Abstract
Patient-centered medical home (PCMH) has spurred primary care reform and improvements in patient care quality. Very little is known about the differences practices implement during PCMH transformation. We examined 105 primary care practice leader experiences during PCMH transformation, asking in semi-structured interviews about the changes they targeted. We used content analysis to classify these PCMH changes and examined how they aligned with what is measured on PCMH-recommended patient experience surveys. During PMCH transformation, practices most commonly targeted changes in care coordination (30%), access to care (25%), and provider communication (24%). Reported areas of PCMH transformation were measured by Clinician & Group Consumer Assessment of Healthcare Providers and Systems (CAHPS), PCMH CAHPS, or supplemental CAHPS survey items, including team-based care (35%), providing more services on site (28%), care management (22%), patient-centered culture (18%), and chronic condition health education (13%). Many PCMH changes are captured by CAHPS patient experience items; some are not. For some uncaptured areas, patients are not the best source of information. To provide practice leaders information they need for PCMH transformation, CAHPS items need to measure care management to support medical and chronic conditions, and chronic condition health education.
Introduction
The US health system faces ongoing challenges with access, care coordination, and quality of primary patient care (1,2). The National Academy of Medicine (formerly known as the Institute of Medicine) (3,4) includes patient-centered care as 1 of 6 domains of quality (2). Yet, the National Academy of Medicine and others also note that a chasm exists between the kind of care patients should have versus what they receive (5). Since 2007, national efforts have sought to improve the quality of care provided patients, including primary care practice transformation from a siloed provider-centric model—a system organized around what physicians and institutions “do” (eg, care provision designed around medical specialties and types of services) into a patient-centered medical home (PCMH) focused on what patients “need” (6). A PCMH aims to improve access, coordination of care, chronic disease management, and responsiveness by implementing team-based care, access strategies such as same-day appointments and extended hours, and coordinated and comprehensive services to better meet the needs of the patient (7 –10). Successful PCMH transformation requires investment in new processes of care delivery, staffing models, and methods of data tracking and coordination within each primary care practice (11,12). Practice leaders implementing these new capabilities are firsthand observers and monitors of these changes.
Practices are required to administer a patient-experience survey for PCMH recognition to the National Committee for Quality Assurance (NCQA) (13). The NCQA recommends practices administer the Consumer Assessment of Healthcare Providers and Systems (CAHPS) Clinician & Group (CG-CAHPS) survey (14,15). Practices can also add 14 PCMH supplemental items to the CG-CAHPS survey (CAHPS PCMH survey) to receive Patient Experience Distinction (6,16,17). Patient Experience Distinction is an annual status given to any practice that administers and submits CAHPS PCMH survey data to NCQA. Over 13 000 practices (15%-18% of primary care physicians) are recognized as a PCMH by NCQA (18,19), but only about 250 practices have this 1-year Patient Experience Distinction (18). Very little is known about the targeted differences in care delivery that practices are implementing during their PCMH transformation and whether these changes are captured on PCMH-recommended patient experience survey tools.
This article examines experiences of 105 primary care practice leaders during PCMH transformation. Specifically, we asked these leaders about the areas they targeted during PCMH transformation and whether CAHPS survey items capture expected changes in patients’ experiences of care.
Methods
Design and Sample
We randomly selected 294 practices from the 2008 to 2017 NCQA directory of PCMH practices by US region, physician count, level and years of PCMH recognition, and history administering the CAHPS PCMH survey. We completed interviews with leaders from 105 primary care practices, a 36% response rate. Practices had varying number of years of NCQA PCMH status; PMCH status was measured as level 1 or 2 (ie, not having obtained NCQA PCMH recognition) or level 3, indicating they had received NCQA PCMH recognition, which we divided into 3 groups: level 3 status for <3 years, 3 to 5 years, and >5 years. Practices at level 1 or 2 completed some PCMH requirements out of the 6 core standards, but not enough to reach level 3 and be recognized as a PCMH. Practices that receive level 3 status are a recognized PCMH and need to reapply after 3 years to maintain their PCMH level 3 status. The sample included practices that currently, previously, or have never administered the CAHPS PCMH survey. Geographically, we considered whether practices were in states with a statewide initiative to obtain PCMH recognition for all primary care practices (ie, Vermont and New York; 25%), in another Northeastern state (25%), in a Southern state (25%), in the Midwest (16%), or in the West (11%).
Data Collection
We conducted semi-structured, hour-long phone interviews from June 2017 to June 2018 with the 105 practice leaders, documenting their perspectives on PCMH transformation and changes in patient experience. We spoke with leaders knowledgeable about the practice’s PCMH history and patient experience data. Verbal informed consent was obtained at the beginning of the interview and then were asked leaders to describe their job, practice location, tasks related to PCMH, and how long they had been involved in PCMH implementation. We discussed practice transformation decisions and change efforts to identify differences between PCMH and traditional provider-centric practices (see Supplementary Table S1 for a list of interview topics). We also gathered information on practice characteristics (see Supplementary Table S2). Interviewers documented field notes and key takeaways following the interviews. Audio recordings were transcribed, and participants received a US$75 honorarium.
Analytic Approach
We entered transcripts into Dedoose (20), a web application for managing and analyzing qualitative data. We established codes that mapped to key research questions (21) and conducted content analysis to identify topics (22) to develop a codebook (21). We developed the code structure using systematic, inductive procedures to generate insights from responses (23) and used content analysis to develop emerging themes (24). Early transcripts were coded independently, noting topics such as practice leader reported differences in care after PCMH recognition, and in which areas of patient experience those differences in care occurred (21).
The 4-person coding team met regularly to reach consensus on topics, identify discrepancies, refine concepts, and define codes (25). We employed inter-rater reliability exercises to refine codes and descriptions. After code training, we compared coding differences between 4 coders and obtained a pooled κ coefficient of .93, indicating “very good” agreement (26 –28). We employed ongoing training among the coding team on emerging subcodes using the Dedoose training module.
To understand whether CAHPS items that are available to practice leaders to administer on their patient experience surveys fully capture the practice’s targeted PCMH areas of improvement, we mapped the reported differences in care to specific domains and items in the PCMH-recommended patient experience surveys (ie, CG-CAHPS core survey, version 3.0, 14 CAHPS PCMH items, and CAHPS supplemental items) or identified them as not covered by these items. We grouped identified domains not covered by CG-CAHPS into care experience domains. For each domain, we inferred who would be the best source of the information and the individuals most likely to experience the change in practice.
Study protocols were approved by the institutional review board of the Human Subjects Protection Committee (IRB_Assurance_No: FWA00003425; IRB_Number: IRB00000051) and approved by the Office of Management and Budget (OMB_No: 0935-0236).
Results
Practice Characteristics
Most practices were small (ie, less than 10 physicians), served both adult and children, and were part of a group/network (see Table 1). Half were affiliated with a hospital. About half were a Federally Qualified Health Center, while a third were privately owned.
Practice Characteristics.
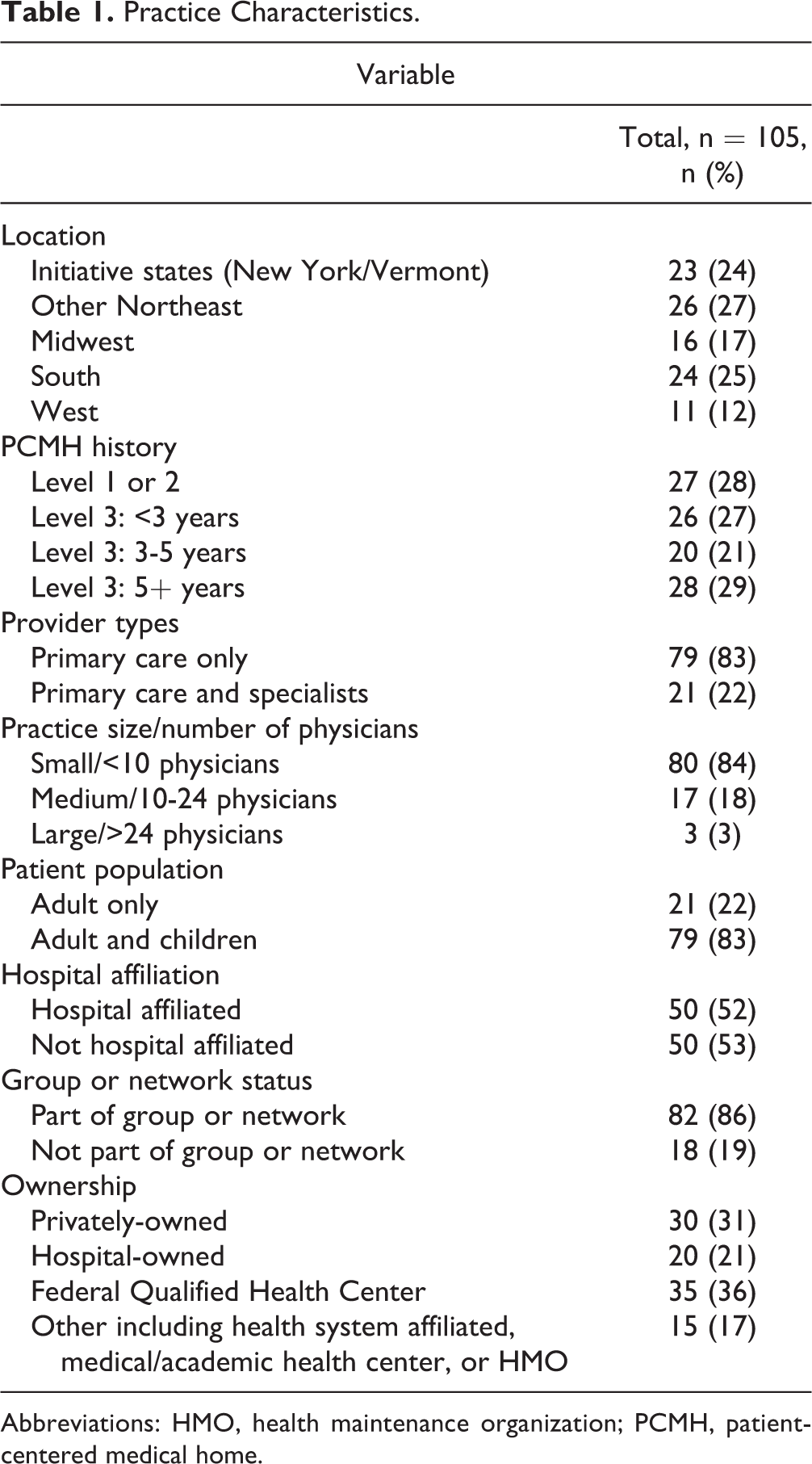

Abbreviations: HMO, health maintenance organization; PCMH, patient-centered medical home.
Practice Leader Characteristics
Two-thirds of the interviewed practice leaders had other job functions besides PCMH transformation (see Table 2). Half of the practices had leaders located at the practice during PCMH implementation, while about 40% of practices had leaders located off-site and managing the implementation process for multiple practices. Seventy-eight percent of practice leaders reported working at the practice the whole time their practice pursued PCMH compared to 22% who reported joining at a later stage of PCMH transformation process. Approximately 60% of practice leaders were involved with the first PCMH application for their practice, while only one-quarter were involved in subsequent applications. Sixty-one percent of practice leaders were on a team of providers and support staff who decided on and implemented the necessary changes to satisfy PCMH standards. Approximately 70% were coordinators for the PCMH efforts at their practice or network, while half (51%) reported being part of a team of providers and support staff that reviewed data to determine changes needed for PCMH.
Practice Leader Characteristics.
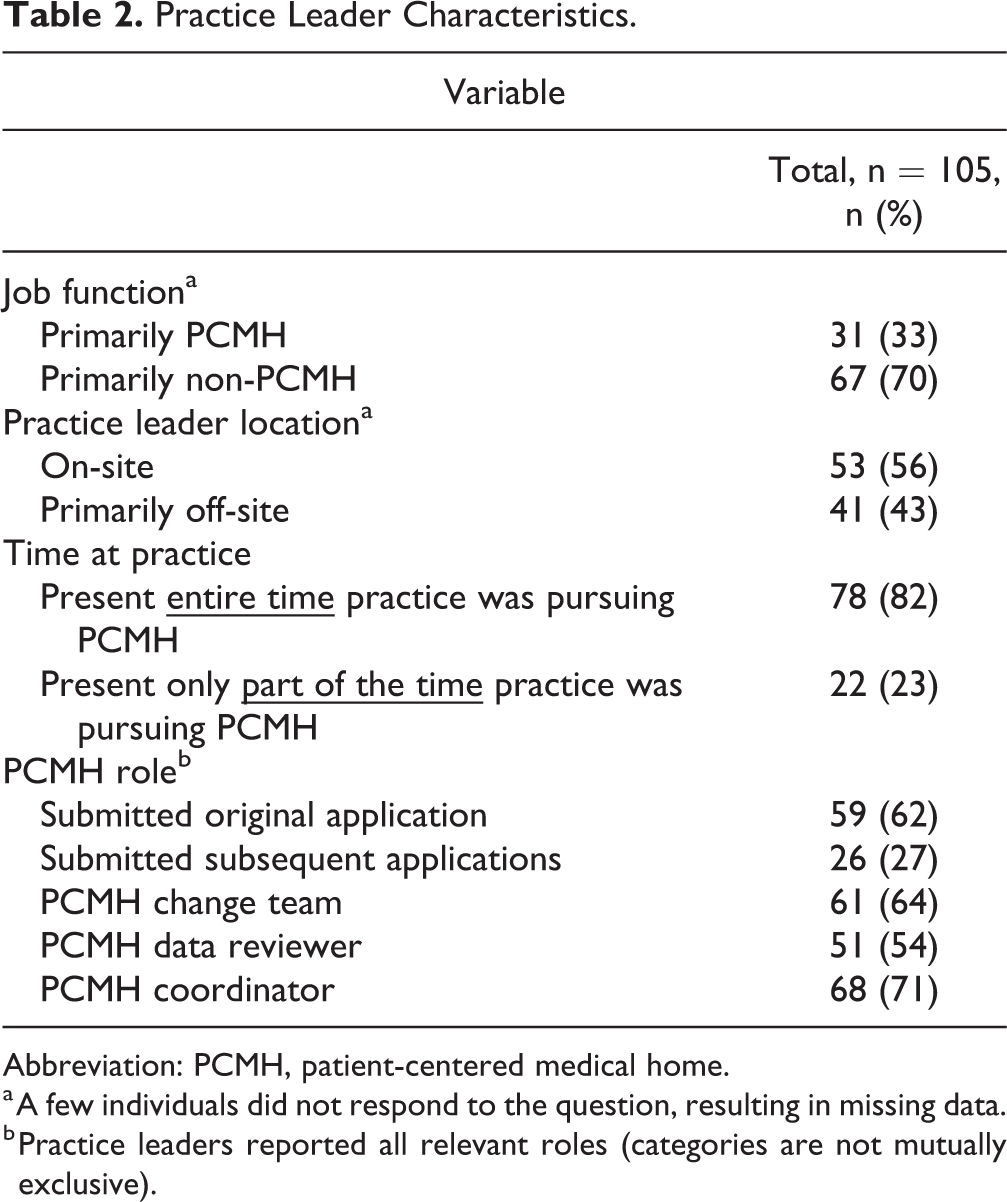
Abbreviation: PCMH, patient-centered medical home.
a A few individuals did not respond to the question, resulting in missing data.
b Practice leaders reported all relevant roles (categories are not mutually exclusive).
Reported Types of PCMH Care Changes
Practice leaders reported that the care they delivered to patients as a PCMH differed most from the care provided prior to pursuing PMCH recognition in terms of care coordination (mentioned by 30% of practices), access to care (25%), and provider communication (24%; see Table 3). Mapping these types of PCMH care changes to the content of CAHPS survey, we found that about one-quarter of the practice leaders indicated areas of targeted PCMH change that could be assessed by CG-CAHPS survey items. These included changes in provider communication (eg, listening carefully [10%], spending enough time [6%]), areas of care coordination such as follow-up on lab test results (10%) or discussions about prescription medicine (9%), and access to care (eg, receiving answers to phone inquiries the same day [8%] or appointments for urgent care [5%]). Some practices also reported PCMH changes in care measured by the CAHPS PCMH items (14%) or other supplemental CAHPS items such as changes in wait times (10%) or shared decision-making (10%).
Practice Leader-Reported Changes in Care During PCMH Transformation, by Domain and Survey, and Listing Best Source of Information.
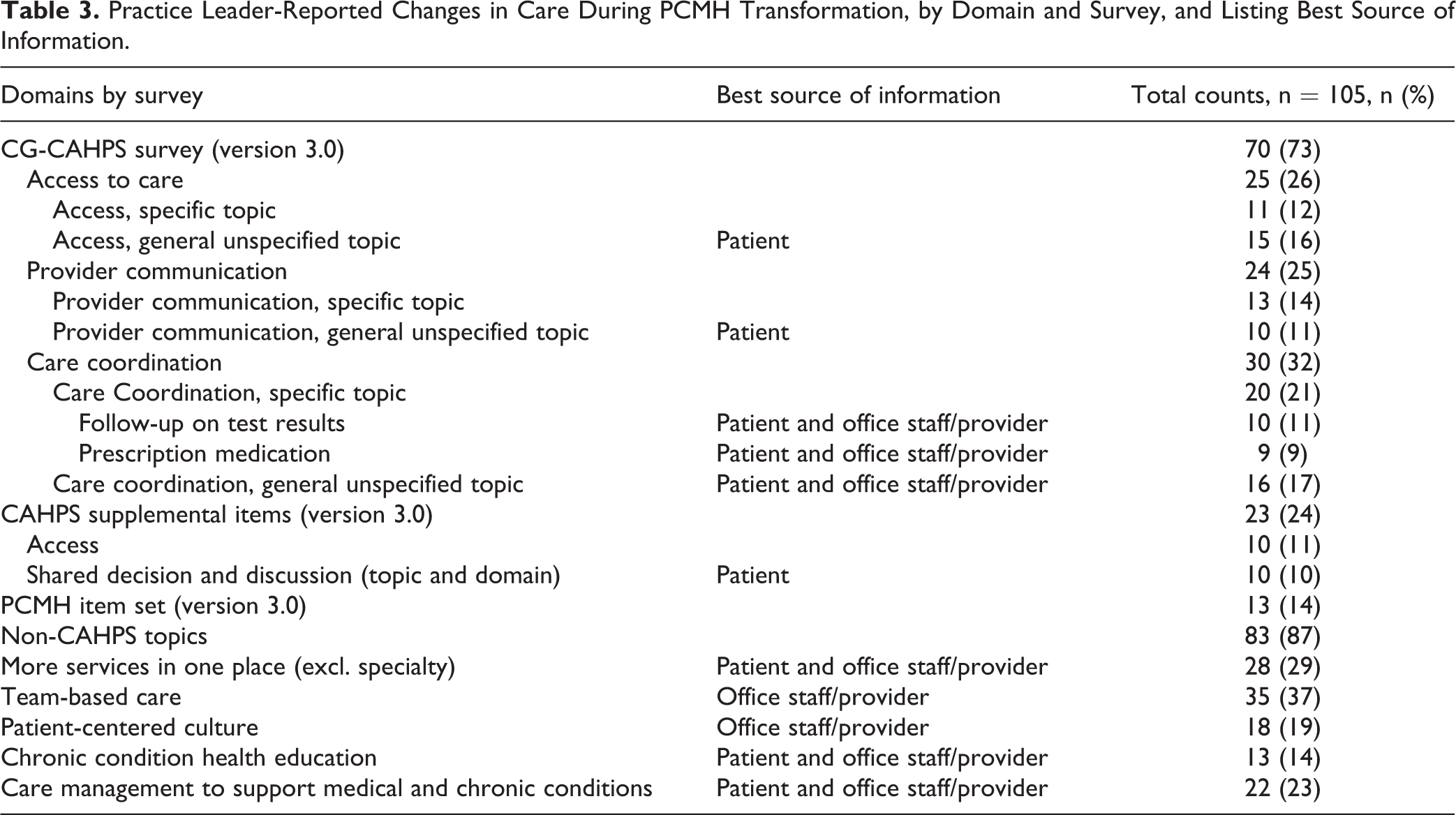
Over 80% of practice leaders reported that they targeted changes during PMCH transformation in areas not measured in the ambulatory CAHPS surveys (ie, CG-CAHPS core survey, version 3.0, 14 CAHPS PCMH items, or CAHPS supplemental items), such as team-based care (35%), providing more services in one place (28%), care management for medical and chronic conditions (22%), patient-centered culture (18%), and chronic condition health education (13%; see Supplementary Table S3 for the definitions of all identified domains of patient experience).
By survey type
Practice leaders reported several PCMH-targeted areas of change where the care they delivered to patients as a PCMH differed from the care provided prior to pursuing PMCH recognition. Of the 105 practices who participated in the study, practice leaders in 70% (n = 73) of practices reported targeting changes that mapped to at least 1 item in the CG-CAHPS core. This included items that were classified as “general” items (ie, items that practice leaders reported that fell under a specific domain but were not specific to a CAHPS item). For example, if a practice leader reported improvements in access, but they did not report whether these improvements were related to urgent care or routine care appointments or ensuring that the patient receives a response to an inquiry in the same day they made the inquiry, the differences would be coded under “access to care” and not attributed to a specific question. Furthermore, practice leaders at 30% (n = 32) of practices reported targeting PCMH changes that mapped to more than 1 item in the CG-CAHPS core.
Leaders at 23% (n = 24) of practices targeted PCMH changes that mapped to at least one of the CAHPS supplemental items. Similarly, 13% (n = 14) of practice leaders reported PCMH changes that mapped to at least 1 item in the CAHPS PCMH item set.
Of the 105 participating practices, practice leaders at 83% (n = 87) of practices reported PCMH changes in domains not covered by the CAHPS surveys (see examples in Table 4).
Exemplar Quotes of Changes in Care Targeted During PCMH Transformation, By CAHPS Survey.

Abbreviations: CAHPS, Consumer Assessment of Healthcare Providers and Systems; HER, electronic health record; PCMH, patient-centered medical home; RN, registered nurse.
By CG-CAHPS core topics
Of the CG-CAHPS domains, care coordination was the most frequently targeted area of PCMH practice transformation reported by practice leaders. Practice leaders at 30% (n = 32) of practices reported targeting changes concerning care coordination. Leaders at 17% (n = 16) of practices reported general changes in care coordination (see Table 4). Also, within the care coordination domain, 11% (n = 10) of practice leaders reported targeting PCMH changes in following up on test results and 9% (n = 9) reported targeting changes in discussions about medicine. For these 2 areas under care coordination, both the patient and the health care provider or staff are the best source of information.
The next most frequently cited CG-CAHPS domain that practice leaders reported as differing due to PCMH transformation was access to care, mentioned by leaders at 25% of the practices. Practice leaders most frequently reported targeting general differences in access to care due to PCMH transformation (15%).
Provider communication was the next and third most frequently cited CG-CAHPS domain that practice leaders targeted due to PCMH transformation (see Table 3). For patient–provider communication, both patients and health care providers or office staff are seen to be the best source of information about communication.
By CAHPS supplemental topics
Of the 105 practices participating in this study, practice leaders at 10% (n = 10) of practices reported targeting areas of PCMH change related to CAHPS supplemental items related to shared decision-making and discussions between the patient and the provider. Another commonly cited domain targeted by practice leaders that relates to CAHPS supplemental item was access to care. PCMH transformation related to access was reported by 11% (n = 11) of practices and included items related to getting answers to questions or getting care on weekends and after hours. For both these patient experience areas, the patient is the best source of information.
Not covered by CAHPS ambulatory surveys
Practice leaders reported transformation efforts in several areas that are not measured by core CG-CAHPS, PCMH items, or other non-PCMH CAHPS supplemental items (see Table 3). Most notably, practice leaders at 35% (n = 37) of practices discussed improvement in team-based care as a key area of change targeted by pursuing PCMH recognition. Team-based care is defined by the National Academy of Medicine as the provision of health services to individuals, families, and/or their communities by at least two health providers who work collaboratively with patients and their caregivers—to the extent preferred by each patient - to accomplish shared goals within and across settings to achieve coordinated, high-quality care. (29
–31)
Care management to support medical and chronic conditions was also reported as an area targeted when pursuing PCMH and maintaining PCMH recognition. Practice leaders at 22% (n = 23) of practices reported targeting PCMH-based transformation of care management (see example in Table 4).
Other areas that practice leaders reported targeting as part of transformation efforts were patient-centered culture (18%) and chronic condition health education (13%). Health care providers or staff are the best source to measure changes in office culture (32), while patients and providers or staff can both be the source of information about chronic condition health education.
Discussion/Conclusion
Practice leaders reported that during PCMH transformation, they targeted changes in care delivery in 3 main areas of patient experience that distinguished care as a PCMH from the care provided prior to pursuing PMCH recognition: access to care, provider communication, and care coordination. These most cited areas of care targeted during PCMH transformation by practice leaders are measured by the patient experience CG-CAHPS core survey items, which is the NCQA PCMH-recommended patient experience survey. Our findings are supported by the current evidence about the importance of provider communication. Provider communication is the aspect of patient experience most correlated with the overall rating of a provider or of a primary care clinic (33 –35). As such, provider communication is an important area of patient experience to target when transforming care delivery to be more patient centered as is by a PCMH. Some evidence exists that care management to support medical and chronic conditions is also one of the foundational aspects of patient experience that practices target when making changes to become a PCMH, followed by a focus on 2 other areas: quality improvement infrastructure and realigning continuity of care (36). Following these 3 types of PCMH-targeted changes, practices in this same study focused on access to care such as adding urgent care, patient portals, or extending hours (36).
Practices in our study used the CG-CAHPS survey as their main patient experience survey and, in general, were more likely to have attained NCQA PCMH recognition (ie, PCMH level 3) for more than 3 years (vs less than 3 years or a designation as a PCMH level 1 or level 2, which indicates a practice is not yet a PCMH). Additionally, leaders from practices with longer PCMH recognition histories (ie, more than 3 years as a PCMH level 3) in general reported targeting the most PCMH-related changes in care, showing that the pursuit of not only PCMH recognition as a level 3 but full PCMH transformation takes time; these practices were also significantly different than more traditional primary care practice models (ie those attaining PCMH level 1 or 2 and not yet PCMH recognized).
Our research identifies how areas of change for PCMH transformation and how these map to the CG-CAHPS survey items can shed light on the usefulness of patient experience surveys, particularly the CG-CAHPS surveys, and provide evidence for possibly adding topics to CAHPS surveys specific to PCMH transformation.
Over 80% of leaders at practices in our sample reported PCMH transformation efforts in areas not measured on the CAHPS survey. These are potentially areas of improvement in patient care that practice leaders are interested in measuring and however are not included in the PCMH-recommended CAHPS patient experience surveys. The 3 most commonly cited areas outside the CAHPS survey targeted during PCMH by practice leaders were team-based care, offering more services on-site at the primary care office, and care management to support medical and chronic conditions. Attention should be paid to who the best source of information would be for this information and whether a patient experience survey would be the best avenue to collect this information. For example, questions on team-based care or a practice having a patient-centered culture are better suited to be reported on by individuals involved with the operation of the practice (ie, providers, staff, or practice managers), given that cultural practices or teamwork demonstrating the principles of PCMH would not be visible to patients. Because of its comprehensive nature, patient-centered culture (including respect of patients’ preferences, coordination and integration of care, considering patients’ physical and emotional comfort, involving family and friends, and prioritizing access and continuity of care for all patients) could at a global level be measured by tracking patients’ overall rating of providers or care, such as the CAHPS overall ratings of provider and care. To understand specific changes, items are needed to measure and monitor specific types of changes in culture related to care as a PCMH.
In terms of health education, there are 7 CG-CAHPS supplemental items known as the Health Promotion and Education item set related to general health promotion and education; however, these items ask about general illness prevention, healthy eating, exercise, stress, or sadness, rather than education that is specific to managing a chronic condition or a medical condition (https://www.ahrq.gov/cahps/surveys-guidance/item-sets/cg/suppl-healthpromotion-cg30-adult.html). Practice leaders were referring to changes in PCMH related to increased education, information, and tools provided to patients related to medical and chronic conditions, not general health.
Our study has limitations. First, although the sample of practices was large, varied, and included practices with a range of PCMH history, it is not a nationally representative sample of practices. As such, results are reported in percentages to show the variety and breadth of responses to inquiries on PCMH changes reported by practice leaders. Second, practice transformation related to patient-centered care and improved patient experiences is reported from the practice leaders’ perspective and not supplemented by patient-reported care experiences. The study attempted to obtain de-identified patient experience data from practices in the sample that used CAHPS surveys but was only able to obtain such permissions, except from 18 practices. Practice leaders, however, know the specific changes made to how care is provided and delivered so are the most knowledgeable about PCMH changes to care in their practices. Future work is needed to determine whether there is alignment between practice leaders’ perspectives and patient care experiences during PCMH transformation. Finally, practices were asked to report their perspectives on transformation efforts via interview, not a survey. As such, the results reported best represent the targeted areas of transformation in care practice leaders perceived to be most important or most able to be experienced by the patient and are not an exhaustive list of differences in care resulting from PCMH.
While many areas of change in patient experience targeted during PCMH transformation are captured by CAHPS items, some are not. For some non-CAHPS areas, such as team-based care, patients are not the best source of information. However, to give practice leaders the information they need to make and track changes in care and care experience during PCMH transformation, CAHPS items are needed to measure patient experiences of care management that support medical and chronic conditions and chronic condition health education.
Supplemental Material
Supplemental Material, Care_Differences_Paper_20190925_Supplemental_1_FINAL - Practice Leaders Report Targeting Several Types of Changes in Care Experienced by Patients During Patient-Centered Medical Home Transformation
Supplemental Material, Care_Differences_Paper_20190925_Supplemental_1_FINAL for Practice Leaders Report Targeting Several Types of Changes in Care Experienced by Patients During Patient-Centered Medical Home Transformation by Denise D Quigley, Nabeel Qureshi, Luma Al- Masarweh and Ron D Hays in Journal of Patient Experience
Supplemental Material
Supplemental Material, Care_Differences_Paper_20190925_Supplemental_2_FINAL_(1) - Practice Leaders Report Targeting Several Types of Changes in Care Experienced by Patients During Patient-Centered Medical Home Transformation
Supplemental Material, Care_Differences_Paper_20190925_Supplemental_2_FINAL_(1) for Practice Leaders Report Targeting Several Types of Changes in Care Experienced by Patients During Patient-Centered Medical Home Transformation by Denise D Quigley, Nabeel Qureshi, Luma Al- Masarweh and Ron D Hays in Journal of Patient Experience
Supplemental Material
Supplemental Material, Care_Differences_Paper_20190925_Supplemental_3_FINAL - Practice Leaders Report Targeting Several Types of Changes in Care Experienced by Patients During Patient-Centered Medical Home Transformation
Supplemental Material, Care_Differences_Paper_20190925_Supplemental_3_FINAL for Practice Leaders Report Targeting Several Types of Changes in Care Experienced by Patients During Patient-Centered Medical Home Transformation by Denise D Quigley, Nabeel Qureshi, Luma Al- Masarweh and Ron D Hays in Journal of Patient Experience
Footnotes
Authors’ Note
All authors met the following 4 criteria: (1) substantial contributions to the conception and design, acquisition, or analysis and interpretation of data; (2) drafting the article or revising it critically for important intellectual content; (3) final approval of the version to be published; and (4) all authors should take public responsibility for their manuscripts.
Acknowledgments
The authors thank Lynn Polite for her time and administrative support of the project; Rosa Elena Garcia for managing the recruitment of study participants, the time spent by the team of recruiters; and finally, the time and support of the interview participants in this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclose receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a cooperative agreement from the Agency for Healthcare Research and Quality (AHRQ; contract number U18 HS025920).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
