Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040. 1
Keywords
Primary Objective
Objective SP1.2: Differential Diagnosis. List the major differential diagnoses for each type of cytology or surgical pathology specimen derived from a lesion or mass and describe appropriate further studies, both special stains and immunohistochemistry.
Competency 3: Diagnostic Medicine and Therapeutic Pathology; Topic: Surgical Pathology (SP); Learning Goal 1: Role in Diagnosis.
Secondary Objectives
Objective N3.1: Morphologic Features of Neoplasia. Describe the essential morphologic features of neoplasms and indicate how these can be used to diagnose, classify, and predict biological behavior of cancers.
Competency 1: Disease Mechanisms and Processes; Topic: Neoplasia (N); Learning Goal 3: Characteristics of Neoplasia.
Objective N1.1: Genetic Mechanisms of Neoplasia. Discuss and provide examples of molecular genetic mechanisms that underlie cancers, including germline mutations (including point mutations, deletions, amplifications, and translocations) and epigenetic changes.
Competency 1: Disease Mechanisms and Processes; Topic: Neoplasia (N); Learning Goal 1: Genetic Basis of Neoplasia.
Patient Presentation
A 63-year-old female with no prior history of pancreatitis is found to have an incidental pancreatic cyst on a computed tomography (CT) scan for a workup of appendicitis. The patient does not report a smoking or alcohol abuse history. The patient denies itching, unintended weight loss, nausea, vomiting, diarrhea, or changes in stool color. Her family history is notable for a grandparent diagnosed with pancreatic cancer at the age of 59 years old.
Diagnostic Findings, Part 1
The patient’s physical examination is only remarkable for right lower quadrant tenderness. The abdomen is soft, nondistended, and positive for bowel sounds. No mass, rebound, or guarding are noted. Her sclera are anicteric. Her liver enzymes, chemistries, and complete blood count are within normal range. Computed tomography findings include a 31 mm hypoattenuating lesion within the pancreatic head and body with no obvious connection to the pancreatic duct. No evidence of main pancreatic duct dilation is identified.
Questions/Discussion Points, Part 1
What Is the Prevalence of Pancreatic Cystic Lesions and Their Significance?
The occurrence of incidentally detected pancreatic cystic lesions is continuously growing due to the increasing use of cross-sectional imaging. The overall population prevalence is estimated to be between 2.5% and 13.5% and shows a strong correlation with increasing age, with 40% of patients over the age of 70 found to have pancreatic cyst(s) after review of magnetic resonance imaging for non-pancreatic indications. 2 -4 Pancreatic cystic lesions can progress into pancreatic cancer, one of the most lethal cancers in the United States with an overall 5-year survival of 8%. 5 The probability of a pancreatic cyst harboring malignancy at the time of imaging, however, is only 0.25% with an overall conversion rate to invasive cancer being 0.24% per year. 6 Surgical intervention is the preferred curative option, but the procedure carries high risks for postoperative morbidity and mortality. 7 Due to the high prevalence, low risk of malignant progression, and high risk of postoperative complications, an evidence-based and cost-effective approach to patient management was recommended by the American Gastroenterological Association and American College of Gastroenterology. 6,8,9 These algorithms guide clinical treatment decisions in which cysts do not need regular surveillance, which should be observed by periodic surveillance, and which require immediate surgical intervention.
What Are Common Pancreatic Cyst Causing Symptoms?
A minority of pancreatic cysts can cause significant clinical symptoms, but the majority of pancreatic cysts are incidentally found and are asymptomatic. Common presenting symptoms from patients with symptomatic pancreatic cysts include abdominal pain (69%), weight loss (38%), pancreatitis (36%), jaundice (18%), back pain (18%), palpable mass (5%), and postprandial fullness (4%). 10 Symptomatic pancreatic cysts are more likely to be malignant compared to asymptomatic pancreatic cysts (36% vs 14%). 11 Therefore, symptomatic pancreatic cysts should be evaluated for surgical resection. The clinical management of asymptomatic cysts, however, relies on identifying the small minority of cysts with premalignant or malignant potential.
What Is the Differential Diagnosis of Pancreatic Cystic Lesions?
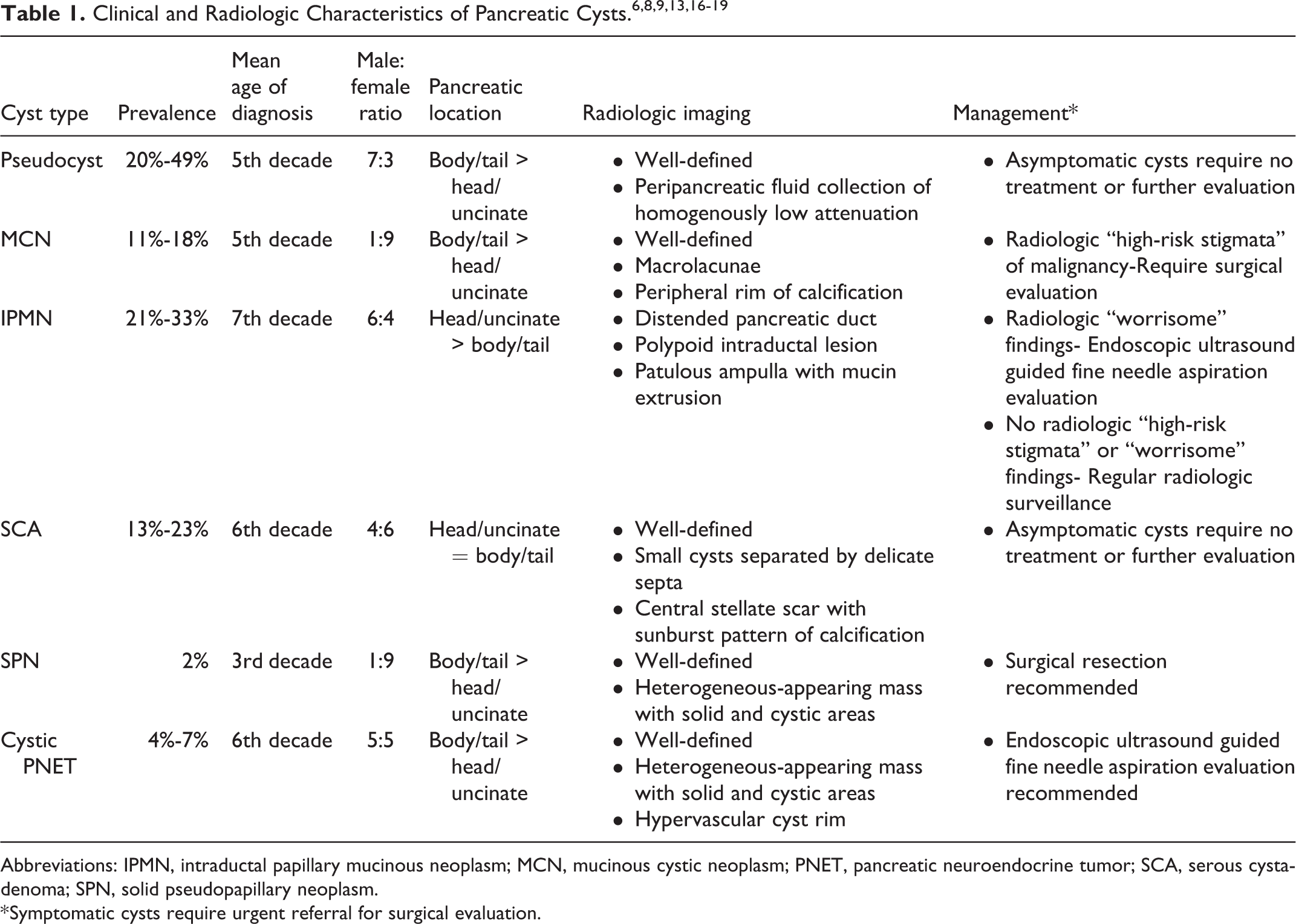
The differential diagnosis of pancreatic cystic lesions is broad and can be categorized as nonneoplastic versus neoplastic cysts. 12 Nonneoplastic cysts include pseudocysts that most commonly occur in patients with a known history of acute and chronic pancreatitis. Pseudocysts are localized collections of necrotic material and inflammatory infiltrate that lack an epithelial lining. If asymptomatic, pseudocysts do not require surveillance or treatment. 8,9 Neoplastic mucin-producing cystic neoplasms include mucinous cystic neoplasm (MCN) and intraductal papillary mucinous neoplasm (IPMN). Mucinous cystic neoplasms are mucin-producing epithelial neoplasms that do not communicate with larger pancreatic ducts. Intraductal papillary mucinous neoplasms are papillary mucin-producing epithelial neoplasms that arise in the main pancreatic duct and/or pancreatic branch ducts. The majority of IPMNs and MCNs are indolent. A significant minority undergo malignant transformation with 30% prevalence in IPMNs involving the main pancreatic duct, 15% prevalence in IPMNs involving a branch duct, and 15% prevalence in MCNs. 13 -16 Neoplastic non-mucin-producing cysts include serous cystadenoma (SCA) and cystic degeneration of solid tumors, such as solid pseudopapillary neoplasm (SPN) and pancreatic neuroendocrine tumor (PNET). Serous cystadenomas are epithelial cystic neoplasms that are well circumscribed and contain thin, watery serous fluid. The risk of malignant progression in SCAs is extremely low at 0.1%, and these lesions are considered clinically benign. 17 Solid pseudopapillary neoplasms are rare neoplasms showing solid and pseudopapillary areas with large areas of hemorrhagic necrosis and pseudocystic spaces. Malignant transformation is seen in approximately 20% of cases, but the long-term prognosis following resection is excellent with a 95% 5-year survival. 18 Pancreatic neuroendocrine tumors with cystic degeneration are commonly nonfunctional and may occur sporadically or in individuals with a genetic predisposition, such as multiple endocrine neoplasia type 1 and tuberous sclerosis. Although cystic pancreatic neuroendocrine tumors show a lower metastatic rate compared to non-cystic neuroendocrine tumors (9.7% vs 34.1%), long-term prognosis is similar in both cystic and non-cystic neuroendocrine tumors (92%). 19 Classic clinical and radiologic findings in pancreatic cysts can be found in Table 1.
Abbreviations: IPMN, intraductal papillary mucinous neoplasm; MCN, mucinous cystic neoplasm; PNET, pancreatic neuroendocrine tumor; SCA, serous cystadenoma; SPN, solid pseudopapillary neoplasm.
* Symptomatic cysts require urgent referral for surgical evaluation.
Diagnostic Findings, Part 2
The patient undergoes abdominal magnetic resonance imaging (MRI) for further evaluation of her pancreatic cyst. Findings include a cluster of cysts in the pancreatic head and body, the largest of which measures 31 × 25 × 22 mm with thin septations. Possible side branch involvement is noted. No main pancreatic duct involvement or mural nodule are identified. The main pancreatic duct is not dilated.
Questions/Discussion Points, Part 2
What Radiologic Findings Warrant Further Evaluation?
The initial evaluation of pancreatic cysts consisted of imaging to characterize the type of cyst and to assess for high-risk features defined by international consensus guideline recommendations. 8,9,20 Magnetic resonance imaging and magnetic resonance cholangiopancreatography (MRCP) are radiologic tests of choice due to lack of radiation exposure and increased assessment accuracy. 6,8,9 Computed tomography and endoscopic ultrasound (EUS) can be used as alternatives in patients unable to undergo MRI. Radiologic findings of “high-risk stigmata” of malignancy, which include an enhancing mural nodule ≥5 mm and dilation of the main pancreatic duct ≥10 mm, should undergo surgical resection without further workup. 8,9,20 “Worrisome features” found on imaging include pancreatic cysts ≥30 mm, enhancing mural nodule <5 mm, dilation of the main pancreatic duct 5 to <10 mm, thickened and enhancing cyst walls, abrupt change in the main pancreatic duct caliber with distal pancreatic atopy, lymphadenopathy, and rapid rate cyst growth ≥5 mm/2 years. 20 If “worrisome features” are present, further evaluation with EUS-guided fine needle aspiration (EUS-FNA) for fluid analysis, cytologic evaluation, and molecular analysis are warranted. 8,9,20 Patients with asymptomatic pancreatic cysts <30 mm without radiologic findings of “high-risk stigmata” and “worrisome features” should undergo radiologic surveillance according to cyst size (<10 mm, 10-<20 mm, 20-<30 mm) for at least 5 years. 8,9,20
Diagnostic Findings 3
An upper EUS-FNA is performed due to the presence of radiologic “worrisome features.” Imaging shows an anechoic and distally enhancing cystic lesion measuring 31 × 26 × 24 mm within the pancreatic head and body. The cyst has thin walls and is found to communicate with a side branch of the pancreatic duct. There is no associated mural nodule or internal debris within the fluid-filled cavity. A diagnostic needle aspiration is performed, and 0.8 mL of slightly viscous fluid is collected and sent for fluid analysis, cytology, and molecular analysis. Cytologic evaluation shows an adequate specimen with cytomorphologic features shown in Figure 1A and B. High-grade epithelial atypia is not seen. Analysis of cyst fluid chemistry shows an elevated carcinoembryonic antigen (CEA; 850 ng/mL) and amylase (810 IU/l). Molecular testing identifies a KRAS mutation (p.G12V) and GNAS mutation (p.R201H) with absence of additional alterations to include TP53, PIK3CA, PTEN, AKT1, and SMAD4.
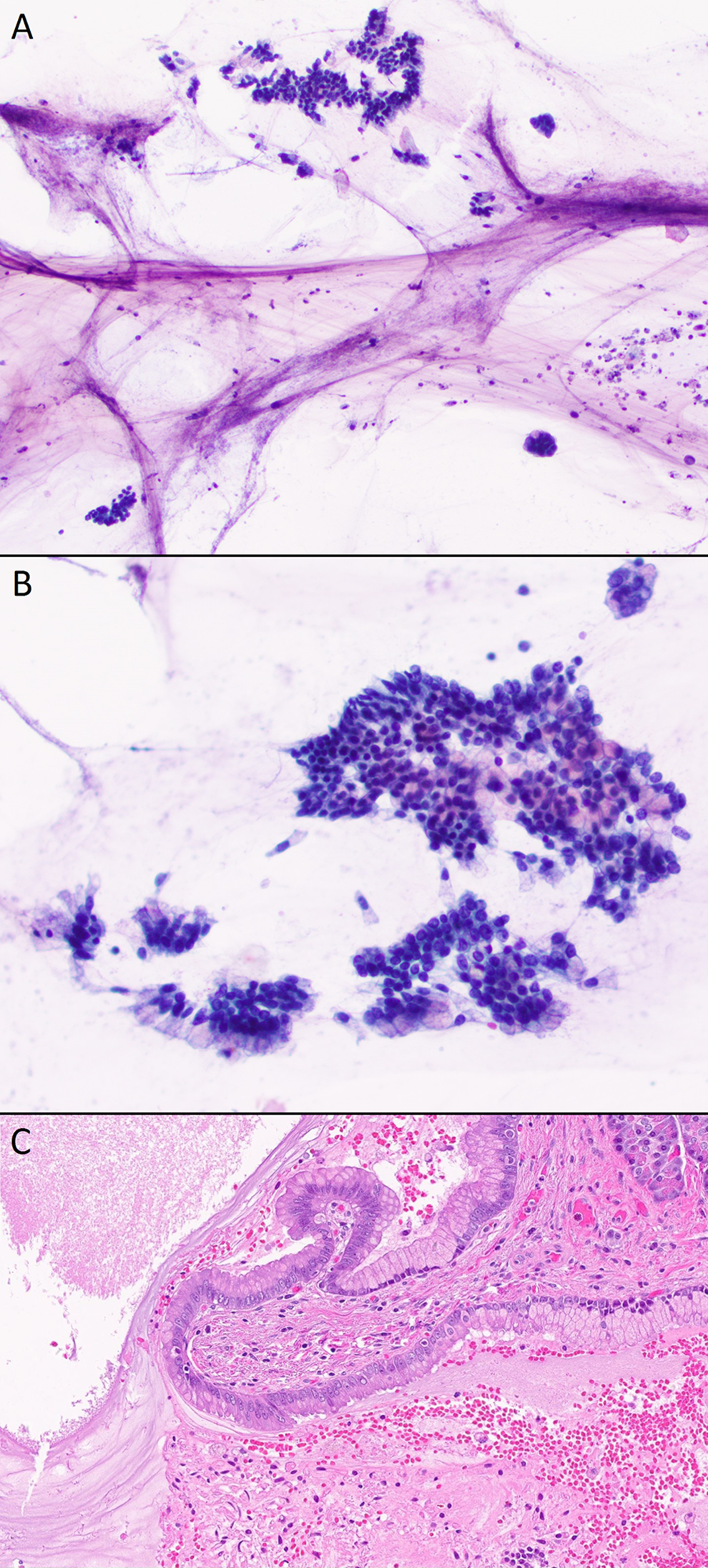
Endoscopic ultrasound-guided fine needle aspiration cytologic (A, B) and histologic (C) correlation of a pancreatic mass. A, Image showing a thick sheet of colloid-like mucin covering most of the slide with scattered foamy histiocytes and few clusters of epithelial cells (Papanicolaou stain, ×100). B, Image highlighting benign-appearing cyst lining epithelial cells in sheets and groups with mucin filling the entire cytoplasm (Papanicolaou stain, ×200). C, Image demonstrating intraductal papillary mucinous neoplasm papillae lined by tall columnar mucin-producing epithelial cells (hematoxylin and eosin, ×200).
Questions/Discussion Points 3
What Is the Role of Cyst Fluid Analysis in Characterizing a Cyst Type?
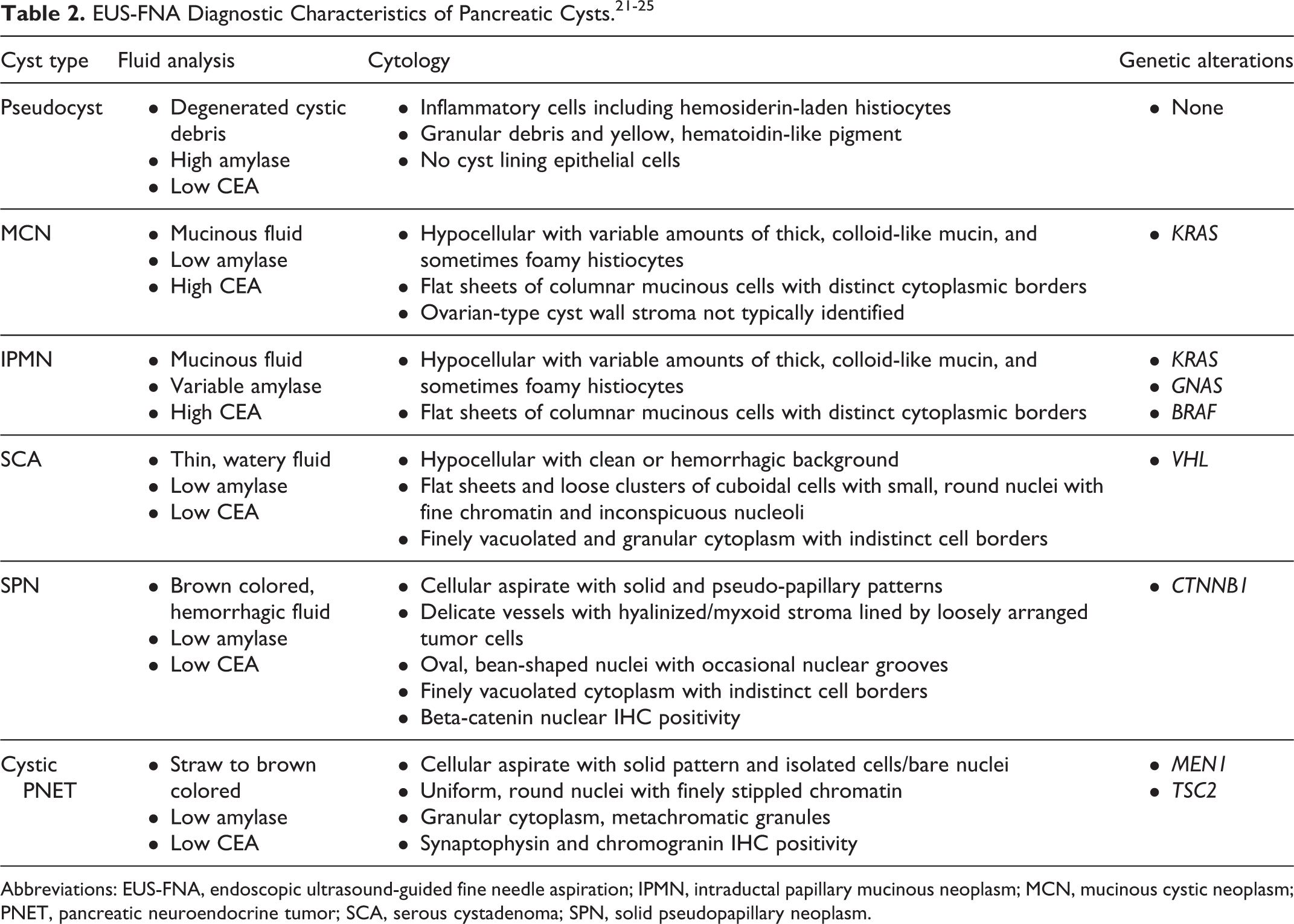
The most commonly measured cyst fluid proteins are CEA and amylase. Meta-analysis has shown that elevated CEA levels >192 ng/mL can help differentiate mucin-producing pancreatic cysts (IPMN and MCN) from non-mucin producing pancreatic cysts, with a sensitivity of 75% and a specificity of 84%. 21 Carcinoembryonic antigen >800 ng/mL has a specificity of 98% and strongly suggests a mucin-producing pancreatic cyst. 22 Amylase is elevated in lesions communicating with pancreatic ducts (pseudocyst, IPMN). Pancreatic cysts with amylase levels <250 IU/L can exclude pseudocysts in 98% of cases. 22 Characteristic cyst fluid biochemical findings of common pancreatic cysts are shown in Table 2. Although CEA and amylase cyst fluid levels can help narrow the differential, cyst fluid chemical analysis cannot be used to identify IPMNs and MCNs with high-grade dysplasia or pancreatic cancer.
Abbreviations: EUS-FNA, endoscopic ultrasound-guided fine needle aspiration; IPMN, intraductal papillary mucinous neoplasm; MCN, mucinous cystic neoplasm; PNET, pancreatic neuroendocrine tumor; SCA, serous cystadenoma; SPN, solid pseudopapillary neoplasm.
What Are Limitations and Advantages of EUS-FNA Cytologic Evaluation?
Although hampered by low cellularity specimens, EUS-FNA cytologic evaluation of a pancreatic cyst can aid in classifying, diagnosing, and determining malignant potential. Classifying cysts as nonneoplastic versus neoplastic and mucin-producing versus non-mucin producing cysts is one important aspect of cytologic evaluation. Identifying inflammatory cells and background debris with no epithelial cyst lining suggests a pseudocyst. Cuboidal cells with granular to clear cytoplasm are seen in SCA. Epithelial mucinous cells with extracellular, thick, and colloid-like mucin are indicative of MCN and IPMN (Table 2). Meta-analysis studies have shown that although cytologic evaluation has a high specificity (88%-93%) for identifying mucinous cysts, the pooled sensitivity was only 54% to 63%. 23,26 The main reason for lower sensitivities is due to low cellularity of pancreatic cyst FNA specimens, with one prospective study finding only 34% of cytology samples having adequate cellular material for evaluation. 26 A second important aspect of cytologic evaluation is identifying high-grade dysplasia or pancreatic cancer in IPMNs or MCNs. Mucinous cysts with high-grade dysplasia show tight atypical epithelial cell clusters with nuclear crowding, loss of polarity, hyperchromatic nuclei, high nuclear to cytoplasmic ratio, and irregular nuclear membranes. 27 The presence of marked anisonucleosis, irregular nuclear membranes, prominent nucleoli, irregular clumps of chromatin separated by clear areas (parachromatin clearing), and background cellular debris/necrosis suggests the possibility of invasion (Figure 2). 27 Cytology may underestimate histologic grade, however, due to low cellularity and cyst lining heterogeneity. 21,28
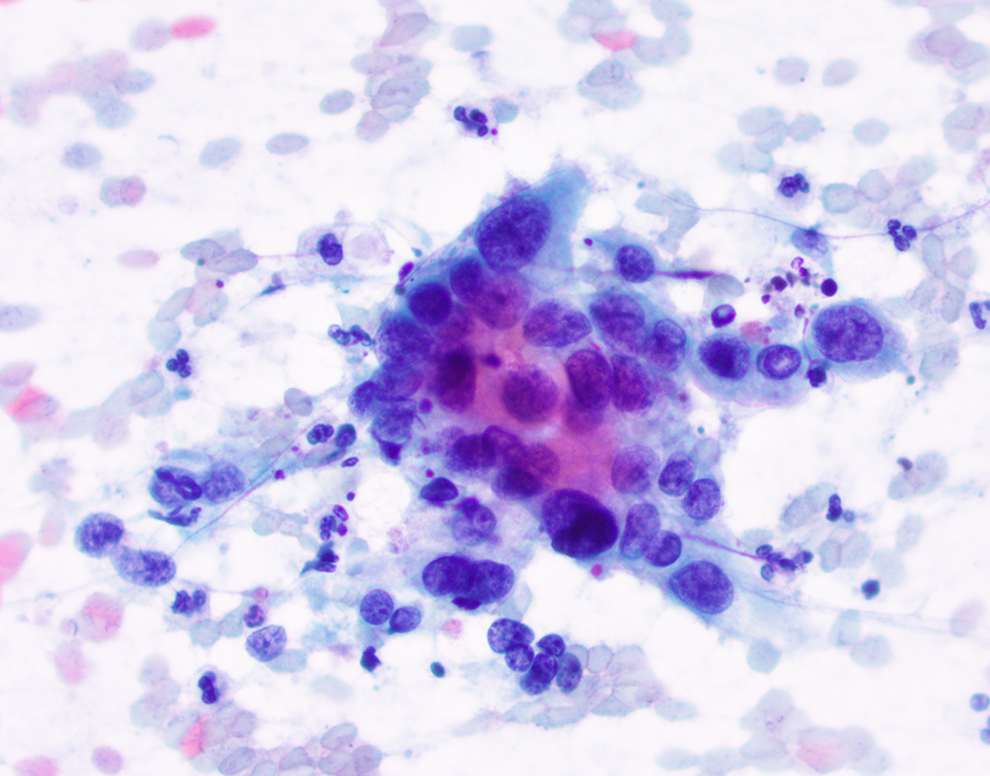
Cytomorphologic features of pancreatic mucinous cysts with advanced neoplasia. Image showing a cluster of atypical epithelial cells with marked anisonucleosis (4:1), irregular nuclear membranes, prominent nucleoli, parachromatin clearing (Papanicolaou stain, ×400).
What Role Does Molecular Testing Have in Pancreatic Cyst Workup?
Molecular studies have identified a number of characteristic genetic alternations that can be used diagnostically and prognostically to classify pancreatic cysts (Table 2). Nucleic acids isolated from exfoliative epithelial cells in pancreatic cysts fluid samples in FNA samples are sequenced using technologies such as next-generation sequencing (NGS). Targeted regions of DNA are isolated, amplified, sequenced, and analyzed to assess for mutations and copy number alternations. Intraductal papillary mucinous neoplasms are characterized by KRAS, GNAS, RNF43, BRAF, and CTNNB1 mutations in over 95% of cysts. 24,25,29 -31 Mucinous cystic neoplasms also have been characterized by KRAS, RNF43, and CTNNB1 mutations in 14% to 50% of cysts but do not harbor GNAS and BRAF mutations, making these mutations specific for IPMN. 24,25,29 -32 Serous cystadenomas and SPNs classically show VHL mutations and CTNNB1 mutations, respectively, in over 90% of cases. 24,25,30,31 Cystic PNET diagnoses can be supported by finding MEN1 and TSC2 mutations. 24,25 In addition its diagnostic role, molecular testing has shown to have a prognostic role when characterizing pancreatic cystic neoplasms. Intraductal papillary mucinous neoplasms associated with high-grade dysplasia and early invasive pancreatic cancer were found to have mutations in KRAS and/or GNAS with concurrent alterations in TP53, PIK3CA, PTEN, or AKT1 in 60% to 88% of cases. 14,24,25,33 Accurate molecular studies are dependent on adequate sampling and preservation of the specimen to limit false negative results.
Based on the Clinical, Radiologic, Cyst Fluid Analysis, Cytologic, and Molecular Findings, What Is Your Diagnosis?
Taken together, the results are indicative of a side branch IPMN with no features of high-grade dysplasia on cytologic and molecular evaluation. Clinical and radiologic findings were suggestive of an IPMN centered in the pancreatic head and body with connection to a side branch. Endoscopic ultrasound-FNA demonstrated a slightly viscous fluid with elevated CEA and amylase. Cytologic evaluation showed thick, colloid-like mucin (Figure 1A) and flat sheets of columnar mucinous cells with distinct cytoplasmic borders (Figure 1B). No cytomorphologic features of high-grade dysplasia or invasive pancreatic cancer were seen. A histologic correlate to the cytological findings is shown in Figure 1C. Furthermore, NGS was positive for mutations specific for IPMN with an absence of mutations associated with advanced pancreatic neoplasia. Due to the low risk of developing pancreatic cancer and high risks associated with surgical resection, the clinical team opposes surgical intervention and recommends biannual cyst surveillance by MRI for at least 5 years. 6,8,9
Teaching Points
Pancreatic cysts are common and often detected incidentally on imaging.
The majority of pancreatic cysts are asymptomatic, and symptomatic pancreatic cysts often present with nonspecific clinical findings.
The differential diagnosis of a pancreatic cyst includes nonneoplastic cysts (eg, pseudocyst), mucin-producing neoplastic cysts (eg, MCN and IPMN), and non-mucin producing neoplastic cysts (eg, SCA, SPN, cystic PNET) that have classic clinical and diagnostic findings.
Magnetic resonance imaging and MRCP are the radiologic tests of choice when characterizing pancreatic cysts and determining malignant potential.
EUS-FNA with cyst fluid analysis, cytology, and molecular testing should be considered in indeterminate pancreatic cysts with radiologic “worrisome features.”
In the absence of concerning radiologic or diagnostic findings that warrant surgery in presumed MCNs and IPMNs, cyst surveillance is recommended for at least 5 years.
Overall, pancreatic cysts have a low risk of malignant potential. Pancreatic surgical intervention portends high risks for postoperative morbidity and mortality; therefore, a multidisciplinary and multimodal diagnostic approach is warranted when determining clinical management strategies.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.