Abstract
Keywords
Primary Objective
Competency 2: Organ System Pathology; Topic: Female Reproductive-Disorders of Pregnancy (FDP); Learning Goal 1: Disorders of Pregnancy
Patient Presentation
An 18-year-old student presents with painless vaginal bleeding. She reports feeling nauseous with vomiting over the past week. The vaginal bleeding began 2 days ago. She describes the bleeding as heavier than her typical menstrual periods and that her last menstrual period was 15 weeks ago. A home pregnancy test was positive 12 weeks ago. She has not received any prenatal care. The patient denies any recent trauma or abdominal pain.
Physical examination reveals a well-appearing individual in no acute distress. Her temperature is 98.5 °F. Her blood pressure is 170/90 mm Hg. Her blood pressure 1 year ago during an employment physical examination was 110/70 mm Hg. No adnexal tenderness or masses are detected. The uterus is large for the gestational age on bimanual examination. A bloody vaginal discharge is noted. The cervical os is closed.
Diagnostic Findings, Part 1
Initial serum beta human chorionic gonadotropin (β-hCG) is 110,000 mIU/mL (4,800-82,000 mIU/mL at 15 weeks’ gestation). 2 Ultrasonography does not demonstrate a fetus within the uterine cavity. An intrauterine mass with cystic spaces (snowstorm pattern) and absent fetus is seen (Figure 1).
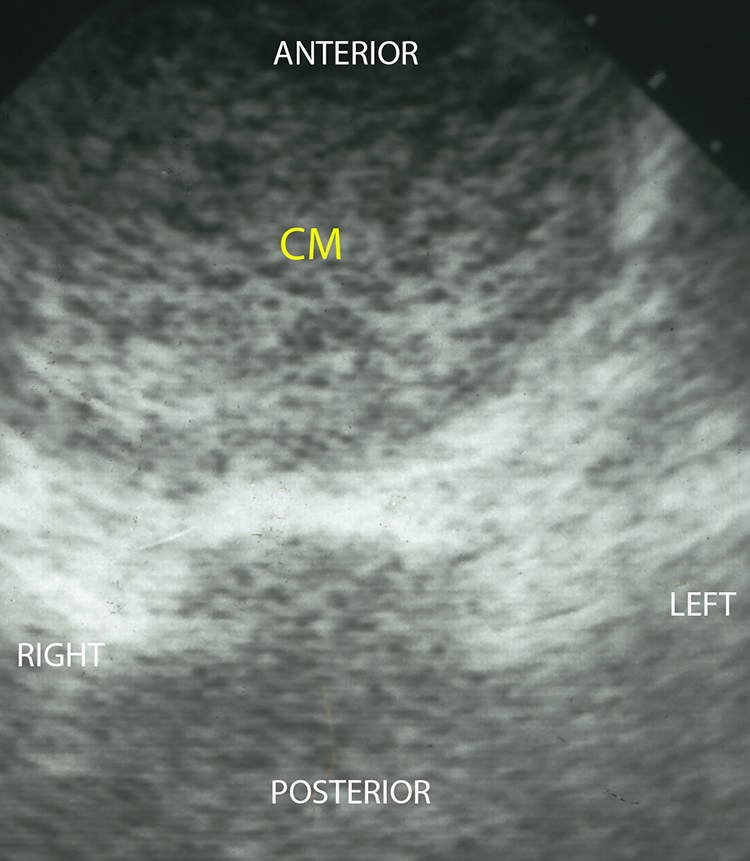
Transverse image of complete hydatidiform mole on ultrasonography. Note the complex intrauterine mass of tissue with cystic spaces (CM). This finding is referred to as a “snowstorm” pattern, sonographically.
Questions/Discussion Points, Part 1
What Is the Differential Diagnosis for Vaginal Bleeding During Pregnancy?
There are several causes of vaginal bleeding in pregnancy that should be ruled out. An uncomplicated intrauterine pregnancy can be associated with nonspecific symptoms including vaginal bleeding, nausea, and abdominal pain. 3,4 The most common nontraumatic cause of first trimester vaginal bleeding is pregnancy loss (spontaneous abortion, miscarriage). If the patient had an incomplete miscarriage, retained products of conception could result in vaginal bleeding typically associated with fever and abdominal pain. 4 Approximately 18% of women who present to the emergency department with vaginal bleeding and abdominal pain are diagnosed with ectopic pregnancy. 5 Ectopic pregnancy or ruptured ectopic pregnancy, while typically occurring 6 to 8 weeks after the last menstrual period, can also occur later in pregnancy. 5 Molar pregnancy (partial or complete) can also result in vaginal bleeding. The diagnosis is indicated by high levels of β-hCG and ultrasonography that shows the absence of an intrauterine pregnancy.
Second and third trimester vaginal bleeding is less common. Cervical insufficiency (incompetent cervix), placenta previa, and placental abruption are recognized etiologies. Cervical insufficiency will present with placental membranes extending beyond the cervical os on examination. Placenta previa, placental tissue extending over the cervical os that can be ruled out with ultrasonography, is different from placental abruption which is the premature separation of the placenta from the uterine wall prior to delivery. 6
What Is the Most Likely Diagnosis Based on the Patient’s Clinical Presentation and Lab and Imaging Findings?
Based on the clinical presentation, the patient is unlikely to have an ectopic pregnancy given the lack of adnexal tenderness and no evidence of ectopic gestation on ultrasonography. The elevated β-hCG level of 110,000 mIU/mL is also uncharacteristic of an ectopic pregnancy. The elevated β-hCG also would not be present in a miscarriage, which would have declining β-hCG levels. Although the enlarged uterus could be characteristic for a twin pregnancy, this would also be confirmed by ultrasonography. Given the clinical presentation of elevated β-hCG, uterus enlarged for the gestational age, vaginal bleeding, intrauterine mass with no evidence of fetus on ultrasonography, and young patient age, the most likely diagnosis is a complete hydatidiform mole. 7,8
A hydatidiform mole is a gestational disorder within the spectrum of gestational trophoblastic disease (GTD) that is characterized by abnormal trophoblast hyperplasia. Hydatidiform mole (classified as complete or partial), invasive mole, placental site trophoblastic tumor, epithelioid trophoblastic tumor, and choriocarcinoma make up the spectrum of GTD. 7,8 Gestational trophoblastic neoplasia (GTN) is a term that describes the following entities: invasive mole, choriocarcinoma, placental site trophoblastic tumor, and epithelioid trophoblastic tumor.
Diagnostic Findings, Part 2
Based on the clinical presentation and ancillary studies, a dilation and curettage (D&C) was performed. The curettings were submitted for pathological examination.
Describe the Findings Seen in the D&C Specimen (Figures 2 -5)
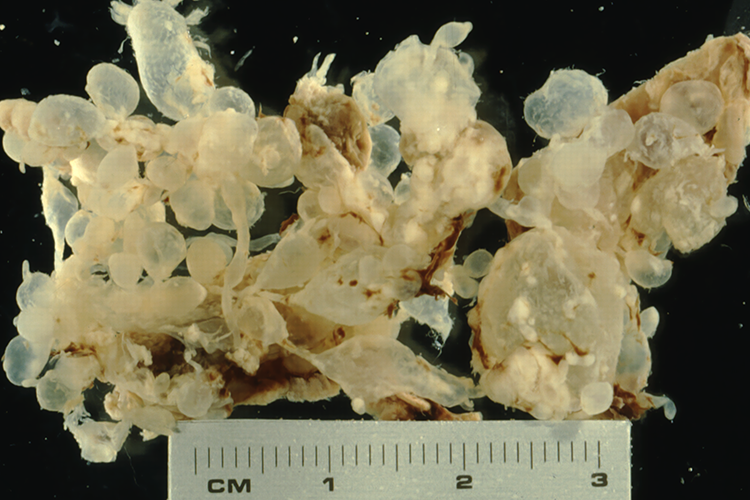
Complete hydatidiform mole. The uterine curettings immersed in water demonstrate uniform dilation of the chorionic villi.
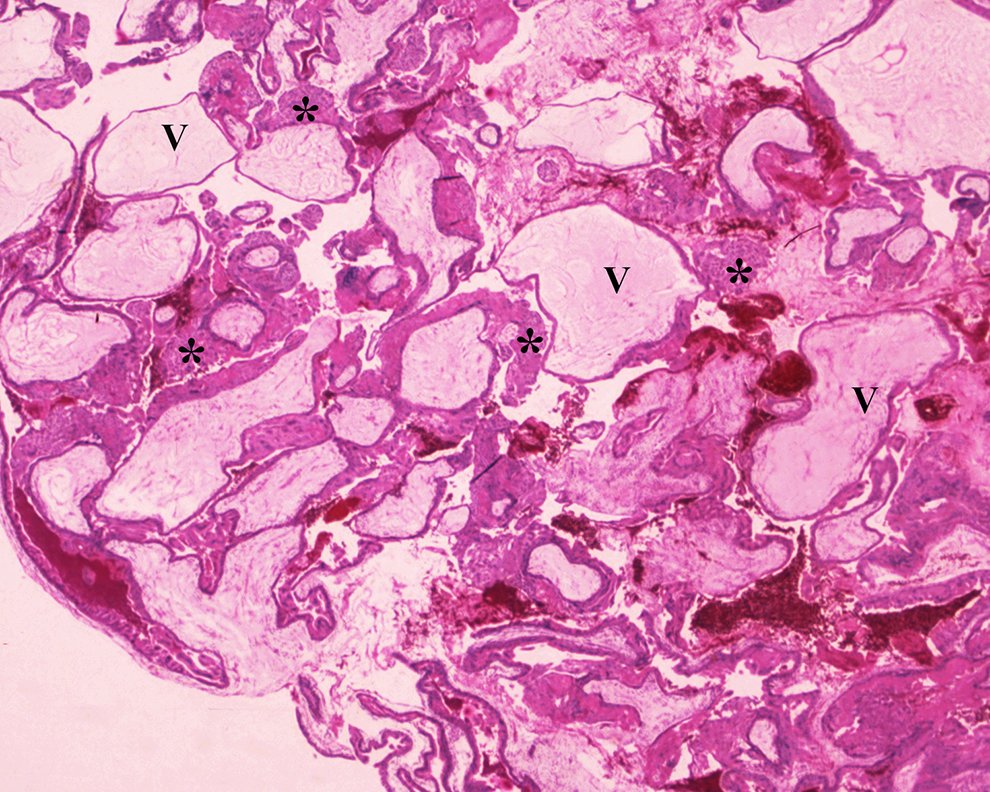
Complete hydatidiform mole. There is prominent trophoblast hyperplasia (*) composed of cytotrophoblast and syncytiotrophoblast circumferentially surrounding the chorionic villi (V). H&E, intermediate power.
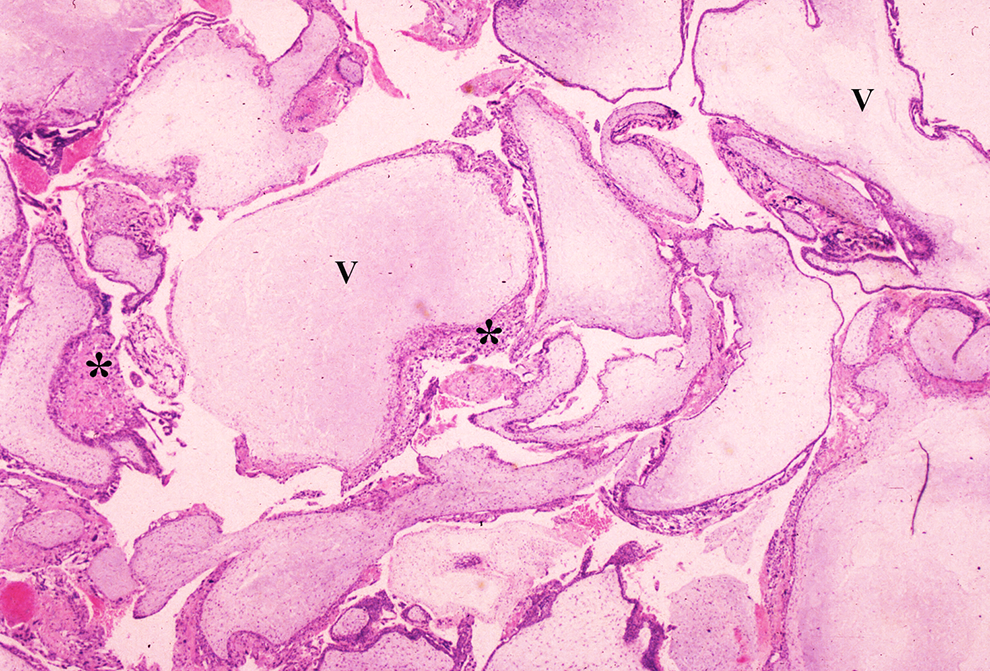
Complete hydatidiform mole. The chorionic villi (V) are uniformly dilated with prominent central cisterns and circumferential trophoblast hyperplasia (*). H&E, low power.
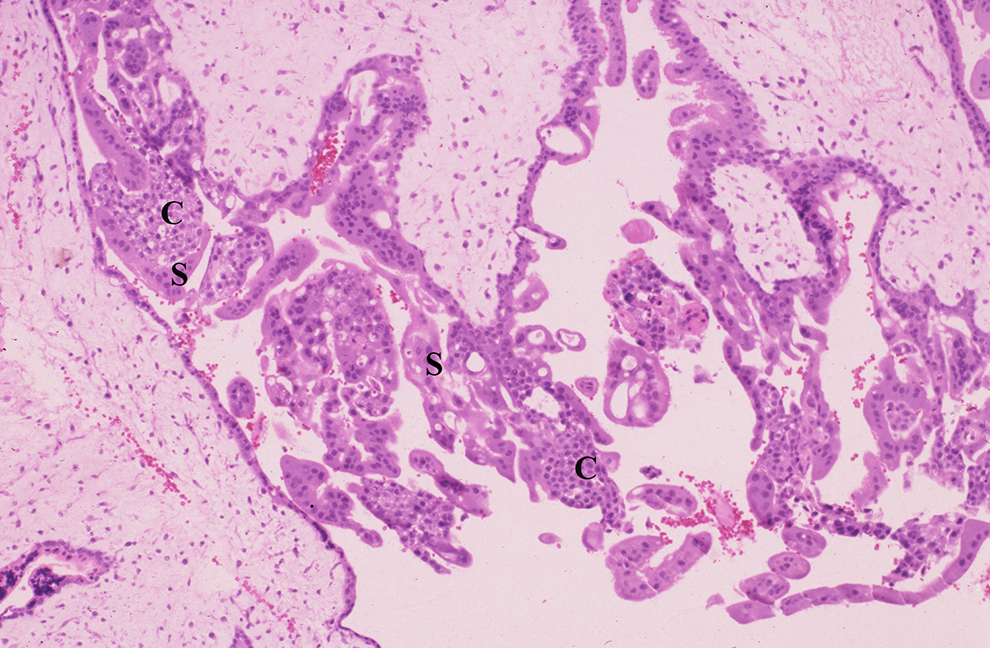
Complete hydatidiform mole. The trophoblast hyperplasia consists of cytotrophoblast (C) and syncytiotrophoblast (S). H&E, intermediate power.
The curettings (immersed in water) show uniform dilation of the chorionic villi on gross examination. Histological examination of the curettings shows uniform dilation of chorionic villi with cistern formation accompanied by marked trophoblast hyperplasia around the circumference of the chorionic villi. No fetal tissue is present (Figures 2 -5).
Questions/Discussion Points, Part 2
What Is the Diagnosis Based on the Pathologic Findings?
The gross and histological features are diagnostic of a complete hydatidiform mole (Figures 2 -5).
Describe the Gross and Microscopic Features of a Complete Molar Pregnancy
On gross appearance, the chorionic villi demonstrate uniform cystic dilation (giving the appearance of a cluster of grapes) that fill the uterine cavity 7 -9 (Figure 6). Microscopically, the chorionic villi are uniformly cystically dilated with trophoblast hyperplasia that surrounds the entire villous circumference (Figure 7). Cytological atypia and mitotic figures are present. Fetal tissue is absent.
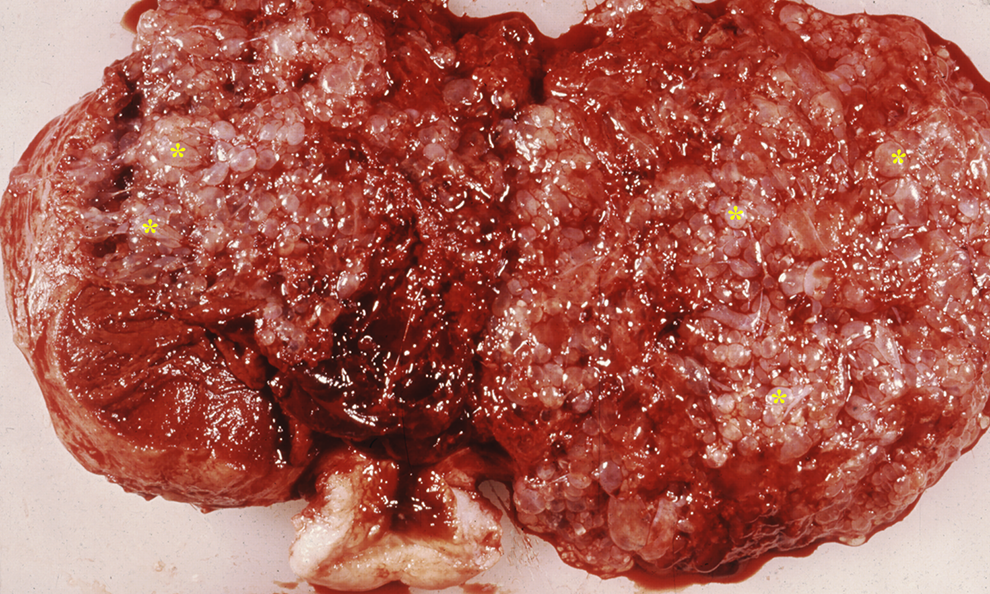
Complete hydatidiform mole. This hysterectomy specimen shows the uterine cavity filled with uniformly dilated chorionic villi (*). No fetal tissue is present.
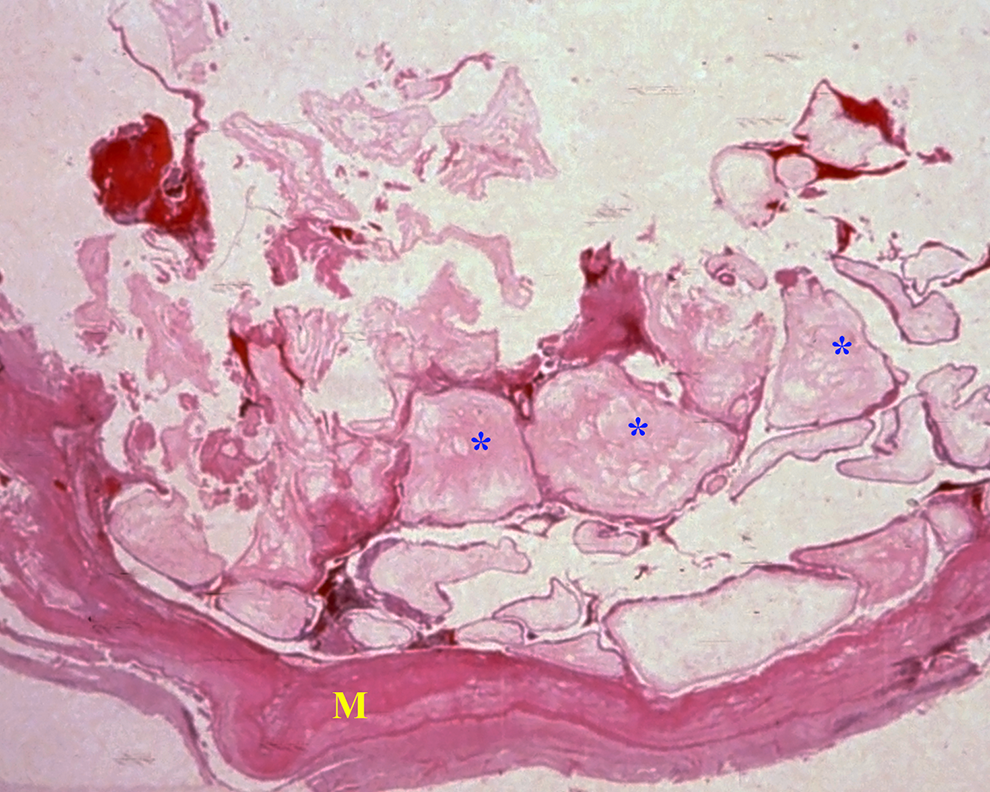
Complete hydatidiform mole. A section from a hysterectomy specimen shows uniform dilation of villi (*) attached to the myometrium (M). H&E, low power.
What Is the Pathogenesis of a Complete Molar Pregnancy?
A molar pregnancy arises from aberrant fertilization. In a complete mole, genetic material is completely supplied by the paternal chromosome, with either 2 spermatozoa or a diploid sperm fertilizing an empty ovum that lacks maternal chromosomes. In approximately 90% of cases, the fertilized ovum is 46, XX. 7,8,10 Morphologic studies of hysterectomy specimens provides evidence that hydatidiform moles arise from a transformation of the inner embryonic cell mass prior to differentiation into embryonic tissue. Without normal differentiation into the embryonic endoderm and ectoderm, the inner cell mass produces extraembryonic mesoderm and molar vesicles leading to the hydatidiform mole. 9
What Is a Partial Molar Pregnancy? Compare and Contrast the Pathological Findings of Partial Mole Versus Complete Mole (Table 1)
Comparison of the Clinicopathological Features of a Complete Versus Partial Mole.
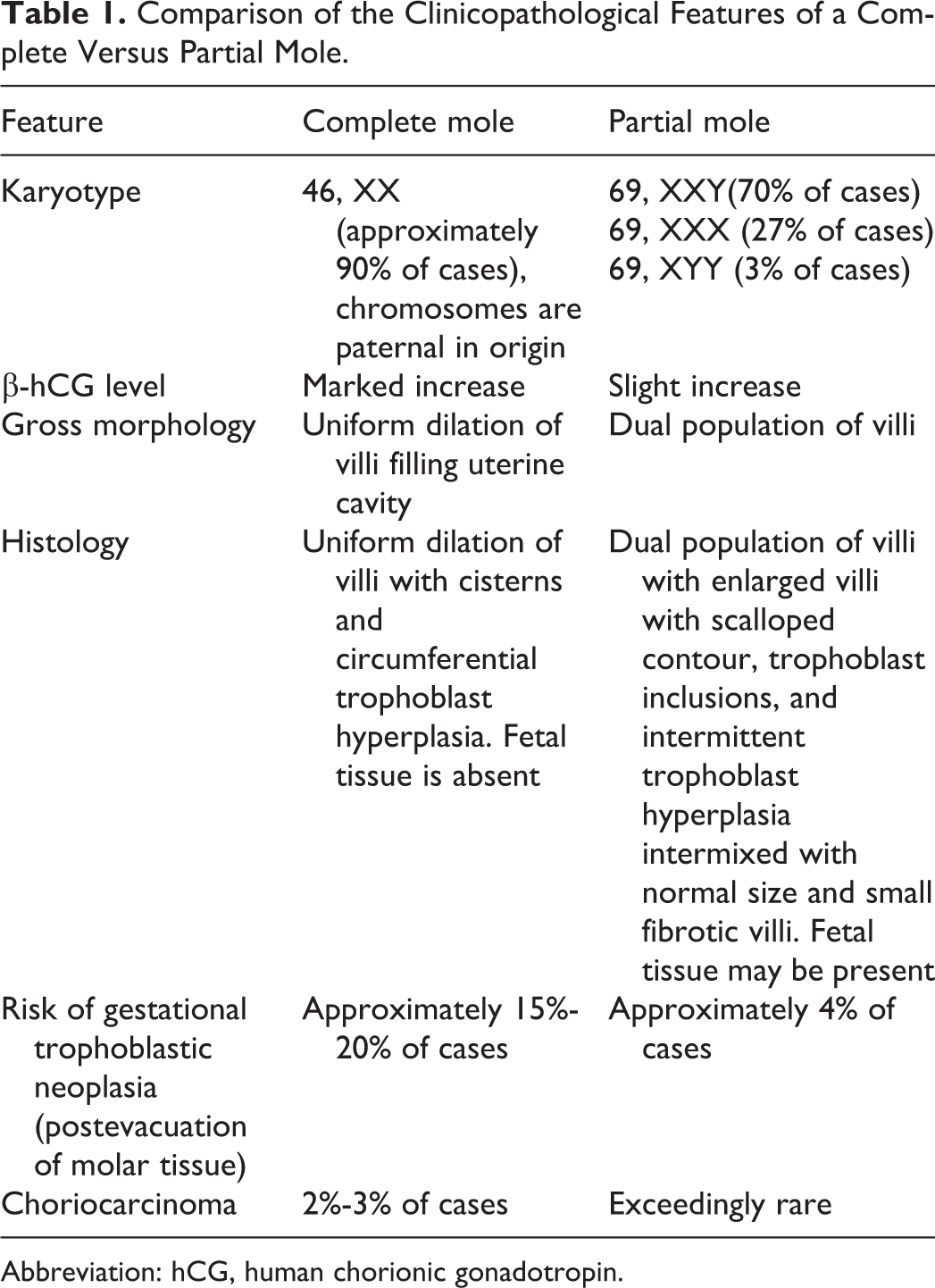
Abbreviation: hCG, human chorionic gonadotropin.
A partial mole is an abnormal pregnancy that has a triploid karyotype with rare exceptions, caused by fertilization of a 23X ovum with 2 haploid sperm or a duplicate sperm. The most common karyotype is 69, XXY (70%), followed by 69, XXX (27%) and 69, XYY (3%). 7,8
Complete moles have 3 classic histological findings: edema of the chorionic villi due to influx of water, avascular villi, and trophoblast proliferation surrounding the edematous villous circumference. Fetal tissue is absent 7 -9 (Figures 3 -7). Complete moles diagnosed early in gestation (less than 10 weeks gestation) demonstrate a different morphologic pattern.
In contrast, a partial mole has a dual population of villi with abnormal enlarged dilated villi with central cisterns intermixed with normal size and small fibrotic villi. The enlarged villi have irregular scalloped contours with trophoblastic inclusions. Trophoblast hyperplasia is intermittent and is not as prominent as seen in complete moles. Fetal tissue and chorionic villi containing capillaries with fetal erythrocytes may be seen 8 (Figures 8 and 9). p57 immunostaining can be utilized to distinguish a complete from a partial mole. 8,10
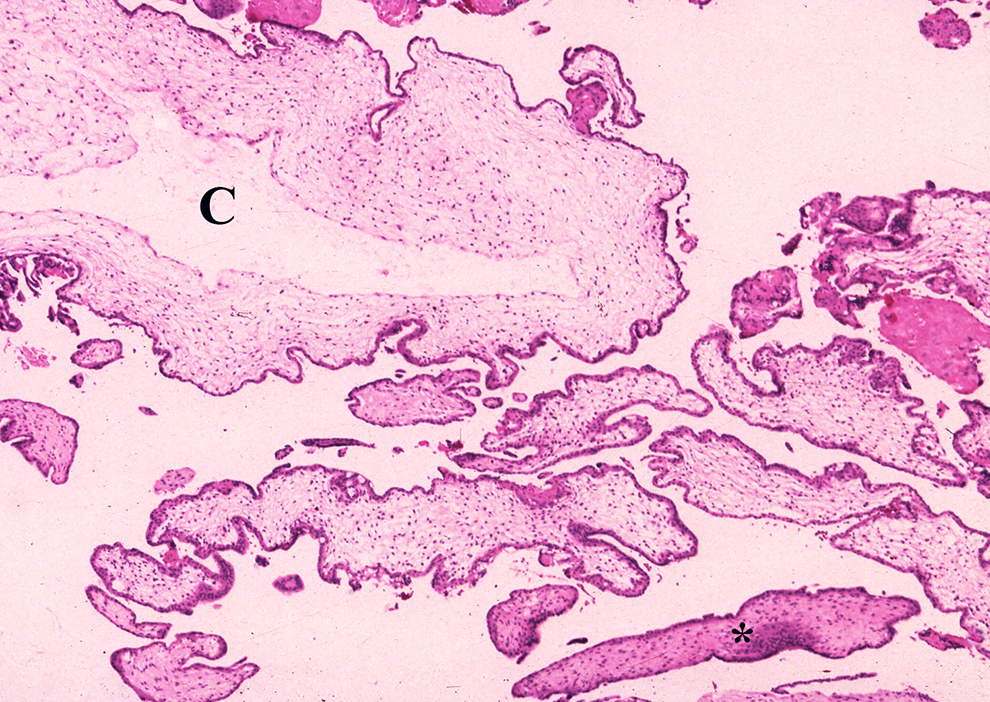
Partial hydatidiform mole. There is a dual population of chorionic villi. A large villus with cistern (C) is intermixed with more normal size and fibrotic villi (*). H&E, intermediate power.
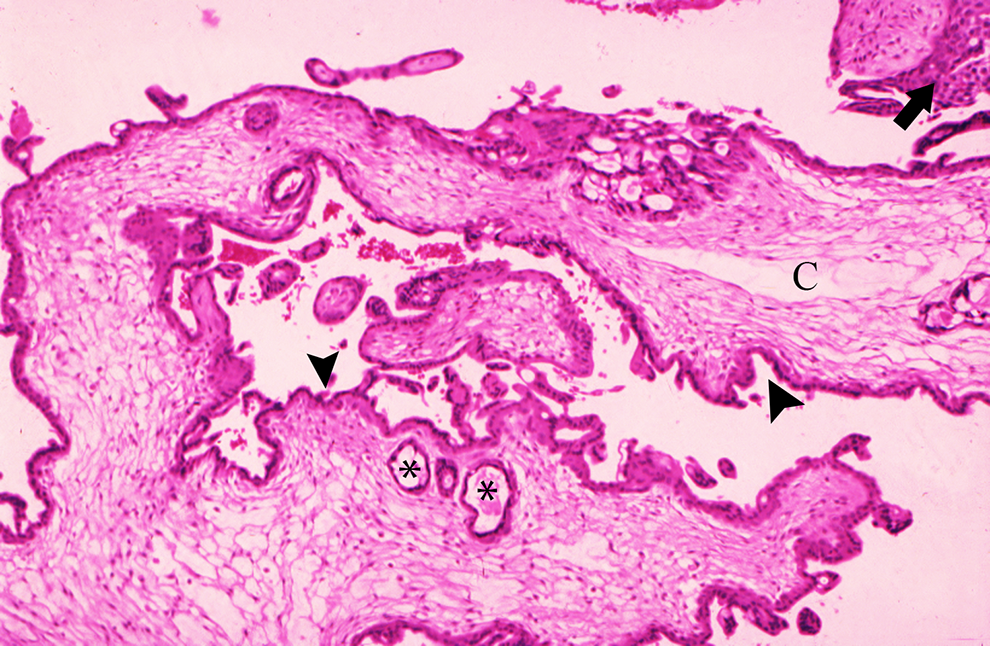
Partial hydatidiform mole. A large villus with scalloped contour (arrowheads), trophoblast inclusions (*), and cistern (C) is present. An adjacent villus with trophoblast hyperplasia is also seen (arrow). H&E, intermediate magnification.
Discuss the Epidemiology and Risk Factors Associated With Molar Pregnancy
The incidence of molar pregnancy in North America and Europe is approximately 1 per 1,000 pregnancies. 7,10 Higher incidences are noted in Asian, Latin American, and Middle Eastern countries; however, there is a wide variation in incidence in these locations. 8,10 Data suggest that a complete mole is significantly more common in Asian populations compared to white populations but less common in Hispanic and African American populations. 10
Several risk factors are associated with molar pregnancies. A history of prior molar pregnancy increases the risk of a repeat molar pregnancy to 1%, which is approximately 10 times the risk for the general population. 7,10,11 The risk of a complete mole is the highest at extremes of maternal age (<15 years and >35 years), and data suggest that ova from older women are more susceptible to abnormal fertilizations. The risk for a complete mole is twice as likely in women >35 years and 7 times as likely in women >40 years. The association with maternal age is mostly correlated with risk of complete molar pregnancy, while the risk of partial molar pregnancy varies very little with age. 10,12
What Are the Common Clinical Features of a Complete Molar Pregnancy?
Due to advances in ultrasonography and quantitative β-hCG measurements, complete molar pregnancies are often detected in the first trimester before the onset of symptoms. 13 If not detected early, the most common presenting symptom is abnormal vaginal bleeding, present in approximately 90% of cases, and is likely due to the separation of the molar villi from the decidua. Increased β-hCG levels inconsistent with the gestational age is also common. An uterine size greater than gestational age is a feature of late first trimester and early second trimester complete moles. 8,10,14 Severe vomiting, consistent with hyperemesis gravidarum, is an additional clinical feature that may be very severe leading to metabolic alkalosis and hospitalization. 10,14
Hyperthyroidism is a clinical feature that develops later in molar pregnancy related to prolonged exposure to elevated β-hCG levels. Due to earlier detection of molar pregnancies, it is not seen as often as in the past. Patients with clinical hyperthyroidism can present with tachycardia, warm skin, and tremors. These patients should be treated with a β-blocker and monitored during D&C as they can present with thyroid storm with the administration of anesthesia. Theca lutein cysts can also develop with prolonged exposure to elevated β-hCG levels and are usually detected on ultrasonography. Although preeclampsia in nonmolar pregnancies typically develops after 34 weeks’ gestation, clinical findings of preeclampsia during the first and early second trimester are suggestive for a molar pregnancy. 8,10,12,14
What Is the Treatment for a Molar Pregnancy?
Suction curettage (evacuation) should be performed in patients who wish to preserve fertility. Patients who do not wish to preserve fertility can undergo hysterectomy. 9,10,15 After evacuation, patients should have weekly β-hCG measurements until undetectable (3 consecutive negatives) and then monthly β-hCG levels for 6 months. Contraception is essential during this time as a new pregnancy would complicate measurement of declining β-hCG levels. 9,10,15
What Are the Complications of a Molar Pregnancy?
Persistent trophoblastic disease is a term used to define the presence of residual molar tissue after curettage. Plateauing or rising β-hCG titers after evacuation indicate persistent disease in women on contraception. Persistent disease is seen where the molar pregnancy was not completely removed or with the development of GTN. Gestational trophoblastic neoplasia may be seen in approximately 15% to 20% of patients after evacuation of a complete mole. Invasive moles comprise the majority of GTN cases after evacuation of a complete mole. 7,8,10,14
An invasive mole is characterized by molar villi that infiltrate into the myometrium, parametrial tissue and enter blood vessels leading to embolization to distant sites, for example, lungs. It occurs in approximately 15% of patients following evacuation of a complete hydatidiform mole and in up to 4% after evacuation of a partial mole. 14 Although benign, an invasive mole can penetrate the myometrium and cause intraperitoneal bleeding or vaginal hemorrhage. 7,8,10,14
Choriocarcinoma is a malignant trophoblastic neoplasm that has early vascular invasion and widespread dissemination, with the most common metastatic sites being the lungs (80%), vagina (30%), brain (10%), and liver (10%). 10 Choriocarcinoma arises in 1 in 20,000 to 30,000 pregnancies in the United States. 7 It can arise after any type of pregnancy, however approximately half of diagnosed choriocarcinomas arise from a complete hydatidiform mole, with 25% following a term pregnancy and 25% occurring after abortion. 8,9 Development of choriocarcinoma after diagnosis of a partial mole is rare. The uterus demonstrates a large hemorrhagic mass on gross examination (Figure 10). Histological examination demonstrates a biphasic trophoblast pattern consisting of syncytiotrophoblast and cytotrophoblast, with cytologic atypia, increased mitotic rate, and absence of chorionic villi (Figure 11). Development of choriocarcinoma is estimated to occur as a sequelae in 2% to 3% of complete moles.
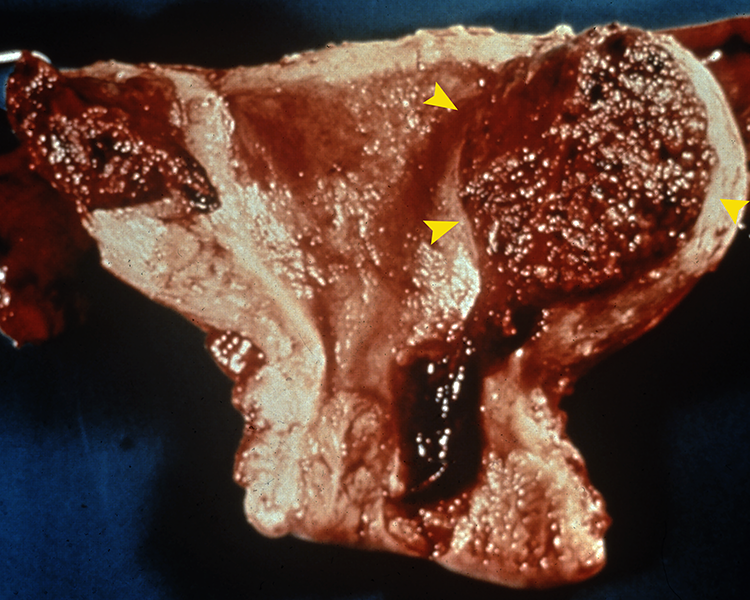
Choriocarcinoma. A hysterectomy specimen shows a large hemorrhagic mass in the uterine corpus (arrowheads).
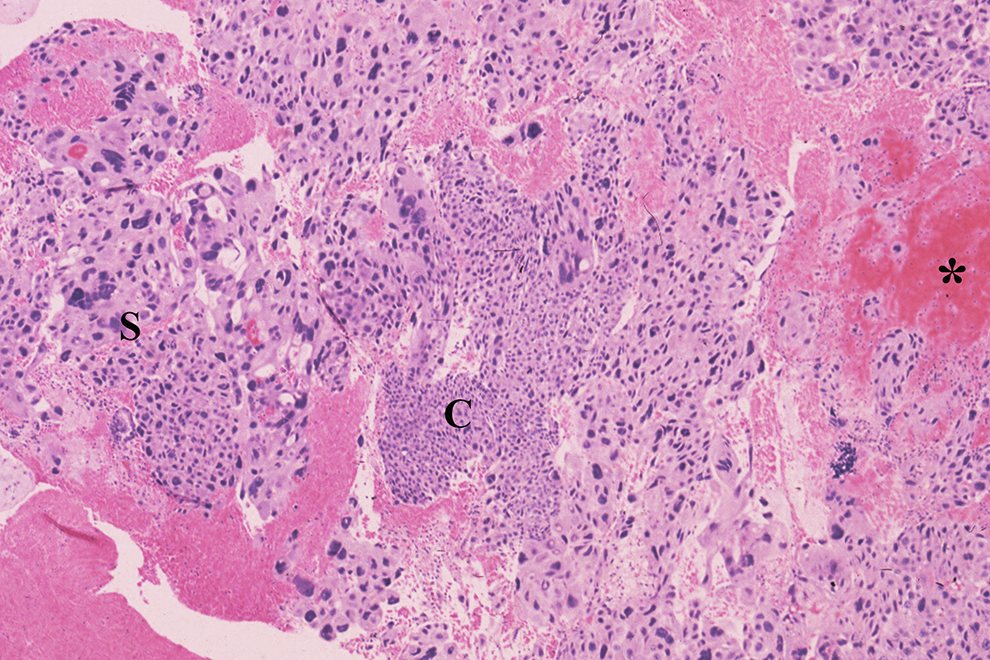
Choriocarcinoma. The classic biphasic pattern of syncytiotrophoblast (S) and cytotrophoblast (C) with cytological atypia and hemorrhage (*) is present. Chorionic villi are absent. H&E, intermediate power.
Describe the Staging and Prognostic Criteria for Molar Pregnancies
Molar pregnancies are currently staged using
Patients with GTN are treated with chemotherapy, and the treatment regimen is dependent on the FIGO staging system and the World Health Organization (WHO) prognostic scoring system, which takes into account 8 risk factors that predict the potential for resistance to single agent chemotherapy treatment. The FIGO staging system is anatomically based. Stage I is GTN confined to the uterus. Stage II is GTN that extends to the adnexa, vagina, or broad ligament but is still limited to the genital structures. Stage III is GTN extension to the lungs, with or without genital involvement. Stage IV is GTN that has spread to all other metastatic sites. The classification difference between stage III and IV was determined by reports that all brain metastases had a coexisting lung metastasis, indicating that GTN first spread to the lungs before further metastasizing. 15,16
The FIGO stage (I, II, III, IV) and the WHO prognostic score are then used in the determination of patient treatment. A risk score of 6 or less is considered low risk. A score greater than 6 predicts a high risk of resistance to single agent chemotherapy and may require combination chemotherapy. 15
Teaching Points
Molar pregnancies arise from aberrant fertilization. A complete mole is diploid, 46, XX (chromosomes of paternal origin) in approximately 90% of cases, while a partial mole is triploid and typically is 69, XXY (70% of cases), followed by 69, XXX (27%) and 69, XYY (3%).
A complete mole is significantly more common in Asian populations compared to white populations. They typically present with elevated β-hCG levels, uterus enlarged for gestational age, vaginal bleeding, and no evidence of a fetus on ultrasound.
A history of prior molar pregnancy and extremes of maternal age (<15 years and >35 years) are risk factors for a complete molar pregnancy.
On gross appearance, a complete mole has numerous fluid-filled villi with a grape-like appearance that fill an empty uterus.
There are 3 classic histological findings with a complete mole: edema of the chorionic villi, avascular villi, and trophoblast proliferation surrounding the villous circumference.
A partial mole has abnormal dilated villi intermixed with small fibrotic and normal size villi. Fetal tissue may be present. Chorionic villi may contain capillaries containing fetal erythrocytes.
Molar pregnancy is treated with suction curettage in patients who wish to preserve fertility and patients are monitored with weekly β-hCG measurements until undetectable.
Gestational trophoblastic neoplasia is a term that includes an invasive mole, choriocarcinoma, placental site trophoblastic tumor, and epithelioid trophoblastic tumor.
Gestational trophoblastic neoplasia occurs in approximately 15% to 20% of patients following evacuation of a complete hydatidiform mole.
Choriocarcinoma is a malignant trophoblastic neoplasm and has early vascular invasion and widespread dissemination, with the most common metastatic sites being the lungs (80%), vagina (30%), brain (10%), and liver (10%).
Approximately half of diagnosed choriocarcinomas arise from a complete hydatidiform mole, with 25% following a term pregnancy and 25% occurring after spontaneous abortion.
Based on the FIGO criteria, if the β-hCG levels remain elevated over the course of several weeks following the evacuation of a molar pregnancy, postmolar GTN is diagnosed.
International Federation of Gynecology and Obstetrics staging and the WHO prognostic score are used in patient management.
Footnotes
Authors’ Note
Figures 1 through ![]() were obtained during the scope of US government employment for Dr Conran.
were obtained during the scope of US government employment for Dr Conran.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
