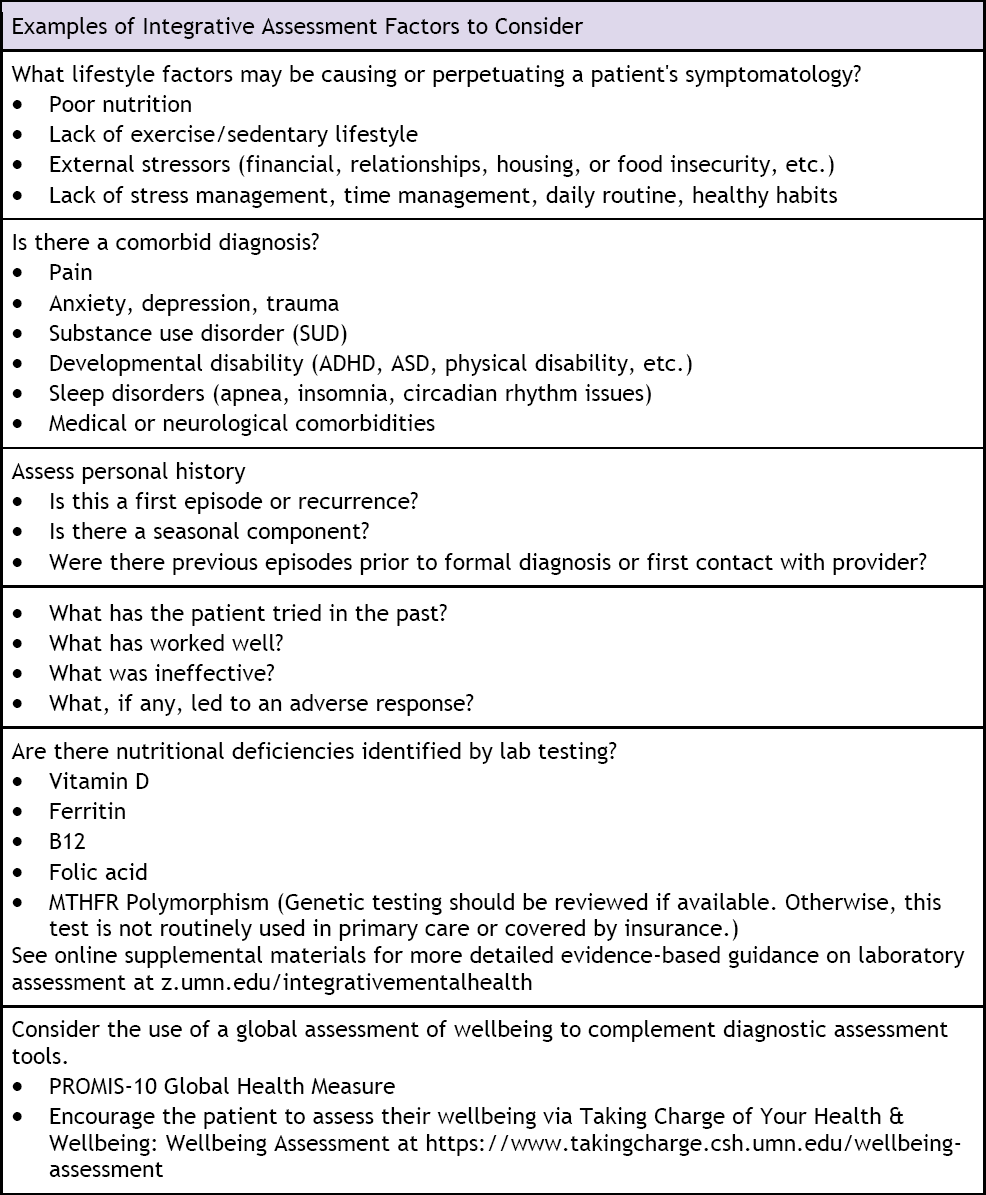
Integrative Mental Health Clinical Pathway: Assessment Section
An integrative approach to care recognizes the importance of understanding the root causes of disease or disturbance in wellbeing. While the advanced practice nurse must follow standard diagnostic assessment procedures for mental illness, the assessment elements in Figure 3 provide an additional level of depth for understanding the individual context and root causes of the mental illness. Following assessment and diagnosis, the nurse must identify mutually agreed upon symptoms as the focus of both non-pharmacological and pharmacological interventions, then begin the development of an individualized plan of care. The nurse and the advanced practice nurse have complementary and overlapping roles when working together to apply an integrative approach to mental health; while diagnostic assessment and prescriptive authority are reserved for the advanced practice nurse, all nurses excel at building rapport, coordinating care, teaching, and practicing hands-on mind/body skills with mental health patients.
Integrative Mental Health Interventions
Integrative interventions for mental health care can be organized into four levels, moving from least intensive to most, depending on the need and context of the patient (Kreitzer et al, 2022). Figure 4 outlines these evidence-based interventions.

Integrative Mental Health Clinical Pathway: Interventions Section
Clinical Vignette
A 43-year-old female presents to the clinic with chief complaints of fatigue, depression, and anxiety. She describes frequent feelings of tearfulness and overwhelm. She reports never feeling rested in the morning, which results in regular afternoon napping and the use of sugar and caffeine to “get through the day.” She gave birth to twins two years ago, which was a precipitating factor in the onset of depression symptoms, separation anxiety, and new OCD tendencies around cleanliness. She has been working with a therapist and getting a massage monthly, which has been helpful. She has a history of depression and anxiety in college. At that time, she tried a selective serotonin reuptake inhibitor (SSRI) and experienced some improvement in depressive symptoms but noted an increase in gastrointestinal upset and decreased libido. She discontinued the medication due to these side effects. Her medical history includes Polycystic Ovary Syndrome (PCOS) and chronic low back pain. Her current medication regimen includes a combined oral contraceptive. She reports an irregular eating pattern, often snacking on processed foods higher in sugar and refined carbohydrates and eating right before bed. Her sleep pattern is irregular, and she is often up late scrolling social media in bed. Her sleep is frequently interrupted by children during the night; she sleeps six hours per night and feels restless. She denies significant snoring. She engages in high- intensity workouts three times weekly, which seems to help with anxiety; however, she feels more fatigued afterwards and has gained weight despite regular exercise. She describes her marriage as supportive. She works full time in logistics; her anxiety is often triggered by work performance and perfectionism.
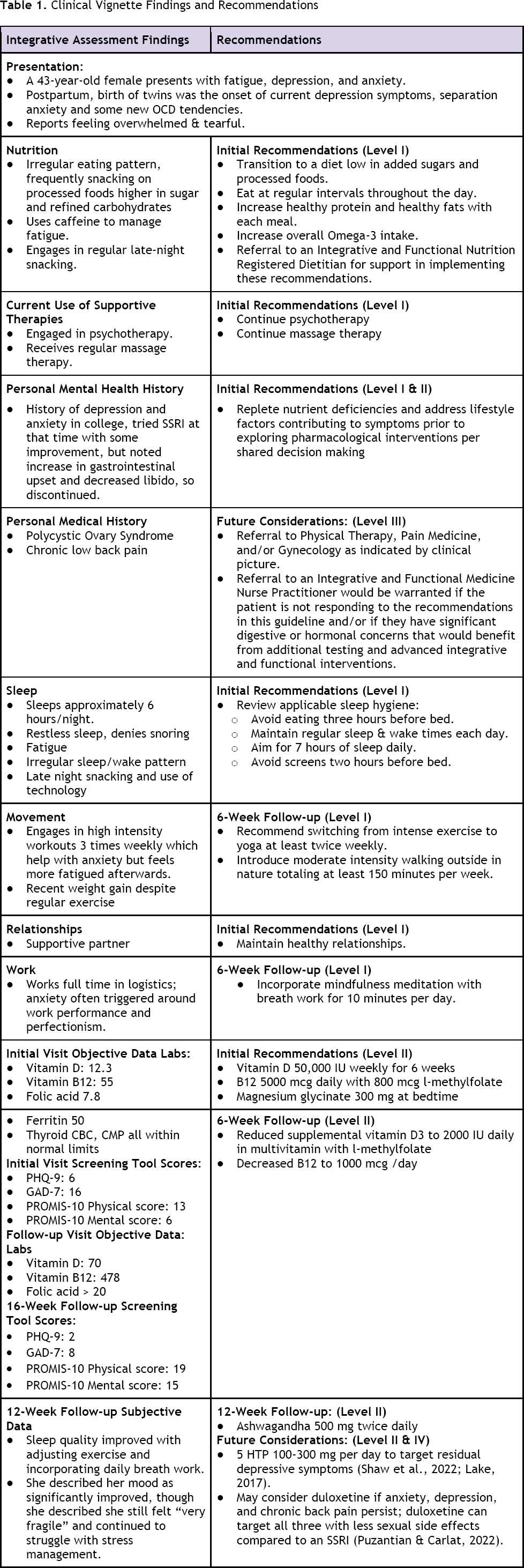
Table 1 outlines assessment findings and interventions at the initial visit, 6-week follow-up, 12-week follow-up, and 16-week follow-up. At the 16-week follow-up, the patient reported her fatigue had resolved completely. Her depression and anxiety symptoms were significantly reduced and were no longer impairing her daily function, as evidenced by her assessment score changes. The maintenance plan of care includes continued supplementation, maintaining lifestyle changes, and annual follow-up for laboratory monitoring and ongoing assessment.
Clinical Vignette Findings and Recommendations
Conclusion
As described in this paper and demonstrated in the clinical vignette, an Integrative Nursing approach to whole-person mental health care begins with deeply listening to the patient's story, with careful focus on the underlying lifestyle factors and environmental and relational contexts that may be causing or perpetuating symptomatology. In the context of relationship-based care, the integrative nurse helps the patient prioritize interventions with shared decision making, starting from the least intensive options when appropriate. This approach often requires lifestyle change and the use of interventions that require time and consistency to demonstrate change; multiple visits over several months are typically required. Ongoing assessment and adjustment of the plan based on the patient's clinical response and readiness to change are crucial. The goal of care is to address the root causes of symptomatology, when possible, to promote the patient's innate capacity for healing and wellbeing, and to provide symptomatic relief, including pharmacotherapeutic interventions when appropriate. The ability to apply the evidence for integrative therapies in a personalized way is the art and science of Integrative Nursing for whole-person mental health.
Supplementary Materials
An online supplement with additional detail on the elements of the integrative mental health clinical pathway can be accessed at z.umn.edu/integrativementalhealth or by scanning this QR code.

Cite this article
Voss, M.E., Sandquist, L., Otremba, K., & Kreitzer, M.J. (2023). Integrative nursing: A framework for whole-person mental health care.
Footnotes
Acknowledgement
The authors would like to acknowledge the contributions of Dr. Lidia Zylowska, MD, and Dr. Crystalin Montgomery, ND, Lac. Their work in integrative psychiatry informed the development of the clinical pathway.
Megan E. Voss DNP, APRN, PMHNP-BC, (she/her), is an Associate Professor and Director of Education at the Earl E. Bakken Center for Spirituality & Healing and an adjunct clinical associate professor in the School of Nursing at the University of Minnesota in Minneapolis, Minnesota, US. She is also a practicing board certified psychiatric mental health nurse practitioner in the M Health System at the University of Minnesota.
Laura Sandquist, DNP, APRN, A-GNP-C, IFMCP, (she/her), is an Integrative & Functional Medicine Nurse Practitioner and Clinical Lead for Integrative & Functional Medicine at the Penny George Institute for Health and Healing at Allina Health in Minneapolis, Minnesota, US. She also co-teaches the graduate level Integrative Mental Health course at the Earl E. Bakken Center for Spirituality & Healing at the University of Minnesota in Minneapolis, Minnesota, US.
Kate Otremba DNP, APRN, A-GNP-C, IFMCP, (she/her), is an Integrative & Functional Medicine Nurse Practitioner at the Penny George Institute for Health and Healing at Allina Health in Minneapolis, Minnesota, US.
Mary Jo Kreitzer, PhD, RN, FAAN, FNAP, (she/her), is the Director of the Earl E. Bakken Center for Spirituality & Healing, and a Professor in the School of Nursing at the University of Minnesota in Minneapolis, Minnesota, US.
