Abstract
With the changing landscape of medicine in general, and pathology in particular, a greater emphasis is being placed on laboratory management as a means of controlling spiraling medical costs and improving health-care efficiency. To meet this challenge, pathology residency programs have begun to incorporate formal laboratory management training into their curricula, using institutional curricula and/or online laboratory management courses offered by professional organizations. At the University of Utah, and its affiliated national reference laboratory, ARUP Laboratories, Inc, interested residents are able to supplement the departmental lecture-based and online laboratory management curriculum by participating in assistant medical directorship programs in one of several pathology subspecialty disciplines. The goals of many of the assistant medical directorship positions include the development of laboratory management skills and competencies. A survey of current and recent assistant medical directorship participants revealed that the assistant medical directorship program serves as an excellent means of improving laboratory management skills, as well as improving performance as a fellow and practicing pathologist.
Introduction
In the rapidly changing field of health care, the scope of practice of new-age pathologists is rapidly expanding. New-in-practice pathologists are required not only to have pathology diagnostic skills and clinical knowledge but to possess laboratory management skills and serve as leaders and stewards of clinical laboratory utilization. 1 –3 Although the skills needed to become a diligent laboratory manager and an effective laboratory leader have been continuously stressed as essential for pathologists in a wide body of literature for almost 25 years, practicing pathologists and prospective employers continuously cite this as the area with the lowest trainee preparation rating. 2,4 –7 In a 2005 survey performed under the auspices of the College of American Pathologists (CAP), it was noted that one-third of recent hires were only somewhat or slightly prepared to enter practice. 6 Common categories of deficiencies noted by respondents included skills in management, interpersonal interactions, regulatory and compliance issues, and billing and reimbursement procedures. Skills such as clinical knowledge, laboratory management, clinical consultation, and informatics were often cited as essential skills required for a community pathologist; however, with the shift toward a more “value-based” health-care system, a focus on more concrete skills has emerged. 8,9 These skills now include test selection strategies and utilization management techniques, knowledge of quality assurance procedures and inspection processes, and strategic laboratory planning including budgeting, personnel management, coding, billing, revenue collection, and contract negotiations. 9 –11
A significant impetus to create lasting and effective changes to residency training program curricula was initiated when, in 2013, after several years of planning, the Accreditation Council for Graduate Medical Education (ACGME) introduced the Next Accreditation System (NAS) for use in all residency programs. The ACGME is the regulatory body that oversees US residency education in all disciplines and, as part of the NAS, designed educational outcomes termed “milestones” in all specialties to assess and provide feedback on resident progress in many areas of competence. Pathology milestones, designed by a pathology working group, were developed to provide uniform training goals for pathology residents. 12 These include many areas of evaluation in laboratory administration and management, in addition to the baseline competencies that residency programs traditionally focus on (patient care, medical knowledge, practice-based learning and improvement, interpersonal and communication skills, professionalism [PROF], and systems-based practice [SBP]). 13
In this study, we describe a program used at the University of Utah to give interested residents the opportunity to engage in assistant medical directorships (AMDs) with an emphasis on augmenting the laboratory management training included in the residency training program, and we also present the results of a survey of current and recent participants in the AMD program.
Methods
Description of the Assistant Medical Directorship Program
The AMD Program in the University of Utah’s Department of Pathology and its ARUP Laboratories is designed as an elective longitudinal experience generally occupying 12 months during which the trainee functions as an apprentice medical director in one of a number of different subspecialty areas. The elective involves work in addition to the core training activities and is thus considered “moonlighting” for the purposes of ACGME time keeping.
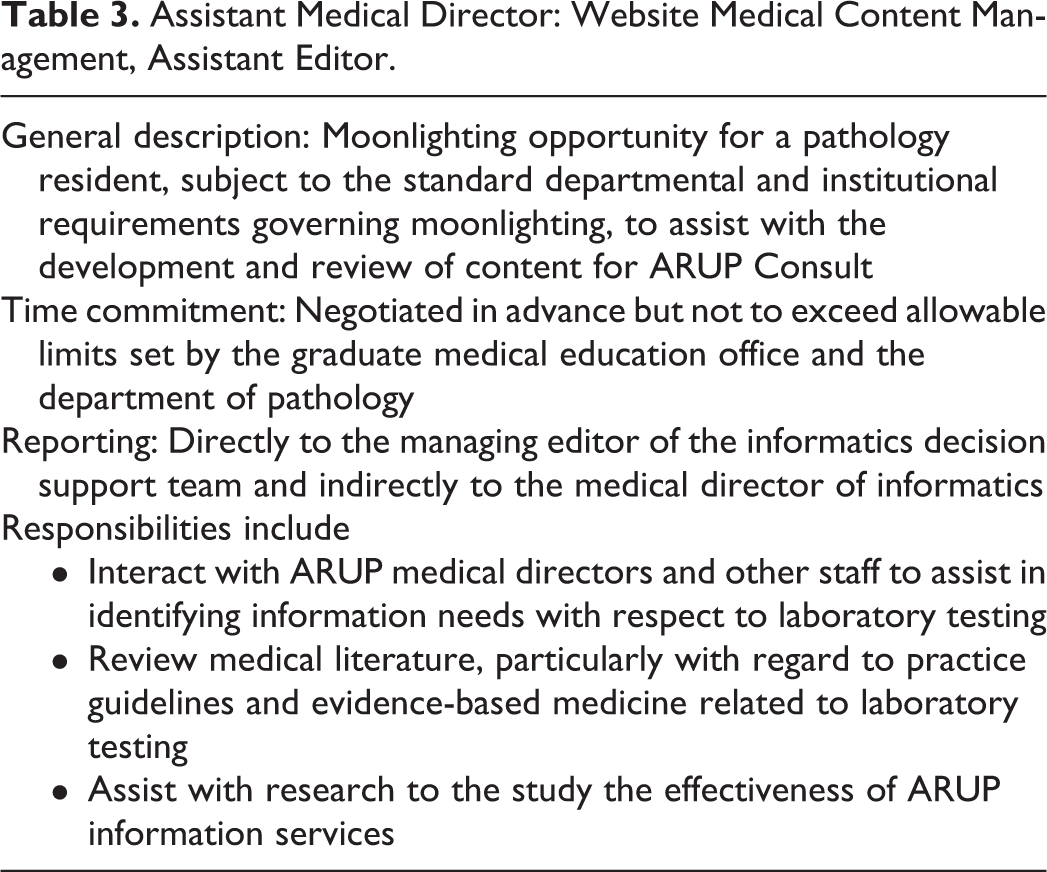
The AMD activities available to interested and qualified residents at the University of Utah are listed in Table 1. Descriptions of several representative examples are found in Tables 2 to 8. Four of these AMD assignments are based on the subspecialty disciplines of clinical chemistry, surgical pathology, and transfusion medicine and have a strong quality assurance theme in their list of responsibilities (see Tables 4 –6 and 8). Two AMDs in informatics (Tables 2 and 3) afford opportunities to participate primarily in postanalytic activities, including the development of enhanced laboratory result reports, laboratory utilization management, and knowledge content development to aid laboratory users, particularly health-care providers, in more informed use of laboratory services. Given the growing interest in and use of digital imaging in pathology, the digital pathology AMD activities involve the resident in projects directed at integrating digital imaging into educational activities as well as process workflow improvements and patient-directed uses. The AMD in hematologic flow cytometry affords the resident the opportunity to participate in graduated responsibilities in clinical service. Here, the AMD integrates into the weekend (generally every fourth weekend, Saturday and Sunday) sign-out schedule with the fellows in hematopathology in their support of the attending hematopathologist who covers that weekend. The anatomic pathology (AP) slide photographer for outside departments is uniquely different from the other AMD assignments in that it was designed to fill the need in meeting slide photography requests from outside the department of pathology, particularly from faculty and house staff from other clinical departments. The assistant medical director reviews these requests, clarifies their purpose (eg, for publication or lectures), and provides the photographs to the requestors. For photography not related to publication, requestors are charged a fee for each photography session prior to release of the photographs. If intended for publication, the resident will ask to be included on the manuscript as the pathologist-of-record with appropriate content review responsibilities. In doing so, the requestor is provided the photographs at no fee, and the resident becomes a cited author on the manuscript. Of note, a number of AMD positions stress the management competencies outlined in phase II of the NAS inspection program of the ACGME. 13 Examples of multiple milestones and management competencies that map to the AMD assignments in the automated core laboratory, endocrinology laboratory, and surgical pathology in our program are described in Table 9.
Available Assistant Medical Directorships (AMD).

Assistant Medical Director (AMD), Informatics.

Assistant Medical Director: Website Medical Content Management, Assistant Editor.

Assistant Medical Director, Automated Core Laboratory.

Abbreviations: CAP, College of American Pathologist; QA, quality assurance; QC, quality control.
Assistant Medical Director, Endocrinology Laboratory.

Abbreviations: CAP, College of American Pathologist; QA, quality assurance; QC, quality control.
Assistant Medical Director, Surgical Pathology.

Abbreviation: QA, quality assurance.
Assistant Medical Director, Digital Pathology.

Assistant Medical Director, Transfusion Services.

Abbreviation: FDA, Food and Drug Administration; QA, quality assurance.
Examples of Pathology Milestones and Competencies Addressed in Assistant Medical Directorships.
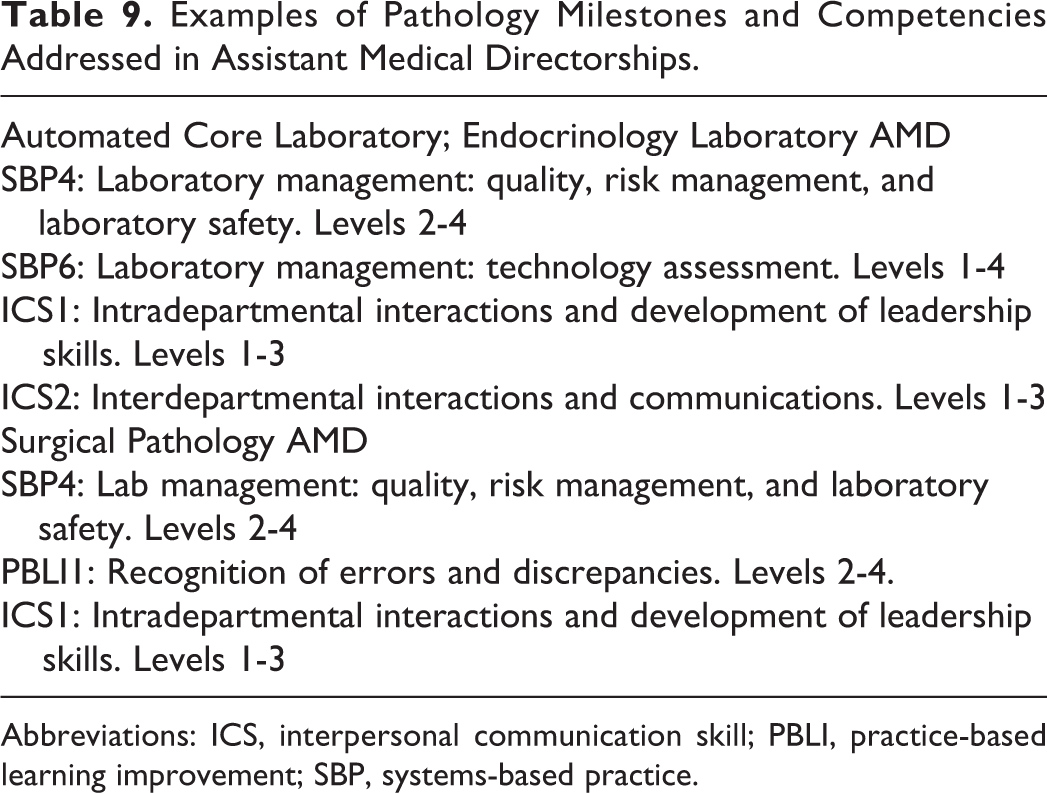
Abbreviations: ICS, interpersonal communication skill; PBLI, practice-based learning improvement; SBP, systems-based practice.
Moonlighting Status and Compensation
Assistant medical directorships are considered to be moonlighting activities by the graduate medical education (GME) office. Moonlighting is considered patient care activities external to the educational program that residents engage in at sites used by the educational program and other health sites. As such, residents must have permission to participate from both the relevant medical director and the residency program director. They must also have a valid Utah medical license. Moonlighting activities cannot take place while the residents are on call, must be entered into the E*Value tracking system, and must count toward the duty hour limitations of the ACGME and participating institution. The length of moonlighting activities, including the AMD, usually runs on the academic year calendar, but shorter time intervals can be considered. Each new resident participating in an AMD must complete the Moonlighting Authorization Form for the GME office and the department of pathology.
Compensation for these AMD activities falls under the guidelines of the GME office and the department of pathology. Specific compensation is determined by the responsible faculty member and may be provided on a continuous or as-needed basis. Rates include those on a per-request basis (photography, US$30 per request), an hourly basis (US$40/hour for the informatics AMD duties), or on a fixed basis per pay period (range: US$165-US$375/pay period).
Survey of Previous Assistant Medical Directors
We contacted 39 former residents who served in AMDs at the University of Utah and ARUP Laboratories, Inc, over the past 10 years. We surveyed them (Table 10) regarding their experience in an AMD and the impact that the AMD program had on their practice of pathology, with an eye toward using their feedback to improve the experience for future AMDs and to describe their collective experience for others in academic pathology.
Survey of Previous Assistant Medical Directors.

Abbreviations: PGY, postgraduate year; RISE, Residency In-Service Examination.
We queried the former assistant medical directors regarding their experience in AMDs, whether the AMD helped them secure a fellowship or attending pathologist position, whether the AMD prepared them for the laboratory management portion of in-service and board examinations, and whether the position prepared them to perform their duties as fellows and practicing pathologists. We also asked the former assistant medical directors to assess the perceived influence that their participation in an AMD had on those interviewing them for fellowship and practice positions and the perceived role the AMD played in them acquiring these positions.
Results
Of the 39 former assistant medical directors contacted, 23 replied for a response rate of 59.0%. The most common AMDs were hematologic flow cytometry (7 respondents) and AP (6 respondents). Four respondents had served in AMDs in the automated core laboratory and 3 each had served in AMDs in informatics and transfusion services. Fewer respondents served in AMDs in slide photography (2), infectious disease laboratory (1 and no longer offered), and website medical content management (1). Most respondents served in AMDs during their third year of residency (19 of 23, 83%), although some served during their fourth (15 of 23, 65%) and second years (3 of 23, 13%). More than half (13 of 23, 56%) of the respondents had served in AMDs during more than 1 year of residency, most commonly during both their third and fourth years. Although most of these respondents served in the same AMD during both years, there were 3 respondents who served in different AMDs during the course of their residencies.
We asked the former assistant medical directors about how their experience prepared them for their future roles as fellows and practicing pathologists. More than two-thirds (18 of 22, 82%) of the respondents were satisfied or very satisfied that the goals of their AMD had been achieved, and a similar number (18 of 23, 78%) felt that the AMD improved their management skills. Despite the fact that most respondents felt that serving in an AMD improved their management skills, a minority (approximately one-third) felt that the experience helped prepare them for the laboratory management portions of American Society for Clinical Pathology (ASCP) Residency In-Service Examination (RISE) and board examinations (Table 11).
AMD Survey Results.
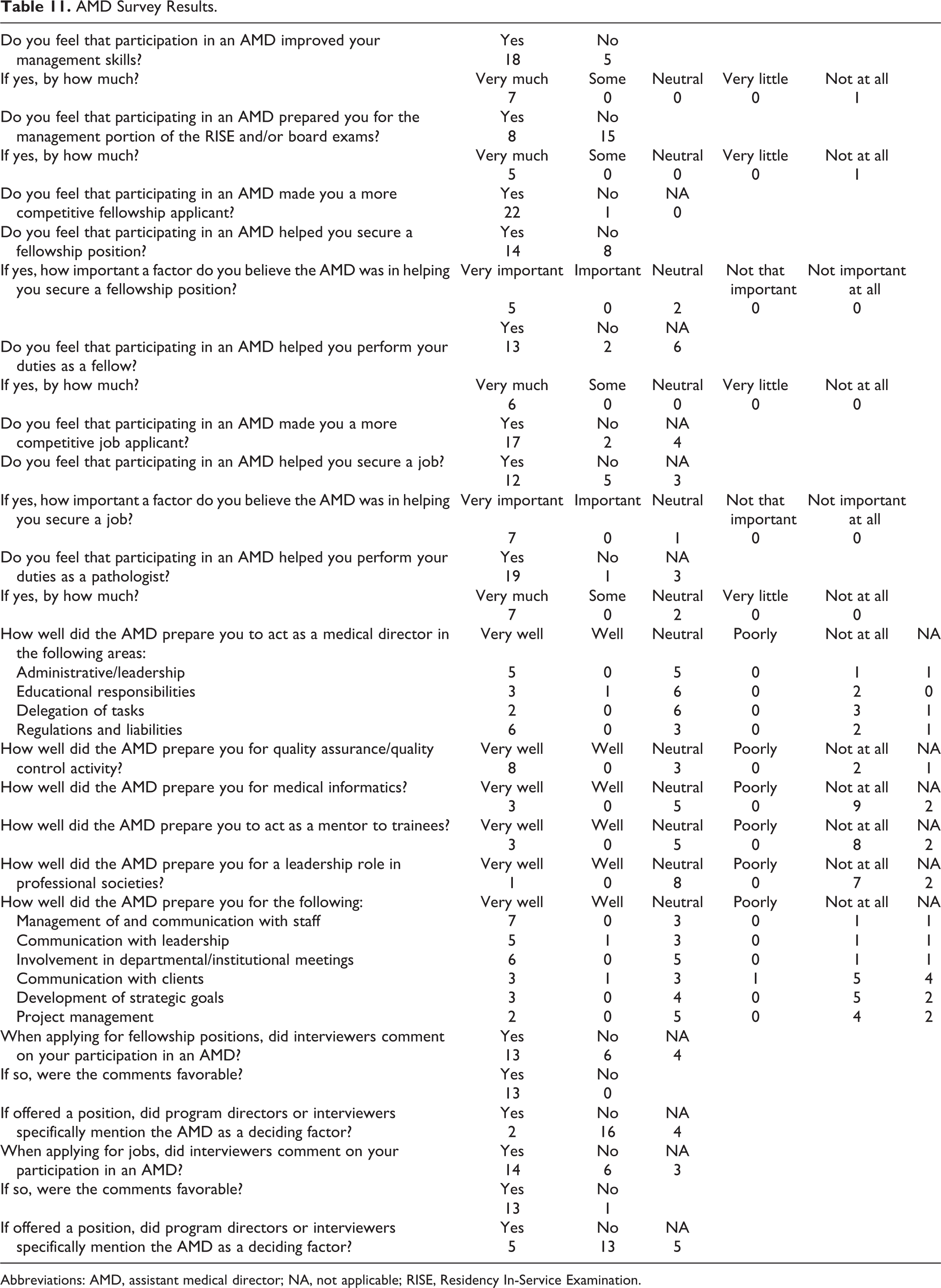
Abbreviations: AMD, assistant medical director; NA, not applicable; RISE, Residency In-Service Examination.
There was almost universal agreement among former assistant medical directors that their experience made them more competitive fellowship and job applicants (Table 11). Respondents felt that the AMD was an important to very important factor in helping them secure fellowship and practicing pathologist positions. Similarly, the majority of respondents felt that the AMD experience was helpful in allowing them to perform their duties as fellows and practicing pathologists. Areas in which the AMDs were rated as deficient included preparation for leadership roles in professional societies, preparation for acting as a mentor to trainees, and, for those residents who did not participate in the informatics AMD, preparation for medical informatics duties.
Finally, the majority of respondents noted that fellowship program directors and job interviewers commented favorably on their participation in an AMD (Table 11). Although most respondents reported that participation was rarely a deciding factor in being offered a position, 2 respondents reported that their participation in an AMD was mentioned by fellowship program interviewers as a deciding factor in being offered a position and more than a quarter of former AMDs reported that their participation in an AMD was mentioned by job interviewers as a deciding factor in being offered a position.
Discussion
Having identified laboratory management and leadership skills as a necessary, but a generally deficient, aspect of residency training, numerous strategies arose to introduce laboratory management curricula into residency training programs. 14 –16 These strategies ranged from informal interactions with laboratory medical directors during required rotations to formal management courses. Approaches included management rotations, lectures from laboratory managers and business people, assigned textbook and procedure manual reading assignments, and formal examinations. Other programs chose to use more involved methods such as requiring trainees to participate in laboratory management research and/or quality improvement projects, participation in laboratory inspections, or shadowing medical directors or laboratory managers during some or all of their daily activities.
In addition to institution-specific training programs, several tools are currently available to encourage the use of a more standardized curriculum approach to laboratory management. 17 In 2013, the ASCP and the American Pathology Foundation introduced Laboratory Management University (LMU), a successful, self-paced certificate program wherein participants learn practical laboratory management and leadership skills through a series of online modules and quizzes. 18 The LMU is now used in a number of pathology residency training programs, including our own, to supplement instruction and firsthand experience in laboratory management techniques. The American Association for Clinical Chemistry also offers an online certificate program in laboratory management. 19 These programs allow laboratories and training programs (in clinical laboratory sciences and pathology) to tailor the courses to their needs. The College of American Pathologists offers the Clinical Pathology Improvement Program, which teaches the principles of laboratory management through 12 involved case studies. 20
Beyond training in the fundamentals of laboratory management, pathology residency programs can also use graduated responsibility to reinforce these knowledge and skill sets. Mentor-based teaching is a cornerstone of clinical medicine and surgery, with bedside rounds and participation in surgical cases a staple in medical student rotations and medical/surgical residencies. However, students entering residencies in pathology often fall into a passive learning style with diminished clinical responsibilities and patient contact. 2 Passive training environments can lead participants to lack confidence, diminish their expertise, and affect their lifelong learning skills. Well-designed graduated responsibility systems can do much to counter these difficulties. However, graduated responsibility is often difficult to achieve in pathology residency programs, given restrictions on billing as well as ACGME rules and regulations regarding supervision. All resident activities relating to patient care must ultimately be reviewed by attending faculty, lessening the ability of pathology residents to engage in decision-making.
Pathology faculty in academic institutions should continue to seek opportunities for residents to take responsibility for diagnostic decisions with progressively less oversight. 21 Rotations in specific laboratories should emphasize graduated responsibility for clinical consultations and interpretation of unusual results, with residents serving as junior practitioners. Pathology residents should have the opportunity to both see and practice the application of management principles they learn. 10
Creating graduated responsibility opportunities for pathology residents is an important means to augment more traditional approaches to knowledge and skills development in AP and clinical pathology (CP). 21 This includes clinical laboratory management training. As our health-care delivery system undergoes medical, technological, and structure changes, pathologists new to practice are in a better position to enter practice with necessary knowledge and skill sets for all aspects of their practice and better prepared to meet the challenges of future medical practice. With laboratory management, in particular, a recent workforce analysis by the CAP presented survey data that showed that 44% of pathologists younger than 40 years and 32% of those older than that “expect to devote more of their time to medical direction of clinical laboratories in the immediate future.” 22
With this view in mind, our training program has combined formal, didactic training in laboratory management with optional opportunities to function as “assistant medical directors” in very specific disciplines and under the guidance/mentorship of the faculty medical directors. Though viewed as moonlighting by the GME office, as the experience is not part of the formal residency curriculum, an assistant medical directorship is, nevertheless, an educational as well as a service opportunity.
In order to assess the perceived value of an AMD opportunity, a survey was conducted with 39 former graduates of the University of Utah Department of Pathology residency training program who had served in AMD’s during their training. Feedback was sought on both the experience itself and the perceived impact that it had on their subsequent employment and practice. With a response rate of 59% (23 of 39), most respondents served in AMDs during their third or fourth year of training, with some doing so for both years. A few also served in more than 1 AMD capacity. Eighteen (82%) of 22 respondents were satisfied with the experience and with the achievement of the position’s goals. Seventy-eight percent (18 of 23 respondents) felt that the experience improved their overall management skills. Not unlike the conclusions of other authors, management training and experience (including the AMD) did not necessarily result in perceived improvements in our resident scores on the ASCP’s RISE or prepare them for laboratory management questions on subsequent board examinations. The RISE for its first 20 years of use focused on both resident self-assessment and residency program evaluation. 23 With introduction of the ACGME’s Outcome Project in 2000, the RISE was refocused on residency program accomplishments. A review of the mean increase in RISE scores by topic from the first to the last year of residency revealed that laboratory administration scores showed the lowest level of mean increase (49.8%) for all topics examined (all topic range: 49.8%-114%).
In today’s competitive job market, prospective employers may view residents and fellows who have had significant graduated responsibility during their training as having more favorable medical knowledge and interpersonal skills than those who have not. 6,21 This may be particularly important for those jobs where the practicing pathologist will need demonstrated skills in laboratory test utilization management or digital imaging, for example. Residency training programs have for years employed a variety of approaches to meeting these training needs in management knowledge and skills. 10,14-15,24 Techniques range from didactic lectures, to commercially available curricula like the LMU, to mandatory rotations in management. In 1 example of the latter approach, the Department of Pathology of Hofstra Northwell School of Medicine combines observational and active participation into a 1-month rotation. 25 The authors describe a rotation in which residents are not only exposed to departmental leaders and managers in real-time management situations but are required to engage in a project of strategic value to the department and its role in the health system. In this form of graduated responsibility, the majority of the residents surveyed felt that the experience enabled them to compete successfully for fellowships and their first employment.
In addition to improving their laboratory management skills, nearly all of the respondents to our survey indicated that participation in the University of Utah AMD program made them more competitive for fellowships or jobs. More than two-thirds noted that fellowship program directors and prospective employers commented favorably on their participation in an AMD during their training. While only 2 respondents noted that the AMD was a deciding factor in being offered a fellowship position, 28% (five of 13) of respondents were told that the AMD was described as a deciding factor in the offer of a job. Although not an overwhelming endorsement of the value of the AMD-graduated responsibility opportunity by future employers, the fact that it was considered favorably by some of them during the application process is noteworthy and encourages support for the program.
Finally, many respondents felt that the AMD experience improved their ability to perform their duties as fellows or practicing pathologists. The experience was credited with helping to prepare them for administrative responsibilities and leadership roles, to improve their interpersonal skills and their understanding of regulatory requirements in the laboratory, and to perform quality assurance activities in the laboratory. Opportunities for the design of future AMD experiences that respondents cited included a lack of adequate preparation for leadership roles in professional societies, a lack of focus on mentorship of others, and a lack of preparation for the needs of medical informatics duties.
In 2014, pathology joined other residency specialties in phase II of the NAS inspection program of the ACGME. 13 The NAS includes 27 pathology milestones in AP and CP residency training. Included in these are 7 SBP milestones directly related to patient safety management, laboratory management, and informatics (SBP1-SBP7). Additionally, there are several related milestones in practice-based learning improvement (PBLI), PROF, and interpersonal communication skills (ICSs) that share some management-related knowledge and skill sets in error and discrepancy assessment (PBLI1), behavior (PROF2), performance feedback (PROF4), leadership skills (ICS1), and interdepartmental and team interactions (ICS2). Milestone levels 1 to 3 competencies generally focus on knowledge acquisition and understanding, whereas levels 4 and 5 require skill demonstrations. Over the course of one’s residency, graduated responsibility should help to foster solid levels 4 and 5 competencies. 13 As mentioned previously, a number of the AMD positions, notably those in the automated core laboratory, the endocrinology laboratory, and surgical pathology, emphasize management competencies that correspond to ACGME milestones (Table 9).
Conclusion
This article has described an innovative program that partially addresses the need for improved pathology residency education in laboratory management skills. The University of Utah Assistant Medical Directorship Program at ARUP Laboratories offers a unique experience for residents to gain skills in quality assurance techniques, personnel management, interdepartmental communication, test management, informatics, administrative experience, and laboratory utilization. The acquisition of these skills is thought to better prepare pathologists in training to enter the workforce by reinforcing subjects felt by the practitioners in many pathology groups to be lacking. Pathology residency programs are encouraged to incorporate some of these methodologies into their curriculum to augment their education in laboratory management.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
