Abstract
Active learning strategies such as case studies, simulations, and role-playing offer powerful tools for preparing public health students to think critically, collaborate effectively, and engage meaningfully with real-world challenges, thereby equipping them for their day-to-day roles as public health practitioners and scholars. However, the examples of active learning approaches remain limited. In this article, we present five structured active learning strategies drawn from graduate public health courses to illustrate how professors of public health utilize case studies, role-plays, and simulations to promote practice-based active learning. First, we describe a town hall role-playing simulation on HPV vaccination policy in schools. Second, we describe a tabletop exercise on disaster preparedness and emergency management. Third, we describe how to use case studies on current infectious disease outbreaks as learning tools. Fourth, we highlight a simulation on global health leadership during an infectious disease outbreak. Finally, we discuss a simulation exercise that prepares students for NIH grant reviews and the process of scientific publishing. To ensure these serve as replicable teaching tools for faculty, we provide descriptions of the exercises, along with learning objectives, a description of the instructor’s role, and an evaluation methodology. This information is further accompanied by practical guidance for implementation. Through these examples, we illustrate how active learning can transform traditional dyadic education into a dynamic, practice-oriented experience that prepares students for future professional challenges.
Introduction
Active learning is a student-centered teaching approach that actively engages students in the learning process rather than expecting them to passively absorb information from lectures (Prince, 2004; Yeatts, 2014). The incorporation of active learning in higher education can be an important part of training for health professionals (Kleinbaum, 2019). For example, the use of real or hypothetical cases simulating real-life scenarios, guided by an instructor, presents complex problems that do not have a clear-cut single answer. Students typically work in groups on the scenario to identify possible solutions. In engaging with the process of developing solutions to pressing and timely public health issues, case-based learning fosters the application of theoretical concepts to bridge the gap between theory and practice, offering the opportunity for students to translate what they have learned in the classroom into practical applications relevant to their current and future jobs (Leon et al., 2015). Cased-based learning is used to foster the application of prior knowledge to authentic scenarios and can be used along with lectures, labs, readings, and other instructional methods to ensure students see the relevance to real life and their future careers (Freedman et al., 2012; McLean, 2016). Equally critical to note is that students overwhelmingly enjoy a case-based learning approach (Thistlethwaite et al., 2012), which can, arguably, help promote a more engaged learning experience; hence, integrating joy—an undervalued but critical aspect of inclusive learning (Cronqvist, 2024)—as an intentional pedagogical value while teaching practical, real-world skills (Thistlethwaite et al., 2012).
Along with case studies, role-playing and simulations are forms of experiential learning that can be powerful active learning tools in the classroom (Barrera et al., 2021; Rao & Stupans, 2012). In role plays and simulations, students assume a role, a character, or a function within a group. Role plays, and simulations aim to authentically emulate a given environment or challenge, giving students the chance to “try out” their role and behave as their character—such as policy analysts or public health decision-makers—would in real life.
These types of experiences have many benefits for student learning. They allow students the opportunity to be immersed in the “real-world” contexts and to apply foundational knowledge in low-stakes environments, allowing them to hone their skills without the high-pressure demands of professional practice (Greece et al., 2015). They can also enhance retention of the material and heighten students’ interest and motivation to learn by linking activities to current relevance and skills, as well as situations that they may face in their future careers (Davis & Wilcock, 2003). The use of inquiry-based learning methods and guided inquiry promotes higher levels of thinking (Chong et al., 2022; Davis & Wilcock, 2003; Lee, 2012; McLean, 2016; Thistlethwaite et al., 2012). For example, engaging in a decision-making process through case studies enables them to grapple with actual challenges where evidence-based reasoning must coexist with cultural sensitivity and account for public trust, engagement, and consensus. Role plays and simulations can positively impact students’ learning by allowing students to view a different perspective in a safe but challenging environment, as well as practice skills that they may need in their future careers (UNSW, 2024). These experiences also foster critical thinking and problem-solving skills as well as encourage teamwork, advocacy, leadership, and effective communication (Owa, 2024; Williams, 2005).
Beyond these transferrable skills, active learning as a teaching tool can be applied in a wide range of subject areas such as public health, community-based participatory research (Reinschmidt et al., 2019), health literacy (Devraj et al., 2010), and infectious diseases modeling (Willem et al., 2014), to name a few. Furthermore, McLean’s (2016) review of 70 articles from around the world relating to the use of case-based learning in medicine found that it has been used at various levels and modalities, from undergraduate to graduate, and in various forms, from live to virtual settings. The review demonstrated the use of case-based learning in many fields of health, including dentistry, pharmacology, occupational and physical therapy, nursing, medicine, allied health fields, among others. Moreover, these active learning approaches can be employed effectively in very small classes to classes with hundreds of students (Lee & Hacioglu, 2023), and across the teaching modalities such as the traditional face-to-face, in-person, or digital teaching (Özöztürk et al., 2023; Phillips, 2005).
Adopting these approaches has some challenges. For example, developing or selecting high-quality cases can be time-consuming (Ghufron & Ermawati, 2018). Instructors who are used to lecture-based teaching may not be comfortable with a more student-led approach. Further, they may lack training in how to best facilitate active learning strategies, especially in facilitating and debriefing. In addition, instructors may not want to devote class time to these activities, as it may reduce time for content delivery. Aligning case-based activities with grading and learning outcomes can be difficult and measuring learning gains from these approaches is often challenging. Finally, some classrooms may not be set up in a way that facilitates small group discussions or these may be harder to implement with large class sizes (Galdames-Calderón et al., 2024; Gallagher & Savage, 2023; Mostert, 2007; Phage et al., 2023).
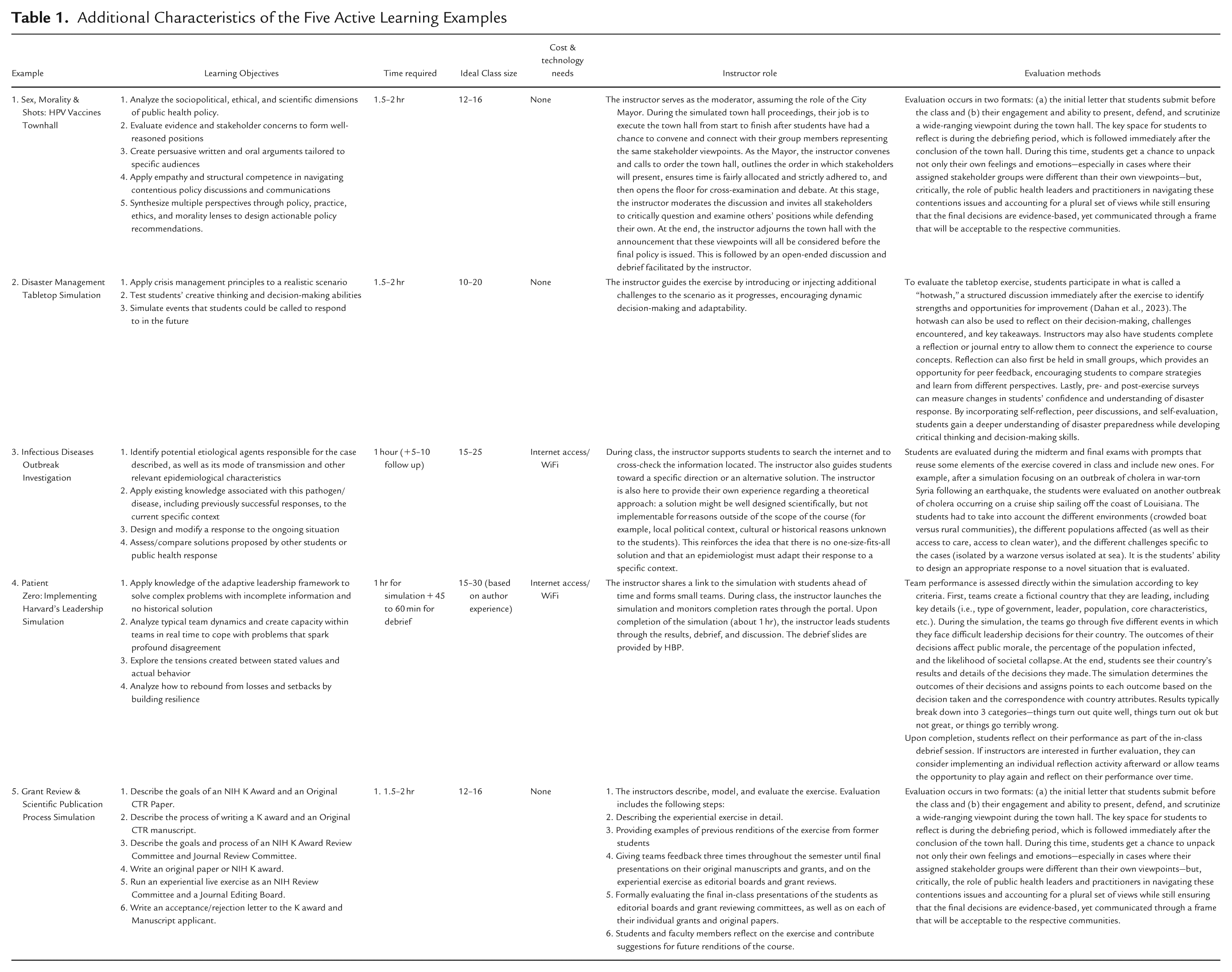
The purpose of this paper is to highlight five examples of innovative active learning strategies for teaching public health students through the incorporation of simulations, role-playing, and case studies that can serve as teaching tools and inspiration for public health educators interested in adapting their teaching to be more practice-based. These were developed and implemented by faculty who teach public health at the University of Southern California in both in-person and online modalities. We include a description of exercises and provide insight and tips on how to implement similar programs. In Table 1, we provide additional details for each example, including learning objectives, instructor role, and evaluation methodology.
Additional Characteristics of the Five Active Learning Examples
Teaching Tool Example 1: Sex, Morality & Shots: HPV Vaccines Townhall
Overview
In the context of public health practice, town halls serve as one of the key mechanisms for stakeholder engagement, community input and education, raising awareness, public health communications, and community-based decision-making (Ryan et al., 2006; Tebes et al., 2022)—especially at the local and state governance levels (Etchegary et al., 2017). Thus, a deeper understanding and appreciation of town halls are critical for competent public health practitioners in the form of class assessments and applied activities. These also enable a dynamic and interactive learning experience, fostering critical thinking, debate, and stakeholder analysis on morally and ethically complex public health questions. By simulating real-world discussions, town halls serve as forums to encourage students to engage with diverse perspectives, develop persuasive arguments, and navigate complex social and policy issues. This innovative assignment format empowers students to think critically, defend their vastly divergent positions, and engage in meaningful discourse, preparing them for real-world decision-making and advocacy. Here, we share an example of a town hall using HPV immunization decision-making as the case study.
Description of the Exercise
This case study used for the “Culture and Health: Global Perspectives” class, includes an exercise called “Sex, Morality & Shots: HPV Vaccine Townhall,” which engages students in a complex, real-world public health policy and practice debate where they critically examine the intersection of health equity, diverging cultural values, and community dynamics through moral and realpolitik lenses (Freedman et al., 2012; Howard et al., 2004). Students are tasked with deciding on mandatory HPV vaccine requirements as a part of the school vaccine schedule in a small town with increasing rates of HPV-related cancers. Students are assigned stakeholder roles—such as conservative religious parents, anti-vaxxer community members, or CDC scientists—and tasked with developing and defending their positions in a written letter to the City Mayor. This is followed by a simulated town hall debate, where they present their arguments and respond to cross-examination, aiming to reach a consensus-based public health policy that takes into account all stakeholder viewpoints.
This exercise remains enormously popular due to its complexity, rigor, depth, and its embrace of contemporary sociopolitical challenges pertinent to public health, as consistently noted by students. In post-simulation debriefs, they often describe feeling more prepared to handle contentious public health challenges and report growth in critical thinking, cultural humility, advocacy, and stakeholder engagement.
Implementation Details
This assessment can be adapted for use with both undergraduate and graduate students in various subject areas, including public health foundations, public health ethics, global health, and public health policy. Both in-person and virtual formats are also adaptable. For undergraduates, this can introduce many of the foundational concepts of stakeholder engagement, cultural perspectives on health, and ethical reasoning in public health policymaking. At the graduate level, in addition to the leadership skills embedded in the applied learning design (Wenzel et al., 2025), it can support a deeper analysis of health equity challenges within the broader sociopolitical ecosystem, policy trade-offs, and advocacy strategies, while serving as a simulation for their day-to-day jobs as public health practitioners who will undertake very similar work in most practice-based public health positions. While true for both formats, for digital execution, intentionally developing and deploying technology competence beyond the content and pedagogical expertise is imperative (Benson & Ward, 2013). For example, pre-planning and communicating the details of logistics, such as properly named break-out rooms in the digital classroom platform (e.g., Zoom) for each stakeholder, is imperative to avoid “digital frustration” among participants (Novak et al., 2023). The ideal class size should be 12 to 16 students. However, the critical aspect is ensuring that 3 to 4, but no more than 5, students are assigned per stakeholder group. Time can be adjusted to range between 1.5 and 2 hr. No unique materials, technology, or costs are required beyond the normatively expected equipment, such as a computer. Other than the preparation materials, such as the assigned readings or completing and submitting the letter ahead of time, no additional prerequisites are needed.
Tips and Challenges
The primary challenge of this exercise is that students often look for explicit and exact guidance on what they should say, struggling with the open-ended nature of crafting arguments from their assigned stakeholder perspective. Additionally, many experience discomfort when tasked with representing viewpoints they personally disagree with, such as advocating for vaccine skepticism. Explaining the pedagogical rationale and learning outcomes helps mitigate some of these challenges, allows them to immerse themselves in real-world applied learning through a case study approach, and contributes to their critical thinking, thought leadership, communications, and creative problem-solving skills.
Teaching Tool Example 2: Disaster Management Tabletop Simulation
Overview
Tabletop exercises are regularly used in disaster preparedness and emergency management (Federal Emergency Management Agency [FEMA], 2023). They are scenario-based learning activities designed to simulate real-world situations used by agencies and organizations to identify opportunities for improvement in their disaster plans, policies, procedures, and capabilities. In the classroom, tabletop exercises can be used to synthesize and practice the material that they have learned over the course of the semester. By incorporating tabletop exercises into the classroom, instructors can create a dynamic and interactive learning environment that not only enhances students’ understanding of the material but also equips them with practical and analytical skills that will serve them in their professional lives.
Description of the Exercise
The exercise is used for a course titled “Public Health Disaster Management and Response.” Students are divided into small groups, representing different stakeholders or team roles. A realistic disaster scenario is presented, such as an earthquake, heat wave, or power outage. Students collaboratively analyze the situation, identify challenges, prioritize actions, and develop a plan to address the issue. Students document their decisions and rationales, which are later discussed as a class. The exercise aims to bridge the gap between theory and practice, providing students with a hands-on opportunity to apply course concepts in a safe and structured environment. For instance, in a public health disaster management class, a tabletop exercise simulates disaster response, highlighting the role of public health practitioners and the importance of effective communication, resource allocation, and adaptability under pressure.
Students report increased engagement and interest in the material, as the exercise makes theoretical concepts more tangible and relatable. The group dynamic fosters teamwork, exposing students to diverse perspectives and approaches to problem-solving. Students gain practical experience in decision-making and learn to navigate uncertainty, which is common in real-life emergency management, preparing them for real-world challenges. The tabletop exercise promotes active learning, helping students retain information more effectively compared to traditional lecture-based methods. For many students, the tabletop exercise is their favorite part of the class and the most impactful component of the course. They appreciate the opportunity to apply knowledge and test their skills in a realistic context. Initially, some students may feel intimidated or uncertain about the open-ended nature of the activity, but most find it rewarding as they gain confidence in their abilities and work through the scenario with their group.
Implementation Details
This exercise could work for undergraduate or graduate students in an in-person or virtual format. It works well with small class sizes and could be adapted for large classes by having students work in small groups as opposed to discussing the cases with the whole class. The ideal time allotted for this exercise is approximately 1.5 hr providing sufficient time for scenario presentation, group problem-solving, and debriefing. Costs are minimal, requiring only basic classroom space or a virtual platform with breakout room capability and access to shared materials. Prerequisite skills include a foundational understanding of public health and disaster management concepts, including the incident command system, as well as the ability to collaborate and think critically in group settings.
Tips and Challenges
There are several measures that can be taken to ensure an optimal experience for students. First, it is important to have clearly defined roles and expectations for students at the start to avoid confusion. Second, select a scenario that is both relevant to the course material, realistic for the geographic region, and engaging for the students. Third, provide sufficient background information and context so students can effectively participate without feeling overwhelmed. Fourth, debrief thoroughly after the exercise, allowing students to reflect on their decisions, discuss lessons learned, and connect the experience to course content. Lastly, encourage creativity and adaptability, emphasizing that there are no “right” answers in complex scenarios. Emphasizing that this is a “no-fault” discussion helps to encourage participation.
Several challenges in conducting a tabletop exercise can be overcome with awareness on the part of the instructor. Time management can be tricky, especially if students need more time to work through the scenario or the debrief runs long. It is important to balance group dynamics, as quieter students may need encouragement to participate fully. The instructor can walk around the room to ensure that all students are participating and ask questions of those who are not to encourage their participation.
Teaching Tool Example 3: Infectious Diseases Outbreak Investigation: Scenario-based Learning
Overview
Every day around the world, there are new outbreaks reported in both scientific and mainstream media. Therefore, students can continuously learn and apply something new about a pandemic that is relevant to the course on the epidemiology of infectious diseases. Epidemiology of infectious diseases involves human populations that are highly diverse. There is no one-size-fits-all approach, meaning that students must constantly adapt and apply the theoretical knowledge accumulated during the week to the unique conditions of the specific cases discussed during the class.
Description of the Exercise
Each week in the course “Introduction to Epidemiology of Infectious Diseases,” a group of pathogens that share a similar transmission mode and general epidemiology is discussed. In a typical week, students start by reading the assigned readings and watching recorded lectures. Then, in class, a 60-min discussion amongst the whole class ensues, focusing on one or two examples of a recent or ongoing outbreak in some part of the world. For some exercises, students might have already heard about the cases in the news, while in other less common cases they may be unfamiliar with the pathogen or disease. Students are asked to submit a brief written plan to explain and justify their response. They are also asked to assess their peers’ plans and provide feedback and suggestions. In the following weeks, as cases develop, they can be briefly revisited to see how things have evolved.
An important step in developing this exercise is the selection of scenarios or cases. These may be chosen based on location (either local, national, and international), spread (from spillover to pandemics), or origin (strictly human, zoonotic from domesticated animal, zoonotic from wildlife, food- or water-borne, linked to environmental and ecosystem, etc.). Depending on the topic of the week, cases can be chosen from an array of local diseases as different as Tuberculosis, Hantavirus, West Nile, or Coccidioidomycosis which illustrate that public health issues will be different in urban downtown Los Angeles and in rural communities. Events of various ranges are also included: from limited spillover, to outbreak, and pandemics. For example, in 1 year, the class covered Dengue in California, a measles outbreak in Florida, different COVID-19 variants circulating in the US, and an Ebola outbreak in the Democratic Republic of Congo. Students also studied the ongoing eradication efforts of Poliovirus in Pakistan and Afghanistan and its resurgence in Yemen, Syria, and Ukraine. Sometimes, cases are happening simultaneously in a different setting, and the class can analyze how they differ, such as comparing outbreaks of Listeria monocytogenes linked to raw milk in the US versus the European Union. Or, a comparison of HIV prevention and access to PrEP in the United Kingdom, the Netherlands, and the US, can highlight policy differences and the important role of epidemiologists in advocating for policies.
Some cases are more complex, involving further debate and problem-solving skills. For a scenario involving multiple etiological agents or multiple outbreaks happening simultaneously, students focus on situation management. Comparing and prioritizing the issues forces them to use foundational knowledge on transmission, mortality/morbidity, social and economic impact, prevention, availability of treatment, etc. Typical scenarios include multiple flu outbreaks at the state level: H1N1 spreading in a middle school, Influenza B found in care homes, and H5N1 cases detected in farms. Students are asked to apply previous knowledge from another outbreak to a new situation. As there are numerous possible responses, all depending on what aspects of the outbreak were prioritized (location, populations, health care, vaccines, and treatment availability, etc.), it provides a valuable learning opportunity.
Some students each semester have worked at a department of public health or in a research lab and are usually happy to share their own experiences, which helps students relate the topic to the real world. A key message that resonates with students is that there is no “one-size-fits-all” approach; constant adaptation is required. The realization that they are equipped with the skills to design response strategies similar to the ones designed by epidemiologists working at leading institutions, such as local health departments or the CDC.
Implementation Details
This exercise could work for undergraduate or graduate students in an in-person or virtual format. It works well with small class sizes (15–25 students) and could be adapted for large classes by having students work in small groups as opposed to discussing the cases with the whole class. The ideal time allotted for this exercise is 60 min, with 5 to 10 min follow up in the following weekly session if suitable (e.g., to check if the outbreak progressed as predicted by the students, or if some policies discussed in class have been applied and their outcome is known). Internet access is helpful during class, as links to newspaper articles and/or public health reports are provided at the beginning of the session. No additional skills or knowledge are required outside the course content.
Tips and Challenges
Numerous resources are available for instructors to identify cases. While it may seem counterintuitive, one of the most important is mainstream media, as students are directly exposed to it. Local news is an especially good source. Of course, specialized resources also exist, such as ProMED mail, the CDC, the WHO, and websites of state/local departments of public health. Scientific journals are not recommended because they tend not to be timely and have a significant lag time due to peer review and the publication process. However, they can still provide valuable supporting information, such as background and previous examples.
Teaching Tool Example 4: Patient Zero: Implementing Harvard’s Leadership Simulation
Overview
While there are several ways to incorporate case studies and simulations when teaching public health, one resource that is particularly valuable is the collection of existing case studies and simulations from Harvard Business Publishing (HBP, 2025). While business schools and MBA programs have long utilized the case teaching method and cases from this collection, a lot of the cases are relevant for teaching public health, particularly from the Global Health Delivery collection, which can be used for courses such as public health leadership. In addition to teaching with case studies from this resource, the online leadership simulation titled Patient Zero has been used in a public health leadership course.
Description of the Exercise
Patient Zero is an adaptive leadership simulation (developed in 2015) that provides an immersive virtual experience where participants adopt the role of high-ranking decision makers in a fictional country in the grips of an unfolding zombie pandemic. Each student must purchase and download the simulation ahead of time from the HBP website. During the simulation, teams create their own country through a step-by-step process, after which they face five events that push against their country’s chosen values where they must make difficult decisions. At the end of the five events, students will see their country results as well as the details of the decisions they made. Wrestling with each of the five dilemmas sets the stage for a debrief about team dynamics and the adaptive leadership framework. The simulation automatically creates debrief slides with each team’s results for instructors to walk through during the debrief.
Students have repeatedly remarked that the lessons learned through playing the simulation resonate with many lessons learned from the real-life COVID-19 pandemic in 2020. They have found the simulation particularly helpful in understanding issues public health leaders have faced, and will undoubtedly face in the future, when dealing with unfolding pandemics without complete information and the challenges associated with acting under uncertainty. Students have unanimously had positive feedback about the simulation in terms of both their learning and their engagement, comparing it with the fun of a video game.
Implementation Details
This exercise can work for undergraduate, graduate, and executive students studying leadership in an in-person or virtual format. The simulation can be played individually or in teams. It can be played outside of class or in-class. It works well with small class sizes if played individually, or in larger class sizes if played in teams. We have found team sizes of 5 to 6 students works well. The ideal time allotted for this exercise in-class is about 2 hr, including a quick introduction (5 min), playing the simulation (60 min), and conducting a debrief (45–60 min). Students need access to WiFi and a computer or tablet to play the simulation. At the time of this writing, the simulation costs less than $20/student. No prerequisite skills are required.
Tips and Challenges
Implementation of the simulation has been simple and straightforward with the teaching resources provided, including a teaching note and debrief slides, along with the simulation. While not necessary, the simulation could also be paired with a lecture about adaptive leadership, negotiation, or conflict resolution. While the simulation can be played individually, it is more effective in small groups. When students play in teams, it involves team dynamics, such as articulating a position, compromise, communication, and collaboration skills. It aligns well with the class learning objectives and adds to the fun factor.
Teaching Tool Example 5: Grant Review & Scientific Publication Process Simulation
Overview
Translation is turning observations in the laboratory, clinic, and community into interventions that improve the health of individuals and the public, from pre-clinical, clinical, dissemination, and implementation, and population-based diagnostics and therapeutics to medical procedures and behavioral changes. Translational science is the field that generates scientific and operational innovations that overcome longstanding challenges along the translational research pipeline. These include scientific, operational, financial, and administrative innovations transforming research, making it faster, more efficient, and more impactful.
Developing grant writing and publishing skills is key to successful careers for many health professionals. Therefore, this exercise, which has been used for the course “Advanced Clinical Translational Research,” uses a structured approach to teach clinical translational researchers in training how to prepare a grant application or original research paper for peer review. The goal is to create an interactive learning environment that mimics real-world scenarios to improve participants’ writing, submitting, and revising skills for NIH committees or journal editorial boards. Overall, the goal is to enhance the skills of clinical translational researchers in preparing competitive NIH grant applications or original research papers for journal publication through a hands-on, interactive simulation experience that mimics the peer review process to better understand the expectations of NIH reviewers or journal editorial boards. This simulation offers a hands-on, immersive learning experience that complements traditional training.
Description of the Exercise
In this simulation, students engage in an NIH grant or a journal peer-review process. Students are assigned to one of three roles: 1. a junior grant writer/author who submits a grant proposal or paper for review, 2. peer reviewers (NIH reviewers or journal editorial board members), or 3. mentors/facilitators, who are experienced grant writers or journal editors who guide the process, provide feedback, and help interpret reviewer comments. The team decides on each of the individual team roles through consensus. The simulation is conducted online through a website, where participants submit proposals/papers and receive feedback from peers acting as reviewers. The review of comments is done online or in person.
To prepare for this simulation, students first learn the basics about the NIH grant process, such as the grant types (R01, R21, K awards, etc.), as well as the key components of a typical NIH grant proposal (such as specific aims, significance, innovation, approach, etc.). They also review the structure of a successful grant proposal, including how to address NIH review criteria (significance, innovation, approach, investigator, and environment). Regarding publishing, the course also covers the journal submission process, including an overview of the manuscript submission and peer review process for academic journals. It also highlights editorial board expectations, reviewer comments, revision processes, and the role of peer review in publishing, such as how reviewers assess research for scientific quality, impact, novelty, and feasibility. Students learn how to craft a concise, compelling abstract that conveys the study’s significance and how to write an introduction that outlines the research problem, literature review, and objectives. The lectures also discuss how to present methods and results clearly and concisely, ensure transparency and reproducibility, interpret the study results in the context of the broader field, identify limitations, and suggest next steps or future research. In addition, the course covers how to tailor the manuscript’s content and language to the specific journal’s audience, guidelines, and style.
Students in the role of reviewers provide constructive feedback to the proposals/manuscripts based on the NIH or journal criteria. Reviewers benefit by identifying common mistakes in writing style, proposal structure, and challenges clinical translational researchers face in understanding NIH expectations and journal submission procedures. After, the students learn how to respond to reviewer comments professionally and effectively. At the conclusion, students revise their submissions based on the feedback received during the peer review stage. The simulation experience can enhance the success of clinical translational researchers in securing NIH funding or journal publications.
The benefits of this activity include acquiring competency in evaluating common strengths and weaknesses of grant proposals and manuscripts created during the simulation, which will inform future applications. Using a practical approach, the benefits of simulated peer review and feedback result in a tangible increase in the quality of research proposals and manuscripts. Additionally, simulation improved participants’ abilities to prepare competitive grant applications or manuscripts.
Implementation Details
This exercise is best suited for graduate students, whether in an in-person or virtual format. It works best with small and medium-sized classes, as students work, present, and evaluate fellow students in groups using a team science framework (Bennett & Gadline, 2012). The time allotted for this exercise includes manuscript and grant writing lectures, team science lectures (5 1-hr classes), completion of an original manuscript or grant (e.g., NIH K or small R awards), as well as in-class work to prepare and present two group updates, homework, a final in-class group presentation, and a final formal grant/manuscript written review of each student by the students divided in two groups. Internet access is required but no other prerequisite skills or knowledge are required.
Tips and Challenges
It is important to clearly describe and demonstrate the expectations and importance of each of the roles of the simulation by creating a manual of procedure that clearly explains the overall goals and individual expectations of the exercise. Students may find the exercise time-consuming; thus, it is recommended that selected sections be assigned (Specific Aims, Abstract, Methods). Dominant students may overshadow quieter peers. Therefore, providing annotated examples and conducting a pre-exercise session is key. Students may score the teams based on presentation rather than merit. Thus, it is essential to reinforce NIH/Journal scoring criteria and calibration exercises. Acknowledging any limitations in the simulation, such as limited time or scope of feedback, and suggestions for further improvement are key. Future directions for refining and expanding the simulation include inviting outside faculty and former students with simulation expertise to participate and evaluate the exercise, gathering structured student feedback on and recommendations for the experience, and emphasizing professionalism and possible impact on the students’ future roles as researchers and reviewers.
Conclusions
Active learning helps to foster student engagement, critical thinking, and the application of knowledge in real-world contexts. These features make it one of the most critical and valuable strategies for public health practice education in programs such as the Master of Public Health (MPH) or a Doctor of Public Health (DrPH), where graduate students are being trained to join the practitioner workforce. Through these unique examples covering a range of subject areas and employing innovative teaching strategies, including case studies, role-playing, and simulation exercises, we highlight how these active learning approaches, adapted for public health education, offer students immersive experiences in which they apply theoretical knowledge to complex, authentic scenarios. Moreover, these serve as teaching tools with guided notes from faculty that highlight “lessons learned” that allow other faculty to adapt and integrate these into their teaching. Finally, these approaches deepen understanding and enhance motivation, retention, and essential skills such as teamwork, communication, and leadership. Such learning experiences are helpful in public health education, where navigating ambiguity, considering diverse viewpoints, and practicing evidence-based decision-making are crucial. These examples illustrate how active learning can transform traditional education into a dynamic, practice-oriented experience that prepares students for future professional challenges.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
