Abstract
Keywords
Primary Learning Objectives
Competency 2: Organ System Pathology; Topic HB: Hepatobiliary; Learning Goal 7: Cholelithiasis
Competency 2: Organ System Pathology; Topic HB: Hepatobiliary; Learning Goal 7: Cholelithiasis
Patient Presentation
A 43-year-old woman presents to the emergency department with persistent, 8/10 right upper abdominal pain and vomiting. She notes associated mild pain around her right scapula. She states that her pain began 6 hours prior, and she does not remember any precipitating factor or trauma. She does recall having intermittent, less severe episodes of abdominal discomfort over the previous year. She mentions that taking antacids does not help with her recurrent pain, which occurs after large meals and resolves spontaneously. She takes combined oral contraceptives and has history of obesity and noninsulin dependent diabetes. She denies chest pain, heartburn, lower abdominal pain, diaphoresis, and dizziness.
Diagnostic Findings, Part I
Vital signs are blood pressure 125/88, heart rate 117, respiratory rate 16, and temperature 37.3 °C. The physical examination reveals marked tenderness to palpation in the right upper quadrant (RUQ) and a positive Murphy’s sign (RUQ pain with inspiration during deep palpation, just below the ribs).
Questions/Discussion Points, Part I
What Pertinent Points in the History and Physical Examination Support the Differential Diagnosis and What Further Testing Is Warranted?
The character and timing of the patients’ chronic pain are known as biliary colic (intermittent, dull, and often postprandial). Patients with an obstruction of the cystic duct, which drains bile from the gallbladder into the bowel, often complain of biliary colic. This pain is related to gallbladder contraction after meals, which is mediated neurohormonally; pressure builds in the gallbladder and stresses the wall. 2 Pain referred from the gallbladder to the scapula is characteristic and is mediated by shared sensory afferent neuronal synapses at the spinal cord.
Gallstones (cholelithiasis) often obstruct the cystic duct and cause disease, and this patient does have several known risk factors for gallstones: age (>40 years old), female sex, obesity, diabetes, and oral contraceptive usage. Additional cholelithiasis risk factors include rapid weight loss, pregnancy, and use of insulin. 3 Other diagnoses which could be investigated are angina, myocardial infarction, peptic ulcer disease, gastroesophageal reflux disease, pancreatitis, hepatobiliary disease, and pelvic inflammatory disease. 4 These can be evaluated through focused history taking. Angina pain is often sharp, located in the chest, and random or exertional, which this patient does not describe. Myocardial infarction most often presents with a pressure or crushing sensation in the chest, and radiation to the arm or jaw, which this patient does not have (although myocardial infarction may present with atypical symptoms in women). Peptic ulcer disease relates to stomach pain caused by gastric acid secretions at meals; that typically is relieved with antacids, which is not the case in this patient. Heartburn is related to irritation of the lower esophagus by gastric acid, which also is relieved by antacids. Diagnostic tests and procedures should be ordered to evaluate each of these diagnoses further, if clinical suspicion exists (ie, electrocardiogram and troponins for myocardial infarction, endoscopy for peptic ulcer disease, amylase and lipase for pancreatitis, liver enzymes for hepatobiliary disease). However, the most likely differential diagnosis in this case is acute gallbladder disease secondary to gallstones (acute calculous cholecystitis). It is important to note that the cystic duct can be intermittently obstructed without symptoms, and without gallstones. Acute gallbladder disease without gallstones (acute acalculous cholecystitis) is unlikely in this patient, because of her history. Patients with acalculous cholecystitis may have RUQ pain or no pain associated with the gallbladder. These patients typically are hospitalized for conditions unrelated to the gallbladder, and so a clinician should remain vigilant for this. Risk factors are sepsis, infection, immunosuppression, chemotherapy, and major trauma or burns. Testing focused on gallbladder disease is pursed because her risk factors, characteristic clinical presentation, and lack of symptoms supportive of another etiology suggest gallstones as the cause of her illness.
Diagnostic Findings, Part II
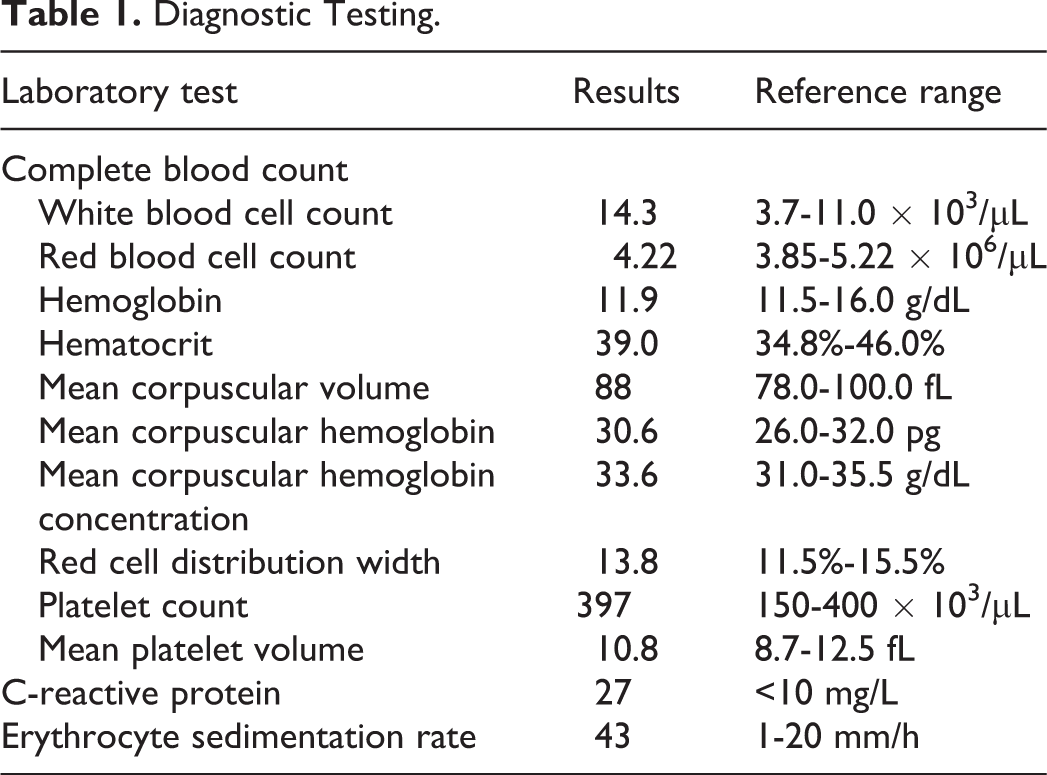
Laboratory test results can be viewed in Table 1. From a complete blood count (CBC), the patient was found to have an elevated white blood cell (WBC) count. White blood cells proliferate because of cytokines produced by immune system cells, as in this patient, in response to inflammation. White blood cells may also proliferate because of unsuppressed WBC growth pathways, as in leukemia. In addition, individual tests of her erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) showed results above the normal reference range. Inflammation and tissue injury causes several cell types to release a variety of protein molecules, including acute phase reactants like fibrinogen and CRP, which increase the viscosity of the blood. Erythrocyte sedimentation rate refers to the rate of in vitro red blood cell (RBC) settling which is normally limited by negative charges on the RBC surface. Positively charged acute phase proteins decrease the negative charge on RBCs, and lead to rouleaux formation, and hence faster RBC settling. C-reactive protein is produced in the liver and transported in the blood, binding to materials which will be identified and attacked by the immune system. Erythrocyte sedimentation rate and CRP, both signify inflammation and can be increased in patients with infection, trauma, infarction, systemic autoimmune and inflammatory diseases, and various neoplasms. At this point, the clinical and laboratory evaluation suggest gallbladder inflammation.
Diagnostic Testing.
Question/Discussion Points, Part II
What Radiographic Studies Can Further Characterize This Patients’ Gallbladder Disease? What Findings Are Seen?
The patient has a transabdominal ultrasound of her gallbladder performed (Figure 1). The ultrasound findings visible in Figure 1 suggest the gallbladder, and specifically gallstones, as a likely source of her acute pain. Pericholecystic fluid accumulation (not depicted in Figure 1) is an ultrasound finding that is supportive of acute gallbladder disease, compared to chronic disease. That finding would be especially useful to guide care in acalculous cholecystitis. In severely ill patients, it is important to be suspicious of acalculous cholecystitis because, left untreated, the complications can be fatal. Of note, gallstones can be missed by ultrasound; a hepatobiliary iminodiacetic acid (HIDA) scan (a contrast material is injected into the veins that should accumulate in the gallbladder if it is not obstructed) is more sensitive for detection of cystic duct occlusion.
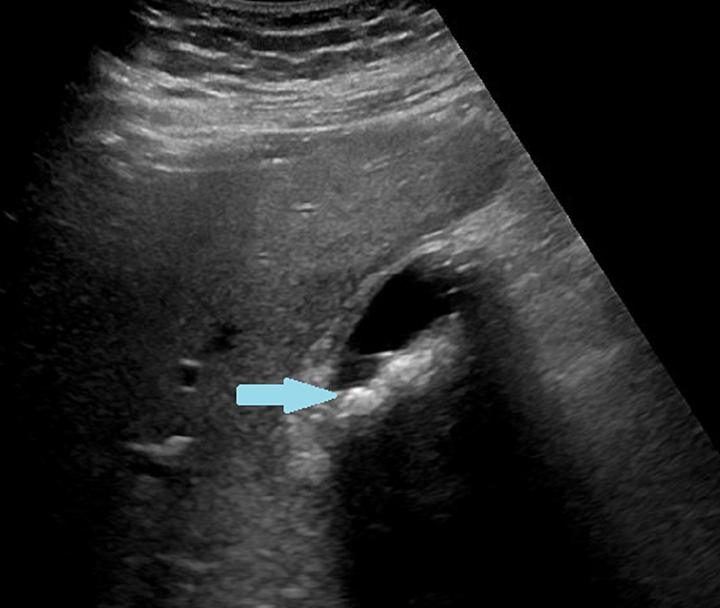
Gallbladder ultrasound showing moderate thickening of the gallbladder wall and gallstones (blue arrow) with associated hypoechoic “shadows” (black area, below gallstones).
This patients’ combination of clinical symptoms, laboratory data in Table 1, and ultrasound findings in Figure 1 results in a decision to perform urgent laparoscopic cholecystectomy. Importantly, the procedure would also be performed in cases of acalculous cholecystitis. Also, the gallbladder could be removed electively in cases of biliary colic because of cholelithiasis. Whether the presence of nonsymptomatic gallstones is an indication for cholecystectomy is controversial.
Diagnostic Findings, Part III
A laparoscopic cholecystectomy was performed where an intact, erythematous gallbladder was freed from the liver bed and removed through a laparoscopy port. The resected gallbladder is sent to Pathology (Figure 2).
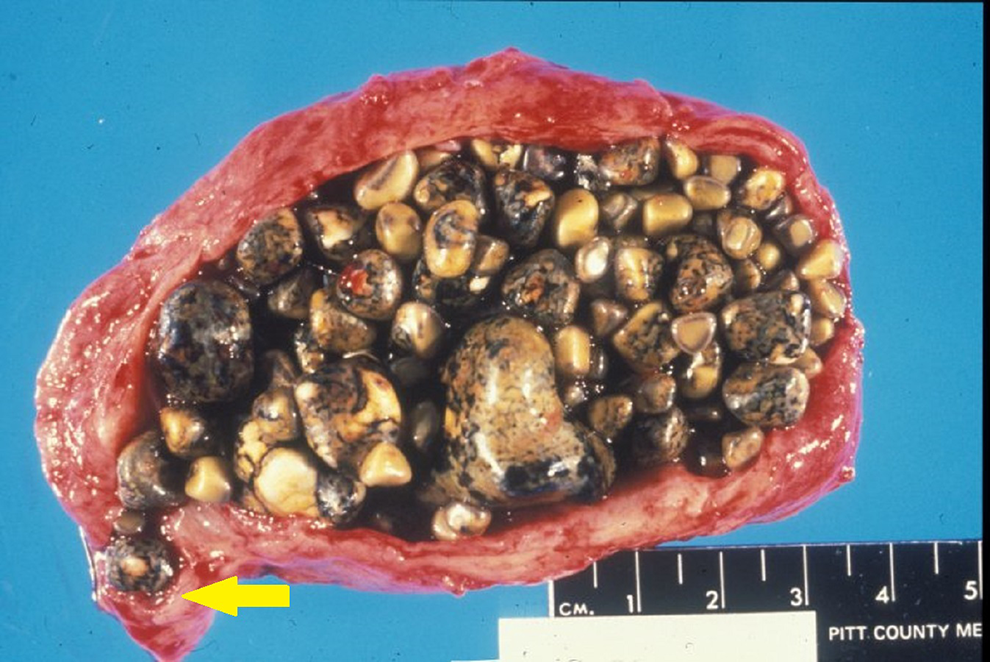
Opened gallbladder, distended by innumerable yellow-black gallstones. A stone occludes the cystic duct (yellow arrow). The inflamed gallbladder wall has thickened to measure 1.0 cm; normal is 0.3 cm or less.
Question/Discussion Points, Part III
What Additional Clinically Relevant Information Could a Gross Gallbladder Specimen Provide?
Examination of the gallbladder in the pathology laboratory definitively shows a gallstone occluding the cystic duct, which is shown in Figure 2. Acute calculous cholecystitis occurs because the gallbladder contracts against a cystic duct that is obstructed by gallstones, causing inflammation, edema, and ischemia of the gallbladder wall. However, gallstones can linger in the gallbladder for years without causing acute cholecystitis. Cholelithiasis often results in chronic inflammation of the gallbladder (chronic cholecystitis). Of note, elevated inflammatory markers
With acute acalculous cholecystitis, bile sludge (sediments of cholesterol, mucin, and mineral salts) maybe seen without obvious cystic duct occlusion. Despite that, inflammation, edema, and ischemia of the gallbladder wall will be present. The pathogenesis arises from compromise of blood flow to the cystic artery leading to gallbladder ischemia, and edema, which further impedes blood flow.
Diagnostic Findings, Part IV
Representative sections of the specimen are taken for microscopic examination (Figures 3, 4, and 5).
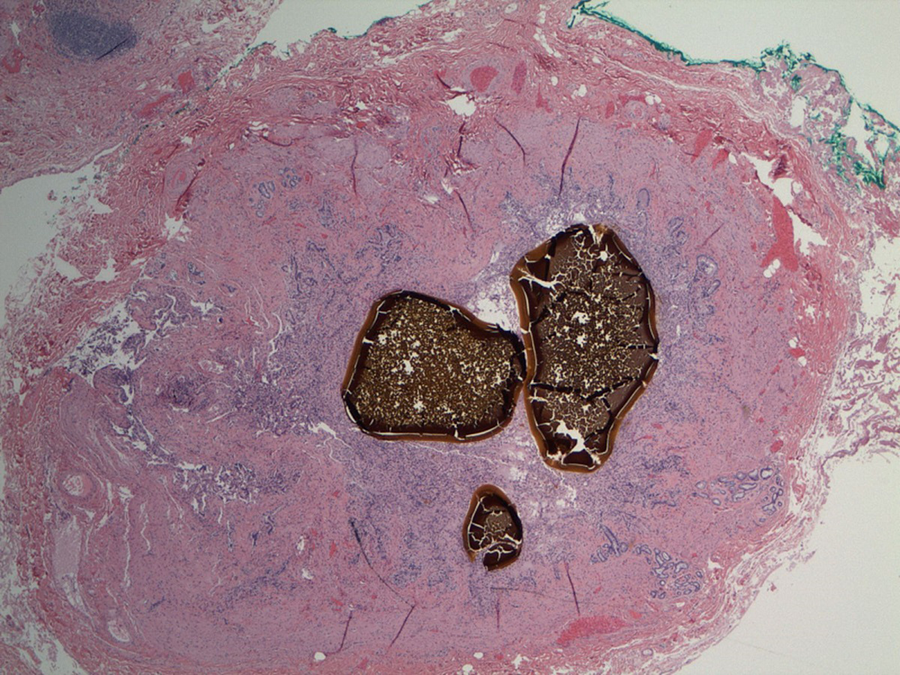
Microscopic image of the cystic duct in cross-section on low power, H&E 2×. A thickened, fibrous cystic duct (pink) and epithelium (purple) encompass the gallstones (brown).
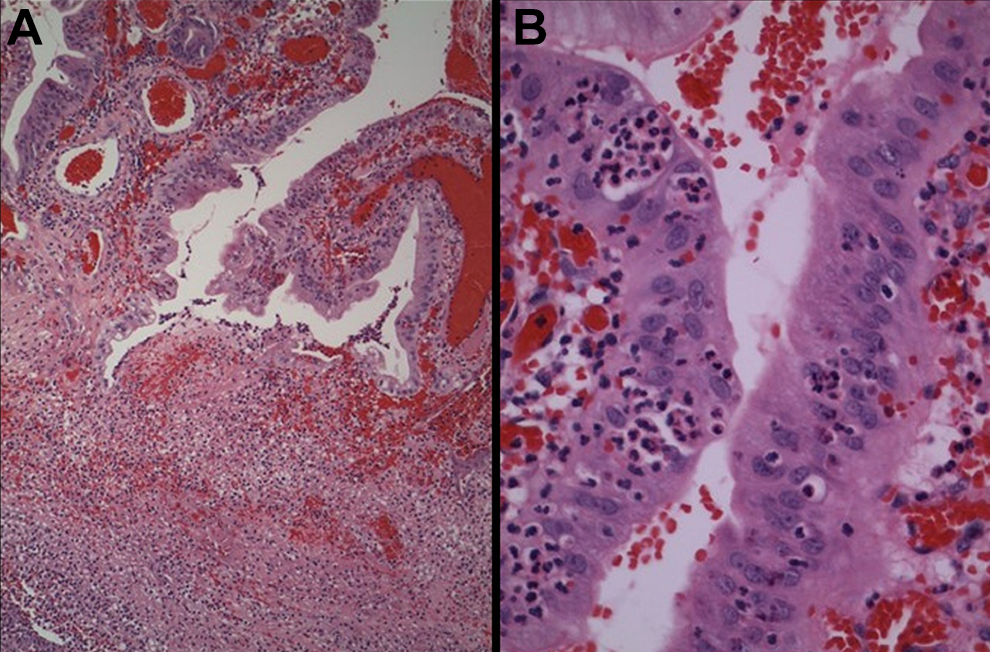
A, Microscopic image of gallbladder mucosa on low power, H&E 10×. Inflamed gallbladder epithelium (purple layers of cells) line the lumen and hemorrhagic lamina propria. Note the dark purple dots throughout which are neutrophils, confirming acute inflammation and diagnostic of acute cholecystitis. B, Microscopic image of gallbladder epithelium on high power, H&E 40×. The crowded, disordered epithelium (light purple layer) is infiltrated by numerous neutrophils, characteristic of acute cholecystitis. Reactive epithelial atypia should not be mistaken for dysplasia or malignancy. Hemorrhage is noted in the lamina propria (bright red cells).
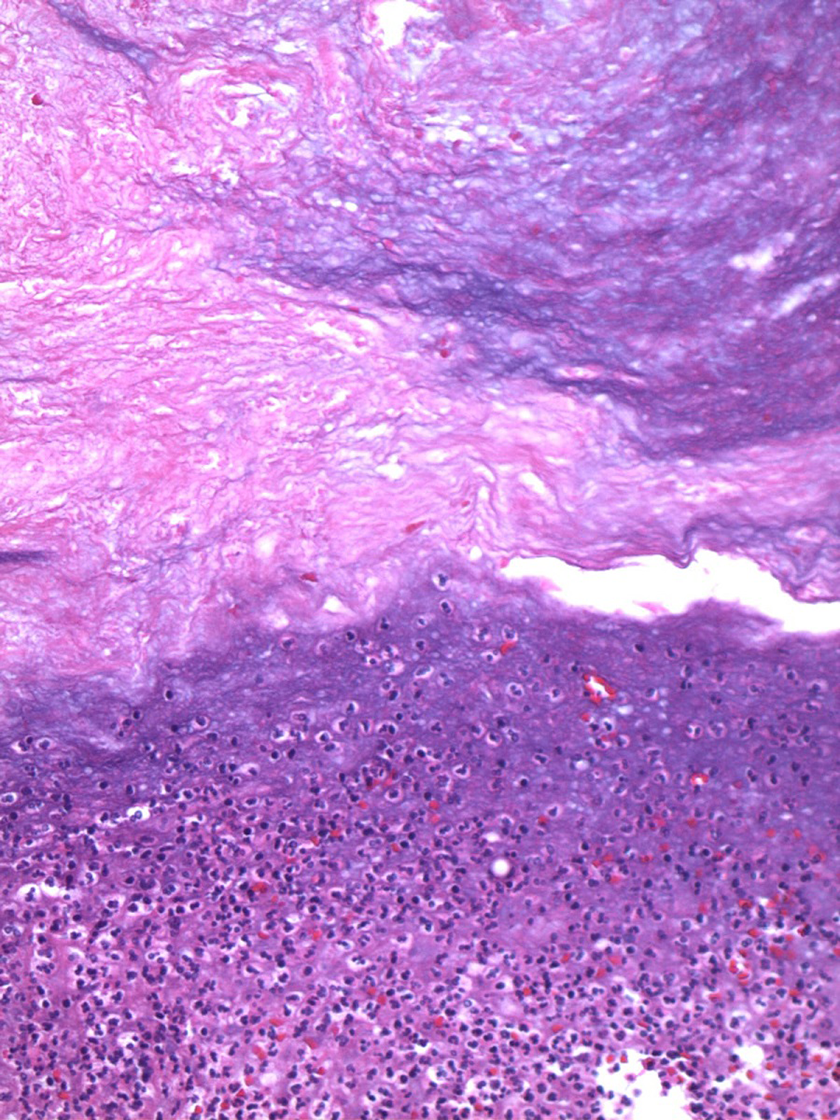
Microscopic image of gangrenous gallbladder mucosa on intermediate power, H&E 20×. Coagulative necrosis (gangrene) is indicated by the absence of nuclei (top portion of image) and presence of necroinflammatory debris (neutrophilic infiltrate with associated necrosis) (bottom portion of the image).
Question/Discussion Points, Part IV
What Additional Clinically Relevant Information Could Histologic Sections of the Gallbladder Provide, Microscopically?
A diagnosis of acute cholecystitis can be made based on histologic evidence of inflammation, with or without evidence of cholelithiasis, as in acalculous cholecystitis. Any number of neutrophils, as shown in Figure 4, present in the tissue indicate acute inflammation although a primarily lymphocytic infiltrate favors chronic inflammation; both maybe present. Histologic examination is negative for adenocarcinoma, which would appear as infiltrative glands with dysplastic epithelium on microscopic examination (which is found in a minority of gallbladders removed for acute cholecystitis typically in elderly patients).
What Is Your Diagnosis?
The patient has acute cholecystitis secondary to cholelithiasis (obstructing gallstone), which was suspected by laboratory, imaging, and clinical findings and confirmed by the pathologic findings. Both the histologic findings, displayed in Figure 3, and the gross findings, shown in Figure 2, are available in the surgical pathology report for the resected gallbladder specimen in the patients chart.
What Can Happen if the Diagnosis and Appropriate Surgical Intervention Is Delayed in Cases of Cholecystitis?
Inflammation injures the wall of the gallbladder. One possible consequences of prolonged inflammation and distension is gangrene (a form of tissue death because of ischemia or complete lack of blood flow and oxygen, Figure 5).
Aside from severe pain, gangrenous cholecystitis can result in perforation of the gallbladder wall with associated pneumoperitoneum (air inside the abdomen) and peritonitis which can be life-threatening (particularly in already critically ill patients). In this setting, gallbladder empyema (filling of the gallbladder with pus) can be seen as well. To avoid these complications, emergent cholecystectomy is indicated in patients with suspected acute cholecystitis.
What Is the Composition and Pathogenesis of Gallstones?
Four types of gallstones are commonly encountered: cholesterol, mixed, combined, and black (bilirubin) stones. 5
Pure Cholesterol Gallstones
Cholesterol is soluble in bile secreted by the hepatobiliary system. When bile becomes supersaturated with cholesterol, crystalline seeds of that lipid form as cholesterol monohydrate. Those serve to nucleate further crystallization, a process that yields gallstones. These stones are typically a pale yellow color. Sizes vary, up to several centimeters, and shapes are often multifaceted and polygonal.
Mixed Gallstones
Mixed stones are composed of between 20% and 80% cholesterol. The other compounds in mixed stones are in variable levels: bilirubin, palmitate phosphate, calcium carbonate, and bile pigments. These stones are often identified in association with infection of the biliary tract. These stones typically appear on radiographs, because their calcium content is radiopaque. With decreasing concentrations of cholesterol, colors range from yellow to grey-white, or black. Size and shapes are variable.
Black Gallstones
Unconjugated bilirubin can form complexes with insoluble calcium salts and inorganic calcium salts to form pigment stones. Conditions which increase the concentration of unconjugated bilirubin in the hepatobiliary system, precipitating pigment stone formation, are hemolytic anemias and parasitic/bacterial infections. Pigment gallstones are produced when bile is supersaturated by unconjugated bilirubin. Black stones contain polymers of the calcium salts of unconjugated bilirubin, trace calcium carbonate, calcium phosphate, and may contain some cholesterol. Brown stones are a subtype of black gallstones, but contain more cholesterol and other fatty acids. Black stones are often innumerable, friable, and less than 1.0 cm. Brown gallstones tend to be soap-like and smooth. Mucin is a prominent matrix component involved with both stones’ composition.
Combined Gallstones
When separate components of 2 of the above types of gallstones are present within single gallstones it is referred to as “combined gallstones.” The stones are almost always a combination of pure cholesterol and mixed gallstones.
Teaching Points
The most common risk factors for gallstones are age (> 40 years old), obesity, noninsulin dependent diabetes mellitus, and oral contraceptive usage.
A chief complaint of acute RUQ pain, especially with a history of biliary colic, should prompt immediate investigation of acute cholecystitis from cholelithiasis.
Patients with acute cholecystitis often have nonspecific findings of elevated WBC, ESR, and CRP because gallbladder inflammation.
An abdominal ultrasound will often identify cholelithiasis. In cases with negative ultrasound findings and high suspicion/high risk for acute cholecystitis, the HIDA scan is the most sensitive radiographic test.
Gallstones are forced into the cystic duct by gallbladder contractions, where they may obstruct the duct lumen and cause pain.
Definitive treatment for acute cholecystitis is cholecystectomy.
The diagnosis of calculous, or acalculous cholecystitis, is confirmed by gross examination, in conjunction with microscopic examination, of the excised gallbladder. Gross and microscopic examination of the gallbladder also aims to rule out the presence of adenocarcinoma.
Prolonged inflammation of the gallbladder may lead to extreme pain secondary to gangrene, which can be further complicated by gallbladder perforation that causes peritonitis.
There are 4 distinct types of gallstones, each with characteristic chemical and physical attributes. They are pure cholesterol, mixed, black, and combined gallstones.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
