Abstract
Racism and colonialism operate as social determinants of health, contributing to inequities among Indigenous Peoples. To counteract these inequities, national and global calls to action have emphasized the need for cultural safety and anti-racism within healthcare. Higher education plays a crucial role in preparing an equipped workforce and shaping professional culture, making it essential to embed cultural safety and anti-racism training into the learning pathways of future health professionals. This study examined the determinants shaping the uptake and implementation of cultural safety and anti-racism training in Master of Public Health (MPH) programs across three universities within one Canadian province. Data were collected through key informant interviews, focus groups, and document analysis. The Consolidated Framework for Implementation Research (CFIR) guided comprehensive analysis of the barriers and facilitators influencing how these training interventions are being put into practice. Findings highlighted similarities and variations in cultural safety and anti-racism training approaches across MPH curricula, highlighting the evolving nature of this training. The study underscores the need for multi-level action that addresses individual, institutional, and systemic challenges, while leveraging existing strengths. The significance of this research lies in its potential to inform curriculum reform, pedagogical practice, policy development, and professional culture in public health and related disciplines. To support academic units, a self-assessment tool developed from the findings offers a structured framework to reflect on and enhance efforts in implementing cultural safety and anti-racism training.
Keywords
Introduction
Indigenous Peoples have long understood and drawn attention to the profound impacts of colonialism and racism on individual and community wellbeing. Mainstream scholarship increasingly recognizes interpersonal, systemic, and structural racism as critical determinants of health (Allan & Smylie, 2015; Krieger, 2014; Loppie et al., 2014). In Canada, there have been numerous calls to action advocating for cultural safety and anti-racism practices, including: the Royal Commission on Aboriginal Peoples (Aboriginal Affairs and Northern Development Canada, 1996), the Truth and Reconciliation Commission (TRC, 2015), National Inquiry into Missing and Murdered Indigenous Women and Girls (2019), and the In Plain Sight Report (Turpel-Lafond, 2020). All these landmark reports put forward clear recommendations that emphasize the need for ongoing training, education, and awareness on issues related to Indigenous-specific racism across all sectors, including public health. Indigenous-led advocacy has led to growing adoption of cultural safety and anti-racism interventions in health organizations, educational institutions, and government bodies in Canada and other countries (Baba, 2013; Greenwood, 2019; Guerra & Kurtz, 2017; Hassen et al., 2021; MacLean et al., 2023; Nickerson, 2019).
Public health is an important discipline for cultural safety and anti-racism training interventions, given the field’s emphasis on promoting social justice and health equity through action on the determinants of health. Graduates from Master of Public Health (MPH) programs contribute to health policy, health authority mandates, service delivery, health promotion, research, and program evaluation, making them key levers of change to address discrimination and racism in the healthcare system and society (Baba, 2012; Canadian Public Health Association, 2019). Implementing cultural safety and anti-racism training in MPH curricula supports efforts to hardwire practices at all levels of the healthcare system and contribute to patients’ experiences of culturally safe healthcare encounters (Greenwood, 2019).
Published literature over the past decade suggests a period of transition from simply calling attention to and advocating for more equitable healthcare for Indigenous Peoples toward action that requires educating healthcare professionals to uphold cultural safety for individuals and communities through respectful practice (Came & Griffith, 2018; Guerra & Kurtz, 2017). Now that there has been significant uptake of such training, we are transitioning to evaluating efforts and identifying best practices. There remains a need for research that details the challenges, strategies, and best practices associated with implementing and sustaining cultural safety and anti-racism training within education curricula and training programs. This study contributes to advancing awareness and knowledge through an in-depth case study analysis of relevant training interventions in MPH programs in Canada, ultimately aiming to inform best practices for broader application across educational and healthcare settings.
Terminology
Among various models of health professional training addressing anti-Indigenous racism, cultural safety and anti-racism were chosen as the popular discourses during the study period (2017–2023). Cultural safety and anti-racism, as complementary concepts, are defined in this context as an approach to public health that ensures care encounters are respectful of individuals’ cultural identities and free from discrimination or racism (Public Health Agency of Canada, 2023; see Background for further details). It is important, however, to acknowledge that the relevance and appropriateness of terms used are both time-bound and context-dependent.
Training is used as a general term to encompass a wide spectrum of teaching and learning strategies, including both formal curricula (e.g., classroom instruction, modules, skills-based practical exercises, experiential learning, practicums) and informal education (e.g., mentorship, modeling, hidden curriculum). This article specifically focuses on training interventions in the curricula of MPH programs, which are graduate-level professional degrees in public health that are, in some cases, accredited by bodies such as the US-based Council on Education for Public Health (CEPH), though accreditation is not universal. The MPH programs included in this study represent the diversity of these programs in Canada, differing in their accreditation status (accredited or non-accredited), the academic units in which they are housed (e.g., schools of public health, faculties of medicine, or health sciences), and the modes of program delivery (e.g., online, in-person, and hybrid formats).
Background
The history of cultural safety and anti-racism training in public health and higher education is rooted in an effort to eliminate Indigenous-specific racism and address systemic inequities faced by Indigenous populations. In public health, manifestations of racism occur both at interpersonal and institutional levels (Came & Griffith, 2018).
Interpersonal racism is experienced by Indigenous individuals and families through everyday interactions with care providers that are disrespectful, demeaning, diminishing, or disempowering toward their cultural identities (Loppie et al., 2014). While such experiences are well-documented in the Canadian healthcare system—often reflected in patient accounts of being stereotyped, mocked, denied treatment, or discharged without adequate planning (Turpel-Lafond, 2020)—similar patterns of racism extend into public health. In public health contexts, racism manifests through the trivialization of Indigenous Peoples’ lived experiences; the prioritization of non-Indigenous populations over Indigenous communities in outreach and interventions; and the exclusion of Indigenous Peoples from decision-making processes in public health programs, research, and policy development that directly impact them (Canadian Public Health Association, 2019).
Institutional racism operates through organizations’ internal culture, policies and procedures. Racism and hegemonic colonial culture permeate Canadian health systems and institutions through physical environments in which Indigenous Peoples do not feel safe and health professional workforces that do not represent them (Nickerson, 2019; Turpel-Lafond, 2020). In public health, institutional racism manifests through policy decisions, program designs, and epidemiological data that often fail to account for the socio-cultural contexts and colonial history of Indigenous Peoples, leading to public health initiatives that are ineffective or even harmful (Came & Griffith, 2018). By extension, education systems feed into institutional racism by shaping individuals’ beliefs, attitudes, and values. Canadian education institutions are steeped in colonial culture, interpersonal racism, and epistemic racism. When education systems are built upon the foundations of racism and colonialism, these harmful ideologies permeate the public health workforce and extend into the care of Indigenous patients and clients (Diffey & Mignone, 2017).
Cultural safety was originally introduced as a postcolonial theoretical framework for nursing practice to address inequities experienced by Māori people in Aotearoa (New Zealand); the concept was developed by Māori nurse Dr. Irihapeti Ramsden in the 1980s (Ramsden, 2002). This concept has since been widely integrated into healthcare practices, policies, and research across the globe, reflecting a growing recognition of its value (Guerra & Kurtz, 2017; Johnson & Sutherland, 2022; MacLean et al., 2023). Cultural safety can be understood as an outcome of an effective care encounter that is respectful of individuals’ cultural identities, and is deemed physically, socially, emotionally, and spiritually safe by a care recipient and/or their family (Ramsden, 2002). Cultural safety encourages health professionals to engage in self-reflection to examine how their socio-cultural locations, beliefs and attitudes shape their professional practice and interactions with Indigenous Peoples. Additionally, cultural safety prompts critical interrogation of unjust social processes and colonial structures within health systems (Baba, 2013). The willingness to engage in these reflective and reflexive practices requires cultural humility, the process of self-reflection to understand personal and systemic biases and privileges (Public Health Agency of Canada, 2023).
Parallel to the evolution of cultural safety, anti-racism has emerged as a key model for education, social services, and healthcare delivery. Originating in the field of education in the early 1980s, anti-racism approaches have recently gained traction in health-related fields (Hassen et al., 2021). Anti-racism aims to confront and dismantle systems of racialized oppression and unpack the legitimization of white privilege, with the goal of eliminating racism in all its forms (Came & Griffith, 2018; Ford et al., 2019) and tackling white supremacy (Liu et al., 2021). Unlike cultural safety, anti-racism removes the term culture, arguing that re-packaging issues of racism, power and privilege as “culture” evades the real issues (Allan & Smylie, 2015).
In 2016, CEPH updated its accreditation competencies, adding one that reads, “Discuss the means by which structural bias, social inequities and racism undermine health and create challenges to achieving health equity at organizational, community, and societal levels” (p. 17). For accredited Schools of Public Health, there is a requirement to align MPH curricula with competencies and knowledge areas developed by accreditation bodies, such as CEPH. While Canada does not have its own public health accreditation body, five Canadian Schools of Public Health are CEPH-accredited. In Canada, MPH programs generally develop their curricula in alignment with the Public Health Agency of Canada’s (PHAC) Core Competencies for Public Health in Canada, which establish professional standards for the essential knowledge and skills required for public health practice in Canada (National Collaborating Centres for Public Health, 2024). Starting in 2023, the six National Collaborating Centres for Public Health were commissioned by the PHAC to modernize and refresh the Core Competencies (National Collaborating Centres for Public Health, 2024), and the revised set will include focused competencies on cultural safety and anti-racism (C. Betker, personal communication, 2023). These recent developments highlight the growing recognition of cultural safety and anti-racism as critical public health concerns, and the evolving nature of their integration into MPH curricula in Canada and America.
A 2023 scoping review that synthesizes the state of knowledge on Indigenous cultural safety training across Canada, United States, Australia, and New Zealand concludes that this topic is still in its early stages of development and uptake, emphasizing the need for future research to clarify the core concepts informing the training interventions (MacLean et al., 2023). The available literature demonstrates that there is a lack of evidence about which conceptual models are most appropriate, what teaching techniques are most effective, and how these can be operationalized and implemented in curricula (Diffey & Mignone, 2017; Guerra & Kurtz, 2017; MacLean et al., 2023). Furthermore, there is considerable variability in how education programs incorporate cultural safety and anti-racism training, differing in format, frequency, duration, and the concepts they teach (Baba, 2013; Guerra & Kurtz, 2017; MacLean et al., 2023). There are an increasing number of parallel initiatives promoting co-aligned concepts with overlapping principles (e.g., equity-oriented, patient-centered, trauma-informed care). The multiplicity of models creates challenges for evaluation and cross-comparison.
There has been a greater emphasis on cultural safety and anti-racism training, and correspondingly more published literature, in the fields of nursing and medicine. This assessment of the body of literature is consistent across four published evidence syntheses: Diffey and Mignone (2017), Guerra and Kurtz (2017), Hassen et al. (2021), and MacLean et al. (2023). These evidence syntheses demonstrate that research on cultural safety and anti-racism training interventions has tended to be on descriptions of the intervention itself or on evaluation of its outcomes, rather than on detailing the implementation processes. One study by Rowan et al. (2013) drew from the field of quality improvement to develop a conceptual model of integration of cultural competence and/or cultural safety into Schools of Nursing, which they applied in a survey of 38 Canadian Schools of Nursing. They concluded that three main elements are required to successfully integrate cultural competency and cultural safety programs into healthcare education and training: contextual (e.g., precipitating environmental conditions, leadership engagement), structural (e.g., appropriate policies, educated faculty), and process (e.g., agreed-upon frameworks, curriculum integration) (Rowan et al., 2013). There is a need for more research that provides insights and practical guidance on effective strategies for implementing and sustaining these types of training interventions in health professional education programs. To contribute to this growing area of inquiry, this study examines the implementation of cultural safety and anti-racism training interventions within MPH programs.
Methodology and Methods
The purpose of this study is to explore the determinants shaping the uptake and implementation of cultural safety and anti-racism training in MPH curricula. This research question is explored within core constructs defined and theorized by implementation science (Birken et al., 2017; Nilsen, 2015), with an added lens of anti-colonial theory (Carlson, 2017). The study was informed by the Consolidated Framework for Implementation Research (CFIR), which provides a comprehensive structure for examining the barriers and facilitators influencing implementation of healthcare interventions (Damschroder et al., 2009). Specifically, it is guided by five primary objectives under the following domains:
The study employed a qualitative case study design across three MPH programs within one Canadian province. By focusing on three cases, the study captures the complexity and nuance of the institutional settings within a unified provincial and national context. The three cases offer diversity in terms of the academic unit in which the MPH program is situated, the disciplinary influences, the organizational size and structure, the focal points of the curricula, the format, and delivery (e.g., online vs. in-person), etc. Consistent with the literature, the three sites exhibited variation in their approaches to teaching cultural safety and anti-racism, prompting data collection to encompass a range of training interventions, including classroom instruction, online modules, experiential learning, and mentorship.
Data were collected from multiple sources to get a comprehensive picture of the processes and context of implementing cultural safety and anti-racism training in MPH curricula. Data collection entailed a combination of interviews, focus groups, and document analysis. Numbers of respondents and included documents are summarized in Tables 1 and 2 respectively. An iterative process of data collection and analysis allowed for ongoing refinement of recruitment and methods as new insights emerged (Benzer et al., 2013; Charmaz & Belgrave, 2012).
Number of Respondents by Case.
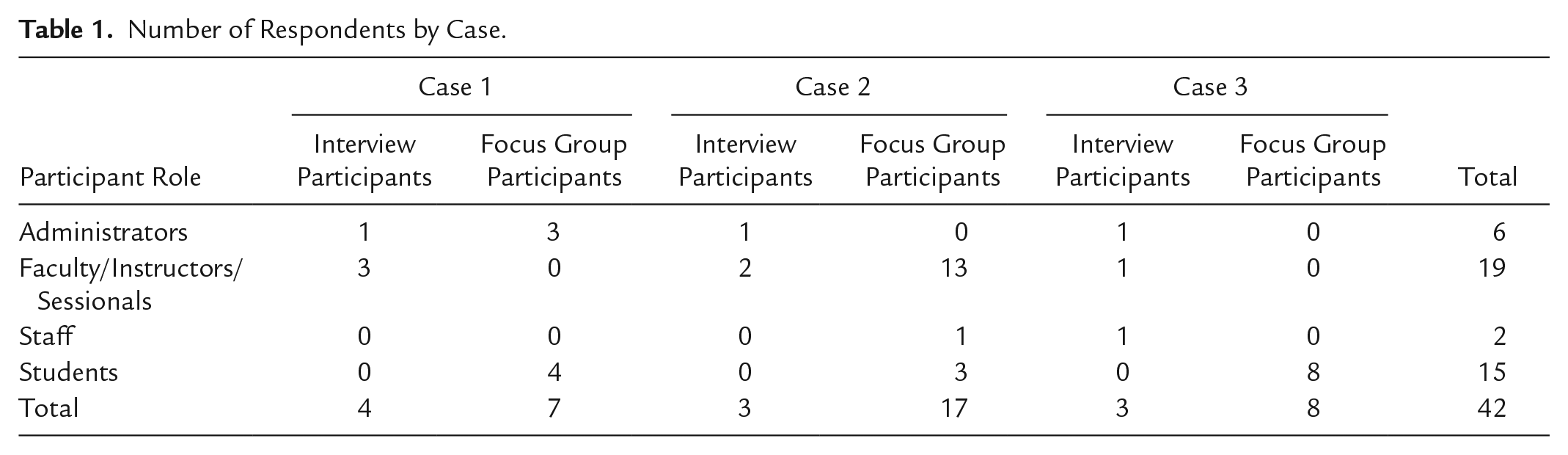
Number of Included Documents by Case.
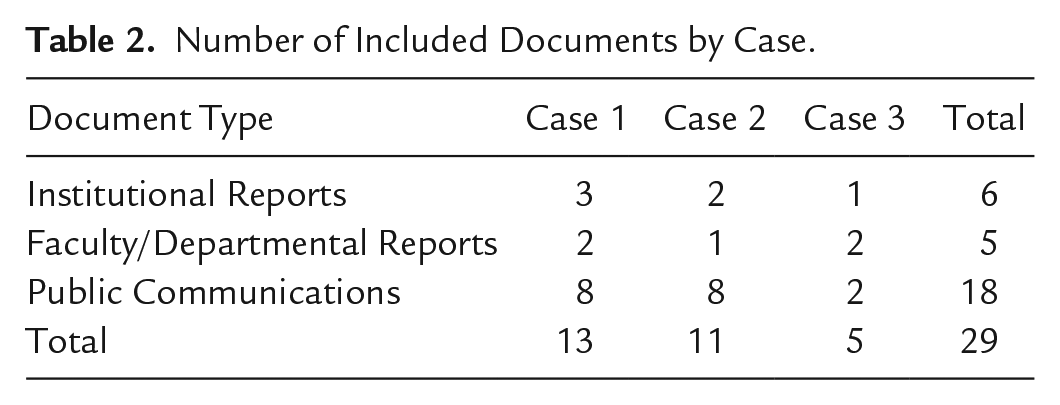
A purposive sampling strategy was employed to ensure representation of the multitude of perspectives and experiences of stakeholders involved in the implementation of cultural safety and anti-racism training. Sampling began with an initial invitation to two to three key informants from each MPH program, who are strategically positioned to influence the development, instruction, and evaluation of cultural safety and anti-racism training. These key informants supported the identification of additional participants through snowball sampling. The participant pool included Deans of the faculties in which public health is situated, Program Directors of MPH programs, Indigenous faculty members, professors who instruct core public health courses or Indigenous health electives, staff involved in supporting implementation, as well as current MPH students to capture their experiences of cultural safety and anti-racism training.
All interviews and focus groups were conducted virtually using Zoom due to institutional restrictions on in-person data collection during the COVID-19 pandemic. Most faculty and administrators participated in individual interviews to accommodate their schedules. However, Case 1 organized a focus group with three administrators, while Case 2 convened a larger focus group that included 14 administrators, faculty, and staff. All student participants contributed through focus groups. In addition to interviews and focus groups, key informants were asked to provide institutional and departmental academic plans that shape MPH curricula or outline commitments to cultural safety and anti-racism training. They also identified additional data sources, such as syllabi, teaching materials, and training manuals.
A pre-existing codebook and NVivo coding shell developed by the CFIR Research Team-Center for Clinical Management Research (2025) were used to guide the coding process, which involved line-by-line coding, thematic analysis, and constant comparison (Charmaz & Belgrave, 2012). Framework analysis was employed to index and interpret the data using domains and constructs from the CFIR (Damschroder et al., 2009; Hill et al., 2018). This approach allows for a systematic and comprehensive examination of the data within the established theoretical framework, enabling elucidation of complex determinants influencing implementation and the relationships between them.
A commitment to relational accountability, a core tenet of anti-colonial theory (Carlson, 2017), was integral to the study’s methodology. This involved early and ongoing consultation with key stakeholders in the health and education systems, as well as mentorship and oversight from Indigenous scholars and Knowledge Holders. Early in the study (May 2021), six subject matter experts and thought leaders in the field participated in a virtual forum to provide feedback on the study design, ensuring that the proposed research was relevant to information needs and priorities. Then in March 2024, 28 knowledge users and participants from across the three institutions participated in an end-of-study knowledge exchange gathering to share findings, mobilize action, and collaboratively envision the future of public health training. The gathering convened a diverse group of knowledge users and leaders involved in developing curriculum, core competencies, and health standards.
As part of the commitment to relational accountability, over the course of the study, the authors developed a knowledge translation output in the form of a self-assessment tool to evaluate cultural safety and anti-racism training in curricula. The tool was carefully crafted as a practical resource to support academic units across all disciplines implement curricular improvements. The indicators in the self-assessment are informed by a comprehensive analysis of innovative approaches and areas for improvement from the study’s findings (see Findings). Additionally, the resource incorporates evidence-informed practices from the literature. To ensure the tool was both relevant and user-friendly, it was shared with all research participants (N = 42) and presented at the end-of-study knowledge exchange gathering, where event participants (N = 28) had the opportunity to provide feedback. This engagement with knowledge users was crucial in refining the tool, ensuring it aligns with the needs and expectations of its end-users. While the initial feedback was valuable, the self-assessment tool requires further validation and refinement to confirm its effectiveness and relevance in supporting academic units in their improvement efforts (see Practical Applications).
The study obtained harmonized ethical approval from all three institutions, and all participants provided informed consent prior to participating.
Findings
The findings of this study highlight key barriers and facilitators influencing the uptake and implementation of cultural safety and anti-racism training in MPH curricula. Guided by the CFIR, these findings are categorized under the following domains: Intervention Characteristics, Characteristics of Individuals, Process, Inner Setting, and Outer Setting. Table 3 provides a snapshot of key barriers and facilitators across the five domains. This is followed by a brief description of how these domains influence the implementation of cultural safety and anti-racism training in MPH programs. Detailed findings across all 39 CFIR constructs can be found in the full dissertation (Kent, 2023), and definitions of constructs can be found in the original article by Damschroder et al. (2009) or the online CFIR Guide (CFIR Research Team-Center for Clinical Management Research, 2025).
Summary of Determinants of Uptake and Implementation Across the Three Cases.
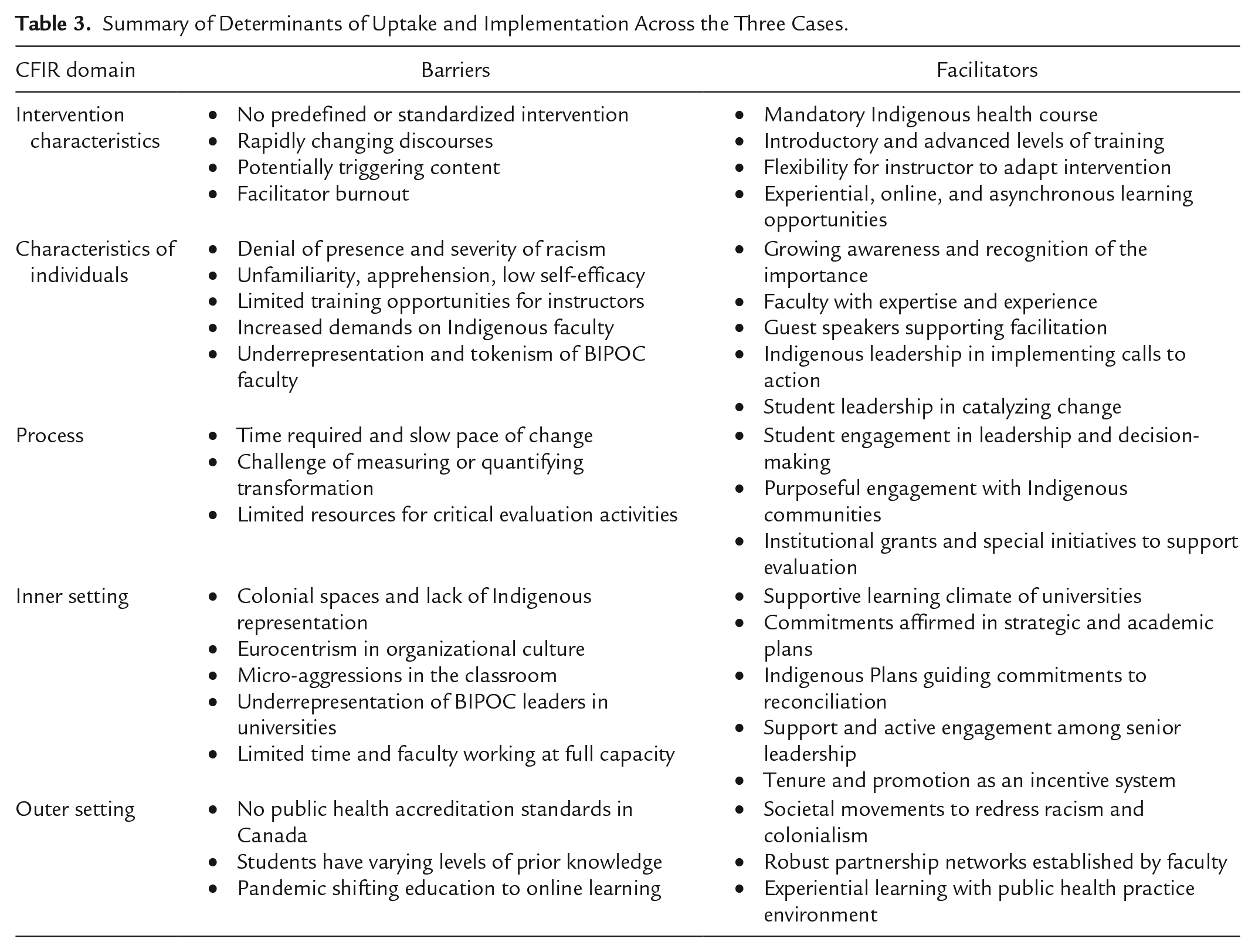
Intervention
Several barriers have been identified within the Intervention domain. Foundationally, the lack of a standardized or predefined approach to cultural safety and anti-racism training represents a key barrier to its consistent implementation across institutions. Interventions vary significantly between instructors and institutions, which makes it difficult to replicate successful models or evaluate their effectiveness. Differences are evident in various aspects such as the location within the curriculum, delivery format, duration and frequency, and whether it is mandatory or elective, as summarized in Table 4. The rapid evolution of discourses around anti-racism and cultural safety exacerbates this challenge, as faculty and students are often left navigating shifting terminology and conceptual frameworks. The emotional labor of teaching this content often leads to instructor burnout. Instructors need to carefully navigate content that can potentially be triggering or may expose Indigenous students to micro-aggressions. Student participants described content related to Indigenous Peoples as “negative,” “deficit-based,” “problematic,” “stigmatizing,” “medicalized,” “pathologizing,” “decontextualized,” and “outdated.” A common example cited was referring to Indigenous Peoples as “a burden,” “high risk,” “vulnerable,” or “needing help/not capable on their own.”
Summary of Intervention Characteristics Across the Three Cases.
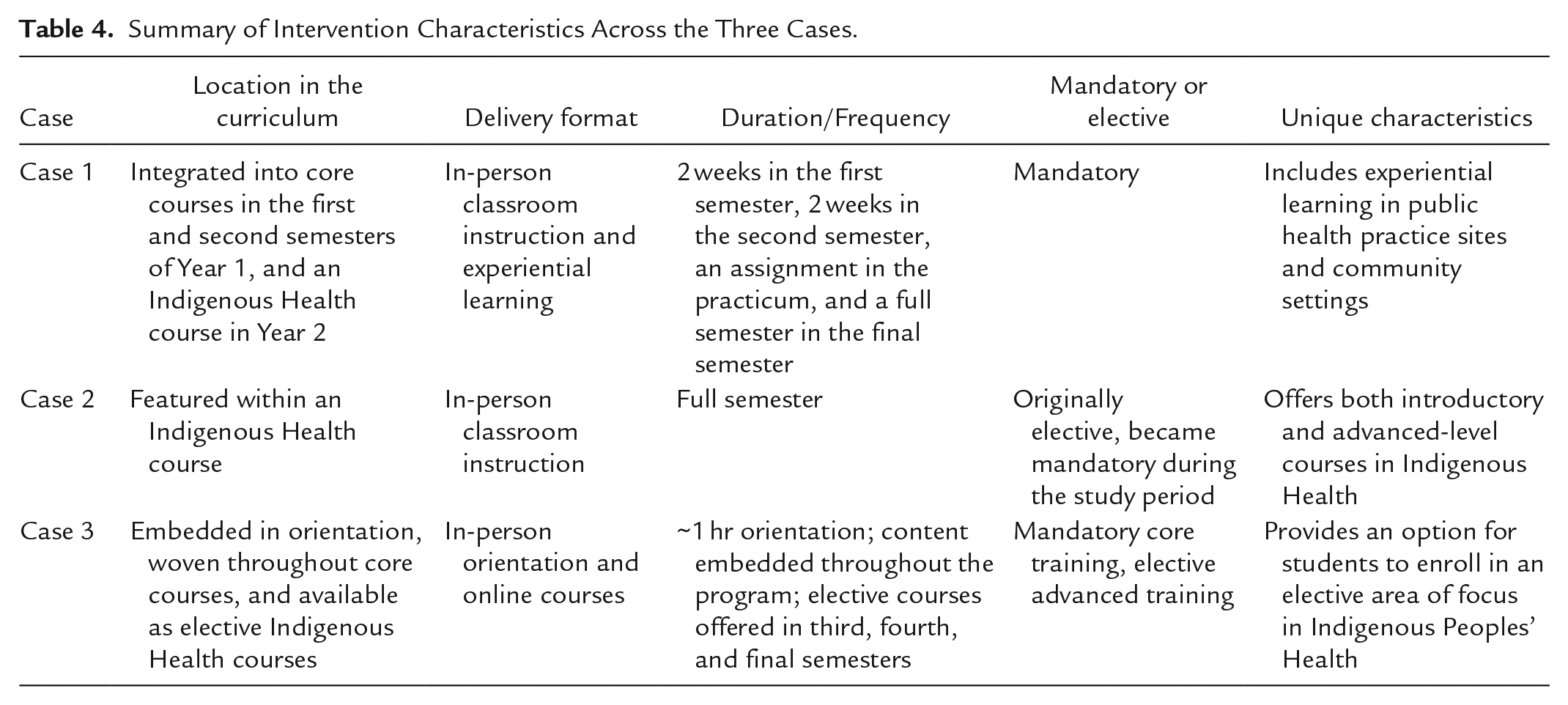
Conversely, several facilitators offer promising pathways for enhancing implementation efforts and intervention effectiveness. One example of these pathways includes having a mandatory, standalone course in Indigenous health, which provides dedicated space for cultural safety and anti-racism content. Furthermore, offering both introductory and advanced levels of Indigenous health courses helps meet learner needs. At the same time, scaffolding cultural safety and anti-racism principles throughout the curricula can reinforce learning and contextualize these concepts. Flexibility in adapting interventions to suit specific contexts allows instructors to tailor their approaches to the diverse needs of students. Designing opportunities for experiential learning can provide learners with hands-on experience to practice relevant skills. Online and asynchronous learning options also offer flexibility to students to engage with challenging content at their own pace.
Characteristics of Individuals
Among the study participants involved in a teaching, learning, or supporting capacity, a significant barrier to implementing cultural safety and anti-racism training lies in the denial of the presence and severity of racism. This denial is often coupled with unfamiliarity, apprehension, and low self-efficacy among instructors, who feel unprepared to teach these topics effectively. The limited availability of training opportunities for faculty further exacerbates these tensions. Indigenous faculty face disproportionate demands, often being called upon to lead cultural safety initiatives without adequate support. This is compounded by the underrepresentation of Black, Indigenous, and People of Color (BIPOC) faculty, markedly in decision-making/resource allocating authority roles. These disparities and other systemic issues within academia contribute to feelings of disconnect and detachment from the institution among Indigenous students and faculty.
While many participants identified that they are in a learning stage of change, participants also acknowledged that there has been significant growth in awareness, knowledge, skills, and enthusiasm among staff, faculty, and administrators in recent years. One participant noted: . . . it’s not at all surprising, it’s women of color who have recognized . . . who just are fed up, and basically said, you know, we cannot be complacent about these issues any longer. We have to have these conversations. . . We have got to have accountability among ourselves to each other.
Study participants recognized faculty members with subject matter expertise and experience facilitating cultural safety and anti-racism training as crucial drivers of change. Additionally, guest speakers have also played a valuable role in facilitating these training interventions, bringing in professional and lived experience, and offering diverse perspectives. Indigenous leadership has been especially instrumental in implementation efforts, with Indigenous faculty and students taking on pivotal roles in mobilizing curriculum innovation and championing anti-racism advocacy. Student leadership has also been a catalyst of change and a source of accountability.
Process
The three MPH programs included in the sample are all in relatively early stages of implementing cultural safety and anti-racism training. Time involved in purposeful engagement with communities and students to inform curricular reform was noted as a significant barrier. This surfaced disagreement around the pace of innovation, as noted by the following three participants: It’s the strangest irony I think of universities. They pride themselves on innovation and new ideas and experimentation. But absolutely elephants when it comes to actually making any change within their own institutions (Participant from Case 1). There’s a kind of school culture of not wanting to make a mistake doing it . . . but they’re not recognizing that if we just continue what we’re doing, we’re using that power to reinforce the status quo . . . It’s this double-edged sword (Participant from Case 2). . . . Let’s hold to good processes let’s continue to walk gently down this path rather than trying to push ahead (Participant from Case 3).
Another challenging aspect of advancing this work is the difficulty in measuring or quantifying transformation over time, especially given the limited resources available for evaluation activities.
Nevertheless, several facilitators have supported the process of implementing and sustaining these initiatives. Engaging students in leadership and decision-making has been impactful, with students leading initiatives to incorporate Indigenous perspectives and anti-racist practices into the curriculum. Purposeful engagement with Indigenous communities has further supported the process, ensuring that cultural safety interventions are grounded in real-world contexts and community priorities. Institutional grants and special initiatives have provided financial resources for evaluation, and to sustain these efforts over time.
Inner Setting
The institutional environment presents several structural barriers to the implementation of cultural safety and anti-racism initiatives. Many academic institutions remain steeped in colonialism and Eurocentrism, which are deeply embedded in organizational culture and are embodied by the built environment. This was most evident in the analysis of key institutional documents, which in some cases reinforced colonial culture through their language and frameworks, while in others, explicitly critiqued and challenged these norms. An article from an independent newspaper reporting on experiences of racism at Case 100 characterized university culture(s) as follows: There is a belief — and criticism — that post-secondary institutions are liberal and progressive. Not true. . . They are simply “a microcosm of the larger society.” “Universities, like any institution, are relatively conservative insofar as we have established practices and policies to maintain the status quo. . .”
A significant theme across all three cases was the complexity of cultivating a culturally safe environment. The classroom environment, whether in-person or online, can be hostile to BIPOC students and faculty, with micro-aggressions and racist comments often going unchecked. Once again, the underrepresentation of BIPOC leaders in academia, combined with faculty working at full capacity, makes it difficult to allocate time and resources to this critical work.
Despite these barriers, the learning climate within universities provides a supportive environment for introducing training interventions. This is especially true when cultural safety and anti-racism are endorsed by institutional commitments and affirmed in strategic or academic plans. All three cases have Indigenous Plans that help advance the institutions’ commitments to reconciliation and that include recommendations in support of cultural safety and anti-racism training. One of the cases has a supplementary guide to help academic units to develop their own plans for implementation. The same case released an institutional report with a series of recommendations dedicated to anti-racism, which was coupled with a strategic framework and “Roadmap for Change” to support implementation in academic units. Alongside these reports, senior leadership, including university presidents, have played a key role in championing decolonization and anti-racism to drive institutional change. The tenure and promotion system can also serve as an incentive for faculty to engage in cultural safety and anti-racism initiatives.
Outer Setting
There are a wide range of determinants external to the immediate training environment. For instance, there are currently no Canadian accreditation standards for public health that mandate cultural safety training (see Background), which leaves much of the responsibility to individual institutions. Several participants critiqued the Core Competencies for inadequately reflecting knowledge and skills related to cultural safety and anti-racism. It is noteworthy that the need to revise these competencies to address these gaps and others has been recognized and a revision is currently underway. Academic programs aim to be responsive to student needs; however, the diverse levels of knowledge and experience students bring create challenges in tailoring interventions effectively. The disruptive shift to online learning due to the COVID-19 pandemic further complicated student-centered design.
However, there are external facilitators that have supported these initiatives. Societal movements to address racism and colonialism, including the Truth and Reconciliation Commission and Black Lives Matter, have generated increased awareness and urgency for change. In a public message, President of Case 100 acknowledged: . . . Over these past months, we have also seen a surge of energy. From protests in the streets to calls for action on social media and in government offices, there has been a renewed societal effort to move towards creating a more inclusive and equitable world. We have the opportunity to join this movement and make [university] a leader for change.
Participants and key documents often referenced TRC Call to Action #24, which calls upon health education programs to provide “skills-based training in intercultural competency, conflict resolution, human rights, and anti-racism” (2015). Faculty actively seek guidance from the public health practice environment to align with workforce priorities and have established strong external partnership networks to tap into valuable expertise. For instance, some MPH programs have arranged experiential learning and practicum placements with health authorities, which can reinforce training by providing opportunities for real-world applications of learning.
These findings illustrate the complex landscape of determinants that influence the implementation of cultural safety and anti-racism training in curricula. By addressing these challenges and leveraging existing strengths, MPH programs can work toward creating more equitable learning environments and better preparing the public health workforce.
Practical Applications
To support MPH programs with implementing their own cultural safety and anti-racism training, the authors developed a self-assessment tool that is designed for academic units across all disciplines. The tool builds off the best practices and areas for improvement identified in the study findings, and integrates evidence offered by the literature. By offering a structured yet adaptable framework, the tool helps academic units to assess their current strengths and pinpoint areas for further growth. The tool serves as both a practical resource and an invitation for continued learning, reflection, and curriculum enhancement. Readers are encouraged to use, adapt, and test it within their own contexts, contributing to the tool’s iterative refinement and broader applicability.
Discussion and Recommendations
This study contributes to the current literature on curriculum innovation in master’s level professional preparation in public health by providing a comprehensive examination of the determinants shaping the uptake and implementation of cultural safety and anti-racism training in MPH programs. This research fills gaps in the current literature by focusing on the implementation processes of cultural safety and anti-racism training interventions, an area that remains underexplored. Unlike prior studies that predominantly assess the effectiveness of these interventions, this study outlined how the training is being implemented and examined the determinants shaping these processes.
The three MPH programs included in the sample are all in relatively early stages of implementing cultural safety and anti-racism training. This is consistent with evidence syntheses in the literature, which indicate that across Canada and other countries, uptake of these types of training interventions in health professional education are in early stages of development and implementation (Baba, 2013; Diffey & Mignone, 2017; MacLean et al., 2023). Similarly, the lack of standardized models and variability across institutions aligns with the literature on cultural safety and anti-racism training, which often points to the absence of consensus on best practices (Baba, 2012; MacLean et al., 2023; Nickerson, 2019). The findings resonate with existing frameworks that emphasize contextual, process, and structural factors as key determinants for successful integration of cultural safety programs in healthcare education (Rowan et al., 2013).
Additionally, the findings highlight the influence of broader patterns of social, cultural, and political factors, such as racism, colonialism and Eurocentrism, that have been studied within education environments (Diffey & Mignone, 2017). Furthermore, this study builds on existing frameworks in the field of healthcare education by complementing the knowledge with the extensive evidence and theories offered by implementation science (Birken et al., 2017; Damschroder et al., 2009; Nilsen, 2015).
The study offers a foundation for future research and policy development in cultural safety and anti-racism training. Further research is needed to validate the assessment tool and evaluate the successful implementation of training interventions. Longitudinal studies that track changes in student competencies and the impact on health outcomes in Indigenous communities could provide valuable insights. Future work should inform the development of core competencies and accreditation criteria that can inform the development of standardized guidelines for cultural safety and anti-racism training in MPH curricula across institutions, while allowing for contextual adaptation.
Limitations
This study aimed to provide practical recommendations to support MPH programs and other academic units in implementing cultural safety and anti-racism training interventions. The data is grounded in the experiences of three MPH programs in one Canadian province; as such, the findings and recommendations are context-specific and subject to considerations of generalizability and transferability. The implementation strategies are put forward to reflect upon and potentially adapt to other practice settings, disciplines, or regions, recognizing that the implementation of such training is highly nuanced and varies by setting. Future applications or adaptations of these recommendations necessitates cultivating relationships and authentically engaging with local Indigenous Nations to seek their leadership in integrating Indigenous knowledge and cultural protocols. Furthermore, it is important to situate the research within its temporal context, understanding that the data is collected over a defined period and may not capture any changes or developments that occur after the data collection period (2021–2023).
Conclusion
This study provides critical insights into advancing cultural safety and anti-racism in master’s level professional preparation in public health, emphasizing the need for systemic change to better prepare future health professionals for culturally safe practice. By examining the determinants influencing the uptake and implementation of relevant training interventions, the research highlighted the key barriers and facilitators that should be considered in curriculum development and ongoing quality improvement. Utilizing the CFIR (Damschroder et al., 2009) provided a valuable framework for understanding determinants of implementation, while facilitating theoretical integration with an existing body of literature from implementation science. Predefined core domains and constructs helped structure and give greater meaning to themes that organically emerged in the data.
Key findings underscore the necessity of a comprehensive, multi-level approach to curriculum reform that not only seeks to modify the knowledge, behaviors, and attitudes of health professionals, but simultaneously addresses policies, decision-making processes, resource allocation, and organizational/professional culture. Widespread uptake of cultural safety and anti-racism training interventions will help ensure that the public health system and the wider healthcare system is appropriately and effectively addressing the health needs of Indigenous Peoples throughout Canada. Moreover, because cultural safety and anti-racism target the underlying power dynamics that connect various forms of intersectional oppression, these interventions contribute to broader aims of enhancing health and education systems for all populations.
Supplemental Material
sj-pdf-1-php-10.1177_23733799251349218 – Supplemental material for Implementing Cultural Safety and Anti-Racism Training in Master of Public Health Curricula: A Multi-Institutional Case Study and Practical Self-Assessment Tool
Supplemental material, sj-pdf-1-php-10.1177_23733799251349218 for Implementing Cultural Safety and Anti-Racism Training in Master of Public Health Curricula: A Multi-Institutional Case Study and Practical Self-Assessment Tool by Alex Kent and Malcolm Steinberg in Pedagogy in Health Promotion
Footnotes
Acknowledgements
We extend our gratitude to the many people and groups who generously contributed their knowledge and feedback to inform this work, including the three participating institutions and all study participants. Special thanks to members of the PhD Supervisory Committee, Dr. John O’Neil, Dr. Charlotte Loppie, and Dr. Jeff Reading, for their expertise, advice, and constructive feedback.
Positionality Statements
AK: I position myself in this area of research as a fifth-generation settler of Dutch, British, and Irish ancestry. I have spent most of my life residing on unceded Indigenous lands in Canada, currently, on the territories of the Syilx Okanagan Nation (Kelowna, British Columbia). MS: I locate myself in this area of work as a first-generation settler of South African and Eastern European ancestry, privileged to reside on the Coast Salish territories of British Columbia.
Data Availability Statement
In accordance with the Tri-Agency Open Access Policy on Publications and REB-approved data management protocols, the original qualitative data is not stored in a public data repository. For access to the de-identified data set, please contact the corresponding author.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The authors are employed by academic institutions that were included as cases in the study.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Canadian Institutes of Health Research (grant #394835).
Ethical Approval
Simon Fraser University Research Ethics Board (H20-03950).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
