Abstract
Background:
Patients’ satisfaction remains an important tool for evaluating quality of care in the emerging global trend of patient-centered care.
Aim:
To assess satisfaction with care received by patients at public secondary hospitals in Abuja, north central Nigeria.
Method:
We measured patients’ satisfaction using structured questionnaire, and Cronbach α was used to assess consistency in item responses. A multivariate mixed-effects linear regression was fitted to identify factors influencing the overall satisfaction.
Results:
All satisfaction domains tested were scored at “intermediate-positive levels” except for the “feeling being valued and appreciated as patients” domain that scored the least positive response level. On the overall, respondents rated the hospitals at high satisfaction level. There was a significant positive association between patients’ satisfaction and careful listening of care providers; patients’ perception of being valued and appreciated by the hospital staff (P = .003 and P = .001, respectively).
Conclusion:
Our findings suggest high satisfaction of care at public hospitals in Abuja Nigeria. Patients satisfaction survey should be integrated into hospital management planning and administration as part of quality improvement.
Introduction
Globally, effective responsiveness to patients’ satisfaction is key to the success of medical practice (1). This is because the relative success of a given health-care intervention may differ significantly between a patient’s perspective and the health-care providers’(HCP) perspective (2,3). HCPs often spend a lot of time managing complaints and handling noncompliant patients - factors and this may reduce healthcare's personnel productivity, and consequenstly negatively impact the healthcare system's efficiency in general. On the contrary, when patients are satisfied, they are easier and more rewarding to care for, as they take up less physician and staff time and are more compliant with their medications and follow-up care (4). Modern medicine is gradually recognizing the importance of the perspectives of the patients in health care. However, more empirical studies are needed to understand the importance of the interrelationships among health needs, satisfaction, and quality of life (1).
Studies have stressed the importance of patients’ views as an essential tool in the processes of monitoring and improving the quality of health-care services (5,6). The patient is a consumer who has legitimate expectation and concerns each time he/she visits the hospital (7); recognizing and meeting these expectations and concerns will contribute to the overall satisfaction of the health-care service received during the visit. Studies have shown that perception of quality of health care received is a subjective attitude relating to the health service but is not equivalent to satisfaction (8). For instance, it has been established that good communication between patients and care providers constitute the single most important component of good medical practice not only because it identifies problems quickly and clearly but it also defines expectations and help to establish trust between the clinician and patient (9,10). Other important factors affecting patient satisfaction of care include cost of health-care services, the technical quality of HCPs, and patients income level. It has been reported that out-of-pocket expenditure accounts for 66% of total health expenditure in Nigeria (11), meaning that households bear the highest burden of health expenditure in the country. Against the backdrop of 62.6% poverty rate (12), out-of-pocket health expenditure often results in catastrophic health expenditure (11,13). Studies show that private health spending seems to have negative correlation with patient satisfaction (11,14). Moreover, a positive correlation between health-care quality and satisfaction has been documented; however, this should be interpreted cautiously because patients who lack technical knowledge assess technical quality of health care (14).
Measures of patient satisfaction with health care are widely used by insurers, providers, and researchers due to their intrinsic value as indicators of consumer preference and their relative ease of measurement (15). In Nigeria, not much studies have been conducted to assess patients’ satisfaction of care at public secondary hospitals. However, some patient satisfaction surveys performed in tertiary hospitals across the country indicate generally high satisfaction, but prolonged waiting time is a concern across board (2,7,9,16,17).
This study therefore aimed at assessing satisfaction of patients with services received from the government-owned secondary hospitals in the Nigeria’s capital city, Abuja and examined the determinants of patient satisfaction in this cosmopolitan setting. Satisfaction was considered from the following domains: waiting time, patient–nurse relationship, patient–doctor relationship, responsiveness of hospital staff, and hospital facilities/environment.
Study Setting
The study was conducted in the Federal Capital Territory Authority (FCTA), Abuja, the administrative capital city of Nigeria. It is located in the north central region of the country and has a population of 1 406 239 people according to 2006 National Population Census (18). The inhabitants of the city are mainly civil servants who belonged to all ethnic groups in Nigeria. The FCTA hospitals provide basically secondary level health-care services in the areas of medicine, surgery, obstetrics/gynecology, pediatrics, laboratory services, and pharmacy, among others. From the unpublished data retrieved from the medical records departments of FCT Hospitals Management Board, the hospitals have an average of 32 000 admissions annually.
Methods
Study Population, Study Design, and Sample Size
This study employed a cross-sectional observational design. A stratified 2-stage cluster sampling was used to recruit respondents into the study. The 12 public secondary hospitals in the study area were stratified into 3 strata based on geographical locations. The first stratum comprised 3 city hospitals, the second stratum included 5 suburban hospitals, and the third one included 4 rural hospitals. Hospitals were considered as clusters and 2 of them were selected within each stratum using a simple random sampling. Study populations were volunteering consented outpatients who had just received health care from the hospitals and inpatients who had just been discharged from admission. Sample size of 382 patients was obtained using Krejcie and Morgan (19) procedure, where we assumed 50% overall satisfaction levels among the average annual of 32 000 patient admissions at the Nigerian FCT secondary public hospitals and set a degree of accuracy at 0.05.
Ethical Considerations
Ethical approval was obtained at the Health Research Ethics Committee of the Federal Capital Territory Administration .
Data Collection
Between November 2013 and June 2014, a pretested structured 28-item questionnaire, adapted from the Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) (20) was administered to the participants to test 9 key domains: communication with doctors, communication with nurses, responsiveness of hospital staff, pain management, communication about medicines, discharge information, cleanliness of the hospital environment, quietness of the hospital environment, and transition of care. The questionnaire was administered to the participants by trained research assistants. Except for the items requesting the participants for suggestions on the improvement of care, other question items were closed ended.
Statistical Analysis
Data were analyzed using Stata version 14.0 (StataCorp, College Station, Texas). Descriptive analysis was performed using the HCAHPS scoring on response and number scale of 1 (never), 2 (sometimes), 3 (usually), and 4 (always) for 5 HCAHPS composites (communication with nurses, communication with doctors, responsiveness of hospital staff, pain management, and communication about medicines) and 2 individual items (cleanliness of hospital environment and quietness of hospital environment). The most positive response is 4 (always), while the intermediate positive response is 3 (usually), the least positive response is 2 (sometimes) or 1 (never). Scoring for the overall hospital rating is on number scale of 1 (worst hospital) to 10 (best hospital). The highest positive response for this variable is “9” or “10,” intermediate positive response is “7” or “8,” while the least positive response is “6” or lower.
We assessed the internal consistency of items responses for satisfaction toward communication with nurses and their responsiveness and toward communication with doctors separately using Cronbach α (21). Item responses were considered to be consistent when the reliability score is between 0.70 and 0.90, below 0.70 is suggestive of low consistency (22) and above 0.90 suggests redundancy in some items (23).
We used multivariable mixed-effects linear regression models with backward selection to identify factors associated with the overall satisfaction. Two groups of potential explanatory variables were considered: sociodemographic variables (residential area, patient’s sex, age, and educational level) and perception variables (frequency with which nurses treated a patient with courtesy and respect, frequency with which nurses listened carefully to a patient, frequency with which nurses explained things to a patient in a way he could understand, frequency with which a patient got help as soon as needed after he called for a nurse, frequency with which doctor treated a patient with courtesy and respect, frequency with which doctors listened carefully to a patient, and frequency with which doctors explained things to a patient in a way he could understand, waiting time, how often a patient’s room/ward and bathroom was kept cleaned, how often the area around a patient’s room was quiet at night, how often a patient felt valued and appreciated at the hospital, and patient’s appreciation of his own health). Hospitals were used as clusters. Variables with highest P value and above 10% were discarded one at a time throughout the model selection. In the final model, we included all sociodemographic variables regardless of their significance level to adjust the effect of perception variables. Restricted maximum-likelihood estimation method was used with Kenward-Roger small-sample adjustment for making inferences (24).
Results
Sociodemographic Data
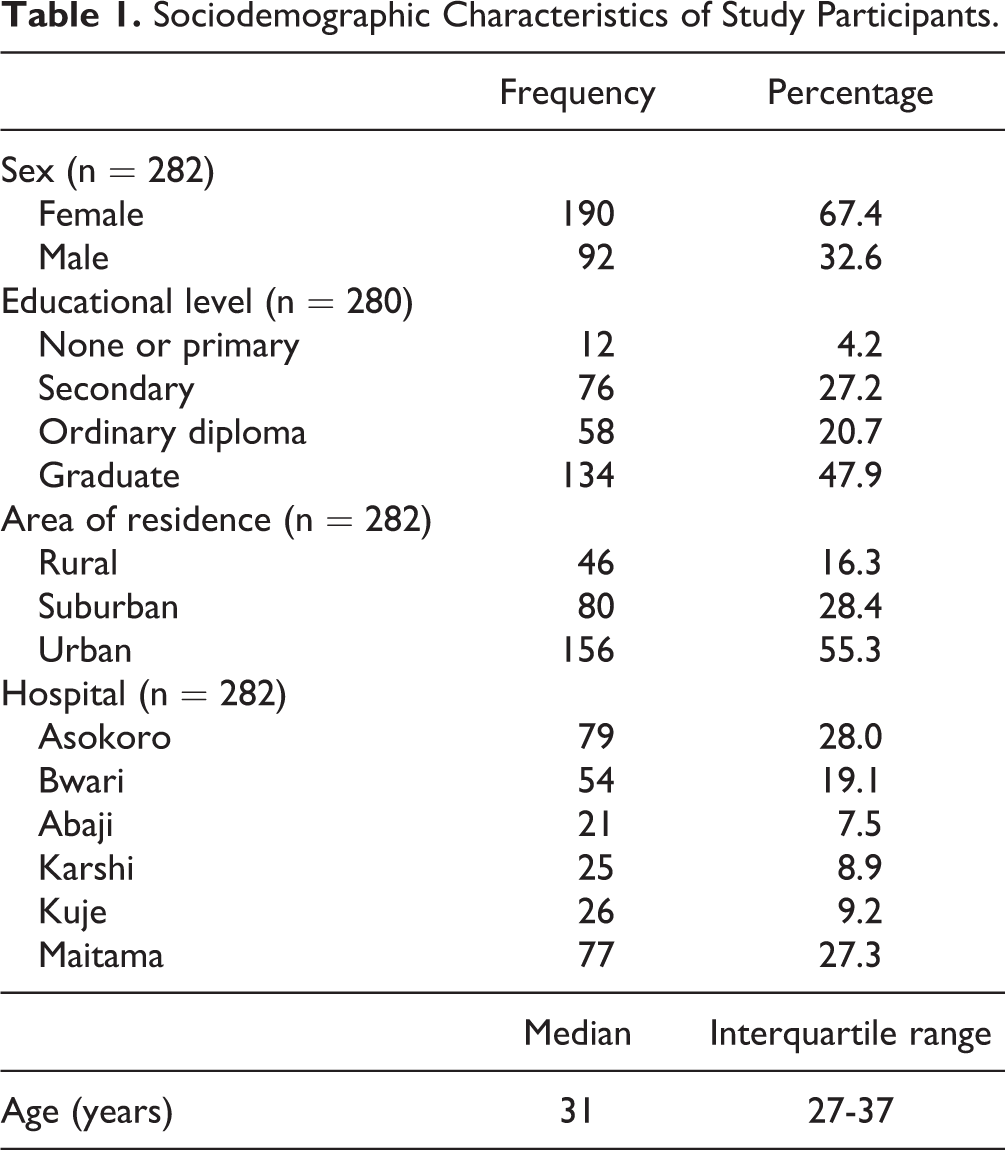
Of 305 completed questionnaires, 23 (7.5%) were invalid. Among the valid respondents, there were 92 (32.6%) males and 190 (67.4%) females, with the age range of 9 to 70 years; 147 (52.1%) were outpatients while 135 (47.9%) were inpatients who were just discharged from admission. Table 1 describes the demographic characteristic of the study participants.
Sociodemographic Characteristics of Study Participants.
Relationship With Nurses and Doctors and Hospital Stay Experience
All individual items that assessed their relationships and communication with doctors and nurses scored mean satisfaction levels >3, except “promptness of responses by nurses when patients called for help” which scored low mean satisfaction level of 2.8. A total of 60.5% of respondents felt being valued and appreciated as a patient during their hospital visits.
Hospital experience by inpatient respondents showed positive average satisfaction score of 3.4 for cleanliness of the ward and bathroom; 3.1 for quietness at night; but low satisfaction score of 2.9 for feeling being valued and appreciated as patients. Detailed information on the abovementioned satisfaction domains is shown in Table 2.
Distribution of Patients’ Satisfaction With Communication and Hospital Stay Experience.

Waiting Time
Table 3 indicates that over 64% of respondents said they spent 60 minutes or less as the waiting time, while average waiting time for all study centers was less than 1 hour.
Distribution of Patients’ Waiting Times.

Average waiting time <60 minutes.
Proportion of respondents whose waiting time was 60 minutes or less = 64.4%
Overall Satisfaction Rating
On a number scale of 1 to 10 (1 being worst hospital and 10 being best hospital), the median satisfaction score was 8, meaning intermediate satisfaction perspective by the patients while 73% of respondents scored the hospitals 7 and higher. Figure 1 shows distribution of the overall satisfaction with hospitals.

Overall satisfaction distribution.
Willingness to Recommend Hospitals
When asked if they were willing to recommend relatives and friends to access health care in the study hospitals, 96.1% (268/279) of the respondents overwhelmingly gave positive responses. Table 4 shows more information on willingness to recommend relatives and friends.
Willingness to Recommend the Hospitals to Relatives and Friends.

Consistency in the subjective assessment of satisfaction
Cronbach α was 0.82 and 0.81 for items assessing satisfaction regarding communication with nurses and their responsiveness and regarding communication with doctors, respectively. This suggested that participants’ assessment of satisfaction toward nurses and doctors were consistent (Table 5).
Consistency of Participants’ Assessment of Satisfaction towards Nurses and Doctors.

Multivariable Analysis
Of 16 potential explanatory variables, only four were found associated with the overall satisfaction score at 10% of significance level. The more nurses listened carefully to a patient, the higher the patient’s satisfaction (effect on overall score = 0.46, 95% confidence interval [CI]: 0.16-0.77; P = .003). The more a patient felt valued and appreciated by hospital staff, the greater was his overall satisfaction score (effect on overall score = 0.62, 95% CI: 0.34-0.91; P < .0001). On the contrary, the less a patient had a good self-appreciation of his health status, the less was his overall satisfaction (effect on overall score = −0.54, 95% CI: −0.85 to −0.24; P < .0001). Education level was negatively associated with overall satisfaction score (effect on overall score = −0.32, 95% CI: −0.49 to −0.15; P < .0001). There was no evidence of association between overall satisfaction and age (P = .49), sex (P = .55), area of residence (P = .18). Table 6 shows the determinants of overall patient satisfaction.
Determinants of Overall Patients’ Satisfaction.

Abbreviation: CI, confidence interval.
aCoded in increasing frequency (1 = never, 2 = sometimes, 3 = usually and 4 = always) and treated as continuous.
bCoded in decreasing perception (1 = excellent, 2 = very good, 3 = good, 4 = fair and 5 = poor) and treated as continuous.
cCoded as 1 = ≤ primary school, 2 = secondary, 3 = ordinary diploma and 4 = graduate and treated as continuous.
dOverall significance test.
Discussion
This study documents the satisfaction of patients with services received from government-owned secondary hospitals in the Nigerian administrative capital city. Respondents were satisfied with patient-HCP relationships at the hospitals, while average waiting time at all study centers was less than 1 hour. Hospital experience by inpatient respondent showed positive average satisfaction score of 3.4 for cleanliness of the ward and bathroom, 3.1 for quietness at night, but low satisfaction score of 2.9 for feeling being valued and appreciated as patients. This would be an area of improvement for the HCPs at the secondary public hospitals. On a scale of 1 to 10, 73% of respondents scored the hospitals 7 and higher for overall performance. This study showed that there is significant positive association between satisfaction and HCP listening carefully to a patient as well as when patients felt valued and appreciated by hospital staff (P = .003 and P = .001, respectively).
There are no standard or universally accepted definitions of waiting times for a broad range of health services and procedures; however, timely access to health-care services has become a primary concern in developed countries (25). For this study, we referred to waiting time as the length of time patients waited to see a health-care service provider. This agrees with that of Rauf et al who defined it as the time from arrival of the patient in the hospital until the start of the consultation by the Medical Practitioners (26). Our study shows an average waiting time of 60 minutes that agrees with findings from the National Hospital, a tertiary health facility in Abuja and other regions of Nigeria (5), but less when compared to the average waiting times of 173 minutes and 73 minutes, respectively observed in 2 health facilities at South South and South West regions of Nigeria. Factors responsible for the waiting time disparity across some of the Nigerian geopolitical regions should be looked into.
Also, our study showed that waiting time fell within the standard set by a District Hospital in South Africa and in accordance with empirical evidence in which stable patients should see the doctor within 2 hours of arrival while unstable patients must be attended to in less than 1 minute (immediately) (26). Given the doctor/population ratio of 1/3001 (27) in our study setting against World Health Organization recommendation ratio of 1 doctor to 600 patients (28), we opine that a 60-minute waiting time should be satisfactory.
Our study shows very good satisfaction level for relationship and communication between doctors/nurses and their patients; this may have largely contributed to the high overall satisfaction score on our study centers. There is consistent evidence across many hospital settings that the most important health service factor affecting satisfaction is the patient/client–practitioner relationship, including information and technical competence (29). This study buttressed by Lim et al in their retrospective study of 226 complaints to the Family Health Service found out that the main reasons for complaints were related to attitude/conduct (28.8%), professional skills (17.8%), patient expectations (16.2%), waiting time (10.0%), and communication (7.8%) (30)—showing that complaints related to attitude/conduct of the professionals was the highest. Effective HCP-patient communication is a vital element in patient-centered care (31). A study carried out at the University of Chicago Hospital’s General Internal Medicine department to determine the relationship between physicians’ communication behaviors and patients’ overall satisfaction with hospital care showed a significant positive relationship between overall satisfaction and overall ratings of attending physician’s communication behaviors (32). Abioye et al showed that patient confidence in the doctor and good communication skills and information provision on the part of the doctor predicted patient satisfaction, whereas patient confidence in the doctor and information provision by the doctor predicted adherence intent (33). Our finding showed positive correlation between HCP-patient relationship and overall satisfaction of care. For instance, the more nurses listened carefully to a patient, the higher was the patient’s satisfaction (effect on overall score = 0.46, 95% CI: 0.16-0.77; P = .003). We did not find any evidence of association between overall satisfaction and age, sex, and area of residence. This contrasts Williams and Calnan who posited that older respondents generally record higher satisfaction—possible explanations include lower expectations of health care and reluctance to articulate their dissatisfaction (34).
Patients rated their overall satisfaction of the hospitals at a median score of 8 on a number scale 1 to 10 (1 being worst hospital and 10 being best hospital). According to the survey instrument used for this study, average score reflects intermediate overall satisfaction perspective by the patients. Generally, 93% of respondents scored the hospitals 5 and above, whereas only 7% scored the hospitals 4 and below. This is similar to Ajayi and colleagues who concluded that there was generally high level of satisfaction in the various aspects of care assessed at University College Hospital, Ibadan, South West Nigeria (16). It is also consistent with findings of Iliyasu et al at Aminu Kano Teaching Hospital, North West Nigeria, where 83% of respondents were satisfied with the services received from the hospital (9).
This study did not evaluate the whole of health-care system at the study sites, and the sample size was small due to limited resources. In addition, our results may not be generalizable to nonconsenting patients unless they have comparable characteristics to those included in this study, which we were unable to assess as data were not available for nonconsenting patients due to research ethics. This study being an evaluation at a specific time point did not account for possible seasonal changes that may occur in the demand for health care within a year and may affect the responsiveness of health facilities. Our sample size calculation ignored possible clustering effect that may lead to a lack of power in our exploratory analysis. Nevertheless, our study has contributed to the emerging body of knowledge on the central roles of patients’ satisfaction in public hospitals in developing countries by providing the platform for further research that would develop appropriate intervention for improving participant satisfaction in hospital care in Nigeria.
Conclusion
This study has provided an overview of satisfaction levels among patients accessing health-care services at Nigerian Federal Capital secondary public hospitals. We have demonstrated that good HCP-patient relationship has positive impact on the overall satisfaction of care. An identified area of improvement is the need for hospital workers to learn to treat patients with courtesy and respect. A take-home message to health administrators and managers is that periodic patient satisfaction survey is crucial to health-care service delivery improvement. Furthermore, HCPs operating in Nigeria should be conversant and strictly adhere to the Service Compact charter (35)—the government’s instrument of ensuring that public institutions deliver quality services designed around customers’ requirements as well as educating the citizens (customers) on their rights.
Footnotes
Authors’ Note
FHREC/2012/07/20/04-07-12.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
