Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective P2.2: Clinical Features of Pancreatic Adenocarcinoma. Explain how the location of a pancreatic neoplasm determines its presenting symptoms and discuss the risk factors for pancreatic adenocarcinoma.
Competency 2 Organ System Pathology; Topic P: Pancreas; Learning Goal 2: Pancreatic Neoplasia.
Secondary Objectives
Objective P2.1: Neoplasia of the Pancreas. Describe the major types of neoplasms affecting the exocrine pancreas.
Competency 2 Organ System Pathology; Topic P: Pancreas; Learning Goal 2: Pancreatic Neoplasia.
Objective SP1.4: Staging. Describe the information that the pathologist obtains from a resected tissue specimen, how this information is reported, how it is combined with clinical information to stage the tumor, and how staging information is used to guide treatment.
Competency 3 Diagnostic Medicine and Therapeutic Pathology; Topic SP: Surgical Pathology; Learning Goal 1: Role in Diagnosis.
Patient Presentation
A 67-year-old male presents to his primary care physician complaining of yellowing of his eyes. He first noticed his “eyes looked different” 2 months ago and since then has experienced increased fatigue and decreased hunger. He notes that his urine has been darker and his stools have been paler than usual. He has no known medical problems, prior surgeries, or significant family history. He drinks 6 beers a day but has never used tobacco or illicit drugs.
Diagnostic Findings, Part 1
Physical exam reveals yellowing of the sclera and mucous membranes. He has mild epigastric tenderness to palpation. There are no other abnormalities on physical exam and he has no blood on rectal exam.
Since his last appointment 6 months ago, he has had an unintentional weight loss of 15 pounds. At this appointment, he has a temperature of 98.7 °F, a blood pressure of 126/82, a pulse of 74 beats per minute, a respiratory rate of 18 breaths per minute, and an oxygen saturation of 98%.
Questions/Discussion Points, Part 1
What Are the Major Classifications of Jaundice? What Are Their Differential Diagnoses?
The patient’s history suggests he may be suffering from jaundice, which can be of prehepatic, hepatic, or posthepatic origin.2,3 Prehepatic jaundice is usually due to hemolysis, which causes an increased release of unconjugated bilirubin into the bloodstream. This results in an increased unconjugated bilirubin level and an abnormal complete blood count (CBC) on laboratory testing. 3 Hepatic jaundice is usually due to hepatocellular damage, which can be secondary to ischemia, toxins, infection, or autoimmune disease. It is associated with elevated aspartate aminotransferase (AST), alanine aminotransferase (ALT), alkaline phosphatase, γ-glutamyl transpeptidase (GGT), and total bilirubin. 2 Since hepatic jaundice can also be caused by congenital impairments in bilirubin conjugation, it can present with elevations in either conjugated or unconjugated bilirubin. 3 Finally, posthepatic jaundice is usually due to biliary obstruction secondary to gallstones, pancreatitis, or malignancies of the biliary system or pancreas. 4 It results in an increase in conjugated bilirubin and alkaline phosphatase, with mild to moderate increase in transaminases. This differentiates it from hepatic jaundice, which has a disproportionate rise of AST and ALT in comparison to the rise in alkaline phosphatase. 2
How Should This Patient Be Worked Up?
The first step in elucidating the origin of this patient’s jaundice is determining whether it is due to unconjugated or conjugated bilirubinemia. This is assessed through serum testing of direct and total bilirubin levels. By calculating these values, indirect bilirubin levels, which are a measure of unconjugated bilirubin, can be deduced. These levels should be done in conjunction with a CBC, AST, ALT, GGT, and alkaline phosphatase. The CBC is useful in indicating whether there is ongoing hemolysis, as there is often an associated decrease in hemoglobin and hematocrit. Aspartate aminotransferase and ALT are indicators of hepatocellular injury while alkaline phosphatase and GGT are markers of cholestasis. When viewed together, these tests can point toward either a hepatocellular or cholestatic origin of a patient’s jaundice. 3 Additionally, if there is concern for pancreatitis, amylase and lipase levels should be drawn. 2
Imaging also plays a pivotal role in delineating the exact cause of a patient’s jaundice. Transabdominal ultrasound should be performed first, as it is cheap and noninvasive. 3 It is useful in detecting stones in the biliary tree and it is highly sensitive for tumors greater than 3 centimeters. 5 If ultrasound is inconclusive, computed tomography (CT) of the abdomen can be performed, as it is useful in diagnosing pancreatitis and smaller masses. 5 Endoscopic retrograde cholangiopancreatography and magnetic resonance cholangiopancreatography (MRCP) are additional studies to help visualize the ductal structures of the biliary system and pancreas. Endoscopic retrograde cholangiopancreatography uses an endoscope to access the pancreatic and bile ducts through the ampulla of Vater in the duodenum. The physician can then inject contrast material into these ducts and subsequently take X-rays of the biliary tree. 2 An MRCP uses magnetic resonance imaging to create a 3-dimensional image of the pancreaticobiliary tree, liver parenchyma, and vascular structures. 3 These studies are useful if there is no evidence of gallstones or masses on ultrasound and the cause of biliary obstruction is unclear.2
If the cause of a patient’s jaundice is still unclear after laboratory studies and imaging are performed, a patient can undergo a liver biopsy. This should only be performed if the results would change patient management, which it does in only about one-third of cases. 3
Diagnostic Findings, Part 2
The primary care team orders a CBC, total bilirubin, direct bilirubin, AST, ALT, GGT, alkaline phosphatase, and lipase. They also order a transabdominal ultrasound.
3
Complete blood count: White blood cells: 5.3 × 103/µL (4.1-10.9 × 103/μL)2
Hemoglobin: 14.2 g/dL (13.8-17.2 g/dL)2
Hematocrit: 42.1% (40%-52%)2
Platelets: 214 × 109 /L (150-400 × 109 /L)2
Liver function tests: Total bilirubin: 15 mg/dL (0.1-1.2 mg/dL)2
Direct bilirubin: 14.4 mg/dL (< 0.3 mg/dL)2
ALT/AST: 60 U/L (7-56 U/L)2/40 U/L (3-35 U/L)2
GGT: 186 U/L (8-88 U/L)2
Alkaline phosphatase: 336 U/L (33-131 U/L)2
Lipase: 87 (6-70 U/L)2
Transabdominal ultrasound: Common bile duct is mildly dilated with no evidence of a stone in the biliary tree.
Following these findings, the team decides to order a CT, which shows hypoattenuation, an area brighter than the surrounding tissue, in the head of the pancreas.
Questions/Discussion Points, Part 2
How Should These Results Be Interpreted? What Conditions Need to Be Ruled Out?
The patient’s laboratory testing results reveal that he has conjugated hyperbilirubinemia, as only his direct, and not his indirect, bilirubin is elevated. Conjugated hyperbilirubinemia can be associated with either hepatic or posthepatic jaundice, as described previously, so it is important to consider his other test results when coming to a conclusion as to the origin of his jaundice. His hemoglobin and hematocrit are normal, suggesting against a hemolytic cause for his jaundice. The patient’s marked increase in alkaline phosphatase and GGT, mild elevations in AST and ALT, and recent history of pale stools and dark urine suggest he most likely has cholestasis. These findings, in addition to imaging showing bile duct dilation and abnormal tissue in the head of the pancreas, point toward a posthepatic jaundice secondary to biliary obstruction at the level of the pancreas. Additionally, his normal white blood cell count and mildly, as opposed to markedly, elevated lipase levels suggest against infection and acute pancreatitis. 2,3
Biliary strictures can be secondary to benign or malignant causes. Benign causes, for example, include chronic pancreatitis, autoimmune disease like primary sclerosing cholangitis, gallstone complications, surgical complications, sphincter of Oddi dysfunction, choledochal cysts, infection, and inflammation. Malignant causes include cholangiocarcinoma originating from the cells of the bile duct, pancreatic carcinoma usually arising from the ductal cells of the pancreas, and ampullary carcinoma from cells distal to the confluence of the common bile and pancreatic ducts. 4
The most important diagnosis to rule out in our patient is pancreatic carcinoma. Pancreatic carcinoma is often associated with fatigue and weight loss, similarly to our patient, and has a poor prognosis. If the neoplasm is in the head of the pancreas, it will often present with painless jaundice and elevated alkaline phosphatase. Another diagnosis to consider is chronic pancreatitis, especially when considering the patient’s alcohol abuse history. Chronic pancreatitis can present with symptoms of biliary stricture and can mimic the appearance of pancreatic carcinoma on imaging. Gallstone pathology is less likely in our patient’s case, due to the absence of stones in the biliary tree, but should be considered, as should autoimmune disease and other carcinomas that present with obstructive jaundice. 2,5,6
What Lesions Can Arise in the Pancreas?
Within the pancreas, both benign and malignant lesions can develop. Benign lesions of the pancreas include serous neoplasms and pseudotumors. Serous neoplasms are rare, accounting for 1% of all pancreatic lesions, and are ductal-type tumors that produce abundant glycogen. Pseudotumors are a heterogeneous category of mass-producing lesions that mimic malignancy and include cysts, heterotopia, hamartoma, and lipomatous pseudohypertrophy. These lesions are important to diagnose properly, as they can present similarly to malignant lesions of the pancreas. 6
In terms of malignant neoplasms, 95% arise from exocrine elements of the pancreas. Ductal adenocarcinomas are the most common lesions, accounting for 85% of all pancreatic neoplasms. They arise from the small ducts of the gland and have a 3:1 head: body/tail ratio. Ductal adenocarcinomas are usually poorly circumscribed and moderately-to-poorly differentiated on diagnosis. They are highly associated with tobacco smoking as well as obesity, alcohol abuse, diabetes mellitus, and chronic pancreatitis. They often present with jaundice, back pain, unexplained weight loss, pruritus, diabetes mellitus, migratory thrombophlebitis, acute pancreatitis, hypoglycemia, and hypercalcemia. 5,6
Other malignant neoplasms that can arise in the pancreas include solid pseudopapillary neoplasms, acinar cell carcinomas, pancreatoblastomas, and neuroendocrine tumors. Some other pancreatic tumors, like intraductal papillary mucinous neoplasms and mucinous cystic neoplasms, are not necessarily malignant but have malignant potential, therefore needing to be entirely examined to exclude carcinoma arising from the neoplasm. 5 -7
Describe the Precursor Lesions and Molecular Changes in the Development of Pancreatic Adenocarcinoma
Invasive adenocarcinoma of the pancreas arises from pancreatic ductal epithelium. It starts as dysplastic change, which is then graded, based on degree, from low to high grade and called pancreatic intraepithelial neoplasia (PanIN) 1, 2, or 3. Within these precursor lesions, there is a spectrum of morphological changes that can occur, ranging from mild dysplastic changes in PanIN1 to severe dysplastic changes in PanIN3. Pancreatic intraepithelial neoplasia is a preinvasive lesion associated with large hyperchromatic nuclei, loss of nuclear polarity, irregular nuclear borders, prominent nucleoli, and increased mitotic activity which may be atypical. Over time, dysplastic ductal epithelial cells of PanIN3 start to invade the stroma, leading to the development of invasive ductal adenocarcinoma (Figure 1). 7
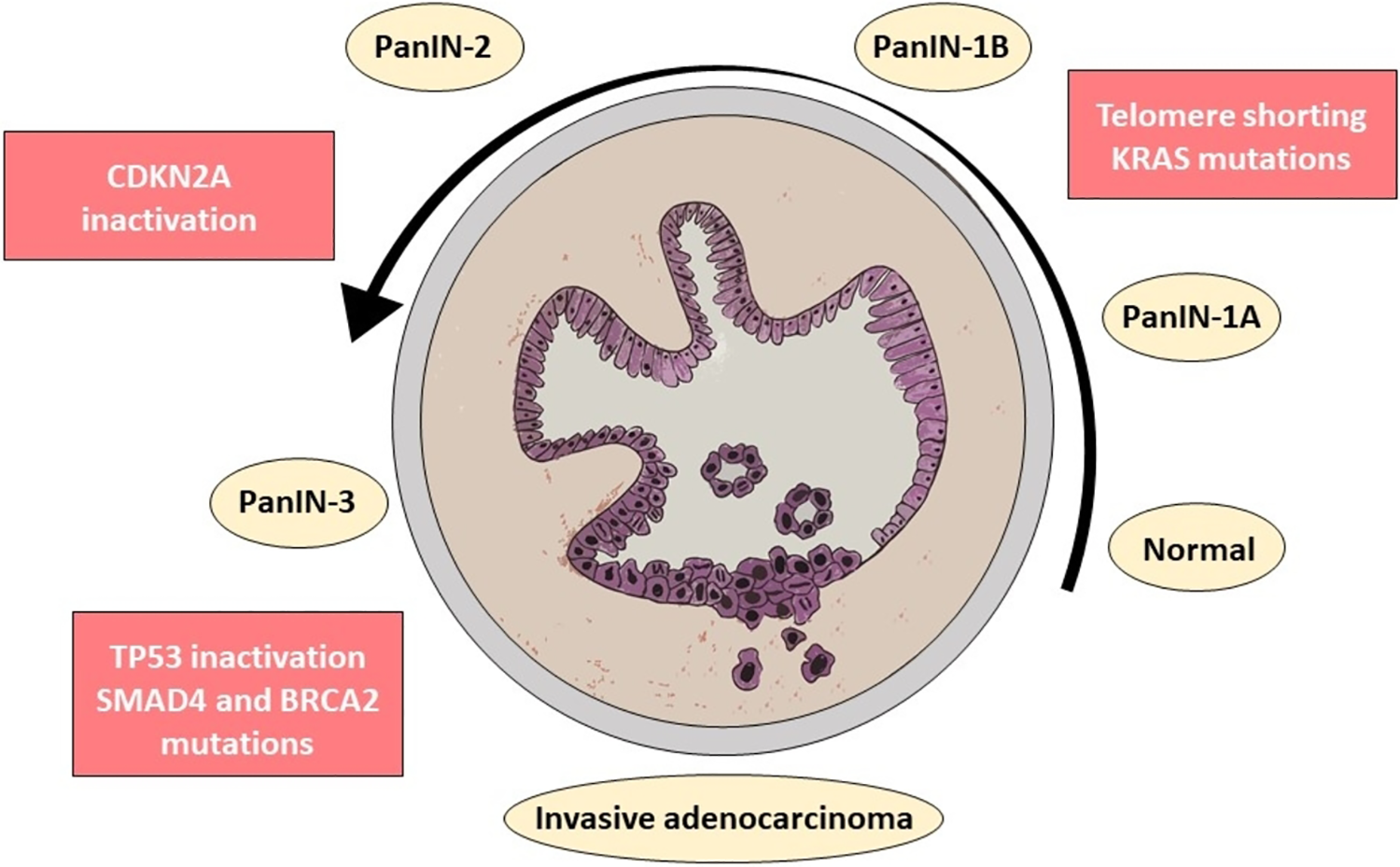
Sketch demonstrating a pancreatic duct with progressive dysplastic changes of ductal epithelium leading to invasive ductal adenocarcinoma (arrow shows the direction of changes). The associated molecular changes are shown.
In the development of invasive ductal adenocarcinoma, pancreatic ductal epithelium will show an accumulation of chromosomal mutations. In early low-grade PanIN lesions (PanIN1), marked telomere shortening is noted along with KRAS oncogene mutations. In intermediate-grade PanIN (PanIN2), inactivating mutations in the CDKN2A gene are observed. In high-grade PanIN (PanIN3) and invasive adenocarcinoma, inactivating mutations in tumor protein p53 (TP53), breast cancer type 2 susceptibility protein, and mothers against decapentaplegic homolog 4 genes are noted. CDKN2A and TP53 are tumor suppressor genes that play an important role in the control of cell cycle progression (Figure 1). 7,8
What Is the Next Best Step?
When differentiating between pancreatitis and pancreatic carcinoma, further workup, specifically imaging-guided biopsy, is warranted. The method of choice is endoscopic ultrasound (EUS)–guided fine-needle aspiration (FNA), as it allows for better visualization of small pancreatic lesions than CT scan and permits simultaneous diagnosis and staging, with real-time visualization of the needle tip, invasion of local structures, and local metastases. Endoscopic ultrasound–guided FNA is more commonly used than conventional core biopsy when sampling pancreatic lesions because next-generation FNA needles (19-25 gauge) allow for better tissue collection and fewer procedure-associated complications, like acute pancreatitis, hemorrhage, or tumor seeding. Additionally, FNA is extremely useful when fluid collection and analysis are important, as in cystic lesions. 5,7,9
Diagnostic Findings, Part 3
The patient underwent an EUS-guided FNA with the cytology smears showing:
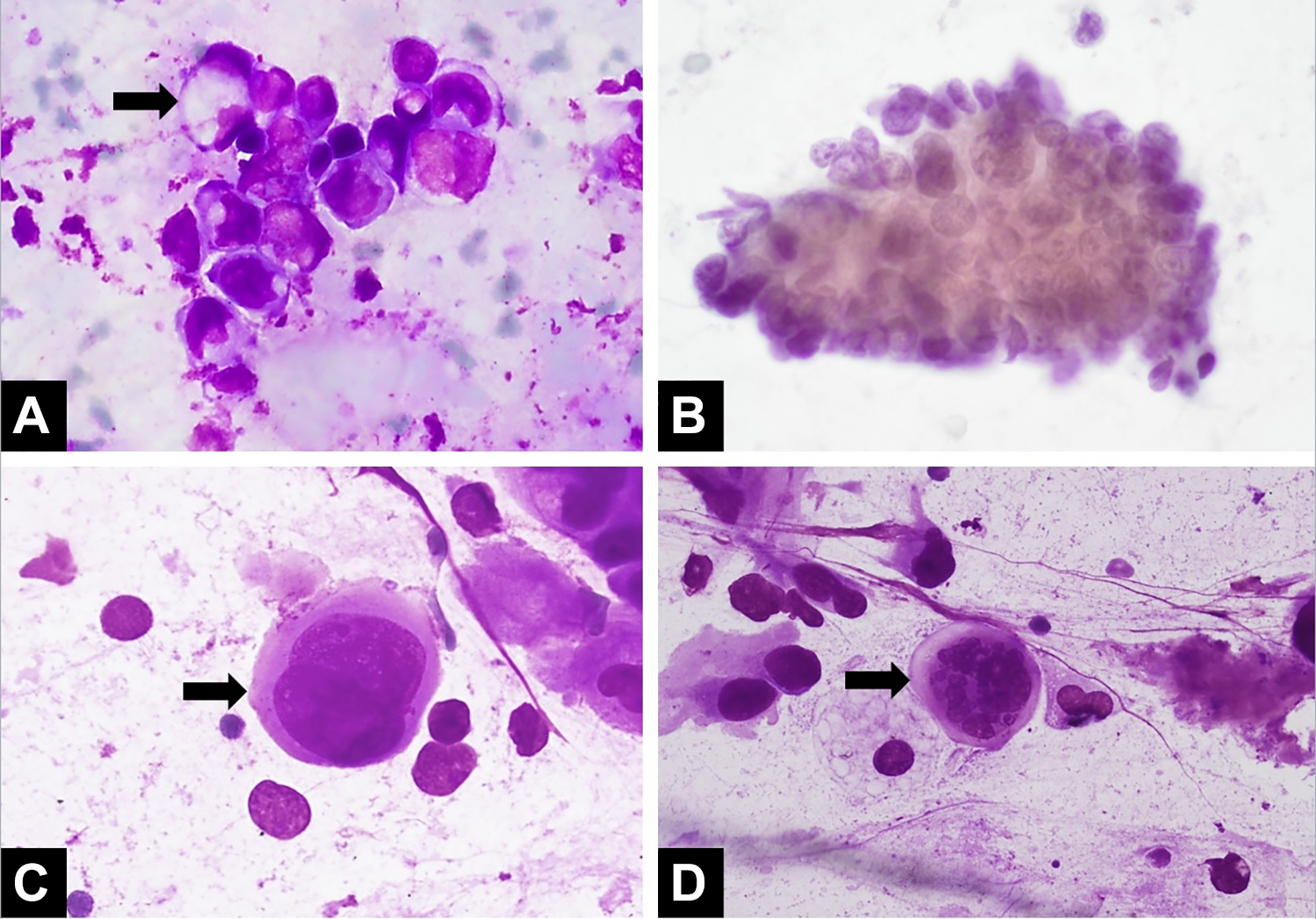
Cytopathology smears from a fine-needle aspiration biopsy of a pancreatic mass. A, Cluster of malignant cells with high N/C ratio, pleomorphism, and hyperchromatism. Cytoplasmic mucin vacuoles noted in some of the cells (arrow; Romanowsky stain, 400×). B, Small sheet of malignant cells with nuclear overlapping and loss of honeycomb appearance (Papanicolaou stain, 400×). C, A single malignant cell with a very high N/C ratio (arrow; Romanowsky stain, 400×). D, A single malignant cell with atypical mitosis (arrow) and a background of granular debris consistent with necrosis (Romanowsky stain, 400×).
Questions/Discussion Points, Part 3
What Is the Most Likely Diagnosis? What Is the Next Best Step?
These features are consistent with invasive pancreatic adenocarcinoma, and the next best step is based on the current stage of the patient’s disease.
How Is Pancreatic Adenocarcinoma Treated?
The treatment of pancreatic adenocarcinoma is dependent on the stage of the disease at the time of diagnosis and the patient’s eligibility for surgical resection. Those with resectable disease should proceed to surgery immediately and receive adjuvant chemotherapy. Sometimes chemotherapy and radiation can be administered prior to surgery in thought that it treats undetectable systemic disease and reduces the risk of local recurrence, although this has not been proven. While the type of resection varies based on the location of the tumor, the most common surgical procedure for those with adenocarcinoma of the head of the pancreas is a pancreaticoduodenectomy (Whipple procedure). This involves resection of the pancreatic head, duodenum, and gallbladder as well as a portion of the stomach. 10
At the time of surgery, the surgeon will first search for any evidence of metastatic disease, such as lesions in the peripancreatic nodes, liver, or peritoneum. If metastasis is not detected, surgery will procced, at which time the surgeon will become most interested in the status of the margins of the resection specimen, as negative margins will confirm complete resection of the tumor. Intraoperative consultations using a frozen section technique can be invaluable in helping guide the surgeons at the time of surgery. Using this technique, a pathologist can examine any suspicious tissue submitted during the procedure and the margin status of the resection specimen determined before the end of the surgery. 7
The treatment regimen for those with borderline resectable disease is not well established. Studies support the delivery of preoperative neoadjuvant chemotherapy or chemoradiation, followed by resection. Those with locally advanced and metastatic disease are considered unresectable and should be treated with chemotherapy or chemoradiation in addition to receiving palliative care. 10
The primary chemotherapeutic regimen for pancreatic adenocarcinoma is gemcitabine and fluorouracil (5-FU), where the use of these agents has been shown to increase median disease-free survival time. Those with more advanced disease can be treated with 5-FU, oxaliplatin, irinotecan, and leucovorin, although studies have shown increased toxicity compared to treatment with gemcitabine and 5-FU alone. 6,10
Diagnostic Findings, Part 4
The patient is determined to have resectable disease. He receives chemotherapy and undergoes a Whipple procedure, which confirms the complete resection of an invasive pancreatic adenocarcinoma with negative margins and no metastasis. The following features were seen on tissue section: Abortive glands Pleomorphic, hyperchromatic nuclei Prominent nuclei Abnormal mitotic figures Stromal desmoplastic reaction to invasive malignant glands with increased fibrosis and collagen deposition around invasive malignant glands (Figure 3C-D) Lymphovascular invasion (Figure 3E) Perineural invasion (Figure 3F)
Although it was not seen on this patient’s resection, it should be noted that there may be necrosis or PanIN (Figure 3B) present within resected pancreatic adenocarcinoma specimens. 7
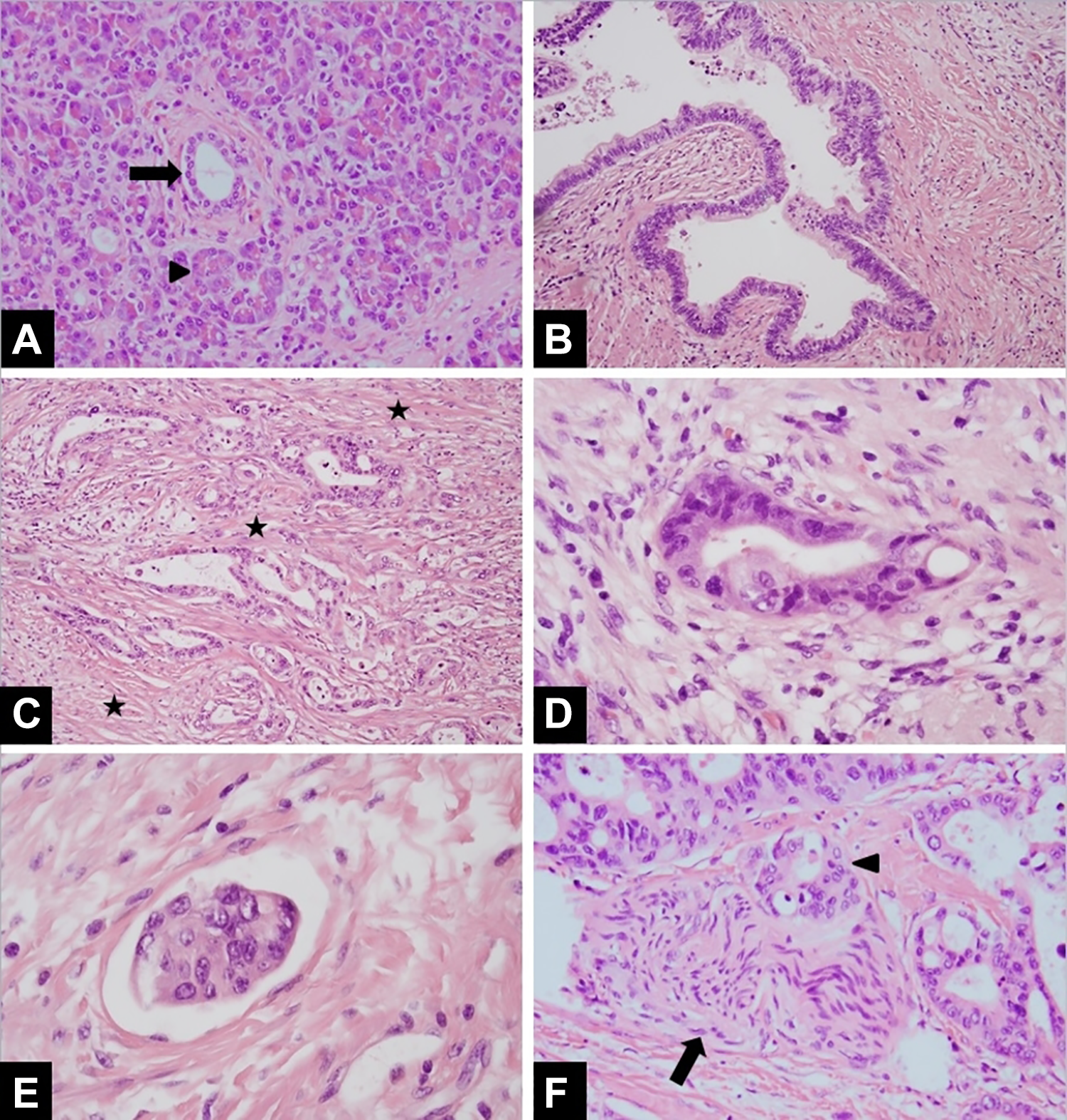
Photomicrographs from a pancreatic mass resection specimen. A, Normal pancreas, benign cuboidal ductal epithelium (arrow) with acinar cells (arrow head; H&E 100×), (B) PanIN, dysplastic columnar pseudostratified ductal epithelium (H&E 100×), (C) invasive ductal adenocarcinoma, infiltrating malignant glands and marked stromal desmoplastic reaction (stars; H&E 100×), (D) a single malignant gland (high power view) with pleomorphic, hyperchromatic nuclei and prominent nucleoli (H&E 400×), (E) lymphovascular invasion, a single malignant gland within a lymphatic channel (H&E 400×), (F) perineural invasion, a malignant gland (arrow head) encasing and invading the sheath of a nerve (arrow; H&E 400×). PanIN indicates pancreatic intraepithelial neoplasia. H&E indicates Hematoxylin and eosin.
Questions/Discussion Points, Part 4
How Is Pancreatic Adenocarcinoma Staged?
Pancreatic adenocarcinoma is often diagnosed late in the disease course, as it is generally asymptomatic until it is large enough to be symptomatic. There are no effective screening methods for early detection of lesions, so 5-year survival has remained low, at approximately 10%. 10,11
Pancreatic adenocarcinoma is staged using the TNM system. T, which stands for tumor, is based on the size of the lesion as well as its involvement of the celiac axis, superior mesenteric artery, and common hepatic artery. The larger the number, from 0 to 4, the larger, or more involved, the neoplasm. N, which stands for lymph nodes, is graded from X to 2, where the higher the number, the more nodes involved. Finally, M, which stands for metastasis, is from 0 to 1, where 1 is metastasis and 0 is none. These grades are used to group the tumor into its final stage, from 0 to 4. The higher the stage, the worse the prognosis. 10
Pancreatic adenocarcinoma can also be classified based on its resectability, which aids in guiding clinical management of the disease. The tumor can be described as resectable, borderline resectable, locally advanced, or metastatic. Resectable neoplasms do not involve the local vasculature, such as the portal vein or hepatic artery. This differentiates them from borderline resectable neoplasms, which involve or occlude the superior mesenteric vein-portal vein confluence and are amenable to reconstruction, abut the superior mesenteric artery for less than 180° of the circumference, or have short segment encasement of the hepatic artery. Locally advanced disease has greater involvement of the associated vasculature with absent extrapancreatic disease, and metastatic disease has evidence of spread to distant organs or the peritoneum. 10
Teaching Points
Jaundice can be of prehepatic, hepatic, or posthepatic origin. Serum studies and imaging, in addition to a complete history and physical exam, should be used to delineate the exact cause of an elevated bilirubin level.
Pancreatic adenocarcinoma often presents with jaundice, back pain, unexplained weight loss, pruritus, diabetes mellitus, migratory thrombophlebitis, and acute pancreatitis. As chronic pancreatitis and autoimmune pancreatitis can mimic these symptoms, it is important to rule out benign causes before proceeding with treatment.
The major risk factors of pancreatic adenocarcinoma are tobacco smoking, obesity, alcohol abuse, diabetes mellitus, and chronic pancreatitis.
Endoscopic ultrasound is useful in diagnosing pancreatic adenocarcinoma since it has higher sensitivity for small tumors and can be used in image guided biopsy.
Invasive adenocarcinoma of the pancreas arises from precancerous lesions termed pancreatic intraepithelial neoplasia or PanIN.
Accumulated molecular changes in the pancreatic ductal epithelium’s oncogenes and tumor suppressor genes will eventually lead to the development of invasive adenocarcinoma.
Pancreatic adenocarcinoma treatment depends on the stage at the time of diagnosis. Most are treated with resection, chemotherapy, radiation, or a combination thereof.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
