Abstract
By 2020, more than 25% of the population in Florida will be more than the age of 65 years, and the population more than the age of 85 years is expected to increase by 40%. Among people more than 65 years today, 69% are expected to need some form of long-term care as they age. It is anticipated that Florida’s 680 licensed nursing homes will have challenges keeping pace with the needs. This article presents findings from an exploratory descriptive study designed to examine the leadership challenges and opportunities in nursing home settings today from the perspective of long-term care nurse leaders in the State of Florida. The target population for the study was directors of nursing in the 680 state licensed nursing homes in Florida. The final sample included 183 completed surveys from directors of nursing in 27% of the nursing homes that were surveyed. An exploratory descriptive survey design was used in this research. An online survey with 40 closed-ended questions and 2 open-ended questions was designed by the authors with input from an expert panel of long-term care nurse leaders who served in an advisory capacity. While less than 50% of the directors of nursing in this study were prepared at the baccalaureate level or higher, these leaders have complex roles and shoulder significant responsibilities. They have seen their roles expand into the management of more medically complex patients as their organizations try to adapt to a changing health-care reimbursement environment. Succession planning is a key concern for these aging leaders but only 40% of facilities had succession plans in place. The highest ranked leadership challenges involved issues with recruiting and retaining staff with the right skill sets. A poor image of long-term care nursing has contributed to recruitment and retention challenges.
Keywords
Introduction
The United States’ Institute of Medicine (IOM, 2010) reports on the Future of Nursing; Leading Change, Advancing Health noted that strong leadership at every organizational level and in every setting is critical if the vision of a transformed health-care system is to realized. This IOM recommendation that nurses develop strong leadership skills is of key importance in long-term care settings. Over the past decade, the services needed by patients in traditional skilled nursing and assisted living facilities in the United States have become medically complex and specialized. Few studies have focused specifically on long-term care nursing leadership but leaders in this area suggest that there are nuances that make leadership in these settings more challenging. Long-term care environments in the United States are highly regulatory driven, have a predominantly nonprofessional workforce, fewer financial resources, and a higher workforce turnover.
The issues and challenges of leadership in long-term care are especially important in the State of Florida. The Florida Healthcare Association (2016) reports that Florida has the fastest aging population in the country. By 2020, more than 25% of the population will be more than the age of 65 years, and the population more than the age of 85 years is expected to increase by 40%. Among people more than 65 years today, 69% are expected to need some form of long-term care as they age. It is anticipated that Florida’s 680 licensed nursing homes will have challenges keeping pace with the needs. This article presents findings from an exploratory descriptive study designed to examine the leadership challenges and opportunities in nursing home settings today from the perspective of long-term care nurse leaders in the State of Florida.
Background
Directors of Nursing (DONs) are thought to play a pivotal role influencing nursing home quality and costs yet there has been little research to examine the extent of their influence (Siegel & Sikma, 2015; Siegel, Young, Leo, & Santillan, 2012; Wunderlich & Kohler, 2001). In addition, the devaluing of the competencies and educational preparation for the DON role has “compromised the capacity of this workforce to promote and sustain high-quality, cost-effective nursing home care” (Siegel, Mueller, Anderson, & Dellefield, 2010, pp. 110–111).
Historically, the U.S. health-care system has focused on delivering acute care and addressing time-limited and specific illnesses and injuries as they occur in episodes. Such a system has not addressed the increasingly complex and long-term needs of people with chronic conditions (IOM, 2008). There has been little recognition of long-term care as an integral part of the continuum of care. This dynamic is shifting with the movement of the Centers for Medicare and Medicaid (2016) to a value-based reimbursement system and new initiatives reimbursing episodes of care across 90 days impacting both acute care and long-term care providers. Today, the spectrum of care has been expanded to include long-term and postacute care services, which includes long-term care nursing facilities, rehabilitation facilities, assisted living facilities, home care, and hospice (Golden & Shier, 2012–2013). Long-term care facilities (LTCFs) today “are a complex health care setting that are a mix of hospital, rehabilitation facility, hospice, and dementia-specific units” (Touhy, 2016). “The degrees of separation between the hospital and nursing home are being compressed” leading to an increased need for expertise in the nurse leader role (Harden & Burger, 2015, p. 17).
Job demands in long-term care settings have increased substantially in scope and complexity as a result of reforms in the health-care system. Changes in public policy, regulatory requirements, payment structures, increases in subacute and other specialty services, residents with more complex needs and higher levels of acuity, and the culture change movement pose new challenges and require new knowledge and skills (Siegel et al., 2012; Siegel, Young, Zysberg, & Santillan, 2015). The development of leaders has not kept pace with role expectations. The current state of professional nursing practice in long-term care facilities and the need to develop nursing leadership capacity is a global concern being addressed by the International Consortium on Professional Nursing Practice in Long-Term Care Homes (McGilton et al., 2016).
Preparation for a DON role is not part of basic nursing education. With the exception of large nursing home chains, little formal preparation emphasizing skills necessary to lead in today’s complex environment is available beyond on-the-job training. Registered nurses (RNs) are often hired for DON positions without the requisite educational preparation and experience in management and administration needed to meet the demands of this job (Rao & Evans, 2015; Vogelsmeier, Farrah, Roam, & Ott, 2010; Young & Siegel, 2016). There is limited recognition and undervaluing of the competencies needed to effectively enact the DON position among health professionals, educators, policy makers, and the long-term care system (Siegel & Sikma, 2015).
DONs struggle to create environments supportive of staff and residents with limited resources and support or recognition of the importance of their role. DONs often have 7 day a week responsibility with little release time, may function as the only RN in the facility, and assume multiple roles such as staff educator and infection control and quality improvement director (Siegel et al., 2010). The majority of their time is spent on regulatory issues, staffing or scheduling, attending to conflicts, overseeing nursing care, and managing costs. One third of their time is devoted to addressing resident and family concerns. Emphasis is on daily management functions rather than leadership and providing strategic direction for nursing within the organization (Rao & Evans, 2015; Siegel et al., 2010).
Despite these challenges, studies of DONs highlight their critical role in obtaining needed resources for nursing services, managing human resources, and problem solving within exiting resource conditions. This reflects the growing body of research on the positive effect of management resources on quality of care. The leadership skills of the DON and how they develop these skills are an important area for further research (Siegel & Sikma, 2015; Siegel et al., 2015). The study reported in this article was conducted with the recognition that eliciting the views of these LTC leaders in Florida would provide insight into strategies to address their concerns and provide support to them in this important role. Further, their reasons for choosing to assume DON roles and work in LTC need to be heard to identify the attitudes, skills, and experiences that promote interest in care of older people. Findings should help policy makers, nursing homes, and educational institutions, and the profession of nursing, meet the challenges of providing nursing expertise and leadership to the growing numbers of older adults.
Study Design and Methods
An exploratory descriptive survey design was used in this research. The aim of the study was to examine the challenges, opportunities and leadership development needs of long-term care nurses, and leaders from the perspective of DON in Florida’s licensed nursing homes. An online survey with 40 closed-ended questions and 2 open-ended questions was designed by the authors with input from an expert panel of long-term care nurse leaders who served in an advisory capacity. Approval for the study was given by the investigational review board at Florida Atlantic University. The study was conducted in the fall of 2014.
Study Sample
The target population for the study was DON in the 680 state licensed nursing homes in Florida. An introductory e-mail with an online link to the study was sent to the director of nursing at all 680 facilities in the state with assistance from the Florida Association of Directors of Nursing and the Florida Healthcare Association who also put a link to the survey on their websites. The final sample included 183 completed surveys from DONs in 27% of the nursing homes that were surveyed.
Director of Nursing (DON) Demographics Sample Size (n = 183).

Data Collection and Analysis
The survey was conducted electronically through Survey Gizmo online survey software. Demographic information was collected both about the leaders and their facilities including gender, age, ethnicity, nursing education, certification, role title, length of time in a leadership role, facility size, and ownership. To gain insight into their leadership challenges and opportunities, participants were asked questions about the following:
Areas of leadership responsibility. Leadership competencies needed in long-term care today and in the future. Their top leadership challenges. Strategies to make long-term care more attractive to future nurse leaders.
Frequencies were tabulated on the closed-ended questions. A content analysis was done by the co-authors on the written responses to two open-ended questions.
Findings
Leadership Responsibilities
While less than 50% of the DONs in this study were prepared at the baccalaureate level or higher in nursing, these leaders have complex roles and shoulder significant responsibilities. They not only have a large number of direct reports but also assume other support roles in their organizations with infection control (68%), quality management (79.2%), staff education (64%), and risk management (57.3%) being the four most common. Unlike their peer leaders in acute care environments, they lack the resources to have dedicated staff to assist with these key responsibilities which are very challenging in this heavily regulated environment.
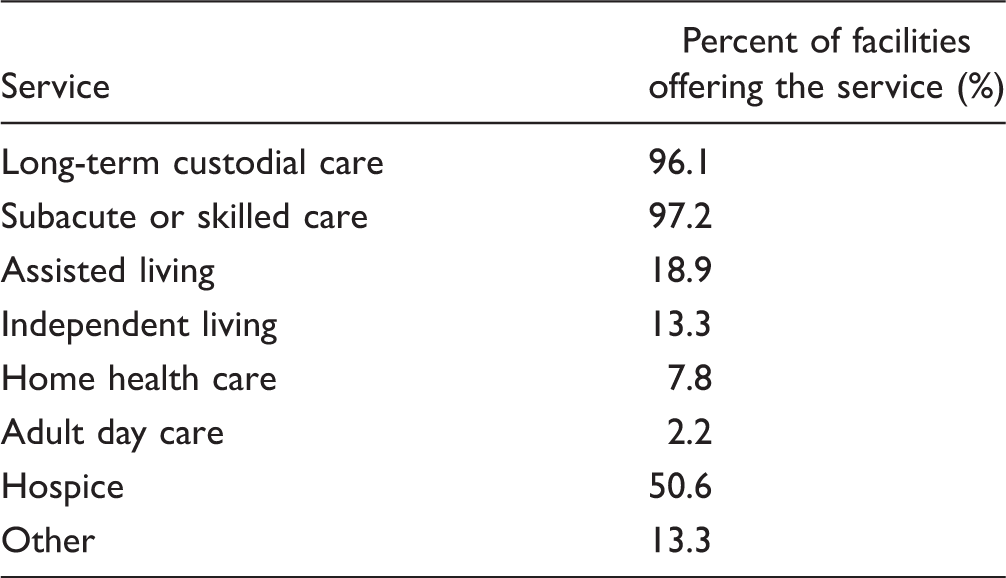
Services Provided by the Nursing Home.
Leadership Competencies Needed in Long-Term Care
In this study, a significant number of DONs (41%) anticipated that they would be retiring within 10 years. Succession planning is a key concern but only 40% of facilities had succession plans in place. From their perspective, three key leadership competencies needed today for the role (Figure 1) include the ability to coach and mentor staff (82.4%), knowledge about quality management (73.9%), and customer service skills (73.3%).
Key Leadership Challenges in Long-Term Care as Identified by Participants.
Moving into the future, the DONs reported that leaders will need stronger nursing knowledge and clinical skills to manage both a diverse patient population and the increasing complexity of illness in their residents. With health reform, funding for long-term care services will continue to be challenging. Future DONs will also need to have stronger competency in both budget and finance and health policy advocacy in order to plan strategically to manage change. Nursing homes have been slow to adopt technology including electronic health records but this will be critical in the future to establish partnerships with acute care facilities that have already made these investments to improve communication and care. But some things will not change. One DON noted that “compassion, communication and the ability to multitask will remain endearing qualities for nurse leaders in long-term care.”
Leadership Challenges
Question – What are the key leadership skills needed in long-term care today for nurses in senior leadership roles. Check all that apply.

At the time of survey, more than half of the DONs reported having recruitment (62.5%) and retention (43.8%) challenges with RN staff. Most (81.8%) were hiring new graduates to fill staff vacancies. RNs and LPNs in long-term care supervise care given by certified nursing assistants. The DONs are reliant on these professionals to do the frontline care management in environments where the acuity of care is increasing. Yet less than half (45.1%) have a dedicated educator to work with staff in key leadership areas such as critical thinking, supervision, delegation, communication, and conflict management.
Improving the Image of Long-Term Care
DONs surveyed were concerned about the image of long-term care and the impact of that image on the recruitment of both nursing staff and future long-term care leaders. One DON noted, “we need to change the image of long-term care as a place where nurses who cannot make it anywhere else go to work. Long-term care is a specialty and requires as much skill as hospital based nursing.” Their suggestions for improvement ranged from better compensation and benefits to reducing the level of regulatory compliance. There are more limited career paths at present in long-term care and significantly less professional education. Some of the stigma, they suggested, comes from other nurse leaders in both acute care and academia. A DON commented, “long-term care should be marketed as a bright future career for young nurses and an area that requires excellent technical and critical thinking skills, and is more autonomous than other areas of nursing.”
Discussion
Study Limitations
These study findings were generated from research conducted with a purposive example of DON working in licensed nursing homes in the State of Florida. Although the sample size is robust, their perspectives about their role and challenges may not be generalizable to the larger population of DONs outside this geographic area.
Implications
The research findings from this study were presented at a 2015 state conference sponsored by the Florida Association Directors of Nursing. There were no surprises in the data from the perspective of seasoned DONs, some of whom participated in the study. Many observed that it has been difficult to get these issues heard by the greater nursing community. The reported challenges faced by long-term care nurse leaders in this study are similar to conclusions drawn by other nurse researchers in long-term care (Rao & Evans, 2015; Siegel et al., 2010; Trinkoff et al., 2013). Historically, licensed nursing homes provided custodial care but this is quickly changing. Today, older adults are entering nursing homes with increasing acute health conditions. Estimates are that 37% of all acute care hospitalizations require postacute care services (Toles et al., 2013). These changes require different competencies for both staff and senior leaders in long-term care. The lack of succession planning in long-term care reported by leaders in this study echoes recent findings conducted with a broader audience of nurse leaders in Florida (Denker, Sherman, Hutton-Woodland, Brunell, & Medina, 2015).
Data from a 2015 employer survey in Florida indicate that the projection of job growth for both RNs and LPNs in the state exceeds the current supply (Florida Center for Nursing, 2016). These workforce shortages will impact all health-care settings, and nursing homes may be hard hit because they are not currently employers of choice. This could come at a pivotal time for the State of Florida which is aging faster than the rest of the country. We now find ourselves at the convergence of a perfect storm in health care. Three million baby boomers will turn 65 each year for the next 20 years (American Hospital Association, 2014). Their growing needs for long-term care services will place huge demands on an already challenged health delivery system.
Improving the image of long-term care and nursing in this setting is an important challenge in recruitment as well as quality of care. LTC nurse leaders and professional organizations should become more active in educating the public and other professionals about the nature of LTC nursing and the skills and knowledge required, as well as the relationship between resident outcomes and professional nursing presence. This is particularly important considering the increasing acuity of patients in subacute facilities.
Many facilities have limited financial resources for staff education, and the DON or Assistant DON are often expected to provide education and staff development as part of their role. Developing the critical thinking skills of staff not only improves outcomes but also enhances the image of nursing in the setting. Facilities must value and support high-quality staff development programs and develop innovative educational opportunities. Certification of the DON in gerontological nursing is one of the most important factors in reducing adverse resident outcomes (Trinkoff et al., 2014). The American Healthcare Association provides resources on their website including an on-line certification preparation program. RNs should be supported to attain certification and be rewarded for demonstrating enhanced competence.
Collaboration with schools of nursing and acute care facilities can also provide additional resources for staff education. The design of clinical experiences is of particular importance. The goal is to enhance student understanding of the setting and the care needs of older people and counteract negative stereotypes and negative images prevalent among society and health-care professional. Most nursing education program today use long-term care settings in the first semester with an emphasis on care related to activities of daily living. The acuity of patients in long-term care settings has changed. Many residents are complex with multiple co-morbidities that require critical thinking, care plan development, and team leadership. Senior level students could benefit from these experiences and it would change their perspective about long-term care and foster enthusiasm for exciting new roles in care of older adults (Touhy, 2016).
Today’s health-care environment is fast paced and constantly changing. The importance of planning for the future may be overlooked due to competing short- and long-term goals which seem to have more immediate impact. Nurse leader consistency is essential to organizations to drive high-quality care and maintain a healthy practice environment especially in long-term care environments where they play such a key role. Recruiting capable nurse leaders into long-term care environments will be challenging without addressing the span of their role responsibilities and absence of support services. Little has happened to improve long-term workforce planning since the 2008 IOM report on Retooling for an Aging America (Dawson & Langston, 2016). Harden and Burger (2015) discussed the potential policy impact of a failure to address the work environment, lack of professional staff, and absence of educational resources available in nursing home environments. They warn that without pivotal action by RNs, consumers, the public, the private sector, and the government, the future of long-term care may worsen. There is no time to waste in designing and funding innovative programs aimed at recruiting and developing both leaders and nurses for long-term care settings.
Conclusion
The development of strong, vibrant, knowledgeable long-term care nursing workforce in Florida is critical to the provision of quality health care of an aging population throughout the state. Yet, many leadership challenges exist in long-term care as an outcome of care becoming more complex coupled with workforce shortages. A whole generation of highly experienced nurse leaders is looking ahead to retirement yet wonder who the next nurse leaders will be given the absence of widespread succession planning efforts in long-term care. The policy implications of inaction are substantive and could have broader ramifications on whether the long-term care workforce can keep pace with the growth of nursing care needs of older adults.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study is supported by Florida Blue Foundation.
