Abstract
Improving patient satisfaction scores has become a key focus of health-care organizations nationwide but can be a struggle for community hospitals with constrained resources, and particularly challenging for hospitalist programs due to provider variance and turnover. Using the framework of appreciative inquiry, we implemented a multipronged intervention including a rounding model whereby hospitalist leaders rounded on patients and relayed commentary back to their hospitalist providers. We communicated positive feedback preferentially over negative feedback to the entire hospitalist group through regular communication. Providers were encouraged to employ best practices including sitting with the patient, reviewing recommendations using teach back, and providing business cards. Scores improved in the physician communication category by approximately 1% annually from fiscal year 2015 through 2018, with our percentile rank improving 35 percentile points during that time. These findings indicate that a multifaceted approach including best practices is associated with improved patient experience regarding communication with physicians.
Keywords
Introduction
Higher patient experience scores, best practice initiatives, and greater staff responsiveness have been associated with perceptions of better quality care (1), better overall outcomes (2), and lower readmission rates (3). Smaller community hospitals may struggle with matching the patient experience scores of larger, more resourced tertiary care facilities given greater restraints on resources. Community hospitals can therefore benefit from improving patient satisfaction using interventions that are evidence-based, cost-effective, and easy to implement within an organization. In 2015, Lawrence General Hospital convened a patient experience committee to redefine strategies to improve patient experience. Since then, the committee has been engaged in a multipronged effort to improve patient satisfaction relying on the framework of appreciative inquiry. Measuring success in improving patient satisfaction scores is possible via the Press Ganey survey distributed to all patients of hospitals throughout the United States following discharge. This includes specific questions regarding physician communication.
Examples of individual initiatives the Lawrence General patient experience committee has launched since 2015 include implementation of hourly rounding by nursing, trials of bedside multidisciplinary rounding, senior leadership rounding on frontline staff, and efforts to better serve Spanish-speaking patients. As a result, the hospital already began to see significant gains in the score of the Press Ganey survey’s broad question of whether patients would recommend the hospital (improvement of 8%) from the beginning of 2015 through the end of 2016 (4).
Physician engagement, and specifically, improving communication with physician ratings became a priority for this committee. The hospital had previously shown that providing discharge instructions using a physician and nurse-centered transition record template can improve patient perceptions with the discharge process (5). The hospital sought out a similarly cost-effective intervention in which to improve patient satisfaction with physician communication. It has been previously shown that simple interventions can have a statistically significant effect on patient satisfaction scores, for example, physicians who handout business cards to patients are perceived to be more effective communicators, have greater medical expertise, and provide higher quality medical care (1). Real-time targeted feedback and regular individualized review of patient experience scores have also been proven effective in improving patient experience scores across an organization (6,7). The hospital’s approach focused mainly on these simple interventions.
Methods
Setting and Patient Population
Lawrence General Hospital is a private, nonprofit community hospital (186 inpatient beds) located in the Merrimack Valley serving Northeastern Massachusetts and Southern New Hampshire, but primarily the city of Lawrence. Lawrence is characterized by having a very large number of residents living below the poverty line (28%), a large immigrant Hispanic population (76%), and having comparatively low levels of education (31.5% of the population does not have a high school education) (8). The city also has a serious housing shortage and is disproportionally affected by the opioid epidemic.
In 2015, Lawrence General hospital instituted a multipronged program engaging with physicians across the hospital, with the goal of improving the patient experience. Patient experience initiatives were discussed at departmental meetings in the 3 departments that together serve nearly all our inpatients (internal medicine, family medicine, and general surgery), but as the majority of patients are served by the general medicine hospitalist program (70%), the primary focus was on the hospitalist group. This included the dissemination of information at quarterly meetings where patient experience, quality/patient safety, and operational goals were rolled out.
Concept of Appreciative Inquiry
Appreciative inquiry is a method for implementing organizational change that advocates an emphasis on studying and promoting what is going well within an organization, with the goal of implementing change without relying on incentives, coercion, or persuasion. The core concept of appreciative inquiry is to decrease the focus on problem-solving techniques and rather affirm strengths and successes within an organization. This process energizes people, inspires positivity, and encourages creativity. It is an approach to organizational change that “utilizes positive inquiry…to determine what individuals and teams appreciate, or value, to discover the best of the organization.” (9) One key principle of appreciative inquiry is the idea that “organization life is expressed in the stories people tell each other everyday, and the story of organization is constantly being co-authored.” (10) Specific topics chosen for emphasis by leadership can have an impact on organizational direction simply from the act of bringing them to regular attention.
Intervention
In response to the problem of low physician communication scores, the hospitalist program implemented a rounding model, whereby senior physician leaders visited the medical floors to talk with patients who were not admitted to their service about issues regarding physician communication. Such leadership rounding has previously been shown to be effective when employed by nurse leaders (11). The goal was to identify themes, both positive and negative, and potential interventions. Another goal was to provide real-time feedback to individual providers, in the spirit of appreciative inquiry. Rounders would share positive comments with the entire hospitalist service via e-mail or at quarterly meetings, and we would relay any negative comments to individual providers privately. It was hypothesized that this would improve patient experience scores of individual providers without stigmatizing those who performed poorly.
Throughout the first year of the intervention, rounding was sporadic, and rounders were not always reliably recording feedback from patients or relaying them back to providers. To address this problem, the hospitalist program implemented a regular rounding schedule in order to track participation and standardize the patient interview process. An online survey site was employed, hosted by Qualtrics—an experience management company, to record patient commentary electronically. For each patient visited, rounders would, in conversational style, try to answer responses to 4 specific questions, whether the patient: (1) knew his or her provider, (2) had been given a business card, (3) understood the plan of care, and (4) was satisfied that physicians communicated well with them. These questions were formulated based upon input from multiple clinical and administrative leaders experienced in patient satisfaction as well as assistance from Press Ganey advisors. Consent to participate in the project was verbally obtained prior to each interview.
Because early data indicated that as few as one-quarter of patients had their provider’s business card, the hospitalist leadership specifically wanted to emphasize this issue. Rounders sought to highlight the importance of handing out a business card to patients and family members in much of their communication. The hospitalist program printed new business cards featuring photographs of individual providers and distributed them to all hospitalists. A summary of our interventions is included in Figure 1.
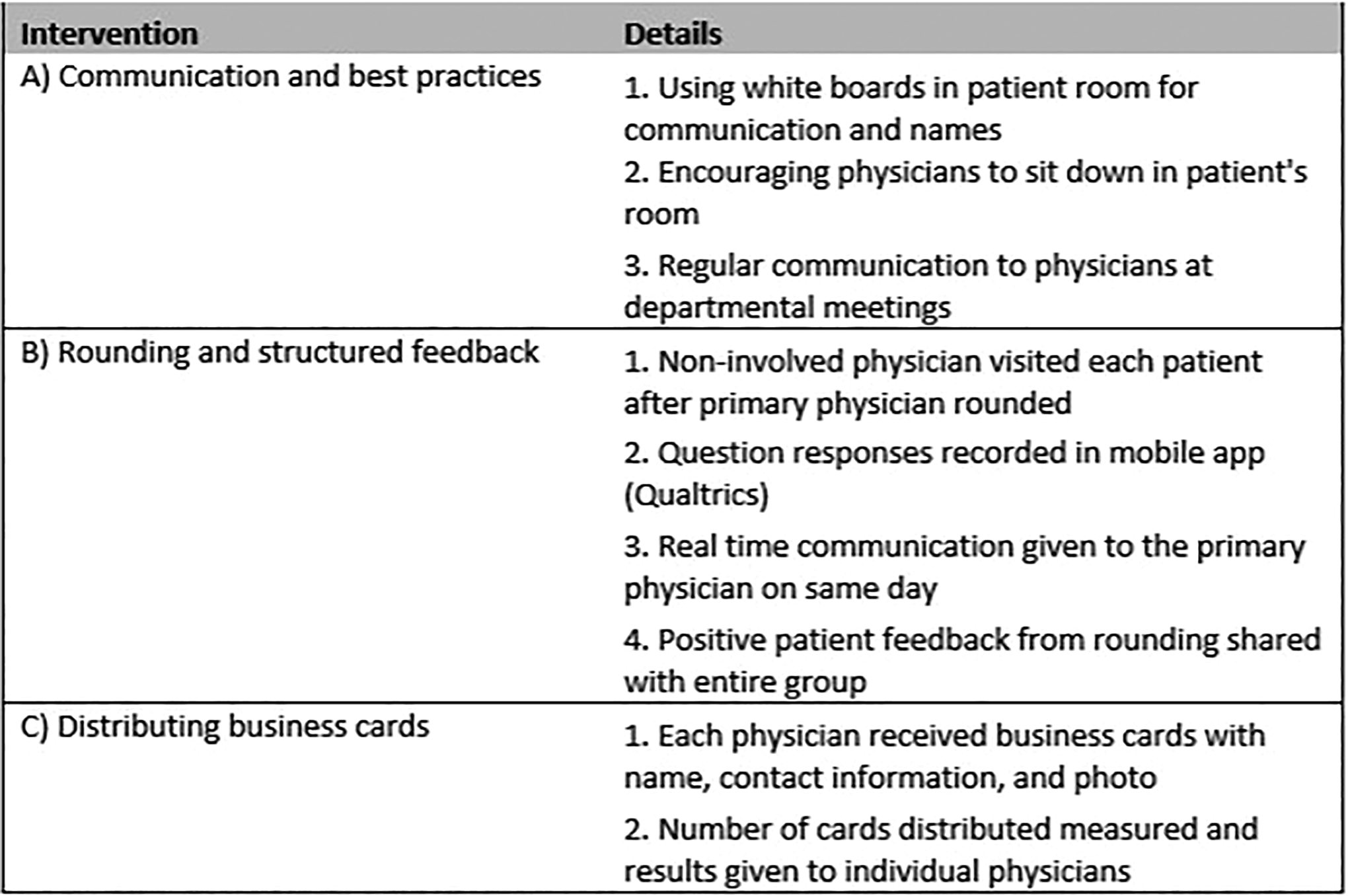
Summary of interventions.
Survey Data
The data in this project represent Lawrence General Hospital’s Press Ganey Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) responses from October 1, 2014, to August 18, 2018. The project focused on data from the “Physician communication” section of the Press Ganey Inpatient Survey. Surveys were sent to all discharged patients. Survey response ranged from 1025 to 1443 surveys returned annually. No responses were excluded and partially completed surveys were included. Fewer than 2% of surveys were returned with incomplete answers in this section. The specific questions asked in the survey were (1) whether physician explanation was understood, (2) whether physicians listened carefully, and (3) whether physicians treated patients with respect. This was the primary data used in this project.
Results
The primary outcome was responses to the Press Ganey HCAHPS survey beginning with Lawrence General Hospital’s fiscal year 2015 (defined as starting October 1 of the preceding year) through the most recent complete year, 2018. Responses to the physician communication questions saw a sustained increase of approximately 1% or more on average annually, rising from 76% in 2015 to 81% in 2018 (Figure 2). When measured as a percentile against the national average, this equated to an increase from 17th percentile to 52nd percentile over the same period. Breaking down responses by specific question, there was an increase from 71% to 76% for physician (MD) explanations understood, an increase of 74% to 80% for MD listened carefully, and an increase from 83% to 87% for MD treated with respect (Figure 3). The hospital score also saw an increase from 67% to 69% during the same period, although this increase was less significant than the increase in physician communication scores P < .001. To confirm the significance of the increase in physician communication scores versus the overall hospital score, we compared the 24-month period of 2017 to 2018 to the 24-month period of 2015 to 2016, and found that there was a statistically significant increase in physician communication scores, P < .05, versus the total hospital score, P = .402.

Comparing Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) score of overall hospital (9 domains) and communication with doctors.

Breakdown by individual question.
Discussion
Improving patient satisfaction scores can be a daunting challenge, particularly for smaller, less-resourced community hospitals. Lawrence General Hospital has shown that statistically significant increases in the domain of communication with doctors can result from simple, multipronged interventions that engage both the hospital leadership and individual providers. Above all, a focus on changing culture across an organization is crucial—there is a statistically significant relationship between an organization’s culture and patient experience scores (12). This hospital was able to accomplish this with its physicians through regular communication, continuously emphasizing examples of best practices—such as sitting with the patient, reviewing recommendations using teach back, and providing business cards—and their positive impact on the patients’ perceptions of both individual providers and the overall quality of care.
A key factor in this success was the hospitalist program’s ability to employ a rounding model involving senior leadership, whereby it ensured that all patients we interviewed knew their provider, had received their provider’s business card, understood the plan of care, and were satisfied with physician communication. It was able to ensure regular rounding through a rounding schedule and a means of recording our data electronically. By continually asking these same questions and providing feedback to providers, this intervention was able to change behaviors.
Engaging patients and keeping them loyal to a health-care organization is becoming increasingly important in an era where relying purely on volume for profit is giving way to value-based care, and retaining patients becomes of greater importance (13). With better patient satisfaction scores being linked not only to better patient retention, but also to better health-care outcomes, lower malpractice risk, and even lower physician turnover (14), it is incumbent upon community hospitals to implement strategies for improving patient satisfaction that are cost-effective, engaging of both leadership and individual providers, and focused on changing the culture of the organization. Lawrence General has shown that such a strategy can have a statistically significant impact on patient satisfaction scores.
Footnotes
Authors’ Note
Pracha Eamranond is now affiliated with Saint Francis Hospital and Medical Center, Trinity Health Of New England, Hartford, CT, USA.
The authors whose names are listed above certify that they have no affiliations with or involvement in any organization or entity with any financial interest, or nonfinancial interest, in the subject matter and materials discussed in this manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
