Abstract
Introduction:
Muslim hemodialysis (HD) patients are motivated to practice fasting in Ramadan. Health-care providers may be unable to make a recommendation based on lack of evidence. The aim of the present study was to investigate patients’ and medical professionals’ opinion toward fasting in 4 HD centers in Egypt as well as the impact of physicians’ attitude on their patient behavior.
Materials and Methods:
This observational multicentric study was conducted on 161 patients undergoing HD and 23 physicians in 4 HD centers in Egypt just after Ramadan 1438 Hijri. Patients’ demographic characteristics as well as any associated comorbidities were recorded. Patients and physician were interviewed and were asked about their opinion toward fasting in HD patients and any experienced complications during fasting.
Results:
Eighty-one (50.3%) patients of the studied HD patients practiced fasting in Ramadan. No statistical difference was observed between fasting and nonfasting groups regarding age, gender, and duration of HD. Eighty percent of patients reported no complications. Fifteen (65.2%) physicians support the opinion that HD patients are capable to fast with precautions. There was a significant variation in fasting frequency among HD patients in the studied centers with a significantly low fasting frequency observed in the third center (10.5%). Most physicians from this HD center adopted that HD patients should not fast.
Conclusion:
HD patients were keen to practice fasting in Ramadan and were to a considerable extent capable of completing this Islamic worship. Patient decision seems to be affected by their physician’s opinion. Absence of clear recommendations to guide fasting in Ramadan in HD patients as in diabetic patients makes permission or prohibition of such practice unjustified.
Introduction
Islam has 5 primary obligations, or pillars of faith, that are considered mandatory for all believers. Fasting during the holy month of Ramadan is the fourth pillar of Islam. It is a time-restricted feeding; abstention from eating, drinking, and other sensual pleasures is obligatory from dawn to sunset.
Although the elderly people who cannot tolerate fasting, the mentally disabled, and the sick person whom fasting might possibly aggravate their condition are exempted from this religious obligation (1), a significant number of ill patients, including hemodialysis (HD) patients, decide to fast. Previous studies observed different frequency of fasting among patients on maintenance HD. Imtiaz and colleagues reported that the frequency of fasting in Ramadan was 13.5% in Pakistani HD patients (2). In another study conducted in Saudi Arabia, 64.1% of the included 635 HD patients fasted (3). The variation in the results of these studies could generally be ascribed to different personal, social, and environmental influences. Personal views and experience of the treating physicians may also have an impact on patients’ motivations toward fasting as patients usually seek the opinion of health professionals on an individual basis. However, HD health-care providers may be unable to make a recommendation due to lack of evidence-based information. Consequently, every physician would have his own attitude built on personal conviction and experience that may challenge patients’ motivation toward fasting. However, the magnitude of the effect of the physicians’ personal opinion and attitude toward fasting of their HD patients has not, to the best of our knowledge, been systematically evaluated.
The current observational study was designed to investigate the opinion of the patients and health-care professionals toward fasting in 4 HD centers in Egypt. The impact of physicians’ attitude on their patient behavior toward fasting was assessed, and the complications noticed by the patients and health-care providers during Ramadan fast were reported.
Materials and Methods
This cross-sectional study was conducted on 161 Muslim patients undergoing HD and 23 physicians in 4 HD centers in Egypt just after the month of Ramadan 1438 Hijri. The investigated centers comprised Mansoura Nephrology and Dialysis Unit (center 1), Mansoura Military Hospital Dialysis Unit (center 2), Damietta General Hospital Dialysis Unit (center 3), and Damietta Specialized Hospital Dialysis Unit (center 4). The study protocol was approved by the local institutional ethical committee. Patients’ demographic characteristics as well as any associated comorbidities were recorded. Patients and physician were interviewed separately by medical students and were asked about their opinion toward fasting of HD patients. Patients who fasted were also asked about any experienced complications during fasting. On the other hand, the treating physicians were asked to report the observed complications in patients who practiced fasting.
The data were eventually collected from the contributing centers, recorded in an excel sheet, processed, and statistically analyzed.
Statistical Analysis
Data analysis was performed by Statistical Package for Social Science (SPSS) Version 16 (Chicago, Illinois). Descriptive analysis of quantitative data was presented in the form of mean and standard deviation or median and (minimum-maximum) for Gaussian and non-Gaussian distributed variables, respectively. On the other hand, the qualitative data were presented in numbers and percentages. The significance of differences between 2 or more continuous variables were assessed by using independent samples t test or 1-way analysis of variance, for normally distributed variables or by Mann-Whitney U test or Kruskal-Wallis test for nonparametric data, respectively. χ2 test was used for the comparison of qualitative variables. Differences were considered statistically significant at P <.05.
Results
Eighty-one (50.3%) patients of the studied HD patients fasted at least 1 day or more in Ramadan (Table 1). The median number of fasting days was 18, with a wide variation ranging from 1 day up to the whole month. Twenty (24.7%) of the fasting patients succeeded to complete fasting of the whole month (Figure 1). There was no statistical difference between fasting and nonfasting groups regarding age, gender, and duration of HD. Similarly, there was no difference between the 2 groups as regard presence of diabetes, liver disease, and hypertension (HTN), while the percentage of ischemic heart disease (IHD) was statistically significantly higher in the nonfasting than in the fasting groups. Interestingly, 7 (9.5%) patients whose opinion was against fasting of HD patients, practiced fasting in Ramadan by themselves (Table 1). Sixty (87%) patients from the fasting HD patients regularly attended all their HD sessions; missed HD sessions ranged from 1 to maximum of 4 sessions in the whole month (data from 69 patients; Figure 2). Eighty percent of patients reported no complications. The most frequently reported complications by the fasting HD patients were hypotension (6.2%), hypoglycemia (2.5%), and uncontrolled HTN (2.5%; Figure 3).
Demographic Data of Studied Groups.

Abbreviations: HD, hemodialysis; SD, standard deviation.

Number of fasting days in fasting hemodialysis (HD) group.

Number of hemodialysis (HD) absence days in fasting HD group.

Patients and physicians reported complications during fasting.
Fifteen (65.2%) physicians supported the opinion that HD patients are capable to fast with some precautions. There was no significant difference in years of experience of medical profession between physicians who advocate and those who oppose fasting of HD patients (Table 2).
Baseline Characteristics and Survey Results in the Studied Centers.
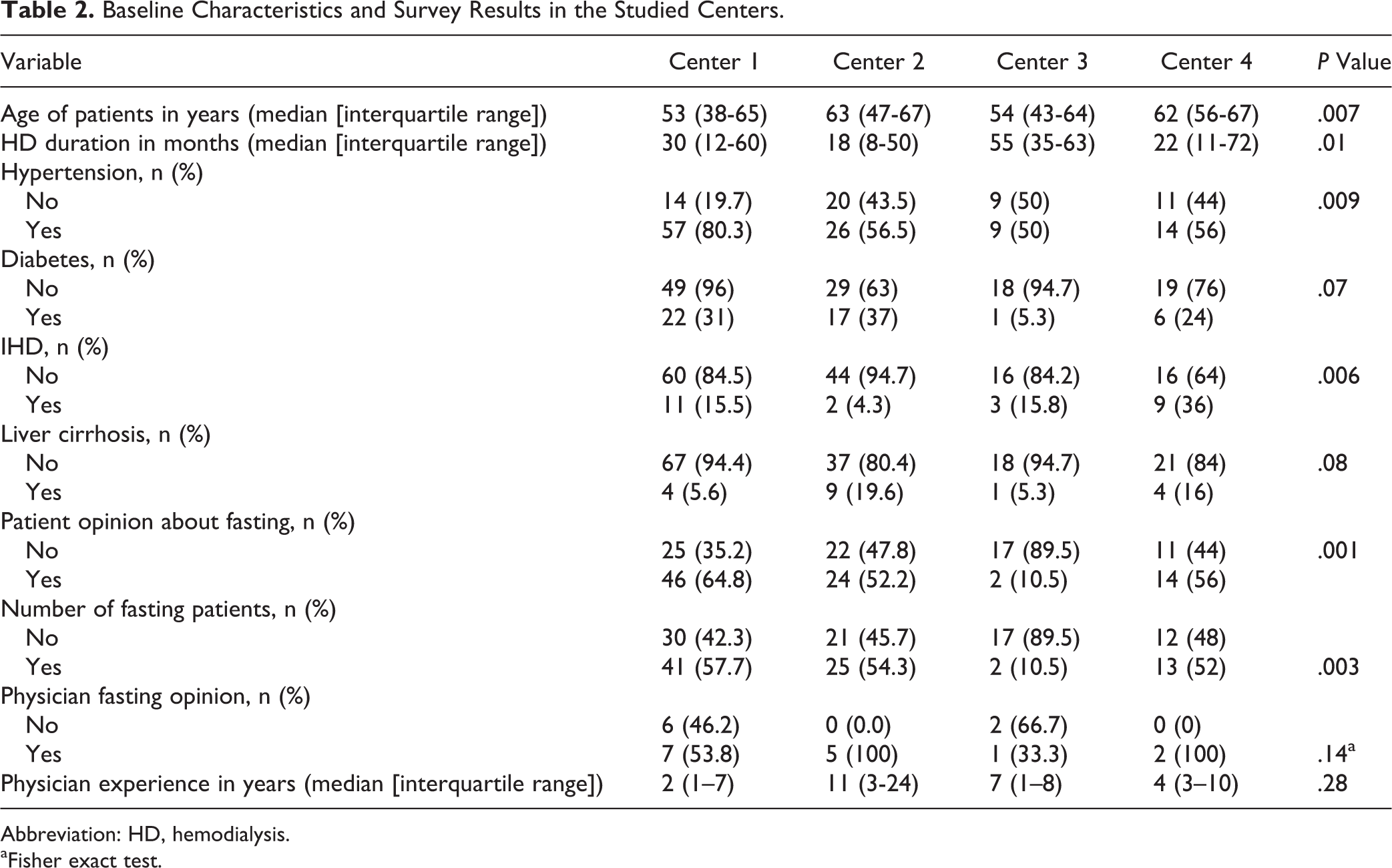
Abbreviation: HD, hemodialysis.
aFisher exact test.
The most common reported complications related to fasting by the treating physicians was hypotension, uncontrolled blood pressure, hypoglycemia, and hyperkalemia (52.1%, 46.2%, 43.5%, and 23.1%, respectively; Figure 3).
Physicians’ opinion and experience were different, although nonsignificantly, in the 4 studied centers. The frequency of fasting of HD patients was significantly different between the studied centers with center 3 (10.5%) having the least observed fasting rate. Patients’ ages and HD durations, and presence of HTN and IHD showed statistically significantly different distribution among the 4 studied centers.
Discussion
Fasting in Ramadan has a unique religious duty with a strong desire among Muslims to participate, even those who are eligible for exemption. Sick people are frankly exempted from fasting, according to Islamic Rules, especially when advised so by a “well-informed” physician, in anticipation that fasting might adversely affect their health. Therefore, the patient’s decision to fast or not is to some extent linked to their physician’s recommendations rather than to a religious scholar’s advice (4).
In the current study, more than half of the included HD patients succeeded to fast and, approximately, one-fourth managed to fast the whole month, uninterruptedly. Despite lack of statistical significance, patients in the fasting group tended to be younger and had significantly much lower prevalence of IHD. Gender, duration of HD, and presence of comorbidities did not seem to have major influence on patients’ ability to fast. Hemodialysis patients’ own believes about their capability to fast were significantly different among the 2 patients’ groups; 9.5% of the fasting patients believed that HD patients should not fast while 14% of nonfasting patients thought that HD patients are capable of fasting. On the other hand, while the majority of the treating physicians supported the opinion promoting fasting of HD patients under some precautions, over a third of them refused this latter opinion and emphasized that fasting could pose serious adverse effects on patients’ health. Furthermore, the difference in opinion between the physicians was not related to the duration of their professional experience.
Individual characteristics of HD patients and their treating physicians recruited from the 4 centers were studied. There was a significant difference in the fasting frequency among patients recruited from different centers. In 3 of the 4 studied centers fasting frequency ranged from 52% to 57.7%, while the fasting frequency in the remaining center (center 3) was significantly low (10.5%). Interestingly, most physicians from this latter center expressed a tendency against fasting of HD patients. This agreement between patients’ behavior and their treating physicians’ opinion reflects the impact of physicians’ opinion on their patients’ attitudes. However, solid conclusion about how physician opinion can affect patient attitude toward fasting is difficult to obtain from these results.
In addition, the frequency of both HTN and IHD was significantly different between patients recruited from each of the 4 studied centers, with the lowest HTN rate observed in center 3 and lowest IHD in center 2. Although statistically insignificant, patients from center 3 also had the lowest frequency of DM and liver cirrhosis. Similarly, significantly longer HD duration was reported in patients recruited from center 3. Long-term HD was documented to be associated with more prevalent complications related to cardiovascular disease, peripheral neuropathy, parathyroid adenoma, parathyroidectomy, and acquired cystic disease of the kidney (5).
Fasting may have both spiritual and physical benefits. However, intermittent fasting performed as a religious practice (eg, fasting in the month of Ramadan) should be viewed distinctly specifically, as eating patterns are not motivated by health reasons (6). During this holy month, there is altered lifestyle and food pattern. In HD patients, fasting also carries a higher risk of dehydration during long fasting hours of the summer season. On the other hand, there is a risk of fluid overload due to increased fluid intake when breaking fast after sunset (7). In support to the latter concept, Rashed noted that patients on long-term HD who fasted during Ramadan may experience an increase in body weight and fluid overload between dialysis sessions due to their tendency to increase food consumption at nights of Ramadan (8). On the other hand, prolonged fasting, which extends over a month, might be expected to cause poor energy intake that could build out the predicament of malnutrition; a known predictor of high mortality in dialysis patients (9). Moreover, fasting usually results in suppression of insulin release; this together with diminished response to epinephrine may be expected to contribute to development of high potassium level in fasting renal patients. Moreover, potassium-rich food items are habitually consumed in large amount in Ramadan, which could aggravate the problem of hyperkalemia. Al Wakeel in a study conducted on 32 HD patients reported that hyperkalemia developed in 25.0% and 15.6% of the HD patients during and after the fasting period; 46% of the patients developed HTN and 36.7% of them developed fluid overload; however, no adverse events requiring hospital admission were observed (7). Recently, Imtiaz and his coworkers noticed a decreasing trend in the mean values of phosphorus levels (4.16 vs 4.25 mg/dL), systolic blood pressure (141.44 vs 143.4 mm Hg), and diastolic blood pressure (79.41 vs 83.26 mm Hg) in 34 HD patients who fasted in Ramadan; however, none of these changes were statistically significant (2).
In the current study, there was a great discrepancy between the frequency of reported complications from patients and their treating physicians. According to HD patients’ comments, 80% of them reported no complications, 6.2% had hypotension, and only 2.5% had hypoglycemia. The physicians’ most common reported complications related to fasting were hypotension, uncontrolled blood pressure, hypoglycemia, and hyperkalemia (52.1%, 46.2%, 43.5%, and 23.1%, respectively). This mismatch may be interpreted as an indication that these patients are so motivated to fast in Ramadan that they under estimate or overlook many of the undesirable consequences of fasting, and furthermore, they tend to deny any causal relationship between their practice and any of the observed complications.
Overall, this study presents observational findings in patients recruited from multiple HD centers in Egypt. It is clearly realized that many HD patients were keen to practice fasting in Ramadan and were to a considerable extent capable of, and even passionate at, completing this Islamic worship. There is a tendency that these enthusiastic patients overlook or minimize reporting the complications that are thought to be related to fasting. Absence of clear evidence-based recommendations or guidelines to guide fasting in Ramadan in HD patients as in diabetic patients makes permission or prohibition of such practice by health-care providers unjustified.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
