Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective EM2.2: Thermal Injury. Discuss thermal injuries, comparing and contrasting the direct and systemic effects of thermal burns, hyperthermia, hypothermia and their mechanisms of injury at the cellular level.
Competency 1: Disease Mechanism and Processes; Topic: Environmental Mechanisms (EM); Learning Goal 2: Physical Injury
Secondary Objective
Objective RRR1.6: Wound Healing. Describe the phases of cutaneous wound healing, the mechanism of healing by first intention (primary union) and second intention (secondary union) and possible clinical consequences of abnormal wound healing.
Competency 1: Disease Mechanism and Processes; Topic: Tissue Renewal, Regeneration, and Repair (RRR); Learning Goal 1: Mechanism of Tissue Regeneration, Renewal and Repair
Patient Presentation
A 74-year-old arrives in the emergency department by ambulance with a large area of burn injury covering a portion of the right abdomen, right arm, and right hand. The patient is unable to respond to questions regarding his condition, though he groans in response to some questions. The patient was involved in a motor vehicle collision in which the fire department was called to the scene. Emergency personnel who transported the patient to the hospital state that his clothes were “blackened.” The patient was not able to answer questions at the scene. He was given intravenous (IV) lactated Ringer’s solution in the ambulance along with IV morphine for pain.
Diagnostic Findings, Part 1
The patient is conscious and oriented to person, but not place or time. Vital signs are as follows: temperature 37.3 °C (99.1 °F), heart rate 108 beats/min, blood pressure 135/74 mmHg, respiration rate 18 breaths/minute. Physical examination reveals burned clothing that has been removed from his body. Over small areas of the right abdomen, right arm, and right hand, there is erythema with pain elicited on palpation. These areas of erythema mostly surround areas where the skin is darkened brown/black and there is no pain to palpation. There is skin sloughing from the wounds in some areas of the right abdomen and an eschar on the hand. This is shown in Figure 1. There is fluid collection in and around many areas of the burn injury. There is no active bleeding. There are no signs of inhalational injury, including no mucosal signs of smoke inhalation on oral exam. The patient is tachycardic, but rhythm is regular with no murmurs. Lungs are clear to auscultation bilaterally and there is no apparent increased work of breathing.
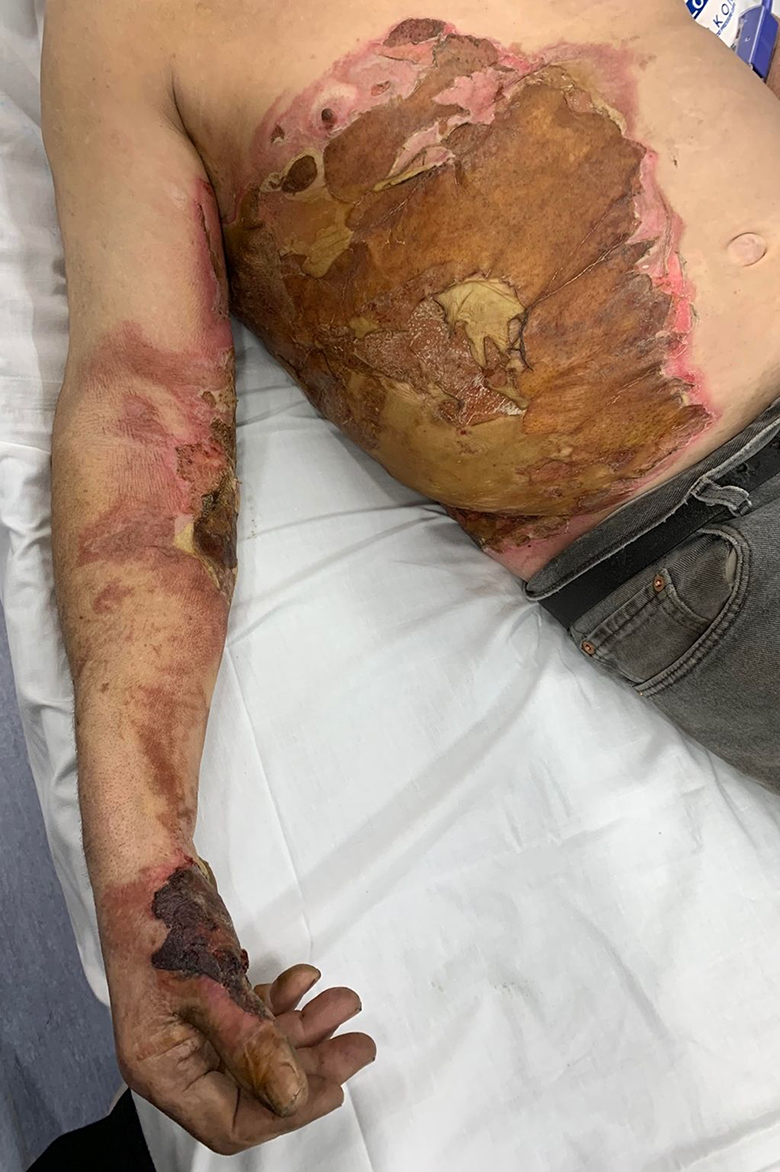
A 74-year-old man with severe burn injury. Note the skin sloughing on the abdomen and the necrotic eschar on the hand.
Questions/Discussion Points, Part 1
What Is the Differential Diagnosis Based on the History and Physical Examination?
Highest on the differential diagnosis list for this patient is severe burn injury, likely thermal given the history provided. Burns are injuries to the skin or other tissues caused by thermal or other acute trauma, such as electricity, chemicals, friction, or radiation. Common sources of thermal burns are hot solids/liquids and flames. Scald injuries account for about 70% of thermal burns in children and are also common in the elderly. 2,3 The most common cause of scald injuries is contact with hot liquids. Flame burns occur during contact with an open flame and are more common in the adult population. In contrast to scalds, flame burns tend to cause deeper burn injuries. Contact burns are most commonly seen in patients with epilepsy, patients who are intoxicated, or during industrial accidents. They result from extensive contact with hot solids and tend to cause severe injuries. 3 The differential diagnosis for this patient includes chemical injury, smoke inhalation injury, necrotizing fasciitis, contact dermatitis, and other vesiculobullous rashes. However, these are highly unlikely given the history of present illness.
List and Describe the Most Common Subtypes of Thermal Burn Injuries
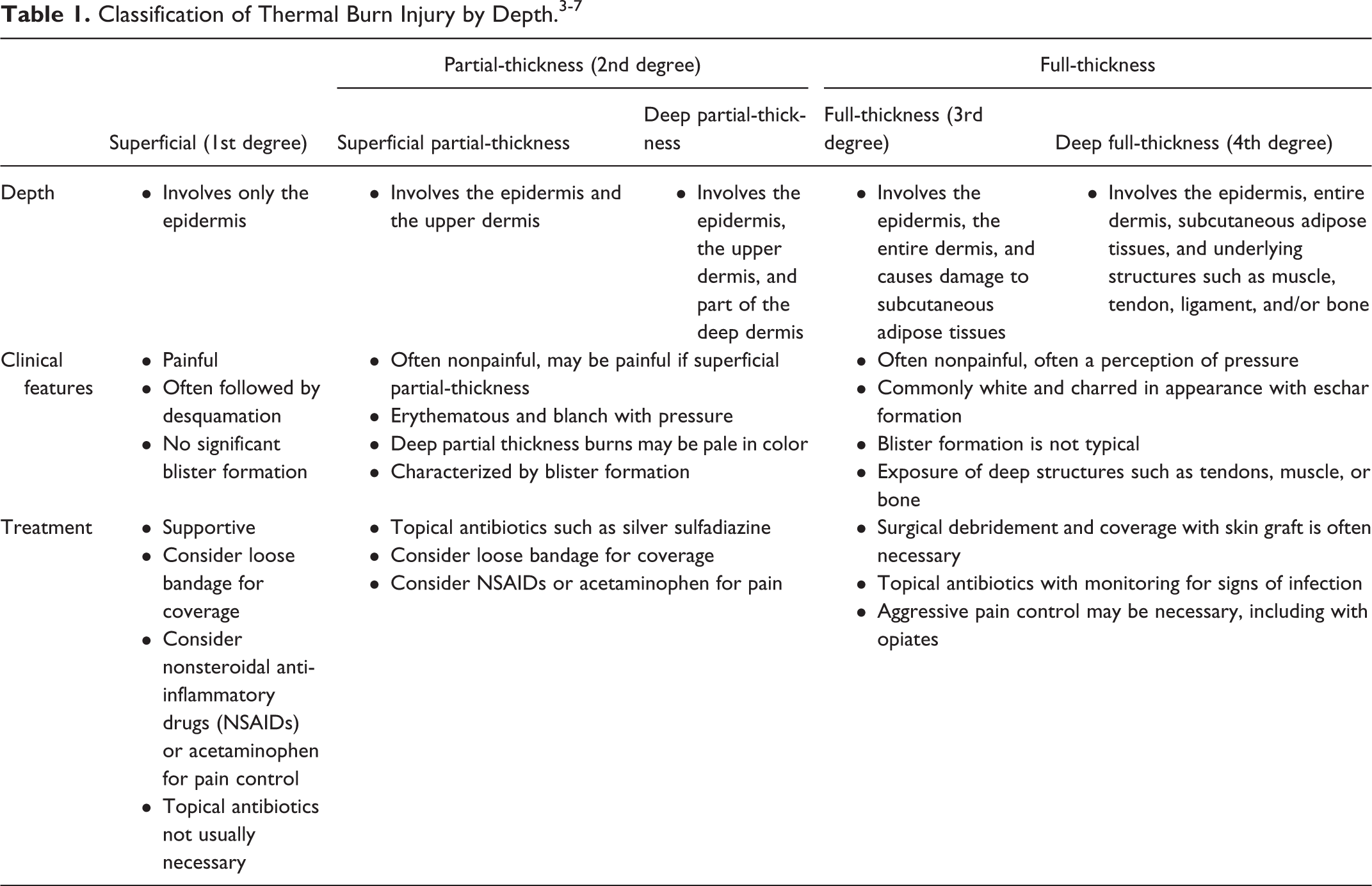
The current classification of cutaneous burn injuries is based on the depth of the injury, as shown in Table 1. Burn wounds are often heterogenous in depth and dynamic injuries, making it difficult to classify the injury into just one category. However, it is important to understand and consider burn depth classification when assessing burn injuries, since burn depth is an important prognostic factor and influences treatment. According to the American Burn Association, there are 5 burn categories based on burn depth: superficial (first-degree), superficial partial-thickness (second-degree), deep partial-thickness (second-degree), full-thickness (third-degree), and deep full-thickness (fourth-degree). 4 While each level of burn has unique characteristics and physical exam findings, it is still a challenge to health care providers to classify burns within these categories. Though clinical assessment is the most common method used to determine the depth of burn injury, it is only accurate in 60% to 75% of cases, even when carried out by experienced burn surgeons. 5,6
Superficial or epidermal burns (first-degree) only involve the epidermis. A common example of this type of burn is seen in mild to moderate sunburn. Superficial burns do not blister but are painful, erythematous and blanch with pressure. They typically resolve over 2 to 3 days and can be followed by peeling, in which the damaged epithelium is replaced by the healed underlying epidermis. These burn injuries typically resolve on their own without scarring or functional impairment. 4
Partial-thickness (second-degree) burns involve both the epidermal and dermal layers of the skin and can be further divided into superficial partial-thickness or deep partial-thickness burns. Superficial partial-thickness burns involve the upper layers of the dermis and are painful, erythematous and blanch with pressure. In contrast to superficial burns, superficial partial-thickness burns characteristically form blisters between the epidermis and dermis within 24 hours of injury. Most superficial partial-thickness burns heal spontaneously within 3 weeks and, similar to superficial burns, scarring and functional impairment are not typically seen. 4,7 Deep partial-thickness burns extend into the deeper layers of the dermis. These injuries are clinically distinguishable from superficial partial-thickness burns but can be difficult to distinguish from full-thickness (third-degree) burns upon evaluation. Deep-partial thickness burns are painful to pressure only, blister, do not typically blanch, and can appear from white to red. 7 Spontaneous healing in a patient without any complications can be expected in 3 to 9 weeks. However, as deep partial-thickness burns heal significant scar formation may occur, with a potential for cause pathologic scarring (hypertrophic or keloid). 7
Full-thickness (third-degree) burns extend through the epidermis, all layers of the dermis and cause damage to deeper subcutaneous structures. The subcutaneous layer of the skin, also known as the hypodermis, is composed primarily of connective tissues like adipose but also contains larger blood vessels and nerves. These burns can have a varied appearance from waxy white to charred and black. Clinically, patients with full-thickness burns have injuries that are typically nonpainful due to nerve damage in the hypodermis, nonblanching, and without blister formation. 7 An important feature of full-thickness burns is eschar formation, which is a combination of necrotic dermis and inflammatory secretions around the wound. The eschar is temporary and eventually separates from the underlying tissue to leave an open wound. Deep full-thickness burns (fourth-degree) involve all layers of the skin as well as deep underlying structures such as muscle, bone, tendons, and ligaments. They have similar characteristics to full-thickness burns.
Describe the Pathophysiology and Mechanism of Thermal Burn Injuries, Including Molecular Events
The body responds to burn injuries much like other types of insult, with the initial release of inflammatory mediators called cytokines that trigger both local and systemic inflammatory reactions. Key cytokines in acute inflammation are tumor necrosis factor alpha (TNF-α), interleukin-1 (IL-1), and IL-6. 8 This cascade is initiated by the activation of nuclear factor kappa beta (NF-κB), a transcription factor, and results in the recruitment and activation of neutrophils, macrophages, and other immune mediators at the site of injury. Additionally, mast cells can be directly activated by tissue trauma and release histamine, which promotes vasodilation and increases local vascular permeability. Prostaglandins (PGD2, PGE2, PGI2) are enzymatically generated from arachidonic acid by cyclooxygenase and are also potent vasodilators that increase vessel permeability. Vasodilation promotes an increase in the rate of oxygen delivery to the damaged tissue, and increased vascular permeability permits transmigration of various components of the acute inflammatory response to the site of injury. Increased vascular permeability also allows for extravasation of exudative fluid into the damaged tissue, resulting in edema that is characteristic of burn injuries. 8 -10
Jackson’s model can be used to help understand the pathophysiology of a burn injury by organizing the wound into 3 concentric zones. It is important to understand that these zones are 3-dimensional, extending both on the surface of the injury as well as deeper into the skin. 3 The zone of coagulation is the area closest to the source of the injury. The high heat exposure in this zone causes the coagulation of proteins and limits blood flow, resulting in ischemic damage. As such, this area skin and underlying tissues undergoes coagulative necrosis and irreversible tissue loss. 3,8 Beyond the zone of coagulation is the zone of stasis. This zone is characterized by reversible cellular injury secondary to decreased blood flow. Restoring adequate perfusion to this zone is crucial in the management of burn injuries to decrease tissue loss and prevent the wound from enlarging. 3,8 The outermost area of the burn forms the zone of hyperemia which is characterized by increased perfusion secondary to various inflammatory mediators, including prostaglandins. 3
Diagnostic Findings, Part 2
Figure 2 and Figure 3 show an example of a skin biopsy from a burn. Histologic findings demonstrate an acute inflammatory reaction including dermal congestion and inflammatory infiltrate at low and high power, respectively. Neutrophilic infiltrate (seen primarily in the first few days post-burn injury) as well as a predominant lymphocytic infiltrate (seen primarily after 4 to 5 days post-burn injury) are seen. Epidermal separation from the dermis, consistent with blister formation, is also seen. Note that biopsy is not typically performed in burn treatment, but a sample is provided here for educational purposes.
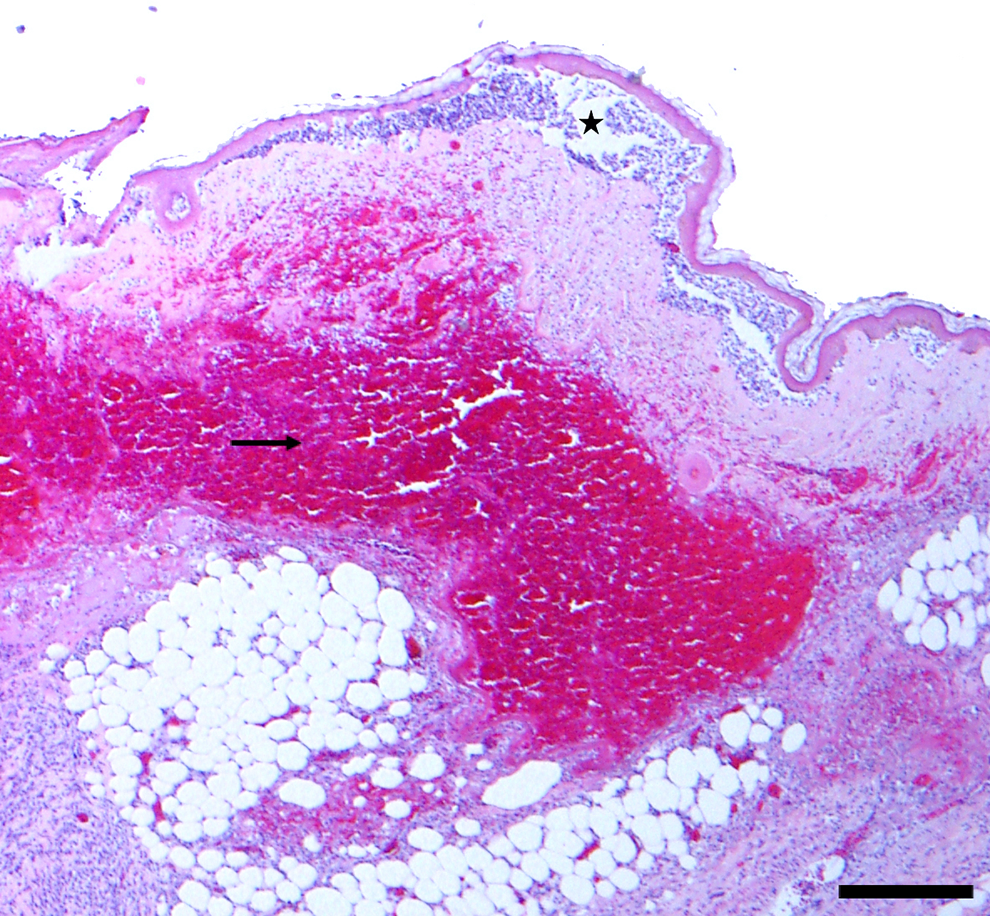
Low magnification (×40) image immediately after a burn showing separation of the epidermis from the dermis consistent with blister formation (star) and hemorrhage (arrow) in the dermis. Hematoxylin and eosin stain. Scale bar = 250 micrometer.
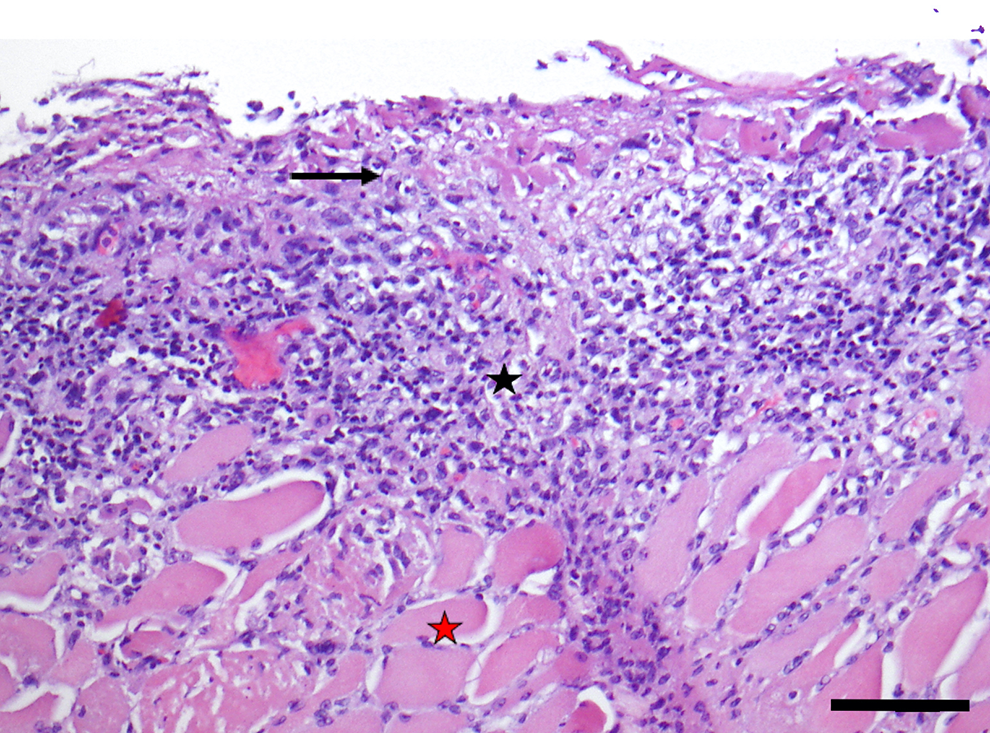
High-magnification image (×200) showing denudation and sloughing of the epidermis after burn injury (arrow). Inflammation in the dermis including neutrophils and lymphocytic infiltrate, heralding the attempts at repair, is also shown (black star). Neutrophils are seen near the sloughing epidermal surface, while the dermal infiltrate is lymphocyte-predominant. Note the underlying skeletal muscle below the dermis (red star) with minimal hypodermis, consistent with an area of the body with minimal subcutaneous adipose tissue. Hematoxylin and eosin stain. Scale bar = 100 micrometers.
Questions/Discussion Points, Part 2
What Is the Pathophysiology of Burn Healing and How Does It Relate to General Wound Healing?
Burn healing is similar to cutaneous wound healing after other types of injuries: first inflammation, then proliferation and remodeling. 11 One key characteristic of cutaneous injuries, including burn injuries, is that the skin is a labile tissue with stem cells in the basal layer of the epidermis. This allows the skin to regenerate in response to damage or cell death as long as the basal layer remains intact. However, deep injuries that destroy the regenerative stem cell layer must heal through scar formation. These healing processes are mediated by the expression of various growth factors that, upon binding to their receptors, initiate intracellular signaling cascades. 9 Important growth factors in the healing cascade include transforming growth factor alpha (TGF-α), transforming growth factor beta (TGF-β), platelet-derived growth factor (PDGF), fibroblast growth factor (FGF), and vascular endothelial growth factor (VEGF). These molecules trigger complex cellular responses via changes in gene expression, but there are some key associations to remember. Vascular endothelial growth factor and FGF are mediators of angiogenesis. Transforming growth factor alpha is an important mediator of epithelial development, including keratinocyte and fibroblast proliferation and function. Transforming growth factor beta is an FGF and, importantly, inhibits the inflammatory response. 9,10
For superficial and superficial partial-thickness burns, healing occurs most often by primary intention, in which the edges of the wound come together. In response to local cytokine effects and signals from the surrounding cellular environment, the stem cells from the basal layer of the epidermis divide and produce keratinocytes that migrate to the surface of the wound. This is typically initiated within hours of the injury, and the surface is usually covered within days to weeks depending on injury severity. Next, the basement membrane forms between the epidermis and the dermis, and deep connective tissues are reformed. 11 As mentioned previously, these burns injuries do not typically form significant scars.
Deep partial-thickness and full thickness burns typically heal by secondary intention and scar formation, which can take months to years. 11 Wound healing by secondary intention occurs when the edges of the wound do not approximate, so the wound must heal from filling of the deficit. Fibroblasts direct granulation tissue formation, which consists of the fibroblasts themselves, myofibroblasts, and capillaries at the site of injury. Initial production of type III collagen by fibroblasts serves as a placeholder and is slowly broken down by collagenases and replaced with stronger type I collagen as the healing process progresses. Myofibroblasts mediate the contraction and closure of the wound via a dynamic process involving actin microfilaments and attachment to components of the extracellular matrix. Although the area of scar tissue will never regain full strength, after about 3 months, the strength of the skin in the area of damage can approach 80%. 12
Describe the Lesions That Occur Due to Excessive Wound Remodeling
Errors in the remodeling phase of wound healing can result in functional and cosmetic defects. Hypertrophic scarring and keloid formation can occur in response to overproduction of connective tissue by fibroblasts during wound healing. The main differences between hypertrophic scarring and keloids include the extent of the excessive scar formation and the orientation of collagen fibers in the scar. If the scar extends beyond the boundaries of the initial wound it is referred to as a keloid. 13 Keloids also tend to have an increased ratio of type I to type III collagen relative to hypertrophic scars (leading to excessively thick and abnormal collagen bands on histology) and are more common in patients with African ancestry. Another wound remodeling complication, excessive scar contracture, is caused by overactivity of myofibroblasts. This can lead to excessive wound contracture in which the closure of the wound leads to cosmetic and functional limitations. This is particularly true if the injury is near or involves soft tissue around a joint, whereby excessive scar contracture can limit mobility via joint contracture.
What Are the Techniques to Estimate the Extent of Thermal Burn Injuries?
As previously discussed, burn depth is an important prognostic feature. In addition to depth, the total body surface area (TBSA) involved and location of the burn injury are critical for patient outcome and management. Injuries to the face, hands, feet, genitals, or respiratory tract are often referred to specialized burn centers to receive higher levels of care. 14 There are various methods commonly used to calculate the TBSA involved in a burn injury. It is important to note that superficial burns are not included in percentage TBSA burn assessment. 7
The Rule of Nines method breaks the body into 11 large portions that are equivalent to 9% TBSA each. The head, arms (×2), thighs (×2), lower legs (×2), chest, abdomen, lower back, and upper back all account for 9% of body surface area each. The genital area accounts for 1% of body surface area. In young children, the head accounts for more TBSA than in adults. The least reliable method commonly used to calculate TBSA involved is the Palm Rule, in which the size of the palm can be estimated as 1% of TBSA. 7
What Are the Medical Management Strategies for Thermal Burns?
The medical/surgical management of burn patients is a complex topic. Here, we provide an introduction to burn treatment for medical students.
All burn victims should be treated initially as trauma patients. The burn should not be the focus of attention on initial assessment, especially in severe burn patients, as airway and cardiopulmonary stabilization and assessment for other traumatic injuries should take precedent. Burns often co-occur with blunt or penetrating trauma, such as explosions or car accidents and Focused Assessment with Sonography for Trauma exam is often performed in these cases. Intubation is indicated in burn victims with signs of inhalational injury, such as soot in or around the mouth or mucosal involvement on oral exam. There should be a high suspicion inhalational injury in patients who have been trapped in a burning building or anywhere that a high level of smoke exposure is likely. Cyanide and carbon monoxide poisoning are also possible in burn victims and should be considered in patients with signs of respiratory distress especially in a setting of lactic acidosis. A detailed history is also important, including SAMPLE: signs and symptoms, allergies, medications, past medical history, last oral intake, and events that lead to the burn. 15 The causal agent of a burn is particularly important, as it may direct treatment decisions.
Finally, the burn wound or wounds should be assessed. The most relevant factors to consider are burn depth and the area of the body that is affected. As discussed previously, burn depth is defined as superficial, superficial partial, deep partial, full thickness, or deep burn. When considering the area of the body affected, both the burn location as well as the percentage of TBSA involved are important to document.
Minor thermal burns are defined by the following features according to the American Burns Association (American Burns Association) 14 :
Superficial or partial thickness
○ Less than 10% TBSA age 10 to 50
○ Less than 5% TBSA in a patient younger than 10 or older than 50
Full thickness
○ Less than 2% TBSA in any age
Also meets the following criteria:
○ Does not involve the genital region, the face, or the surface of the hands/feet
○ Does not involve major joints
○ Does not involve inhalation chemical injury or high-voltage electrical injury
Minor burn management is less complicated than management of severe burns and can typically take place in the outpatient setting. The mainstays of initial treatment include cooling the wound, cleaning the wound, and pain control. Cooling of the wound should begin immediately at the time of injury and should be done with room temperature or slightly cool water. Importantly, ice should be avoided, as ice has the potential to increase burn depth. Burns should be cleaned gently daily with soap and water, as other agents or more vigorous washing risk impairing wound healing. Pain control is usually achieved with acetaminophen, nonsteroidal anti-inflammatory drugs, or a combination of the two.
Topical antibiotics and wound dressings are commonly applied for partial thickness and full thickness minor burns but are generally not necessary for superficial burns. Common topical antibiotics that are used, if indicated, are silver sulfadiazine, mafenide acetate, and triple antibiotic ointment (bacitracin/neomycin/polymyxin). Silver sulfadiazine is commonly used but is avoided on the face, as it can lead to eye irritation. Mafenide acetate is used in cases where eschar penetration and improved Pseudomonas coverage are desired, but it can lead to a lactic acidosis and can cause significant pain on application. Triple antibiotic ointments are often used for burns of the face, as they are less irritating. If a patient has not had TDaP vaccination within 5 years, they should receive vaccination, as even minor burns are susceptible to Clostridium tetani infection. 16
In general, moderate and severe burns are deeper and cover a larger area of the body relative to minor burns. They often require inpatient management in a burn center. This section focuses on treatment of severe thermal burns, which account for 86% of admissions to burn centers in the United States and include fire/flame, scalding, and hot surface injuries. 17 Severe thermal burns are specifically defined as partial or full thickness burns that involve more than 20% of TBSA in adults. In children and geriatric patients, smaller surface areas may be considered severe. 18 The treatment of severe burns is complicated, multidisciplinary, and expensive. Treatment of a single patient with a severe burn can cost between 1.6 and 10 million dollars in the United States, depending on degree of complications and length of hospital stay. 17
After initial stabilization and assessment for concomitant trauma, the medical management of severe thermal burns begins quickly. As with minor burns, cleaning/cooling the affected areas and controlling pain are important. However, pain control in severe burns often requires IV opioids, and benzodiazepines are often used acutely to keep the victim calm if they are conscious. 19 In addition, the treatment of severe burns involves many additional considerations, including warming the treatment room and resuscitating the patient with IV fluids. Patients with severe burns are at high risk for hypothermia, as the skin is a major thermoregulator for the body. 16 Fluid replacement is also critical for patients for severe burns. In a severe burn, capillary damage leads to extravasation of fluid into the affected tissue and thus significant intravascular fluid loss. 20 Early and aggressive fluid replacement (often with lactated Ringer’s solution) maintains end-organ perfusion and reduces risk of mortality due to multisystem organ failure. 19
Metabolic and nutritional considerations are also important in patients with severe burns. Hypermetabolism, often up to a 100% to 150% increase in the metabolic rate, is common in patients with severe burns as the body fights to maintain body temperature and heal the skin quickly. The increase in metabolic rate is generally proportional to the TBSA affected by the burn injury. Nitrogen loss is an important consideration in patients with severe burns. The hypermetabolic state seen in burn patients is partly due to muscle catabolism, which provides amino acids to rebuild skin tissue. As such, aggressive protein replacement with adequate nutrition is a crucial aspect of treatment in severe burn patients. 17 Enteral (gastrointestinal [GI]) feeding, often with nasoenteral tube, is preferred to parenteral (IV) feeding, as enteral feeding reduces the risk of mortality in burn patients. Enteral feeding both protects the GI tract to reduce the risk of GI-related sepsis and avoids the risk of sepsis associated with venous-catheters in parenteral feeding. 21 Phosphorus replacement may also be necessary, as the body spends copious amounts of ATP to repair itself.
What Are the Surgical Management Options for Burns?
Surgical management of burns is most common in moderate and severe burns, especially in full thickness and deep burn injuries. 21 Plastic or general surgeons with fellowship training in burn care are the most common surgeons involved in burn wound management, often in burn centers. Removal of burn tissue and wound closure are fundamental in the surgical management of burns, as these procedures reduce the risk of infection and decrease mortality. 17,22 Necrotic tissue provides nutrient-rich medium for bacterial growth and is generally removed as soon as possible after burn injury. Thus, in general, burns with signs of eschar are excised and covered early during a burn victim’s hospital course. There are a variety of options for burn wound coverage, including various types of skin grafts. 17 Possible options include autografts, allografts, xenografts, lab-based materials, and combinations of these approaches. 21
Autographs are grafts taken from healthy areas of the burn patient’s own skin. Autografts are generally the preferred method of wound closure, when feasible, but may be limited by the amount of harvestable healthy skin in patients with large TBSA burns. 17 When available healthy skin is a limiting factor, meshing techniques are used to increase the area of coverage that is possible with a graft. 23,24 Allografts are of human origin but are so-named because they are not derived from the skin of the burn victim. The root “allo-”derives from the Greek work for “other.” As with all transplants, allografts have the risk of rejection, but may be necessary in large TBSA burns as there may not be enough healthy skin on the burn victim to provide full wound coverage with autograft. 17 Xenografts are derived from other animals such as pigs. Allografts and xenografts often serve the purpose of temporary wound coverage, or as an adjunct to autograft. For example, cadaveric skin (allograft) and porcine skin (xenograft) are commonly loosely grafted over partial burns until the underlying skin can heal and be harvested as an autograft. This is common in patients with large TBSA burns that have burns of varying severity across their body surface.
Skin grafts are also classified as full-thickness or split-thickness, referring to the thickness of the donor tissue. These terms are most commonly used in association with autografts. Full-thickness grafts involve both the epidermis and the dermis, and thus have the advantage of containing all layers of the skin, which may improve cosmetic and functional outcomes. However, as the donor site no longer retains the dermis, it must be closed with sutures to allow for healing. In addition, the thickness of the graft makes full vascularization more challenging, increasing the risk of graft failure in poorly perfused areas. Split-thickness grafts are most commonly used and may be used in conjunction with lab-based dermal replacements such as Alloderm. 17,18,23,24
What Are the Specific Risks and Complications in a Burn Patient?
The most important complications of severe burns are hypothermia, fluid imbalances, nutritional deficiency associated with hypermetabolism, compartment syndrome, and infection. Hypothermia, fluid imbalances, and nutritional issues are discussed previously.
Infection is an important complication of burn injuries and may occur in any burn minor to severe. However, risk for severe infection, including sepsis, is highest in severe burns. As mentioned previously, prompt wound debridement and coverage are essential in the care of severe burns to reduce the risk of infection. Topical antibiotic therapies alone with wound debridement are not sufficient for infection prophylaxis. 25 If a burn-related infection is suspected, wound cultures are obtained immediately. The two most likely pathogens are Pseudomonas aeruginosa (often later in the hospital course) and Staphylococcus aureus (often earlier in the hospital course), though other organisms are possible. 25 Burn treatment depends on whether there are signs of invasion. Noninvasive infections are treated with wound debridement, if not already completed, and topical antibiotics as discussed previously. If signs of systemic infection or sepsis are observed, such as fever or hypotension, empiric IV treatment with anti-Pseudomonal antibiotics and anti-Staphylococcal antibiotics is recommended pending final cultures and sensitivities. One possible regimen is piperacillin/tazobactam in combination with vancomycin. 17,25,26
One possible complication seen in severe burns with eschar formation is compartment syndrome. If the burn eschar is circumferentially around a body appendage, the neck, or the chest it has potential to lead to compartment syndrome. 4,7 Following eschar formation, the skin loses its normal elastic properties in the area of damage and underlying structures such as blood vessels become compressed as the pressure within the tissues increases. Combined with the increased tissue edema as a result of acute inflammation, high interstitial pressures develop at the site of injury. In the extremities, this increased pressure can compress arteries and veins and can lead to ischemic damage or necrosis. 4 In the neck, the airway may be compromised in addition to blood supply to the brain. In the chest, circumferential eschar may impair chest wall movement and cause respiratory distress. In all cases, urgent escharotomy, which can often be done at the bedside, is required.
Additional complications of severe burns are also possible, including but not limited to: sensory loss secondary to nervous tissue damage, heterotopic ossification of healing tissue, and keloid or hypertrophic scar formation. 18 Psychological consequences, including depression and posttraumatic stress disorder (PTSD), are also common and are detailed below in a subsequent section.
What Are the Basic Principles of Electrical and Chemical Burn Injury Including Treatment and Potential Complications?
Electrical injuries are the second-most common burn subtype to lead to admission to a burn center in the United States. 17 Electrical burns can be either low voltage, such as contact with a home electrical outlet, or high voltage, which is most common in the workplace. Lightning injury is a rare but extremely high voltage electrical injury that presents with a classic “fernlike” pattern on the skin called Lichtenberg figures. In general, electrical burns are treated similarly to thermal burns in terms of cutaneous wound management. Low-voltage burns are often treated outpatient. However, high-voltage electrical burns require assessment for internal organ dysfunction, often in a burn or trauma center. 27 Renal dysfunction secondary to rhabdomyolysis is the most concerning complication of high-voltage electrical injury, which may be associated with hyperkalemia. Cardiac arrythmia secondary to a high-voltage injury is also possible and could be immediately fatal. Nervous system dysfunction is another possible complication and could manifest as a seizure disorder later in life. 28
Chemical injuries are the third-most common burn subtype to lead to admission to a burn center in the United States. 17 Chemical burns can be caused by a variety of substances, including but not limited to caustic acids (lab chemicals such as hydrochloric acid, battery acid), caustic bases (bleach, drain cleaner), and even fertilizer. Irrigation of the burn with water is the preferred initial treatment and should occur as soon as possible. In general, only water should be used for irrigation, and neutralization of acids with bases or bases with acids is contraindicated due to risk for exothermic reaction and further tissue damage. An exception to the water rule is a burn from an elemental metal such as sodium, potassium, or magnesium, because water can interact with elemental metals and cause exothermic damage. Mineral oil or another hydrophobic compound is often used in these cases. 29 Wound care for chemical burns is otherwise similar to thermal burns.
What Are the Important Psychosocial Considerations and Racial Disparities in Burn Care?
Certain psychosocial considerations are also important in the evaluation and treatment of burn patients. For example, it is important to consider the possibility of child abuse manifesting as burn injury. Perfectly round burns may be indicative of burn with a cigarette. Scald burns with sharp edges, especially symmetrically on the buttocks without associated splash marks, may indicate intentional immersion injury in a hot bath. 30,31 A classic pattern to look out for is the “doughnut sign,” in which an area of unburned skin, the part in contact with the bathtub and thus protected from the water, is surrounded by a burn. 3 In addition, it is important to consider the possible psychological consequences of burn injuries for burn victims, including PTSD and depression associated with trauma and disfigurement. 32 Often, clinical psychologists and psychiatrists are part of the care team for severely burned patients.
Racial disparities in burn care are also important to consider. One study of more than 180,000 patients in the United States demonstrated increased mortality in Black male burn victims regardless of access to care. 33 In addition, rates of certain complications in burn healing are more common in persons of color. Patients with darker skin pigmentation, especially Black patients, are more likely to experience keloid formation during burn healing. 34
Teaching Points
Work-up of burn injuries should always be initiated with the general trauma survey followed by closer assessment of the injury of concern.
Classification of burns is based upon the depth of the injury and can be categorized into:
○ Superficial
○ Superficial partial thickness
○ Deep partial thickness
○ Full thickness
○ Deep full thickness
Initial burn injury is centered around the acute inflammatory response and the release of cytokines IL-1, TNF-α, IL-6, and prostaglandins. Jackson’s Model describes the pathophysiology of burns by understanding the burn as a 3-dimensional entity with 3 zones: the zone of coagulation, the zone of stasis, and the zone of hyperemia.
Wound healing is mediated by key cytokines TGF-β, PDGF, VEGF, and FGF and occurs similarly in burns as in other cutaneous injuries. Burns that are deep enough to disrupt the stem cell layer of the epidermis often result in scar formation.
Complications of wound healing include hypertrophic scarring and keloid formation. Compared to a hypertrophic scar, a keloid extends well beyond the borders of the original wound and contains abnormally thickened and misoriented collagen bundles. Joint contractures occur when soft tissue scar extends across joints leading to limitations of joint function.
Burn treatment depends on severity, which is determined by both the classification of a burn (depth of injury) as well as the total body surface area (TBSA) involved with burn. A common method to estimate TBSA in adults is the Rule of Nines.
Fluid replacement in burn management is crucial, as burn patients lose large amounts of fluid due to capillary injury and local inflammation. Fluid replacement is often with lactated Ringer’s solution.
Surgical management of burn injury is most common for severe burns and often involves wound debridement and autograft skin grafting as early as possible in the hospital course. One major limitation to autograft coverage of burn wounds is TBSA involved in the burn.
Complications of burn injuries are numerous and include the following high-yield topics: infection (Pseudomonas and Staphylococcus aureus are most common pathogens), hypermetabolic syndrome, and compartment syndrome secondary to circumferential eschar formation.
Less common subtypes of burn injury include high-voltage electrical injury and chemical burns, which have special considerations in management.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The article processing fee for this article was funded by an Open Access Award given by the Society of ‘67, which supports the mission of the Association of Pathology Chairs to produce the next generation of outstanding investigators and educational scholars in the field of pathology. This award helps to promote the publication of high-quality original scholarship in Academic Pathology by authors at an early stage of academic development.