Abstract


Objective:
Fluorescence-guided laparoscopic partial adrenalectomy (LPA) 1 in patients with a solitary adrenal gland may enable preservation of adrenal function while ensuring disease control.
Materials and Methods:
A 35-year-old woman presented with progressive symptoms, including hirsutism, facial acne, central weight gain, increased appetite, and violaceous abdominal striae over the past 6 months. The patient had previously undergone laparoscopic left adrenalectomy for an adrenocorticotropic hormone (ACTH)-independent cortisol-producing adrenal adenoma measuring 3 cm, with no evidence of tumor or hyperplasia in the right adrenal gland. After a prolonged remission, the patient re-presented in 2024 with clinical and biochemical findings suggestive of disease recurrence. Diagnostic laboratory parameters revealed elevated 24-hour urinary cortisol (235 µg/day; normal range: 3–43 µg/day), suppressed ACTH (<5 pg/mL; normal range: 10–60 pg/mL), and lack of suppression on 1 mg and 2 mg dexamethasone suppression tests. Diagnostic findings were consistent with Cushing’s syndrome, and imaging revealed a new 46 × 30 × 40 mm right adrenal lesion on contrast-enhanced computed tomography with radiological features consistent with a benign adenoma.
Results:
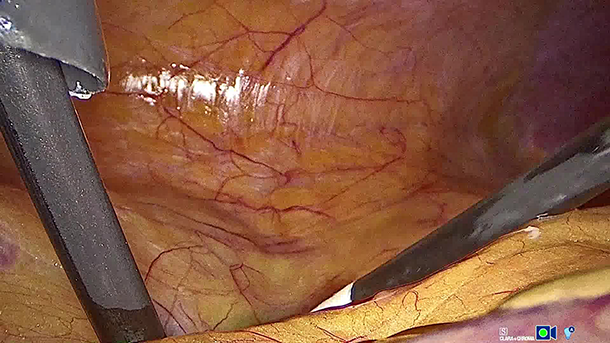
In light of the need to preserve adrenal function, LPA using ICG (indocyanine green) dye with near-infrared fluorescence (NIRF) imaging was planned. The procedure was performed by one of the authors (A.T.). To aid in intraoperative visualization, 5 mg of ICG diluted in 10 mL of sterile water was administered intravenously prior to tumor dissection. The lesion was noted to be hypofluorescent relative to normal adrenal parenchyma. Thus, the resection margin was precisely determined, and the lesion was resected while preserving the rest of the adrenal gland and adrenal vein. Histopathological examination revealed adrenocortical adenoma abundance of Cushing’s syndrome. In our prior series, a total of eight patients with a median age of 39 years underwent LPA using ICG with NIRF imaging for either functional (n = 5) or non-functional adrenal masses (n = 3). The median tumor size and operative time were 43 (23–78) mm, and 70 (50–100) minutes, respectively. All procedures were conducted via a transperitoneal approach and achieved negative surgical margins without perioperative complications or conversion to open surgery. The median follow-up duration was 10 (4–14) months. Postoperatively, no disease recurrence was observed, and all patients maintained adrenal function, obviating the need for steroid replacement therapy. Our current case uniquely demonstrated that LPA using ICG with NIRF imaging in a patient with a solitary adrenal gland successfully preserved adrenal function in the absence of a contralateral gland and highlighting the technique’s precision and efficacy in a challenging clinical situation. In the 3rd month follow-up, the patient remained in complete remission without recurrence or need for ongoing corticosteroid therapy. The morning serum cortisol level at that time was 5.3 µg/dL (normal range: 3–16 µg/dL).
Conclusion:
This case supports the feasibility and safety of fluorescence-guided LPA for a functional benign adrenal lesion in patients with a solitary adrenal gland. To our knowledge, this is the first case in which fluorescence-guided LPA was applied in the resection of benign adenoma in a solitary adrenal gland.
Consent was obtained for the publication of this case report. The author(s) have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
Source of work:
Clinical practice.
The authors of this article have no conflicts of interest to disclose.
Runtime of video:
6 mins 51 secs.
