Abstract
Background:
Minimal research focuses on interactions between providers and new ostomy patients. Studies show that provider communication is important for patient health outcomes.
Objective:
The purpose of this study was to investigate ostomy patients’ perceptions of provider communication following surgery and whether interactions adequately prepare ostomy patients to care for their new appliance.
Method:
Using a nonprobability national sample of 381 ostomy patients, we conducted a retrospective quantitative study. We measured adequacy of provider communication from self-reports from ostomy patients.
Results:
The results show that almost half of the sample (49%) reported receiving inadequate communication from providers. We also found a relationship between ostomy patients’ educational level and their perceptions of receiving adequate communication. Notably, patients with lower educational attainment reported receiving adequate communication up to 4 times more than patients with higher educational attainment.
Conclusion:
Our results suggest that not only do ostomy patients need better communication from providers following their surgery but also patients with higher educational attainment appear to expect more information from providers than patients with lower educational attainment.
Introduction
Provider–patient interaction is a key factor in patient care and an essential component of the health-care system. Provider–patient interactions can impact psychosocial exchange, patient trust, satisfaction, and emotional well-being (1,2). Effective provider–patient interactions are shown to result in higher patient adherence (3), more informed decision-making, and increased coping strategies (2). In contrast, deficient provider–patient interactions may result in misdiagnoses (3), leave patients feeling disrespected or unheard (4), and produce feelings of distrust (5). These examples are true for many patient populations. Effective communication from providers is likely even more critical for patients who receive life-altering procedures, such as an ostomy. An ostomy refers to “the surgically created opening in the body for the discharge of body wastes” (6). Ostomies may be temporary or permanent and result from bladder or intestinal diseases, such as cancer, inflammatory bowel disease, trauma, or other reasons.
Several studies have demonstrated that having an ostomy can negatively impact an individual’s quality of life (7 –9), produce feelings of shame (10), stigmatization (11), and depression/anxiety (12). Qualitative studies have shown what it is like living with an ostomy (10). Few studies, however, have examined health-care-related interactions of people with an ostomy and providers. Additionally, little attention has been paid to whether hospital providers’ information and communication are adequate for new ostomates (Note 1). The current study takes a quantitative approach in understanding ostomy patients’ experiences at the hospital after receiving an ostomy. More specifically, we examine whether new ostomates feel they received adequate information and communication from hospital providers when they first received their ostomy and whether this information differs by patient demographics.
Background
Approximately 1 million people live with an ostomy in the United States. It is estimated that over 100,000 people receive an ostomy each year (6). New ostomates are especially in need of positive provider–patient interactions and effective provider communication. Literature focusing on provider-ostomate interactions is lacking. Although, one recent study of colorectal cancer ostomates showed that positive interactions with providers, such as receiving preoperative information, allowed ostomates to have a “sense of control” over their situation (13). In this same study, ostomates mentioned “teaching failures” when learning how to care for their ostomy due to unknowledgeable medical providers. Collectively, this group of ostomates described frustration and how negative interactions with their providers made adjusting to their ostomies more difficult. Ostomates face a unique life-changing situation and their first line of support and ostomy-specific information comes from their providers upon receiving their ostomy. Given this, it is crucial that providers deliver proper care and adequate information to new ostomates.
Research Questions
Therefore, the aim of the current study is to answer 2 research questions: (a) Do ostomates receive adequate information and communication from providers while at the hospital? (b) Does the information and communication from hospital providers differ by ostomates’ demographic characteristics?
Method
Sample and Data Collection
We use original data collected from ostomates in summer and fall of 2017. Using a nonprobability approach, we contacted and sent a questionnaire link to 49 ostomy support groups in the United States affiliated with the United Ostomy Association of America (UOAA). The support groups were located throughout the United States. We also posted the questionnaire link on UOAA’s discussion board, which is accessed by ostomates in the United States and abroad. In addition, we recruited through social media sites (Facebook, Twitter, and Reddit) and mailed questionnaires as requested.
The questionnaire was self-administered by respondents. To be eligible to participate in the overall project, respondents had to (a) have an ostomy, (b) be aged 18 or older, and (c) read and write English well enough to complete the survey. Respondents signed an informed consent form prior to having access to the questionnaire. The questionnaire is a mixture of closed-ended and open-ended questions. The questionnaire was pretested with a small group of advanced doctoral students trained in methodology as well as a faculty member with an ostomate. The study and methods were approved by the IRB at The University of Oklahoma.
A total of 393 ostomates filled out the questionnaire, either online (94% of the respondents) or via hardcopy (6%). Of the 393 total respondents, 381 ostomates are included in the analyses; we excluded 12 respondents who had missing data on the variables used in the current analyses. Analyses of the excluded respondents show that those excluded were similar to that of the overall patient characteristics in the sample (data not presented, but available upon request).
Variables
Dependent Variable
To measure perceptions of receiving adequate information and communication from hospital providers in order to make ostomates feel prepared to care for their ostomy at home, we analyzed responses to the open-ended question, “Was there anything that the medical staff could have done to make you feel better prepared to take care of your ostomy at home?” We used open coding to create general coding categories that reflected what the response explicitly stated. Open coding is an initial classification of concepts pertaining to “naming and categorizing…phenomena through close examination of data” (14, p377). Two researchers with advanced methodology training reviewed all responses separately and coded responses into categories using a detailed coding sheet that included definitions for each category. Interrater reliability was computed, and κ scores ranged from 0.46 to 0.99 agreement, which indicates moderate to high agreement. All disagreements were reconciled to achieve 100% agreement.
Responses were coded as adequate or inadequate provider information and communication. A response was coded as inadequate if the respondent wrote a statement conveying a perception of some sort of inadequacy, such as the provider was not nice and had an attitude toward the patient or the patient felt dismissed by their provider. Examples of adequate information and communication include “I received excellent instruction both times…the nurses were professional, kind, and very helpful. I can’t say enough good things about them.” Or “No. Everything was explained while I was still in hospital on a daily basis. Then on my return home I had several home visits over the next three months.” When a respondent left no comment (n = 137, 36%) to the question, we coded the nonresponse as adequate.
Independent Variables
The independent variables of interest include self-reported patient race, gender, educational attainment, age, and income. Race was coded as white or nonwhite. Gender was coded as male or female. Educational categories included (a) completed less than high school or some high school, (b) high school graduate, (c) some college, (d) bachelor’s degree, or (e) postgraduate degree. Age categories included ages (a) 18 to 25, (b) 26 to 35, (c) 36 to 50, (d) 51 to 65, or (e) age 66 or older. Income was determined by the question, “how difficult is it for you to live on your total household income right now?” The income category choices were (a) not at all difficult, (b) somewhat difficult, (c) difficult or can barely get by, (d) very difficult, and (e) extremely difficult or impossible. We coded these responses into a binary outcome: difficult to live on total household income (coded 1) or not at all difficult to live on total household income (coded 0).
Analyses
We first present basic descriptive statistics of the study sample. For unadjusted bivariate analyses, we present 2-way frequencies with a χ2 test of independence. The dependent variable is dichotomous. Thus, we present odds ratios from binary logistic regressions predicting adequate provider information and communication. The models show adjusted (multivariate) analyses for predicted provider information and communication on patient demographics.
Results
Characteristics of the Study Sample
Three hundred eighty-one ostomates are included in this study. Table 1 shows frequencies and percentages of variables describing the patient sample. The sample is largely female (79%) and white (88%). The majority of the sample have some college or higher (83%). More than half (60%) of the ostomates in the sample said that they have a difficult time living on their total household income. A little more than half (59%) of the sample are aged 51 years or older.
Patient Characteristics in the Sample.a

an = 381.
Quality of Information and Communication
Research question 1 asked whether ostomates receive adequate information and communication from providers while at the hospital. We found that about half of the sample (51%) reported receiving adequate information and communication from their medical provider while at the hospital. Whereas 49% of ostomates reported that the information and communication from hospital providers were inadequate.
Patient Characteristics and Quality of Information and Communication
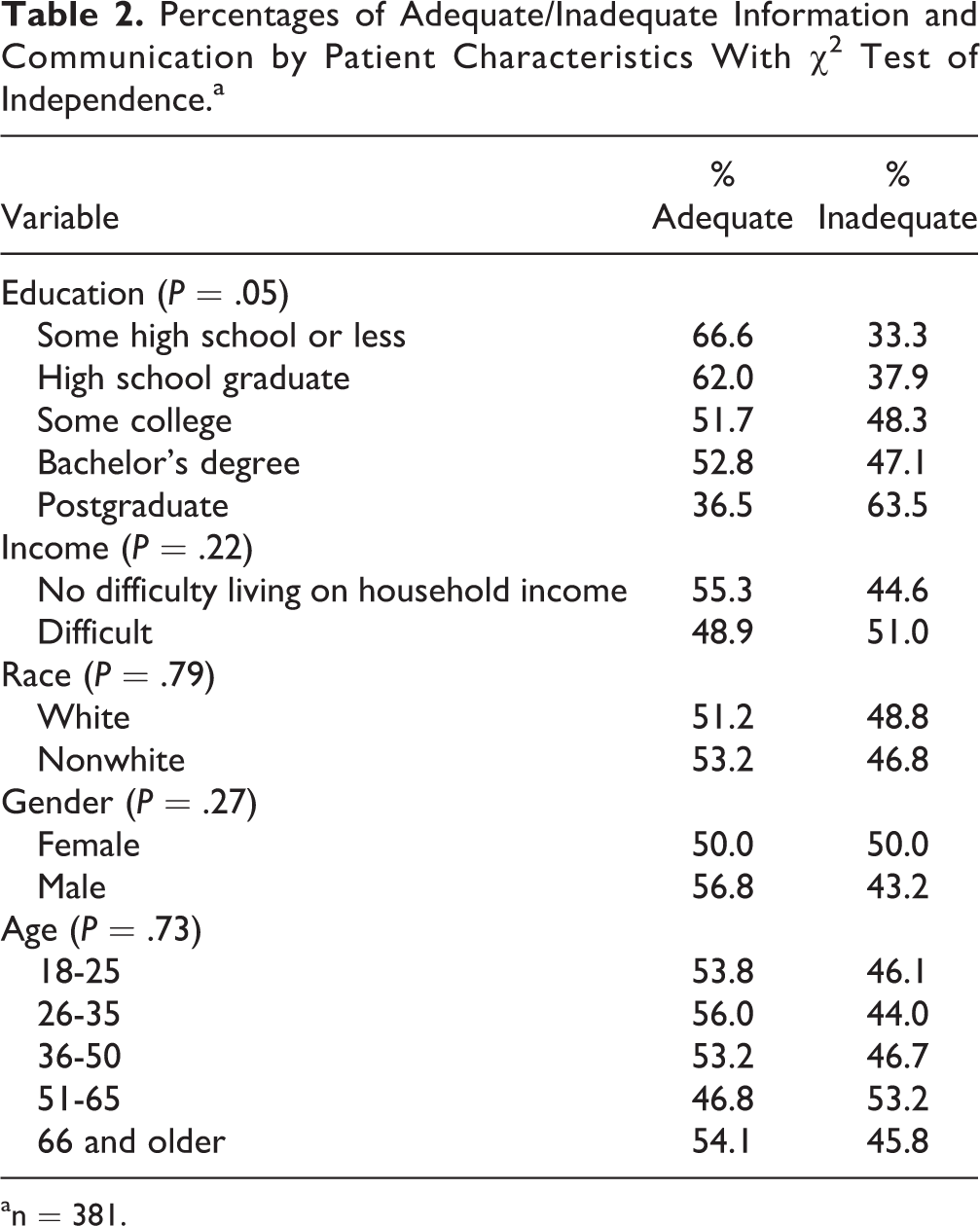
Table 2 presents percentages of provider information and communication by patient characteristics. We present 2-way frequency distributions with Pearson χ2 test of independence for the bivariate relationship between patient demographics and provider information and communication.
Percentages of Adequate/Inadequate Information and Communication by Patient Characteristics With χ2 Test of Independence.a
an = 381.
We found that ostomates with a high school degree or less were more likely to report receiving adequate information from their providers than other educational categories. Specifically, 66.6% of ostomates with some high school and 62% high school educated ostomates perceived adequate information and communication from their hospital providers. Whereas, only 36.5% of ostomates with a postgraduate degree reported receiving adequate information and communication from their providers. Differences in education level were statistically significant at the .05 level. Patient income, race, gender, and age did not achieve significance.
Table 3 presents adjusted (multivariate) analyses for ostomates’ demographics on receiving adequate information and communication from hospital providers. The numbers are odds ratios from binary logistic regressions. We found that patients’ level of education is significantly associated with reporting adequate information and communication received from hospital providers. Particularly, ostomates with a high school degree or less reported receiving adequate information and communication 4 times as much compared to postgraduates. Most notable, the odds of reporting adequate information and communication decreased as ostomates’ level of education increased. We found marginal significance for the effect of income on provider communication. Specifically, the odds of lower income ostomates were less likely to report receiving adequate information and communication compared to higher income ostomates (P < .10). Lastly, race, gender, and age did not achieve significance, which is consistent with the bivariate relationships shown in Table 2.
Logistic Regression With Odds Ratios of Ostomates’ Demographics on Receiving Adequate, Information, and Communication From Hospital Providers.a

Abbreviations: OR, odds ratio; SE, standard error.
an = 381.
Discussion and Conclusion
In this study, we took a quantitative approach to examine whether ostomates perceived adequate information and communication from hospital providers in order for ostomates to feel prepared to care for their new appliance. We found that when ostomates leave the hospital with a life-altering appliance, about half of the sample perceived some sort of inadequacy with their care. This finding confirms previous studies on ostomates’ initial interactions with providers; specifically, Sun et al (13) found that ostomates expressed that nurses lacked knowledge of ostomy care. Only 51% of ostomates rated the information and communication from providers as adequate. This finding is quite low compared to other measures of quality of care from providers, such as ratings of patient satisfaction (15), and patient understanding of medical information (16).
We also found ostomates’ level of education and income levels matter more for provider information and communication than other patient demographics. For instance, patient race, gender, and age were not significantly related to information and communication. These findings suggest that while patient race, gender, and age matter a great deal within other medical contexts, such as primary care visits, this does not seem to be the case for ostomates in hospital settings. For instance, primary care visits tend to be brief, and providers’ initial impressions of patients have been shown to influence provider communication (17). Hospital encounters can span several days; thus, this contradictory finding could be due to the complexity of hospital visits and the length of time spent with hospital providers.
We found that level of education was significantly related to whether ostomates perceived adequate information and communication from their hospital provider. Notably, we found that as ostomates’ educational attainment increased, their perceptions of receiving adequate information and communication decreased. Ostomates with lower educational attainment reported receiving adequate information and communication up to 4 times more than postgraduate degree holders. The inverse effect of education is possibly related to an ostomy patient’s health literacy level. Health literacy is the “degree to which individuals can obtain, process, and understand the basic health information and services they need to make appropriate health decisions” (18, p6). Studies show that health literacy is related to educational attainment (19). Perhaps ostomates in the current study with lower educational attainment reported receiving adequate information and communication because of their limited health literacy. This suggests a limited understanding of the health information from their medical provider, which may lead them to assess the information and communication from their provider as sufficient.
The findings must be interpreted with limitations in mind. First, the sample was largely white and female. We recruited our sample largely from ostomy support groups. It could be that white female ostomates participate in ostomy support groups more than male ostomates and nonwhite ostomates. A larger male and nonwhite ostomate sample could shed light on different hospital experiences. Second, the sample was a nonprobability sample. Therefore, it is difficult to discern whether the findings can extend to other ostomates’ experiences with their medical providers. Third, we used a retrospective design to determine whether new ostomates receive adequate information and communication from providers. Retrospective measurements have the potential to introduce recall bias. It is possible our participants remembered “their former state as better or worse than it actually was” (20, p112). Although, “events of emotional significance” are more likely to be recalled accurately than more mundane events (21).
Lastly, we measured adequate information and communication by including nonresponses to the question: “was there anything else that the medical staff could have done to make you feel better prepared to care for your ostomy at home?” By including nonresponses, we assumed that the ostomate perceived adequate information and communication from their provider. However, we recognize the possibility of other reasons why someone would not leave a comment, such as feeling incapable of articulating his or her thoughts or less able or willing to answer. To address this potential limitation, we ran analyses on ostomates who left no comment versus those who did leave a comment. We found no significant differences in ostomate demographics between those who commented or not. In addition, we conducted an analysis using only patients who left an explicit comment that indicated adequate or inadequate communication from the provider. The results did not change substantively; the significant effect for education was still present for the lowest educational category.
Overall, this study demonstrates that hospital provider information and communication can improve for new ostomates. Future research is needed to assess what is driving ostomates’ perceptions of adequate provider information and communication, such as the hospital where the ostomate had their surgery, the method of instruction (if any) that was given, whether the specific instruction helped or hindered the ostomates’ ability to care for their new appliance. Also, future studies need to include possible mediating and moderating variables, such as complications since ostomy surgery, the type of ostomy, reason for the ostomy, and time since surgery. To explore whether medical characteristics changed the relationships found in the models presented, we included the type of ostomy (ileostomy and all others), reason for the ostomy (cancer and all others), and time since surgery (ranged from 1 year to 65 years since surgery), and all relationships were the same as the current full model (analyses not shown).
Hospital care is different from primary care visits as primary care visits generally provide acute care, whereas hospital care spans over several days. As such, the interaction between hospital providers and patients is more complex and has unique implications on patient health outcomes, especially for ostomates. Understanding mechanisms that influence the interaction between providers and ostomates not only has the potential to improve hospital processes and decrease costs but also positively impact ostomates’ adjustment to their new appliance.
Receiving an ostomy is a life-altering procedure. Individuals with an ostomy may experience not only disruption in their lives but feelings of stigma and shame. Medical providers are the initial and most important source of care for patients receiving an ostomy. Therefore, providers are in a unique position to help patients maneuver this new way of life and perhaps help alleviate the negative feelings ostomates sometimes feel. Taken together, this study provides pertinent information in an effort to guide nursing care, training and practice, and hospital processes.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was funded by a “Graduate College Foundation Fellowship from the Department of Sociology and the Graduate College at the University of Oklahoma” to Leslie Miller. The funding does not impact the study in anyway.
