Abstract
Purpose:
To describe the unmet informational, psychological, emotional, social, practical, and physical needs and preferences for posttreatment survivorship care of individuals living with multiple myeloma to inform the development of relevant, person-centered, survivorship services.
Methods:
An exploratory, descriptive study using 2 focus groups with 14 participants, 6 to 49 months postdiagnosis.
Results:
Thematic analysis revealed 7 key themes: information needs, experience with health-care professionals, coping with side effects, communicating with family and friends, dealing with emotions, support needs, and living with the chronicity of myeloma. Participants described key characteristics of survivorship care relevant to their needs and indicated they would like a more whole of person approach to follow-up when the main treatment phases had completed.
Conclusion:
Participants in this study described unmet needs across a breadth of domains that varied over time. The development of flexible, person-centered approaches to comprehensive survivorship care is needed to address the considerable quality-of-life issues experienced by people living with multiple myeloma. Nurse-led care may offer 1 viable model to deliver enhanced patient experience—providing the vital “link” that people described as missing from their survivorship care.
Introduction
Around 1700 people are diagnosed with multiple myeloma (myeloma) each year in Australia with approximately 840 people dying from the disease annually (1). Myeloma is a malignant incurable plasma cell disorder (2). Treatment depends on disease stage, general health and age, aiming to suppress disease and control symptoms through chemotherapy, radiotherapy, immunotherapy regimens, including autologous transplantation (3,4). Symptoms of myeloma include bone pain, fractures, renal disease, anemia, infection, and fatigue, all of which have considerable impact on lifestyle, role functioning, and quality of life (5,6).
In a qualitative study of 20 people living with myeloma 5 years after diagnosis (7), the considerable impact on emotional, social, role and work-related areas of life, and fears regarding uncertainty of the future was described (7). In a survey of 113 hematological cancer survivors, including myeloma patients in the first 12 months following initial treatment (8), managing fear of recurrence was the most frequently endorsed unmet need (n = 42, 73%). This was followed by the need for care coordination (n = 22, 33%) with two-thirds (n = 39, 59%) reporting the opportunity to discuss diagnosis and treatment experiences with a health-care professional would have been helpful (8).
We set out to explore the experiences of a cohort of patients living with myeloma. In accordance with the definition of a cancer survivor as articulated by the National Coalition for Cancer Survivorship (9), patients recruited to this study were cancer survivors living with, through, and beyond a diagnosis of myeloma. Despite the recognized profile of chronic, complex symptoms and treatment side effects experienced by people living with myeloma, little is known about their preferences for support and survivorship care. This project aimed to establish the unmet needs and preferences for survivorship support in a cohort of patients 6 to 49 months postdiagnosis of myeloma.
Methods
Design
A descriptive, exploratory study was chosen, as it allowed for in-depth investigation of experiences and survivorship care needs of participants, while maintaining a focus on study aims, through the use of semistructured focus group prompts (10,11). Thematic content analysis was chosen as the approach to focus group data, ensuring issues of importance to participants were revealed (12). The study was undertaken in accordance with the ethical standards of the Human Research Ethics Committees of Sir Charles Gardiner Hospital (Ref. 2012-135) and the University of Notre Dame Australia (Ref. 013030F).
Sample
The local Cancer Registry recorded 248 new cases of myeloma between July 1, 2009 and December 1, 2013 from the study site. A manual search of patient hospital records determined the date of diagnosis and treatments received to ascertain study eligibility. The Death Registry was searched to avoid contacting families of deceased patients. Sixty-three eligible participants were sent a letter of invitation from the study site hematologist; a participant information and consent form and an opt-out form to be returned within 2 weeks. Six opt-out forms were returned, 5 without indicating a reason and 1 objection to recruitment. The research assistant telephoned remaining eligible participants (n = 57) 1 week later to further explain the study and provide focus group location and time details.
Inclusion Criteria
Aged between 25 and 85 years.
Fluent in English.
No cognitive impairment (as indicated by medical record or during recruitment process).
May be receiving oral chemotherapy considered as disease maintenance.
Exclusion Criteria
Receiving care or follow-up at another hospital (where experiences could have potentially influenced interview data).
Undergoing an autologous transplant (exposure to a group setting considered a potential health risk).
Focus Groups
Two 90-min focus groups were conducted at a large tertiary cancer center in Western Australia. All participants provided written informed consent prior to participation. Focus group questions were derived from a comprehensive literature review of key issues and concerns in this cohort and research team clinical experience (Table 1). They prompted participants to discuss informational, psychological, emotional, spiritual, social, practical, and physical needs, along with views about survivorship support and care.
Guiding Questions for Myeloma Focus Groups.

Focus groups were facilitated by a hematology clinical psychologist experienced in facilitating focus groups with vulnerable populations, digitally recorded, and transcribed verbatim. Codes replaced participant names, and clinician identifiers were removed to ensure anonymity of responses prior to analysis. Electronic transcriptions were stored in a password-protected file on a secure server.
Data Analysis
NVivo 11 was used to manage data and undertake analysis. Transcripts were read and analyzed independently by C.B., T.M., and K.T. with content assigned to codes and themes generated from the data (12). These researchers discussed the coding and reached consensus on emerging themes. Rigor of the data analysis process was ensured by applying the criteria of credibility, auditability, and fittingness (13). Independent coding and researcher checking to ensure categories accurately captured issues being discussed maintained credibility. Extensive use of examples from the data demonstrated fittingness. Auditability was maintained by documenting research planning through to analysis, and through a reflective process of discussion, and debrief with colleagues. The merging of individuals with and without hematology expertise added to the richness of interpreted data and provided a balance to the analytical process.
Results
Participants
Eighteen (31.5%) of 57 eligible individuals agreed to participate. Fourteen participants attended on the scheduled day (Figure 1). On average, 31 months (standard deviation [SD]: 13.8; range: 6-49 months) had elapsed since diagnosis. Thirteen participants had a partner and 5 indicated at least 1 child <20 years of age living at home. Participants in focus group 1 had received 1 line of treatment and an autologous transplant (n = 5). Seven participants in focus group 2 had received at least 2 lines of treatment. Five participants had received 1 autologous transplant, and 1 participant had received a second autologous transplant.
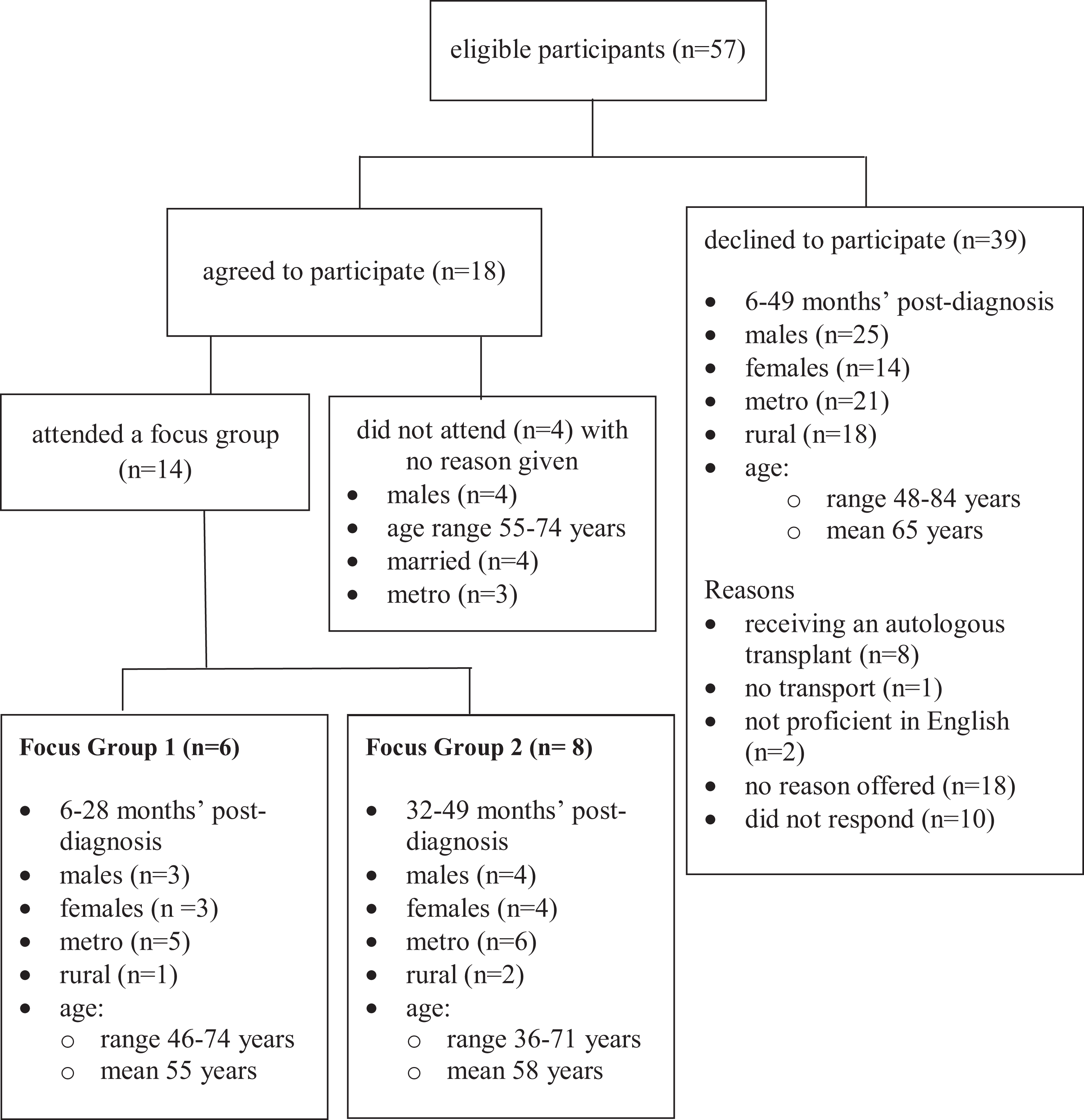
Recruitment and participant characteristics.
Age range and time since diagnosis were comparable with those who did participate. The majority of nonresponders preferred to not provide a reason (Figure 1).
Main Themes
The following 7 themes emerged and reflect data from both groups: information needs, experience with health-care professionals, coping with side effects, communicating with family and friends, dealing with emotions, support needs, and living with the chronicity of myeloma.
Information Needs (Box 1)
Information Needs and Experiences of Health-Care Professionals.

Participants had differing views about the amount of information they had received at diagnosis and most had never heard of myeloma before. Some were overwhelmed and felt they couldn’t absorb the information, others felt they were not given enough. All participants reported using the Internet. Many felt a list of reputable and reliable sites to search would have been helpful and may have made the diagnosis less confronting. [I] typed in multiple myeloma and read something about ‘it’s not curable’ and turned the computer off and went ‘no!’.…the average person out there who goes online doesn’t get the full medical details…that’s the information you want. (MM2-7)
Experiences with Health-Care Professionals (Box 1)
Participants suggest, in the main, their experiences of medical care were positive, but some said it was difficult to obtain “holistic support.” Participants discussed ways to maximize the value of their consultation appointments. Some indicated they would have liked to review blood results prior to appointments, to process the information and determine the “right questions to ask,” agreeing this would help reduce anxiety. …but if you’re told that [out of remission] at an appointment, you’re just in shock, you’re useless. So yes [before appointment] it does make a much better consultation. (MM2-2)
Coping With Side Effects (Box 2)
Coping With Side Effects.

Most participants struggled with treatment side effects, described as “the most difficult part of their experience.” Participants felt health professional support and guidance in preparing for, coping with, and managing side effects were inadequate. I found one of the challenging things is understanding and dealing with the side effects. My issue is about coping…so I never quite know if it’s an important side effect or not. I don’t want to waste the doctor’s time on unimportant things. (MM2 -1)
Participants described a sense of loss, as the disease and treatment had changed their life. They discussed the difficulty of appearing “well on the outside,” while dealing with challenging side effects not physically obvious to others. In a sense, the cancer was viewed as “forgotten,” and there was an expectation to resume normal duties and roles. Support from loved ones wavered when participants began to improve and look better.
Communicating with Family and Friends (Box 3)
Communicating With Family and Friends and Dealing With Emotions.

Families were supportive; however, at times the ways in which they tried to help was not useful or even wanted. There was a sense that family and friends were uncomfortable or unable to cope when the participant was “down” or wanted to talk about prognosis. One participant spoke of the difficulty in having to refuse advice perceived as helpful. …and in the end with all the herbal things and stuff I just had to say, ‘I’ve chosen conventional treatment, I’m happy, it’s working for me, just leave me alone’…. you’re trying to manage yourself but also all those people around you so it’s really hard work. (MM2-2) It’s very hard, she was only 9 when I was diagnosed, so, to try and tell her what was going to happen to me, we have to sort of tread lightly, because she’s known cancer to be deadly…both her grandparents [died]…to say those words that her mum had it, would’ve been just traumatic. I had to try and find ways to explain it to her, that I wasn’t going to end up in a coffin, you know? (MM1-2)
Dealing With Emotions (Box 3)
Many participants perceived stress was a contributing factor to their diagnosis and response to treatment. …stress, I think that’s a massive part of my diagnosis, I was separated [at] diagnosis…I have noticed that when it’s stressful…that’s when my levels go up. (MM2-3) Food and exercise. Book a holiday. Always have something to look forward to. (MM2-3)
A reluctance to accept professional psychological support was described and a few felt by the time they had an appointment the need had passed. Participants who had accessed an experienced cancer care psychologist at the hospital found it beneficial.
Support Needs (Box 4)
Support Needs and Living With the Chronicity of the Disease.

Gaps in service provision were identified during discussions, and participants made suggestions on what they would have found helpful. Participants described changing needs with regard to individual or group support at different stages in their cancer journey. They recognized individual differences existed in the types of support they may choose to access or want provided. Some found support groups useful to share experiences and gain informational, emotional, and social support. Others felt the group environment would be intimidating, or they would be unable to connect with others. Another issue was hearing about different treatment regimens, making them feel insecure about their treatment. However, for most there was a longing to be connected with others of a similar age and life stage. I found it really hard to go to the clinic and have my treatment because I didn’t want to be sitting next to people who were quite a bit older than me. I couldn’t talk to them because I felt like I didn’t have anything in common. Obviously I did, because I had the disease…MM1-2
Participants felt a health professional link/support person was required, who had expert knowledge, be able to offer information, advice, and provide reassurance. This person could also act as the contact between participants and the wider support team and help facilitate communication.
Living With the Chronicity of the Disease (Box 4)
Participants discussed the chronicity of myeloma, living with an incurable disease and inevitability of relapse. Well, they say ‘it’s going to come back, it’s not curable, it’s treatable, but don’t kid yourself because we can’t cure you’, so there’s always this ‘oh my gosh’. It’s tough because you know you’ve got to go through it all again [treatment]. (MM1-6) I’m not on drugs, I’m on a roll, and then you get symptomatic again and it was confirmed it was bad. It was devastating. (MM2-2)
Discussion
Reports of the experiences of people living with myeloma and a description of their unmet needs are limited in published literature (14,15). Our study contributes to an understanding of the experiences of care and treatment for this group of people. Consistent with recent work (16,17), our findings indicate that support is required for people to adjust to living with an incurable disease has an unpredictable trajectory of remission, relapse, and refractory disease (18,19). This is an important area for future intervention. Most of the people in our study had never heard of myeloma before their own diagnosis, and as such, the need to ensure that patients and their support networks are well informed about the disease and what they can do to keep themselves well is an important consideration for enhancing survivorship experience (20,21).
Treatment side effects were described as one of the worst aspects of the experience, with many people reporting feeling unprepared to recognize or cope with them (20,22). Preparation and strategies for self-management of side effects were identified as a priority area where more intervention is required. Fatigue and peripheral neuropathy were reported as particularly challenging, as they impact negatively on daily functioning and the quality of life (16). These present important areas for future multidisciplinary, survivorship research. Developing effective, feasible resources that enable prompt, access to information about the disease, its treatments, and side effects is an important focus for survivorship innovation to minimize or ameliorate these unmet and highly burdensome needs. Survivorship research to minimize the physical and psychological impact of the complex symptoms and side effects of myeloma is urgently needed.
System issues highlighted as opportunities to improve posttreatment experiences included knowing blood results prior to an appointment, as a way of reducing anxiety and maximizing time for discussions at hospital appointments (16), and ensuring a focus on addressing emotional needs as well as medical issues.
Participants spoke about having to manage family’s feelings and reactions while they tried to cope with their own. Development of survivorship services or resources targeted at family members/support networks may enhance posttreatment experiences for all affected by this disabling and complex disease.
Given the rarity and incurability of myeloma (23), some patients identified myeloma support groups as an important component of their survivorship care, providing information, emotional support, and a venue for shared understanding of their experience. A health professional “link” person was consistently identified as an important component of supportive survivorship care.
Limitations
This study reflects the views of a specific cohort of myeloma patients who self-selected to participate in our qualitative, exploratory study. The intent was to offer deeper understanding of the experiences of an underresearched group of people about whom we know little about their experiences. Given the intent of the work, the small number of people who took part and the heterogeneity across participants does not present methodological limitations as they would in a quantitative study. The findings are offered as an opportunity to build further research informed by patients’ experiences. We acknowledge that disclosure by the focus group facilitator of her role as a psychologist may have influenced the content participants chose to share and issues discussed, but the similarity of our data with that reported from other studies undertaken with this group of patients indicates that this did not influence the information shared.
Conclusion
Participants in this study described unmet needs across a breadth of domains that varied over time. The development of flexible, person-centered approaches to comprehensive survivorship care is needed to address the considerable quality-of-life issues experienced by people living with multiple myeloma. Nurse-led care may offer 1 viable model to deliver enhanced patient experiences—providing the vital “link” that people described as missing from their survivorship care.
Footnotes
Acknowledgments
We thank all participants for their willingness to take part in this important study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was supported by funding from the Cancer and Palliative Care Research and Evaluation Unit, Western Australian Cancer and Palliative Care Network.
