Abstract
Introduction:
The rapidly aging US population is resulting in major challenges including delivering quality care at lower costs in the face of a critical health-care workforce shortage. The movement toward home care has dramatically increased the need for qualified, paid personal care aides (PCAs). Adequate PCA training that focuses on skills for person-centered, at home support is an imperative. This study provides evidence that clients of PCAs who have completed a comprehensive, evidence-based PCA training program, titled Building Training…Building Quality (BTBQ), report higher satisfaction and better health outcomes, compared to clients of PCAs with lesser or other training.
Methods:
A mixed-methods, quasi-experimental design was used to compare self-reported survey responses from clients of BTBQ-trained PCAs (treatment group) with responses from clients of non-BTBQ-trained PCAs (control group).
Results:
Clients of BTBQ-trained PCAs had significantly fewer falls and emergency department visits compared to clients whose PCAs had no BTBQ training (P < .05). Conclusion: BTBQ-like PCA training reduces costly adverse events.
Keywords
Introduction
The US population is rapidly aging, creating multiple public health and economic challenges (1 –3) including a critical health-care workforce shortage (4 –6) and pressure to improve health-care experiences and outcomes at lower cost (7). While family members still provide most in-home care, a larger, highly skilled home care workforce is crucial to meeting these major challenges. Up to 80% of all paid in-home care is provided by direct care workers (DCWs) (8). By 2020, they are expected to comprise the largest occupational group of the US workforce at nearly 5 million (8). When trained, DCWs are capable of providing safe, person-centered and cost-effective care in clients’ own homes where most older adults prefer to live (9 –11). Personal care aides (PCAs), who go by many titles, are a subset of DCWs who assist clients with tasks such as dressing and bathing, housekeeping, meal preparation, and medication management (8). They are in a pivotal position to monitor their client’s status, recognize and report changes, potentially avert costly emergency department (ED) visits or hospital stays, and diminish or contribute to quality of life. Yet their work is characterized by unstable hours, few if any benefits, low pay, and little if any training (12 –15), which results in ongoing and devastating high turnover rates and compromised quality of care. Training is one key to breaking this cycle. There is growing evidence of the impact of direct care workforce training on patient outcomes and cost (16 –22) and of PCA training on specific measures including job satisfaction (23). Yet, little research exists on the link between PCA training and patient outcomes.
In 2010, Michigan received a Health Resources and Services Administration (HRSA) Personal and Home Care Aide State Training (PHCAST) demonstration grant to develop, implement, and test a comprehensive PCA training program. A successful, evidence-based program resulted, titled Building Training…Building Quality (BTBQ), with key findings including a significant correlation between training and improved job skills, employment status, and job satisfaction. Further, key characteristics contributing to the success of this PCA training were identified, which has relevance for beginning to determine what constitutes a “gold standard” program. In 2014, the Michigan State University Pearl Aldrich Endowment program funded a follow-up project to determine the effect of BTBQ training on self-reported client health outcomes. This article reports important new findings, which provide evidence that clients of PCAs who have completed a comprehensive, evidence-based PCA training program report higher satisfaction and better health outcomes, including fewer ED visits and falls, compared to clients of PCAs with lesser or other training. These findings will be of interest to all those who strive for improved patient satisfaction, quality of care, and outcomes. The study was approved by the Michigan State University Institutional Review Board.
Methods
This study utilized a mixed-methods, quasi-experimental design to compare survey responses from clients of BTBQ-trained PCAs (treatment group) with responses from clients of non-BTBQ-trained PCAs (control group). To account for variation in client “level of need” and service “dosage” (amount of time PCAs spent with client), the survey included data on client’s clinical complexity and service use.
Client Recruitment and Data Collection
Clients were recruited in two ways. First, BTBQ-trained PCAs were contacted by phone and invited to participate by providing current clients with study invitation packets. Of the 383 BTBQ completers, 124 were eligible, for example, they had a current client and agreed to participate. Most of the PCAs had 1 client. Some had 2 to 3, which resulted in a total of 248 packets being mailed. The PCAs were required to send confirmation that packets had actually been delivered in order to receive their incentive. Although not foolproof, this helped reduce the possibility of introducing bias into the findings as a result of PCAs delivering packets to some clients and not others. In addition, the PCAs were not told what the packets contained and were asked not to help the client respond. Once clients received the packet, they communicated directly with the research team and there was no longer any PCA involvement. Client participation was voluntary and confidential.
Second, clients enrolled in the MI Choice waiver program (Michigan’s community and home-based waiver program for Medicaid-eligible elderly and disabled individuals) received packets via their case managers (N = 1099 across 5 regions). Each packet contained a summary of the study, contact numbers for more information, a consent form, a postage-paid return envelope, and a short questionnaire with 4 questions: How many PCAs provide you with supports and services? How many hours per week does each PCA work with you? What type of training does each of these PCAs have? What is the approximate month and year that each PCA started working with you?
The questionnaire included instructions that specified if the client was unsure of the answers, they could ask a family member or responsible party to assist. It was in grid form so that responses to questions 2 to 4 could be provided for up to 3 PCAs. For question 3, there were 5 check off choices including (1) BTBQ, (2) no special training other than “on-the-job” training, (3) certified nurse assistant (CNA), (4) training provided by the agency (if PCA was employed by an agency), and (5) other, with a request for explanation. Clients who returned a consent form were sent a self-report survey with a postage paid return envelope. Reminder letters were sent if a completed survey was not returned within 3 to 4 weeks. Of the 1347 clients total who received a packet, 205 returned a consent form, and of these, 179, representing all 5 regions, returned a completed survey for a final response rate of 13%. A higher rate was limited by reliance on busy case managers to deliver packets and provide sufficient explanation of the contents or study and/or the capacity of frail elders to respond to self-report surveys. All respondents received a store gift card for US $20.
Client Assignment to Study Groups
For study success, it was imperative that the research design and assignment recognize that clients generally have more than 1 PCA, typically 2 to 4 different PCAs who take shifts, and that each of the client’s PCAs may have a different level of training. A client may have a “team” that includes a BTBQ-trained PCA as well as nontrained-PCAs or PCAs with different training such as CNAs who have completed 75 hours of CNA training. The CNA training shares some content with BTBQ but does not address required home care skills. We devised a way to isolate the impact of BTBQ-trained PCAs versus PCAs with other levels of training by examining client outcomes in terms of the composition of training within their PCA “team” and then conducted comparisons across these teams. Based on the hypothesis that having a BTBQ-trained PCA adds value to the team regardless of the level of training of other PCAs in the group, we assigned clients to 1 of 3 “team types”: Group A: clients with at least 1 PCA with BTBQ training (treatment group), Group B: clients with at least 1 PCA with CNA training and no PCAs with BTBQ training (control), Group C: clients who had PCAs with lesser or no training only (control).
Data Collection Instruments
Client surveys consisted of 34 multiple-choice and short answer questions that collected both quantitative and qualitative data on the number of care hours received per week, their PCA’s level of training, demographics, living arrangements, diagnoses, and service utilization. Health-related questions were based on the Minimum Data Set–Home Care (MDS-HC) forms required by MI Choice modified to allow self-report. Examples include number and reason for hospitalizations, ED visits, fractures, falls, pressure ulcers, and urinary tract infections in the past 12 months. Additional questions focused on tasks provided by PCAs including 5 activities of daily living (ADLs), 6 instrumental activities of daily living (IADLs), companionship, and “other” using check offs and a 4-point Likert scale from “no assistance needed” to “need help/perform less than 50% of task on own.” Respondents were asked to rate their health (poor, fair, good, and excellent) and report on skin conditions, nutrition, and hydration in the past 1, 3, and 12 months. Finally, they were asked to share their perspective on PCA training and how PCA training affects quality of care and client health, using Yes/No/Not Sure responses to statements such as “Having a well-trained PCA” followed by choices such as “Improved the quality of care I receive,” “Reduces my risk of falling,” “Reduces the number of times I have to go to the ER,” and “Improves my ability to stay in my own home.”
Open-ended questions provided the opportunity to expand on specific ways in which PCAs had made a difference in the client’s own personal health. Finally, clients were asked to rate the importance of 18 PCA training topics using a 4-point Likert scale ranging from “not important” to “very important” which included topics from professionalism and infection control to bathing, meal preparation, and client rights.
Analyses
Descriptive statistics and frequencies were generated for client surveys using SAS software. Analyses were conducted to determine if there were differences between client treatment and control group characteristics, for example, chi-square analysis was conducted to determine whether the 3 client groups were comparable in terms of demographics such as age, marital status, living arrangements, and health status; the Fisher Exact test and Kruskal-Wallis test were conducted to test for differences in service utilization and number of incidents; and an ordinal logistic model was used to test for possible relationships between significant demographic differences and service utilization and number of incidents; using a P value of less than .05 to indicate significance. Diagnosis scores were also determined by assigning one point each time a client checked “yes” to any of the 8 disease diagnoses listed, with higher total points indicating a higher diagnosis score. No significant differences existed between the 3 groups in the mean diagnosis scores, ability to perform ADLs and IADLs, or program utilization. When examining individual diagnoses included in the overall score, only 4 statistically significant differences were found, each indicating a difference within the 3 groups but not pinpointing which group differed from the others. Raw numbers suggested that group A had a higher prevalence of clients with dementia and cancer and group B had a higher prevalence of clients with diabetes and those who needed medication to be prepared by another person. However, additional statistical testing indicated that these differences did not compromise evidence of program impact. Specifically, there was no differential influence on falls and ED visits related to these variables meaning that true outcome differences in these outcomes, based on BTBQ, existed. Therefore, treatment and control groups were determined to be comparable for the purposes of this study.
Qualitative data were analyzed using narrative analyses techniques and NVivo 10 qualitative software (QSR International Pty Ltd, Melbourne, Australia). Text was read line by line and coded by 2 readers from the research team. Coding was iterative; it was first guided by survey questions and then by additional concepts that emerged from the data. Concepts were then organized into discrete categories with shared attributes from which common patterns and points of divergence could be identified. Each concept and category was further discussed by the research team to reach consensus for high inter-rater reliability. Several prominent categories or recurring themes emerged based on the frequency with which clients raised specific issues and perspectives.
Results
Client Self-Reported Health Outcomes (Comparing Across Groups)
Although the survey response rate was low, the sample size was sufficient to conduct meaningful comparisons across treatment and control groups and determine statistical significance. No statistically significant difference between client groups was found in the number of inpatient hospital admissions over the last 12 months. However, the data suggest a possible trend (P value = .192) with raw numbers indicating that group A clients (BTBQ trained) clearly experienced fewer hospital admissions than groups B and C. Sixty-five percent of group A clients had no hospital admissions compared to 46% of group B and 49% of group C. This trend may prove significant with a larger sample size. Analyses determined that overall, training made a statistically significant difference in the number of ED visits among all 3 groups (Table 1; Fisher Exact test, P value ≤ .01) with group A clients reporting fewer ED visits than group B (P value ≤ .01). Although not statistically significant, group A clients also experienced fewer ED visits, in terms of raw numbers, than group C. Surprisingly, group B, with trained CNAs, experienced a statistically significant higher prevalence of ED visits than group C (P value ≤ .05). This counterintuitive finding underscores the need for additional research. One might posit that CNA training combines a heightened ability to detect a potential need for emergency assistance (compared to those with no training) with a medical model ethos that provides the CNA with fewer skills or options for responding to such situations (than those with BTBQ training). A second important finding is that training made a statistically significant difference in the number of falls among all groups (Table 2; Kruskal-Wallis Test, P value ≤ .05), with group A having fewer falls than group B (Wilcoxon 2-sample test, P value ≤ .01) and also fewer than group C (Wilcoxon 2-sample test, P value = .05). Seventy percent of group A clients reported zero falls and only 43% of group B and 54% of group C clients reported zero falls. In other words, A is better than both B and C (has fewer falls). No significant difference was detected between the 3 groups in terms of pressure ulcers or other skin condition issues*.
Effect of Training Type on the Number of Client ED Visits in the Previous 12 Months*.

Abbreviations: ED, emergency department; BTBQ, Building Training…Building Quality; CNA, certified nurse assistant; PCA, personal care aide.
Effect of Training Type on the Number of Client Falls in the Previous 12 Months*.
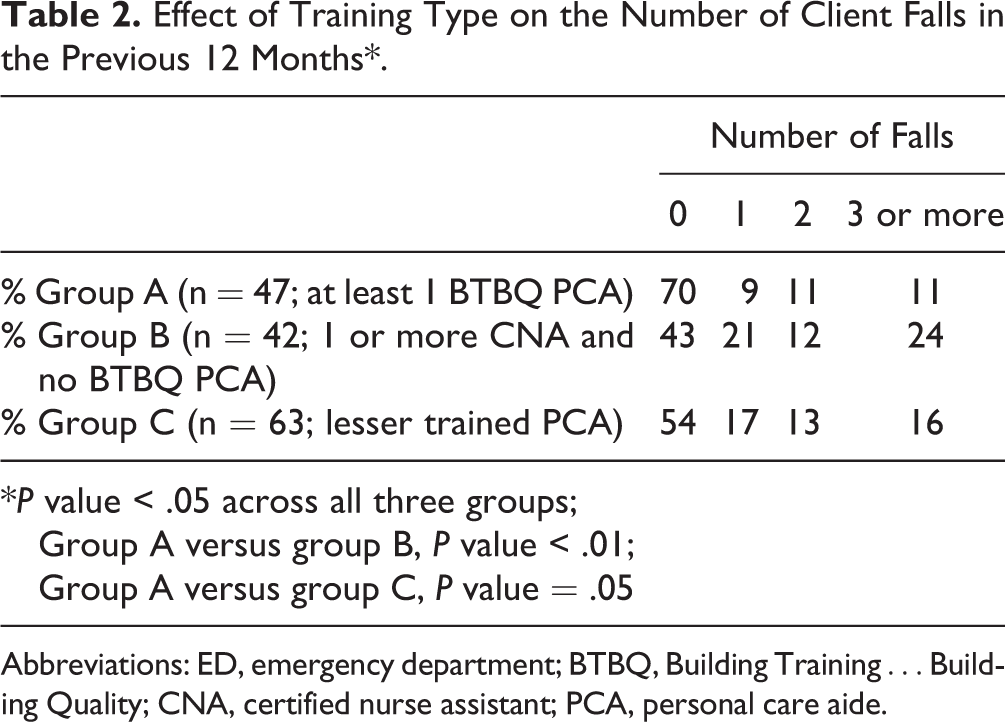
Abbreviations: ED, emergency department; BTBQ, Building Training…Building Quality; CNA, certified nurse assistant; PCA, personal care aide.
Client Satisfaction and Perceptions of PCA Training on PCA Performance and Client Health
All 3 groups placed a high value on PCA training and three-quarters (75%) stated PCAs should receive adequate training before working as a PCA. The most prominent theme to emerge from qualitative analyses was the perception that training has an impact on health outcomes and quality of care. Specifically, clients believed that a trained PCA is directly related to reduced risk of falling (76%) and number of ED visits (54%), and improved overall physical health (77%), emotional health (78%), and ability to remain at home (79%). The data were rich with multiple, powerful comments from clients in all 3 groups underscoring this theme including the following: Having a well-trained PCA improves the quality of care I receive: an untrained PCA is nothing more than a babysitter who is ill-equipped to handle my needs. (Group C) [Trained PCAs are] making me feel human again.(Group B) If they are well trained, they are more likely to recognize a problem before it becomes an emergency. (Group C) They know what to watch for and if possible prevent the issue that would cause the ER visit. (Group B) I get less infections because my PCA (BTBQ trained) knows how to properly clean me and any skin breakdowns. (Group A) My PCA follows all med orders, takes good care of my skin, feet and eyes. She feeds me good. She knows my needs before I do. (Group A) They keep me active and provide healthy meals, keep me from preventable accidents. If you’re healthy and happy, your system is also. (Group B) [My PCA] makes me feel cared for by treating me with respect and being sensitive to problems that erupt in my life. (Group C) [The] companionship helps me feel less helpless. (Group C) It helps cheer me up, I get very depressed, suicidal sometimes. (Group B)
Importantly, qualitative analyses substantiated differences between group A and groups B and C. Perhaps most compelling are the stories clients shared in which they described specific times when their PCA’s training made a critical difference in their life. The majority of these stories were from clients of BTBQ-trained PCAs and focused on the ability to respond in a person-centered way to serious situations in which an adverse event was happening or potentially could occur, as in the following exemplary quotes: I had surgery, leaked blood all over my bed sheets, my trained PCA knew how to get the blood out and care for my wound.…[She] supported my emotional embarrassment. My blood pressure dropped super low. I almost passed out at my kitchen table. She did not panic and knew what to do to keep me from falling and passing out. (Group A) My PCA learned the signs of having a heart attack and saved my life by getting me to the emergency room!!(Group A) I don’t think my aides had any training. [I’ve] had some real bad ones. (Group C) My right leg was broken once long ago by an untrained PCA not understanding the technique of positioning using the barrel roll. (Group C) In 911 call situations—presently PCAs freeze when it’s a need to call after a falling situation. I had to direct a PCA what to do after I fell outside recently. (Group C) I have never had a trained PCA that I know of. Once one of my girls did go to a training program but she moved to another state. I really think training would help…the main thing they need to know is how important it is to listen to clients and to follow directions! They need to know body mechanics. (Group C) I’m tired of training them. The first caregiver had a family of her own so she was a natural. The second one was the same way. Third one didn’t even know how to make a bed and spent most of the time on her cell phone. [I’ve had a] long string of PCAs that I’ve trained and I’m tired. (Group C)
Limitations
This pilot study had several limitations including the fact that one recruitment method was to have invitational packets given to clients by their BTBQ-trained PCA, which could have potentially introduced bias into the sample and findings. Bias was mitigated as much as possible by (1) providing PCAs with sealed packets so that contents were unknown, (2) explaining that the study could improve PCA training and make them eligible for participation in future studies, (3) requiring PCAs to send delivery confirmation to the Principal Investigator in order to receive their incentive, and (4) instructions to clients specifying that they should not ask their PCA for assistance. A second recruitment method relied on busy case managers with limited time to explain packet contents or the study to clients. Moreover, the study relied on frail older adults completing a lengthy survey. The difficulty of this could have been compounded by any cognitive impairments. These limits resulted in a fairly low sample size which makes it difficult to generalize to a much larger population. Although limits such as these, as well as challenges related to multiple partners (community based), issues of confidentiality, and identifying PCA/client dyads underscore the complexity of a project such as this, the study led to important lessons learned that will inform a larger study and the sample size was sufficient to be able to determine several significant, and critical differences between treatment and control groups.
Discussion
This study provides evidence that clients of BTBQ-trained PCAs had fewer ED visits and falls than clients of PCAs with lesser or other training, including CNAs. It also reveals several trends in support of BTBQ training, such as potentially lower hospital admissions, that warrant further investigation, using larger sample sizes.
Further, PCA training is highly valued by clients who clearly believe it contributes to both physical and emotional health and that insufficient training results in negative consequences. In summary, the wide range of skills required for PCAs to provide high-quality, person-centered care delivered with respect and dignity is critical for older disabled or frail adults staying safely in their own homes. Attaining this level of skill requires comprehensive training. While CNA training includes training appropriate for a nursing home setting, this study indicates that it is inadequate for those PCAs providing in-home care.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a Michigan State University Pearl J. Aldrich Endowment in Aging Related Research and Education award (RT083166).
