Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective M4.1: Identification of Mycobacteria. Describe the diagnostic tests available for the identification of mycobacteria including culture methods and new molecular tests.
Competency 3: Diagnostic Medicine and Therapeutic Pathology; Topic M: Microbiology; Learning Goal 4: Mycobacteria
Patient Presentation
The patient is a 55-year-old Caucasian female who presents to the emergency department with a 3-day history of hemoptysis. She reports a 2-month history of progressive dyspnea, productive cough, worsening fatigue, and subjective chills. She reports 10 pounds weight loss during this time.
She has a past medical history of gastroesophageal reflux disease, chronic obstructive pulmonary disease (COPD), and hyperlipidemia. She is a one pack per day smoker (she began smoking at age 35) and was recently homeless for about 6 months during which time she stayed in a local homeless shelter.
Pertinent social history includes no known sick contacts, no travel abroad, and she is currently unemployed.
Her HIV status is unknown, and she does not take any medications on a regular basis.
Physical examination reveals a thin female who appears older than her stated age. Her vital signs are within normal limits. There is no cyanosis or clubbing of her nails. Her fingertips are yellow-tinged. She appears to be breathing comfortably at rest without use of accessory muscles. An increased expiratory time is noted. She has an occasional cough.
Further examination reveals equal curvature of her chest bilaterally, mild barreling is appreciated. No bruising, masses, or sinus tracts are observed. Chest auscultation reveals diminished breath sounds bilaterally. Fine inspiratory crackles in the lower lung fields are present. No wheezing or rhonchi are heard. She does not report any chest pain.
The differential diagnosis includes COPD exacerbation and, given her reports of hemoptysis, we must also consider malignancy and community-acquired pneumonia with atypical organisms such as mycobacteria.
Diagnostic Findings, Part 1
Imaging Studies
Chest X-ray/chest computed tomography
Her chest computed tomography (CT)-scan reveals a large cavitary lesion in the right upper lobe (Figure 1). Also noted on chest CT are scattered right upper lobe and left upper lobe tree-in-bud opacities and bibasilar atelectasis.
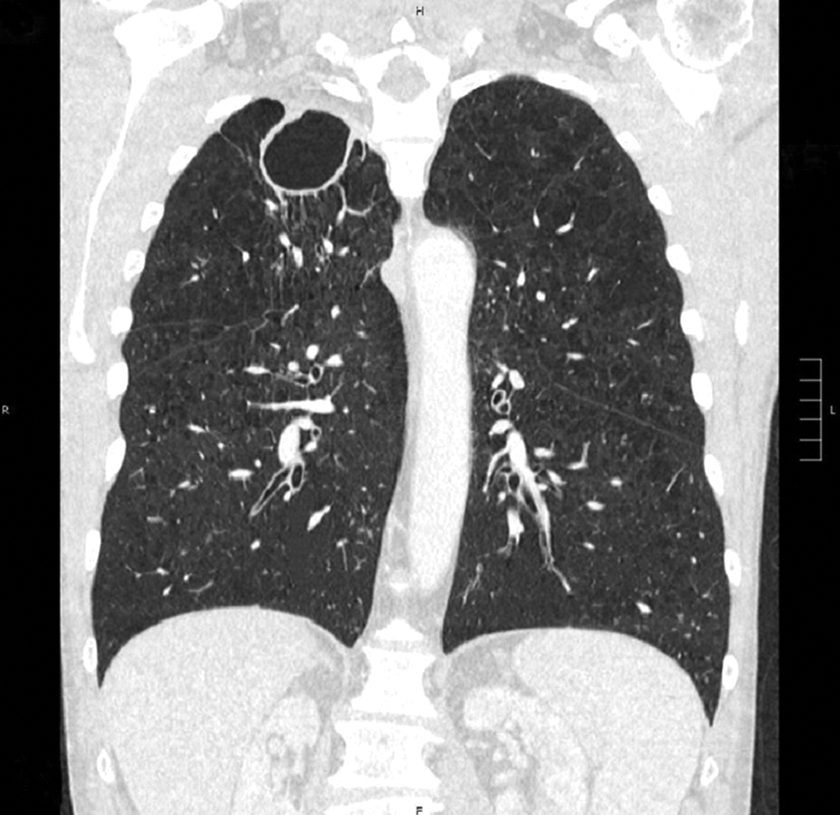
Anterior cross-sectional image from the patient’s high-resolution computed tomography (CT) scan showing a large cavitary lesion in the right upper lobe.
Questions and Discussion, Part 1
What Is Our Differential Diagnosis Given the Patient’s Computed Tomography Scan?
The differential diagnosis for cavitation includes malignancy, Mycobacterium tuberculosis, and nontuberculous mycobacterial infections. The tree-in-bud opacities can indicate fungal versus nontuberculous mycobacterial infections. Further workup is needed to determine the etiology of these findings.
What Additional Diagnostic Tests Are Indicated for This Patient?
Due to the nonspecific nature of radiographic findings, further workup should include microbiologic confirmation. To rule-out mycobacterial infection, the patient’s sputum should be tested for the presence of mycobacteria via acid-fast bacilli (AFB) stain and culture. 2 Three sputum specimens are ordered, each to be collected on separate days in the early morning. If specimens cannot be collected on separate days, there must be a minimum of 8 hours between specimens, but one must be collected in the early morning. 2 Sufficient volume for recovery of Mycobacteria is a minimum of 5 mL. The patient should rinse their mouth with water before providing a sputum specimen, but oral care with chlorhexidine or other hygiene products should be avoided for optimal recovery of mycobacteria.
Can a Mantoux Tuberculin Skin Test or an Interferon-γ Release Assay Help Us Identify the Species of Mycobacteria?
No, while interferon-γ release assay testing is more specific than Tuberculin Skin Testing for the detection of M. tuberculosis, the gold standard for species identification is a sputum culture.
Diagnostic Findings, Part 2
Laboratory Data
Sputum cultures
The AFB stain yields 1+ AFB on the direct smear using the Kinyoun stain (Figure 2), a process that includes the use of carbol fuchsin, acid alcohol decolorizer, and a methylene blue counterstain. In Figure 2, we see the beaded appearance of long, narrow AFB stained red by the carbol fuchsin dye while the background and non-acid-fast bacteria retain the methylene blue counterstain.
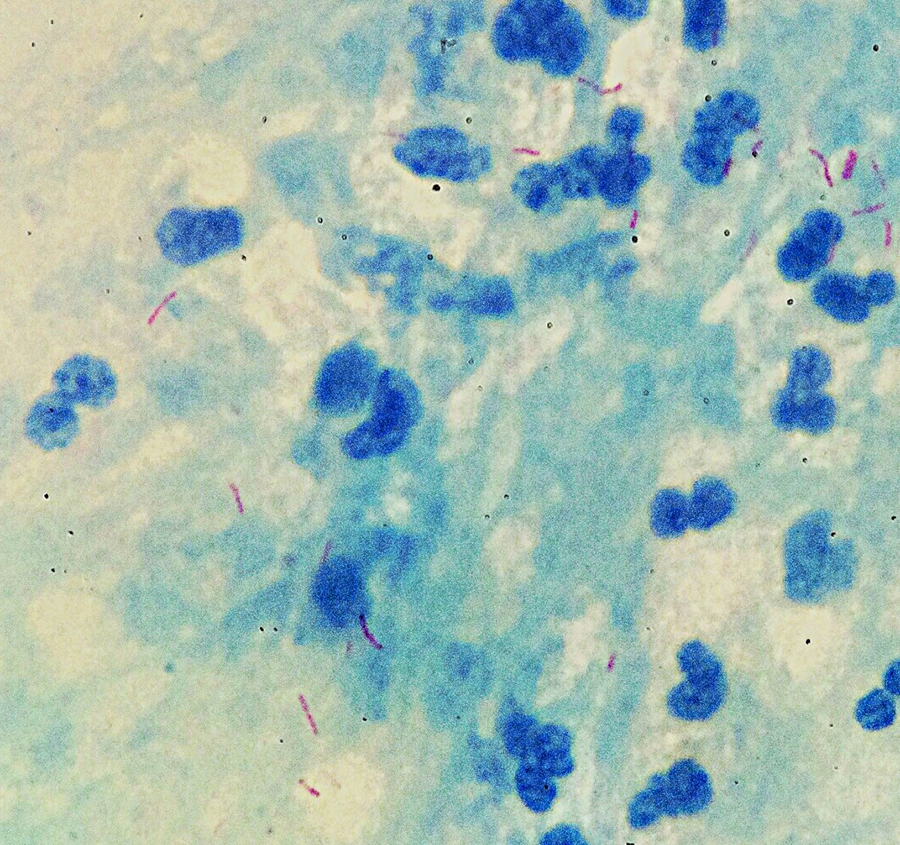
Acid-fast bacilli (AFB) with a beaded appearance, seen here retaining the red carbol fuchsin dye in contrast to the blue extracellular debris which are retaining the methylene blue counterstain.
Ten days later, the culture on solid Lowenstein Jensen (LJ) media grows AFB (Figure 3). In Figure 3, we see smooth yellow colonies, characteristic of certain Mycobacteria, growing on the LJ media.
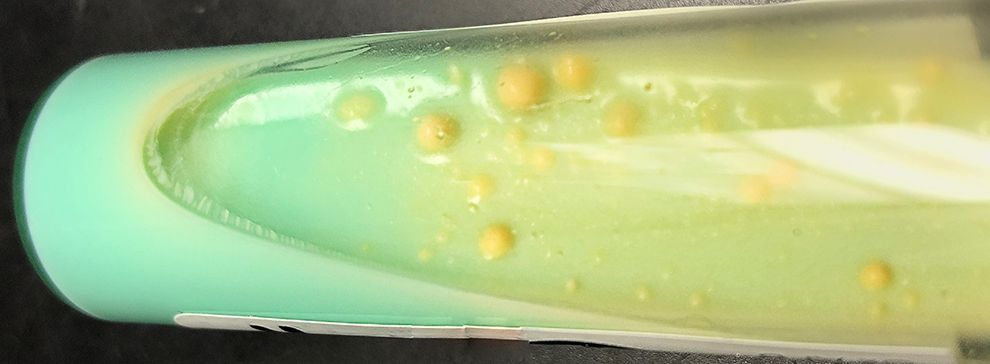
Smooth yellow colonies are seen growing on the Lowenstein Jensen (LJ) slant. This colony morphology is characteristic of certain mycobacteria species.
Questions and Discussion, Part 2
What Is Your Differential Diagnosis Based on the Clinical History and Microbiological Findings?
Given the presence of AFB seen on direct smear, both Nocardia and Mycobacteria species (nontuberculous mycobacteria [NTM] and Tuberculosis (TB)) are on our differential. It’s important to remember that nontuberculous mycobacteria and M. tuberculosis are indistinguishable based on AFB-staining alone. 3 We must utilize molecular testing methods to assist in species identification.
With her history of COPD, a structural lung disease, this is a recognized risk factor for NTM lung disease. 4 Nontuberculous mycobacterial infection is also commonly seen in patients with other structural lung diseases including cystic fibrosis, pulmonary alveolar proteinosis (PAP), bronchiectasis, pneumoconiosis, and prior (treated) TB. 4 -6 Additionally, NTM is more commonly seen in females greater than 50 years of age as is the case with this patient. 4,7
What Points of Her Social History Must We Also Consider and Why?
Her social history includes a period of homelessness. This is a known risk factor for M. tuberculosis infection due to prolonged time spent at homeless shelters, in close proximity with other individuals. 6 This is particularly worrisome in shelters where individuals spend the night because this ensures 8 hours of exposure to airborne pathogens from anyone sharing a room in the shelter. Given this risk factor and the fact that our patient’s sputum is smear-positive, we should isolate the patient in airborne isolation until the species of this bacteria can be ascertained.
This highlights the importance of correlating the history and physical with laboratory findings to determine the likelihood of mycobacterial lung disease. 6,8 For example, chronic smokers should lead us to think more about NTM, and patients with a history of incarceration increase our suspicion for TB. 6 Ultimately, it will come down to laboratory confirmation, but these risk factors from the patient interview can help clue us in to the need for AFB sputum cultures.
What Are the Diagnostic Criteria for Nontuberculous Mycobacterial Lung Diseases?
The minimum evaluation of a patient with suspected NTM lung disease includes:
4
Chest X-ray (CXR) or high-resolution computed tomography (HRCT). The former is only diagnostic if cavitation is seen. If no cavitation is seen on CXR, a HRCT should be used for further investigation. Three or more sputum specimens for AFB stain and culture
2
(Note: One bronchoalveolar lavage or tissue biopsy showing either AFB or granulomatous inflammation can also be used in conjunction with a positive culture to fulfill the microbiological diagnostic requirement.). Exclusion of other lung diagnoses (eg, Tuberculosis
9
or malignancy).
What Diagnostic Tests Are Used to Identify Acid-Fast Bacilli in Specimens?
Direct smear Ziehl-Neelsen—carbol fuchsin, acid alcohol, and methylene blue Kinyoun Stain—same components as the Ziehl-Neelsen, but the Kinyoun stain is a no-heat alternative that utilizes a higher concentration of carbol fuchsin
Fluorochrome technique with semiquantitative analysis (eg, 1+, 2+, 3+, 4+) using either: Auramine-O or Auramine-Rhodamine stain
Culture Techniques
Broth/liquid media
Middlebrook 7H9 broth—supplemented with glycerol, oleic acid, albumin, and dextrose to support the growth of mycobacteria. The 7H9 liquid medium is used in Mycobacteria Growth Indicator Tubes (MGIT) in the BACTEC automated mycobacterial detection system (Becton Dickinson, Sparks, Maryland). The MGIT contains a fluorescent compound that is suppressed in the presence of oxygen. As bacterial growth increases inside the tube, oxygen is consumed and fluorescence increases to a detectable level. The BACTEC MGIT scans tubes every hour for the presence of fluorescence.
Solid media
Lowenstein Jensen slant growth media—contain low levels of penicillin and nalidixic acid which inhibit the growth of gram-positive and gram-negative bacteria, therefore limiting growth primarily to Mycobacteria species.
Tissue Samples
Tissue samples may be obtained (biopsies, resections, etc) via bronchoscopy or open surgical biopsy/resection. The main histologic clue that there may be a mycobacterial infection is the presence of caseating granulomas (Figure 4). Acid-fast bacilli special stain can be used to highlight the organisms (Figure 5). Speciation can then be performed on the formalin-fixed paraffin embedded tissue via the molecular diagnostics outlined below.
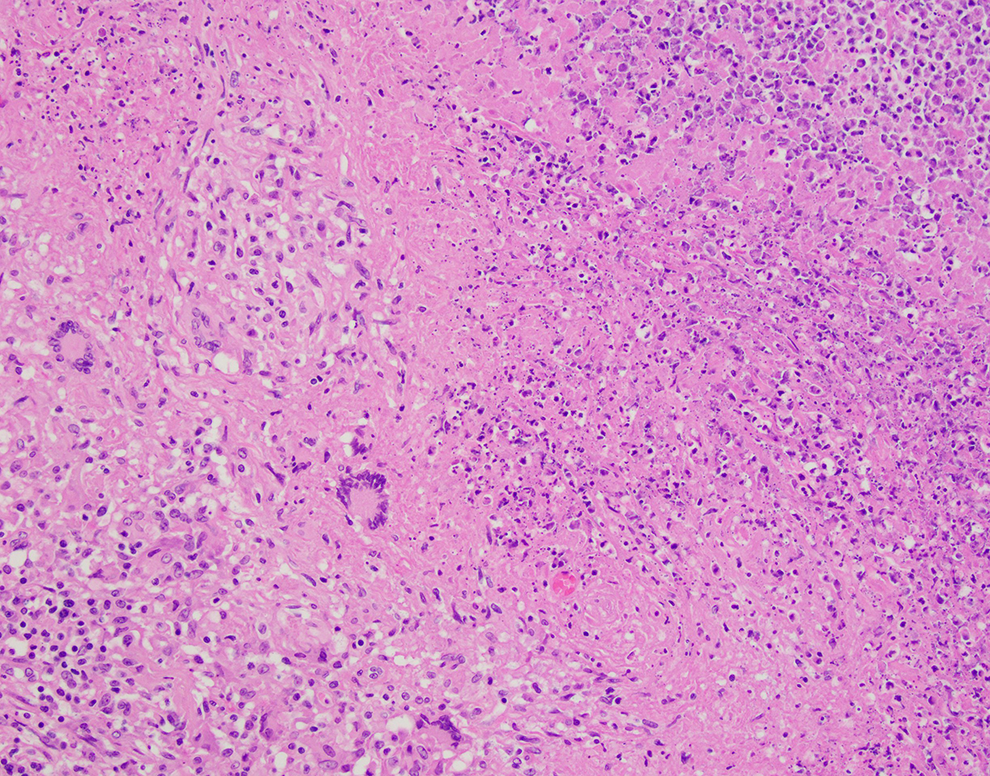
Hematoxylin and eosin (H&E) stain showing granulomatous inflammation including caseation (necrosis) and multinucleated giant cells (×20).
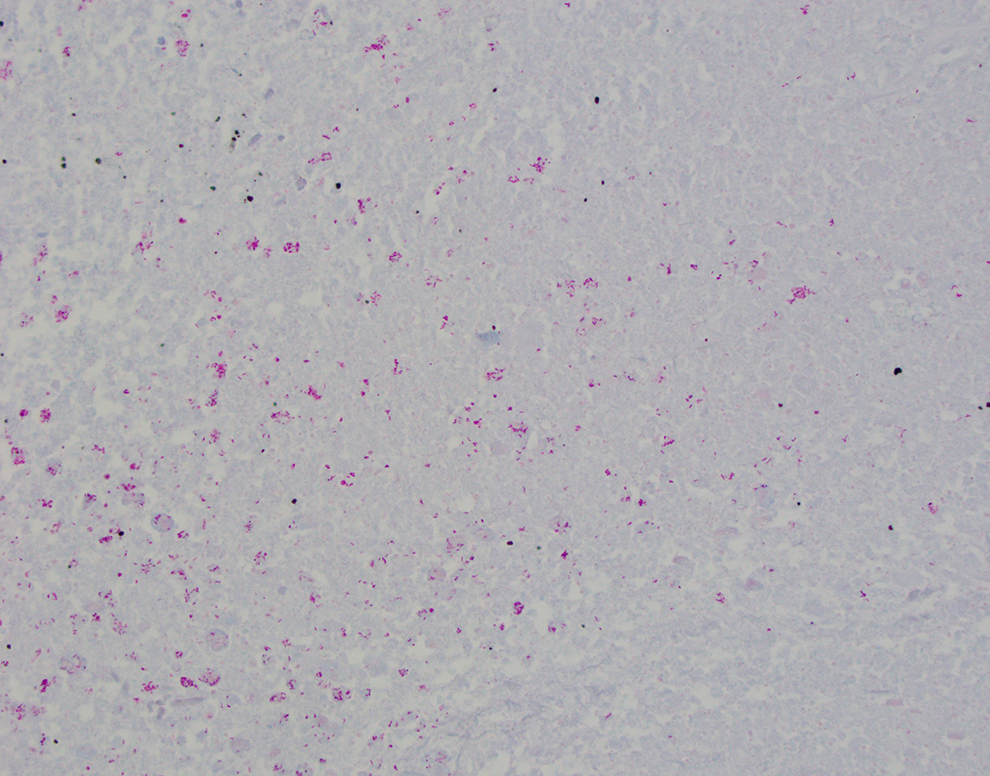
Acid-fast bacilli special stain showing numerous acid-fast organisms (×40).
What Tests Can We Perform to Further Identify the Acid-Fast Bacilli in This Patient’s Sputum? What Diagnostic Tests Are Available for Species Identification of Mycobacteria?
Any of the following molecular tests could be used to further identify the AFB found in this patient’s sputum. The use of these molecular testing methods does not replace the need for AFB smear and culture. 9 The use of one molecular testing system over another will depend primarily on its availability at the treatment facility or at a nearby public health laboratory.
Molecular diagnostics
Cepheid Xpert MTB/RIF is a fully automated nucleic acid amplification test that provides 2-hour detection of M. tuberculosis complex and rifampin resistance mutations (Cepheid Inc, Sunnyvale, California).
The 16S rRNA sequencing—encodes the prokaryotic ribosomal subunit. Variations in the 16S rRNA hypervariable regions A and B can be used to distinguish different mycobacterial species (MicroSeq 500; PE Applied Biosystems, Waltham, Massachusetts). 4
The hsp65-PRA—encodes the 441-base pair sequence of the heat shock protein (hsp65). Using polymerase chain reaction restriction analysis, the length of the restriction fragments can help genotypically identify mycobacteria on a species level.
The rpoB gene sequencing—encodes the beta-subunit of the bacterial RNA polymerase. Sequencing the rpoB gene can be used for phylogenetic tracing of mycobacterial species.
Based on the Results of the Molecular Testing on this Patient’s Sputum, We Learn That She Has a Nontuberculous Mycobacteria. What Public Health Implications Do We Face?
None, actually. Unlike TB, NTM are acquired through environmental exposure, not via person-to-person transmission. 10 They are ubiquitous in the environment and are common in soil and treated water. 11,12 The patient no longer requires airborne isolation.
Would the Public Health Implications Vary If Molecular Testing Revealed M. tuberculosis?
Yes, we would continue to isolate the patient in airborne isolation (or home isolation if outpatient), report the findings to our local health department, and notify the infection prevention department at the facility where the patient is/was being treated. 2,10
Teaching Points
Nontuberculous mycobacteria and TB are indistinguishable based on AFB-staining alone. 3 Additional molecular test methods can assist in species identification.
Multiple risk factors and symptoms must be collected when assessing a patient’s risk for mycobacterial lung disease. 8
A thorough history and physical can help the clinician choose the most appropriate laboratory tests based on the patient’s risk factors and clinical presentation.
Nontuberculous mycobacterial infection is commonly seen in patients with structural lung disease such as COPD, CF, PAP, bronchiectasis, pneumoconiosis, and prior (treated) TB. 4,5
The main histologic clue that there may be a mycobacterial infection is the presence of caseating granulomas (Figure 4).
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The article processing fee for this article was funded by an Open Access Award given by the Society of ‘67, which supports the mission of the Association of Pathology Chairs to produce the next generation of outstanding investigators and educational scholars in the field of pathology. This award helps to promote the publication of high-quality original scholarship in Academic Pathology by authors at an early stage of academic development.
