Abstract
Pediatric populations from lower-income countries may experience a higher incidence of zinc deficiency, which may cause physical and neurological dysfunctions. This case control study aims to assess different levels of zinc between malnourished and well-nourished children. Our study included 108 participants, all children less than 12 years of age. Out of the 108, 54 were malnourished children (cases), while 54 were well nourished (control group) and were screened for zinc deficiencies. Zinc deficiencies were 4 times more common in malnourished cases than in controls (OR: 3.89 95% CI: 1.1-14.9) with median value of zinc in cases being 91.69 and that of controls was 117.6. Our findings indicate significant deficiencies in malnourished children as compared to well-nourished children. Additionally, our findings support literature surveyed that suggest dietary changes alone would not be able to replenish zinc levels in children.
Introduction
Malnutrition is an alarming international issue resulting in indelible negative impacts on the physical and mental growth of children, along with immune deficits and cognitive impairment. Malnourishment can lead to severe macronutrient deficiencies in children including protein calorie malnutrition that has dreadful impacts on a child’s health. Micronutrient deficiency is now becoming a significant issue with deleterious outcomes. 1 Zinc is an essential micronutrient required by the body to perform several biochemical reactions. Zinc is mostly stored in the skeletal muscles, and the total amount of zinc in an adult human body is approximately 2 to 3 g, with a daily requirement of 12 to 16 mg/day.2,3 Decreased intake, malabsorption or high loses of micronutrients from the gut may lead to zinc deficiency, resulting in impaired growth, neuronal abnormalities, iron deficiency anemia due to decreased iron absorption, and even cardiovascular diseases. 2 With zinc deficiency targeting more than 2 billion people worldwide, it results in more than 0.5 million deaths per year in infants and children below 5 years of age.2,4
With no stored forms of zinc in the human body, a regular dietary intake of this micronutrient is essential for maintaining recommend amounts. Pediatric populations and women from lower-income countries, including sub-Saharan Africa and South-East Asia, who usually consume plant-based diets may experience higher incidence rates of zinc deficiencies.5,6 Countries with more than 25% of their population consuming a zinc-deficient diet are considered to be at-risk of developing zinc deficiency. 7 With roughly 17% of global population consuming a zinc-deficient diet, around a quarter of the pediatric population below the age of 5 suffers from stunted growth. 8 In Pakistan, as concluded by Khalid et al, 3 20.6% of the pediatric population of Pakistan had zinc levels below 60 μg/dL.
Several measures have been taken in order to counter zinc deficiency and to prevent its occurrence, including recommendations by the WHO and UNICEF to administer 20 mg oral zinc supplements for 10 to 14 days in children suffering from diarrhea to recover micronutrient losses, as zinc supplements reduce deaths by diarrhea as well as from pneumonia in children by 13% and 15%, respectively.9,10 Various other international agencies and groups have also lent their hands in tackling the prevalence of zinc deficiency through a diverse range of initiatives, including Food Fortification Initiative, Global Alliance for Improved Nutrition, HarvestPlus, International Zinc Association and Micronutrient Forum.11-15 The National Wheat Flour Fortification Program in Pakistan was introduced to fortify wheat flour with zinc to rectify zinc deficiencies. 16
While many studies have been conducted to evaluate zinc deficiency and its prevalence, they have only quantified the frequency of zinc deficiencies sans any comparison to otherwise-healthy children—with or without diarrhea. There is, however, minimal data that compares the prevalence and levels of zinc deficiency in malnourished children with a healthier population in the Pediatric age group. This case-control study aims to assess different levels of zinc between malnourished cases, and healthier controls, to better understand the prevalence of zinc deficiency, and its control.
Methods
This case-control study was conducted in the pediatric department of AbbasI Sheheed Hospital, Karachi Pakistan. The Institutional Review Board (IRB) of Abbasi Shaheed Hospital approved this study.
The sample size was calculated through non-probability consecutive sampling in a 1:1 ratio of controls verses cases of zinc deficiency.
Participants between the ages of 2 months to 12 years, cases with <−2 SD weight for their age, and controls with a normal weight for their age were all included in the study. Informed consent was taken from parents and guardians. Children who were malnourished below 3 SD, those on zinc supplementations, and those with chronic illnesses—chronic renal failure, type 1 diabetes, cardiac diseases—were excluded from the study.
Cases were enrolled from in-patient departments and healthy controls were enrolled form the OPD and vaccination centers. Baseline variables—age, sex, and weight—were taken. For the zinc analysis, 3 mL of blood was collected into plastic tubes (Nalgene Sybron Corporation, Rochester, New York), and centrifuged within an hour to avoid hemolysis. Outcomes were then assessed for a zinc deficiency. The researcher on pre-approved proforma recorded the information.
Data was entered and analyzed using SPSS version 18. Frequency and percentages were recorded for qualitative variables like sex and zinc deficiency. Mean ± SD were recorded for quantitative variables like age, weight, and serum zinc level. A logistic regression was applied to calculated odds ratio and a 95% confidence interval (CI). Stratification was done based on age, sex, and weight for possible effects as confounders through the chi-square test. P < .005 was considered as significant.
Results
A total of 108 children were included in this study, with equal number of (n = 54) malnourished cases and healthy controls. Age distributions for all children are presented in (see Figure 1). 22.22% of cases and 14.81% controls were below 1 year of age. 33.33% cases and 42.59% controls were between ages 1.1 and 5 years of age. The Majority of participants fell in the age group 5.1 to 12 years of age with 44.44% cases and 42.59% controls. The median age of all participants was 5 (IQR = 7.2) years. The average age and weight of the children had no significant impact on zinc deficiency between cases and controls (see Table 1). Out of 108 children, 63 (58.3%) were male and 45 (41.7%) were female. Gender distribution with respect to cases and controls is presented in (see Figure 2).

Age distribution with respect to age groups.
Comparison of Characteristics Between Cases and Control Groups.


Gender distribution according to groups.
The average serum zinc was significantly low in cases as compared to control (P = .0005), with the median value of zinc in cases being 91.69, and 117.61 in controls. This is shown in (see Table 2), which illustrates that zinc deficiencies were 4 times more common in cases as compared to controls (OR: 3.86 95% CI: 1.1-14.9). Zinc deficiencies were shown to stay fairly consistent across age groups. The rate of patients with a zinc deficiency was also not significantly different when sex was taken into account. No significant difference was observed for children below and equal to 15 kg, and those above. A multivariate logistic regression model was used to predict zinc deficiency (see Table 3). Malnourished children (our cases) were significantly associated with zinc deficiency.
Zinc Deficiency in Malnourished Children as Compared to Healthy Children.
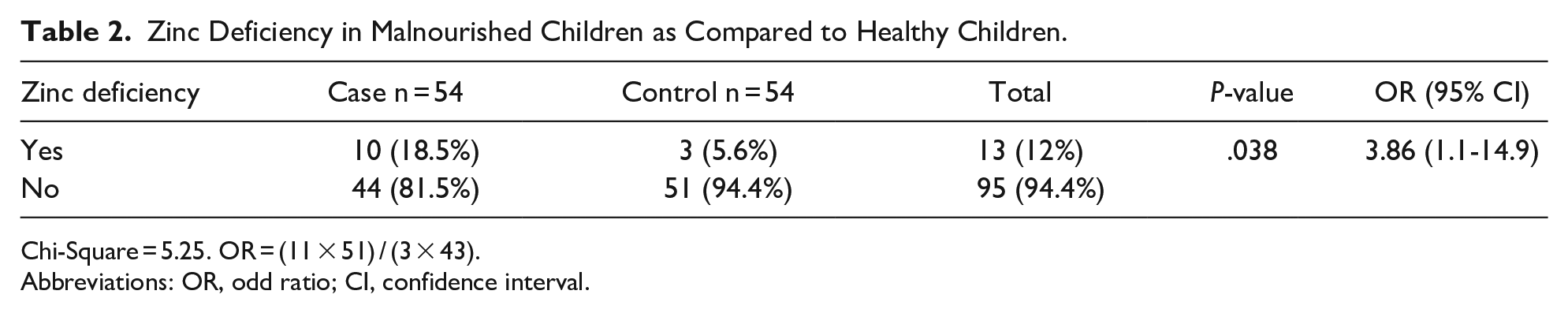
Chi-Square = 5.25. OR = (11 × 51) / (3 × 43).
Abbreviations: OR, odd ratio; CI, confidence interval.
Multivariate Logistic Regression Model to Predict Zinc Deficiency.

Discussion
Zinc is a vitally important micronutrient in the human body that plays many roles, including normal gene functioning, cellular growth, reproduction and the maintenance of the immune system. 16 Deficient zinc levels may result in growth restrictions; neurological deficits, poor wound healing, and reduced sensation of taste.17-19 With approximately 50% of the global population suspected to be consuming zinc-deficient diets, inadequate zinc levels are also linked to the deaths of more than 800 000 children below the age of 5 due to diarrhea, pneumonia and malaria.20,21 Even after an adequate intake of dietary zinc, a high intake of Phytate—an inhibitor of zinc absorption and resent in plant-based diet such as cereals, legumes and whole grain—can also lead to a zinc deficiency. Bioavailability of zinc and the inhibitory effect of phytate over zinc absorption can be assessed using the phytate/zinc molar ratio. 22
Our study documents the prevalence of zinc deficiency in malnourished children when compared to an otherwise healthier pediatric population. Several other studies have reported zinc deficiency in children, but no comparison with well-nourished population has been drawn. In a study conducted in the urban slums of Peshawar, Pakistan, malnutrition was observed in children between the ages of 6 and 24 months. 23 Eijaz and Latif 24 conducted a similar study to evaluate the pattern of growth restriction in malnourished patients, and included study participants between the ages of 12 to 23 months. In our study, the median age of study was 5 (IQR = 7.2) years. A previous study revealed that males (58.3%) were slightly more affected than females (41.7%). Local data also showed similar findings, reporting that males (53%) were slightly more affected than females (47%). 24
Compared to adults, children require more zinc for their daily functions, and for the fact that they are more likely to deplete zinc stories in their body if not otherwise replenished. In 1 study, children with malnutrition had serum zinc levels that were significantly low when compared to healthy, well-nourished controls (P = .0005). A similar result was also observed in Khubchandani et al 25 study where serum copper levels and serum zinc were reduced (P < .05) when compared between malnourished and well-nourished children.
Additionally, Ahmad et al 26 and Javeed et al 27 concluded that malnourished children are significantly zinc-deficient (P value <.0001), further supporting the findings of our study. Similarly, data from other developing nations such as South America, Turkey, India, and Bangladesh also shows a pattern of zinc deficiencies in malnourished children. A systematic review performed in Latin America and the Caribbean showed that 19.1% to 56.3% of children under 6, and women between the ages 12 to 49, had a significant zinc deficiency. 28 A similar study was carried out in the Altindag district of Ankara, Turkey, concluding that 27.8% of the pediatric population suffered zinc deficiencies, considering serum zinc levels, dietary intake and the prevalence of stunting in these children. 29 Additionally, India, where malnourishment in children is prevalent (47% of all children), showed major zinc deficiency levels of 43.8% in its children—attributed primarily to low socio-economic statues and a decreased dietary intake of zinc according to Akhtar. 16 In our study, similar results were concluded from malnourished children, with prevalence rates of 18.8% in children less than 15 kg, and 18.2% in children more than 15 kg. Similar results were gathered from a study in Bangladesh, with 43% of children showing stunted growth, suggesting a zinc deficiency. 30
The majority of physicians and nutritionists prescribe dietary supplementation as the primary intervention for various nutritional deficiencies; however, a study conducted by Elizabeth et al on malnourished children less than 5 years of age, as compared to controls, for a period of 3 months, showed no significant difference pre-and post-supplementation effects of magnesium, zinc, copper, calcium, and albumin. It proposed that dietary supplementation alone was inadequate in replenishing nutritional deficiencies in children with protein energy malnutrition (PEM), which required the additional supplementation of micronutrients and trace elements. 31 As children with PEM are already immune-compromised, zinc deficiencies can leave them more vulnerable to diseases like pneumonia and diarrhea. Zinc supplementation aids in avoiding adverse outcomes, whilst also enhancing growth, promoting would healing, and reducing the incidence of infections.32-34 In order to stave off the negative effects of a zinc deficiency, along with an iron deficiency, among infants and children, the WHO has set various goals for doctors and nutritionists to tackle this issue, which includes the reduction of stunting in children less than 5 years of age by 40% and a 5% reduction in childhood wasting. 35 Zinc supplementation, zinc fortification, and a diverse dietary intake have also been found to be beneficial in preventing a zinc deficiency. 36 These measures, if followed accurately might help doctors and nutritionists to make this world a better place for a pediatric population currently suffering from malnutrition and its complications.
Our study directly demonstrates this relationship, and if not for ethical considerations, a delayed treatment plan would have allowed aforementioned adverse outcomes to manifest. Therefore, in order to address the specter of malnutrition, a national, as well as international, strategy should be developed to address its burden on developing nations. Our study faced some major limitations, including in the assessment of the long-term consequences of zinc-deficiency. Due to ethical concerns, patients were supplemented for deficiencies, while financial constraints of from the institution limited us to testing only for zinc deficiencies as opposed to more. Lastly, since a large majority of our patients belonged to socioeconomically disadvantaged groups, follow-up after discharge was impossible.
Conclusion
Zinc deficiency has extreme multisystem effects and is more common in the malnourished pediatric population than in well-nourished children. Our findings have conclusively proven a significant difference in serum zinc level between malnourished and well-nourished children. Moreover, our findings were able to help clinicians to predict the course of the patient, which led them to develop successful intervention plans that were beneficial for patients. Since the financial status of families did not allow for dietary replacement, and literature also suggested that dietary replacement alone would not be beneficial, zinc supplementation was chosen as the primary mode of intervention. Zinc supplementation should be used to compensate for the zinc-deficiency during rehabilitation from malnourishment. Our study has the unique distinction of being the only case-control comparison with such a high significance in malnourished children.
Footnotes
Acknowledgements
The authors would like to acknowledge all the children the developing world and beyond that suffer from nutritional deficiencies of any kind and hope that eventually malnutrition could be eradicated.
Author Contributions
All authors contributed equally towards the development of this manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Ethics
The Institutional Review Board (IRB) of Abbasi Shaheed Hospital, Karachi, Pakistan, approved this study.
