Abstract
This article presents findings from a 4-year series of surveys of new-in-practice pathologists, and a survey of physician employers of new pathologists, assessing how pathology graduate medical education prepares its graduates for practice. Using the methodology described in our previous study, we develop evidence for the importance of residency training for various practice areas, comparing findings over different practice settings, sizes, and lengths of time in practice. The principal findings are (1) while new-in-practice pathologists and their employers report residency generally prepared them well for practice, some areas—billing and coding, laboratory management, molecular pathology, and pathology informatics—consistently were identified as being important in practice but inadequately prepared for in residency; (2) other areas—autopsy pathology, and subspecialized apheresis and blood donor center blood banking services—consistently were identified as relatively unimportant in practice and excessively prepared for in residency; (3) the notion of a single comprehensive model for categorical training in residency is challenged by the disparity between broad general practice in some settings and narrower subspecialty practice in others; and (4) the need for preparation in some areas evolves during practice, raising questions about the appropriate mode and circumstance for training in these areas. The implications of these findings range from rebalancing the emphasis among practice areas in residency, to reconsidering the structure of graduate medical education in pathology to meet present and evolving future practice needs.
Introduction
In December 2013, leaders of 24 general medical and pathology organizations convened a Pathology Workforce Summit (Supplemental Table 1) to address concerns about the future of the pathology workforce and concomitant concerns about the effectiveness of graduate medical education (GME) in pathology. 1 The Summit participants achieved consensus on the following significant points: (1) the supply of pathologists will substantively decrease; (2) the demand for pathology services will change (likely increase due to the changing US demographics, ie, aging population), (3) new technology and new health care delivery systems will change pathology practice, and (4) there was a prospective quantitative mismatch of graduating trainees coming into practice with pathologists leaving the workforce.
Subsequently, in 2014, representatives from 5 major pathology organizations American Board of Pathology [ABPath], American Society for Clinical Pathology [ASCP], Association of Pathology Chairs [APC], College of American Pathologists [CAP], and the United States and Canadian Association of Pathology [USCAP]) established an interorganizational Taskforce to glean best practices in GME. The Taskforce’s specific charge was to bring an evidence base to pathology GME, with a particular focus on how to most effectively and efficiently use the ∼3200 annually funded pathology GME positions (2400 residents and 800 fellows) to prepare pathology trainees for practice. With the number of pathologists who are now retiring each year exceeding the number entering practice, 2 -4 the Pathology Summit Taskforce called for a rigorous assessment of how well the specialty was using these funded positions to train pathologists.
The Taskforce developed a methodology that is generalizable to medical training in other specialties. We have described this previously. 5 This article presents the specific findings on pathology residency training derived from 4 years of data collection. Specifically, this analysis assesses the extent to which pathology residency currently provides what every pathologist needs to know to competently enter into practice. It also provides comparative assessments between different groups of new-in-practice pathologists, based on their practice setting, their years in practice, and the extent to which their practice is subspecialized versus general.
Current GME Content Specifications
Two primary agencies set the existing specifications for training in pathology. The Accreditation Council for Graduate Medical Education (ACGME) establishes the requirements for accreditation of pathology training programs, while the ABPath determines the criteria for certification of individual pathology practitioners. While each entity addresses both structure and content aspects of training, the ACGME is primarily structure and program focused, 6 whereas the ABPath is more content and trainee focused. 7 Taken together, the ACGME program requirements and ABPath examination blueprints implicitly constitute the current content area benchmarks for training in pathology, around which there is nevertheless some curricular variation. 8 Here we present findings and conclusions derived from a series of surveys, using our published methodology to evaluate how pathology graduate medical education (GME) prepares its graduates for practice. It also identifies specific areas, where enhanced pathology GME is needed.
Methods
We designed 2 distinctly different surveys, one for the new-in-practice pathologists and one for employers of new-in-practice pathologists. Both surveys assessed how well pathology GME aligns with the knowledge and skills required for actual practice. 5
The ABPath fielded the new-in-practice pathologist survey in conjunction with the biennial Continuing Certification (CC) reporting cycle it requires of recent diplomates (previously called “Maintenance of Certification”). The surveys (see Supplemental Table 2 for measurement parameters) have been fielded continuously since the 2014-2015 CC reporting cycle. Although the surveys are conducted annually, the results reported herein reflect only the initial 4-year period during which there was general uniformity of the questions over consecutive cycles. Based on the nearly identical findings from 2014-2015 through 2017-2018, survey planners subsequently chose to condense some practice areas and eliminate others to introduce new sets of questions.
The CAP fielded a new pathologist employer survey in 2015. Its function was to validate the new-in-practice pathologist survey rather than to serve as a freestanding assessment tool.
Alterations to Surveys During the Study Period
Several minor changes were introduced following the initial CC survey in 2014-2015. “Hematopathology” and “Hematology” used in 2014-2015 were subsequently clarified to “Hematopathology (lymph nodes, spleen, etc.)” and “Laboratory Hematology (bone marrows, peripheral blood),” respectively. Likewise, a new practice area, “Next Generation Sequencing” (NGS), was included. Then, in 2016-2017 and 2017-2018, the 8 previously lowest rated areas of reported practice importance (Apheresis, Blood Center Donor Services, Bone Marrow Procedure, Cardiovascular Pathology, Electrophoresis, Hematology, Tissue Typing/HLA, and Transplant Pathology) were eliminated. The space freed permitted the addition of 17 more specific “drill down” subsidiary areas within the 3 general areas (Laboratory Administration, Molecular Diagnostics, and Pathology Informatics) that consistently had been reported as highest in both practice importance and need for additional residency training.
Despite these changes, all four CC surveys returned remarkably consistent responses. To isolate the impact of residency training in any given practice area from fellowship training in that same area, our analysis for a given practice area excluded pathologists who received related fellowship training in that subspecialty area. The weighted average “Practice Importance” and “Training Needed” were then calculated for each subspecialty practice area. These calculated values were compared among the 4 CC surveys, first by data visualization and then statistically. Responses were summarized using descriptive statistics. The Pearson correlation coefficient, Student t test, and Fisher Exact test were used to compare results across survey administrations and among respondent groups. Statistical analyses were performed using IBM SPSS Statistics for Windows, version 25.0 (IBM Corp) and Microsoft
Results
CC Survey Response Rates and Demographics
The response rates varied by year but were high, with 34% to 54% of diplomates opening the survey, 74% to 83% of those opening the surveys meeting the eligibility requirements, and 84% to 91% of those meeting eligibility requirements completing the surveys. Furthermore, consecutive participating CC survey groups are necessarily distinct because the respondents were credentialed either in odd or in even years. For the same reason, the 2 odd-year surveys (2014-2015 and 2016-2017) predominantly represented repeat survey cohorts as did the 2 even-year surveys (2015-2016 and 2017-2018). Comparisons among sequential CC survey responses for odd-years, even-years, and all 4 survey years thus provided a consistency check for the findings.
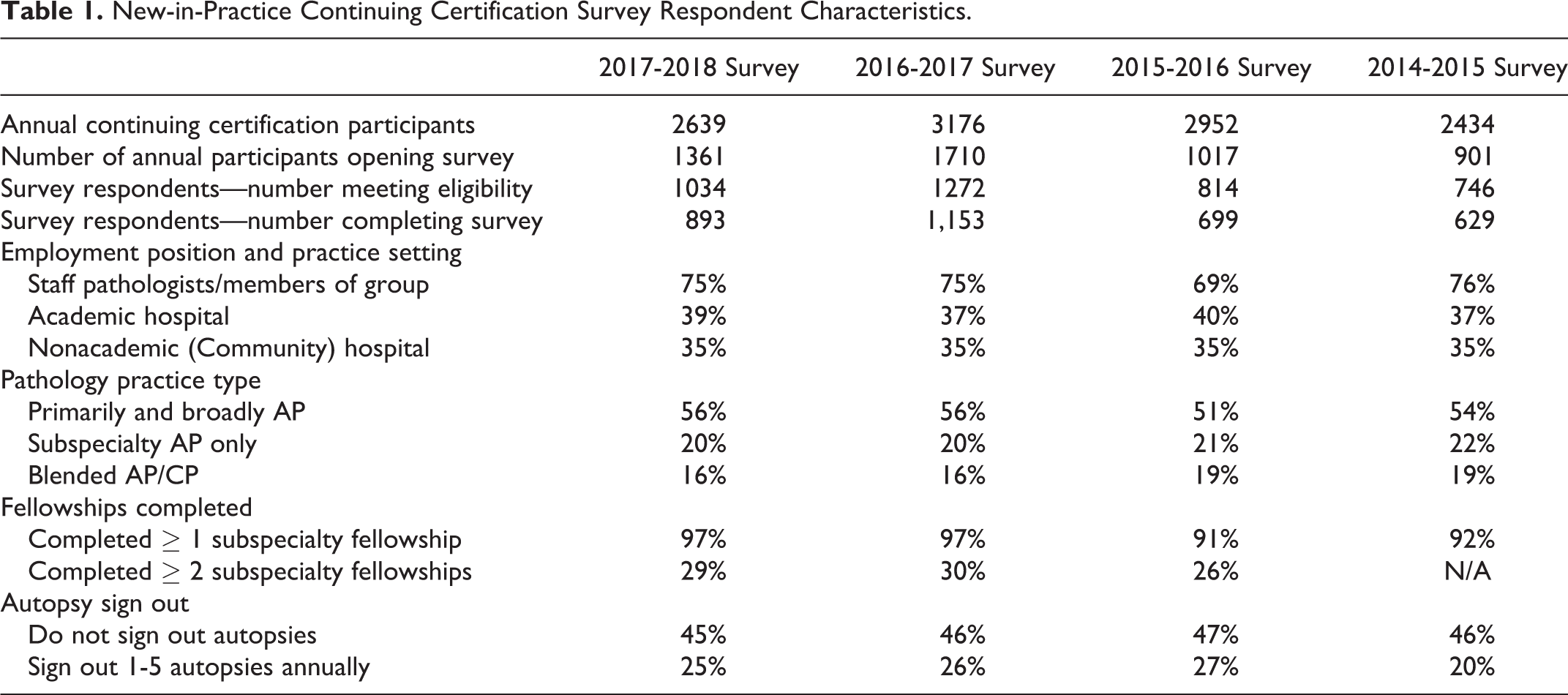
Throughout all surveys, the respondents’ practice demographics remained similar (Table 1), with over 90% of respondents completing at least one subspecialty fellowship (97% in 2017-18). About three-quarters practiced as staff pathologists or members of a pathology group, with about 40% practicing in academic hospitals (defined in these surveys as those with pathology residency programs) and 35% practiced in nonacademic (community) hospitals. Slightly more than half practiced primarily and broadly in AP, while about 20% practiced subspecialty-only pathology in AP areas; 6% practiced in CP areas only, and 3% practiced primarily in CP areas. The rest practiced a blend of all areas of pathology. Roughly half did not sign out autopsies, and another quarter signed out fewer than 5 autopsies annually.
New-in-Practice Continuing Certification Survey Respondent Characteristics.
Employer Survey Response Rates
The response rate for the Employer Survey, which served as a reality check on the CC (new-in-practice) surveys, was substantially lower than the latter surveys. In total, 2,383 pathologists received an invitation to complete the online employer survey. Among those who opened the survey, 60 were eliminated because their practices had not hired a new-in-practice pathologist within the last 5 years and 49 because the respondent had not been the one responsible for hiring or supervising the new-in-practice pathologist. A total of 204 (8.6%) participants opened and completed the survey, providing complete data for at least 1 new-in-practice pathologist.
Comparison of CC Survey and Employer Survey Results
As previously reported, all 4 CC surveys, despite minor changes in survey content, returned strikingly consistent responses showing highly significant intersurvey agreement. In particular, all 4 CC surveys showed concordance on the need for more or less residency training in each practice area. The employers’ survey was likewise highly correlated with the new-in-practice surveys (Pearson r = .96; P < .00001), although employer responses showed more variation than among the CC surveys (Figure 1).
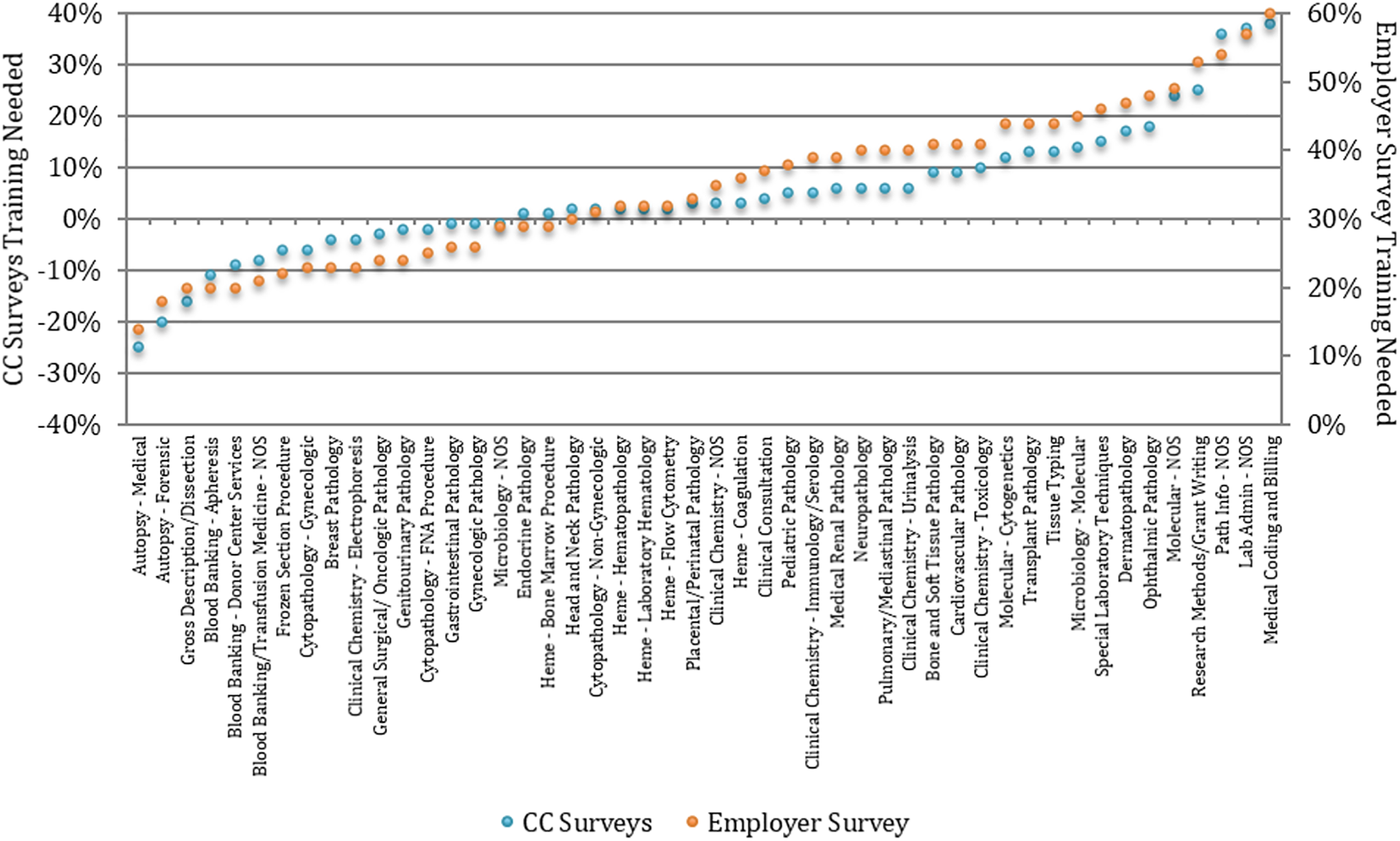
Training needed by practice area, based on combined CC surveys and employer surveys. The training needed by practice area as reported by new-in-practice respondents (4 CC surveys combined) and by the employers. Note that the scale of the CC surveys ranges symmetrically from need for less (−) training through need for more (+) training, while the unadjusted scale of the employers’ survey is restricted to reporting the degree of need for more (+) training. NOS indicates not otherwise specified.
New-in-practice respondents reported a full scale of responses, ranging from more (positive) training needed to about right (neutral) and to less (negative) training required. While employers can readily determine whether their employees have a (positive) need for more training or are adequately trained (neutral), they are not able to discern whether their employees might have had excessive training in any practice area—training over that required for practice (a negative need for additional training). Thus, the employers’ scale is intrinsically truncated relative to that of the new-in-practice pathologists, spanning only a range of more (positive) training needed to adequate (neutral) training. The consequence is that employers’ responses are numerically positive relative to those of the new-in-practice pathologists in every category. Irrespective of this intrinsic difference in scale, the significant finding is that the employers’ responses closely parallel those of the new-in-practice pathologists.
Another significant limitation in comparing the CC surveys with the employer survey is the difference in survey logic between the 2 instruments. Both survey types asked similar questions, but to minimize the time required for employers to complete the survey, they were first asked in which of a small number of broad practice categories the employee had responsibilities. They were then only asked to respond on specifics within the broad practice categories selected. For example, unless the pathologist being rated had at least some practice responsibilities within the general practice category of cytopathology, no employer assessment was sought on the specific subsidiary areas (GYN, non-GYN, and FNA) of cytopathology. This led to fewer ratings at the low end of practice importance than the CC surveys, with any reported practice areas rated more important. Thus, the employers’ average area importance ratings averaged 17% higher overall than those of the new-in-practice respondents. Despite greater variation in employer responses for practice importance and, hence, the lower correlation with the ratings reported in the CC surveys, the correlation between the employer surveys and the CC surveys remained highly significant (Pearson r = 0.83; P < .00001; Figure. 2).
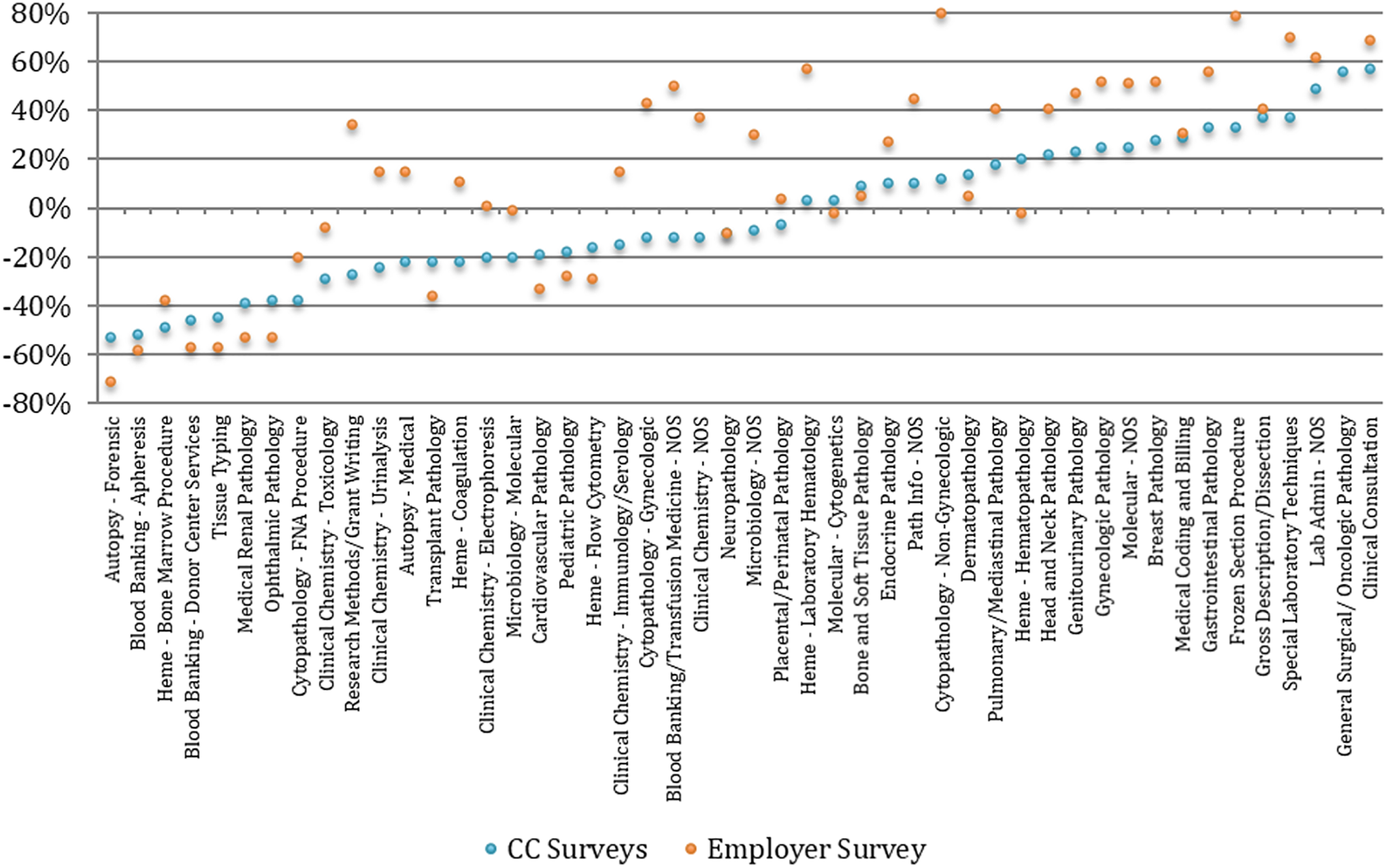
Practice importance by practice area, based on Employer vs Combined CC Surveys—Assessment of Practice Area Importance. NOS indicates not otherwise specified.
Alignment of Training Need and Practice Importance Survey Results
The focus of the rest of this article deals with the alignment of categorical residency training to practice. The following analyses address differential importance ratings of practice areas in which new practitioners have not taken fellowship training. The complementary analyses, comparing practice area assessments by residency-only trained practitioners to those of their peers who have also taken fellowship training in the practice area, will be the subject of a subsequent article.
The combination by practice area of a new-in-practice pathologist’s ratings of practice importance and residency preparation provides a measure of the alignment of that pathologist’s residency training with his or her subsequent practice responsibilities. To the extent that such findings are consistent across the population of recently trained pathologists, they provide a general assessment of residency training’s alignment with practice. Figure 3A and B provides 2-dimensional graphical representations of how the training received during categorical residency in each practice area compared with that needed for actual practice (on the ordinate) and how important that same area was in practice (on the abscissa). Figure 3A is from the quadrant of practice areas assessed by respondents as both important in practice and needing more residency training. In contrast, Figure 3B comes from the opposite quadrant, that is, practice areas deemed less important in practice and where training was more than that useful for practice.
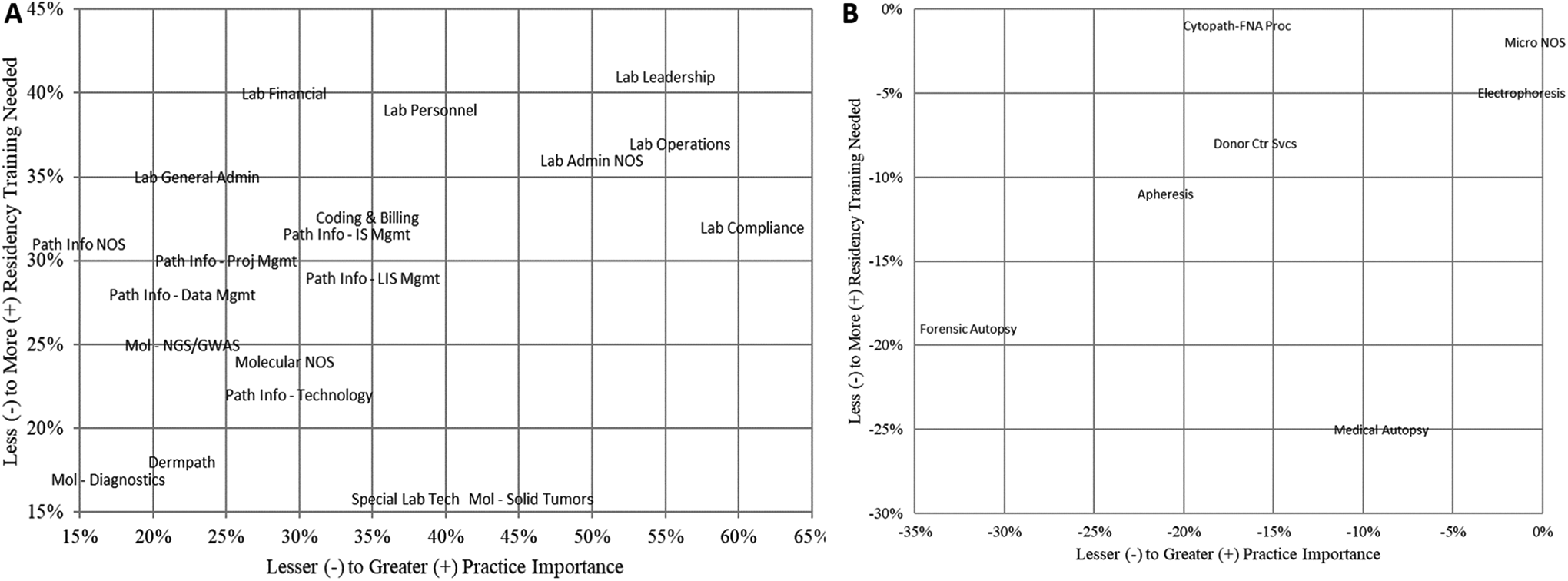
Misalignment of training and practice. (A) Areas more important in practice and in need of more residency training. Upper right portion of 2-dimensional distribution of CC survey responses showing areas rated most important in practice and most in need of more training in residency. (B) Areas less important in practice and in need of less residency training. Lower left portion of 2-dimensional distribution of CC survey responses showing areas rated least important in practice and most in need of less training in residency.
The significance of our findings, and how and why they vary by practice circumstances, is the principal subject of the remainder of this article. A comparable, although less focused graphical representation of practice areas without specific discussion appeared in our earlier publication 5 . Before exploring the relatively small number of practice areas for which our findings suggest residency is suboptimally aligned with practice, we note that the new practitioners reported the residency preparation they received in most areas to have been “about right” for them to commence practice. We make this statement with the caveat that young pathologists entering the job market will do their best to find jobs for which their training has appropriately prepared them. And likewise, their prospective employers will seek to ensure each new hire is appropriately ready for his or her position.
Two practice areas (autopsy pathology and specialized blood banking) were deemed most eligible for decreased training in residency (Figure 3B). Only 15% of surveyed pathologists signed out more than 15 autopsies per year, and, of those few who did, more than half (54%) were subspecialty trained in 1 of the 4 fellowship areas, where autopsy expertise is a core requirement: forensic pathology, neuropathology, pediatric pathology, or cardiovascular pathology. Of the 9% of all respondents who performed over 30 autopsies per year, 74% had 1 of those 4 fellowships. Similarly, 61% and 67% of new-in-practice pathologists who had Blood Banking fellowships rated apheresis and blood donor center services as, respectively, very or critically important, as compared with just 5% and 8% of those who did not have a blood banking fellowship.
Our methodology of excluding from analysis subspecialty areas where the new-in-practice respondent received subsequent fellowship training permits identification of areas that might benefit from additional training during categorical residency (Figure 3A). Conversely, for those subspecialty areas characterized by active practitioners having predominantly taken further training as fellows, it would appear reasonable to refocus the emphasis of training from residency to the fellowship period.
To suggest reducing the residency training in these areas is not to imply a lack of medical importance. Instead, it indicates a misalignment between training received in residency and preparation required for practice, even allowing for employee and employer having sought a good “fit.” Reducing the residency time spent training in these areas would provide the additional time needed in other areas. 8
Several important practice areas that graduates needed in their new jobs stood out in these surveys. They noted deficiencies in laboratory administration, pathology informatics, and molecular pathology (Figure 3A). These are areas of professional responsibility that typically only a small subset of pathologists perform in settings where residency training occurs. In addition to not being broadly performed by residency program faculty, neither laboratory administration nor pathology informatics is case based in the traditional sense, meaning that training in these topics is less typically a core rotation. Training thus often relies instead on didactic modalities or set-aside training experiences. 9 -11 Instead, programs might consider alternative training models that consist of a core of general training with a selection of advanced modules, either general or subspecialty (a model resembling what the ABPath has designed for its CC process). 12 Such a model may be particularly relevant for trainees whose direction is established early during categorical training. Molecular pathology is a rapidly evolving subdiscipline, bringing a new understanding of disease states and new diagnostic and therapeutic opportunities. Consequently, the field of molecular pathology is in flux, both among and within institutions, with education lagging practice, and the information transfer from academia to the community typically associated with newly trained practitioners entering community practice also lagging. We explore the educational implications of these circumstances in these 3 areas below.
Medical coding and billing, like laboratory administration and pathology informatics, holds less interest among residency program faculty. Such responsibilities are often centralized to a group practice billing department. Advancement for faculty typically depends substantially on academic productivity as well as provision of billable services, and training in an academic setting will thus not spontaneously align with requirements of community practice.
Dermatopathology is the only area of traditional case-based diagnostic experiential learning that appears in the essential and undertaught portion of our analysis (Figure 3A). Although confidentiality in data collection precludes tracing responses back to specific training institutions, we speculate that redirection of dermatopathology specimens away from teaching institutions’ pathology departments may impair teaching in this vital subdiscipline.
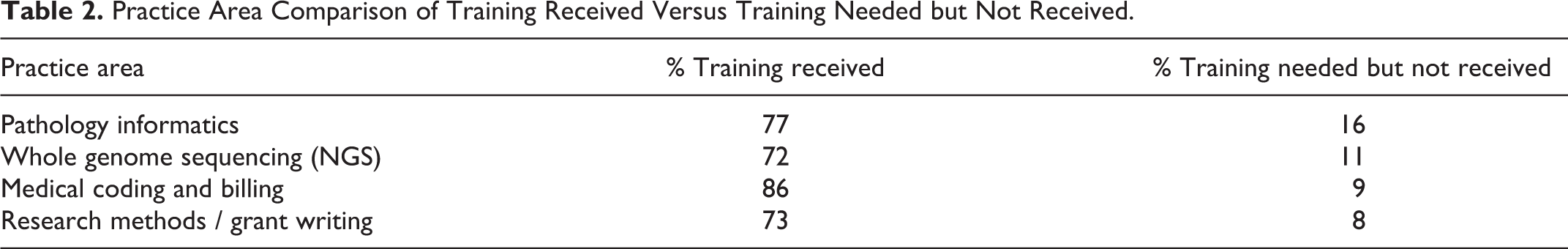
Our surveys, seeking to identify training deficiencies, looked at practice areas where the training received was less than what was needed in subsequent practice. For each practice area, respondents could submit a rating of “No Knowledge Needed” and/or a rating of “No Training Received” in residency. Disparities in these responses between training needed and training received (Table 2) stood out in 4 areas: pathology informatics, whole genome sequencing (NGS), medical coding and billing, and research methods and grant writing, ranging from 8% to 16%. The area with the most striking difference was informatics in which nearly a quarter (23%) reported receiving no training in residency; while 16%, fully two-thirds of the 23% with no training, reported needing knowledge in their subsequent practice.
Practice Area Comparison of Training Received Versus Training Needed but Not Received.
Anatomic Pathology Versus Clinical Pathology
Pathologist trainees can choose any 1 of 4 pathways leading to primary ABPath certification in pathology. The vast majority (83%) of trainees certify in AP/CP, 12% pursue AP-only, 4% CP-only, and 1% AP-Neuropathology. 13 We specifically assessed practice area differences between AP-only and CP-only trained respondents for both practice importance and training needed. To determine the difference, we analyzed the effect of including versus excluding AP-only and CP-only certified respondents from practice areas irrelevant to respective certificates (eg, excluding blood banking for AP-only and medical autopsy for CP-only). The difference between including all responses and excluding the certificate-irrelevant responses proved minimal (Figure 4). In particular, changes in the most critical survey measure, Training Needed, ranged from 0% to 2% because most CP-only respondents had already excluded themselves from rating AP-only practice areas by responding “no training” received and vice versa for the AP-only respondents.
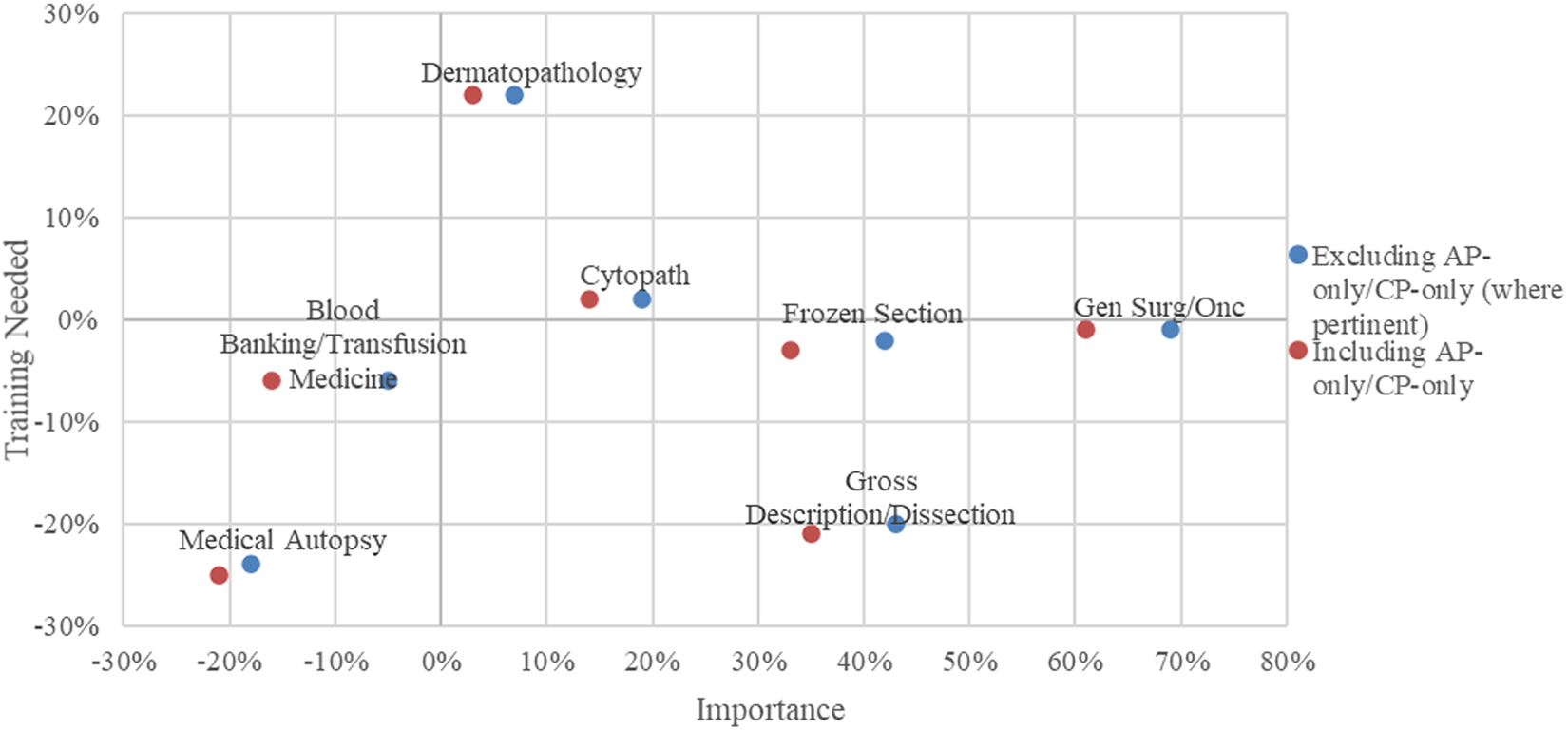
Effect of including versus excluding AP-only and CP-only certified respondents from practice importance and training needed ratings in 2019-2020 CC Survey. This analysis focused on these 7 practice areas because the 2019-2020 CC survey was abbreviated to 13 practice areas, with the remaining 6 areas being applicable to both AP and CP.
Pathologist and Work Setting Variables
Since no common model characterizes all pathology practices, we next explored how multiple interrelated variables influence the workplace. These included work setting, practice size, years in practice for the new-in-practice respondent, and the degree to which practice is subspecialized versus general. Subset analyses stratified our new-in-practice respondents by practice size (<6, 6-15, and >15 pathologists); practice setting 8 (academic/teaching hospital vs nonacademic/community hospital); and years in practice (≤3, 3+ to 5, and 5+ to 10). As an illustrative (and validating) example, for most subset analyses, respondents in large practices overall rated both practice importance and residency preparation similar to those in academic practices. The understandable exception was that academic practice pathologists reported a net need for additional training in Research Methods and Grant Writing, while large practice nonacademic pathologists did not (Figure 5).
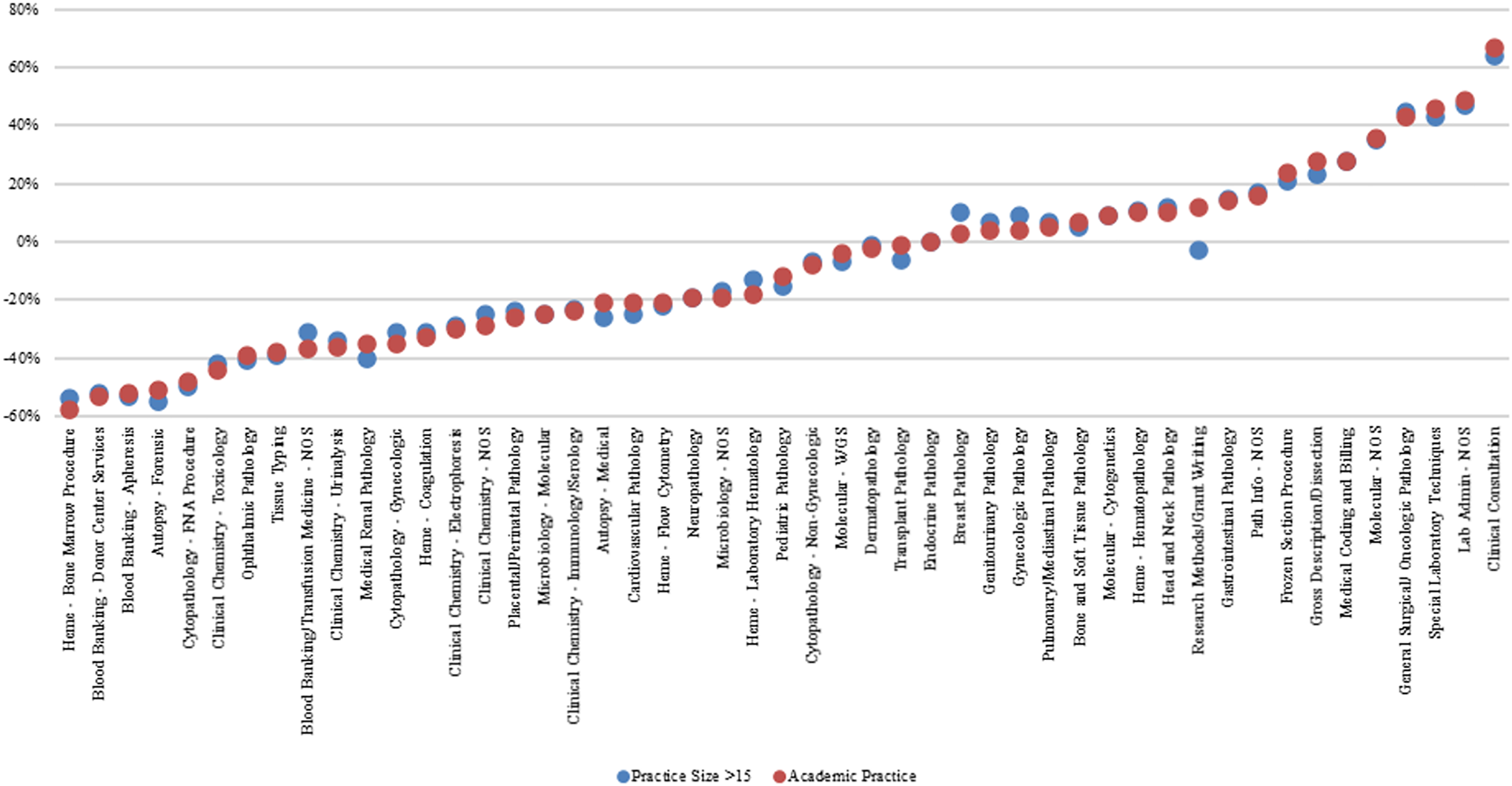
Practice area importance ratings by practice size and setting. Four-survey combined CC practice importance ratings showing the broad similarity between the overlapping subsets of respondents in large (>15 pathologists) practices and those in academic practice settings. NOS indicates not otherwise specified.
The importance ratings of 54 of the 71 practice areas were essentially the same from the academic and large practice setting respondents and from the community and small practice respondents (data not shown). For 17 practice areas, the differences were striking. Four practice areas were rated higher in importance by academic and large practice setting respondents than by community and small practice respondents; the reverse was true for the other 13 areas. Figure 6 visually compares the 17 practice area importance ratings that differed between new-in-practice pathologists at large (>15 pathologists) versus small (<6 pathologists) and at academic versus other (nonacademic/community) hospital practices.
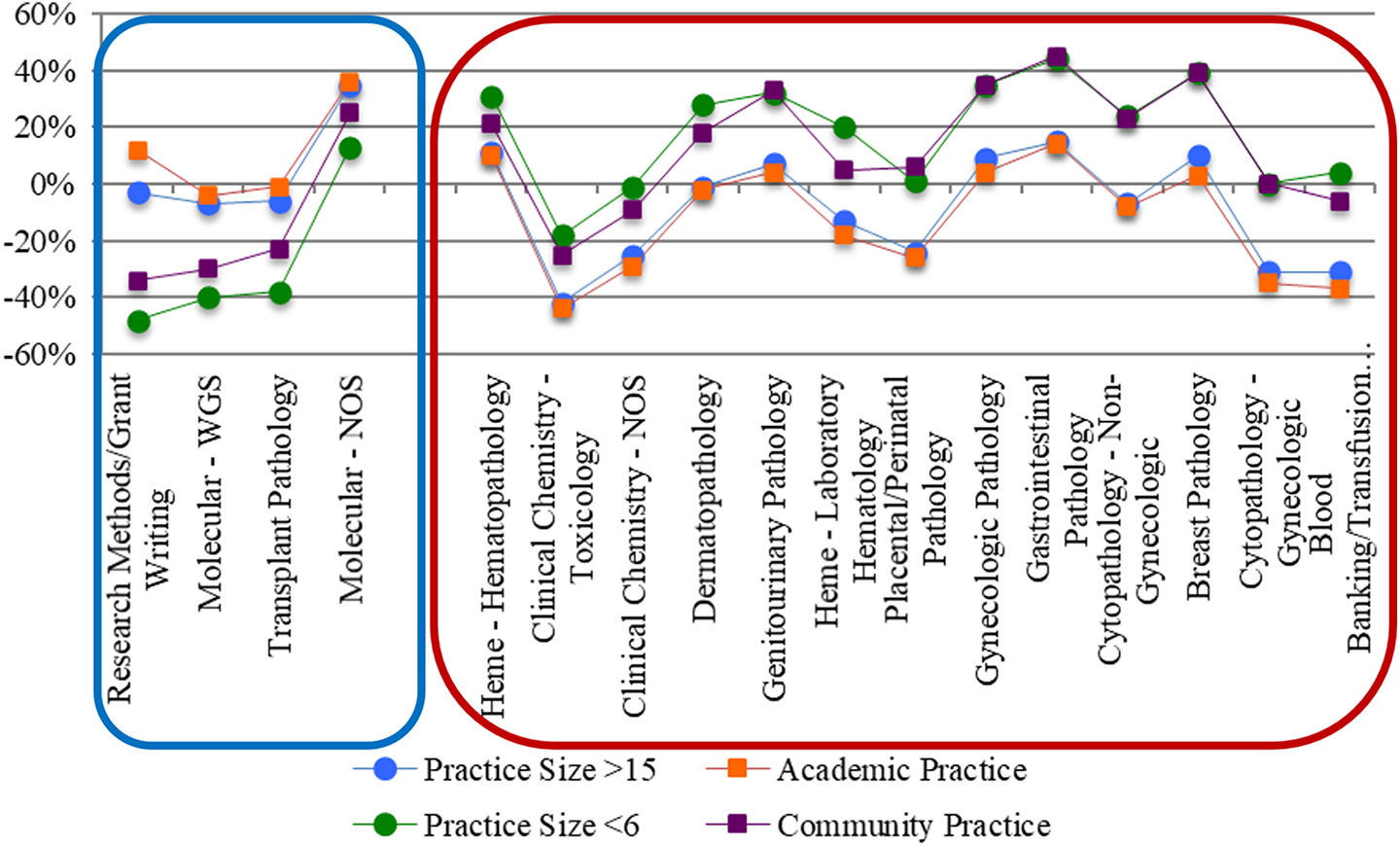
Practice area importance ratings by practice size (large vs small) and setting (academic vs community). Comparison of distinct practice subsets—academic versus community hospital respondents and large versus small practice respondents; unlike Figure 5, which displays responses for all practice, areas, Figure 6 selectively shows the 13 practice areas in which community and small practice respondents differ substantially from academic and large practices. NOS indicates not-otherwise-specified; WGS, whole genome sequencing.
Respondents from both academic and large practices rated the first group of areas—research methods and grant writing, molecular diagnostics, and transplant pathology (blue box; Figure 6)—more highly than those reporting from small and from nonacademic practices. In contrast, those from the community and small practices rated the following areas more important: blood banking / transfusion medicine, cytopathology, breast, gastrointestinal, gynecologic, placental / perinatal, genitourinary and dermatopathology, clinical chemistry, laboratory hematology, and hematopathology (red box; Figure 6).
Although the first (blue box) set of differences may be intuitively understood based on academic and/or referral institution characteristics, how can the second (red box) set of differences be understood? Would breast pathology, for example, be less important for large or academic practices? The answer is intuitively, no.
Analysis of the per respondent count of practice area importance ratings revealed that pathologists in both large practices and academic settings benefit from subspecialization. Considering subspecialization in the context of current pathology practice requires distinguishing how pathologists were trained from how they actually practice. After the ABPath discontinued the credentialing year requirement, pathology residency graduates have nearly universally come to take subspecialty fellowship training. But the corresponding extent and circumstances of subspecialized practice have not previously been quantitatively characterized.
By definition, subspecialized practice is limited in scope to narrow areas within a broad field of practice. A practice is subspecialized if a few practice areas are highly important to the practitioner and most others are much less important; a practice is general if most or all practice areas are important while few or none are unimportant. For example, a pathologist whose practice is exclusively in surgical pathology of the breast would rate Breast Pathology as Critically Important. Related practice areas (eg, frozen section procedure, gross description/dissection, medical coding and billing, and special laboratory techniques) might also rate as very or even critically important, while unrelated pathology practice areas would rate as less (or even un) important.
Analysis of the proportion of practice areas each respondent rated as highly important versus less (or un)important) shows that this second (red box) set of practice areas are the ones in which subspecialty practice is prevalent. These are the areas that practitioners in large and academic practices rated their own subspecialties critically or very important, while rating other areas less or unimportant. This inhomogeneous (variably high and low) rating by practitioners in large and academic practices is what decreases the average importance ratings in these settings. Meanwhile, their more generalist contemporaries in small and nonacademic practices, who have responsibilities in most areas, rate most areas at least very important and thus report more homogeneously high average importance ratings across all practice areas. These surveys, therefore, provide the first quantitative identification of the practice areas in which subspecialization is prevalent and how it varies by practice size and setting.
To quantify and illustrate the degree of subspecialization among academic practitioners versus community practitioners, we calculated and graphed for each new-in-practice pathologist the fraction of practice areas they rated as highly (critically or very) important (abscissa) versus the fraction they rated less important (ordinate). General practitioners are those for whom most practice areas are highly important and few practice areas are less important. Conversely, subspecialized practitioners are those for whom the majority of practice areas are of less importance than the minority that are highly important. As demarcated by an arbitrarily chosen 60% dividing line in Figure 7, subspecialists can be considered as those who rate at least 60% of practice areas less important (blue box), and generalists those who rate fewer than 60% of practice areas less important (red box). On this basis, 33% of new-in-practice academic pathologists are subspecialized. In contrast, 91% in community practice are generalists.
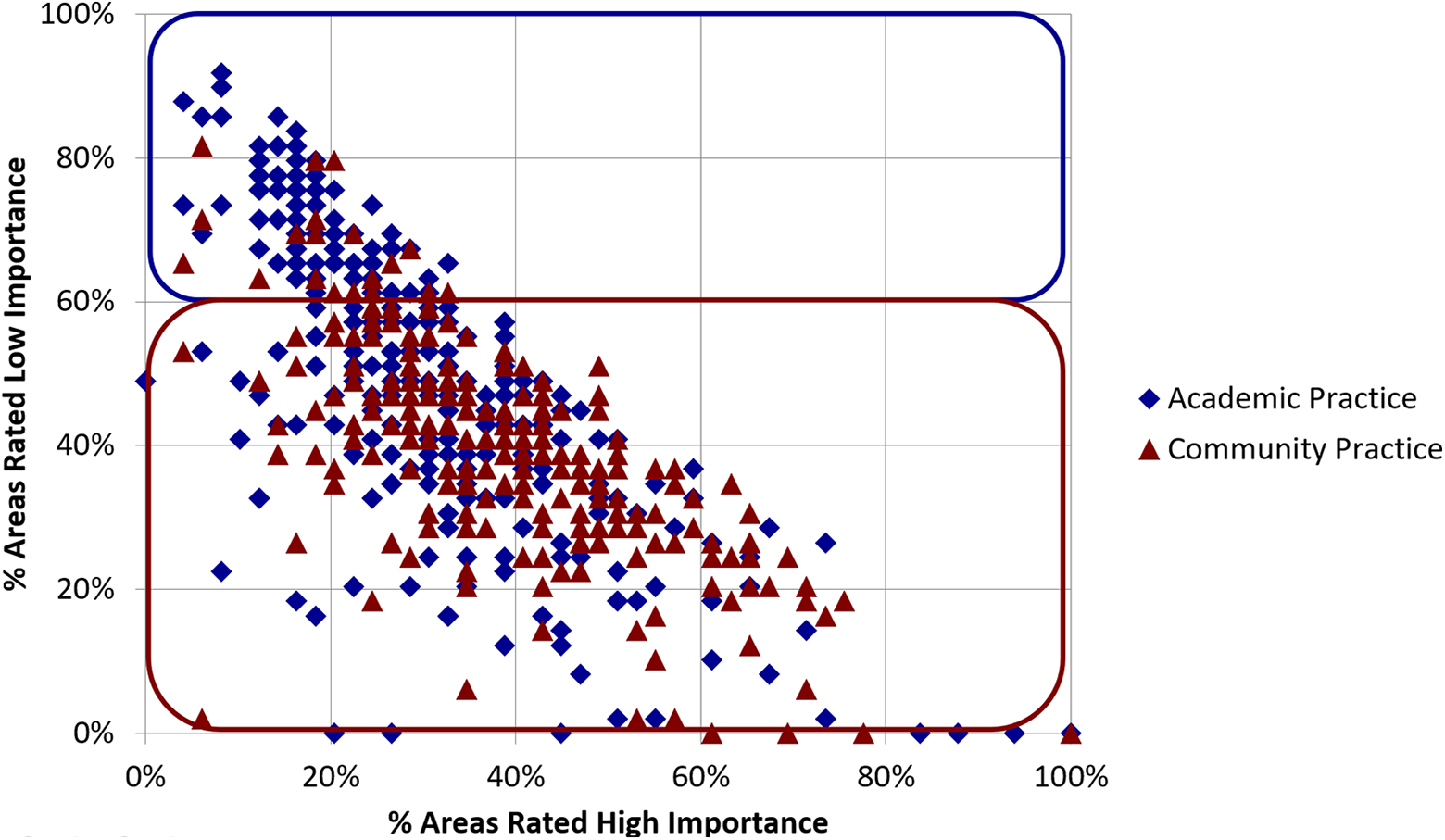
Subspecialty versus general practice in academic and community practices. Per respondent plot of fraction of practice areas rated critically or very important versus less important, with subspecialty practice (blue box) characterized by rating at least 60% of practice areas less than very important.
The findings were similar when comparing pathologists in small practices who were more likely to be generalists for whom a broad range of areas is at least very important and few (or no) areas unimportant, to those in large practices, who are more likely to be subspecialized. By the same criteria, 33% of new-in-practice pathologists in large practices are subspecialized, while 90% of those in small practices are generalists.
The 2016 and 2017 surveys were enhanced to explore 3 specific practice areas in greater depth, namely, laboratory administration, pathology informatics, and molecular diagnostics. The new, more granular, and specific subsidiary practice areas within these 3 areas confirmed their importance and need for more practice preparation (Figure 3A) but also revealed differences by years in practice (Figures 8 –10). Respondents further out from training considered several of these subsidiary practice areas more important to their practice and expressed more need for additional training than their less senior though still new-in-practice colleagues. For example, for the subsidiary laboratory administration area of personnel management, the weighted average for more training needed response was +39% among ≤3-year respondents, +40% among 3+ to 5-year respondents, and rose to +49% among 5+ to 10-year respondents (Figure 8).
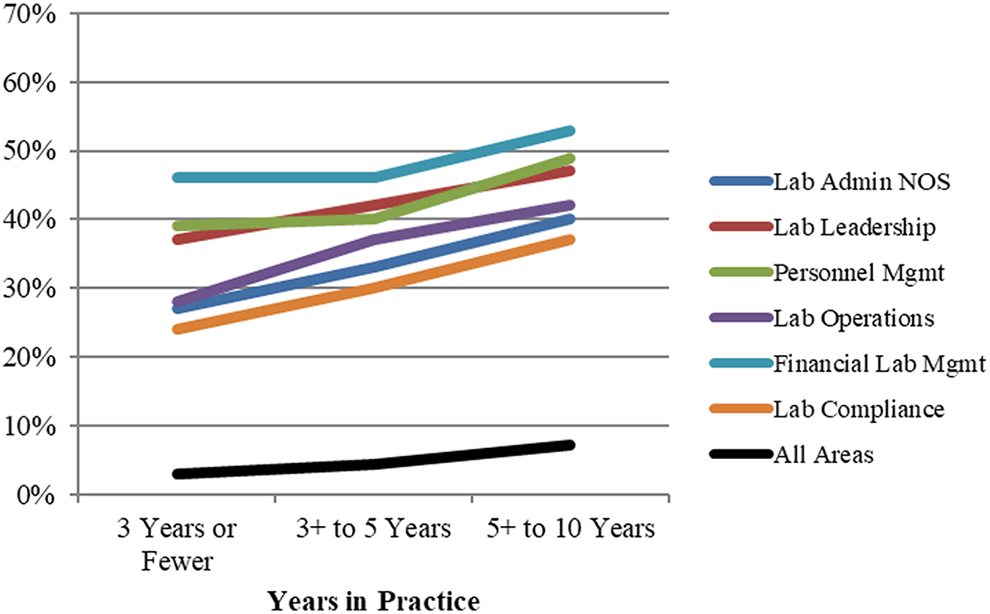
Laboratory administration more training needed—subsidiary Areas. Training needed responses among subsidiary areas, broken down by years in practice. Admin indicates Administration; Mgmt, management; NOS, Not otherwise specified.
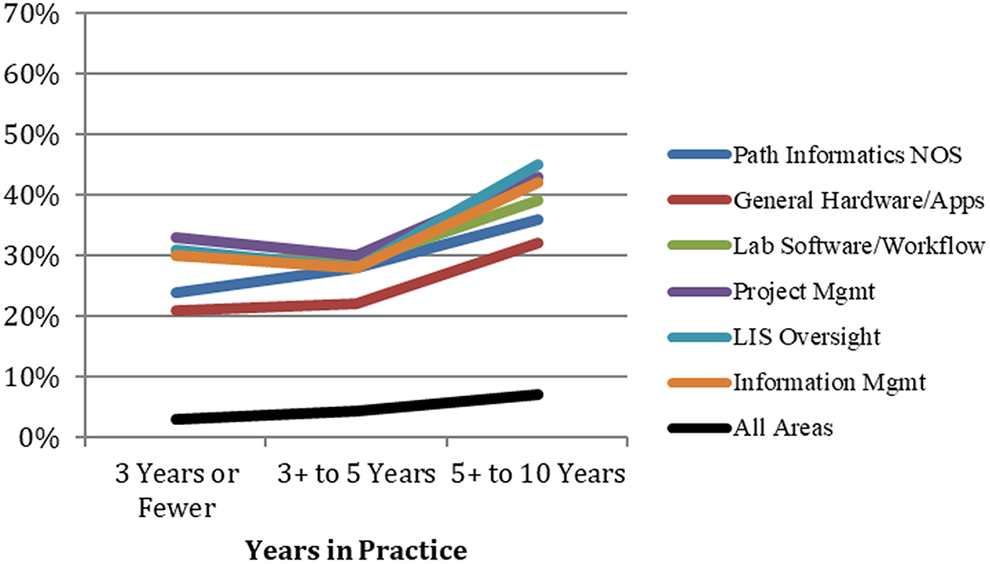
Pathology informatics more training needed—Subsidiary Areas. Training needed responses among subsidiary areas, broken down by years in practice. Apps indicates Applications; LIS, laboratory information system; Mgmt, management; NOS, not otherwise specified.
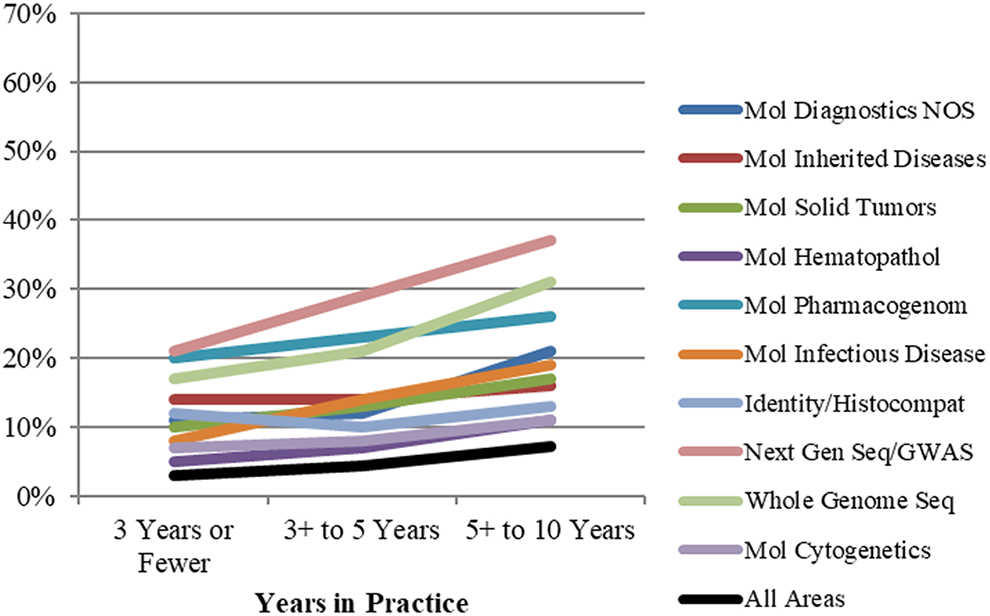
Molecular diagnostics more training needed—subsidiary areas. Training needed responses among subsidiary areas, broken down by years in practice.
Three potential hypotheses might account for the new-in-practice pathologists reporting an increasing perceived training deficiency with increasing years in practice. (1) More recent residents are better trained; (2) these are emerging areas of practice, about which less was known (and therefore taught) previously; (3) practice responsibilities of junior and more senior pathologists differ, with the latter requiring more skills in these areas. Of course, these hypotheses are not mutually exclusive, and very likely more than one applies in any particular instance. Nevertheless, they are conceptually vital because they differ in how the educational challenge implicit in each hypothesis might best be addressed.
If the graphically illustrated findings in the areas above (Figures 8 –10) reflect better recent residency training, we might be gratified. Without such evidence, it is more reasonable to consider this change over time in practice as reflecting a combination of the need for new knowledge in practice (life-long learning, practice-based learning, and improvement, continuing medical education) and assumption of additional practice responsibility with seniority. Specifically, new knowledge seems most likely to explain the shift in molecular diagnostics, while the shift in laboratory administration seems most likely due to advancing professional responsibilities with seniority in practice. The shift in pathology informatics, which is qualitatively similar to that in the other two areas and quantitatively intermediate to them, would plausibly reflect a mix of both phenomena. These findings raise questions about how most effectively to teach essential skills that would typically not be utilized until several years into practice.
Discussion
The rapid evolution of science and technology in a setting both of changing systems for health care delivery and the expected net decrease in the future pathologist workforce demands assessment and adaptation in pathologists’ training for practice. 8 The one-size-fits-all residency approach based on the presumed relative advancement of academic over community practice can no longer be relied upon to assure pathologists are optimally prepared for future practice. As there are calls today to reexamine the whole of US medical education, 14 still fundamentally based on the now 110-year-old Flexner report, each medical specialty must consider how best to deploy the educational resources entrusted to it.
This study constitutes the most extensive quantitative assessment of how residency training in pathology prepares for practice upon graduation. We sought to examine both the efficacy and the efficiency of our educational processes. The data obtained should enable us to focus on what in our existing curriculum and educational methods requires change, if we are to properly equip new-in-practice pathologists for successful entry into the workplace, and for the assumption of increasing responsibility in subsequent years.
Multiple conclusions emerge from our work.
First, the new-in-practice pathologists share strikingly consistent perceptions about what is essential in pathology practice and how residency prepared them.
Second, the preparedness that the new-in-practice pathologists and their pathologist employers reported for practice in each practice area is almost identical. Both groups reported virtually the same degree of import.
Third, both groups agreed that three broad practice areas need additional training—laboratory administration, pathology informatics, and molecular diagnostics. Others have also commented on the need for enhanced GME in these areas. 15,16 In 2010, survey data showed 11% of all pathologist effort was in laboratory medical direction and another 6% in general medical administration. The total percent effort in laboratory administration was projected to rise to 24% by 2030. 17 The educational challenges implicit in these deficiencies may at least partially be addressed by specific curricular materials. To this end, the APC, through its residency program directors section (PRODS), sponsored the development of a program for training residents in genomics (TRIG). The APC PRODS likewise sponsored the creation of pathology informatics essentials for residents (PIER), in conjunction with the association for pathology informatics and the CAP. 18 -21 Various programs and concepts for teaching laboratory administration have appeared but are not yet widely practiced. 9 -11,22 -26 The development by professional societies of focused curricular materials for resident training in medical coding and billing might likewise help meet new-in-practice pathologists’ needs in this area of educational deficiency.
Fourth, some categorical areas of resident training require reconsideration as principally subspecialty areas of practice. These are medical and forensic autopsy and apheresis and blood donor center services among blood banking practice areas. Other than those who also had fellowship training in these areas, few new-in-practice pathologists identified these areas as important in practice. At the same time, many reported having had substantially more training than was practically useful.
Fifth, practice area ratings of importance vary by practice setting and size. Except for research methods and grant writing, which was of importance only in academic practice, pathologists in large practices and academic practices rated the importance of practice areas similarly. Those in small and community practice likewise ranked practice areas similarly in importance. Two sorts of differences appeared in how they rated practice importance. Some differences related to community versus referral hospital patients (eg, need for genomic analysis or transplant services), while the other differences corresponded to different approaches to providing more routine care: subspecialized versus general practice. These surveys quantitatively demonstrate how practice areas differ in services provided between pathologists working in smaller, typically community hospitals and those working in large or academic hospitals. This variability points to the need for a flexible training system—one offering options that efficiently address the broad observed spectrum of practice from general to subspecialty. A modular system could potentially more effectively utilize the present typical 5 to 6 years (4 of residency plus 1 or 2 of fellowship) time in training for pathologists. For example, published proposals for a modular system could more efficiently utilize this available time in training to cover the full observed spectrum of need, from gaining deep expertise in a few subspecialty areas to training broadly for general practice. 15,16 Such modularity could potentially also serve to bridge the observed differences in structure and content of training among different sized residency programs. 27
Sixth, in the last 2 CC surveys, we “drilled-down” on subsidiary areas within the 3 broad practice areas of greatest practical importance and most need of more training: laboratory administration, pathology informatics, and molecular diagnostics. All subsidiary areas of laboratory administration and pathology informatics showed high importance and need for more training. In contrast, the only subsidiary area of molecular diagnostics high in both was NGS. It was not that respondents felt well trained in the other subsidiary areas of molecular diagnostics, but rather that the other subsidiary areas were not perceived to be high in practice importance. These findings point out that we need to incorporate our best projections of each area’s future practice importance in deciding how such findings should inform curricular decisions—education is intrinsically for the future.
Seventh, we found as pathologists advanced in years in practice, they felt the need for additional postgraduate training for several subsidiary practice areas. This finding raises the question of how most effectively to teach essential skills that will typically not be utilized until several years into practice. Many professional responsibilities begin only several years after one enters practice. In such cases, the requisite training may not be best addressed during residency or even fellowship but rather by more flexible modular or continuing education closer to its application in practice. We do observe that enhanced training in laboratory management has successfully been incorporated into categorical pathology residency training in some programs. 27 -29 Pathology societies, such as the APC, ASCP, CAP, and USCAP, may wish to work with the ABPath to develop innovative longitudinal courses with practicums involving projects and experience in pathologists’ current home practice settings. Additionally, it is imperative that a foundation of life-long learning be instilled in trainees during their formative residency and fellowship experience, and programs should take pains to create an environment of academic inquiry and self-directed study that will foster such an approach to practice.
There are limitations to our research. Recall bias could have influenced survey responses, given that our survey gathered information about training received up to 10 years prior. However, the striking consistency of new-in-practice results across years combined with the similarity between new-in-practice and pathologist employer responses suggests recall bias likely had minimal impact on our conclusions.
Further, response rates for the new-in-practice survey varied across years from 34% to 54%. The reason for this variation is unknown, and response rates for online surveys can vary widely depending on factors, such as the length of the survey, purpose, and respondent motivation to participate. 30 The average response rate for online surveys ranges from 20% to 33%, so our response rate is excellent compared to this norm. 31,32
Finally, the data reported are from the 2014-2015 to 2017-2018 CC reporting cycles, which makes it somewhat dated. Although the survey continues to be conducted annually, our analysis does not include data from the 2018-2019 or 2019-2020 cycles because of changes in the survey format beginning in 2018-2019. However, because of the consistency of results across survey years reported within this article and the similarity of subsequent years’ results for those practice areas that were not changed, we do not expect additional years’ data to affect our conclusions.
In summary, and perhaps most importantly, our work points out that there are areas important in practice in which new practitioners consistently report they were inadequately trained. Some areas involve “the first day on the job” responsibilities, while others only become important with longevity in practice. Some areas are consistently reported as having been taught in residency to a greater extent than proved practically useful. These are areas in which practice is functionally restricted to those who have fellowship training. Furthermore, for many other practice areas, there are significant disparities among the need for broad training across most or all areas versus narrower expertise in only some, and these latter do not solely correspond to fellowship-trained areas. The aggregate import of these observations suggests that the current fixed 3- or 4-year “one-size-fits-all” residency curriculum, plus 1 or 2 one-year fellowships, is not structurally well suited to align with the breadth and variety of actual practice. Quantified for the first time, these issues point to the need for a core-plus-modules model for GME (and beyond) in pathology. For analogous reasons, the ABPath has already adopted such a model in its program of continuing certification.
Continuing assessment, based on ongoing monitoring of pathology trainees entering into practice, is needed to determine optimal paths to most efficiently utilize the resources at hand to produce the best-prepared pathologists. These issues include assessing the significance of inconsistent assignment of progressive responsibility among residency programs and the role fellowship training plays in the selective performance of some practice areas. Based on new-in-practice pathologists reporting perceived deficiencies, studies may also helpfully examine the following hypotheses. Are our more recent residents better trained than graduates from a decade ago? Are there emerging areas of practice that we might anticipate and for which we might design better instructional programs? How should we do this if practice responsibilities differ between junior and more senior pathologists? If pathologists in practice for 5 to 10 years need skills different from or in addition to those new in practice, how do we assess and assure training for those pathologists 10 to 20 years or longer in practice? All these start with measuring the present effectiveness of our educational systems. The pathology community has much at stake and should be actively involved in the most appropriate training for future pathologists.
Supplemental Material
Supplemental Material, sj-docx-1-apc-10.1177_23742895211002816 - Evidence-Based Alignment of Pathology Residency With Practice II: Findings and Implications
Supplemental Material, sj-docx-1-apc-10.1177_23742895211002816 for Evidence-Based Alignment of Pathology Residency With Practice II: Findings and Implications by W. Stephen Black-Schaffer, Stanley J. Robboy, David J. Gross, James M. Crawford, Kristen Johnson, Melissa Austin, Donald S. Karcher, Rebecca L. Johnson, Suzanne Z. Powell, Joseph Sanfrancesco and Michael B. Cohen in Academic Pathology
Supplemental Material
Supplemental Material, sj-docx-2-apc-10.1177_23742895211002816 - Evidence-Based Alignment of Pathology Residency With Practice II: Findings and Implications
Supplemental Material, sj-docx-2-apc-10.1177_23742895211002816 for Evidence-Based Alignment of Pathology Residency With Practice II: Findings and Implications by W. Stephen Black-Schaffer, Stanley J. Robboy, David J. Gross, James M. Crawford, Kristen Johnson, Melissa Austin, Donald S. Karcher, Rebecca L. Johnson, Suzanne Z. Powell, Joseph Sanfrancesco and Michael B. Cohen in Academic Pathology
Footnotes
Acknowledgments
The authors wish to acknowledge the contributions of Jason Park, MD, PhD, and Aidan DeLisle, MPP, for their contributions in the preparation of the manuscript. They also acknowledge the contributions of several people who were consulted in the research that contributed to the development of this article, particularly Barbara S. Ducatman, MD; Kimberly A. Gyure, MD, and Karen L. Kaul, MD, PhD. The authors take full responsibility for any errors and omissions contained in this article. Any opinions expressed in this article represent those of the authors and not those of the institutions with which they are associated.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
