Abstract
Beta-thalassemia is one of the most frequently occurring hematological disorders in [Removed for blinded peer-review]. Regular blood transfusion is required in almost all cases for management. However, this is associated with significant major complications like red blood cell (RBC) alloimmunization. This retrospective cross-sectional is conducted to evaluate the RBC alloimmunization frequency in children with beta-thalassemia aged between 6 months and 16 years in [Removed for blinded peer-review]. Antibody screening was performed using the Dia clon3 cell antigen panel. If the screening came back positive, a detailed panel was created for the identification of specific antibody. In our sample, the frequency of RBC alloimmunization was found in 22 (26.19%) patients. Of these 22 patients, the Rhesus system was found in most patients 17 (77.3%), followed by Kell 5 (22.7%). RBC alloimmunization was significantly associated with a family history of a blood disorder and splenectomy.
Introduction
Thalassemia, a widespread global genetic disorder, is the inherited disorder of hemoglobin production that leads to fatal anemia and requires daily blood transfusion for management.1-3 Individuals belonging to the South-East Asian, Middle East, and Mediterranean region were affected mainly with thalassemia.4,5 As per the World Health Organization (WHO) statement, among all hemoglobinopathies, beta-thalassemia is the most fatal worldwide and requires strict attention. 6 In different regions of the world, the prevalence of thalassemia has been discovered to be varied. 7 Every year, between 5000 and 9000 children are born with beta-thalassemia. 8
Regular red cell blood transfusion in beta-thalassemia causes complications such as RBC alloimmunization. 9 This complicates red blood cell cross-matching, shortens transfused cell survival in the body, delays the supply of healthy blood transfusion, and speeds up tissue iron loading. 10 Studies reported that alloimmunization rates largely varied in thalassemia patients.11,12 However, there is limited data on the extent of this problem from [Removed for blinded peer-review]. Therefore, the current study aims to determine how common alloimmunization is among patients with thalassemia in the local population. Various blood banks currently provide extensive services day in and day out by making ABO and Rh-D-matched screened blood for transfusion in thalassemic patients. Identifying the scope of the problem will be eye-opening, and the findings will support the development of local guidelines to supply extended phenotypically matched blood to all children who require regular blood transfusions.
Methods
This retrospective cross-sectional research was carried out at the Department of Pediatrics of [Removed for blinded peer-review], from March 2016 to March 2020. Before conducting the study, ethical approval was obtained from [Removed for blinded peer-review]. Moreover, before recruitment in the study, all study participants gave informed consent.
All major thalassemia patients, whose duration since diagnosis was at least 1 month and who had received at least 1 blood transfusion of either sex, aged between 6 months and 16 years, were consecutively included.
All vitally unstable patients requiring ICU admission were excluded. Also, all those receiving blood transfusions due to some other hemoglobinopathies, such as Sickle Cell Disease, Sickle Cell Trait, Hemoglobin C, Hemoglobin E, and Hemoglobin D, were excluded.
Blood was collected in plain tubes for red cell antibody detection. Blood samples for complete blood counts and a direct Coombs Test were collected in Ethylene diamine tetra acetic acid tubes. The antibody screening process was performed using the Dia clon3 cell antigen panel by adding 2 drops of serum and 1 drop of red cell antigens in 3 phases: saline, albumin, and Coombs. Tubes were examined for agglutinating activity and/or hemolysis after centrifugation. All negative tubes had check cells added to them. If the screening was positive (indicated by agglutination or hemolysis), the same procedure was conducted by an expanded panel including Rh, Kell, Duffy, Kidd, MNS antigens to classify the underlying antibodies.
SPSS version 24 was used for statistical analysis. Quantitative variables like age, weight, age at the time of diagnosis, age at the time of the first transfusion, the total number of transfusions, and the number of hospitalizations due to thalassemia were expressed as median, interquartile range. In addition, frequencies and percentages were computed for qualitative variables such as gender, ethnicity, consanguineous marriages, family history of blood problems, splenectomy, blood type, and RBC alloimmunization. Finally, the chi-square/Fisher Exact test and the Mann-Whitney U test were used to investigate inferential statistics, with a P-value of .05 considered significant.
Results
Of 84 patients, the median age was 7 years. 51 (59.5%) males and 33 (40.5%) females. The median weight of the patients was 17.5 kg. The majority of the patients, that is, 50 (58.3%), reported consanguineous marriage. A total of 44 (52.4%) individuals had a family history of blood disorders (Table 1).
Frequency of Categorical Variables.

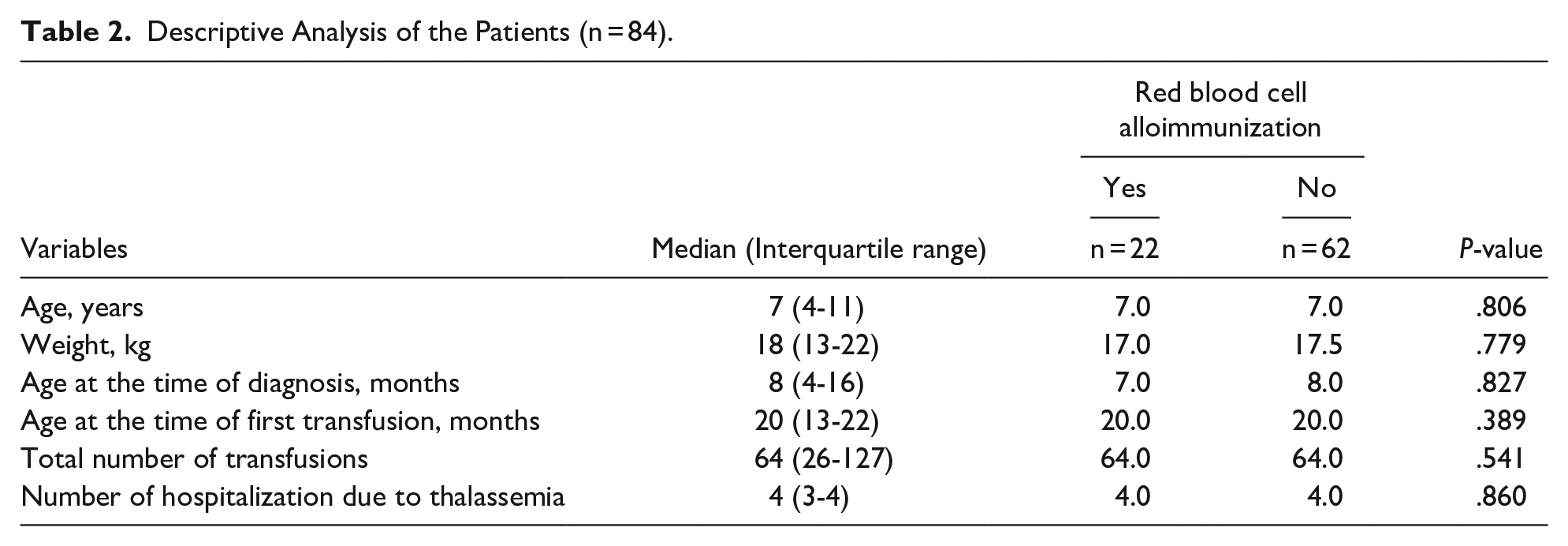
The median age at the time of diagnosis, age at the time of the first transfusion, the total number of transfusions, and the number of hospitalization due to thalassemia was found to be 8 (4-16) months, 20 (13-22) months, 64 (26-127), and 4 (3-4) respectively (Table 2).
Descriptive Analysis of the Patients (n = 84).
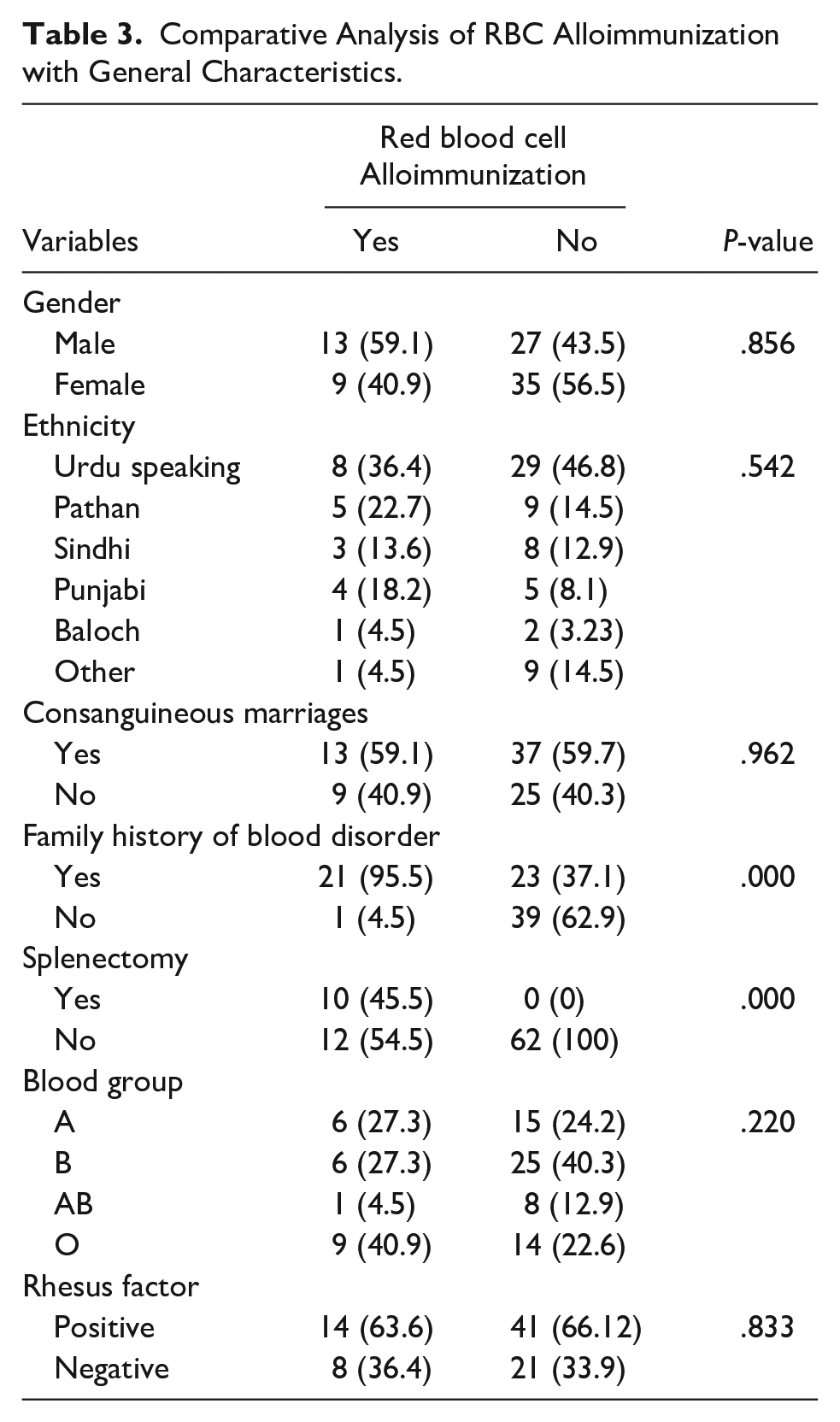
There were 10 (11.9%) patients in whom splenectomy was observed. The blood group showed that group B was observed in the majority, that is, 31 (36.9%) patients, followed by blood group O in 23 (27.4%), blood group A in 21 (25%), and blood group AB in 9 (10.7%) patients. The Rh-positive factor was reported in most patients, that is, 55 (65.5%), whereas Rh-negative was found in 29 (34.5%) (Table 3).
Comparative Analysis of RBC Alloimmunization with General Characteristics.
The frequency of RBC alloimmunization was found in 22 (26.2%) patients. Of these 22 patients, antibodies against the Rhesus system were found in the majority of the patients 17 (77.3%), in which antibodies against E were found in 2 individuals and D was also found in 2 out of the 17 with anti-rhesus antibodies (due to false negative results in blood donors with weak D typing). Antibodies against Kell were found in 5 (22.7%) individuals (Table 1).
A significant association of RBC alloimmunization was found with a family history of a blood disorder (P-value .000) and splenectomy (P-value .000) (Table 3). However, upon performing binary logistic regression on splenectomy and family history of blood disorder, both were not independent risk factors for RBC alloimmunization after controlling for gender, ethnicity, blood group, age, consanguineous marriage, and age at first transfusion (Table 4)
Binary Logistic Regression.

Discussion
The current study findings have revealed the frequency of RBC alloimmunization in twenty-six percent of thalassemic patients. Similar to findings of this study, a study conducted in Egypt, anti-red cell alloantibodies were detected in almost twenty-three percent of major thalassemia patients. 13 Moreover, a study from Saudi Arabia reported twenty-two percent, and a study from China reported 23% prevalence.14,15 However, a lower alloantibodies prevalence was reported in studies conducted in the neighboring country Iran, where prevalence ranges from 2.87% to 18.7%.16-18 In addition to this, studies conducted from other parts of Asia also reported a lower prevalence compared to the current study findings.16,18-21 In a recent survey conducted in Iraq, a much lower prevalence was also reported. 23 The uniformity of RBC antigens in blood donors and recipients is thought to cause the decline in alloimmunization. Some alloantibodies are hemolytic, resulting in hemolytic transfusion responses and reducing the number of compatible RBC units available for transfusion. Others are negligible from a clinical standpoint. 19 In addition, it appears that delaying a regular transfusion schedule increases the occurrence of RBC alloimmunization.19-23
According to the current study findings, of twenty-two patients in whom alloimmunization was observed, the Rhesus system was observed in around seventy-seven percent of the cases. Furthermore, Kell was found in approximately twenty-three percent. A previous study recorded that 72% of the cases with RBC alloimmunization, were anti-Rhesus systems, and sixty-four percent were anti-Kell. More than a single alloantibody was found in nearly half of these patients. 24
No significant difference in age, weight, gender, and consanguineous marriage was observed in the current study with alloimmunization. The non-significant association of gender with alloimmunization was also reported in previous studies.20,25,26 Furthermore, similar to the present study findings, Ghasemi et al 18 reported a non-significant association of alloimmunization with not only gender but age as well.
The current study’s findings also reported no significant median difference in age at the time of diagnosis of thalassemia, age at the time of the first transfusion, the total number of transfusions, and the number of hospitalizations in patients with and without alloimmunization. Abdulqader et al 22 also reported somewhat similar findings in their study.
In the current study, all patients with splenectomy had alloimmunization. Similar findings were reported in previous studies as well.19,22,27
However, in a few studies, a lower prevalence of alloimmunization with splenectomy was also reported.22,28-30
The research’s findings could be featured because this study reported results from a single center of [Removed for blinded peer-review]. Moreover, certain important factors like the history of transfusion reaction and the comparison of different detection methods were not studied. Moreover, the current study was conducted in an Urban setting that might not generalize to the larger at-risk population. Despite these limitations, this study has reported current estimates of alloimmunization in thalassemia patients of our people. Furthermore, the presence of antibodies in positive cases was also reported. The present study’s findings further highlighted the relevance of using cross-matched blood from the start of the transfusion in patients with thalassemia major. It is also suggested that the types of alloantibodies existing in the region’s population should be determined and that thalassemia patients should be given blood with utmost compatibility to prevent the development of alloantibodies more effectively. Further large-scale multicenter studies are recommended to preclude the outcome of this study.
Conclusion
Alloimmunization in routinely transfused beta-thalassemia patients is a severe issue in our part of the globe, as shown by the high prevalence of RBC alloimmunization in the current research.
Footnotes
Acknowledgements
No acknowledgments
Authors’ Contributions
Kiran Minhas, Muzamil Shabana Ejaz, and Alaa Tukruna: Wrote the initial draft of the manuscript and constructed the questionnaire; Aabiya Arif: performed the statistical analysis; Maryam Haider and Sameer Saleem Tebha: Wrote the discussion and edited the manuscript, along with the final review and proofreading of the manuscript; All authors approved the final version for publication.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethics approval for the study was given by the Ethics committee of Dow University of Health Sciences
Data availability statement
Not applicable
