Abstract
Quality and Patient Safety education for resident physicians is necessary to prepare them for independent practice and to meet accreditation requirements. Integrating such education into the residents’ routine work can provide them with valuable practical experience, while advancing the institution’s quality priorities. We committed to Quality and Patient Safety education for our pathology residents but found no published program that met their specific needs. To fill this gap in pathology residency education, we designed and implemented a new curriculum that spans the 4-year duration of residency training. Curriculum content was drawn from the pathology milestones, and educational strategies were based on the principles of adult learning. The curriculum was implemented in the 2018 to 19 academic year, and residents were assessed before and after their participation. The residents engaged in several Quality and Patient Safety activities and projects under faculty supervision, and improved their scores on objective assessments (Quality and Patient Safety quiz and in-service examination). Implementation was facilitated by a Quality and Patient Safety chief resident, and the recruitment of faculty with demonstrated Quality and Patient Safety interest. Our comprehensive Quality and Patient Safety curriculum is feasible to implement and can help pathology residents develop the knowledge and skills needed to lead quality initiatives. We believe that the curriculum framework is readily adaptable to other residency programs.
Introduction
Led by the release of To Err is Human: Building a Safer Health System by the Institute of Medicine, nearly 20 years ago, the health care industry has put great effort into optimizing Quality and Patient Safety (QPS). 1 As resident physicians are often frontline providers of health care, it is essential to integrate them into organizational quality initiatives. Quality and Patient Safety education for resident physicians was addressed by the Accreditation Council for Graduate Medical Education (ACGME) as far back as the 1999 Outcome Project 2 and is mandated by the present Common Program Requirements. 3 A recent review of over 9000 residency and fellowship programs reported an overall improvement in organizational QPS efforts but identified a shortfall in the integration of trainees in these efforts. 4
In pathology, serious interest in QPS was prompted by a 1987 newspaper article about “Pap mills,” high-volume cytology laboratories that prioritized quantity over quality. 5 This adverse publicity resulted in the quality requirements specified by the Clinical Laboratory Improvement Amendments (CLIA) of 1988, 6 giving pathology departments a head start in implementing QPS. However, the associated skills and methods have generally not been formally taught to residents. This education gap has significant implications for their future independent practice, where they will be expected to lead quality initiatives.
In 2014, we started work on developing a QPS program for our pathology residents. A literature search at the time yielded descriptions of QPS education programs for residents in several clinical disciplines. The programs were typically designed around didactic teaching and QPS projects. Most programs were offered as short rotations (weeks to months), and there were a few longer programs integrated through a year or more of residency training. 7 -13 However, no program addressed the scope of pathology practice, that is, the strict regulatory and accreditation requirements that must be satisfied, the highly process-driven nature of laboratory operations, and a practice environment in which vital information is often communicated without face-to-face contact. In this article, we describe the creation and implementation of a comprehensive QPS curriculum, intended specifically for pathology residents. We note that a patient safety curriculum for Anatomic Pathology residents was published while we were developing and implementing our curriculum. 14
Materials and Methods
Setting
Our pathology residency program is based at a large tertiary care center. The program has 83 faculty members and admits 7 residents each year. The clinical material available for resident education is obtained from over 18.5 million laboratory tests and procedures each year, including approximately 185 000 surgical pathology accessions and 250 autopsy cases.
Description of the Innovation
Curriculum design
We used the 6 steps of Problem Identification, Needs Assessment, Goals and Objectives, Educational Strategies, Implementation, and Program Evaluation. 15 Throughout the process, including the Implementation phase, we actively solicited input from the principal stakeholders, that is, the residents, the residency Program Director, and selected members of departmental leadership, and modified the curriculum in response to their needs and expectations.
We identified 4 major topics for the curriculum, based on the ACGME Pathology Milestones in effect at the time: Hand-off Communication, Error Management, Laboratory Accreditation and Process Improvement (HELP). 16 For each topic, we developed goals and specific objectives based on the residents’ routine work, and educational strategies based on the principles of adult learning, that is, self-directed learning, active learning through work-related activities, problem-centered learning, learning dependent on social context, and reflective learning (Table 1). 17,18
Curriculum Content, Format, and Attendance Requirements.

Abbreviations: CAP, College of American Pathologists; IHI, Institute for Healthcare Improvement; PGY, postgraduate year.
The self-study components of the curriculum were based on online courses from the Institute for Healthcare Improvement (IHI) Open School 19 and the College of American Pathologists (CAP), supplemented with pertinent journal articles 20 -28 and website links. Sets of assessment questions were developed to guide self-directed reading and to facilitate discussion in the faculty-led group sessions.
To identify any unanticipated, major practical difficulties, portions of the curriculum were field-tested on 2 senior residents (postgraduate year [PGY] 3-4). Their feedback on the quantity and quality of the content was positive; however, the task of implementing the curriculum for the entire program required further planning and creativity.
Curriculum delivery
Learning modules were created in our institution’s online residency management system (MedHub). The modules contained introductory components for self-directed learning, and faculty-led group sessions that included interactive discussion, video simulations, role-play, feedback, and reflection. In addition, residents participated in real-life QPS activities, namely, laboratory inspections, committee service and QPS projects. Completion of the modules was tracked automatically online for some components, and via the portfolio system for the remainder.
Curriculum implementation
We implemented the curriculum in the 2018 to 2019 academic year. A QPS chief resident 29 was selected from among the PGY3 and PGY4 residents, with responsibility for planning and tracking curriculum activities, and to represent the residents on departmental and institutional QPS committees.
The Hand-off Communication modules were administered every year, given the critical nature of the topic for the residents’ daily work. The other modules were administered on an approximately 2-year cycle. Thus, residents were engaged in QPS activities throughout their 4-year program and had the opportunity to repeat faculty-led sessions and reinforce learning.
Each year, 3 QPS projects were selected by the program director from among proposals submitted by the faculty. This selection was made in January, and every resident in the program was assigned to a project. The project teams had several months to work on their assignments, after which the results were reported at departmental Grand Rounds in December, and submitted for presentation at the institution’s annual Patient Safety Day event.
Curriculum assessment
A 42-question multiple-choice quiz based on the curriculum content was designed by the program director and QPS chief resident. This quiz was administered to the residents before starting the curriculum and again, after approximately 10 months. The question set is provided as Supplementary File 1.
De-identified (aggregate average) results of the Laboratory Administration category of the Pathology Resident In-Service Exam (RISE; ASCP) were reviewed for the year before and the 2 years after curriculum implementation.
A 4-question survey was developed by the program director to gauge the residents’ ease with QPS topics. This survey was administered before starting the curriculum and again, after the first year. The survey questions are provided as Supplementary File 2.
We were advised by the institutional review board that our curriculum assessment was exempt from review, as it was a part of the evaluation of an educational program.
Results
Outcomes Measured
After a year of participating in the QPS curriculum, there was an increase in mean scores on the QPS quiz (Table 2) and the RISE Laboratory Administration section (Table 3) for every PGY level. Improved RISE scores were also noted for the resident cohorts progressing from 1 PGY level to the next (Figure 1).
Mean Scores (%) on the QPS Quiz Before Implementing the QPS Curriculum and Approximately 10 Months After Curriculum Implementation.
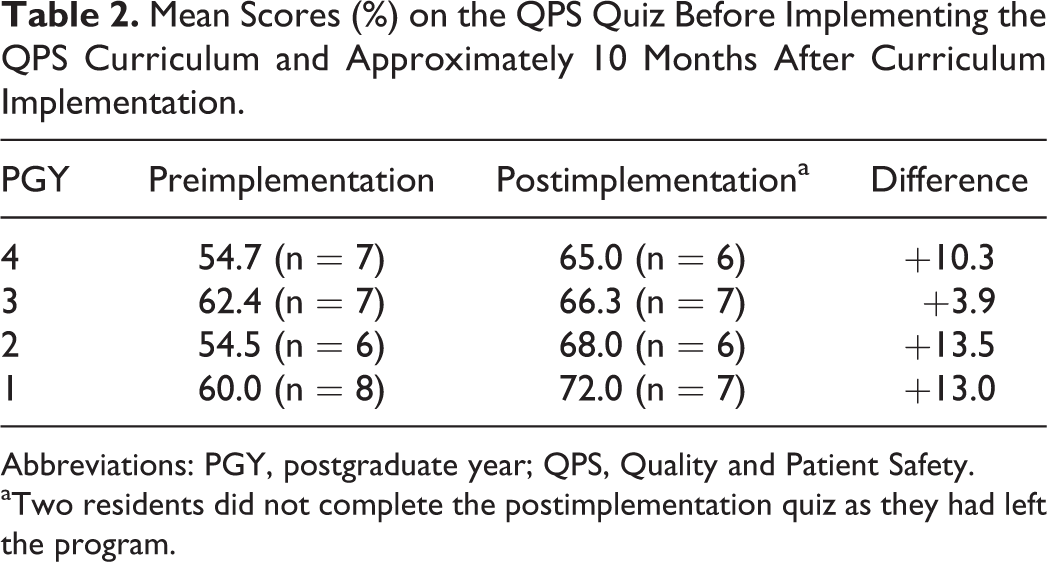
Abbreviations: PGY, postgraduate year; QPS, Quality and Patient Safety.
aTwo residents did not complete the postimplementation quiz as they had left the program.
Aggregate Average RISE Laboratory Accreditation Section Scores (Percentile) Before and After Implementing the QPS Curriculum.
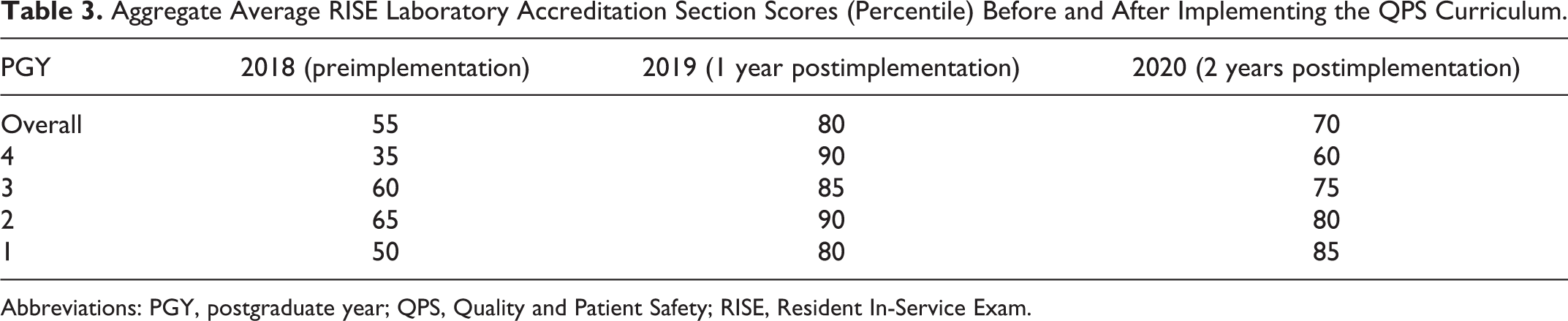
Abbreviations: PGY, postgraduate year; QPS, Quality and Patient Safety; RISE, Resident In-Service Exam.
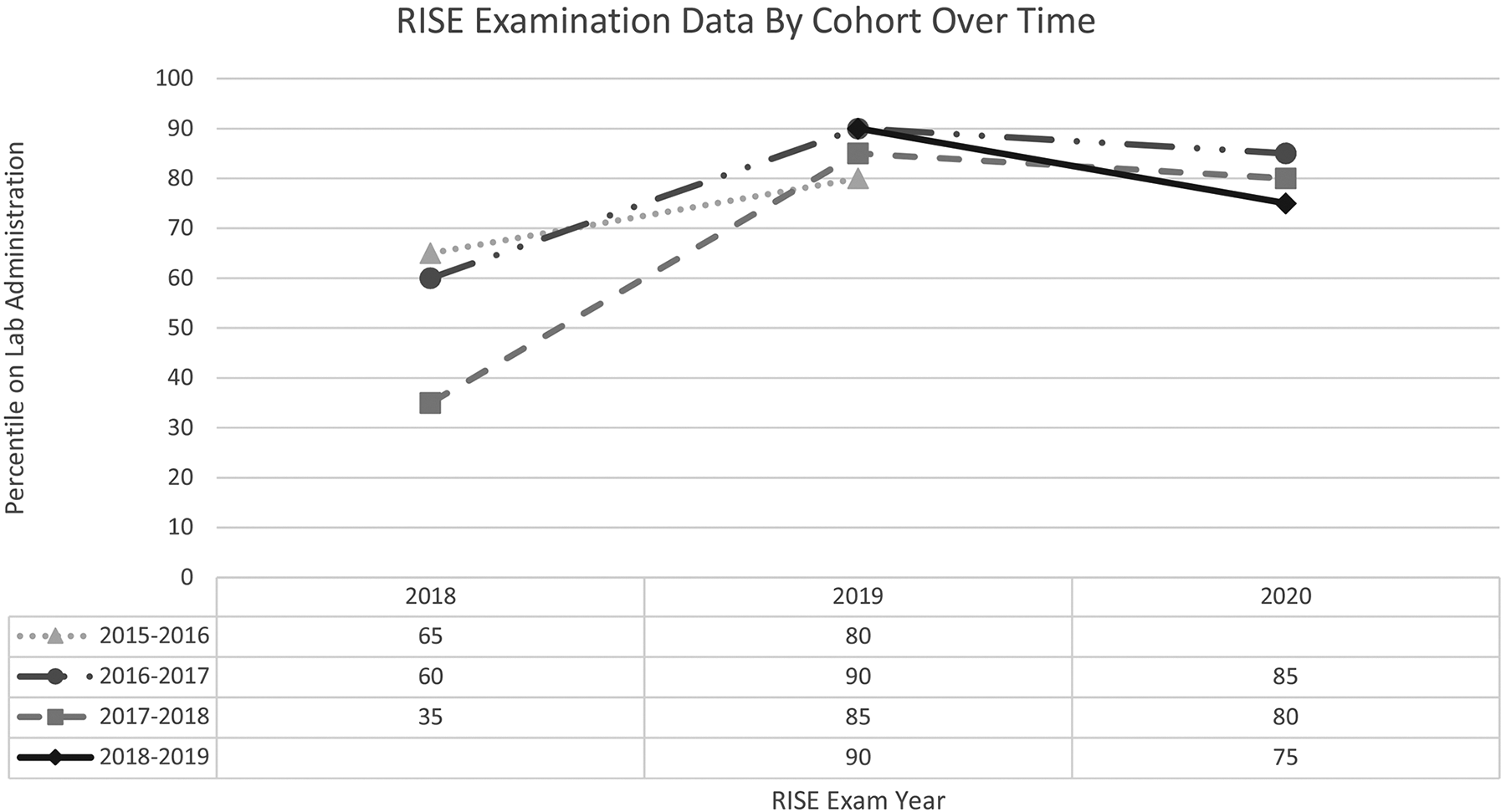
Aggregate average RISE laboratory accreditation section scores (percentile) by PGY cohort before (RISE year 2018) and after (RISE years 2019 and 2020) implementing the QPS curriculum. The label for each cohort indicates the first year of residency. PGY indicates postgraduate year; QPS, Quality and Patient Safety; RISE, Resident In-Service Exam.
The residents’ QPS projects included topics in blood management, laboratory reference ranges, handling of urgent samples, callback of critical results, and frozen section sampling, all of which were closely aligned with the department’s quality and operational priorities. In the two years since implementation of the curriculum, every PGY2-4 resident has completed one project each year. All of the projects were presented internally, and one secured the best poster award at the 2019 institutional Patient Safety Day event. In addition, all of the projects were presented externally, including 2 at national conferences.
Quality committees on which the residents have served include 11 intradepartmental and 2 cross-departmental committees. The average length of service was 3 months.
The laboratory accreditation inspections conducted by the residents include internal midterm inspections and one inspection of an external laboratory.
Cost
The design of the QPS curriculum was funded through an institutional Medical Education Fellowship awarded to one of the authors. The cost of creating the QPS chief resident position included support for attending a national QPS meeting (up to USD 1750, up to 5 meeting days) and the CAP Laboratory Director online course (cost USD 180).
The time commitment for coordinating QPS activities was estimated at approximately 12 hours a month. The QPS chief resident was not provided with protected time for this responsibility.
There was no additional direct cost for curriculum implementation; the online courses (IHI, CAP) had already been purchased for other educational use, and curriculum delivery and tracking were achieved through existing systems.
Feasibility
The self-directed components of the learning modules allowed the residents significant flexibility in time management. However, organizing the faculty-led group sessions was challenged by time constraints and faculty participation. To address the time constraints, we scheduled faculty-led sessions during existing slots in the residents’ regular lecture calendar. We used only four slots over the entire year by simultaneously running the sessions for PGY1-2 (4 meetings) and PGY3-4 (3 meetings). To encourage faculty participation, the program director invited key faculty members with high engagement in QPS and residency education (eg, laboratory directors, section heads). Four such faculty members led the group sessions for review of self-assessment questions, and for the simulation sessions on hand-offs, root cause analysis, proficiency testing and test utilization.
The QPS chief resident had an invaluable role in facilitating delivery of the curriculum and overcoming day-to-day implementation challenges. His involvement included orienting new residents in QPS at orientation, scheduling group sessions, assisting the faculty to develop content for group sessions, updating curriculum content (eg, course links), coordinating resident assignments for committee service and laboratory inspections, monitoring resident completion of assigned modules, and acting as a liaison for quality and patient safety issues involving the department.
As the process of selecting QPS projects is repeated every year, every resident may expect to participate in at least 3 QPS projects, building significant QPS experience and expertise over the duration of residency.
Acceptance
Most residents (60%) felt that the curriculum provided the right amount of content. They reported an increased ease with QPS issues after the first year of the curriculum, with 60% of residents indicating that they felt “somewhat comfortable” or “very comfortable,” compared to 39% before curriculum implementation. Significantly, one-third of the residents reported QPS projects as an effective educational strategy, compared to only 6% before curriculum implementation.
Discussions at the monthly pathology education committee meetings indicate that the residents have come to value the unique experiences of practical QPS activities that form the backbone of the QPS curriculum. Their acceptance of the QPS curriculum has been likely boosted by the ready affirmation of their constructive feedback, which has been channeled into curriculum improvements.
Discussion
We report the successful implementation of a comprehensive new QPS curriculum intended specifically for pathology residents and integrated into the entire 4-year duration of their training. As the practical elements of the curriculum, including quality projects, quality committees, and inspections, are integral and ongoing parts of pathology operations, the residents’ participation in these activities have required little more than coordination of scheduling by the QPS chief resident. The residents have shown sustained objective improvement in QPS knowledge and have successfully completed several QPS projects in support of the department’s quality agenda. Group participation in QPS projects has encouraged the development of mentoring relationships between junior and senior residents, and promoted the equitable distribution of workload.
After our 2-year implementation experience, we expect the additional effort of maintaining the curriculum to be limited to calendar coordination and minor content updates. However, we plan to continue using objective assessment and subjective feedback to ensure that it meets the residents’ needs for QPS education.
While the QPS curriculum was developed specifically for a pathology residency program, our experience with its design and implementation is limited to a single institution, and only short-term outcome data are available. The definitive measure of our curriculum, the reported experience of our graduates entering practice and dealing with real-life quality initiatives, is awaited. Nevertheless, our QPS curriculum offers a framework that other residency programs—pathology or non-pathology—may adapt to suit their own context. Potential users of this curriculum may elaborate further on its elements, by creating tools to evaluate the quality of learning and developing a formal faculty development program. We suggest, however, that implementation of the curriculum not be delayed until every detail is in place; the educational value of an imperfect process that must be negotiated through trial and error should not be underestimated, especially in the context of learning QPS.
In conclusion, we believe that the new QPS curriculum is helping our residents to gain the knowledge, skills, and experience needed to supervise a laboratory and contribute effectively to quality and practice improvements in pathology. Integrating the curriculum into routine practice has ensured that the residents are actively engaged in departmental quality priorities. The curriculum can be feasibly implemented within the time and resource constraints of a busy pathology residency program.
Supplemental Material
Supplemental Material, sj-pdf-1-apc-10.1177_2374289521998046 - Implementation of a Quality and Patient Safety Curriculum for Pathology Residency Training
Supplemental Material, sj-pdf-1-apc-10.1177_2374289521998046 for Implementation of a Quality and Patient Safety Curriculum for Pathology Residency Training by Suneeti Sapatnekar, Ryan Demkowicz and Deborah J. Chute in Academic Pathology
Supplemental Material
Supplemental Material, sj-pdf-2-apc-10.1177_2374289521998046 - Implementation of a Quality and Patient Safety Curriculum for Pathology Residency Training
Supplemental Material, sj-pdf-2-apc-10.1177_2374289521998046 for Implementation of a Quality and Patient Safety Curriculum for Pathology Residency Training by Suneeti Sapatnekar, Ryan Demkowicz and Deborah J. Chute in Academic Pathology
Footnotes
Authors’ Note
This work was presented in poster form at the 2015 and 2020 ASCP Annual Meetings:
Sapatnekar S, Figueroa PI, Colbert CY. A quality improvement curriculum for Pathology residents. ASCP Annual Meeting, October 28-30, 2015, Long Beach, CA.
Demkowicz R, Sapatnekar S, Chute D. Quality and Patient Safety in a Pathology Residency Training Program. 2020 ASCP Annual Meeting (virtual event).
Acknowledgments
The authors gratefully acknowledge the invaluable guidance of Colleen Colbert, PhD, Director of Educator & Scholar Development, Education Institute, Cleveland Clinic. The authors thank Karl Theil, MD, former Residency Program Director, Cleveland Clinic, for identifying resources and mechanisms of module deployment. The authors thank Amber Smith, MD, and Joseph Sanfrancesco, MD, for field testing the curriculum.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The creation of the curriculum described in this manuscript was supported by a Medical Education Fellowship awarded by the Education Institute, Cleveland Clinic, to Suneeti Sapatnekar, MD, PhD.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
