Abstract
Introduction
The dementia disease affects both the family caregivers’ health and social and psychological well-being. The aim of this review was to identify and describe the needs of family caregivers living with a person with dementia at home.
Method
The literature review, conducted using the matrix method, was also inspired by Thomas and Harden’s thematic synthesis.
Results
Three themes were identified: (1) the family caregiver’s new roles and relationships; (2) caregiver burdens; and (3) the caregiver’s need for information and support.
Conclusion
When family caregivers gradually lose their reciprocal relationship with the person with dementia, and sometimes also with family and friends, the need for other kinds of social contact arises e.g. with others in a similar situation. They also need to have some respite to provide room to pursue their own interests and take care of their own health. Also, a high level of individually tailored information is needed.
In recent years, dementia has become a worldwide important issue as estimates indicate that the number of individuals living with dementia worldwide will increase from 47 million people in 2015 to 75 million in 2030 and 135 million people by 2050 (Alzheimer’s Disease International, 2018; World Health Organization, 2017). Higgs and Gilleard (2017) argue that conditions concerning dementia go beyond its epidemiological significance and lead to loss of a personal basic infrastructure that supports one’s agency, awareness, communication judgement and reasoning. Confronted with this scenario the person living with dementia fears to lose his mind, and his place in the adult world leading to having a considerably influence on his life but also on the lives of his family (Higgs & Gilleard 2017).
In the European Union (2012) relatives are becoming an increasingly important resource in providing care for family members due to political incentives designed to reduce severe constraints on fiscal policy (Bremer et al., 2017; Colombo et al., 2011).
Thus, family caregivers represent a pillar in future care, for which reason it becomes relevant to reflect on how family caregivers manage this new life situation involving both practical and emotional challenges concerning conditions due to dementia.
Thus, transitioning into becoming a family caregiver entails major individual consequences, often leading to intertwined changed roles and reshaping of the caregiver’s life course (Pearlin, 2010). Previous research shows that caring for a person living with dementia can affect health and social and psychological well-being of caregivers; often referred to as the caregiver burden (Brodaty & Donkin, 2009; Campbell et al., 2008; Lethin et al., 2020). The literature, however, often overlooks how family caregivers experience their own individual challenges and needs (Bangerter et al., 2019) for which reason the elucidation of the needs of the individual family caregiver can be important to promoting quality of life, decreasing stress and delaying hospitalisation of the person with dementia (Brodaty & Donkin, 2009).
The aim of this article is to identify and describe the challenges and the needs that emerge among family caregivers living together with a person with dementia.
This target group is chosen as they are being confronted 24/7 with new challenges and changed behaviour of a beloved family member which is assumed having a considerable impact on daily living and well-being of the family caregiver.
The existing literature use various terms for family caregivers, e.g. relatives, caregiver or informal caregiver synonymously. This review consistently uses the term family caregiver, regardless of the terms used in the articles referred to.
Literature Search
To secure a firm structure, the Matrix Method was used as the overall approach to the literature review (Gerrard, 2007). This method consists of four parts: A paper trail to keep track of the search and selection process, a compilation of digital versions and hardcopies of all selected articles, a matrix to get an overview over them and, lastly, a written synthesis based on a thorough analysis.
We conducted a block search with key terms divided into four blocks including the Boolean operators AND and OR as shown in Figure 1.

Search Strategy.
We ran the block search in PubMed, Embase, PsycINFO, Idunn and SweMed+, supplemented with snowball technique, which is a metaphoric term referring to – like a snowball that gathers more and more layers of snow – the process of gathering new layers of references by following relevant references in the articles’ reference lists (Gerrard, 2007).
Inclusion and Exclusion Criteria
Articles focusing on family caregivers living with a person with dementia written in Danish, English, German, Norwegian, Spanish and Swedish were included. Studies focusing on family caregivers, who did not live with the person living with dementia, were excluded. We applied no criteria for publication dates or research methods but only peer-reviewed articles were included. No further quality assessments were applied.
Selection of Articles
Our searches resulted in 2050 articles, which were examined for suitability based on review of titles, abstracts, and full text, leading to a gradual selection of 34 scientific articles as shown in Figure 2, and they were registered into a matrix (Gerrard, 2007) as shown in Table 1.

Flowchart.

Matrix – Characteristics of Included Studies.
Analysis
Since the Matrix Method does not offer a specific process for the analysis itself, our analysis is inspired by the thematic synthesis developed by Thomas and Harden (2008), who consider all text under the headings findings or results as data. Based on our research interest, we extracted 267 excerpts about the challenges and needs of family caregivers that were either directly mentioned or indirectly embedded in the text. To secure rigour in the analysing process each article was labelled with a letter A, B, C etc. At the end of the alphabet, we doubled the letters AA, BB, CC… AAA, BBB etc. Excerpts were identified and numbered. The first excerpt in the first article was given A-1, the next A-2. The first excerpt in the fourth article was given D-1 etc. By labelling every excerpt we ensured the possibility to find the original context no matter how far we went in the decontextualizing process.
Step one of the analysis involved coding each excerpt with a key term. Step two involved creating a hierarchical structure based on the coding that comprised 13 descriptive themes and 69 sub-themes. Based on the descriptive themes, step three entailed going “beyond the content of the original studies” (Thomas & Harden, 2008, p. 7) to generate analytical themes. To get a deeper understanding of the experiences of living together with a person suffering from dementia we created new descriptions representing the meaning embedded in each sub-theme. As a process of internal validation, these representative descriptions were continuously compared to the original excerpts to ensure that the meaning was not altered in a contradictive way. Getting deeper into the meaning of the descriptive themes, three analytical themes appeared across the descriptive themes, which will be presented in the findings below.
Findings
Undertaking the role of family caregiver to a person with dementia often leads to a new, unexpected and unwanted life situation. Caregivers must adjust to new roles, tasks, and responsibilities as the dementia disease progresses. Adapting to this new situation is an act of becoming, which implies a quest to imagine a new kind of life for themselves as a family caregiver, i.e. to become a different kind of person due to the changed life situation. As shown in Figure 3, three analytical themes including seven sub-themes were extracted: (1) the family caregiver’s new roles and relationships, (2) caregiver burdens, and (3) information and support. In accordance with the aim of the study, each theme will be briefly followed by perspectives on challenges and needs.
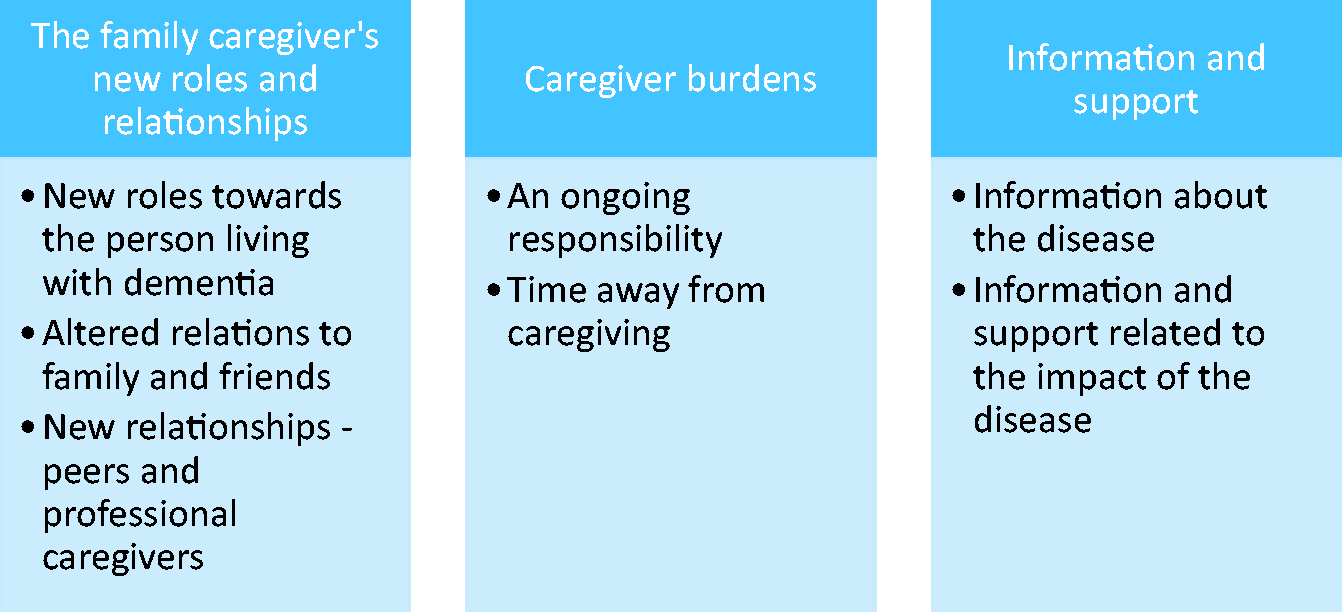
The Thematic Structure.
The Family Caregiver’s New Roles and Relationships
Being a family caregiver to a person with dementia implies undertaking new roles in relation to people within the caregiver’s inner social circle, primarily the person with dementia, family members and close friends, whose well-known roles and relationships will change as the dementia disease progresses.
Many family caregivers can no longer understand how their relative experiences day-to-day life. This situation may lead to an inability to empathise with one another and thus, feelings of interpersonal distance and grief (Pini et al., 2018). This sense of distance in the relationship grows as the disease develops and as the personality of the demented person gradually erodes. Sometimes memory problems can cause difficulties in conversations and even lead to conflicts and family caregivers might miss the everyday talk and intimate conversations when the person with dementia is no longer able to go into an equal dialogue (Storjord & Lykkeslet, 2017).
New Roles Towards the Person Living with Dementia
When the personality of the person living with dementia changes, also the perception of being a couple can gradually change and the role of the healthy spouse may be experienced more like a care provider rather than a spouse (Meyer et al., 2016). The literature describes a variety of new roles taken on by family caregivers, e.g. being a formal guardian (Landmark et al., 2013), handling the finances (Kuhn, 1998) or taking care of intimate tasks (Rayment et al., 2019). Some husbands struggle to improve their housekeeping skills and worry about providing healthy meals (Fjellström et al., 2010), while another study shows that many female spouses feel that the caregiver role “fell within their normative expectations of the spousal role” (Stirling et al., 2010, p. 7). In addition, family caregivers undertake various roles, e.g. as a supervisor, facilitator, or parent based on the situation at hand. Shifting between the assorted functions is described as becoming “full-time actors and for the play to end, the spouse or partner had to leave the common stage permanently, in some way or another” (Lövenmark et al., 2018, p. 4).
Altered Relations to Family and Friends
Family caregivers also experience feelings of loneliness due to a reduced social network (Flynn & Mulcahy, 2013; Johannessen et al., 2017; Pini et al., 2018). Arranging and participating in social activities demand energy, and as friends and family can find it difficult to deal with awkward situations due to conditions caused by the dementia, they often withdraw from the person living with dementia and thus the family caregiver might feel lonely (Shanley et al., 2011). In addition, the concerns about how the diseased relative might behave in public in general can be a reason for staying at home, causing further social isolation. Some family caregivers find ways to set up social interaction with friends (Pini et al., 2018); but even relationships with close family members can break if the family caregiver does not have the energy to maintain the relationships by visiting others or attending activities outside the home.
New Relationships – Peers and Professional Caregivers
Family caregivers value contact with other people who are in a similar situation (Huis in het Veld et al., 2018; McKechnie et al., 2014; Rayment et al., 2019; Torp et al., 2008). In peer groups, family caregivers can experience a personal space that allows them to let off steam and to feel like they are not alone in recognising the experiences of other group members. Thus, peer groups are a source of social support that provides family caregivers with opportunities to learn new ways of coping (Melunsky et al., 2015). Similarities in age, position in the family, disease progression and behavioural changes is considered important (McKechnie et al., 2014; O’Connell et al., 2014).
As the disease progresses, the need for professional support grows and professional caregivers enter the home and gradually establish joint responsibility for taking care of the person with dementia. However, the professionals also need to be aware of the family caregiver’s own needs (Storjord & Lykkeslet, 2017), and family caregivers value professionals who recognise the complexity of their responsibilities. It is emphasized that it is important for family caregivers to “feel they were still seen as the primary caregiver and genuinely involved in decisions about care of the person with dementia” (Shanley et al., 2011, p. 332).
Family caregivers find it important that professionals relate to the person with dementia on a personal level and focus on the same goals as preferred by the person with dementia and the family caregiver. In this regard, trusting relationships are important for family caregivers to allow professionals to meet the needs of the person with dementia and of the family caregiver. They might worry whether the professionals can deliver the needed care to their relative (Macleod et al., 2017; Shanley et al., 2011). In addition to this, it also appears to have an impact on the family caregiver’s relationship with the professionals, that there is a continuity within the staff, as they are concerned about frequent changes, which can be upsetting for the person with dementia (Macleod et al., 2017).
Challenges and Needs Related to New Roles and Relationships
As the reciprocal relationship between the family caregiver and the person living with dementia gradually diminishes, the family caregiver needs to have social contacts outside the home. When living with a person with dementia the family caregiver needs to be prepared for the challenges that will arise. They need to learn how to perform new, unknown care activities and how to handle difficult, somewhat awkward situations. When professional caregivers enter the home family caregivers need to be acknowledged in their efforts to do the best for their loved one, and they need to be actively involved in decisions about the person with dementia.
Caregiver Burdens
An Ongoing Responsibility
Taking care of a person with dementia implies a full-time responsibility. The burden implies constant fear for safety and security of the person with dementia if, for example the person attempts to leave the home unaccompanied (Olsson et al., 2012). To relieve the ongoing dependency on the family caregiver, a study shows that “Assistive technology that enabled the person with dementia to become more independent and undertake meaningful activities during the day, like mastering the TV remote control, was considered important” (Holthe et al., 2018, p. 758).
Family caregivers experience an overwhelming sense of responsibility in terms of dealing with e.g. medication (Rayment et al., 2019), feeding, and cooking, which for inexperienced food providers can be a major challenge (Fjellström et al., 2010). Also the financial costs of caregiving e.g. due to the loss of income can be of major concern (Flynn & Mulcahy, 2013) as well as an uncontrolled spending money by the person with dementia which can be challenging for the family caregiver to deal with (Johannessen et al., 2017).
Time Away From Caregiving
In addition to the above mentioned burdens household chores and practical tasks, such as shopping or paperwork, can take up their extra time, leaving little time left for the family caregivers themselves (Pini et al., 2018; Shanley et al., 2011). Formal respite services or support from friends and family can generate valuable time away from caregiving responsibility and are by some seen as an opportunity to maintain their social network (Shanley et al., 2011; Strandli et al., 2016). However, the quality of respite services and the feeling that the person with dementia is safe and taken good care of can be of great importance in allowing the family caregivers to feel relaxed (Macleod et al., 2017; Pini et al., 2018; Shanley et al., 2011; Strandli et al., 2016). Lack of time away from caregiving affects the family caregiver’s well-being, stress level, and ability to care for the person with dementia (Ducharme et al., 2014; Macleod et al., 2017; Meyer et al., 2016; Rayment et al., 2019). Furthermore, they might find that asking for help is embarrassing or that it is an indication of them not being capable of caring for the person with dementia on their own (Macleod et al., 2017, p. 770).
Coping with the limbo of not knowing how one’s life situation will turn out in the long run can be tough as concerns about an unpredictable and unknown future are ongoing, just knowing that it will get worse (Storjord & Lykkeslet, 2017). Caregiver burdens may vary in form and intensity, but a common issue for family caregivers is that they feel full responsibility for carrying every kind of burden, regardless of the efforts of the professionals, and this responsibility will remain throughout the course of the disease. They do not have the option to refrain from caregiving, they are constantly in a position where they must balance between their own needs, and those of their relatives, which in general are prioritized (Quinn et al., 2015).
Challenges and Needs Related to Caregiver Burdens
Because of the constant responsibility and pressure, family caregivers need to be aware of their own health and well-being. Therefore, they need respite time to manage stress and pursue their own interests in life. Nevertheless, spending time away from caregiving can be a great challenge. Paradoxically, it seems that arranging respite time might add to the amounts of burdens instead of relieving the burdens the family caregivers need a break from. In other words, burdens may obstruct having time away from burdens.
Information and Support
Information About the Disease
When a dementia disease enters the daily living, the family caregivers need a variety of information (Flynn & Mulcahy, 2013; Huis in het Veld et al., 2018; Peeters et al., 2010; Rosa et al., 2010; Steiner et al., 2016; Torp et al., 2008; Vaingankar et al., 2013). Many family caregivers feel unprepared and in great need of knowledge about the dementia disease and illness trajectory. They need to know what to expect at present and in the future. A study reveals that information about the “illness and the illness trajectory was of particular interest as it gave them a greater understanding of what they could reasonably expect of their spouse and they were also better prepared for what was likely to occur in the future” (Torp et al., 2008, p. 79).
Although the need for information about the disease is predominant, some studies also mention family caregivers who experienced an overload of information about the disease at times when they were not yet ready to receive it (Holthe et al., 2018; Huis in het Veld et al., 2018; Rayment et al., 2019). This indicates that the individual timing, of when information is delivered, is important and that family caregivers often prefer to get the specific information, when they need it (Huis in het Veld et al., 2018; Wawrziczny et al., 2016). Some caregivers explained that they preferred to only get information about the initial stages of the disease at the beginning of the disease trajectory and then wait with information about the final stages until their loved one faced the last stages (Killin et al., 2018). Meyer et al. (2016), on the other hand, indicate that some family caregivers consider that information about dementia should be provided at an early stage.
Overall, the needs of family caregivers concerning when to receive which kind of information seems best met using an individual approach, since the families are in different situations. Furthermore, some studies mention that family caregivers think that it is important to have one person providing the information as independently searching all over for information can be difficult and confusing (Chan et al., 2010; Diehl-Schmid et al., 2013; Shanley et al., 2011).
Information and Support Related to the Impact of the Disease
Apart from information about the dementia disease itself, family caregivers need support to develop effective carer-to-patient communication skills (Rosa et al., 2010) and to learn how to act towards and communicate patiently with the person with dementia (Kuhn, 1998). A key factor for benefiting from the information appears to be that it is provided in a way that helps the family caregiver feeling competent and in control of the situation. Consequently, providing the information and supporting new skills in a caring and non-judgmental way appears to be essential since dealing with an array of opinions and judgements may make caregivers feel unsettled (Huis in het Veld et al., 2018; Pini et al., 2018; Shanley et al., 2011).
The family caregivers also need information about legal and financial issues, as well as advice on how to submit applications for service (Ducharme et al., 2014; Johannessen et al., 2017; Macleod et al., 2017; Stokes et al., 2014). Furthermore, they need information about the transition to a nursing home and how to gain access to respite care (Shanley et al., 2011; Vaingankar et al., 2013) as well as how to manage their own stress (Steiner et al., 2016).
As social and emotional support is imperative for family caregivers, relatives, experienced professionals, and peers are important sources of emotional support (McKechnie et al., 2014; Rayment et al., 2019; Shanley et al., 2011; Torp et al., 2008). Some of the benefits of support are not to feel alone and the feeling of being understood through shared experience (McKechnie et al., 2014).
Technological solutions can represent another source of support, which some caregivers find helpful while others experience it as challenging. A study concludes that support “can be provided to some extent through eHealth, but this cannot replace personal contact entirely. Support must always be geared to the personal situation” (Huit in het Veld et al., 2018, p. 158).
The availability of an accessible resource person with knowledge about the dementia combined with experience to understand the family caregiver’s situation, and who can help them to navigate through available information, can be helpful (Shanley et al., 2011). The family caregivers want to have just one person who can provide all kinds of information and they need what Diehl-Schmid et al. (2013) call all-inclusive information packages. However, all-inclusive information packages do not mean one-size-fits-all standard information, as non-specific information can be perceived as unhelpful (Ducharme et al., 2014; Macleod et al., 2017).
Challenges and Needs Related to Information and Support
Family caregivers need to learn new skills and knowledge to be able to manage to adapt to their new situation. They have an extensive need for information about dementia and about what kinds of support is available, as well as a need to receive various kinds of support. There is a need for information that is individually tailored that takes into account the circumstances within each family to ensure proper information and support without overloading the family caregiver.
Discussion
Our study shows that the family caregivers´ burdens and subsequent needs are overwhelming, and they have to adapt to their circumstances and learn new skills in an extremely strained situation. An overall look at the findings in our review brings two perspectives for further discussion into focus. Firstly, the similarities and differences in the needs of family caregivers will be discussed in relation to other studies. Secondly, the study reveals that the family is placed in a key role as caregivers for people living with dementia, which entails an apparent imbalance between the family caregiver´s burdens and needs and societýs general expectations toward caregivers. This discrepancy between the needs of family caregivers and existing dementia care policies will be discussed in the light of Tönnies’ (2002) concepts of
Similarities and Differences in the Needs of Family Caregivers
At first glance, the lives of family caregivers appear to be similar but with a closer look, individual differences become important regarding how to understand and support family caregivers. People living with dementia go through all-encompassing changes in cognitive skills, psychological state and behaviour that permeate the lives of family caregivers in many similar ways. Relationships are broken and the family caregivers have overwhelming burdens with almost no time to spend on themselves. They neglect their own needs and they have lost a beloved person they once knew. In that light, it could be tempting to perceive family caregivers as a homogenous group with the same needs for support.
However, family caregivers comprise of many different kinds of individuals, each living in distinctive contexts. People living with dementia also differ from one another, as dementia is an umbrella term for many diseases developing individually (World Health Organization, 2020). Consequently, although family caregivers at first may appear to look alike, understanding each caregiver´s individual needs and grasping how to support those needs on an individual basis is crucial (Bangerter et al., 2019; Brodaty & Donkin, 2009; Kaschowitz & Brandt, 2017). The apparent sameness and underlying differences between family caregivers spans the themes in the review, and their individual differences prepare the ground for a discussion of how to support them individually. A study of family caregivers’ use of services made available for them implied that “caregiver service use is related to caregiver characteristics” (Martindale-Adams et al., 2016, p. 1053), which supports the notion of adapting the support to each individual caregiver. A review of the effects of social support interventions shows that the effects are inconsistent, i.e. what works for some of the caregivers, does not work for others (Dam et al., 2016). Another review (Farina et al., 2017) emphasises that supporting the caregivers’ own health, their independence, and their possibilities to pursue their own interests is the most important factor in sustaining their quality of life. A study on developing online support for family caregivers (Davies et al., 2019) underlines the need to feel in control of the care situation. The above mentioned studies indicate that not all family caregivers benefit from the same kind of support, which is why the support should be customised to meet the individual needs of caregivers.
The Discrepancy Between Needs and Care Policies
Expecting family caregivers to lift their burdens without buckling under to become the next in line for help is almost unrealistic. Accordingly, Martindale-Adams et al. (2016) suggested that the costs society incurs should cover the services family caregivers use for themselves as receiving support from society appears to be crucial for their well-being. The unclear mixture of societal and family obligations is a well-known topic in many areas, where society, together with the family, is supposed to take care of family members in need of support. Our review shows that the two perspectives mix in modern society, with society gradually taking over some traditional family obligations, only to draw back again in some cases, leaving more responsibilities to the family.
The principles of
Family caregivers likewise try to meet
Conclusion
Becoming a family caregiver to a person living with dementia involves entering unknown territory. The family caregiver faces a range of new tasks and challenges as the dementia disease progresses. Taking a full-time responsibility to care for a person living with dementia is a burdensome task. Gradually, the family situation changes, often leaving the family caregiver more and more socially isolated, coupled with the sorrow of losing perhaps the person they are closest to in life. Managing this situation alone can be overwhelming. Having full-time responsibility for the person living with dementia often leaves caregivers with no energy to take care of their own needs, which has implications for their own health and well-being. The process of becoming a family caregiver to a person with dementia entails a range of needs. It spans from the need for social contact with people in a similar situation, for knowledge about the dementia disease and its consequences, to a need for support in daily life in terms of care activities and in receiving help to provide some respite for caregivers to allow them to pursue self-care. Since social norms and political policies are often embedded with the expectation that the family is the primary caregiver to people living with dementia, society must also support family caregivers in successfully executing that care.
Implications for Practice
The revealed problems in modern societýs unclear mixing of
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research including publication of this article: This work was supported by Interreg Germany-Denmark with funds from The European Regional Development Fund.
