Abstract
National Quality Improvement Project (NSQIP) semiannual reports (SARs) revealed high observed to expected ratios for venous thromboembolic events (VTEs) on the surgical service. Press Ganey scores identified an area of particular weakness in shared decision-making in patient care. Patients reported little to no participation in shared decision-making. A performance improvement project was developed with a 2-fold objective: decrease the percentages of patients sustaining VTE through adequate screening and prophylaxis (VTEP) and to engage patients in shared decision-making to accept VTEP through enhanced patient-centered discussions and education on the risks and benefits of VTEP. A clinical pathway was developed to implement VTEP using a standardized risk assessment tool. Patient-centered discussion introduced VTEP and impact on perioperative safety. Results included telephone survey, NSQIP SARs, and Press Ganey patient experience survey. Using NSQIP data and a pathway developed for both VTE risk assessment and patient engagement, the authors observe immediate improvements in patient experience and decreased rates of VTE.
Keywords
Introduction
Venous thromboembolism (VTE) can be comprised of a deep vein thrombosis (DVT) and/or a pulmonary embolism. It is estimated that approximately 900 000 people are affected by VTE annually in the United States (1), with hospitalized patients forming the majority of affected individuals as they experience a 100-fold incidence of VTE when compared with the general population (2). Furthermore, VTE can be found in approximately 80% of surgical patients who were not placed on thromboprophylaxis (3). Although several reports from randomized controlled trials have demonstrated the effectiveness and safety of thromboprophylaxis in the prevention of VTE (4), several studies have shown that these interventions are underutilized in hospitals (5,6). The increased morbidity and mortality associated with VTE highlights the great importance of treating and preventing VTE.
In May 2013, Jacobi Medical Center joined the American College of Surgeons National Quality Improvement Project (NSQIP) (7). The NSQIP measures and tracks risk-adjusted surgical outcomes and gives unbiased comparisons of results between hospitals. Data from NSQIP indicated that our facility had a higher than expected incidence of venous thromboembolic events, with multiple surgical subspecialty services needing significant improvement (Figure 1). Concurrently, our corporation added Press Ganey scores to the hospital scorecard performance indicators. These scores demonstrated that one area of particular weakness was in shared decision-making in patient care.
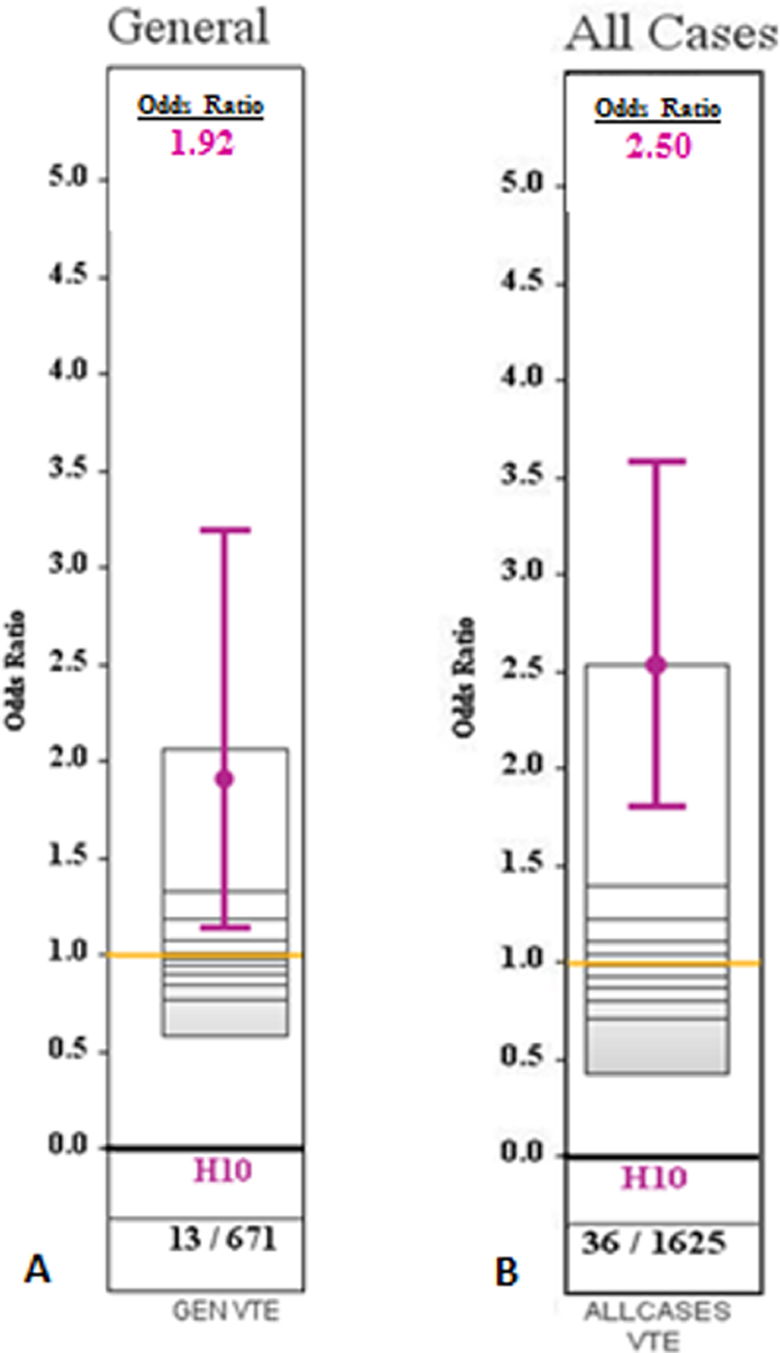
(A) Baseline NSQIP O:E, division of general surgery. (B) Baseline NSQIP O:E, all surgical divisions.
A recent study aimed at understanding patient perceptions of VTE prevention found that patients typically had poor understanding about VTE, the severity of postop VTE, and VTE prevention (8). Kahn et al in a recent review which examined system-wide interventions that contributed to the implementation of VTE in surgical patients reported that the alerts were associated with more patients receiving prophylaxis (4). Their findings emphasized the importance of both patient understanding and patient compliance in appropriately addressing these problems.
Our objective was 2-fold: first to decrease the percentages of patients sustaining VTE through adequate screening and prophylaxis (VTEP) and second to engage patients in shared decision-making to accept VTEP through enhanced patient-centered discussions and education on the risks and benefits of VTEP. It was hypothesized by the authors that this shared decision-making would lead to improved patient experience.
Methods
Formation of VTEP Protocol
Prior to data collection, a Quality Improvement (QI) program was created. Given that corrective action for implementation of VTEP program would cross multiple disciplines, a comprehensive steering committee was formed. Representatives of the departments of Surgery, Perioperative Nursing, and Anesthesia convened and performed a gap analysis. The group reviewed the literature regarding VTEP and evaluated existing risk assessment tools. The General Surgery service was selected for the study. The Caprini VTE Risk Factor Assessment Tool (9) was chosen to assess patient risk for VTE and a process was developed for risk assessment and administration of VTEP. During monthly Operating Room (OR) committee meetings, education was provided to the members of the departments of surgery, anesthesia, and nursing on Caprini risk assessment, VTEP, and patient-centered discussions. Special attention was paid to the frontline surgical physician assistants (PAs), who would be responsible for ordering VTEP.
Patient Selection and Assessment
This was a prospective interventional study of all patients undergoing surgery in the general surgery division between November 2016 and October 2017. All patients undergoing general surgery procedures at our institution were identified as potential candidates for VTEP and score for VTE risk preoperatively. Exclusion criteria are patients from non-general surgery service specialties (neurosurgery, ophthalmology, otolaryngology) and patients with contraindications for administration of VTEP: active bleeding, ingestion of oral anticoagulants, administration of glycoprotein IIb/IIIa inhibitors, and history of heparin-induced thrombocytopenia. Although some cases were day cases, not all with bleeding risks, the final decision to give VTEP was ultimately determined by the attending surgeon based on risk of VTE versus risk of postoperative bleeding. The risk of VTE far outweighed the risk of postoperative bleeding and no surgeon refused to give VTEP for high-risk patients. Using the Caprini score scale (Figure 2), a risk factor score was generated by nursing during the preoperative assessment. The score was recalculated the day of surgery by surgical PA staff trained in VTEP. Patients with total risk factor scores ≥3, reflecting moderate- to high-risk levels, indicating a 20% to 40% incidence of DVT, were identified. An alert was attached to the patient’s chart to indicate a moderate- to high-risk patient requiring VTEP.

Risk assessment tool.
Pre- and Postoperative Patient Discussion and Interventions
The VTE alerts in turn prompted 2 separate discussions between surgeon, nurse, and patient regarding safety and VTEP. The initial discussion was done by phone by perioperative nurses during preadmission evaluation. The second discussion takes place face-to-face with the patient on the day of surgery in the holding area by both the surgeon and anesthesiologist. The patients were asked to describe their knowledge of blood clots. The risks and benefits of VTEP were explained to the patient after which patient comprehension was evaluated. The surgeon was then informed of risk assessment for final approval, and if warranted, preoperative VTEP was administered at recommended doses in the same day surgery holding unit. To facilitate discussion and to limit variation in message to patient, a scripted dialogue was developed for both assessment and follow-up with focus on patient-centered discussion (Figure 3). Telephone surveys were conducted 3 to 5 days postoperatively to assess patient understanding, perception, and experience. Outcomes measures included DVT, VTE, and patient experience with special attention to shared decision-making. Methods are summarized in Figure 4.

Script.

Clinical pathway.
Statistical Analysis
Patient satisfaction was assessed in 2 different ways. First, by a scripted telephone survey and second by the Press Ganey Ambulatory surgery satisfaction scores filtered for the general surgery specialty services.
The percentile ranking compares our institution to all hospitals in the Press Ganey (PG) database (1621 hospitals), our institution to the other H+H facilities (11 hospitals), and our institution to like hospitals in NY State (70 hospitals). Both DVT and VTE were assessed by using observed to expected ratios (O:E). The VTEP initiative has since been extended to include all surgical services, including orthopedic surgery (initially with the highest VTE rate).
Results
Gap analysis revealed a high degree of variability regarding VTEP on the surgical service with lack of both a standardized risk assessment tool and defined process for VTE risk assessment. Of 109 patients prior to the VTEP intervention, only 4 patients recalled having a conversation with their doctor before surgery about the following: risk of blood clots during their operation, need for VTEP, and patient safety being a top priority. The remaining 105 patients did not recall any conversation on any of these 3 topics. After implementing the VTEP project on the General Surgery Service, the observed to expected ratio (O:E) for VTE decreased from 1.92 to 1.07. The VTEP initiative has since been extended to include all surgical services, including orthopedic surgery (initially with highest VTE rate). Although O:E has not normalized, a significant reduction in VTE is shown on the general surgery service. The absolute rate decreased as the absolute number of VTE events decreased across all surgical services (Table 1, Figures 5 and 6).
Observed to Expected Ratios for General Surgery Division and All Divisions.


Results, division of general surgery pre (A) and post (B) VTEP project implementation.
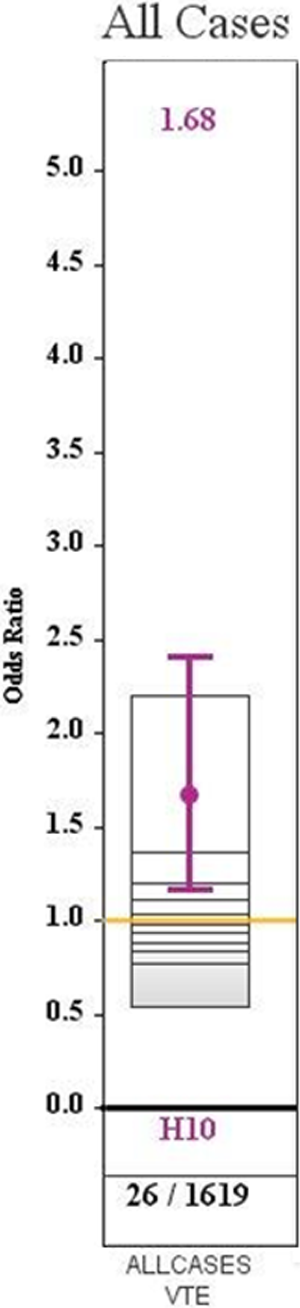
Results, all surgical divisions.
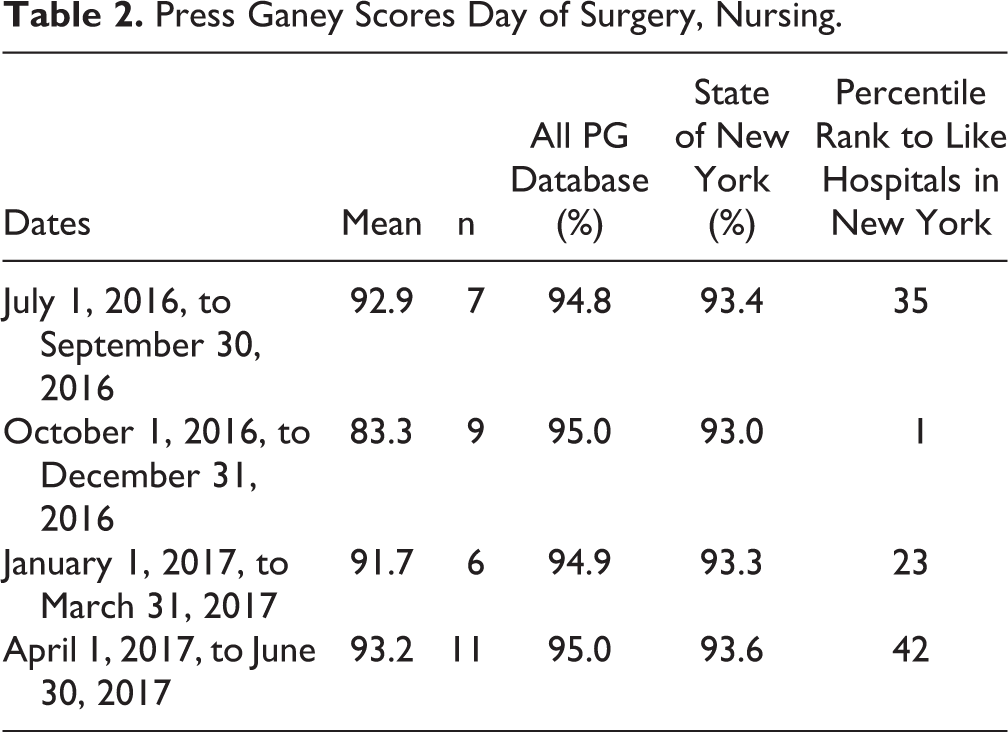
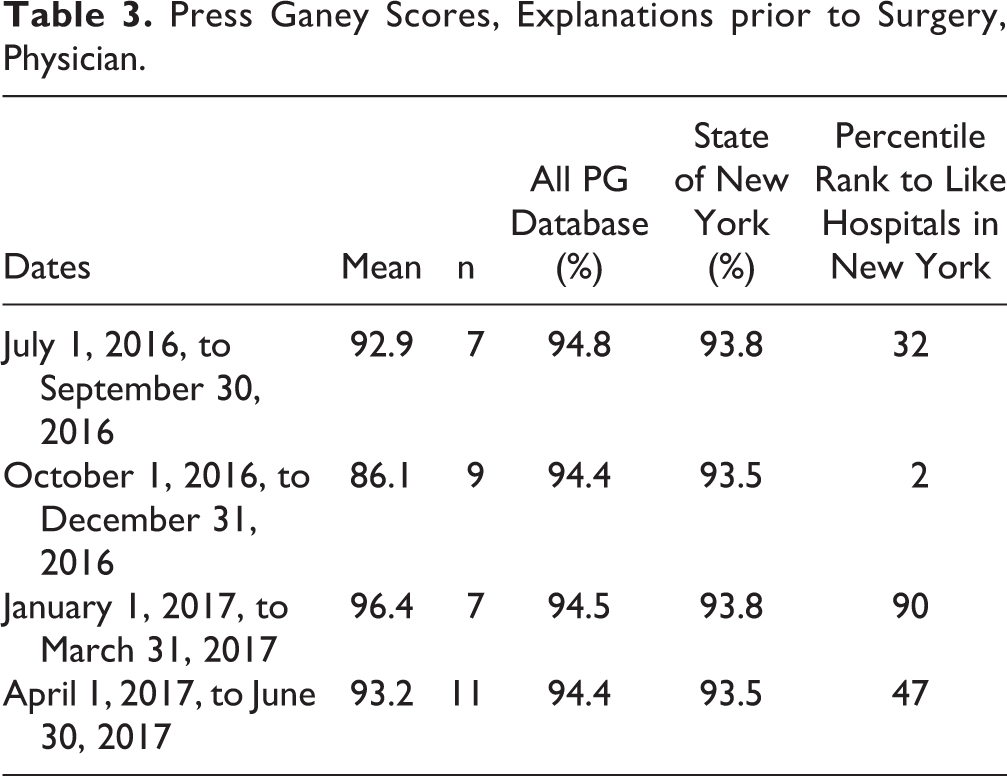
Data through 1 year, November 2016 to October 2017, were studied. Of the 186 patients screened for VTEP, there was a 96% (179/186) follow-up rate in 6 months. Of the 186 patients, 89% of the patients in the study were deemed high risk. Of this group, 94 received preoperative VTEP. Telephone surveys were attempted for all 186 patients. Thirty-nine surveys were unable to be completed for the following reasons: disconnected phones, incorrect phone numbers, patient refusals to participate in the survey, and failure to return calls. Of the patients for whom the surveys were completed, 99% (145/147) of patients reported that the indications, risks, and benefits of VTEP were explained well or very well. Of these patients, 99.5% (146/147) felt that safety and well-being were a priority based on preoperative discussions. There were no incidences of VTE in this cohort. The Press Ganey Ambulatory surgery satisfaction scores filtered for the general surgery specialty services found our institution to be well above the target 50th percentile. There is no significant difference on PG results when comparing pre- and postimplementation of the VTEP program with satisfaction scores in the areas that most closely reflected perioperative performance. Press Ganey Ambulatory surgery satisfaction scores from the following 2 categories are found in Tables 2 and 3, respectively: information on the day of surgery by nurse (Table 2) and explanations prior to surgery by physician (Table 3).
Press Ganey Scores Day of Surgery, Nursing.
Press Ganey Scores, Explanations prior to Surgery, Physician.
Discussion
In this study, we assessed VTE, DVT, and patient experience after designing and implementing a QI program by analyzing O:E of VTE, patient satisfaction (telephone survey), and Press Ganey scores. We found that on the General Surgery Service O:E decreased, the absolute number of VTE events decreased, approximately 99% of high-risk patients felt that the risks and benefits were well explained and that there was no incidence of VTE in this cohort. The Press Ganey Ambulatory surgery satisfaction score found this institution to be well above the target of 50th percentile; however, there were no significant differences on PG results when comparing pre- and postimplementation of the VTEP program.
Team engagement is critical to success in patient engagement. It affects outcome data as well. Working as a collaborative team with surgeons, anesthesiologists, and nurses; input and ideas from all disciplines have led to improved patient outcomes and decreased incidence of VTE since program implementation. At the outset, there were several obstacles in instituting this initiative: lack of standardized VTEP protocols, lack of standard risk assessment tools, and a belief system that VTEP may cause bleeding intraoperatively. Once the initial obstacles of program implementation were overcome, a greater than 95% response rate from patients reported that safety and well-being are a priority based on preoperative discussions on VTEP. The VTE improvement soon followed in NSQIP reports.
The VTEP initiative has since been extended to include all surgical services, including orthopedic surgery (initially with the highest VTE rate). Based on our data, the Orthopedic surgery team has made modifications to VTEP dosing for their patients. Consequently, the Orthopedic service has recently begun to see improvements in their VTE O:E ratio. The authors have recently expanded the project to include the gynecology service.
The PG results have not reflected the improved immediate survey results for several reasons. Different aspects of patient care determine patient experience. The ability of clinicians to empathize, respect the preferences of patients, and include them in decision-making are much harder to quantify than functional aspects of care such as timeliness of care, clean and safe environments, and effective coordination of services. However, both aspects of care are incorporated into PG data. Telephone survey targeting the conversation regarding VTEP shows an improvement that relates specifically to patient-centered discussions on VTEP.
Although scripted dialogue was prepared, measures used to capture patient satisfaction still reflect interpersonal care experiences, such as patient–provider communication, which represent a unique dimension of quality. A telephone survey done within 3 to 5 days of hospitalization does align with prior studies that show positive associations with outcome measures (10 –12). One drawback is the average lag between measured experience feedback and outcome of 3.9 years (13). In addition, the PG questions are much vaguer and may reflect or are biased by total day of surgery experience.
Numerous studies have demonstrated significant positive relationships between patients’ perceptions of their care experiences and outcomes (14). Patient experience is positively associated with clinical effectiveness and patient safety and supports the inclusion of patient experience in quality initiatives (15) In addition, measures of health-care quality such as compliance with recommended treatment, better clinical outcomes, improved patient safety, and more efficient health care utilization correlate positively with patient satisfaction (16). Our findings offer further support for these studies. As we found, VTEP patient-centered discussion and shared-discussion did affect patients’ perceptions of their care and their outcomes.
There are limitations to such a study. The actual quality of the individual interactions is difficult to quantify and may vary significantly from provider to provider. Indeed, interaction may vary from day to day with an individual provider. Further, the actual understanding of the medical information by the patient cannot be quantified. However, the Ask-Tell-Ask paradigm (17) was developed for collaborative communication which included assessing the patient’s existing knowledge on VTE and VTEP before sharing information on VTEP, as patients were not asked to reiterate the risk and benefits of VTEP. The level of understanding and correlation with outcomes is similarly not quantifiable. While the authors are satisfied with the integrity of the NSQIP data in showing overall institutional improvement, the authors acknowledge that NSQIP is sampling methodology and not all cases may have been captured. Moving forward, the authors seek to develop a randomized multi-institutional study.
Conclusion
Using NSQIP data and a program developed for both VTE risk assessment and patient experience, the authors observe immediate improvements in patient satisfaction and no VTE. Although there are unresolved methodology related to the measurement and interpretation of patient experiences regarding survey content, and timing of survey administration, we believe quality care and patient engagement can improve the patient experience and outcomes. Patient-centered discussions have had positive impact on patient’s perioperative experience regarding VTEP and safety as a top priority.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
