Abstract
Long COVID is a growing health concern with data continuing to emerge about the psychosocial consequences of this new chronic condition. We aimed to improve understanding of the experiences of patients with Long COVID, focusing on emotional impacts arising from experiences of loss and grief caused by persistent physical symptoms and changes in lifestyle and social support. Patients (n = 21) were recruited August to September 2022 from a post-COVID recovery clinic to participate in semistructured interviews. We found that Long COVID patients (1) reported experiencing loss across multiple domains including loss of physical health, mental health, social support and connections, roles in their families, and self-identities, and (2) described experiences of grief that mirrored the 5 stages of grief in the Kubler-Ross model: denial, anger, bargaining, depression, and for some, acceptance. Our findings highlight the importance of evaluating the experiences of loss and grief among Long COVID patients as well as support systems for this patient population. Providers may be encouraged to incorporate mental health and bereavement support resources to address critical needs of Long COVID patients.
Introduction
Long COVID has been estimated to impact at least 65 million individuals globally, with a complex and varied symptoms profile that includes fatigue, cognitive impairment, and postexertional malaise that extends beyond an acute COVID infection.1,2 Symptoms of mental health conditions, including feelings of anxiety and depression, have been commonly reported among Long COVID patients. 3 While there is increasing acknowledgment of the emotional challenges individuals face when experiencing Long COVID, less is known about potential stressors that contribute to declining mental health among this patient population.
One possible mental health stressor is the experience of grief, drawing similarities to individuals bereaving the loss of a loved one. These individuals have been shown to be at higher risk of experiencing mental health conditions such as anxiety and depression as they navigate their grief. 4 The experience of having Long COVID may similarly evoke feelings of bereavement, fueled by the loss of physical health and the implications of such loss on their personal lives. The goal of this study was to explore the perspectives of Long COVID patients to understand their experiences related to the emotional impact of Long COVID and its implications through the lenses of loss and grief. Expanding our understanding of how Long COVID impacts mental health can inform the development of treatment and support options that may improve emotional and social well-being in this patient population.
Methods
Our study included one-on-one interviews with patients from the Post-COVID Recovery Clinic within The Ohio State University Wexner Medical Center. Eligible patients were identified by clinic staff. Patients were eligible if they were at least 18 years of age, spoke English, and continued to experience decreased ability to function 3 months or more after COVID-19 infection, despite having functioned well in daily life prior to being infected with COVID-19. This study was approved by The Ohio State University Institutional Review Board, and all participants provided verbal informed consent.
Eligible patients were sent an email about the research opportunity, and those patients who were interested contacted the study team to set up an interview time. Five study team members completed interviews with eligible patients between August and September 2022 using a semistructured interview guide. The interview guide was designed to explore the perspectives of Long COVID patients and included questions about symptom burden, impacts of Long COVID on physical and mental health, and support or lack of support from friends and family. We conducted interviews until saturation was reached, as indicated by no new themes emerging in subsequent interviews. 5 Interviews were conducted by phone or videoconference and were audio recorded and transcribed verbatim. Participants were given a $25 Amazon gift card in appreciation for their participation.
Thematic analysis was used to analyze interview transcripts, and both deductive and inductive coding were used to identify trends in the data. 6 First, a preliminary coding dictionary of a priori codes was developed based on questions asked in the interview guide and was used by 4 members of the research team to jointly code one transcript to confirm agreement about the a priori codes and consider emergent codes. Revisions were made to the initial coding dictionary, and the remaining transcripts were divided among the 4 research team members for coding. Frequent meetings were held to ensure coding consistency across all transcripts. From this preliminary coding, we examined quotations categorized by the codes of Impact-Mental Health and Support Groups, Isolation, Loss, Stigma, Concern-Long COVID, and Expectations-Long COVID. Three team members reviewed this subset of the data and identified emergent subthemes around loss and grief that we found to align with the Kubler-Ross Model of Five Stages of Grief, a model which describes a process through which people experience grief in 5 stages: denial, anger, bargaining, depression, and acceptance. 7 ATLAS.ti software was used to support our analysis.
Results
Twenty-one Long COVID patients participated in this study. Patient demographics are presented in Table 1. Patients had a mean age of 47.6 years (range: 19-68). Interviews ranged from 26 to 84 min with an average length of 49.5 min. Across interviews, we identified subthemes related to loss and grief that patients associated with their experience with Long COVID (Table 2).
Demographics of Study Participants.

Summary of Themes and Subthemes.
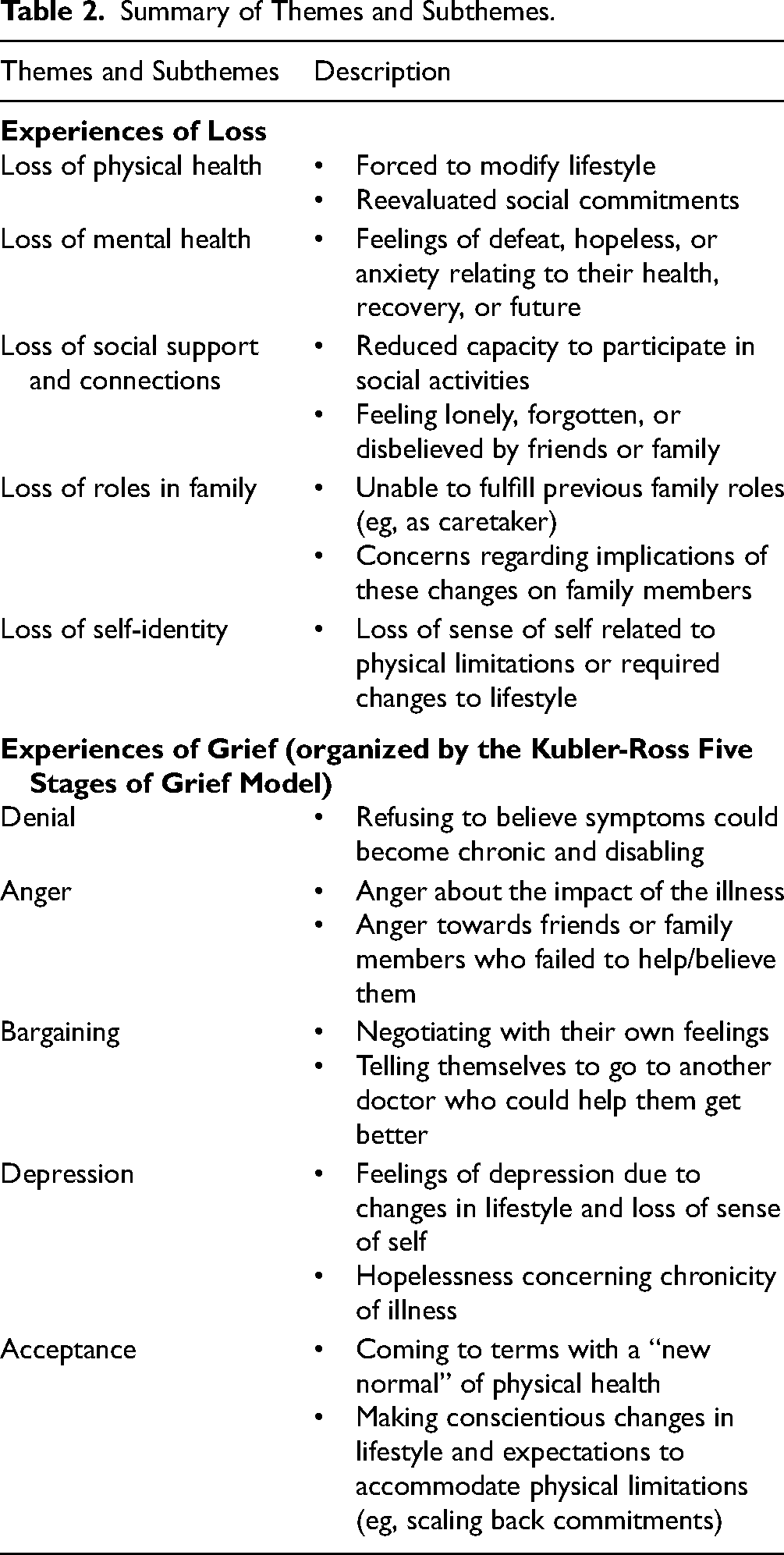
Experiences of Loss
We found that participants with Long COVID experienced profound feelings of loss that impacted multiple aspects of their lives, including losses of physical health, mental health, social support and connections, family roles, and self-identity. These aspects of loss are explained further below.
Loss of Physical Health
Participants extensively described the impact of the loss of their physical health, and these descriptions often entailed a comparison between one's physical abilities before and after the onset of Long COVID. As one participant described, “I'm also struggling with fatigue, inability to do much of anything in comparison to where I was a couple years back. Things that were easy for me to do has now been a real chore.” Participants also described how the loss of physical health introduced limitations in their life, causing changes in their way of living. One participant described their experience as, “I keep trying to go back to living my old way, like, oh yeah, I had eight hours of sleep, I should feel great today. And then I'll, like, charge through the day, and then I crash. I just can't go with that pace. I can’t put that many things on my schedule. I just have to put a lot of limits on my life.”
Loss of Mental Health
Participants also noted a loss in their mental health. These experiences spanned feelings of anxiety, uncertainty, isolation, loneliness, and hopelessness. One participant described the unexpected impact that isolation had on their mental health: “The isolation was brutal. So, that didn't do good things for my mental health. … The mental health impacts, they were very surprising to me. Like, I had no idea that it was going to affect me in that way.” Another participant described the impact of Long COVID on their mental health in the context of feeling overwhelmed and hopeless: “I guess it's a depression and the hopelessness, just, I'll, I start crying and it's a lot. And it's like, it's just feels like it's just too much sometimes.”
Loss of Social Support and Connections
The experience of loss was also revealed in the descriptions of loss of social support and connection through affected relationships with family and friends. Participants described this loss of connection as stemming from a reduced capacity to interact with others, for example, due to physical limitations such as fatigue. One participant shared, “I have withdrawn from society … I don't go out and don't go places … I don't do the things that I used to do with friends.” Participants also often described loss of connection as feeling “forgotten” or “left behind” when support from their friends and family members declined over time. For example, one participant reflected, “My brother, my sister, my parents, no one even asks anymore how I am.” Some patients also described fractured connections with friends or family who did not believe their symptoms or dismissed their illness. One participant shared, “She [my mom] basically refused to believe I’m sick at all and has the same expectations of me as she did prior to me getting sick. And it's just really hard to have somebody just completely deny that you are sick when you feel it every single day.”
Loss of Family Roles
Some participants also described a loss of former roles, particularly within their families. One participant explained the impact of Long COVID on their perceived role as a grandmother: “I sleep a lot, or I'm in bed, or not as much fun. And not as active. And so that's hard on them because I really was like, I was like the really cool grandma.” Another participant recognized the perceived changes in their role as a mother and how this also impacted the members of her family: “They kind of lost the mom that they were used to. A mom that was active and was always involved and doing things. And we're all learning to try to accept where I'm at.”
Loss of Self-identity
Finally, participants described the loss of self-identity during their experience with Long COVID. For example, one participant shared, “I don't see an end in sight. … I'm kind of out of hope for that, and I'm looking around with the way that I live now, which is, I’m a shell of the person that I used to be.” For another participant, this loss of self-identity was coupled with the challenge of accepting the need to now identify as someone who was not feeling well and needed help: “I feel I struggle with not being well, and I don't want to be a burden. I want my old life back. … It was so hard for me to ask for that (accessible parking placard) because part of that was admitting that I was sick enough that I needed it.”
Experiences of Grief
Participants often described the emotional impact of Long COVID by using language related to grief. For instance, one participant explained, “And I think over time, as I learned to deal with certain things a little bit better, I kind of grieved. I had a process of grieving my life.” Framing these comments using Kubler-Ross's model, 6 we characterized participants’ explanations of different aspects of grief by mapping their comments to the 5 stages of grief: denial, anger, bargaining, depression, and acceptance. We describe Long COVID patients’ experiences of grief within this framework in further detail below.
Denial
Notably, some participants described experiencing denial. For instance, several interviewees described denying that their Long COVID symptoms would persist. One participant reflected, “It may be for the first six months, even for the first nine months, I had some hope, you know, thinking, well, it's got to get better any day now.” Another explained how they were unable to believe that Long COVID would not go away: “It [Long COVID] was impacting so many areas of my life. And I was just wondering, like, is this going to be my new normal forever?”
Anger
Concerning anger, participants described anger about both the disease itself and the implications on their lives. One participant commented, “Things are not right with our bodies that there's no good reason for. And, like, it's not just an inconvenience. It's literally destroying people's lives.” Several participants reported experiencing anger due to the impact of Long COVID on their relationships with friends and family members. One noted, “I feel like that a lot of my friends really look down on me, they think I'm just lazy. … I try to explain to them, some of them. But some of them, I don't care enough about. Bye. Don’t let the door hit you in the ass on the way out. I don't need you.”
Bargaining
With respect to bargaining, some participants reported feeling that if they could persist through this difficult time, there might be a breakthrough. For example, one stated, “Again, no one gave a timeline, and no one knows. But I kept thinking I'm going to be better in a week. … And we were all hoping. And then we put all our eggs in the basket. As soon as a pulmonologist is on board, I’ll get better. As soon as the Long COVID doctor, I'll get better.” Another participant explained bargaining about their own expectations: “I can't expect to go back to my old lifestyle. And now that I've basically let go of my professional goals, and I've let go of my financial goals, and I've let go of trying to be the person I used to be, I don't have the level of chest pain that I used to have.”
Depression
Depression was commonly referenced by the patients we interviewed. One participant described experiencing depression related to their loss of physical health: “I just wish that people understood how incredibly heartbreaking it is to just be sick all the time, even if it's just feeling tired every day. It's just your quality of life is completely different.” Another participant reported depression related to the impact of Long COVID on their lifestyle: “I have been extremely depressed. It's really hard to have to completely change your lifestyle because you don't feel well all the time. I had a lot of hobbies. I used to go do things with friends. And I couldn't do anything.” A third participant shared their feelings of depression surrounding losing their self-identity: “It's just been very depressing, feeling like you’re never going to get better or be back to yourself.”
Acceptance
Finally, while less common, several participants’ comments suggested that they had reached a form of acceptance about their condition. For instance, one participant noted, “I feel better now. I think I'm doing better with the whole trauma thing. Like, I'm less fearful now. So, I'm a little bit more resigned to, okay, I got the vaccines, I mask when I'm out in the world. That's just what I do.” Another reflected on acceptance of their new life: “I mean it has been an emotional journey for me. The initial anxiety, sadness about saying goodbye to the life that I had before, and then accepting the fact that I have a life that looks very different, and then trying to think about how I'm going to move forward with this life.”
Discussion
Our interviews revealed shared experiences around the emotional impacts of Long COVID including feelings of loss and grief. Participants described experiences of physical and psychosocial loss, including changes in mental health, social support and connections, their roles in their families, and their self-identities. These findings extend prior work considering the general mental health implications of Long COVID.8–10 Many of the patients in our study detailed feelings of depression and anxiety when describing their experiences of loss and coping with grief. Symptoms of depression and anxiety are frequently reported by patients in this population, where the etiology of these symptoms could be related to the changes in physical functioning impacting quality of life or from the physiological impact of the disease itself.11–14
While similar experiences of loss and changes in social support for patients with Long COVID have been described in other studies,8–10 our study is the first to examine these experiences using the Kubler-Ross Five Stages of Grief model. 7 It is important to note that the stages of grief in this model are not necessarily linear, nor experienced in the same way by all people.15,16 Some stages may take longer for some individuals, while healing itself may occur on a continuum with some days being harder on patients’ bodies and minds than others. Furthermore, for patients whose comments suggested acceptance of Long COVID, this does not imply that their grief journey had ended. This model has been previously applied to the perspectives and experiences of patients with disabilities and other invisible illnesses, 15 and our results suggest that Long COVID patients, as survivors of this new illness, share similar challenges with loss and grief.
Examining Long COVID patients’ experiences through the same lens as patients with other invisible chronic illnesses may provide opportunities to consider symptom management approaches that can support this patient population. For example, health care providers could consider recommendations for self-care management, bereavement support, and palliative care,17–20 which are being explored as avenues of support for patients with fibromyalgia. 21 Cognitive Behavioral Therapy has also been recommended to manage symptoms and negative mood for patients with fibromyalgia or chronic fatigue syndrome.22–24 Primary care providers are well-positioned to screen for these needs in Long COVID patients, as well as leverage existing support resources available to patients with similar experiences of loss and grief as a result of a chronic illness.21,25
While assessment and treatment of symptoms for anxiety and depression are becoming components of Long COVID symptom management,12,26 our study findings also suggest the need for advocacy for social programs, such as nonpharmacological treatment options and peer support groups for Long COVID patients.27,28 Health care providers might consider the needs of Long COVID patients with respect to their support systems as well as acute experiences of loss and grief through ongoing assessment as part of clinical care. Health care systems may also consider serving as hubs offering and encouraging peer support for the Long COVID patient population.
Limitations and Future Directions
Limitations of this study include our focus on patients recruited from a specialized Long COVID treatment clinic. As a result, we were unable to assess the perspectives of patients from the broader Long COVID community who may have had different experiences receiving support for their illness. Of note, our participant characteristics are similar when compared to studies of larger populations who are experiencing Long COVID.29–31 Second, as we recruited patients who were at various timepoints in their Long COVID journey, we recognize that different stages of their diagnosis and treatment plans may have impacted their perspectives about Long COVID. Third, we did not explicitly ask about participants’ mental health prior to their Long COVID experience. We recognize that individuals with preexisting conditions, including anxiety and depression, have been shown to have a higher likelihood of experiencing Long COVID. 32 Finally, as our study elicited perspectives from patients at only one point in time, exploring longitudinal perspectives would help inform our understanding about how these perspectives might change over the course of patients’ experiences with Long COVID.
Conclusions
This study assessed Long COVID patients’ perspectives about their illness as they described experiences of loss across personal and professional domains, feelings of abandonment and disbelief from friends and family, and grief related to the emotional and functional impacts of this illness on their lives. Increased awareness about the acuity of these experiences of Long COVID patients may help improve efforts to support the millions of Long COVID patients as they struggle with their diagnosis, care, and the management of this new chronic disease.
Footnotes
Data Sharing Statement
Data will not be made publicly available due to concerns for participant privacy.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval to report this case was obtained from The Ohio State University Institutional Review Board, approval number 2020B0288.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: National Cancer Institute (U54CA260582).
Statement of Human and Animal Rights
All procedures in this study were conducted in accordance with The Ohio State University's (2020B0288) approved protocols.
Statement of Informed Consent
Verbal informed consent was obtained from the patients for their anonymized information to be published in this article.
