Abstract
Developing partnerships among patients and healthcare providers improves quality of virtual care. Successful patient engagement is influenced by digital literacy. Although adults (35–64) with chronic health challenges may be motivated to use virtual services, they may not have the required skills or orientation to effectively participate on their virtual team. This scoping review aimed to identify resources available to enable adults with chronic health challenges to participate as partners on their virtual teams. Peer-reviewed and grey literature data from 2011 to 2022 were searched. A total of 432 peer-reviewed and 357 grey literature sources were retrieved and screened, and 14 and 84 sources, respectively, met the inclusion criteria. Relevant information from the sources was extracted and analyzed in duplicate and synthesized qualitatively. Key findings include (1) virtual workflow processes/frameworks, (2) ‘webside manner’ guidelines which emphasize “the how” as opposed to “the what” of facilitating team interactions, and (3) virtual patient support personnel. Overall, analyses suggest there are persisting gaps to be addressed in synchronous virtual care resources for adults with chronic health challenges.
Introduction
In Canada, virtual healthcare visits increased from 4% to 60% at the onset of the COVID-19 pandemic. 1 Although virtual care has existed for decades, the pandemic resulted in a dramatic and rapid shift in service delivery. Given the increasing demand for both timely, cost-effective, and quality care, patient satisfaction with virtual care, and government investment in virtual infrastructure, virtual care has become a standardized form of service delivery. 1
A widely adopted definition of virtual care is “any interaction between patients and/or members of their circle of care, occurring remotely, using any forms of communication or information technologies, with the aim of facilitating or maximizing the quality and effectiveness of patient care”. 2 (p609) Virtual care can be characterized as asynchronous, synchronous, or hybrid; healthcare teams may adopt any of these approaches. 2 Many terms are used interchangeably across the literature, such as digital health, telehealth, and telemedicine, obfuscating the unique aspects of each. These terms will likely continue to evolve as the virtual care landscape advances.
Healthcare providers (HCPs) within interprofessional care teams have reported that the transition to virtual care has shifted the nature of interprofessional collaboration as it resulted in HCP role changes, restructuring of team dynamics, the development of new professional responsibilities, and decreased wait times for patients to access team members.3,4 Virtual care seems to have strengthened interprofessional team collaboration and patient partnerships.3,4
The patient role has evolved to one requiring greater preparation for virtual visits. 5 Developing mutually beneficial partnerships among patients and their healthcare team is critical to facilitate optimal engagement and improve quality of care.6-8 Variable patient engagement patterns in virtual care are largely based on digital literacy, which has meant some individuals are disadvantaged from optimal participation. 5 Digital literacy refers to an individual's ability to find, understand, appraise health information and utilize technology to address a health concern. 9 Health literacy is defined as the ability to obtain, read, understand, and use healthcare information to make appropriate/informed health decisions. 10 Even though digital literacy and health literacy are related to digital health literacy, the relationship is bidirectional and complex. 11 Older populations typically have a lower degree of digital literacy than younger populations. Pre-pandemic, it was reported that younger populations were most open to virtual care, adults were willing to use it whereas older adults were least interested. 12 Therefore, adult patients (35-64) with chronic health challenges are the focus of this research as this demographic is motivated to use virtual services to manage their health, but may not have had the opportunity to do so until the start of the COVID-19 pandemic.
Adults (35-64) with chronic health challenges must rely on the healthcare system twice as frequently as those without chronic conditions. 13 Chronic health is defined as conditions that persist for one year or more, require ongoing medical attention, and limit activities of daily living. 14 Common chronic conditions experienced by adults include hypertension, osteoarthritis, mood or anxiety disorders, osteoporosis, diabetes, asthma, chronic obstructive pulmonary disease, ischemic heart disease, cancer, and dementia. 15 Chronic health conditions are managed optimally when interprofessional teams work collaboratively and include the patient in shared decision-making. 16 Although adults with chronic health challenges are adopting virtual care to manage their health, there is concern that they are not prepared to participate effectively on their virtual care team. 17
The literature about virtual care primarily focuses on system and team delivery, emphasizing HCPs’ capacity to drive team-based care.2,18,19 Therefore, an enhanced understanding of the resources available to promote equitable engagement of patients on virtual teams is required to improve quality of care. The Stanford Virtual Health Patient Engagement Model is a recent attempt to consider the interaction among clinical teams, system and technology support and customized patient care. 5 Yet, more work is needed to understand what is required for adult patients with chronic health challenges to optimize participation as a partner of their care team. Therefore, this scoping review aimed to address the following research question: What resources are available that enable adults with chronic health challenges to participate as partners on their virtual team?
Methodology
Scoping reviews are particularly relevant within fields of research that have emerging levels of evidence, such as new evidence on virtual care using evolving technologies and health system changes. 20 A scoping review that maps available knowledge regarding resources to enable patients as partners of their interprofessional care team are timely. This scoping review followed the Joanna Briggs Institute methodology as it is an evidence-based and comprehensive guide. 21 Reporting follows the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) Extension for Scoping Reviews (ScR). 22 PRISMA-ScR is a checklist/guideline to ensure the research being conducted is evidence-based. 22
Eligibility Criteria
Synchronous virtual visits attempt to closely mirror in-person interactions and foster authentic partnerships between patients and their interprofessional care team more than asynchronous or hybrid approaches. Thus, the search was constructed to ensure that the term ‘virtual care’ referred to HCP(s)-patient interactions (see Appendix A for search terms used). This study defines virtual care as synchronous interactions that occurred via phone, video, and/or live chat.
To be included, the peer-reviewed and grey literature sources needed to be published between 2011 and 2022. There has been noticeable progress towards virtual care during this timeframe with the significant advancement to virtual health platforms occurring most recently. The sources needed to be published in English given the feasibility, cost, and time restrictions related to translation demands and relevance to a North American context. Lastly, sources were only considered if there was unrestricted access to the full text.
Search
The search strategy aimed to locate both peer-reviewed and grey literature via independent searches. Crafting the search was an iterative process and additional keywords/search terms were incorporated into the final search algorithms. As the reviewers gained increasing familiarity with the existing literature, modifications were made to refine the search, eligibility criteria and definitions. Additional modifications were made once the reviewers consulted with two university research librarians, a telemedicine adoption specialist and completed a pilot search.
A piloted search of the Medical Literature Analysis and Retrieval System Online (MEDLINE) database (Appendix A) was conducted. The text words in the titles/abstracts of relevant articles and the index terms that described the articles were used to develop comprehensive search strategies for each database. This scoping review was conducted from November 2021 to June 2022. Specifically, the peer-reviewed literature search was conducted on November 21, 2021. A hand-search of relevant peer-reviewed journal repositories was conducted in January 2022. The peer-reviewed data considered was not limited to any geographical region. The grey literature search was conducted on June 10, 2022, and was restricted to North America due to feasibility. The peer-reviewed search strategy was modified for the grey literature Google Engine search and was developed in consultation with a university research librarian (Appendix B). Overall, the peer-reviewed search retrieved 432 sources and the grey literature search retrieved 357 sources before in-depth screening was performed in correspondence with the inclusion criteria.
Information Sources
Peer-reviewed data were collected from MEDLINE, Cumulated Index to Nursing and Allied Health Literature (CINAHL), Public/Publisher MEDLINE (PubMed) and Psychological Information Database (PsychInfo). Subsequently, a hand search of the Patient Experience Journal and the Journal of Patient Experience was also conducted. Grey literature was derived from performing a Google search and a hand-search of the top 10 Canadian hospital websites and Canadian Government Ministry of Health websites. The top 10 Canadian hospitals included: Toronto General, Sunnybrook Health Sciences Centre, Mount Sinai, North York General, Jewish General (Montreal), Centre Hospitalier de l’Université de Montréal, Vancouver General, Montreal General - McGill University Health Centre, St. Michael's, and Rockyview General. 23 This ranking was developed by Statistia Inc. based on recommendations from medical professionals, patient surveys, and medical performance indicators. 23 All other Canadian hospitals were excluded from the present scoping review for the purpose of adhering to this ranking, although they may implement virtual care. The Google sources were selected by scanning the results of the first 5-pages of each search (Appendix B).
Selection of Sources of Evidence
All empirical studies and grey literature documents that met inclusion criteria were included in this screening. Sources identified in the peer-reviewed literature search were screened using Covidence Software and duplicates were automatically removed. The grey literature was not compatible with Covidence; therefore, all data were screened manually. The Google search was completed by 1 reviewer (ST) for consistency as Google algorithms differ by the account holder. Likewise, the hand-searches of the Canadian hospitals and Ministry of Health websites were completed by 1 reviewer (VC). A pilot test was conducted by the reviewers prior to embarking on the source selection process for both the peer-reviewed and grey literature data. For the peer-reviewed data, a random sample of 20 titles/abstracts was selected and screened by two reviewers (VC and ST). The reviewers met to discuss and resolve discrepancies as needed.
Following the pilot screen, all peer-reviewed titles/abstracts were screened by two reviewers (VC and ST). Next, relevant sources were retrieved for full-text review, which was conducted in duplicate. Reasons for exclusion included lack of HCP(s)-patient interaction (46), lack of synchronous virtual care (21), and incorrect patient population or year (14). Evidently, the primary reason for exclusion related to lack of HCP(s)-patient interaction as many studies focused on HCP-HCP interactions. Any disagreements between the reviewers were resolved through discussion and did not require a third reviewer for consensus. See Figure 1.

PRISMA flow diagram.
Data Charting Process
Two separate data extraction charts were jointly developed using Google Sheets by two reviewers (VC and ST) to determine which variables to extract for the peer-reviewed and grey literature data respectively. The peer-reviewed data extraction chart included the following headings: author, year of publication and specific details about the participants, concept, context, study methods, and pertinent findings. The reviewers (VC and ST) became familiar with the source results and trialed the extraction chart for two sources to ensure all relevant results were extracted. As for the grey literature data, the reviewers engaged in a similar process and piloted this data set. However, the headings utilized in the grey literature data extraction chart differed and included: date, organization name and website URL/search engine, search strategy(s) including how items were selected, number of items retrieved/search results and number of items screened and piloted in this data set. Only a portion of the peer-reviewed and grey literature data are included in the references due to the number of sources in the review.
Results
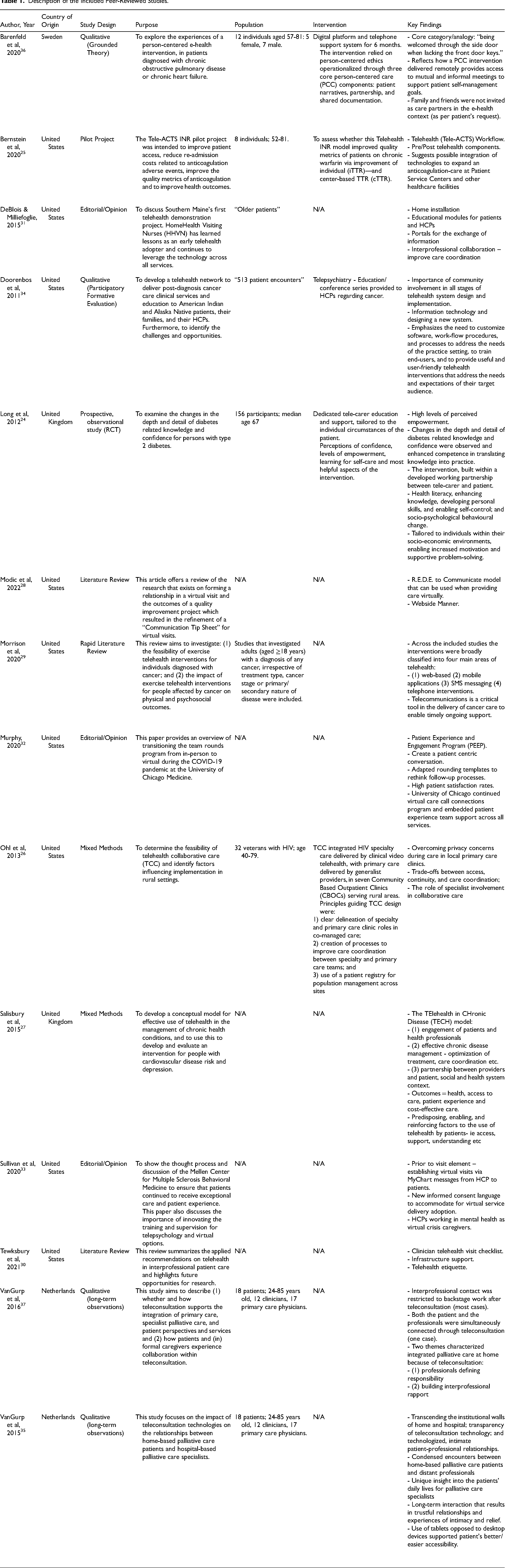
MEDLINE, CINHAL, PubMed, and PsychInfo database searches retrieved 432 peer-reviewed articles. After duplicates were removed and the reviewers applied the inclusion criteria to the titles/abstracts, 95 articles remained. Subsequently, these 95 articles underwent full-text screening and were discussed by two reviewers (VC and ST) until a consensus was achieved. These discussions predominantly revolved around the definition of virtual care to ensure the studies included in this scoping review interpreted virtual care as synchronous HCP(s)-patient interactions. A total of 14 articles met the scoping review criteria and were published in English between 2011-2022. The 14 studies consisted of the following research designs/methods: one quantitative (randomized control trial), 24 one pilot project, 25 two mixed methods,26,27 three literature reviews,28-30 three editorial/opinion papers,31-33 and four qualitative designs.34-37 Half of the studies were descriptive and did not include participants but described virtual care resources and practices. The other half of the studies were empirical and included participants. Moreover, half of the studies were published pre-pandemic (2011-2016) and half were published during the pandemic (2020-2022). These studies took place in the United States (9), United Kingdom (2), Netherlands (2) and Sweden (1). See Table 1.
Description of the Included Peer-Reviewed Studies.
The hand-search of the top 10 Canadian hospitals and Ministry of Health websites returned 21 sources and the Google search returned 336 sources for 357 grey literature data. After the screening was completed by each reviewer (VC and ST), 20 websites from the hand-search and 64 sources from the Google search met the inclusion criteria. The Centre Hospitalier de l’Université de Montréal website was excluded as it was published in French and all excluded sources from Google related to a lack of synchronous virtual care. In total, 84 grey literature sources were included in this study, ranging from Canadian government/hospital websites to private practice websites within North America. Other grey literature sources included links that consisted of surveys, virtual care checklists, virtual technology training resources (i.e., “how to” videos), virtual etiquette or ‘webside manner’ guidelines, and best practice standards. The majority of the grey literature sources were published during the pandemic (2019–2022).
Key Themes
The peer-reviewed and grey literature sources share the following 3 themes: (1) Virtual Workflow Processes/Frameworks, (2) Webside Manner Guidelines and (3) Virtual Patient Support Personnel. The reviewers utilized Braun and Clark's 6-phase framework for conducting a thematic analysis: (1) Become familiar with the data, (2) Generate initial codes, (3) Search for themes, (4) Review themes, (5) Define themes, (6) Write-up. 38 In brief, as the two reviewers (VC and ST) became familiar with the data they maintained individual logs of meaningful topics and patterns (codes) that were discovered throughout the screening process. Following data selection, the reviewers met to compare their generated codes and collaborated to construct descriptive themes. The themes were defined and refined throughout the data selection process. The 3 themes are interdependent despite not being explicit in each data source.
Theme 1: Virtual Workflow Processes/Frameworks
Proposed workflow processes/frameworks that promote an effective ‘webside manner’ were prevalent in both the peer-reviewed and grey literature. These workflow processes/frameworks aimed to mirror in-person healthcare visits (i.e., virtual waiting rooms) while addressing the need for increased preparation ahead of virtual appointments.
Theme 2: ‘Webside Manner’ Guidelines
‘Webside manner’ or virtual etiquette was the primary theme of this review. Literature included context-specific guidelines and general recommendations whereas others proposed the need for HCPs to adhere to standardized virtual care policies developed by each regulated health profession.
Theme 3: Virtual Patient Support Personnel
This theme aligns with the proposed workflow processes/frameworks as they often incorporated a pre-visit and post-visit component. These pre/post-visit interactions were often facilitated by virtual support personnel as opposed to the HCPs themselves. Not only do the sources in this review corroborate the need for direct patient support to prepare for synchronous virtual care appointments, but they also provided indirect patient support by sharing resources to promote continuity of care and digital literacy development.
Discussion
The goals of this scoping review were to explore the resources that enable adult patients with chronic health challenges to participate as partners on their virtual team and to reveal gaps for future research. Although the sources included in this review referenced chronic health challenges experienced by adults, it was noted that the findings are generalizable to any population. Only 14 peer-reviewed studies were included in this scoping review compared to 84 grey literature sources. Overall, the key recommendations and resources included adhering to virtual workflow processes/frameworks, implementing ‘webside manner’ guidelines, and providing virtual patient support personnel.
The number of sources retrieved suggests that there is a high demand for resources and communication about this topic that still needs to be captured in scientific databases. Arguably, grey literature is a more accessible form of knowledge translation for patients, especially those who lack digital literacy. Family members play an integral role within a patient's care team. 39 However, the specific role of family members was not addressed within this review. For example, participants in Barenfeld and colleagues’ study declined to have their family members involved in their virtual care. 36 Family involvement often varies based upon the level and type of support required by the individual with the chronic illness. 40 Family members of adults with severe chronic illness provide more formal health/caregiver support. 40
The seven studies published pre-pandemic emphasized the importance of access to technology, HCP/patient readiness to use technology, and their willingness to adopt virtual care. Post-pandemic studies focused on virtual care adoption strategies and standards; for example, standardizing how HCPs deliver virtual care and assisting patients in navigating virtual platforms. Doorenbos and colleagues were among the first to discuss the need to design workflow processes, educate technology users, and provide user-friendly virtual care interventions that address the needs of patients. 34 The need for virtual care workflow processes/frameworks was evident across the grey literature. However, only Bernstein and colleagues proposed a “preparatory phase” prior to engaging in the virtual interaction to enable patients to participate as partners in their care team (Figure 2). 25 This preparatory phase was facilitated by a virtual care coordinator to raise awareness about virtual care service delivery which was also discussed by Long and colleagues. 24 In addition to providing education to patients on how to use virtual care platforms, virtual etiquette and ‘webside manner’ was elaborated upon in two studies.28,30 ‘Webside manner’ is the virtual equivalent to bedside manner which is recognized as the ways that HCPs interact with patients. 9 Translating key elements of the conventional in-person visit to the virtual experience is a foundational step towards building the virtual care infrastructure. 5

Workflow processes emerged as an important concept for enabling patient engagement in virtual care. The use of virtual patient support personnel to assist patients with preparing for virtual sessions was evident, especially within community outreach programs. 41 There are many resources that promote digital literacy acquisition via virtual training for patients and HCPs. Many of the grey literature sources outlined virtual etiquette for patients and ‘webside manner’ for HCPs. As the virtual care literature continues to grow, a more expansive review of the peer-reviewed and grey literature could address the importance of synchronous virtual care resources, their effects on team-based care in chronic disease management, and health outcomes.
It is essential to prepare patients prior to their virtual visit to promote effective patient engagement and enable time for HCP(s)-patient rapport building. This relates to the Stanford Virtual Health Patient Engagement Model as the breakdown of this model included a workflow (Stanford Virtual Health Clinical Process) that mirrored in-person visits (i.e., virtual waiting room) while ensuring continuity of care was maintained. 5
Limitations and Recommendations
The terms related to ‘virtual care’ are not consistent in the literature. Thus, this search strategy may have identified sources that ascribe different meanings to this term. However, to ensure the search was comprehensive, a consistent definition of synchronous virtual care was developed. This study also defined “adult” as age 35–64 since the literature for adults age 65+ addressed unique later-life issues. Due to variable definitions of “adult” and a focus on chronic diseases, some sources included patients beyond 64 years. We do note, however, that we were unable to differentiate patient populations by health literacy or other sociodemographic factors. Although the scoping review includes sources from 2011 to 2022, the peer-reviewed database search only included studies published until November 2021. To compensate for this, the reviewers completed a hand-search and grey literature search that included sources published in 2022. The peer-reviewed data was not limited to any geographical location, but the grey literature was limited to North America due to feasibility. Likewise, all sources were restricted to English but if research was translated to English for publication it was included. Future research should include non-English literature to gain an understanding of the resources available to patients across geographical boundaries.
Conclusion
This scoping review aimed to address what resources enable adults with chronic health challenges to participate as partners on their virtual team. The results suggest that resources are beginning to proliferate within peer-reviewed and grey literature. This scoping review's findings align with the Stanford Virtual Health Patient Engagement Model which posits that clinical team support, system/technology support and patient care support are the three main pillars of promoting patient engagement. 5 Alongside the overarching argument that “patient engagement is the key driver of high-quality healthcare outcomes”. 5 (p3)
Given increasing calls to make health services accessible, and the value technologies have in doing so, many interprofessional health teams supporting adults with chronic conditions are likely to amplify their use of virtual platforms. 1 As such, supporting patients to engage as partners on their care teams and navigate new and evolving virtual technologies is a pressing priority. It is hoped that this scoping review will influence interprofessional healthcare teams who are supporting patients virtually to develop or modify existing virtual care approaches to be more accessible and patient-centred. Ultimately, from this study, there was evidence for using a virtual care coordinator to prepare patients for synchronous virtual sessions that foster ‘webside manner’. Future research should explore interprofessional HCPs’ experiences engaging patients within virtual care teams to identify what additional resources are needed to improve quality of care.
Footnotes
Appendix A
Peer-Reviewed Literature: MEDLINE Search Strategy
Ovid MEDLINE: Epub Ahead of Print, In-Process & Other Non-Indexed Citations, Ovid MEDLINE® Daily and Ovid MEDLINE® <1946-Present
Appendix B
Grey Literature - Google Engine Search Strategy
● 64 sources screened ● 21 included
● 80 sources screened ● 5 included
● 64 sources screened ● 15 included
● 56 sources screened ● 14 included
● 68 sources screened ● 10 included
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
