Abstract
Background:
The study objective was to investigate the willingness to pay (WTP) for teledermoscopy services among students at a university health center. The hypothesis was that WTP for teledermoscopy among students would exceed the costs for traditional consultation.
Methods:
Between November 2013 and May 2014, students at a university health center were surveyed for their perceptions of teledermoscopy. One set of responses was collected from students visiting the health center for any reason (anonymous sample). An additional set of responses was collected from students visiting for dermatologic lesions (in-person sample). A contingent valuation method with a maximum likelihood estimation procedure was used to estimate the WTP distribution.
Results:
A total of 214 surveys were collected for the anonymous sample and 41 responses for the in-person sample. The mean (standard deviation [SD]) WTP for the anonymous sample was $55.27 ($39.11; 95% confidence interval [CI]: $49.99-$60.55). The mean (SD) WTP for the in-person sample was $52.37 ($26.56; 95% CI: $43.99-$60.75). Median WTP for the 2 samples was similar: $48.84 and $48.01.
Conclusions:
We conclude that students would be willing to pay for teledermoscopy services that would provide the potential for significant system cost savings. This may be especially true in college health or similar settings where dermatology services may not be available.
Assessment of skin lesions is common in primary care practices. Determining whether patients with these skin lesions should be reassured, have biopsies done, or be referred to a dermatologic specialist is a common dilemma. Along with the high costs of both biopsy and referral of benign skin lesions, there is a continuing shortage of dermatologists in the United States, with wait times for appointments exceeding 60 days, even in urban areas (1). Dermoscopy allows for visualization of the ultrastructure of skin lesions and facilitates clinical diagnosis without a biopsy. Store-and-forward in-person teledermoscopy is a combination of teledermatology and dermoscopy. Teledermoscopy has recently emerged as a clinically effective mechanism (in terms of diagnostic precision and concordance) to improve access and decrease wait times (2,3). Published studies have established the diagnostic precision and concordance of teledermatology with dermoscopy, face-to-face evaluation, and histopathology (4).
Despite the convenience and clinical effectiveness of teledermoscopy, its diffusion and adoption have been slow. Possible reasons for this include lack of availability of store-and-forward in-person teledermoscopy services for primary care practices, insurance companies not covering the costs of teledermoscopy, and the costs to patients (5). Moreover, teledermoscopy is still considered a noncovered service under Medicare.
With the prevalence of health savings accounts and increasing copayments, patient “willingness to pay” (WTP) for the service (either as partial copayment or full payment) may be a critical determinant for wider acceptance of this innovative practice. The WTP for any patient can also help establish the value of teledermoscopy services from the patient perspective. Value in health-care settings can be measured not only by patient-centered outcomes of health-care delivery but also in part from the patient’s cost perspective (6). As part of its Triple Aim, the Institute of Healthcare Improvement has included lower cost per capita as one of its goals in assessing health-care delivery (7). One element of the current American College of Physicians High Value Care program is helping physicians to provide the best care and avoid unnecessary costs (8).
Teledermoscopy has been used to deliver care in rural medicine and other medical settings. However, patient preferences for teledermoscopy and their WTP for such services have not been examined thoroughly. This is especially the case for young adult populations, such as those at university student health services. Although primary care practitioners are present in many of these settings, students with skin lesions may lack time to get to dermatology specialists or lack access to local dermatology specialists or primary care clinicians with expertise in dermoscopy. Offering teledermoscopy services to a population already comfortable with mobile technologies would seem especially attractive (9).
The overall cost of teledermoscopy equipment is minimal and can be transmitted via secure encrypted lines (about $1500 for an unlocked smartphone to capture the clinical [www.apple.com] and camera lens attachments [www.dermlite.com]). The purpose of this study was to determine WTP for teledermoscopy services among patients at a university health center and to compare this amount with the cost of traditional consultation. The research hypothesis is that the amount that students are willing to pay for store-and-forward in-person teledermoscopy consultation will be higher than the prevalent insurance copay amount paid for traditional consultation. We further explored factors influencing WTP, including brand reputation of the provider, service convenience perception, and service satisfaction.
Methods
Population and Sample
The population for this study comprised students at a large university in the southwestern United States. Since available research budget allowed us to offer only 50 free teledermoscopy consultation, 2 samples were collected to increase sample of subjects surveyed in the study. We used a convenience sample of the 2 groups (usual and those requiring dermatology consultation), but the size of the first sample makes it more likely to be representative of the general population of students using services. The first sample (anonymous sample) included university students who visited the health center for a general consultation in a 6-month period (November 9, 2013, through May 30, 2014). The required sample size was computed using the guidelines given in the study by Mitchell and Carson (10). For the real WTP to be within 25% of the estimated WTP, we required approximately 180 usable responses. The sampling of students visiting the health center ensured that this was a representative sample of the student population using the health center services.
The second sample (in-person sample) included students visiting the university’s health center for skin lesions during the same time period. If the clinician was unsure about the clinical diagnosis, a free teledermoscopy consultation was offered to the patient. The image capture of the lesions was performed by the university’s health center staff at the direction of the clinician. The clinical and dermatoscopic images were interpreted by a staff dermatologist at Mayo Clinic Arizona. A total of 50 free consultations were offered, and responses were collected from this sample. Responses with missing values in either the dependent or independent variables were dropped from the analysis.
Design and Procedures
Institutional review board approval was obtained for study design and procedures. For the anonymous sample, students waiting in the lobby were approached by the health center staff. Students were eligible to participate if they indicated that they were older than 18 years. The online survey was developed in Qualtrics (Qualtrics [https://www.qualtrics.com/research-core/] is a research platform that enables design and execution of survey questionnaires. The survey questionnaire was created using the Qualtrics platform and made available to respondents via a web URL), and students had the option of using either their own mobile device or a terminal available in the health center to complete the survey. For the in-person sample group, after determination by the primary provider that the person had a skin lesion, the patient consented to have teledermoscopy and completed the survey postprocedure.
Instruments
The dermoscopy tools used included an iPhone 4s (www.apple.com) with an attached Canfield Dermscope (www.canfieldsci.com). Images were captured and immediately uploaded to the interpreting dermatologist via Wi-Fi using a Virtual Private Network. The iPhone did not have cellular service in order to minimize privacy risks. After interpreting the images, the dermatologist created a medical note describing the clinical findings. That medical note was sent to the requesting provider within 48 hours.
Instruments used in the survey have been previously validated (included in the supplementary files). These included the 3-item service convenience scale (11), a 3-item scale for brand reputation (12), and a 4-item scale for satisfaction (see Table 1 for item descriptions). All 3 instruments have been recognized as important constructs in the services marketing literature. Service convenience is included in this study because it is one of the most important determinants of consumer purchase decision (11). Because a well-known health system (Mayo Clinic) was providing the specialist service, we included the brand reputation scale. The reputation of the organization providing the specialist care can influence consumer WTP. Finally, we hypothesized that satisfaction with the health-center services can influence patient perceptions of the quality of teledermoscopy service offered. As such, we included an instrument to measure satisfaction.
Composite Score Summaries for Instruments.
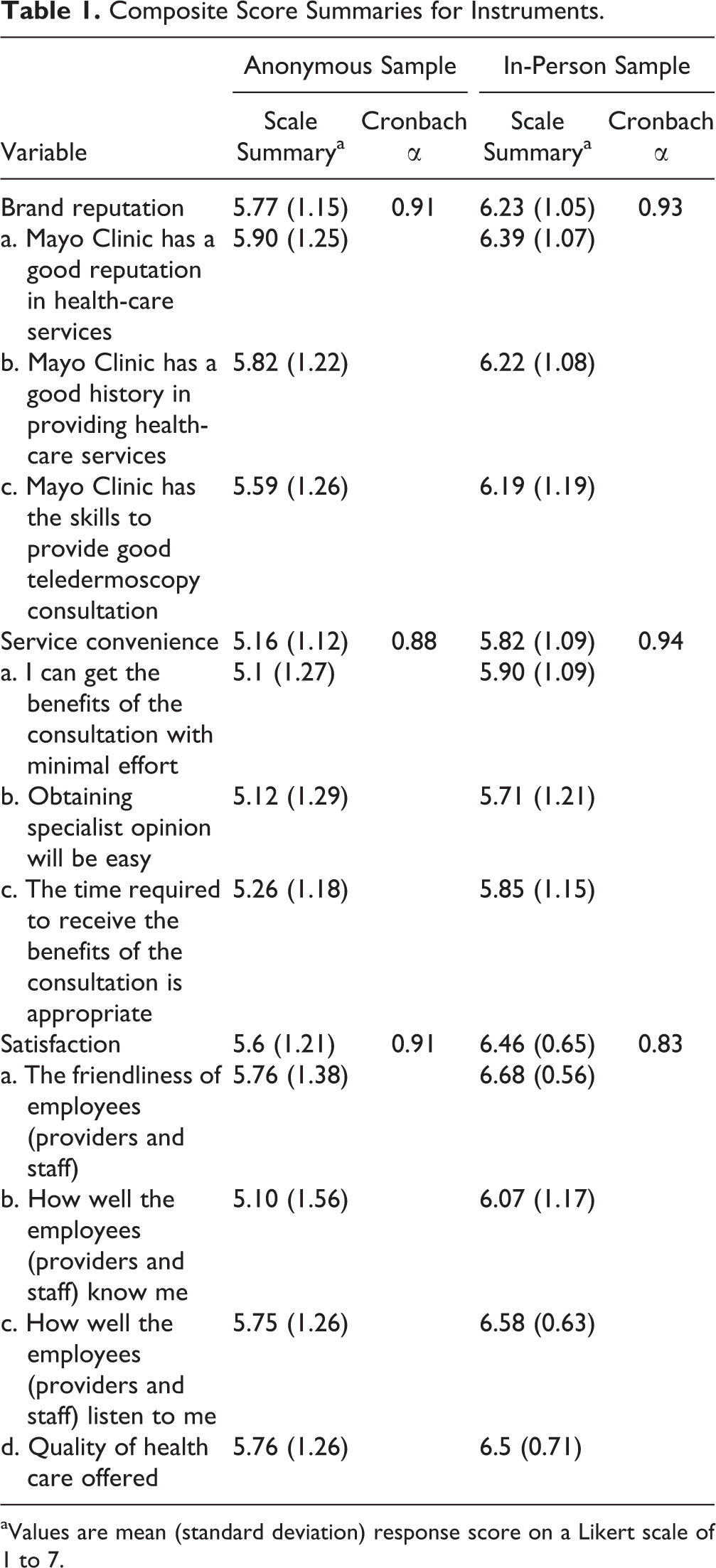
aValues are mean (standard deviation) response score on a Likert scale of 1 to 7.
Willingness to Pay Measurement
Willingness to pay measures the dollar value that a customer attributes to the service offering. The empirical measurement assumes a random utility framework in computing WTP. The double-bound-dichotomous-choice (DBDC) contingent valuation method was used for WTP measurement (13 –15) because it is a well-established method to assess consumer value for technology-based services (16 –18).
A unique feature of the DBDC procedure is that it places very little cognitive burden on respondents. The procedure asks respondents a sequence of WTP questions (with different dollar amounts) for which they simply have to choose either yes or no answers. Each respondent sees 2 dollar amounts from a set of 3 values ($AL<$A1< $AH). The respondent is first presented with the question “Are you willing to pay $A1 for teledermoscopy service?” If the answer is “Yes,” the second amount presented is $AH; if the response is “No,” then the second amount presented is $AL. If the response to the second amount, $AH, is also “Yes,” the respondent is asked to state the highest amount they are willing to pay. A “No” response ends the WTP question sequence and bounds the WTP between $A1 and $AH. If the response to the second amount, $AL, is “No,” the respondent is asked to state the lowest amount they are willing to pay. A “Yes” response ends the WTP question sequence and bounds the WTP between $AL and $A1.
To improve the estimation accuracy of the WTP distribution, multiple sets of values for $AL, $A1, and $AH were constructed and randomly presented to individual respondents such that there was more granularity in the upper and lower bounds of the unobserved true WTP (17,18). The amount range in the study was $10 to $100 in increments of $10. The value sets therefore started from $10, $20, $30 to $80, $90, $100, for a total of 7 distinct sets of values. To reduce hypothetical bias in eliciting WTP, the “cheap talk” procedure was implemented (19), which explicitly asks the respondents to imagine paying for the service in a real scenario. As such, it is standard practice to describe an anchor price (where available) and any characteristics/features of the product/service and available alternatives. We therefore anchored the survey on prevailing copay amounts in the local market ($30) and also indicated expected wait times for specialist access.
Statistical Analysis
Data analysis was conducted in Stata version 12 (StataCorp, College Station, Texas, USA). Sample characteristics of the anonymous and in-person samples were first compared using χ2 and Fisher exact tests before separate estimation of models from the 2 samples. Significance was set at the P <.10 level. Cronbach α was used to measure reliability of the service convenience, satisfaction, and brand reputation constructs. For very good internal consistency of measurement scales, Cronbach α scores should be greater than 0.8 (20). The rotated (oblique) confirmatory factor analysis loaded the construct items separately on distinct factors. Variance extracted for these constructs higher than 0.5 and composite reliability higher than 0.85 suggest very good convergent and discriminant validity (21). Composite scores computed after confirmatory factor analysis of the 3 constructs were used in empirical estimations. Willingness to pay probability for the sample is specified as a log-likelihood function as explained by Raghu et al (18). In the log-likelihood function, each yes/no response sequence for WTP questions is expressed using a cumulative probability distribution. The parameters of the probability distribution are estimated using the study covariates. The sample probability distribution can be estimated using any nonnegative distributions such as lognormal, log-logistic, γ, Weibull, or Gumbel. The Gumbel distribution provided the best overall fit for the WTP distribution function in both samples (based on the Akaike information criterion (10)). The WTP estimation procedure yielded estimates for the location (µ) and scale parameter (β) of the Gumbel distribution. Mean of the Gumbel distribution is
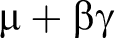
where (γ is the Euler-Mascheroni constant [0.5772]), median is µ − β ln (ln[2]), and standard deviation (SD) is βπ√6.
To measure the association of demographic and perception variables with WTP, a WTP model with covariates was estimated. In the model, demographic variable categories were condensed to make more meaningful inferences. International students were compared against other student groups, and income category was condensed to 2 and compared against the group with income less than $25 000. Willingness to pay for masters and above students was compared against all other groups, and part-time employed students and other groups were compared against full-time employed students.
Results
For the anonymous group, 484 students were contacted during the study period, and 214 completed surveys were collected. From the 50 free teledermoscopy consultations, 41 useable responses were collected to make up the in-person sample. Descriptive statistics for the 2 samples are summarized in Table 2. The only variable significantly different between the groups at the P <.10 level was insurance (P = .06).
Respondent Characteristics.a

Abbreviations: GED, General Educational Development; HMO/PPO, health maintenance organization/preferred provider organization.
aValues are no. of respondents (%).
bχ2 test.
cFisher exact test.
For the survey instruments, internal consistency of the scales related to service convenience, brand reputation, and satisfaction were measured using the Cronbach α (Table 1). All scores were higher than 0.8 in both surveys, which indicates very good internal consistency. The rotated (oblique) confirmatory factor analysis loaded the construct items separately on distinct factors. The average variances extracted for these constructs were all higher than 0.5, and the composite reliability was higher than 0.85, which suggests very good convergent and discriminant validity.
The proportion of respondents in the anonymous sample willing to pay for service at each value level is shown in Figure 1. The mean (SD) WTP for the anonymous sample was $55.27 ($39.11) and for the in-person sample was $52.37 ($26.56). The 95% confidence intervals of WTP in the 2 samples were overlapping—$49.99-$60.55 versus $43.99-$60.75—which indicate no difference between the groups. Median WTP for the 2 samples was similar: $48.84 versus $48.01.

Proportion of Patients in the anonymous sample willing to pay for teledermoscopy service by price point (WTP). WTP indicates willingness to pay.
In the WTP model, service convenience was significantly positively associated with WTP in both samples (anonymous: β = 5.787, P = .04; in-person: β = 5.820, P = .08; Table 3). In other words, 1-unit increase in service convenience increases mean WTP by $5.7. Brand reputation also was positively associated with WTP in both samples (anonymous: β = 7.724, P = .007; in-person: β = 7.640, P = .04). Provider satisfaction was not a significant predictor of WTP in either sample. Income more than $25 000 (β = 19.73, P = .01) and part-time employment status (β = 21.38, P = .01) were strong positive predictors in the in-person sample only. Student respondents with a master’s degree and above were associated with lower WTP in the in-person sample (β = −12.34, P = .04). Although not reported in the model in Table 3, other demographic variables were not found to be associated with WTP in either sample.
Willingness to Pay Estimation With Covariates.a

aValues are estimation coefficient in the model (Standard Error).
b P<.05.
c P<.1.
d P<.01.
Of the 50 patients in the study who completed teledermoscopy, 17 had clinical findings (as assessed by the remote dermatologist) that required further in-person subspecialty consultation. The other 33 had clinical and dermatoscopic findings that, upon dermatologist review, required no further evaluation. At the typical Medicare reimbursement rate for dermatologic consultation of $73.06 (level 3 new patient Current Procedural Terminology code: 99213; Noridian, Medicare [https://med.noridianmedicare.com/documents/10534/8423690/2017_jf_az_mpfs_122316.pdf]) and accounting for the costs of teledermoscopy interpretation of $25.78 ($154.98 per hour for a dermatologist [http://swz.salary.com/salarywizard/dermatologist-Salary-Details.aspx]; 10 minutes per teledermoscopy interpretation), the teledermoscopy service decreased the overall cost of care for those 50 patients by $1121.98 ($73.06 × 50 − [$25.78 × 50 + $73.06 × 17]). This represents a savings of about 31% compared with all 50 patients visiting a specialist at Medicare reimbursement rates.
Discussion
This study examined university students’ WTP for teledermoscopy services. University students are a relatively unique population in that they are usually served by a university-based health service that uses a primary care home-type model and may have limited access to specialty care, depending on their geographic location. Most of these health services do not employ higher salaried specialists to provide consultative care. Indeed, for our 50 patients, who had teledermoscopy not been available, all would have been referred for in-person consultation with a dermatology specialist. In addition, on many campuses, students may lack the funds, free time, or transportation to obtain this usually higher priced specialty consultation. Finding unique solutions to determine when further specialty consultation or intervention is necessary during the primary care visit would be important for patient care. In addition, this would meet health systems’ needs to deliver on the Institute for Healthcare Improvement’s Triple Aim and the American College of Physicians’ High Value Care.
Although not all demographic characteristics of our cohort have available equivalent comparisons to a more general population, we were able to compare some of the demographics. In the whole cohort, 69.8% were covered by an employer health maintenance organization/preferred provider organization and 16.3% were uninsured/did not know. These percentages are close to the national average per a 2008 US Government Accountability Office report (22): close to 20% of college students are uninsured and 67% have employer-sponsored plans. In our sample, 55.9% of the respondents disclosed their race as white; both the national (Census bureau) population and the university’s student population are 59% white.
In our study, the two sample populations derived a robust estimate of WTP. The WTP estimates from the 2 samples overlapped, with a median of approximately $48. The study validated our hypothesis that patient WTP was higher than the prevailing copay amount for such services. Since the DBDC contingent valuation method was used for estimation, the proportion of patients willing to pay for teledermoscopy service can be determined for various price points. At about $30 out-of-pocket expense, approximately 65% of the sample were willing to pay for teledermoscopy service (Figure 1). This suggests that teledermoscopy services in universities can be attractive to a sizeable portion of the student population.
Two key variables were influential in our WTP models. First, reputation of the provider was a significant estimator of WTP. If universities want to offer teledermoscopy services, it is important to partner with a reputed provider. The health-care organization providing the teledermoscopy service must have a strong brand reputation. Second, service convenience perception was a significant contributor to WTP. The ability to get an answer without having to schedule a separate appointment and pay a second copayment for services is truly a service convenience perception.
Limitations
The study findings are limited to respondents from a single university health-care center. As such, replication of the WTP survey in other universities is needed to generalize the study findings. To provide a reference for comparison, we compared some relevant demographics with the latest American College Health Association-National College Health Assessment (ACHA-NCHA-II) survey report (23). As shown in Table 2, of those who responded to the questions, most were white (55.9% and 63.4% vs ACHA-NCHA-II: 78%) and private insurance holders (66.5% and 58.5% vs ACHA-NCHA-II: 69.1%). We also had more international student respondents (20.5% and 21.9% vs ACHA-NCHA-II: 9%). Funding limitations curtailed our ability to offer free teledermoscopy service to a larger group of students. However, given the similarity of the WTP in the two samples, we believe the findings are robust for this population. That is, the teledermoscopy experience did not alter the WTP perceptions significantly.
Savings from teledermoscopy are contingent on the cost difference between reading services and the costs of in-person consultation. The savings are also dependent on the proportion of consultations eliminated due to teledermoscopy. To retain the cost and service convenience benefits, it is also important to incur minimal costs for information transfer to the patients.
Conclusions
On the basis of our study findings, patients were willing to pay for teledermoscopy services, which would mean a significant savings to the system. We recommend that university-based primary care health facilities without on-site dermatology staff employ the use of teledermoscopy. Past studies have shown that teledermatology and in-person consultation assessments are concomitant (24,25).
In summary, we found that the WTP for teledermoscopy services was close to $50, more than the prevailing copay amount. We also found that service convenience and service provider reputation were significantly associated with higher WTP. Based on current reimbursement levels for specialty consultation, we believe that teledermoscopy can provide a significant cost savings to patients and health systems when in-office dermoscopy is not available. Teledermoscopy also offers significant societal benefits by shortening wait times for patients.
Supplemental Material
Supplemental Material, SCO2017-011_Appendix - Willingness to Pay for Teledermoscopy Services at a University Health Center
Supplemental Material, SCO2017-011_Appendix for Willingness to Pay for Teledermoscopy Services at a University Health Center by T S Raghu, James Yiannias, Nita Sharma, and Allan L Markus in Journal of Patient Experience
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
