Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective GT 1.1: Congenital Disorders of the Gut. Discuss the clinicopathological features of tracheoesophageal fistula, pyloric stenosis, intestinal atresia, Meckel diverticulum, and Hirschsprung disease.
Competency 2: Organ System Pathology; Topic GT: Gastrointestinal Tract; Learning Goal 1: Embryology of the Gut.
Patient Presentation
A 36-hour-old male neonate born at 39 weeks’ gestational age to a 35-year-old G5P4004 woman presents from an outside hospital with failure to pass meconium after 24 hours. The pregnancy was without complications and he was delivered spontaneously via vaginal delivery. Family history is unremarkable.
Diagnostic Findings, Part 1
Physical examination shows an alert, active neonate with abdominal distension and hypoactive bowel sounds, a reducible umbilical hernia, and bilateral hydroceles. The anus is patent. Attempts at feeding with formula has caused him to have bilious, nonbloody emesis.
Question/Discussion Points, Part 1
What Is the Differential Diagnosis for an Infant That Fails to Pass Meconium 24 Hours After Birth?
The differential diagnosis for failure to pass meconium includes both small and large bowel obstructive causes. It can be due to structural issues (atresia, malformation, strictures, malrotation, or volvulus), problems with motility (Hirschsprung disease [HD], small left colon syndrome), blockage (meconium plug, meconium ileus due to cystic fibrosis), neonatal medical conditions (hypothyroidism, prematurity), or maternal causes (illicit drug or medication use, maternal infection). 2,3
What Would Be the Next Step in Diagnosis?
The next step in diagnosis would be to obtain imaging, specifically abdominal X-ray and barium enema, to search for anatomical etiologies or for a blockage.
Diagnostic Findings, Part 2
Abdominal X-ray revealed a largely distended, gas-filled intestine with no air in the rectum. Barium enema findings are seen in Figure 1. A suction rectal biopsy is performed, but the specimen was inadequate. An open rectal biopsy was subsequently taken, and representative histologic findings are illustrated in Figure 2.
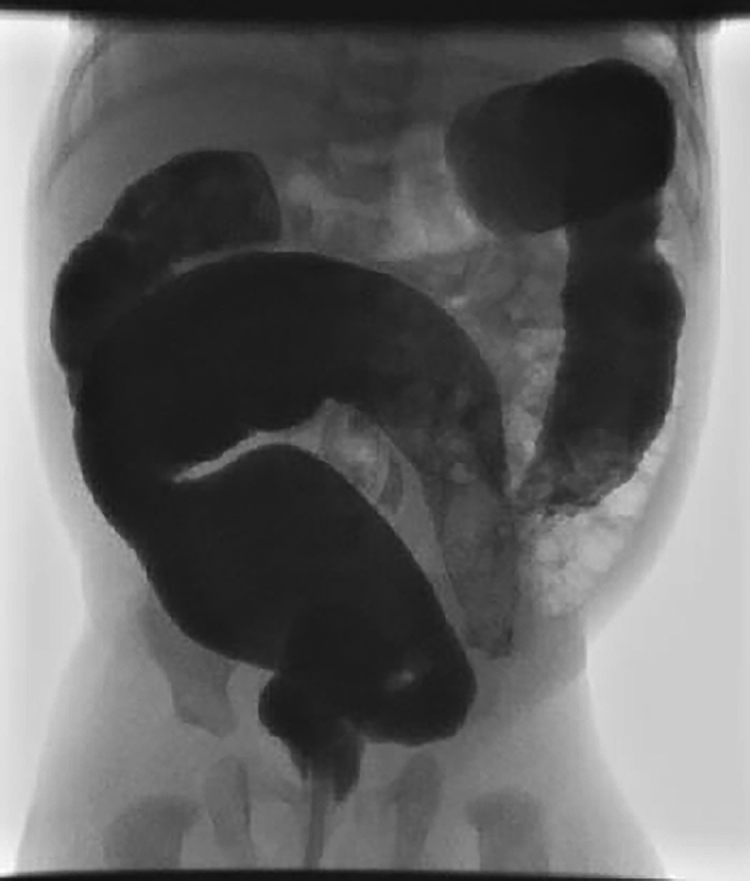
Barium colon enema showing an abnormal rectosigmoid ratio, with dilatation of the proximal sigmoid colon, small caliber rectum, and a transition zone at the rectosigmoid junction.
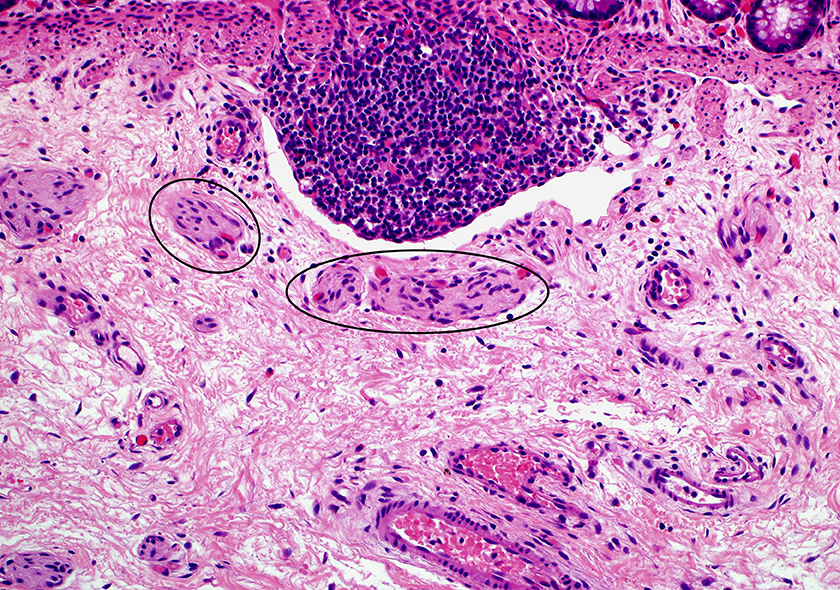
Histological slide showing hypertrophic submucosal nerve fibers (circles) within the abnormally innervated colonic segments. These nerve fibers measure >40 µm in thickness. Note the lack of ganglion cells (×200).
Question/Discussion Points, Part 2
Describe the Radiographic Features in Figure 1
Figure 1 shows dilatation of the proximal sigmoid colon with a small-caliber rectum and a transition point at the rectosigmoid junction.
Describe the Histological Features in Figure 2. What Is This Patient’s Diagnosis?
Figure 2 demonstrates an adequate suction rectal biopsy consisting of mucosa and submucosa. The submucosa contains hypertrophic nerves measuring >40 µm in thickness. No ganglion cells are seen. Examination of multiple levels demonstrated identical findings. The clinical presentation and histologic features are diagnostic of HD.
What Is Hirschsprung Disease and What Is the Pathophysiology Behind the Disease?
Hirschsprung disease is the congenital absence of parasympathetic ganglionic cells within the distal intestine. Part of the enteric nervous system, these ganglia are normally present within the submucosal and myenteric plexuses of the gut, as seen in Figure 3. They are responsible for gut motility through tonic contraction as well as relaxation of the internal rectal sphincter.
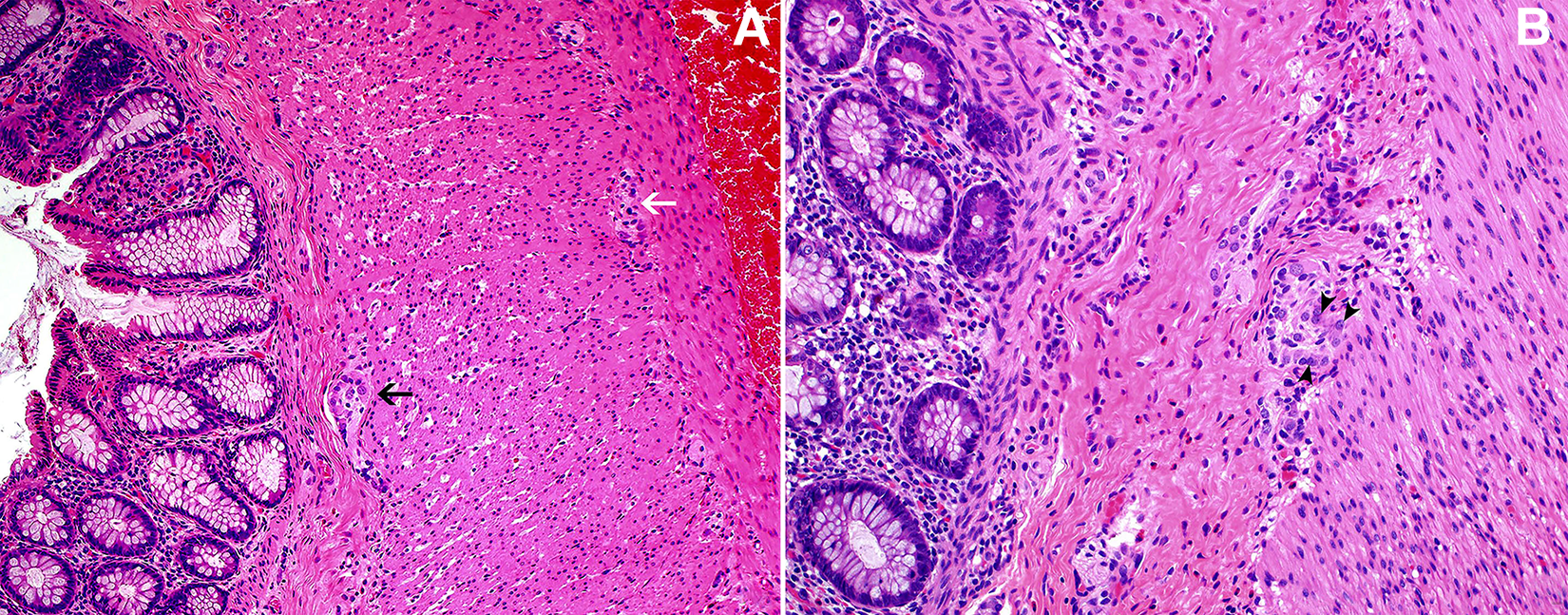
Histological slides from the normally innervated colonic segment. The mucosa, submucosa, and the muscularis propria (including the circular and longitudinal layer) are represented in (A; ×100) The submucosal plexus (black arrow) can be seen within the submucosa, and the myenteric plexus (white arrow) can be found between the circular and longitudinal smooth muscle layer within the muscularis propria. B, A normally innervated submucosal plexus within the colon. Ganglionic cells, which have large, vesicular nuclei and prominent nucleoli, are present (arrowheads; ×200).
Between the 5th and 12th week of gestation, the enteric neural crest cells migrate from the vagal area of the neural crest along the vagal nerves to the mesenchyme of the foregut. They then spread throughout the gut in the craniocaudal direction, innervating the proximal intestine first and rectum last. Interruptions in this process, whether it be through migrational challenges, lack of proliferation or survival, or problems with differentiation, lead to aganglionosis of the gut in a longitudinal manner. As such, the anal sphincter is always involved, with varying degrees of more proximal innervation.
Without ganglion cells, the colonic segments remain in a permanently tonic and contracted state. The internal anal sphincter is unable to relax in response to fecal presence. This leads to a lack of gut motility, stool stasis, and constipation. 4
What Is the Epidemiology and Other Syndromes Associated With the Disease?
Hirschsprung disease affects 1 in 5000 live births. It is divided into 2 types based on the degree of innervation. Short segment, which only affects the rectosigmoid region of the gut, is the most common and is seen in 80% of patients with HD. Long segment, defined as agangliosis extending beyond the sigmoid flexure, is less common, accounting for 10% of cases. Up to 60% of patients with long-segment disease lack ganglion cells throughout the entire colon, which is known as total colonic aganglionosis. Rare cases can involve the distal small bowel as well. 3
Short-segment disease is 2 to 4 times more likely in males than females, though long-segment disease has equal gender ratios. 4 Long-segment disease is also more associated with a familial hereditary pattern; multiple genetic defects have been identified in these patients, most commonly RET mutations. 3
Hirschsprung disease is more often an isolated congenital defect. In 35% of cases, however, other anomalies may be present. Patients with Down syndrome (trisomy 21) are 100 times more likely to have HD than the normal population. 4
Discuss the Different Imaging Modalities for Hirschsprung Disease
Abdominal X-ray, contrast enema, and anorectal manometry can all help raise suspicion for a diagnosis of HD. Abdominal X-ray can show dilated loops of bowel and a lack of stool and gas in the rectum. These findings are nonspecific but can be used to rule out other etiologies of failure to pass meconium.
Contrast enema reveals a dilated proximal colon and a narrow rectum with a cone-shaped transitional zone between the 2 segments. The dilated portion corresponds to the normally innervated colon and the narrowed area is the portion without ganglion cells, which is in a permanent state of contraction. If a transitional zone is present, the positive predictive value for the patient having HD is 100%; the negative predictive value is 60%, especially in infants. 5
Bowel diameters in this area can be used to calculate a “rectosigmoid index.” Hirschsprung disease should be considered if the ratio of the rectal diameter to the sigmoid colon diameter is less than 1 (ie, the sigmoid is larger than the rectum). 3 Retention of more than 50% of the contrast is also helpful for diagnosing HD; lack of any retention rules out the disease. However, the variability of ganglion presence can interfere with the usefulness of contrast enema imaging. Patients with involvement only of the rectum or total colonic aganglionosis may not demonstrate a transitional zone, and a normal-appearing contrast enema does not rule out HD. The sensitivity of this modality overall is 70%. Meconium plugs can cause false positives, and rectal washouts and digital rectal examinations can cause false negatives. 6
Rectal manometry measures the pressure and inhibitory reflex of the internal anal sphincter muscle. In HD, this reflex should be completely absent, with a negative predictive value of 100%. 6 Measurement can take place as early as week 26 of gestation and while under anesthesia, making it useful in uncooperative or very young patients. Its sensitivity and specificity are 90% to 94%, and its accuracy ranges between 75% and 95%. Technical expertise is needed to perform the test, and it is best done in older, more cooperative children. 5
How Else Might Hirschsprung Disease Present, and What Are the Potential Complications of This Disease?
The classic triad of symptoms in HD is abdominal distension, vomiting, and delayed passage of meconium. The latter symptom is seen within 80% to 90% of afflicted patients. 5 The anal sphincter may be tight, and digital examination can lead to an explosive passage of stool.
About one-third of patients can present with enterocolitis. Fecal stasis leads to overgrowth of bacteria and mucosal inflammation, causing explosive diarrhea, abdominal distension, fever, and vomiting, along with leukocytosis. 6 If untreated, perforation of the bowel, septic shock, and death can result. Overall, 18% to 50% of patients with HD develop enterocolitis in their lifetime. 3
Rarely, HD is seen in older children, which manifests as chronic constipation refractory to treatment. Abdominal distension is not present, but the rectum is filled with feces from the anal verge to the perineum. 5
What Is the Gold Standard for Diagnosis of Hirschsprung Disease?
Rectal mucosal biopsy, suction or open, showing aganglionosis is the gold standard for diagnosis. Suction biopsies sample only the submucosal plexus, whereas open biopsies sample both the submucosal and myenteric plexus.
Suction biopsy can be performed at the bedside and should be taken from the posterior wall of the rectum. Below the dentate line, the rectum is physiologically hypoganglionic; therefore, the biopsy site should be at least 2 cm above the dentate line. The presence of squamous or anal transitional epithelium renders the sample inadequate as this means the biopsy was too distal. 7 An adequate biopsy must be at least 3 mm in diameter and the submucosa must be at least one-third of the thickness of the specimen; 8% to 26% of specimens are inadequate, often due to a lack of technical expertise and not applying enough suction. Complications are rare and include bleeding, perforation, and sepsis. These issues are more likely to be seen in younger infants, as their tissues are thinner and easier to damage. 8
Open rectal biopsy may also be performed and are typically taken in older children or when prior suction rectal biopsies have been inadequate. These seromuscular biopsies show aganglionosis in both the submucosal and myenteric plexus.
After receiving the specimen, the tissue is fixed in formalin and embedded in paraffin, forming a block. Slices measuring around 5 µm in thickness are shaved off the block and placed on a glass slide, which is then stained with H&E so histological features can be seen. The number of levels and slides prepared and examined vary from institution to institution. Some practices take slices from every level of the block and scan for the presence of ganglion cells in each slide. Other practices will take 2 representative slices from different depths of the block to assess the plexuses, under the reasoning that the transition from aganglionic to ganglionic segments is continuous. Calretinin staining can be performed for confirmation of aganglionosis within the plexuses and help support the diagnosis of HD.
What Are the Histological Findings and Immunohistochemical Staining Patterns in Hirschsprung Disease?
The diagnostic finding is a lack of ganglionic cells within the myenteric and submucosal plexuses of the colon. The presence of a single ganglion cell excludes the diagnosis of classic HD. Over 90% of patients with Hirschsprung disease also have hypertrophic extrinsic nerve fibers (which are believed to arise from nerve fibers extrinsic to the rectum) within the submucosa; this is less commonly seen in patients with total colonic aganglionosis. These can be highlighted with acetylcholinesterase (AChE), though the utility of this stain is limited to fresh, frozen tissue. Acetylcholinesterase immunohistochemical staining has largely been replaced by calretinin immunohistochemistry, which can be used on tissue that has been fixed in formalin and embedded in paraffin. In normal patients, the enteric neurons within the submucosal and myenteric plexuses, in addition to their nerve fibers within the lamina propria and muscularis mucosae, contain calcium-binding proteins that are highlighted by this stain. A lack of calretinin staining in these plexuses helps support a diagnosis of HD. Both stains can be difficult to interpret or can be falsely negative if within the transitional zone. 7 Figure 4 demonstrates the calretinin staining pattern in a normal bowel; Figure 5 shows the lack of staining for calretinin in a patient with HD.
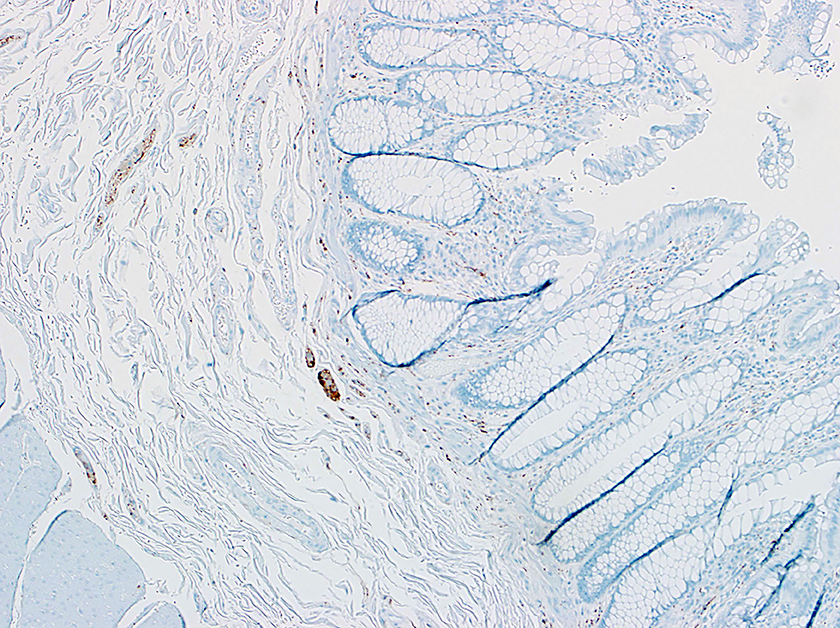
Histological slide of normal colonic segment with immunohistological staining for calretinin. Calretinin immunostain highlights ganglion cells and nerve fibers in the mucosa and muscularis mucosae and submucosa (×100).
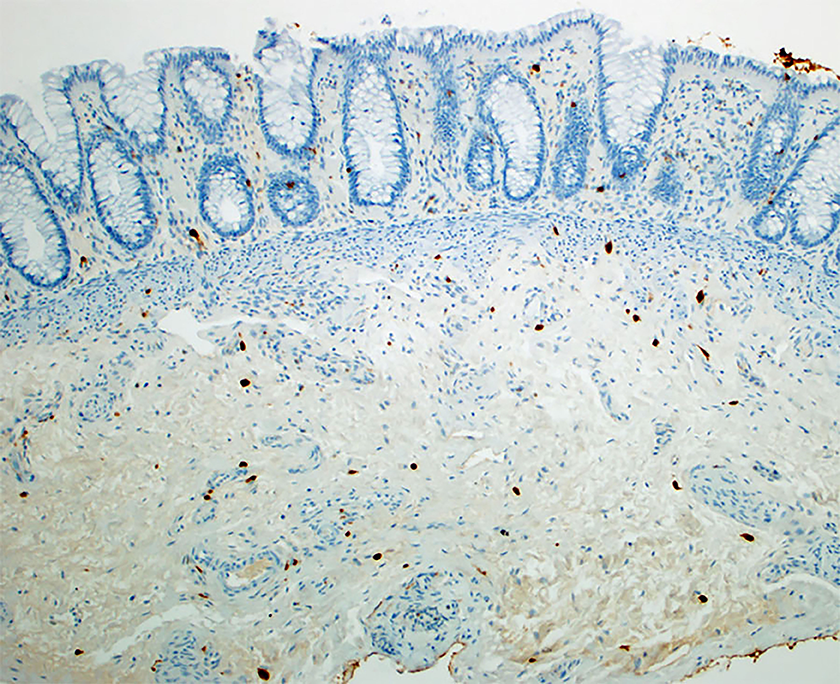
Histological slide of a colonic segment of a patient with Hirschsprung disease (HD) with immunohistological staining for calretinin. There is a lack of ganglion cells within the section, as calretinin confirms. Note that calretinin staining may persist in extrinsic nerves of the submucosa in HD; scattered mast cells can also stain positively, as seen here (×100).
What Is Next in the Management of This Patient?
Surgery is the definitive management for patients with HD. The goal of surgery is to resect the aganglionic part of the colon and connect the innervated part to the rectum to restore function. Prior to surgery, serial rectal irrigations should be performed to help prevent enterocolitis and decompress the bowel.
Intraoperative biopsies of the colon are sent to pathology to be assessed for ganglionic innervation. The goal is to identify both the transitional zone and the unaffected segment with ganglion more proximal to the zone, as that will become the new rectum. Once the normal colonic segment beyond the transitional zone is identified, the surgeon removes the bowel distal to the area and pulls the innervated segment to the dentate line. Anastomosis of the healthy bowel to the rectal tissue proximal to the dentate line is essential to maintain fecal continence and prevent injury to the pelvic nerves and internal anal sphincter. 4,6
A contraindication to immediate surgery is acute enterocolitis. In these patients, a stoma may be formed at the distalmost dilated bowel, and daily rectal washouts are instituted to allow for passage of stool while the patient recovers. Enterocolitis is treated with nasogastric decompression, intravenous fluids, and antibiotics to cover gram-negative bacteria and anaerobes (most commonly metronidazole, with the addition of ampicillin and gentamicin if acutely ill). 3,6 After resolution, the patient may then be scheduled for surgery.
What Are the Postoperative Complications of Hirschsprung Disease, and How Can They Be Treated?
Early postoperative complications include perianal excoriation, fecal soiling, and enterocolitis. The first 2 often resolve over a few months and treatment is primarily symptomatic. Barrier creams can be used for excoriation. Fecal soiling can be from injury to the anal sphincter during surgery, abnormal rectal sensation, or is a result of constipation causing overflow incontinence. Patients should add fiber to the diet and use loperamide or other antidiarrheal pharmacotherapy. Enterocolitis is experienced in 22% to 38% of infants postoperatively and is treated as described in the previous question. 3 There should be high suspicion for the disease even years after surgical treatment. 9
Long-term complications are experienced by 60% of patients, with 10% needing further surgery or a colostomy after initial treatment. The most common complication is constipation, the etiology of which is many and varied, ranging from stricture, to residual or recurrent aganglionosis, to anal sphincter achalasia. Strictures can be from leakage of the anastomosis or stenosis of the rectal cuff and is usually treated by daily or weekly anal dilation, performed by the parents or in the office setting. Supportive care in the form of increased fiber, laxatives, and oral hydration is also instituted. Repetition of the pull-through surgery or permanent colostomy can be used to treat recurrent or residual aganglionosis. Anal sphincter achalasia can be treated with Botox injections, topical nitrous oxide applications, or posterior myomectomy. Fecal soiling may also be a long-term complication and often requires bowel management routines and possible permanent colostomy on top of the previously described treatments to manage. 6
Teaching Points
Failure to pass meconium within 24 hours can be due to structural issues, motility problems, blockage, or maternal or neonatal medical conditions.
Hirschsprung disease is the congenital absence of parasympathetic ganglionic cells due to the failure of the migrating enteric neurons to migrate during development.
Short-segment HD is the most common form and only affects the rectosigmoid gut region. Long-segment HD has aganglionosis of the bowel beyond the sigmoid flexure.
Hirschsprung disease has an incidence of 1:5000 and is seen more often in patients with trisomy 21 (Down syndrome).
Most patients present with abdominal distension, vomiting, and delayed passage of meconium. The anus is often tight with explosive passage of stool on digital examination.
Abdominal X-ray, contrast enema, and rectal manometry are the most common imaging modalities for HD. Contrast enema shows a dilated proximal colon, narrow rectum, and cone-shaped transitional zone. Rectal manometry shows an absence of the internal anal sphincter inhibitory reflex.
Rectal mucosal biopsy is the gold standard for diagnosis. Biopsies should be taken at least 2 cm above the dentate line.
Histologically, a lack of ganglion cells within the myenteric and submucosal plexuses of the colon is seen. Hypertrophy of nerve fibers is often present, which can be highlighted with AChE staining. Calretinin staining is often negative within the muscularis mucosae plexuses.
Definitive management for the disease is surgery, using the “pull-through” method.
One complication of HD is enterocolitis, which presents with explosive diarrhea, distension of the abdomen, fever, vomiting, and leukocytosis; this is a contraindication to surgical management.
Treatment of enterocolitis includes nasogastric decompression, intravenous fluids, and antibiotics (metronidazole ± ampicillin and gentamicin).
The clinician should be aware that enterocolitis may also be seen after corrective surgery in patients with Hirschsprung disease.
Early postoperative complications include perianal excoriation, fecal soiling, and enterocolitis and are managed symptomatically. Long-term complications include constipation and fecal soiling. A small percentage of patients require further surgery or permanent colostomy formation.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The article processing fee for this article was funded by an Open Access Award given by the Society of ’67, which supports the mission of the Association of Pathology Chairs to produce the next generation of outstanding investigators and educational scholars in the field of pathology. This award helps to promote the publication of high-quality original scholarship in Academic Pathology by authors at an early stage of academic development.
