Abstract
Thomas D. Kinney and Duke University started the first formal university-based training program for pathologists’ assistants in 1969. Over the next 2 years, 2 more university-based programs were established. All 3 programs were affiliated with nearby Veterans Administration Hospitals and were funded as a pilot study by the US Veterans Administration to address a looming shortage of pathologists. Early graduates of these programs discovered that the concept of pathologists’ assistants with well-defined skill sets encompassing both surgical and autopsy pathology was not initially accepted by important elements of organized pathology. Indeed, many academic pathologists were opposed to the concept from the outset. In the face of such opposition, a group of practicing pathologists’ assistants created and incorporated their own professional organization, the American Association of Pathologists’ Assistants, to provide support, advocacy, and continuing education for individual practicing pathologists’ assistants. The history of the American Association of Pathologists’ Assistants and its role in the establishment and success of the pathologists’ assistant profession are described utilizing personal communications as well as published historical sources.
Keywords
Introduction
The concept of university-trained pathologists’ assistants (PAs) as physician extenders for anatomical pathology was the brainchild of Thomas D. Kinney, MD (1909-1977) of Duke University. Dr Kinney witnessed the successful creation of the first physician assistant training program by a colleague at Duke University in 1965 and then started the first formal PA training program in 1969. 1,2 Although there were already a small number of informal hospital-based PA training programs in existence, Kinney believed these to be highly variable in quality. 3 With Kinney’s urging, grants from the “Pathology and Allied Science Service” of the Veterans Administration (VA) were instrumental in supporting the establishment of the first 3 formal university-based PA training programs at Duke University, the University of Alabama, and Quinnipiac College. 2,3
It is worthy of note that the American Medical Association (AMA) immediately championed the physician’s assistant concept. They brought to bear considerable resources to establish an accreditation process for training programs, as well as certification and licensing processes for individuals. They even mounted an intense public relations campaign to market the new profession. 4 The same cannot be said however, for the PA concept, which was not well accepted by the medical community or by important elements of organized pathology. It was, therefore, left to a small number of practicing PAs in the workforce to fend for themselves in their efforts to organize and achieve recognition within the medical community.
Historical Obstacles to Overcome: Hurdles to Clear
Two major organized pathology groups, the College of American Pathologists (CAP) and the American Society of Clinical Pathologists (NB, the organization later changed its name to American Society for Clinical Pathology [ASCP]), resisted the PA concept from the beginning. The absence of support by the ASCP might at first seem surprising because its leadership had immediately embraced overseeing the training, examining, and certification of technologists performing clinical pathology laboratory testing. 5 However, the nature of anatomical pathology seemed fundamentally different to many practicing pathologists and the ASCP. Because of this, many pathologists were uncomfortable with the idea that PAs were being trained to perform tasks that, up until this time, had been performed exclusively by pathologists or pathology residents. 2,6,7 However, the highly protective stance that only physicians could perform anatomical pathology tasks is perhaps less surprising when one remembers the critical importance this work played in establishing their own profession in the 1920s. 8,9 It should also be remembered that the ASCP was established in 1922 because hospital-based clinical laboratories were rapidly losing ground to “mail order” commercial laboratories and were, according to ASCP founders, 5,10 believed to be well on their way to extinction. It was the ASCP leadership’s astute recognition that the leadership of the American College of Surgeons (ACS), a powerful group of surgeons attempting to standardize hospitals, did not really care where clinical pathology testing was performed but desperately wanted easy access to surgical pathology, intraoperative frozen sections, and autopsy pathology, none of which could be adequately provided by non-hospital-based commercial laboratories. Therefore, the leadership of these 2 organizations worked together to make hospital-based surgical pathology, autopsies, and clinical pathology integral parts of the ACS Minimum Standards for Hospitals, the predecessor of current-day Joint Commission hospital accreditation, by 1926. 8,9,11 Since it seemed improper to charge patients for surgical pathology or families for autopsies, the lucrative clinical pathology work (ie, high-volume work often performed by technologists under the supervision of pathologists) was used to subsidize these important quality assurance measures and the non-hospital-based commercial laboratory business model immediately became nonviable. 9
By the late 1920s, the ASCP was heavily involved in the training and certification of clinical pathology technologists to assist pathologists. However, it was decided at that time that anatomical pathology work could only be performed by physicians, a stance that was never questioned until the late 1960s, when autopsy workload became overwhelming (see below).
It is likely that for these historical reasons that elements of organized pathology did not readily embrace the concept of PAs. It should be noted that the narrative of early opposition to the PA profession by ASCP and CAP presented in the current paper is built upon records in the American Association of Pathologists’ Assistants (AAPA) archives and interviews with AAPA founders. Hence, although our article likely has some inherent bias, we hope robust peer-review and the provision of additional historical context have helped address this.
Events Leading up to the Formation of the American Association of Pathologists’ Assistants
As the 3 university-based formal PA training programs were being established, little information was available to the medical community about the rigorous training provided. Early graduates adopted the designation “PA-C” to highlight their university degree. 12 Several early Duke graduates observed that their status as professionals was accepted primarily by a few pathologists who were already familiar with the Duke PA program. In fact, early graduates were often hired by pathologists they knew from their training institution who were starting new positions elsewhere. For instance, PAs Coy W. Wagoner and Rob Heineman were recruited to the University of Kentucky: Wagoner by Jacinto J. Vasquez, MD, and Heineman by Joseph C. Parker Jr, MD, who were pathologists they knew from Duke [oral personal communication, Coy W. Wagoner, BS, PA(ASCP)CM December 2019]. Making their way into the workforce in the early 1970s, these graduates encountered other laboratory personnel calling themselves PAs who, without formal training, were working for individual pathologists or hospital pathology groups. The existence of these on-the-job-trained (OJT) PAs complicated matters for early university-trained PAs (see below) and precipitated an identity crisis. 12 However, in actuality, their job descriptions were very different. According to the remaining “founding fathers” of the PA profession in the United States (Wagoner, Heineman, and Norm Gerard), most OJTs in the early 1970s were “dieners, laboratory assistants, and morticians” (see below) who worked exclusively in the autopsy suite; those with any surgical pathology duties handled only small biopsies and not large or complex specimens. Therefore, the real overlap in these early days was the common use of the name “pathologists’ assistant”, which the university-trained PAs felt should be reserved for highly trained PAs practicing the full scope of the new profession.
In 1971, a small group of practicing university-trained PAs, seeking to organize themselves and to advance their newly emerging health profession, sought membership in the American Association (later renamed Academy) of Physician’s Assistants [oral personal communication, Coy W. Wagoner, BS, PA(ASCP)CM December 2019]. The physician’s assistant group, however, denied the request without explanation. A follow-up conversation with a member of their leadership provided the following explanations: (1) PAs are not clinically trained (and therefore are not a good fit), (2) PAs are too few in number, and (3) PA physician support should come from organized pathology rather than the AMA. Therefore, the first 5 graduates of the Duke University PA training program held a series of meetings in the fall of 1971 to address the potential for creating an organization of and for PAs. The original formative meeting was held at Duke University in September 1971. Representative PAs from the 2 other early PA training programs were invited. The purpose of the meeting was to discuss differences in curricula with an eye to creating uniformity among the programs and to assess interest in the idea of creating a formal organization. Although the second topic was discussed at length, the other 2 programs, given the opportunity to either agree or disagree, were noncommital. Additional meetings that fall led to the decision to arrange a formal planning meeting to take the ultimate step, establishing our own organization [oral personal communication, Robert E. Heineman, PA(ASCP)CM January 2020].
The formal planning meeting was held in February 1972 at the University of Kentucky Medical Center in Lexington, Kentucky. Present were Coy Wagoner and Norman Gerard, graduates of the inaugural class of the Duke University program, as well as Harvey Gibson, Robert Heineman, and John McNamee who graduated the following year. Their goal was to form a nonprofit organization to foster the education of PAs at recognized medical centers and universities across the country.
The meeting provided a forum for discussions to determine the major goals, governance structure, legal status, and other requirements necessary to create a nonprofit organization. Harvey Gibson, who was working in the Dayton, Ohio area, had engaged an attorney there and brought information on incorporation requirements and application materials with him to the meeting. In accordance with the requirements, the 5 wrote goals, defined officers and terms, and created articles of incorporation. Harvey took the application back with him, and his attorney subsequently filed it in Dayton, Ohio. By consensus, the primary objective of the organization was to establish an identity for certified, university-trained PAs that would clearly set them apart from any other informally trained or OJT laboratory personnel working as PAs and identifying themselves as certified.
The funding for the effort was shared equally by those present. The meeting proved to be the spark that ignited the creation of the organization that adopted the name of the “American Association of Pathologists’ Assistants.” The group identified the major goals of the Association, and each of the principals were given specific assignments in an organized pursuit of those goals [oral personal communication, Norman F. Gerard, PA(ASCP)CM December 2019].
Harvey Gibson and his lawyer finalized the incorporation paperwork. Norman Gerard (University of Kentucky) and Robert Heineman (University of Kentucky) together created and edited an Association Newsletter for distribution to its members as well as prospective members. Heineman also organized the effort to create guidelines for training programs and developed a continuing education (CE) program for AAPA members and an AAPA “fellowship” examination for potential members. Coy Wagoner (University of Kentucky) contacted all states’ attorneys’ general to ascertain if there were any existing state statutes that would either allow or prevent PAs to perform their duties.
Creation of the American Association of Pathologists’ Assistants
The AAPA was officially incorporated in the city of Dayton, Ohio, on April 14, 1972, under the statutes of the state of Ohio as a nonprofit organization. The first officers/trustees of the AAPA signed “Articles of Incorporation.” 13 The 5 trustees/officers/founding fathers of the corporation were president: Harvey L. Gibson; first vice president: Norman F. Gerard; second vice president: Coy W. Wagoner; third vice president: Robert P. Heineman; and secretary/treasurer: John R. McNamee.
Of the 5 founding fathers, 2 went on to pursue other disciplines. Harvey Gibson and John McNamee both worked as teaching assistants to Kenneth A. Broda, PhD (born 1941), Director of the Duke University PA Program, but left the profession within a few years. The 3 remaining founding fathers all forged lengthy careers as PAs (Figure 1). Norm Gerard worked for over 40 years as a PA, 23 years of which were spent at the University of Wisconsin Unitypoint Health Center in Madison, Wisconsin. Coy Wagoner spent nearly 50 years as a PA at a variety of medical centers and community hospitals. Rob Heineman also worked as a teaching assistant to Dr Broda at Duke University for a short time and had a 40 plus year career as a PA, predominantly at the University of Minnesota Medical Center in Minneapolis, Minnesota.
It is noteworthy that the AAPA will celebrate its 50th anniversary in 2022.

Three of the AAPA “founding fathers”: Norm Gerard, Coy Wagoner, and Rob Heineman in 2010. The photograph was taken at the 36th annual meeting of the AAPA in Indianapolis, Indiana. AAPA indicates American Association of Pathologists’ Assistants. Credit: AAPA Archives.
American Association of Pathologists’ Assistants Governance: Code of Regulations
From the beginning, the AAPA was dedicated to advocating for individual PAs and to advancing their newly emerging allied health profession. The AAPA’s early major goals were to create guidelines for training programs (see below), develop a de facto certification/membership examination, provide CE for its members, and obtain national recognition for individual PAs and for the profession. The first official document defining the AAPA’s activities and governance, the “AAPA Code of Regulations,” was created in December 1972. Recognizing that there were informally trained or OJT PAs in the workforce, the AAPA debated and then took an inclusive stance, offering them a path to membership. 12 A provisional clause was included in the Code of Regulations stipulating that such individuals could become AAPA members if, after examination by the Association’s Membership Committee, they were found to be qualified in accordance with criteria established by the Association.
American Association of Pathologists’ Assistants Membership and the Fellowship Examination
The first annual meeting of the AAPA was held in the fall of 1975 in Atlanta, Georgia. According to John Mitchell, a University of Alabama PA Program graduate who was elected president at that meeting, “while it was primarily a business/organizational meeting, there were very heated discussions regarding formally trained versus OJT members [oral personal communication, John E. Mitchell, MSBA, PA(ASCP)CM November 2019].” The AAPA fellows present ultimately decided to offer an internal “fellowship” examination. Those OJTs who were qualified to take the examination (based on a minimum of 2 years of surgical pathology and autopsy experience and recommendation of a pathologist) and who passed became “fellow” member. Those who failed the examination or who were not qualified to take it (ie, students and OJTs without sufficient qualifying experience) were offered “affiliate” membership (not included in Table 1). Membership privileges and responsibilities for fellow members were greater than for affiliate members.
American Association of Pathologists’ Assistant Membership Numbers (1972-2020).
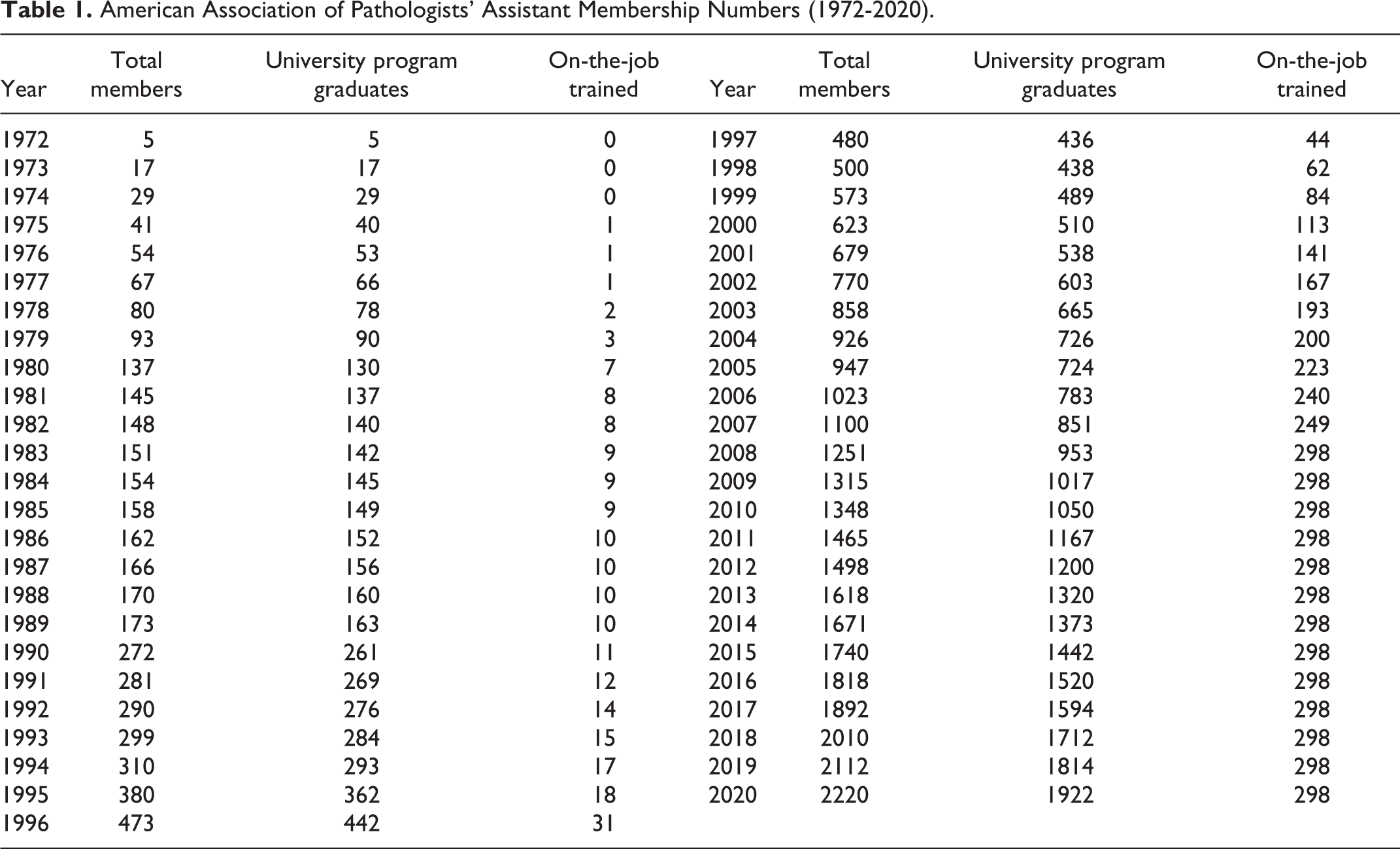
The OJT membership issue would prove to be complex and contentious for many years. On one hand, many fellow members held the view that AAPA membership should be limited to university-based training program graduates who passed the fellowship examination. On the other hand, AAPA leadership recognized that there were OJTs in the workforce and that offering them a membership category and a path to fellow membership would serve to legitimize their place in the profession and would boost membership numbers. While initially there were very few OJTs practicing the surgical pathology component of the profession who were eligible to write the fellowship examination, this pool increased over the next few decades, often with their OJT training provided by university-trained PAs. The OJT issue would be revisited over the years, coming to a head in the late 1990s when national certification for PAs loomed on the horizon; the membership voted and formally approved the inclusive approach in accepting the ASCP board of registry’s (BOR) proposal in 2005 (see below).
The first “fellowship” examination was administered at the second annual AAPA meeting in Virginia Beach, Virginia, in October 1976, only a few years after its incorporation. It took much of that interval for the few AAPA members to create an examination database and organize offering the examination. It was devised as a means to offer OJTs a way to attain equal status with university-trained PAs, as both were required to pass the examination. The fellowship examination was improved year by year and sufficed until the national certification examination was available (see below).
Although AAPA leadership offered OJT membership based upon passing the fellowship examination, not many OJT chose this route early in the history of the organization; as given in Table 1, OJTs represented only about 5% of the membership for the first half of the AAPA’s existence. However, for those OJTs who were granted membership by passing the fellowship examination, their status was the same as university-trained PAs who had passed the fellowship examination. The reason for the initial low uptake is likely the variability of the educational and work experiences of the OJTs. It is the recollection of the 3 remaining founding fathers that most OJTs were initially autopsy assistants with little or no exposure to surgical pathology and who would therefore be ineligible. However, OJT PAs after this often received both surgical pathology and autopsy training. After 1995, the OJT membership increased precipitously. While OJT membership represented only 4.7% in 1995, it represented 20% in 2001 and peaked at 23% in 2008. The percentage has declined since that time as the door was permanently closed in 2008 (see below).
In a related matter, many members felt that all training programs should be master’s programs. James Lewis, a Duke graduate and AAPA treasurer in 1975, was among many who were adamant about requiring a masters. He says he clashed with some AAPA members in leadership roles because “I was hawkish on requiring a masters and eliminating OJT and Affiliate AAPA membership [oral personal communication, James Lewis, PhD, PA(ASCP)CM November 2019].” Lewis went on to earn his PhD and would become director of the Duke PA program when it became a master’s program in 1994. It should be noted here that several PA training programs began as either certificate programs or bachelor’s degrees, all eventually became master’s degree programs. 2 The last program to convert was Wayne State University in 2014.
One positive outcome of the 1975 annual meeting was that the AAPA fellow members present were able to agree on an acceptable definition of a PA: “A pathologists’ assistant is a professional person qualified by academic and practical training in anatomic pathology to provide patient service under the supervision and direction of a licensed pathologist who is responsible for the performance of the assistant.” That definition would be minimally amended based on discussions between the AAPA, Intersociety Pathology Council (IPC), and Association of Pathology Chairs (APC) at a meeting in September 1976 (see below).
The AAPA definition of a PA was issued as a news release in the CAP monthly magazine
The definition adopted by founding convention is of interest. The concept of the pathologists’ assistant has proven so controversial that the CAP and ASCP have taken an official hands-off stance, although Pathologist has carried numerous articles and letters on the topic. Regardless of your own attitude, it’s refreshing to see someone working in the laboratory field define themselves in the fashion the AAPA has done. Only time and the course of future AAPA/CAP relationships will tell whether the auspicious beginning will endure.
14
Continuing Education
In their efforts to gain recognition and sponsorship from a national medical association, members of the AAPA board of trustees (BOT) foresaw the desirability and necessity of establishing a membership/certification examination and implementing the means of continual advancement in knowledge and professional skills for AAPA members. A CE program was established in 1976 during the second annual meeting, requiring members to attain a minimum of 25 to 30 hours of AAPA accepted structured educational experiences per year. The AAPA Newsletter offered the first CE article in March 1977, and the June 1977 issue offered an instructional packet outlining the steps to produce self-instructional audiovisual training programs. In the early 1990s, CE requirements were increased to 45 credits per year. Members who met that requirement were presented CE certificates. However, since the AAPA was still a small organization with only an internal examination and CE program, it was initially difficult to find a professional organization to validate its CE. In 2000, the AAPA, largely through the efforts of BOT member W. Rae Rader, became an approved
Early Support From 2 Pathology Organizations
Despite early opposition by the AMA, CAP, and ASCP, 2 pathology organizations were supportive. The IPC and the APC were willing to work with the AAPA to address national certification and other issues that would affect the future of the organization and the profession. The IPC and APC, recognizing the growing shortage of pathologists and the need for more qualified PAs, created an ad hoc committee on PAs and contacted the AAPA requesting to meet with its officers [oral personal communication, Norm Gerard, PA(ASCP)CM November 2019]. On September 15, 1976, AAPA trustees/officers and the ad hoc committee, members of which included Thomas D. Kinney, MD, Marjorie Williams (-Jensen), MD (1925-2013), William D. Dolan, MD (c1913-1999), and Fairfield Goodale, MD (1923-2015), met at the VA Central Office in Washington, DC.
Dr Goodale opened the meeting by extending official IPC congratulations to the founding and current AAPA officers for creating the Association. The IPC also expressed an interest in gaining statistical information about practicing PAs and on the ideals and goals of the Association. Dr Kinney who, as chair of pathology at Duke, had established the first training program noted that the main goals of the AAPA should be the creation of criteria for approved training programs, the development of new training programs, and the creation of a certification examination at a national level. He also suggested that the APC would be the most suitable organization for supporting the AAPA.
15
One of the outcomes of the meeting was that a formal definition of a PA was agreed upon. Based upon the recommendations of Drs Kinney and Goodale, the amended definition read as follows: “A
Another conference dealing with the need for and the training of PAs, “The Future of Academic Pathology” was held at the University of Maryland on September 22 to 24, 1976. It was sponsored by the Universities Associated for Research and Education in Pathology, the Intersociety for Research Potential in Pathology, and the APC. A panel discussion was held on “Technical Training of Assistants to Pathologists.” The panel’s conclusion was that there was a continuing and growing need for qualified PAs from standardized degree programs. The panel recommended that either the IPC or the APC be asked to take the leadership role in the organization of a “Commission on Pathologists Assistants,” which would address the issues of educational standards, program accreditation, certification, and funding. 15 Unfortunately, PA training program founder and champion Thomas Kinney died in June 1977, and so his powerful positive influence was lost, which likely slowed progress and neither organization took a leadership role.
National Recognition
The overarching goal of the newly incorporated AAPA was to obtain national recognition for the newly emerging profession and for individual PAs. Other major goals in the pursuit of national recognition were to create guidelines for formal training programs, develop a de facto certification examination that would also establish AAPA fellow membership status, and develop a CE program for its members.
Realizing that until it could be sponsored by a national pathology organization, the AAPA would necessarily be responsible for internally accrediting existing and future training programs. It formed a committee in 1976 to establish such criteria and identify ways to facilitate training program development (see below). The resulting criteria and guidelines for accreditation were refined over a period of years, and in 1983, the Association of Pathologists’ Assistant Training Programs (APATP) was incorporated. Its first president was Kenneth Broda, PhD, director of the Duke University PA program. One of the first accomplishments of the APATP was to develop and publish the “Minimum Essentials for Pathologists’ Assistants Training Programs,” necessary for future accreditation. 16
At the 1977 annual AAPA meeting, a consensus of fellows present recommended that the AAPA again pursue an affiliation with the American Academy of Physician’s Assistants, seeking strength in numbers. The Academy, however, once again rebuffed the AAPA’s overture, providing the same reasons as earlier. 17
In 1978, the AAPA submitted a formal request to the ASCP asking them to consider offering a PA registry. The ASCP/BOR responded by establishing an ad hoc committee to explore the possibility. The AAPA President Leo J. Kelly reported in the December 1979 AAPA Newsletter that
At CAP/ASCP’s suggestion, we are following established channels for national recognition of PAs. The first step involves recognition as a newly emerging health profession. This is accomplished through the AMA’s Council on Allied Health Education and Accreditation. PA certification would occur through the ASCP/BOR or possibly through the National Commission on Certification of Physician’s Assistants.
18
In 1980, the AAPA BOT submitted its first official application to the AMA for national recognition as a “Newly Emerging Allied Health Profession.” 19 The AMA denied the application, citing small membership numbers (137 at that time) and inadequate financial strength as major liabilities.
The AAPA leadership continued to focus its energy on seeking sponsorship from major pathology organizations and on its pursuit of national recognition. In November 1987, the AAPA BOT communicated with the AMA board of directors, again requesting recognition as a newly emerging health profession. The board of directors informed them that without the support of a national organization of physicians representing the AAPA’s subspecialty, they would not approve an application.
During the decade plus since its incorporation, the number of active programs grew (Table 2), as did the AAPA membership (Table 1). The AAPA, however, still found it difficult to make significant strides toward achieving national recognition. The AAPA leadership recognized the need to effectively spread the word about the value of PAs among anatomic pathologists and so they initiated a “grassroots” effort, asking individual AAPA members to reach out to their pathologists, asking them to share their positive experiences working with PAs with their peers.
University-Based Pathologists’ Assistant Training Programs (1969 to Present).
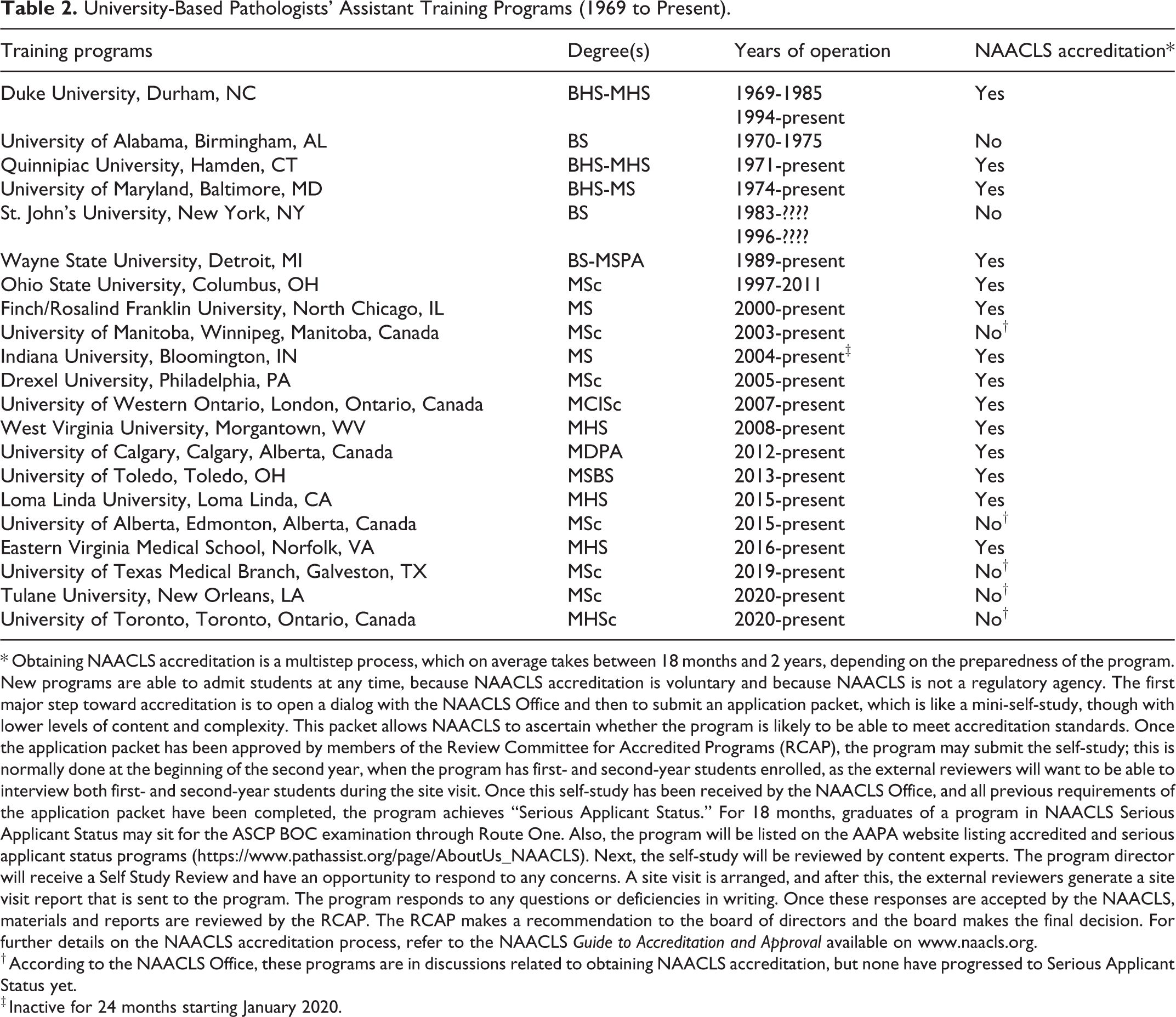
* Obtaining NAACLS accreditation is a multistep process, which on average takes between 18 months and 2 years, depending on the preparedness of the program. New programs are able to admit students at any time, because NAACLS accreditation is voluntary and because NAACLS is not a regulatory agency. The first major step toward accreditation is to open a dialog with the NAACLS Office and then to submit an application packet, which is like a mini-self-study, though with lower levels of content and complexity. This packet allows NAACLS to ascertain whether the program is likely to be able to meet accreditation standards. Once the application packet has been approved by members of the Review Committee for Accredited Programs (RCAP), the program may submit the self-study; this is normally done at the beginning of the second year, when the program has first- and second-year students enrolled, as the external reviewers will want to be able to interview both first- and second-year students during the site visit. Once this self-study has been received by the NAACLS Office, and all previous requirements of the application packet have been completed, the program achieves “Serious Applicant Status.” For 18 months, graduates of a program in NAACLS Serious Applicant Status may sit for the ASCP BOC examination through Route One. Also, the program will be listed on the AAPA website listing accredited and serious applicant status programs (https://www.pathassist.org/page/AboutUs_NAACLS). Next, the self-study will be reviewed by content experts. The program director will receive a Self Study Review and have an opportunity to respond to any concerns. A site visit is arranged, and after this, the external reviewers generate a site visit report that is sent to the program. The program responds to any questions or deficiencies in writing. Once these responses are accepted by the NAACLS, materials and reports are reviewed by the RCAP. The RCAP makes a recommendation to the board of directors and the board makes the final decision. For further details on the NAACLS accreditation process, refer to the NAACLS
† According to the NAACLS Office, these programs are in discussions related to obtaining NAACLS accreditation, but none have progressed to Serious Applicant Status yet.
‡ Inactive for 24 months starting January 2020.
The AAPA reached out to national organizations to gain support for achieving their goal of national recognition. Two such organizations were the American Society of Allied Health Professionals (ASAHP) and the International Academy of Pathology (IAP). In 1988, Jeff Watterson, then AAPA president, was invited to speak with the ASAHP board of directors at their annual conference. The ASAHP reconsidered however, and cancelled it, telling the AAPA that they did not feel that a meeting between the 2 would convince them to offer their support. 20 Initial contact with the IAP was made by the AAPA Public Relations Chair Ann Walsh-Feeks in 1987. The dialogue led to the AAPA being given complimentary exhibit space at the US and Canadian Academy of Pathology meeting in Washington, DC, in 1988. This offer continued thereafter. In 2004, IAP President Robin Cooke, MD, began discussions with the AAPA about expanding the utilization of PAs internationally. Members of the AAPA BOT gave a formal presentation about the AAPA and the PA profession at the IAP Congress in Brisbane, Australia, in 2004 and the IAP Congress in Athens, Greece, in 2008.
Continuing its proactive professional outreach program, the AAPA BOT submitted to the executive director of CAP in March 1988 a packet of information containing a formal request for their support of the AAPA’s second application to the AMA for recognition as a newly emerging allied health profession. The packet and request were presented to the CAP board of governors in June 1988. The request was denied by a vote of the board of governors, who cited in part a lack of unanimity among individual pathologists as to the appropriateness of nonphysicians performing tasks that they considered to be within the purview of pathologists alone. 21
In 1991, the AAPA BOT created an ad hoc committee on national recognition. The committee was charged with following the activities of CAP and ASCP with respect to the issue of PAs. The AAPA President Ann Walsh-Feeks attended the 1991 fall ASCP/CAP meeting in Dallas, Texas, where the issue of manpower shortage in pathology was discussed at length (NB, the term manpower, although sexist and unacceptable now, is historically correct and was the terminology used throughout most of the 20th century). Walsh-Feeks reported that projections showed that there would only be enough pathologists to fill 39% to 45% positions vacated in the next 5 years. She also reported that, while many pathologists at the meeting felt that PAs could have a positive impact in the setting of manpower shortages, they also voiced a concern that there were not enough PA training programs to produce adequate numbers of PAs to fill even the available positions. 22
In continuing to strive for national recognition, AAPA leadership realized the value and importance of maintaining relationships with peer and parent organizations and maintaining open communications with key figures in CAP, ASCP, and IAP. In 1996, the National Association of Medical Examiners contacted the AAPA regarding the utilization of PAs in forensic pathology. The AAPA provided them with information regarding the PA profession but nothing further came of it. 23 In all likelihood, the PA’s surgical pathology skills resulted in overqualification and the required autopsy skills could be acquired more economically. Nevertheless, some AAPA members have assisted medical examiners since the early years of the organization.
Relationships were also forged with the Association of Directors of Anatomic and Surgical Pathology (ADASP). The AAPA’s efforts to attain national recognition continued to be followed with much interest by pathology organizations. In trying to gain a better understanding of the utilization of PAs, Mark Wick, MD, on behalf of the ADASP and in conjunction with the Resident Physician Section of the ASCP, surveyed their pathology training program liaisons. 24 This survey was sent to 153 ASCP-Resident Physician Section liaisons with a 56% response rate. The 1997 survey results revealed that PAs functioned in a variety of capacities varying from program to program and that residents generally had a positive view of PAs. On the impact of PAs on the future practice of pathology, most residents, particularly those in programs utilizing PAs, thought that the use of PAs would have no discernible effect.
Training Programs and National Accrediting Agency for Clinical Laboratory Sciences
On October 7, 1990, the AAPA BOT hosted representative educators of 4 existing university-based PA training programs and the APATP in a first joint meeting during the Providence, RI, AAPA Fall Conference. The AAPA and APATP began to define the procedures and policies on essentials for educational standards of PA training, the first step in creating commonality among all training programs [oral personal communication, Steven D. Suvalsky, MHS, PA(ASCP)CM November 2019]. By 1991, the internal AAPA program approval process, the “Guidelines for Establishment of an AAPA-approved Training Program,” was functioning as designed, and in 1992, the first AAPA-approved training programs (Duke University, Quinnipiac College, the University of Maryland, and Wayne State University) were recognized by the BOT as having achieved
In November 1993, the BOT commissioned AAPA members Steve Suvalsky and Jerry Phipps to participate in an NAACLS Accreditation Workshop in which the entire accreditation process was explained in a stepwise manner for programs pursuing initial accreditation, as well as programs needing to renew accreditation. The workshop further explained in depth how the essentials/standards were established, interpreted, and utilized to demonstrate evidence of compliance. The information was reported to the BOT and was reviewed by both the BOT and the APATP. After all concerns were addressed, the BOT voted to partner with NAACLS to develop a PA training program accreditation process. By 1995, the process had been developed.
The NAACLS representatives attended the 1995 AAPA annual meeting in Tucson, Arizona, to present the proposal to establish training program accreditation. The AAPA membership voted to accept the NAACLS proposal and thus was born the external, independent accreditation process for PA training programs. Wayne State University was the first program to enter the new accreditation process in the spring of 1996. All of the AAPA-approved programs achieved NAACLS accreditation within several years.
A measure of the success of the AAPA’s efforts to achieve national recognition was that CAP and ASCP, heretofore unsupportive of the AAPA, were active in reviewing and approving the NAACLS Training Program Essentials in 1997. 25 They also approved the outline of professional responsibilities of PAs (see below). From then until the present day, the PA profession has grown significantly, creating demands throughout the United States and internationally for program accreditation details. The NAACLS Essentials remain the standard for such accreditation today. Currently, there are 12 active NAACLS-accredited PA training programs and more in the pipeline (Table 2).
Clinical Laboratories Improvement Amendments of 1988
In 1992, the AAPA created an ad hoc committee on Clinical Laboratories Improvement Amendments of 1988 (CLIA’88) and sent a letter to the Healthcare Financing Administration commenting on proposed CLIA’88 regulations, specifically on the language describing personnel standards for laboratories performing high complexity testing, and to request that the wording be changed to allow laboratories to hire PAs to perform high complexity testing. In 1993, it was agreed that program-trained PAs met and surpassed the requirements and the guidelines were changed to allow pathologists to continue utilizing PAs as they had in the past.
National Commission for Certification of Pathologists’ Assistants
In 1999, the AAPA BOT voted to form a national committee to study the possibility of creating a national certification for PAs. 26 The committee was created as an independent entity, and the BOT subsequently officially sponsored the “National Committee for Certification of Pathologists’ Assistants” (NCCPA).
The NCCPA was officially formed in 2000 and held its first meeting in Toronto in conjunction with the annual AAPA meeting. The meeting was chaired by James W. Moore, executive director. In attendance were representatives from the AAPA, the APATP, the ASCP, the APC, and the ADASP. Also invited were representatives from NAACLS, the American Board of Pathology, the Federation of State Medical Boards, the World Association of Societies of Pathology, CAP, and 3 professional consultants to facilitate the process.
The Commission was charged with assuring the development and implementation of a national and ultimately international certification process for PAs. The first order of business was to perform an extensive review of the AAPA fellowship examination database to determine whether it was psychometrically sound, contained a sufficient quantity of examination items, and covered the breadth of knowledge to satisfy the critical elements of a national certification examination. The second step was to conduct a needs analysis, including a detailed study of the health care industry to determine the potential scope of a certification program and the perceived need, validity and cost–benefit evaluation of such a program.
As the Commission initially began work on the needs analysis in October 2000, members of the Pathology and Laboratory Medicine Department of Allegheny General Hospital (Pittsburgh, PA) expressed an interest in a collaborative project with the AAPA and the Commission. The project would be a survey distributed to a national sample of pathologists, investigating the use of nonphysician lab personnel in surgical pathology and gathering information about the effect of PAs on the pathologist manpower shortage. The needs analysis project, however, became larger and more time-consuming than anticipated, and so it was decided that the collaborative project would not be pursued. 27 Subsequently, the Allegheny General Hospital performed the survey independently, with help from one of us (T.L.R.). It was completed, and the results were published in 2004; pathology quality assurance specialists Richard Zarbo, MD, and Stephen Raab, MD, were coinvestigators. 28 An earlier study on the usefulness of PAs by Grzybicki et al 29 in 1999 concluded that cost and time calculations indicated that PAs are highly useful because they conserve pathologist time and decrease practice expenditures.
The needs analysis survey was sent out to 1300 PAs (both AAPA members and nonmembers) and their employers (pathologists and lab managers). Its main purpose was to determine the level of interest in certification among potential candidates and the level of support from their employers. It included research on pathology workforce issues, including PA practice characteristics. In a related 2001 study, Grzybicki et al conducted a survey of some 515 US PAs registered as members of the AAPA. The PAs were sent a questionnaire containing items relating to subject demographics, practice characteristics, specific task performance, and the amount of time spent per day on the performance of specific tasks. The conclusion was that there was a great degree of diversity in terms of individuals’ roles. 30
In 2003, the CAP invited the AAPA and NCCPA to attend a mutual fact-finding meeting regarding national certification at CAP headquarters in Washington, DC. The discussions were collegial and informative. At the close, CAP agreed to maintain open lines of communication with both groups. By 2003, the Commission had worked with multiple vendors to request proposals and had ultimately developed 2 final business plans. The first was for an independent certification program to be overseen by the AAPA and the second for a conjoint certification program between the AAPA and the ASCP BOR. The plans were presented to the AAPA BOT in the fall of 2003, and in December 2003, the BOT elected to partner with the ASCP BOR.
The following year, the AAPA BOT and the ASCP BOR developed a memorandum of understanding outlining the first national certification program for PAs and the development of a membership category for PAs within the ASCP. They signed the memorandum of understanding at the fall annual AAPA meeting in Chicago, Illinois. The AAPA and ASCP BOR created a CE program which required that every 3 years a certified PA must demonstrate sufficient CE to maintain ASCP certification. 31 Beginning in November 2004, AAPA fellow members were given the opportunity to be grandfathered into ASCP certification. For the initial group of fellows, the AAPA fellowship examination was accepted. All AAPA fellows were grandfathered without having to sit for the new certification examination. The AAPA BOT and officers made a concerted effort to encourage all affiliate members to sit for the fellowship examination at the Toronto annual meeting so that they might attain fellow member status and be included in the grandfathering offer. By the December 31, 2005, deadline, some 730 AAPA fellows were grandfathered. The first national certification examination for PAs was offered in Boston, Massachusetts, in September 2005 in conjunction with the annual AAPA meeting.
Pathologist Manpower Projections Fuel the Need for Assistants
In the 1960s and early 1970s, projections related to manpower needs in pathology had predicted a massive shortage of pathologists. After 1929, teaching hospitals (ie, all hospitals wanting to train interns and residents) were required to perform autopsies on a minimum of 15% of hospital deaths, and by the late 1960s, many hospitals had autopsy rates of 40% to 60%.
2
At this time, some academic physicians were pushing for even higher autopsy rates, while at the same time, some pathologists were warning that further capacity was not available. There was a humorous barrage of letters to the editor in the
It seems reasonable to assume that by 1975, every pathologist engaged in autopsy work may well be expected to be responsible for the performance of a minimum of 4 to 5 complete autopsies each day, seven days a week, 365 days a year.
38
p(16)
Pathologists recognized that the additional work could not be handled by residents and so plans to cope with these projected needs began to focus on creating “nonphysician prosecutors” with skill sets exceeding those of dieners who could perform autopsies under the supervision of a pathologist 39 ; in fact, some academic centers were already hiring and training licensed morticians to perform autopsies. 40
In a 1970 article in
On-the-Job-Trained Pathologists’ Assistants: The United States and Canada
From the very beginning, the founding fathers of the AAPA wanted to set a standard for its members based on their education and formal training. As they entered the workforce in the early 1970s, the first university-based program graduates encountered OJT PAs, who at that time did almost exclusively autopsy work. However, over the next few decades, a new more broadly trained group of OJTs arose. As mentioned above, the acceptance of OJTs as AAPA members and their membership status would be the source of much debate over the years, as some university-trained PAs expressed concerns that OJTs would diminish their professional status, potentially flood the job market and negatively affect salaries. The AAPA’s persistent inclusive stance, however, eventually resulted in a significant increase in membership numbers and greater financial strength. Both would have a positive impact on their quest for national recognition. During the final stages of creating a national certification process, the AAPA leadership decided to gradually phase out the OJT route to membership. 46 Under the terms of the phase-out process, OJTs already in the membership pipeline were given time to meet the requirements for and to take the fellowship examination. Passing the examination within the allotted time would qualify them to be certified along with other fellow members. An OJT subcommittee was created to help OJTs with their applications. On-the-job-trained PAs were provided a new examination handbook and mentors to help them prepare for the examination. The rapid increase in OJT fellow members as the deadline approached shows the effectiveness of the AAPA’s program to help OJTs successfully meet the standard by passing the fellowship examination (Table 1).
In Canada, the PA profession was slower to develop and evolve, but, otherwise, the pattern has been similar. The Canadian Association of Pathologists–Association canadienne des pathologistes (CAP-ACP) formed a PA Section in 2006, and it functions like the AAPA. The CAP-ACP PA Section published its position statement outlining policy topics including membership requirements and key competencies and responsibilities for Canadian PAs. 47 Some PAs in Canada were enthusiastic to simply adopt the existing American certification process, and this almost happened. As noted above, when the certification process was being developed for American PAs, time-limited “grandparenting” allowed senior American OJT PAs who had passed the fellowship examination to become ASCP certified, but this door closed forever in 2007. Also in 2007, the first NAACLS-accredited Canadian PA training program opened its doors with a second accredited program beginning in 2012. 2 Graduates of these accredited training programs were eligible to become board-certified by passing the ASCP examination. This resulted in a new generation of board-certified PAs and a more senior group of OJT PAs in Canada. Because the organization of PAs in Canada had lagged behind, there was not an opportunity to address the certification needs of senior Canadian OJT PAs who began the profession in Canada. Therefore, a separate Canadian Certification Council of Canada (CCCPA-CCCAP) was created in 2012, in anticipation of developing a Canadian PA certification examination. This seemed redundant to many and so, in 2013 to 2014, the CAP-ACP PA Section leadership and one of us (J.R.W.), representing the Canadian Chairs of Pathology & Laboratory Medicine, held discussions with both the NAACLS and the ASCP to determine whether they would consider time-limited grandparenting for senior Canadian OJT PAs willing to write the ASCP examination. Because of the perceived contentiousness of the earlier debate in the United States, this did not happen, and so, after achieving ISO 17024 compliance, a Canadian certification examination (CCCPA-CCCAP) was implemented on June 12, 2017. 2 This has resulted in confusion for the profession on both sides of the border. Currently, there are 10 active NAACLS-accredited PA training programs in the United States and 2 in Canada; graduates of these programs are all eligible to take the ASCP BOC examination and can practice on either side of the border. Graduates of the 2 Canadian programs can also become certified by the CCCPA-CCCAP. However, there are currently 2 active training programs in Canada that are not NAACLS-accredited but have already produced graduates, and because of the CCCPA-CCCAP certification criteria, 48,49 these graduates are ineligible to write the certification examination in either country. Addressing the poor planning that created this unfortunate situation as well as the shortage of PAs required an extension of the planned “sunsetting” of grandparenting for certification of OJT PAs in Canada (after mid-2021, only graduates of NAACLS MSc training programs were to have been eligible for Canadian certification). 48,49 Currently, graduates of unaccredited programs in Canada can sit the Canadian, but not the American examination, after obtaining 2 years of work experience using the still open Canadian OJT grandfathering route, which has now been extended to 2024. This unfortunate situation may eventually result in a separate Canadian accreditation system for training programs in Canada 50,51 and loss of the ability of some North American PAs to work seamlessly on either side of the border. Considering that, currently, almost 30% of the active PA training programs are in Canada (see Table 2), it is important that these issues be resolved.
Scope of Practice
The scope of practice for PAs as it exists today had its humble beginnings in the “AAPA Job Description Project” in the late 1970s and early 1980s. The major accomplishment of the project was the development of a protocol detailing the scope of “gross tissue examination and personnel qualifications for nonphysicians doing grossing.” From that protocol arose a document created in 1983 entitled “Professional Responsibilities of the Pathologists’ Assistant.” In 1994, this document was submitted to an ad hoc committee of the ASCP for review. The document was reviewed and accepted by the ad hoc committee and subsequently by the ASCP.
During the fall 1997 ASCP/CAP meeting, 2 separate resolutions, each addressing the role and scope of practice of PAs, were submitted to the CAP board of delegates by pathologists in favor of utilizing PAs in their practices. The resolutions were so similar that they were combined for the purpose of being studied by a board of delegates ad hoc committee on PAs. After 2 years of review and deliberation, the report on the utilization and global impact of PAs was presented at the fall 1999 ASCP/CAP meeting.
26
The report generated significant discussion, which resulted in 6 recommendations being added to the report. The recommendations were as follows: Future PAs be at least baccalaureate graduates of accredited training programs. A national certification process be developed. New questions for the CAP Laboratory Accreditation Checklist regarding appropriate supervision of PAs and appropriate protocols for specimen dissection be developed. New questions for CAP Practice Characteristics surveys be developed. Delineation of PA functions versus pathologist functions in anatomic pathology be clarified. All recommendations for compliance with CLIA’88 be monitored.
In 2003, the AAPA BOT initiated contact with CAP to discuss a collaborative effort to create a scope of practice for PAs. In 2004, after a series of meetings, the AAPA’s “Professional Responsibilities of Pathologists’ Assistants” document was utilized by the AAPA and CAP as the basis for the collaborative creation of the first official “Scope of Practice of Pathologists’ Assistants” document.
Licensure
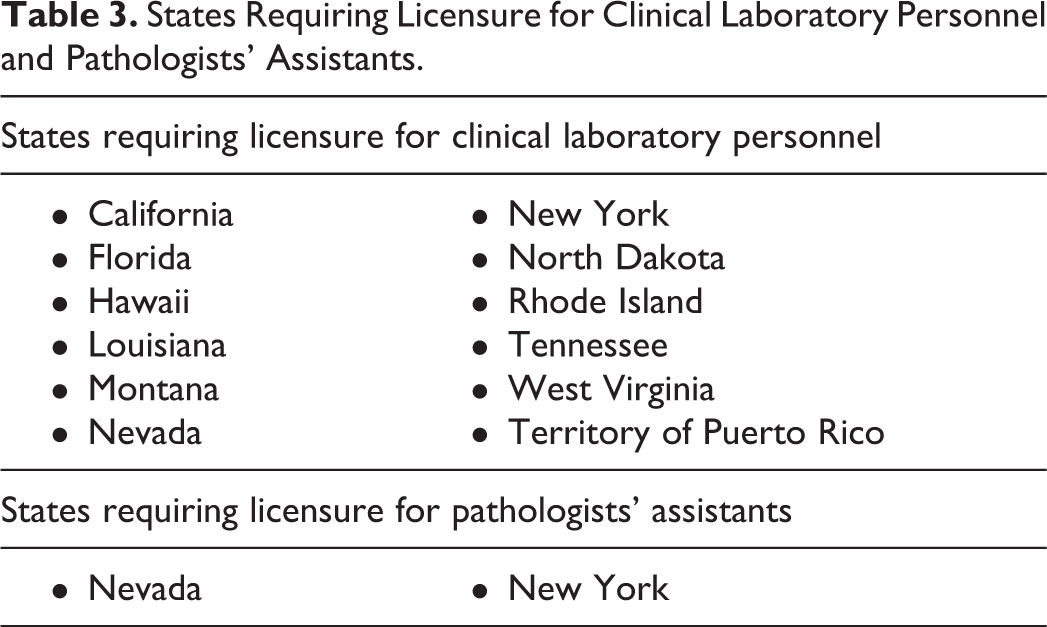
Many states have laws requiring the licensing of laboratory personnel such as medical technologists, medical technicians, histotechnologists, cytotechnologists, and so on. Most of these laws were passed many decades ago, when PAs did not yet exist. 2,5 Although licensure for laboratory technologists was initially opposed by both the ASCP and the AMA, which had developed their own mechanism to regulate these professions in the 1930s, some state legislatures did not bow to these pressures. 5 States which currently require licensure for clinical laboratory personnel are given in Table 3. Five other states are currently considering licensing of clinical laboratory personnel. Currently, only 2 states require licensure for PAs (see Table 3). The AAPA continues to monitor licensure issues and individual state licensure bill proposals across the country and to contribute appropriate information about PAs and the Association to all interested parties.
States Requiring Licensure for Clinical Laboratory Personnel and Pathologists’ Assistants.

The AAPA BOT issued a
In our opinion, appropriate licensure is that which places the interests of patients first, with all other objectives secondarily. The AAPA will support legislation that aims at improving patient care and will oppose legislation that does not. The AAPA advocates for our profession and for our members, and, to the extent we are able, we will protect them. Consequently, the AAPA will address any legislation that threatens our members’ ability to practice.
53
In December 2008, CAP weighed in on the licensure issue, announcing that they were changing their position regarding licensing of clinical laboratory personnel and would now support state licensing bills providing they met certain specific criteria. Pathologists’ assistants were not included in their specific criteria list. 54
Grossing Guidelines
In 2010, the AAPA offered a new CE source titled
The following year, AAPA BOT Chair Jon Wagner proposed that the AAPA published a set of “Grossing Guidelines,” which would highlight the PA’s specialized skill set and work. The project would be a major collaboration with CAP and the American Joint Committee on Cancer and would utilize CAP’s cancer protocols. The development of the Grossing Guidelines was a 5-year undertaking, culminating with the release on April 14, 2017, of the
Conclusion
The founding fathers of the AAPA managed to create in 1972 a professional allied health organization in the face of opposition from elements of the medical community and organized pathology. Their vision for a nonprofit organization was to create guidelines for training programs, develop a de facto certification/membership examination, develop a CE program for its members, and actively pursue national recognition. From its inception, the AAPA has been a volunteer-driven organization, although in order to manage its growth, it has financially contracted with a Central Office since the 1980s.
As the AAPA’s early goals were achieved, new goals were established to further cement its place in the medical community. The AAPA has played a significant role in the establishment, growth, and success of the PA profession. Although they adopted a proactive stance in pursuing their goals, the AAPA also recognized the importance of the influence that individual PAs could exert at the grassroots level. They encouraged individual PAs to inform their pathologists about the Association and keep them current on matters affecting the profession, establishing relationships in the workplace, and winning over individual pathologists based on their abilities and professionalism. The AAPA membership numbers grew from 5 in 1972 to greater than 2200 as of 2020. A brief historical timeline is summarized in Table 4.
Historical Timeline for the Pathologists’ Assistant Profession in the United States.

Over many years, the AAPA forged successful professional relationships within the medical community and with organized pathology groups, building further support for the profession. The creation of a national certification process and the development of training program accreditation proved to be the springboards to achieving national recognition. The number of active, accredited training programs has grown from 4 in 1975 to 12 in 2020, with more in the pipeline. The role of the PA has expanded in anatomic pathology; in addition to the traditional work in surgical and autopsy pathology, PAs are currently involved in laboratory management/administration, teaching, research, bio-banking, and so on. The AAPA is well positioned to maintain its leadership role in advocating for its members, supporting the profession, and cementing its place in the medical community.
Footnotes
Acknowledgments
The authors thank AAPA founding fathers Norman Gerard and Coy Wagoner; Michelle Sok, AAPA Central Office; Pamela Vollmer, Duke University Medical Center; Jessica Jasso and Michele Stevenson, NAACLS; Kristin Rodgers, The Ohio State University Medical Heritage Center; Thomas Kryton, BFA; and Charlotte Monroe.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Thomas L. Reilly is Board of Trustees Historian for the AAPA. James R. Wright Jr is medical director for a NAACLS-accredited training program in Canada and a former member of the Canadian Chairs of Pathology & Laboratory Medicine. This article is an expression of the authors’ opinions and does not represent an official publication of the AAPA or any other organization.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
