Abstract
Spinal cord cavernous malformation is a rare and uncommon vascular malformation, it may remain asymptomatic for a long period or manifest as a sudden or gradual change in spinal cord functioning. The diagnosis relies essentially on magnetic resonance imaging (MRI). Surgery constitutes the majority of management with all the complications that can occur during and after surgery. We report a case of intramedullary cavernoma of a 12-year-old patient admitted for acute paraparesia with bowel and bladder dysfunction. MRI revealed 2 intramedullary cavernomas at T6-T7 and T11-T12. Through this case report, we discuss the clinical and radiological characteristics of this unusual intramedullary malformation.
Introduction
Spinal Cord Cavernous Malformation (SCCM) is rare spinal cord lesion representing 5% of intramedullary lesions in adults and 1% of intramedullary lesions in children. 1 These Angiographically concealed vascular abnormalities known as cavernous malformations (CMs) in the central nervous system are characterized by aberrant, larger vascular channels without interposing neural or glial tissue. 2 Patients may present with various symptoms, from asymptomatic to acute or chronic progressive myelopathy. The diagnostic modality of choice for spinal cavernous malformations is MRI.
Case Report
A 12-year-old female child presented to the hospital with acute paraparesis, backache, and bowel dysfunction. There was no family history of similar manifestation. General physical examination found an oriented and alert patient, apyretic with normal cognitive function with motor and sensory deficits of the 2 legs with bowel and bladder dysfunction.
Spine MR imaging revealed 2 intramedullary lesions widening the spinal cord at T6-T7 and T11-T12 with a popcorn appearance and heterogeneous signal in T1 and T2 weighted images, surrounded by a hypointense rim on all sequences (Figure 1) representing hemosiderin. Susceptibility-weighted imaging shows hypointense lesions “blooming” (Figure 2), with adjacent intramedullary hemorrhage, without enhancement (Figure 3).
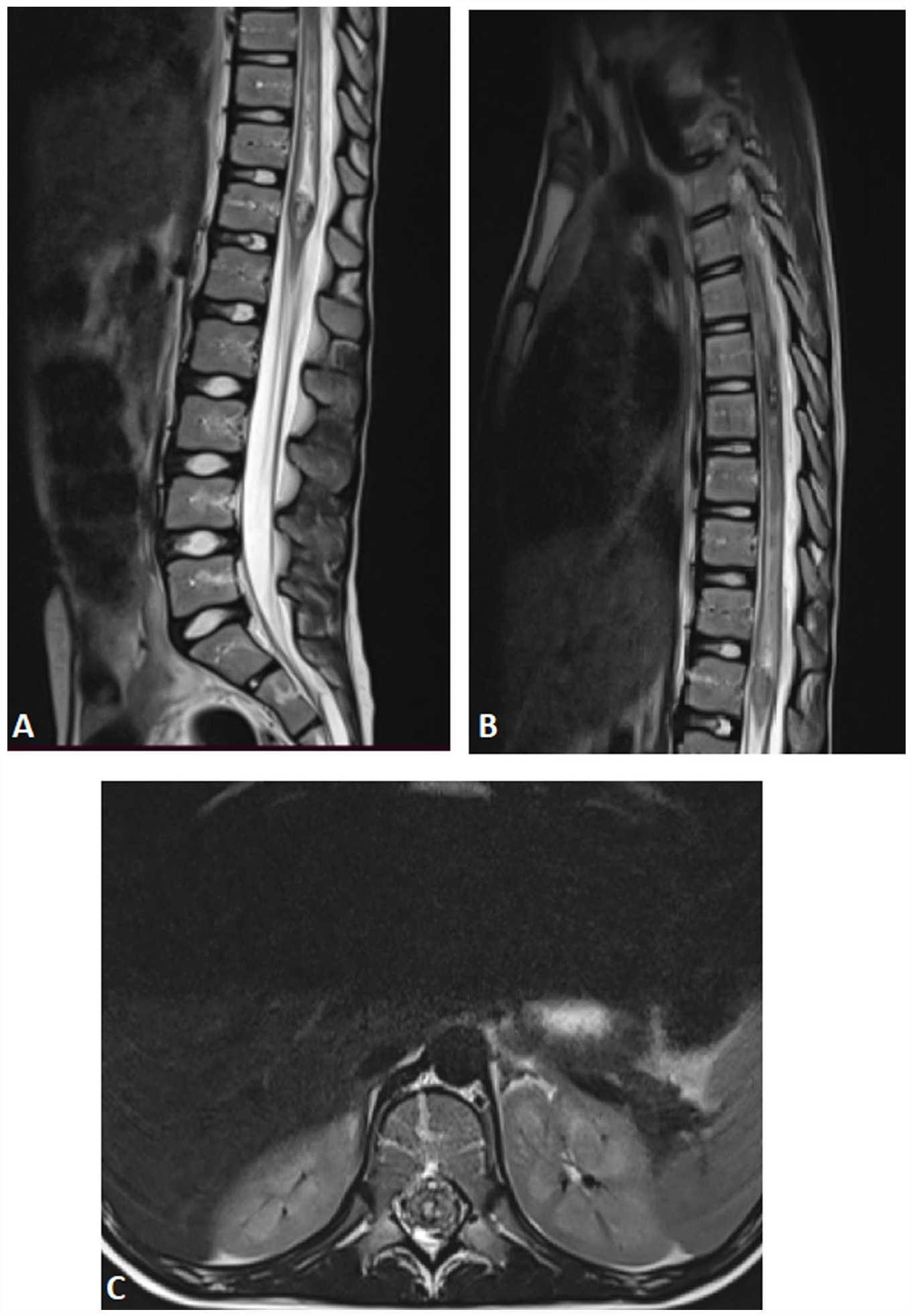
Sagittal (A and B) and axial (C) T2-W spinal MR images shows 2 focal hyperintensity with hypointense edge with surrounding spinal cord edema, this appearance described as « Popcorn ».

Susceptibility-weighted imaging gradient echo (GE) shows hypointense lesions “blooming.”

Sagittal T1-W spinal MR images before (A) and after injection of Gadolinium (B) shows 2 focal hyperintensity with no enhancement (pink arrows), with linear hyperintensity reflect adjacent intramedullary bleeding (yellow arrow).
As a result, the diagnosis of SCCM was established based on clinical presentation and radiological imaging. Unfortunately, the patient didn’t receive any genetic testing for SCCM mutation.
Discussion
SCCMs are dilated capillary-type low-flow vascular malformations that develop over time and are susceptible to recurrent bleeding. 2 They could be discovered in the brain or the spinal cord, and there is a strong link among both multiple cranial CMs and familial transmission, heterozygous loss of function mutations in CCM1/KRIT1, CCM2/MGC4607, and CCM3/PDCD10 genes are identified in about 90% of familial cases of CCMs and two-thirds of sporadic cases with multiple lesions.
Even though SCCMs are less common and considered rare, with comparatively minimal interest in the literature and the majority of reported cases being sporadic nonfamilial, 3 they have a more aggressive clinical course than intracerebral cavernomas, due to the spinal cavity’s narrowness, which has a low tolerance for space-occupying lesions. 4
Every year, the risk of bleeding increases by about 2% to 3%, and patients with a size greater than 1 cm, 5 symptomatic patients, and those with a history of bleeding have significantly higher rates of new bleeding (9% -10%).
The most common signs and symptoms seem to be motor and, sensory disturbances (58%-61%), pain (34%), urinary or bowel dysfunction (24%), and respiratory failure (0.5%) with upper spinal cord involvement. 6
MRI has made tremendous advances in the radiological diagnosis of SCCM. Indeed, it is now the recommended exam for clearly evoking the diagnosis of cavernoma at least in its typical form. The appearance of a reticulated core of mixed signal intensity and a surrounding rim of decreased signal intensity on T2-weighted MRI with minor contrast enhancement suggests the diagnosis.
Susceptibility-weighted imaging offers a high degree of sensitivity for even modest levels of blood products and can help with the identification of these lesions. Adjacent intramedullary bleeding is also common and is typically eccentric and bidirectional. 7
We should note that up to 34% of patients have associated venous malformations, and calcification occurs less frequently than in cerebral cavernous malformations. 8
The differential diagnosis might emerge with a thrombosed arteriovenous malformation (AVM), telangiectasia, or hemangioblastoma. Angiography is rarely used since blood flows very slowly through a cavernous malformation, it cannot provide much useful information. Gadolinium injection afford the distinction between intramedullary hemorrhagic tumors and cavernomas. 7
The therapy is mostly surgical, and the indication arises in the presence of a patient with a neurological disability and the ideal time for surgical intervention in these patients remains controversial while asymptomatic cases require medical treatment with clinical and radiological monitoring. Usually, it’s postponed in cases of abrupt paraplegia to prevent spinal cord aggression by the surgical act, as was the situation with our patient. 9 A recent retrospective study has analyzed the surgical outcomes of the SCCM, 10 and found that surgical strategies should be preferred for severe symptomatic SCCMs avoiding the risk of severe complications with subsequent lesion hemorrhage. Furthermore, earlier (usually within 3 months of symptom duration) surgical resection generally may lead to a better prognosis. Other larger systematics reviews11,12 recommended also that patients with symptoms should undergo surgery within 3 months. However, more research is needed to understand how conservative treatment can be beneficial for symptomatic patients.
The surgical procedure is identical to that used for intramedullary tumor processes. Following a laminectomy and dural opening centered on the pathological zone, the hematoma must be evacuated and the malformation fully removed under a surgical microscope, since they don’t infiltrate the adjacent tissue. 13 Patients with deep-seated lesions might be at higher risk for postoperative deficits specially when the lesions are located in the ventral portion of the spinal cord. 12
Gross et al, in their study, propose the removal of exophytic lesions regardless of clinical presentation, monitoring of asymptomatic deep-seated lesions, and surgical intervention for deep-seated symptomatic lesions only in severe or progressive symptom cases. 14
In the pediatric population, surgical excision of SCM may offer a satisfactory functional result. Although the majority of patients stayed unaltered from their preoperative state, more than half improved throughout a 4-year mean follow-up period. 15
Conclusion
SCCM are rare vascular malformations that can cause various symptoms. The diagnosis is made using MRI, and surgical intervention is mostly used in symptomatic patients. Further research is needed to determine the ideal time for surgical intervention and to improve the treatment of these rare lesions.
Footnotes
Authors’ Contributions
All authors contributed to this work. All authors have read and approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient Consent
Written informed consent for publication was obtained from the legally authorized representative of the patient.
