Abstract
Family perspectives on short-term recovery after spinal fusion for neuromuscular scoliosis are essential for improving patient outcomes. Semistructured interviews were conducted with 18 families of children within 3 months after spinal fusion performed August 2017 to January 2019 at a children’s hospital. Interviews were recorded, transcribed, and coded line-by-line by 2 independent reviewers using grounded theory to identify themes. Five themes emerged among families when reflecting back on the postoperative recovery: (1) communicating and making shared decisions regarding postoperative care in a patient- and family-centered manner, (2) setting hospital discharge goals and being ready for discharge, (3) planning for transportation from hospital to home, (4) acquiring supports for caregiving at home after discharge, and (5) anticipating a long recovery at home. Important family perceptions were elicited about the recovery of children from spinal fusion for neuromuscular scoliosis that will inform better perioperative planning for clinicians, future patients, and their families.
Introduction
Recovery after major surgery in children is often more difficult than patients or families initially anticipate (1). Preoperative discussions about recovery from major surgery, when conducted, focus mostly on the anticipated hospital experience, including risk of complications (2 –5). Recovery beyond hospitalization is critical to discuss because it can impact a child and family’s life in several areas, including physical and emotional health as well as education, employment, and finances. Improved understanding of the comprehensive patient and family experience about recovery—from hospital to home—could enhance the ability of clinicians to optimally prepare children and their families for major surgery. Discussing anticipated long-term outcomes is also important for understanding patient and family goals and expectations upfront, in order to help better align patient and provider expectations for the surgery and recovery.
Spinal fusion—along with other major elective surgeries and procedures—accounts for a large proportion of hospital care experienced by children with medical complexity (6 –8). Recovery from spinal fusion can be arduous and unpredictable. Spinal fusion for neuromuscular scoliosis in children, in particular, is associated with major physiologic stress, prolonged recovery, and high complication rates (9 –11). After spinal fusion, children are at risk for wound infections as well as functional impairment of the gastrointestinal, pulmonary, urinary, and other organ systems (12 –16). Parents of children with neuromuscular scoliosis undergoing spinal fusion report that they, in retrospect, wished that they had been better prepared for the recovery experience (17). Parents, who have observed their child’s experience with spinal fusion, can provide unique perspectives on their child’s recovery, including the postoperative inpatient phase, hospital discharge, and recovery at home. Prior studies have examined patient and parent experiences, including stressors and coping strategies with spinal fusion for idiopathic scoliosis in otherwise healthy children (18). The current study advances knowledge by assessing the postoperative experiences of children with neuromuscular scoliosis and their families to provide a roadmap for a more comprehensive conversation about recovery and to better prepare future parents and patients considering spinal fusion.
Methods
Study Design, Setting, and Participants
We conducted a qualitative study using semistructured phone interviews from August 2017 to January 2019 with parents of children with neuromuscular scoliosis who recently underwent spinal fusion surgery at a freestanding children’s hospital. Operation procedures remained unchanged during the study. The interview guide was developed with input from the parent partner on our research team, discussions with others parents of spinal fusion patients, literature review of patient and family experiences with spine surgery, and the Consumer Assessment of Healthcare Providers and Systems Surgical Care Survey (19). Approval for this research was obtained (IRB15-2971) by the institutional review board of Boston Children’s Hospital.
Postoperative Interview Procedures
Participants were identified from a prospective list of children with neuromuscular scoliosis scheduled for spinal fusion maintained for quality improvement purposes. A study team member approached parents for study participation by phone or in person during their child’s postoperative stay. Informed written consent was obtained from parents at that time. Phone interviews were scheduled 3 to 6 weeks after surgery. Of families successfully contacted for postoperative interviews, none declined to participate.
The interview focused on in-hospital recovery, transition home from the hospital, and recovery at home. Example questions that followed the course of the postoperative period included, “How did your child’s recovery compare to what you expected?,” “Can you tell me about your child’s experience leaving the hospital?,” and “How has your child’s recovery progressed?” Interviewers did not have a clinical relationship with the patients or parents. Interviews were audio recorded and transcribed verbatim and were continued until thematic saturation occurred.
Qualitative Analysis
Two study team members independently reviewed each interview transcript using line-by-line coding to generate themes about recovery without introducing coder bias (19). Then, those 2 team members reviewed the themes and related codes with the full study team to harmonize findings and set the final nomenclature for the themes. To assess reliability of findings, data were concurrently collected and analyzed, thereby confirming recurrent ideas generated (20). Two parent study team members (L.B. and E.W.), whose children previously underwent spinal fusion, corroborated the parent experiences. Interviews were discontinued once theme saturation was achieved.
Results
Characteristics of the Study Population
Results draw on 18 semistructured postoperative interviews lasting a median 31 minutes (interquartile range [IQR] 20-42 minutes) that were conducted a median of 66 days (IQR: 50-77 days) after surgery (Table 1). For families interviewed, the children had a median age of 15 years, and the median number of vertebrae fused was 15. After surgery and prior to the interview, approximately 72% of patients had at least one complication, and 39% of patients required a second procedure due to a surgical complication (eg, wound infection, pneumothorax). Perceptions of families did not differ between children with versus without a complication. After surgery, the median length of hospital stay was 8 days (IQR: 5-14 days).
Characteristics of the Study Population and Family Interviews.
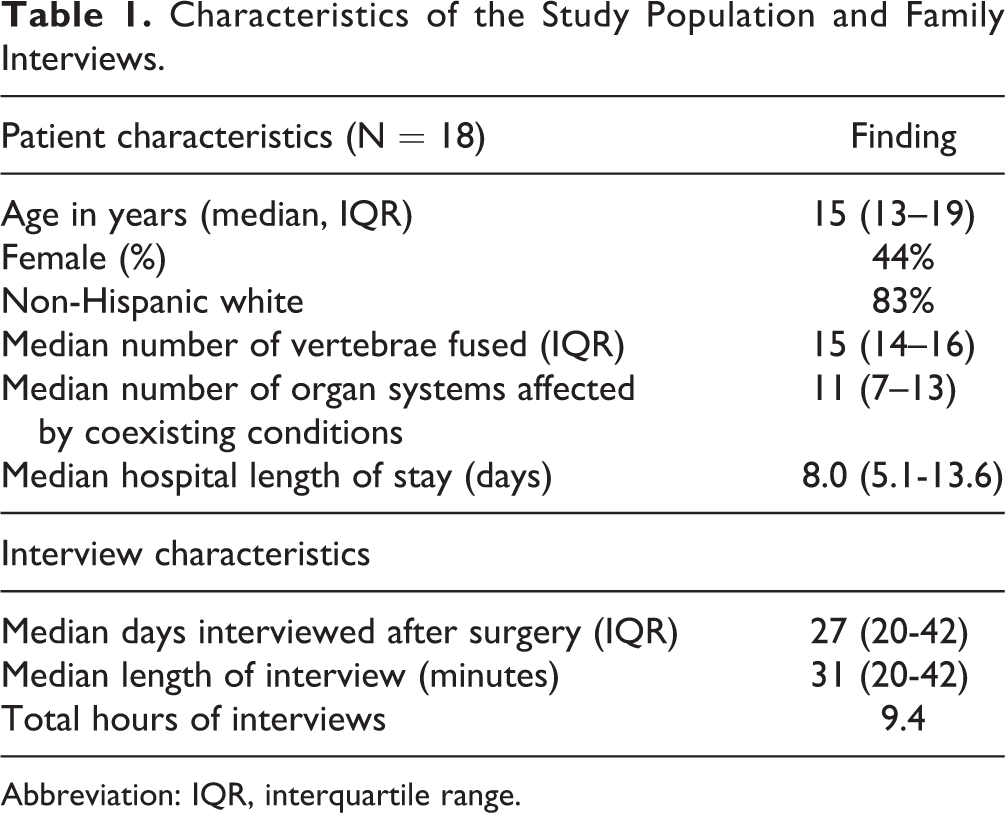
Abbreviation: IQR, interquartile range.
Themes on Recovery Following Spinal Fusion
Over the course of the postoperative period, 5 themes about short-term recovery emerged: (1) engaging in patient- and family-centered postoperative care planning, (2) setting hospital discharge goals and being ready for discharge, (3) planning for transportation from hospital to home, (4) securing caregiving help at home after discharge, and (5) anticipating long recovery at home. The results for each theme are presented below.
Theme 1: Engaging in patient- and family-centered postoperative care planning
Some parents highlighted the importance of strong, direct communication regarding the plan of care with their child’s postoperative providers. They expressed frustration when medical decisions (eg, when to extubate the breathing tube after surgery) were made without their input. Some parents were unclear on “the best person to have a good pow-wow with” about their child’s recovery and postoperative plan of care, because there were so many providers (eg, nurses, residents, fellows, and attending physicians) involved in their child’s postoperative care. Some parents conveyed that they were unsure which provider was “in charge” of the postoperative plan. For example (also see Table 2):
Going in, they needed to do a better job of telling me what they were doing. Because their plan was different than what the plan was when he left from surgery. They needed to do a better job of communicating to me that that plan had changed and why.
Family Perceptions of Their Child’s In-Hospital Recovery.

Theme 2: Setting hospital discharge goals and being ready for discharge
Many parents reported having different opinions with the hospital staff about the timing of discharge. Some parents wanted to leave before the clinical team felt like the child was recovered enough to go home. Other parents felt that their children recover best at home; they wanted to leave as soon as their children were medically stable and the clinicians felt comfortable with them leaving the hospital. Other parents felt like their child needed a few more days in the hospital, despite clinicians saying their child was ready to go home. A few parents reported asking the perioperative team if they could stay in the hospital an extra day or 2 because they did not feel prepared to take their child home. For example: The only thing that made him stay longer was I didn’t want to have to bring him back here. [The orthopedic team] asked me if we could send him home…and I said no. To me, it was too early. And it just worked out that the same nurse who had checked my child into the floor when we arrived was the women who discharged him. We knew her, we were comfortable with her, [and] she was comfortable with us so the process…felt really comfortable.
Family Perceptions of Their Child’s Hospital Discharge.

Family Perceptions of Their Child at Home After Hospital Discharge.

Theme 3: Planning for transportation from hospital to home
Many parents reported significant stress and difficulty coordinating transportation home from the hospital. Many parents had to decide between a car, plane, transport van, and/or ambulance while considering the comfort and well-being of their child as well as the feasibility and cost of the transportation. For example: We were back and forth between airplane being the best way or car ride, and in the end, we decided car ride because we could lay her down, as opposed to an airplane where we would have to lay her up on her back and you can’t really rest that area. So it worked out. I feel that the doctors really leaned forward trying to get us discharged, which I appreciate.
Parent comments underscored the need to provide comprehensive and coordinated care for all aspects of discharge—including transportation, equipment, medication changes, home nursing or care needs, and therapeutic interventions and for team roles to clearly define who will follow through with these action items.
Theme 4: Securing caregiving help at home after discharge
Many parents noted that caregiving at home after discharge was particularly challenging, especially with insufficient sleep and rest while in the hospital and with feelings of stress about their child’s recovery. Some parents noted the importance of self-care (ie, care for themselves) in order to provide the best care for their child. Many parents perceived that greater help from home nurses would have been beneficial. Many parents expressed the desire for increased hours of home nursing after their child’s surgery. Many parents confessed that they did not seriously consider asking for home nursing until it was too late (eg, they were already home) and retrospectively wished they had asked for more help at home. For example: I’m kicking myself because I realized I should’ve asked for help. I didn’t realize what that would look like when I got home.
Theme 5: Anticipating long recovery at home
In general, most parents reported that their child’s hospital recovery was smoother than they anticipated but that long-term recovery following discharge was slow and nonlinear. Most parents were very pleased with their children’s ability to sit upright after spine surgery. However, as one parent noted, “The immediate recovery doesn’t even touch what the actual recovery is.” Some parents reported that their children experienced prolonged weakness and fatigue and that—even a few months after surgery—recovery was still ongoing and sometimes frustrating. Although most parents noted home physical therapy helped to some degree, the therapy exercises were difficult to conduct when their child was recovering and in pain. Overall, most parents reported improved quality of life after surgery which they attributed to decreased back pain, as well as improved respiratory health and reduced constipation. However, some parents reported that their child continued to experience significant pain and stiffness several months after surgery. For example: At first, his recovery was stellar. I was like oh my God! This is too good to be true. And in true [child] fashion, the swelling reared its ugly head and that put us back.
Discussion
Parents whose children underwent spinal fusion for neuromuscular scoliosis conveyed unique and important perspectives about short-term recovery in hospital, the hospital discharge experience, and on-going recovery at home. In particular, parents highlighted (1) engaging in patient- and family-centered postoperative care planning, (2) setting hospital discharge goals and being ready for discharge, (3) planning for transportation from hospital to home, (4) securing caregiving help at home after discharge, and (5) anticipating long recovery at home. Embedded throughout all of these areas were critical family and social aspects of patient recovery that ranged from seemingly simple constructs (eg, transportation home from the hospital) to more complicated matters (eg, ability and comfort level of parents taking care of their child at home with significant postoperative impairments; Figure 1). All of the themes raised by parents suggest that perioperative care may benefit the most from a more patient and family-centered approach that focuses on clear communication about plans and anticipatory guidance.

Pathway of short-term recovery after spinal fusion.
The challenges with patient and family-centered postoperative care conveyed by parents in the current study merits further attention. Prior studies underscore the value of fully partnering with parents in making decisions about their child’s postoperative care plans (21,22). Care is more likely optimized when families are empowered to “speak up” about their needs and concerns, especially when clinicians are not sufficiently involving and informing them (23). Across patients, there are routine aspects to postoperative care management that could serve as touch points to ensure high-quality patient and family-centered care. These include, for example, decisions about extubation from ventilatory support following surgery, initiation of enteral diet after the use of IV nutrition, and weaning patients from postoperative pain medications. These are anticipated decision points in postsurgical care that could be first reviewed and discussed in perioperative clinical discussions with the family. Family-centered rounds during hospitalization—particularly with these postoperative aspects of care in mind—might be beneficial to ensure that patient and family perceptions and preferences are explicitly sought, conveyed, and used in medical decision-making. Family-centered rounds have an established impact on improving patient communication, education, safety, and satisfaction (24 –27).
Of the themes conveyed by families, setting discharge goals and deriving discharge plans carried particular weight among the families who were interviewed; these themes may represent the most critical components of postoperative spinal fusion care to optimize. Establishing discharge goals, including the achievement of a stable postoperative physiologic state, is a foundational step to pediatric hospital discharge care (3). Clearly, many parents in the current study expressed concerns about discordant family provider views of the optimal timing of hospital discharge. Disagreement about discharge readiness among physicians, nurses, and pediatric patients and families is not uncommon (28 –30). Prior studies report higher rates of unplanned, hospital readmission when children and families are discharged before they feel ready to leave the hospital (31). High rates of readmission are reported among children with neuromuscular scoliosis undergoing spinal fusion (14,32,33). Considerations for discharge goals after spinal fusion routinely include sufficient postoperative pain control, cardiopulmonary stability, nutrition/hydration, and bowel and bladder functioning. Perhaps these and related clinical issues could be better addressed through discussion early in the admission—or even ahead of surgery altogether—to best educate and prepare patients and families to anticipate the process and planning for hospital discharge (28).
Once home, many parents noted that they underestimated the amount of time and effort needed to care for their child. Prior studies of children undergoing other high-risk operations (eg, solid organ transplant) report high rates of familial struggles coping with children’s health, well-being, and cares after discharge (34). Multiple parents in the current study mentioned the need for home health care assistance. Setting up home health care for children expeditiously—especially for children and families using it for the first time—can be a challenging task. The supply of pediatric home health care providers often does not match the demand for them (35). Perhaps, with further inquiry on the specific aspects of home health for which families need the most help (eg, lifting and transitioning their children, adjustments needed with, and new acquisition of medical equipment), other clinical personnel options (eg, personal care attendant) could be explored preoperatively. In particular, postdischarge home visits for hospitalized children with medical complexity conducted by hospital providers have been valuable to help families work through challenges in caregiving that they are experiencing at home (36).
There are several limitations to our study. Parent perceptions of recovery were measured within a few months of surgery. Longer term perspectives may reveal new important themes about recovery. The current study involved a single freestanding children’s hospital. Additional investigation of parent experiences in other hospitals is needed to assess the generalizability of the study findings. The qualitative approach to the current study is not positioned to assess correlations or causality between the themes and the perioperative health outcomes experienced by the children. Perceptions of recovery from the viewpoint of clinicians (eg, nurses, physicians, and adjunct staff) were not obtained in the current study. Relatedly, the viewpoint of the child was not elicited in the current study. Future studies should assess and compare these perceptions with those conveyed by families.
The current study elucidates several opportunities to optimize in-hospital recovery, hospital discharge, and at home recovery from spinal fusion for neuromuscular scoliosis in children, especially regarding (1) patient and family-centered postoperative care, (2) discharge goal setting, (3) planning for transportation home, (4) caregiver support after discharge home, and (5) home recovery trajectories. These important constructs may be used to derive the clinical structure and content of perioperative care plans (eg, through a template) for use by families and providers. Certainly, such a structure may help standardize the derivation of high-quality care plans. Articulating families’ needs throughout the recovery process and sharing them with clinicians and future families considering spinal fusion may heighten attention to the recovery process after spinal fusion surgery. Future studies are needed to evaluate the feasibility and impact of integrating families’ perspectives and experiences outlined in this study in the care of future families whose children will undergo spinal fusion for neuromuscular scoliosis. Efforts to evaluate the impact of parent-to-parent advice, in particular, are needed; it is possible that such advice may help shape and augment perioperative care planning discussions and decision-making.
Footnotes
Acknowledgments
Members of the EHRLL working group are as follows: J Emans, T Hresko, D Hedequist, ME McCann, R Brustowicz, Boston Children’s Hospital, Boston; TS Yap, Y Kaya, C Retzios, Northeastern University, Boston.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funded by the Agency for Healthcare Research and Quality (1P30HS024453-01). Approval for this research was obtained (IRB15-2971) by the Boston Children’s Hospital Institutional Review Board.
