Abstract
Background:
The epidemiology of abdominal aortic aneurysm (AAA) is changing. Outcomes for aortic surgery have improved. However, the accepted guideline for the management of AAAs has remained unchanged over the last 2 decades. We aimed to gain insight into the patients’ experience while they are managed under the traditional clinical pathway.
Method:
With the help of a patient focus group, we designed a survey to assess the patients’ perception of the disease and their experience during different stages of the AAA clinical care pathway (surveillance, perioperative care, postoperative follow-up). An invitation to participate in the survey was sent to all patients with AAA who were receiving care at the Oxford Regional Vascular Services Unit, part of the Oxford University Hospitals NHS Trust.
Results:
We received 194 responses from patients with AAA. One hundred seventy-seven were male, with a median age of 75 to 79 years. Just over a third had undergone surgery already, and the remaining 63% were either in surveillance or awaiting surgery. Their experience during the AAA management pathway was mostly positive. Of the issues that were most important to them in terms of their medical care, the provision of explanation and regularity of monitoring stood out as the most common considerations.
Conclusion:
Patients are generally satisfied with the care they received, but there is room for improvement. They have also highlighted key areas that are most important to them in terms of their medical care. These should guide the future direction for quality improvement and research.
Introduction
An abdominal aortic aneurysm (AAA) is a pathological dilatation of the abdominal aorta and is typically defined by an AAA diameter >3 cm. Abdominal aortic aneurysms are a major public health-care problem. A catastrophic complication from untreated AAA is its gradual expansion and eventual rupture, leading to internal hemorrhage. Ruptured aneurysms result in high mortality even when treated by emergency surgery (1). There are approximately 10,000 deaths from ruptured AAA in the United States alone each year (2), with further 6,000 deaths from the United Kingdom (1).
Abdominal aortic aneurysms are often diagnosed incidentally from investigations performed for other purposes or via dedicated screening scans (1). In the NHS (National Health Service, United Kingdom), a national abdominal aortic aneurysm screening program (NAAASP) has been in operation since 2009 (3): Men are invited by the NAAASP to undertake a screening ultrasound scan when they reach the age of 65 years. Those diagnosed with a small AAA through this mechanism are offered an appointment with a specialist nurse to discuss the diagnosis and life style optimization. The existing guidelines recommends elective intervention when an AAA diameter exceeds 5.5 cm. Smaller AAAs are typically monitored on a regular basis, typically by ultrasound scans (4 -6). In the NHS, large AAAs (>5.5 cm) are referred for urgent review by a vascular surgeon with the aim to proceed to prompt surgical intervention. The surveillance of small AAAs depends on the AAA diameter (3 to 4.4 cm: yearly, 4.5 to 5.5 cm: 3 monthly). Information regarding every aspect of the management is also provided by dedicated NHS and Government websites (7,8).
Despite the clear recommendation by international guidelines, there are significant discrepancies in the adherence of this surgical threshold (AAA diameter of 5.5 cm) between different countries (9). For example, the average diameter of AAAs undergoing surgical intervention is lower in the United States compared to in the United Kingdom (10). Varied treatment patterns may be a result of the inherence differences in the health-care models. Although patient preference as an incentive driver for this is currently unknown, there is possibility that in a system with a fee for service environment, this plays a role in the clinical decision-making process.
It has previously been reported that patients who are diagnosed with AAA and placed in surveillance suffer a deterioration in Quality of Life scores (11). Patient anxiety has also been reported in the small aneurysm trials, and the crossover rate to the early treatment arm in the Positive impact of endovascular options for treating aneurysm early (PIVOTAL) trial was 11% after randomization, suggesting this effect plays a part, given the safety of surveillance (12).
Patient preferences do not currently form part of the decision-making algorithm in aneurysmal surgery. Outcomes for risk assessment are defined in terms of mortality, and softer outcomes such as patient anxiety are not factored in. In high-risk procedures, it is assumed that patients would prefer surveillance over intervention, but as the risk of mortality from the procedure decreases, the lines are not as clearly drawn. This survey of patients with AAA was conducted at a major regional vascular services hub in the United Kingdom. The aim was to ascertain patients’ experience during the NHS clinical care pathway, which encompasses surveillance and intervention.
Method
The survey was conducted as part of the Oxford Abdominal Aortic Aneurysm study (UK Southwest Research Ethics Committee approval Ref: 13/SW/250). We first engaged a patient focus group to help refine the survey questionnaire. This focus group consisted of patients with small AAAs under surveillance, a patient who had undergone surgical repair, a relative of a patient with an AAA, and a healthy volunteer. The aim of the focus group was to improve the wording and content of the survey to ensure we captured information that were important to the patients and that the wording is easily understandable. Participants to the focus group (listed in the acknowledgement of the manuscript) were sent the survey draft before the focus group meeting for prior reading. During the focus group session, we discussed each question of the survey and updated each section accordingly.
We sent the survey with a reply-paid envelope to everyone on the registry (n ∼ 600) of the Oxford Regional Vascular Services AAA database, at the Oxford University Hospitals NHS Trust, United Kingdom. We also made the survey available through several internet sites in order to allow potential participants to respond directly online. The active link to the survey is http://tinyurl.com/oxaaasurvey2016 (“e-supplemental material”). This survey was available on the following websites: (a) OxAAA study webpage—Nuffield Department of Surgical Sciences, University of Oxford (www.nds.ox.ac.uk/research/oxaaa), and (b) Patients Active in Research Thames Valley (http://patientsactiveinresearch.org.uk/oxaaa-survey-tell-us-what-you-think-is-important).
The nature of the survey was as such that patient would only respond to the survey if they gave implicit consent to take part. In the survey, participants had to provide basic demographic details such as gender and age but had the choice to remain anonymous. We included questions regarding aspects of the NHS clinical management pathway (diagnosis, monitoring, perioperative care, and postoperative follow-up). We asked for a response for each question either according to a visual analogue scale mapped to its corresponding description (eg, very clear, acceptable, not clear, and not applicable) or a binary response (yes or no). For most questions, we also allowed for the entry of free texts for comments.
Results
The focus group feedback was instrumental in implementing the final survey. They refined the type of questions asked, how they were asked and this ensured that it was simple to understand for a nonmedical audience. Examples of modification to the survey included the following:
Initially, we didn’t provide a field for patients to enter their name, as we wished to make this an anonymous survey. The focus group unanimously recommended that we should provide a “name” field as they would have liked to leave their name. Initially, we only included 2 questions regarding the provision of explanations during AAA: “Was there clear communication from the hospital (eg, about appointments)?” and “What would be done if/when your AAA had grown to ‘surgical’ size?” Based on the discussion during the focus group, the questions were updated to “Frequency of AAA monitoring?”; “What would be done if/when the AAA had grown to “surgical” size?”; and “What AAA surgery would involve, if/when that became applicable?” The focus group suggested to include the question: “If you had AAA surgery, how satisfied were you with your care on the ward? (very satisfied/acceptable/not satisfied).”
Of the 194 respondents, 177 were male with a median age of 75 to 79 years. Just over a third had undergone surgery already, and the remaining 63% were either in surveillance or awaiting surgery. The proportion of surgical patients receiving a traditional open operation compared to an endovascular repair (Endovascular aneurysm repair [EVAR], “keyhole”) was 3:2.
Of the 178 respondents that were enrolled as part of the surveillance program, 30 patients were “very preoccupied” with the size of their aneurysm and a further 63 were “somewhat” preoccupied by it. The remaining 85 were either “rarely” preoccupied (42/178) or said they “never think about it” (43/178) (Figure 1). Although 52% of the patients were preoccupied with their aneurysm, only 15% reported anxiety around the time of their surveillance scans. Patients were asked to comment on anything in the monitoring process that surprised them. Most of the comments relate to the key issues of information provision and frequency of monitoring (Table 1).
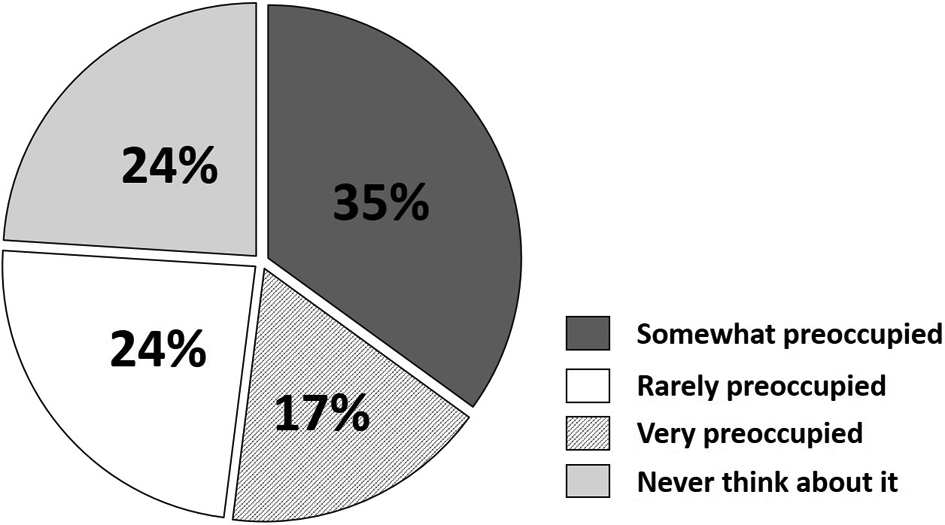
Patients’ response regarding how preoccupied they were with the size or growth of their aneurysm.
Comments Raised by the Patients Regarding if Anything Surprised Them During the AAA Surveillance Process.

Abbreviation: AAA, abdominal aortic aneurysm; EVAR, Endovascular aneurysm repair; NICE, onal Institute for Health and Care Excellence.
The majority of patients (72%) felt that the explanation of “what is an AAA?” was very clear and only a minority (3%) were not given an explanation or felt that the explanation of what an AAA was, and was not, clear (8%; Figure 2A). Eighty-nine percent of patients felt the that the explanation of what the monitoring process involved was explained very well (69%) or acceptably (30%), while a few felt that it was not clear (7%) or no explanation at all was given at all (3%; Figure 2B). Again, most of the patients (88%) felt that they were given a clear explanation regarding the reasons for surgery in the future.

Patients’ response regarding the explanation regarding the diagnosis of abdominal aortic aneurysm (AAA) and the surveillance process. A, Most patients felt that they were satisfied with the explanation that they were provided on “what is an AAA?” B, Similarly, they responded positively when asked if the monitoring process was adequately explained.
During the monitoring process, most patients felt that frequency of follow-up was well explained (78% very clear, 17% acceptable). Eighty-one percent felt that they were given a clear explanation of what would happen once the aneurysm had reached a “surgical size,” but the remaining 19% were not given an explanation (14% not clear, 5% no explanation at all). Also, a third were not given any explanation of what the surgery would involve. However, 92% of those that underwent surgery were satisfied by the care received in the ward (79% very satisfied, 13% acceptable). Their comments regarding if anything surprised them about surgery are listed in Table 2.
Comments Raised by the Patients Regarding if Anything Surprised them Regarding Their AAA Surgery.

Abbreviation: AAA, abdominal aortic aneurysm; RAF, Royal Air Force.
Patients feel strongly that an aortic aneurysm is not a disease. Only 21% of patients felt that aortic aneurysm is a disease. Their comments justifying their decision were related to it being noncommunicable, whereas all respondents who thought that it was a disease felt “cured” after the AAA surgical intervention.
When asked what was most important to patients in the AAA care pathway, 93 patients volunteered comments on the above question and there were 4 main themes: (a) provision of explanations and information (26 comments); (b) regularity of monitoring (25 comments); (c) that there is expertise in the health-care team (8 comments); and (d) immediacy in action when required (7 comments; Table 3). Upon further examination of these comments, there appears to be different emphases on what was most important to them in terms of their care related to AAA. About 80% of the comments relating to the regularity of monitoring came from those patients who were still under surveillance, whereas the majority of the other comments (relating to explanations offered during their care, immediacy of treatment when required, and their confidence in the expertise of the surgical team) came from those patients who have had surgery.
Comments Raised by Patients as to What Was Most Important to Them During the Clinical Care Pathway for Their AAAs.

Abbreviations: AAA, abdominal aortic aneurysm; ICU, intensive care unit; JRH, John Radcliffe Hospital.
Discussion
Our data provide a snapshot of patient experience in a contemporary cohort receiving aneurysm care within a regional NHS Vascular Services Unit. It is reassuring to see that in every category of questions, the far majority of patients registered a positive response. That a low minority of individuals chose a negative response for each of the questions serves as a reminder to clinicians that there is always room for improvement in every aspect of the clinical care delivery. It is important to note that this survey is not aimed to assess the patients’ quality of life, which requires a different assessment strategy.
Although patients reported being preoccupied with the size of their aneurysm, it was good to know that only a small proportion of patients was anxious about having the aneurysm. This may be related to the high levels of satisfaction with the explanations given, as well as the monitoring and follow-up process.
An interesting observation is the majority of patients do not view AAA as a disease, mainly as it is noncommunicable. This was interesting as we also surveyed over 200 vascular surgeons internationally to see whether they thought patients would view AAA a disease. In stark contrast, 80% of our vascular surgical colleagues thought patients would view their AAA as a disease (manuscript under revision). This only serves to highlight the differences in clinicians’ perceptions and that of patients.
Most importantly, our work identified several themes that patients felt were important to them regarding AAA management: provision of information and explanation and regular monitoring of AAA were the most frequently cited themes. In the NHS, screening for AAA has been implemented throughout the United Kingdom since the end of 2013. As part of the AAA screening program, extensive online resources are available for educating patients about the AAA management pathway (7,8,13). However, as the median age group of our patients is between 70 and 75 years, we need to be mindful that not all may be able to use the technology required to access the wealth of online information. It has also been shown that these online education materials may not be of sufficient quality and readability (14). Alternative aids may be helpful to enhance the patients’ experience during the clinical care pathway (such as signposting the library of information to family members who may be more adept at accessing the online information).
Although the provision of information/explanation is important to many patients, we also need to respect patients’ wishes regarding the amount of explanation each individual would prefer. It is clear that for some patients, having more explanation may not be to their benefit, as was the case for the patient who did not want to know much about their condition. The ability to tailor the amount of information to suit the individual patient is perhaps the one overlooked pillar of “personalised” medicine. These types of interaction skills should be a focus during medical and surgical training and hopefully the subject of further qualitative research.
As evident by comments listed in Table 3, the regularity of monitoring for AAAs is clearly a priority for many patients. In the existing guideline, the frequency of monitoring by the NHS AAA Surveillance Program is 12 monthly for aneurysms between 3 and 4.4 cm, and 3 monthly when above 4.4 cm in diameter. This schedule is based on the conventional wisdom that larger aneurysms grow faster than smaller aneurysms, which is likely to be true for the population in general. However, the landmark trials of AAAs have also demonstrated that the rate of AAA growth varies between individuals. Although the AAA screening program is offered at a population level, the surveillance interval for each patient could be personalized according to the individual’s propensity of AAA growth. Those with likely fast-growing AAAs would perhaps benefit from more frequent monitoring and vice versa. There is as yet no established biomarker for the prediction of future AAA growth (15). However, such candidate biomarkers are emerging (16,17). This highlights another pillar of personalized management in AAA that warrants further translational research.
Conclusion
We provide a snapshot of the experience of patients receiving AAA management in an NHS setting. The recruitment of a focus group facilitated a smooth survey process. Patients are generally satisfied with the care they received, but there is room for improvement. They have also highlighted key areas that are most important to them in terms of their medical care. These should guide the future direction for quality improvement and research.
Footnotes
Acknowledgment
The authors acknowledge the support by the following: Patient Active in Research Thames Valley; National Institute of Health Research (NIHR) Oxford Biomedical Research Centre; Research Development Services Southcentral Region UK; Medical Research Fund by Medical Sciences Division; and Oxford University Vice Chancellor’s Public Engagement for Research Seed Fund Award. The authors thank the following for their input during the patient focus group: (Lara Huttenga, Christina Burton, Trevor Lea, James Taylor, James De La Porte).
Declaration of Conflicting Interests
The author(s) declared no potential conflict of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
